Understanding stomatitis in adults symptoms pictures is paramount for effective diagnosis and management. This comprehensive article delves into the diverse manifestations of stomatitis in adults, detailing visual cues and associated discomfort to facilitate early identification and appropriate intervention.
stomatitis in adults Symptoms Pictures
Recognizing the stomatitis in adults symptoms pictures is the first step towards seeking appropriate care. Stomatitis, an inflammatory condition affecting the oral mucosa, presents with a wide array of symptoms that can range from mild discomfort to severe pain, significantly impacting daily activities like eating, speaking, and swallowing. The clinical presentation varies depending on the underlying cause, but common visual and experiential symptoms include:
- Oral Ulcers and Sores: These are among the most common and distressing symptoms of stomatitis. They appear as breaks in the oral mucosal lining, exposing sensitive underlying tissues.
- Aphthous Ulcers (Canker Sores): Typically round or oval with a distinct red halo and a yellowish-white pseudomembranous center. They range in size from a few millimeters (minor aphthae) to over a centimeter (major aphthae) and are exquisitely painful, especially when touched or exposed to certain foods. Major aphthae can be deeper, take weeks to heal, and may leave scars. Herpetiform aphthae appear as numerous pinpoint ulcers that often coalesce into larger, irregular lesions.
- Herpetic Ulcers: Initially manifest as clusters of small, fluid-filled vesicles on a reddened base. These vesicles rapidly rupture, forming shallow, painful ulcers that often crust over, particularly on the lips. They tend to occur on keratinized tissues such as the attached gingiva, hard palate, and vermilion border.
- Traumatic Ulcers: Often irregular in shape, caused by physical injury such as biting the cheek, sharp tooth edges, or ill-fitting dentures. The location often provides a clue to the etiology.
- Redness (Erythema) and Swelling (Edema): Inflammation often leads to areas of the oral mucosa appearing visibly redder than surrounding healthy tissue. This erythema can be localized around a specific lesion or diffuse, covering larger areas. Swelling, or edema, is also common, making the affected tissues appear puffy and sometimes causing a sensation of fullness or tightness in the mouth. In denture stomatitis, for example, the palate beneath the denture often appears uniformly red and swollen.
- Burning Sensation or Pain: A burning or stinging sensation is a frequent complaint, often preceding the appearance of visible lesions (prodromal symptom) or accompanying existing ones. The pain can range from a dull ache to sharp, intense discomfort, exacerbated by hot, spicy, acidic, or rough foods. This symptom is particularly prevalent in conditions like aphthous stomatitis, oral candidiasis, and some forms of glossitis.
- Difficulty Eating, Drinking, or Speaking: Due to the pain and inflammation, individuals with stomatitis often experience significant challenges with mastication and deglutition. Chewing and swallowing can become arduous, leading to reduced food intake, dehydration, and potential weight loss. Speech may also be impaired if lesions affect the tongue, lips, or soft palate, causing slurred words or an altered voice quality.
- Dry Mouth (Xerostomia): While not a primary symptom of all stomatitis types, dry mouth can exacerbate the discomfort of oral lesions and make the mucosa more susceptible to injury and infection. Conditions that cause stomatitis can sometimes also affect salivary gland function, or painful lesions might make it difficult to drink enough fluids, leading to secondary xerostomia.
- Bleeding: Fragile or severely inflamed tissues can bleed easily, especially during brushing, eating, or even spontaneous instances. Ulcerated lesions might present with a hemorrhagic base or surrounding petechiae. This is particularly noticeable in severe forms of desquamative gingivitis or necrotizing ulcerative stomatitis.
- Altered Taste Perception (Dysgeusia): Inflammation and the presence of lesions on the tongue or other taste-bud-bearing areas can interfere with normal taste perception, leading to a metallic, bitter, or generalized loss of taste. This symptom can further contribute to a reduced appetite.
- Fever and Malaise: Systemic symptoms such as fever, fatigue (malaise), and generalized body aches can accompany more severe or widespread forms of stomatitis, particularly in primary herpetic gingivostomatitis or stomatitis secondary to systemic infections or autoimmune conditions. Lymphadenopathy (swollen lymph nodes) in the neck is also a common associated sign, indicating an active immune response.
- Cracking and Fissuring: Especially notable in angular cheilitis (perleche), which affects the corners of the mouth. This presents as painful cracks, fissures, erythema, and crusting at the labial commissures. The lesions can extend onto the perioral skin and are often caused by a combination of fungal (Candida) or bacterial infections, along with moisture accumulation.
- White Patches or Plaques: In conditions like oral candidiasis (thrush), creamy white, cottage cheese-like patches are observed on the tongue, buccal mucosa, palate, or throat. These pseudomembranous lesions can often be wiped away, revealing an underlying erythematous or bleeding surface. Other white lesions, such as those seen in oral lichen planus or leukoplakia, may be firmly adherent and cannot be removed by scraping, indicating different underlying pathologies.
Signs of stomatitis in adults Pictures
Observing the specific signs of stomatitis in adults pictures provides crucial diagnostic clues, guiding healthcare professionals toward the correct etiology and treatment plan. These objective clinical manifestations offer a more detailed insight into the nature and severity of the oral inflammation. Key observable signs include:
- Erythematous Patches and Macules: These are flattened, reddened areas of the oral mucosa that may be localized or diffuse. They indicate inflammation and increased blood flow to the affected tissue.
- Diffuse Erythema: Often seen in denture stomatitis, where the entire palatal mucosa covered by a denture appears uniformly red.
- Focal Erythema: A red patch that might represent an early lesion, such as the initial stage of an aphthous ulcer or the base around a developing vesicle.
- Maculopapular Rash: Flat (macular) or slightly raised (papular) reddened areas that can be associated with systemic viral infections or drug reactions, sometimes extending into the oral cavity.
- Ulcerative Lesions: These are distinct breaks in the continuity of the oral epithelium, characterized by loss of tissue.
- Round/Oval Ulcers with Halos: Characteristic of minor aphthous stomatitis, with a distinct red inflammatory halo surrounding a yellowish-gray fibrinopurulent membrane.
- Irregularly Shaped Ulcers: Often seen after the rupture of vesicles (e.g., herpetic stomatitis, erythema multiforme) or traumatic injuries. These ulcers can vary significantly in size and depth.
- Deep, Crater-like Ulcers: Indicative of major aphthous stomatitis or more severe conditions, potentially leading to scarring upon healing.
- Vesicles and Bullae: These are fluid-filled lesions, differing primarily in size.
- Vesicles: Small (typically less than 5 mm) blisters, frequently seen in herpetic stomatitis, where they appear in clusters before rupturing into ulcers.
- Bullae: Larger (greater than 5 mm) blisters, indicative of conditions such as pemphigus vulgaris, mucous membrane pemphigoid, or erythema multiforme. These lesions are generally fragile in pemphigus and tense in pemphigoid, rapidly rupturing to form extensive erosions.
- White Patches and Plaques: These can be categorized by their removability.
- Pseudomembranous Plaques: Creamy white, “cottage cheese” like lesions that can be scraped off, revealing an erythematous or bleeding base. This is the hallmark of acute pseudomembranous candidiasis (thrush).
- Non-Removable White Plaques: Firmly adherent white lesions that cannot be scraped away. Examples include leukoplakia, oral lichen planus (reticular pattern with Wickham’s striae), and hyperkeratosis. These require careful diagnosis to rule out premalignant or malignant changes.
- Fissures and Cracks: Linear ulcerations or grooves in the mucosa.
- Angular Fissures: Cracks at the commissures of the lips, characteristic of angular cheilitis. These can be shallow or deep, often with associated erythema and crusting.
- Tongue Fissures: Deep grooves on the dorsal surface of the tongue, which can become inflamed or infected in stomatitis, particularly if coupled with a dry mouth.
- Edema (Swelling): Observable enlargement of oral tissues due to fluid accumulation. This can make the mucosa appear puffy and distorted. It often accompanies erythema and can lead to indentations from teeth (scalloping).
- Atrophy: Thinning of the oral mucosa, causing it to appear smooth, shiny, and often redder due to the underlying vasculature being more visible. Atrophic glossitis (bald tongue) is a classic example, where the papillae are lost, leaving a smooth, red, and often painful tongue, commonly associated with nutritional deficiencies.
- Petechiae and Purpura: Small (petechiae) or larger (purpura) red or purple spots representing extravasated blood into the tissues. They indicate capillary fragility or a bleeding disorder. Can be seen in viral infections (e.g., infectious mononucleosis) or thrombocytopenia.
- Lymphadenopathy: Palpable enlargement of regional lymph nodes (submandibular, cervical) indicates an inflammatory or infectious process in the oral cavity. The nodes may be tender to the touch and firm.
- Crusting and Coalescence: Lesions, especially on the lips and perioral skin (e.g., herpetic lesions, erythema multiforme), can develop a hemorrhagic crust as they heal or when fluid-filled lesions rupture and dry. In some conditions, multiple smaller lesions may merge to form larger, more extensive areas of involvement.
Early stomatitis in adults Photos
Early identification of early stomatitis in adults photos is crucial for prompt intervention and preventing the progression to more severe or widespread disease. The initial stages of stomatitis are often subtle, characterized by a range of prodromal symptoms and minor visual changes that might be easily overlooked. Recognizing these nascent signs can significantly impact the course of the condition. Key early indicators include:
- Prodromal Sensations: Before any visible lesion appears, many types of stomatitis begin with specific sensations.
- Localized Tingling, Burning, or Itching: This is a very common early warning sign, particularly for aphthous ulcers and herpetic lesions. The sensation is typically confined to the exact spot where the lesion will subsequently erupt, lasting for a few hours to a day.
- Mild Soreness or Discomfort: A vague, localized tenderness or sensitivity in a specific area of the mouth, which may become more pronounced with touch or mild irritation. This can be an early indicator of developing inflammation.
- A Feeling of Roughness or “Tightness”: A subtle change in the texture or sensation of a specific area of the oral mucosa, often preceding more significant swelling or lesion formation.
- Focal Redness (Erythema): One of the earliest visible signs is a small, circumscribed area of redness. This initial erythema indicates localized inflammation and increased blood flow to the site.
- For an aphthous ulcer, a small red macule or papule might appear before the central ulceration develops.
- In herpetic infections, pinpoint red spots often precede the formation of vesicles.
- In early denture stomatitis, a very light blush of redness might be observed on the palate before diffuse erythema becomes apparent.
- Slight Swelling or Elevation: A localized, barely perceptible elevation or swelling of the oral mucosa can be an early sign. This slight edema might feel like a small bump to the tongue, even if it’s not yet clearly visible.
- In some cases, a small, soft papule or mound may precede ulceration or vesicle formation.
- For allergic reactions, a localized area of slight swelling might be the first indication before more widespread edema or vesiculation.
- Pinpoint Vesicles or Pustules: In conditions like herpetic stomatitis, the very first visible lesions can be extremely tiny, fluid-filled vesicles or pus-filled pustules. These are often difficult to discern with the naked eye and may quickly coalesce or rupture, making their initial appearance fleeting. Recognizing these early, minute lesions is key for timely antiviral therapy.
- Nascent Ulcerations or Erosions: Once a vesicle ruptures or an early inflammatory papule erodes, a very shallow, often irregular ulcer forms. At this initial stage, the base of the ulcer might not yet have developed the characteristic yellowish-gray pseudomembrane typical of more mature lesions. The borders might also be less defined than later stages.
- Subtle White Specks or Film: For conditions like oral candidiasis, the earliest signs might be isolated, sparse white specks on the mucosa that are easily wiped away, rather than the thick, creamy plaques seen in more advanced stages. These represent initial colonization and biofilm formation by Candida.
- Minor Cracking at the Corners of the Mouth: In early angular cheilitis, there may only be minimal dryness, slight erythema, and a very shallow crack at the commissures, which may progress to deeper fissures and crusting if untreated.
- Changes in Mucosal Texture: A subtle alteration in the smooth texture of the oral lining, perhaps a slight rough patch or a dullness to the usually shiny surface, can be an early indication of developing inflammation or hyperkeratosis.
These early signs of stomatitis, whether sensory or visual, underscore the importance of regular oral self-examination and prompt consultation with a healthcare professional. Early detection often allows for simpler, more effective treatment and prevents the condition from becoming more painful, extensive, or complicated. Maintaining good oral hygiene and being aware of any new or unusual sensations within the mouth can greatly aid in recognizing stomatitis at its most nascent stages.
Skin rash stomatitis in adults Images
When skin rash stomatitis in adults images are considered, it points to systemic conditions where oral lesions are accompanied by dermatological manifestations elsewhere on the body. These presentations are often more severe and can indicate a serious underlying disease requiring prompt and specialized medical attention. Understanding the co-occurrence of oral and skin lesions is critical for accurate diagnosis and management. Key conditions exhibiting both oral stomatitis and skin rashes include:
- Erythema Multiforme (EM):
- Oral Lesions: Often severe and debilitating. They begin as bullae (large blisters) that rapidly rupture to form widespread, painful erosions and ulcers with a characteristic hemorrhagic crust, especially on the lips. The buccal mucosa, tongue, and palate are frequently affected, making eating and drinking extremely difficult.
- Skin Rash: The hallmark is the “target lesion” (or iris lesion), which consists of concentric rings of erythema and edema, often with a darker center or vesicle. These lesions typically appear suddenly on the extremities (palms, soles), face, and trunk. EM is often triggered by infections (e.g., Herpes Simplex Virus) or medications.
- Stevens-Johnson Syndrome (SJS) and Toxic Epidermal Necrolysis (TEN):
- Oral Lesions: These are life-threatening conditions. Oral involvement is severe, presenting with extensive, painful bullae and erosions that are often hemorrhagic and cover large areas of the oral mucosa, pharynx, and even the esophagus. Profound difficulty with hydration and nutrition is common.
- Skin Rash: Characterized by widespread erythematous macules and atypical target lesions that rapidly progress to blistering and epidermal detachment (skin peeling). SJS involves less than 10% of the body surface area (BSA) detachment, while TEN involves more than 30% BSA detachment. These conditions are typically drug-induced and require immediate hospitalization.
- Oral Lichen Planus (OLP) with Cutaneous Lichen Planus:
- Oral Lesions: OLP manifests in various forms: reticular (most common, lacy white lines known as Wickham’s striae, often on the buccal mucosa), papular, plaque-like, atrophic (red, shiny, tender mucosa), erosive (painful, raw areas), or bullous (blisters that rupture into ulcers). Oral lesions can be persistent and may undergo malignant transformation in erosive forms.
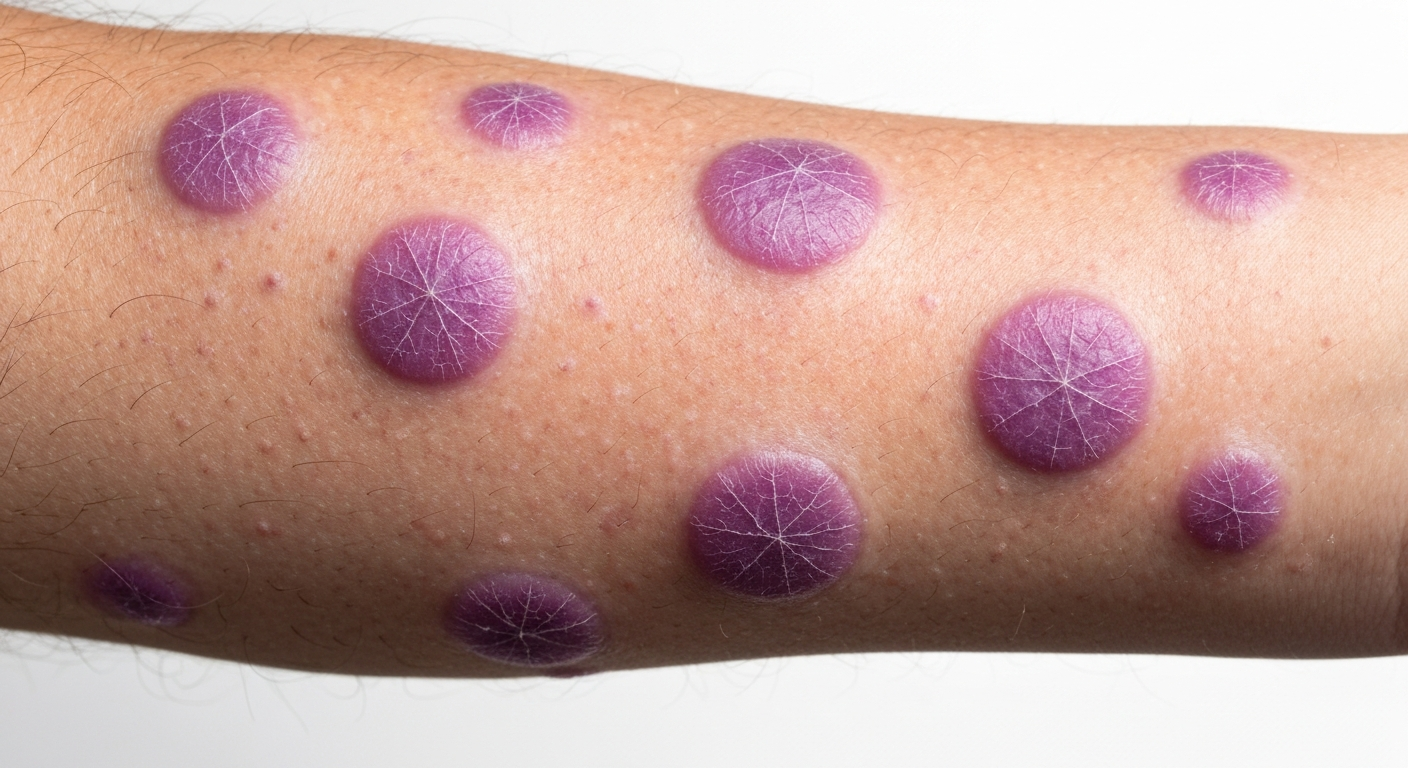
- Skin Rash: The classic presentation is pruritic (itchy), purple, polygonal, planar papules and plaques. These lesions commonly affect the flexor surfaces of the wrists and ankles, lower back, and shins. Fine white striae (Wickham’s striae) can sometimes be seen on the surface of the skin lesions.
- Pemphigus Vulgaris (PV):
- Oral Lesions: Often the initial manifestation, preceding skin lesions by months. Flaccid bullae (blisters) form but rupture almost immediately upon formation, leaving painful, persistent, irregularly shaped erosions. A positive Nikolsky’s sign (the ability to dislodge superficial epidermis by lateral pressure) is often present.
- Skin Rash: Characterized by flaccid bullae on normal-appearing skin that easily rupture, leading to painful erosions that heal slowly. Lesions are widespread and can lead to significant fluid loss and secondary infections.
- Mucous Membrane Pemphigoid (MMP) / Bullous Pemphigoid (BP):
- Oral Lesions (MMP): Affects mucous membranes primarily, including the mouth. Tense bullae are formed that are more resistant to rupture compared to pemphigus. When they rupture, they leave erosions that heal with scarring. Desquamative gingivitis (red, painful, peeling gums) is a common and distinctive feature.
- Skin Rash (BP): Characterized by large, tense bullae on an erythematous (red) or urticarial (hive-like) base. These bullae are typically more resistant to rupture than those in pemphigus. BP predominantly affects elderly individuals, often on the flexor surfaces of limbs and the trunk. Oral lesions are less frequent in classic BP than in MMP.
- Hand-Foot-and-Mouth Disease (HFMD): (While more common in children, severe forms can affect adults, especially those with compromised immunity or exposure.)
- Oral Lesions: Multiple small vesicles rapidly ulcerate on the buccal mucosa, tongue, soft palate, and pharynx, causing significant pain and difficulty with oral intake.
- Skin Rash: Presents as a macular, papular, or vesicular rash, typically affecting the palms of the hands, soles of the feet, and sometimes the buttocks. The rash is usually non-itchy.
- Drug Reaction with Eosinophilia and Systemic Symptoms (DRESS) Syndrome:
- Oral Lesions: May include varying degrees of stomatitis, cheilitis, or xerostomia. The oral symptoms can sometimes be subtle compared to the systemic involvement.
- Skin Rash: A widespread maculopapular rash that often evolves into erythroderma (generalized redness and scaling) or exfoliative dermatitis. This syndrome is a severe drug hypersensitivity reaction associated with fever, lymphadenopathy, and internal organ involvement (e.g., liver, kidney).
The presence of both oral lesions and a skin rash necessitates a thorough medical evaluation, often involving biopsy of affected tissues and specialized laboratory tests to determine the precise diagnosis. Collaboration between dermatologists, oral medicine specialists, and other medical professionals is frequently required for the comprehensive management of these complex mucocutaneous conditions.
stomatitis in adults Treatment
Effective stomatitis in adults treatment focuses on alleviating symptoms, promoting healing, and addressing the underlying cause. Given the diverse etiologies of stomatitis, a tailored approach is essential. Treatment strategies can range from simple home remedies and improved oral hygiene to targeted pharmacological interventions and management of systemic diseases. The primary goals are to reduce pain, prevent secondary infections, and shorten the duration of the lesions.
I. General Supportive Care and Symptomatic Relief:
- Pain Management:
- Topical Anesthetics: Over-the-counter or prescription-strength topical agents such as lidocaine viscous, benzocaine gels, or dyclonine hydrochloride solutions can provide temporary numbing, especially before meals. Applying these directly to lesions helps reduce immediate discomfort.
- Systemic Analgesics: Non-steroidal anti-inflammatory drugs (NSAIDs) like ibuprofen or naproxen, or acetaminophen, can be used for general pain relief, particularly if the pain is widespread or severe.
- Protective Barriers: Over-the-counter pastes containing sucralfate or film-forming agents can cover and protect ulcers from irritation, aiding in comfort and healing.
- Oral Hygiene and Rinses:
- Gentle Brushing: Use a soft-bristled toothbrush to gently clean teeth and gums, avoiding direct trauma to lesions.
- Non-Irritating Mouthwashes: Rinsing with warm saline (salt water) several times a day can help keep the mouth clean and promote healing. A baking soda rinse (one teaspoon of baking soda in a glass of warm water) is also soothing and helps neutralize oral acidity.
- Avoidance of Irritants: Steer clear of alcohol-containing mouthwashes, which can dry out and irritate inflamed mucosa.
- Dietary Modifications:
- Soft, Bland Foods: Opt for a diet of soft, non-acidic, non-spicy, and non-rough foods (e.g., yogurt, mashed potatoes, smoothies, cooked cereals, scrambled eggs).
- Temperature Control: Avoid very hot or very cold foods and beverages that can exacerbate pain. Lukewarm or cool items are generally better tolerated.
- Hydration: Drink plenty of fluids to prevent dehydration, especially if swallowing is painful.
- Nutritional Support: Ensure adequate intake of vitamins and minerals, as deficiencies can contribute to stomatitis.
II. Targeted Pharmacological Treatments (Based on Etiology):
- For Aphthous Stomatitis (Canker Sores):
- Topical Corticosteroids: Fluocinonide, clobetasol, or triamcinolone acetonide in an adhesive paste or gel applied directly to the ulcers reduces inflammation and pain, and can speed healing. Dexamethasone elixir rinses may be prescribed for multiple lesions.
- Topical Immunomodulators: Amlexanox oral paste can be used to promote healing.
- Systemic Corticosteroids: For severe, recurrent, or major aphthae, a short course of oral corticosteroids (e.g., prednisone) may be considered under strict medical supervision.
- Nutritional Supplements: If deficiencies in B12, iron, or folate are identified, supplementation is crucial.
- For Herpetic Stomatitis (Oral Herpes):
- Antiviral Medications: Oral acyclovir, valacyclovir, or famciclovir are most effective if started during the prodromal phase (tingling/burning) or within the first 48-72 hours of lesion onset. They reduce the duration, severity, and frequency of outbreaks. Topical antivirals (e.g., penciclovir cream) may also be used for labial herpes.
- For Fungal Stomatitis (e.g., Oral Candidiasis, Angular Cheilitis):
- Topical Antifungals: Nystatin oral suspension (swish and swallow), clotrimazole troches (lozenges), or miconazole buccal tablets are commonly prescribed.
- Systemic Antifungals: For widespread, persistent, or immunocompromised patients, oral fluconazole or itraconazole may be necessary.
- For Angular Cheilitis: Topical antifungal creams (e.g., nystatin) often combined with a mild corticosteroid (e.g., hydrocortisone) or topical antibiotics (e.g., mupirocin) if bacterial involvement is suspected.
- For Bacterial Infections (e.g., Necrotizing Ulcerative Stomatitis):
- Antibiotics: Systemic antibiotics (e.g., metronidazole, amoxicillin) are indicated for significant bacterial infections, often along with aggressive debridement and improved oral hygiene.
- For Allergic Stomatitis:
- Elimination of Allergen: Identifying and removing the causative agent (e.g., specific toothpaste ingredient, dental material, food additive, medication) is paramount.
- Topical Corticosteroids: May be used to manage acute symptoms while the allergen is being identified or avoided.
- Antihistamines: For widespread allergic reactions or associated itching.
- For Autoimmune Conditions (e.g., Oral Lichen Planus, Pemphigus, Pemphigoid, Erythema Multiforme):
- Topical Corticosteroids: High-potency topical corticosteroids are the first-line treatment for localized lesions (e.g., clobetasol, fluocinonide).
- Systemic Immunosuppressants: For severe, widespread, or refractory cases, systemic corticosteroids (e.g., prednisone), or other immunosuppressive agents (e.g., azathioprine, mycophenolate mofetil, cyclosporine) may be required. Biologic agents are also used for some conditions. These treatments are typically managed by specialists (dermatologists, oral medicine specialists, rheumatologists).
- Other Agents: Dapsone, tetracyclines, and niacinamide may be used for specific autoimmune bullous diseases.
III. Addressing Underlying Causes:
- Nutritional Deficiencies: Correcting deficiencies in iron, vitamin B12, folate, or other essential nutrients through diet and supplementation.
- Systemic Diseases: Optimal management of any underlying systemic conditions such as inflammatory bowel disease, diabetes, or immune deficiencies.
- Denture Care: For denture stomatitis, proper denture hygiene (daily cleaning, removal at night), and ensuring a well-fitting prosthesis are crucial.
- Smoking Cessation: Quitting smoking can significantly reduce oral irritation and the risk of various oral lesions.
IV. Referral to Specialists:
- Persistent lesions, recurrent episodes, severe pain, or cases unresponsive to initial treatment warrant referral to an oral medicine specialist, dermatologist, or rheumatologist for further investigation, including biopsy, and specialized management. Complex systemic conditions often require a multidisciplinary approach.
The successful treatment of stomatitis in adults relies on an accurate diagnosis, which guides the choice of specific therapies. Symptomatic relief is a critical component for improving quality of life, but identifying and managing the root cause is paramount for long-term resolution and prevention of recurrence.