This comprehensive guide details the visual characteristics associated with erysipelas, offering specific descriptions that correlate to real-world erysipelas symptoms pictures. Understanding these distinct visual markers is crucial for recognizing this acute bacterial skin infection. Here, we delve into the manifold presentations, from early indicators to advanced stages, providing invaluable context for those examining erysipelas symptoms pictures.
erysipelas Symptoms Pictures
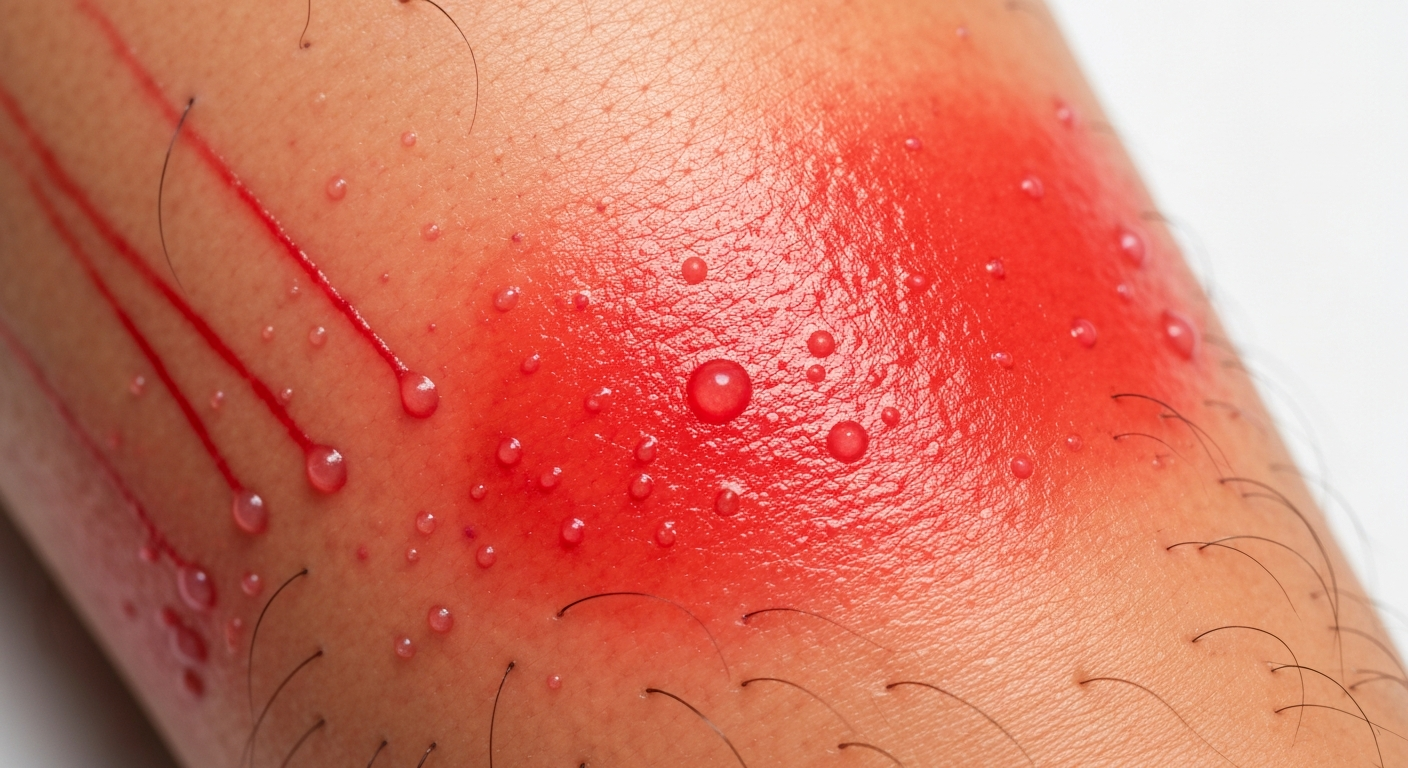
Examining erysipelas symptoms pictures reveals a distinctive pattern of skin inflammation. The most striking feature is a bright red, often fiery-red, skin patch that is intensely warm to the touch. This erythema typically has a sharp, raised, and well-demarcated border, creating a palpable edge that clearly separates the infected skin from the healthy surrounding tissue. The affected area often appears swollen, firm, and shiny, reflecting the underlying dermal edema and inflammatory response. Patients frequently report significant tenderness and pain upon palpation of the lesion, which can be visualized as a guarded or protective posture in photos. The speed of onset and progression is another hallmark; what starts as a small patch can rapidly expand over hours or a few days, illustrating the acute nature of the bacterial skin infection.
The distribution of these visible erysipelas symptoms is highly indicative. On the face, erysipelas often presents with a characteristic “butterfly” pattern, involving the bridge of the nose and cheeks, though it can affect any part of the face, including the ears. Facial erysipelas symptoms pictures frequently show significant periorbital edema. When located on the lower extremities, typically the shins or feet, the lesion can appear quite extensive, covering large areas of the leg or foot. Swelling can be so pronounced that the skin may appear stretched and taut. In some cases, lymphatic streaking, appearing as thin red lines extending from the primary lesion towards regional lymph nodes, can be observed, highlighting the lymphatic involvement in this bacterial skin disease. Fever and chills are systemic symptoms that often accompany the visual skin changes, leading to a general appearance of illness in patients.
Key Visual Markers of Erysipelas in Pictures:
- Intense Redness (Erythema): The skin presents with a vibrant, often fiery-red or scarlet hue, indicative of a robust inflammatory response. This redness is typically uniform across the affected area.
- Swelling (Edema): Significant swelling makes the skin appear visibly raised, thickened, and often taut. This palpable induration contributes to the feeling of firmness in the lesion.
- Induration: The affected skin feels firm and hard to the touch due to underlying inflammation and fluid accumulation, a characteristic easily conveyed in the texture seen in erysipelas symptoms pictures.
- Warmth: The inflamed area is noticeably warmer than the surrounding healthy skin, a direct result of increased blood flow and metabolic activity in response to the infection.
- Tenderness and Pain: Patients experience considerable tenderness and localized pain, which might manifest as recoil or wincing in some clinical images, indicating the severity of the discomfort.
- Sharp, Raised, Well-Demarcated Border: This is arguably the most diagnostic visual feature. The edge of the lesion is distinct, palpable, and clearly elevated, creating a sharp boundary between infected and uninfected skin. This contrasts sharply with the often diffuse borders of cellulitis.
- Shiny Appearance: The tautness and swelling of the skin can give it a smooth, glossy, or shiny look, particularly over areas with significant edema.
- ‘Peau d’Orange’ Texture: In cases with pronounced lymphatic obstruction or swelling, the skin surface may take on a dimpled appearance, resembling an orange peel, due to accentuation of hair follicles and sweat gland pores. This particular texture is a strong indicator of significant dermal involvement.
- Vesicles and Bullae: As the condition progresses, small fluid-filled blisters (vesicles) or larger blisters (bullae) may form on the surface of the erythematous patch, indicating a more severe inflammatory reaction and potentially deeper tissue damage. These can be clear, turbid, or hemorrhagic.
- Purpura and Petechiae: In some instances, particularly with more severe or hemorrhagic forms of erysipelas, small pinprick-sized red or purple spots (petechiae) or larger bruises (purpura) may be visible within the lesion, signifying capillary damage and extravasation of blood.
- Lymphangitic Streaking: Red linear streaks extending proximally from the main lesion are visual evidence of inflammation spreading along lymphatic channels, often towards regional lymph nodes.
Common Locations for Erysipelas Lesions in Pictures:
- Face: Frequently affects the cheeks, bridge of the nose, and periorbital area, sometimes presenting as a “butterfly rash.” Facial erysipelas can lead to significant swelling around the eyes and mouth.
- Ears: Involvement of the ear (perichondritis) can lead to a swollen, red, and painful earlobe or pinna, often with the characteristic sharp border.
- Lower Extremities: The most common site, particularly the shins, ankles, and feet. Lesions here can be extensive, covering large portions of the leg, and are often associated with underlying lymphedema or venous insufficiency.
- Upper Extremities: Less common than lower extremity involvement but can occur, especially in individuals with lymphedema post-mastectomy or due to other causes.
- Trunk: While rarer, erysipelas can manifest on the abdomen or back, often in patients with existing skin conditions or obesity where skin folds create an environment conducive to infection.
- Surgical Sites and Wounds: Any break in the skin barrier, including surgical incisions, traumatic wounds, or injection sites, can serve as an entry point for the bacteria, leading to localized erysipelas.
- Umbilicus (in neonates): Neonatal erysipelas, though rare, can present around the umbilical stump and spread rapidly, representing a severe form of the disease in infants.
Signs of erysipelas Pictures
When reviewing signs of erysipelas pictures, the acute inflammatory response is unmistakably evident. The skin lesions are not merely red; they are often described as having an ‘orange peel’ texture, or peau d’orange, due to lymphatic swelling that makes hair follicles more prominent. This specific textural change, combined with the intense erythema and marked edema, creates a highly characteristic visual signature for erysipelas. The clarity of the lesion’s border, consistently depicted as sharp and raised, remains a critical diagnostic sign in photos, differentiating it from more diffuse infections like cellulitis. In more severe cases, photos might reveal the formation of vesicles and bullae, which are fluid-filled blisters overlying the inflamed skin. These blisters can be clear, cloudy, or even hemorrhagic, signifying a more profound inflammatory process and potential for skin necrosis. The presence of petechiae or purpura (small red or purple spots, or larger bruises) within the erythematous area indicates microvascular damage and extravasation of blood, a sign of severe inflammation or a more virulent streptococcal infection.
Beyond the immediate skin lesion, signs of erysipelas pictures can also indirectly convey systemic involvement. Patients often present with symptoms of systemic illness, even before the skin lesion becomes pronounced. Prodromal symptoms such as sudden onset of high fever, chills, and malaise are frequently reported. While these aren’t directly visible in a skin photo, the overall appearance of the patient in clinical images, potentially looking distressed or unwell, can be suggestive. The development of regional lymphadenopathy, where lymph nodes in the drainage area of the infection become swollen and tender, is another key sign. Although not always visible externally unless severe, swelling in the groin for a leg infection, or in the neck for a facial infection, can be inferred or captured in more comprehensive patient photos. Lymphatic streaking, visible as red lines radiating from the primary lesion, offers direct visual evidence of the spread along lymphatic channels, a classic sign of streptococcal infections like erysipelas. These signs collectively contribute to a comprehensive understanding of the disease’s progression.
Characteristic Skin Lesion Signs in Erysipelas Pictures:
- Bright Red, Fiery-Red Appearance: The intensity of the redness is a hallmark, often appearing as a vivid, almost glowing crimson, clearly indicating a robust inflammatory process. This color is due to pronounced vasodilation and increased blood flow to the affected dermal layers.
- Elevated Border: The edge of the erysipelas lesion is not flat; it is consistently raised above the level of the surrounding healthy skin. This elevation is caused by significant dermal edema and cellular infiltration at the infection front.
- Palpable Edge: Corresponding to the elevated border, the edge is also firm and palpable, providing a distinct tactile sensation upon examination. This firm margin is a crucial differentiator in clinical assessment.
- Firm Consistency: The entire affected patch of skin feels tense and firm due to the extensive edema and inflammation. This induration is a key visual and tactile sign of acute dermal infection.
- Shiny, Taut Appearance: The extreme swelling stretches the skin, giving it a characteristic smooth, glossy, or shiny appearance. This tautness often suggests significant underlying fluid accumulation.
- Pitting Edema (Rarely): While non-pitting edema is more common, in very severe cases or in areas with pre-existing lymphatic compromise, pressure on the lesion may leave a temporary indentation, indicating profound fluid overload.
- Non-Blanching Erythema (in Hemorrhagic Forms): In instances where petechiae or purpura are present, these specific red or purple spots will not fade when pressed, indicating extravasated blood rather than just increased blood flow. The background erythema, however, typically blanches.
- Vesicle and Bulla Formation: The presence of small (vesicles) or large (bullae) fluid-filled blisters on the surface of the erythematous patch signals a more severe infection, indicating deeper dermal damage and potential epidermal detachment. These can be clear, turbid, or hemorrhagic.
- Lymphangitic Streaking: Visibly striking as red linear streaks ascending from the lesion towards regional lymph nodes, these streaks are a direct sign of bacterial spread via the lymphatic system, a characteristic feature of streptococcal infections.
- Regional Lymphadenopathy: Swollen, tender lymph nodes in the drainage area of the affected skin, although not always directly visible in skin pictures, are a crucial accompanying sign. Palpation would confirm their presence.
Associated Systemic Signs and Symptoms that Can be Inferred from Clinical Erysipelas Pictures:
- High Fever: Patients often experience a sudden onset of high fever (38-40°C), a clear systemic response to the infection, which can be inferred from the patient’s general appearance in a comprehensive clinical photograph.
- Chills and Rigors: Shaking chills and rigors frequently accompany the fever, indicating a significant systemic inflammatory reaction. A patient’s posture or expression in a photo might suggest discomfort.
- Malaise: A general feeling of discomfort, illness, or uneasiness is common, contributing to a patient’s overall sickly appearance in clinical images.
- Fatigue: Profound tiredness and lack of energy are typical, often making patients appear lethargic or weak.
- Headache: A common systemic symptom, often accompanying the fever and general inflammatory state.
- Nausea and Vomiting: Gastrointestinal disturbances, including nausea and sometimes vomiting, can occur, especially during the initial febrile phase.
- Joint Pain (Arthralgia) and Muscle Aches (Myalgia): Generalized body aches and pains are frequent, stemming from the systemic inflammatory response.
- Sudden Onset: The rapid development of both systemic symptoms and the localized skin lesion is characteristic, making it distinct from more gradual inflammatory processes.
- Increased White Blood Cell Count (Leukocytosis): While not visually apparent, a patient’s clinical state with fever and chills often correlates with an elevated WBC count, confirming an active infection.
Early erysipelas Photos
Early erysipelas photos typically capture the initial, often subtle, yet rapidly evolving stages of this bacterial skin infection. The first visual manifestation is usually a small, red, slightly raised patch of skin that rapidly expands over a few hours. Unlike later stages where the border is strikingly sharp, the initial border might be less defined, but it quickly develops its characteristic elevated and palpable edge. These early images often show a localized area of erythema that is already warm and tender to the touch, distinguishing it from simple irritation or a minor rash. The speed of progression is a crucial element; what might appear as a minor redness in the morning can develop into a significantly larger, fiery lesion by evening, emphasizing the importance of prompt recognition and intervention. In photos depicting early facial erysipelas, the initial redness might appear near the nose or cheek, with subtle swelling that gradually becomes more pronounced.
Before the visible skin lesion emerges, individuals often experience prodromal symptoms that can set the stage for the dramatic skin changes. While these aren’t visible in skin photos themselves, understanding them helps in interpreting the context of early erysipelas photos. Symptoms like a sudden onset of high fever, chills, malaise, and even localized itching or burning at the site where the lesion will soon appear, frequently precede the skin eruption by several hours. Therefore, an individual appearing unwell in an early clinical photo, even with only a nascent skin lesion, is highly consistent with the presentation of early erysipelas. The initial lesion’s appearance is often mistaken for an insect bite or a minor scratch, but its rapid progression, increasing warmth, and intense tenderness quickly differentiate it. The distinctive “orange peel” texture (peau d’orange) may not be present in the very earliest stages but can develop quickly as the edema worsens, providing another key visual marker for distinguishing this acute bacterial infection from other dermatological conditions.
Prodromal Symptoms (Preceding Visible Skin Lesion) Relevant to Early Erysipelas Photos:
- Sudden Onset of Systemic Illness: This is a key precursor. Patients often feel acutely unwell hours before the skin lesion becomes noticeable, characterized by a rapid escalation of systemic symptoms.
- High Fever: A sudden spike in body temperature, often reaching 38-40°C (100.4-104°F), is a common initial manifestation, indicative of the body’s immediate inflammatory response to the bacterial invasion.
- Chills and Rigors: Shivering and intense shaking (rigors) frequently accompany the sudden onset of fever, underscoring the severity of the systemic reaction.
- Malaise: A general feeling of unwellness, fatigue, and discomfort that often precedes the appearance of the skin rash.
- Headache: A common associated symptom, contributing to the overall systemic distress experienced by the patient.
- Nausea: Some individuals may experience nausea, and occasionally vomiting, as part of the initial systemic response to the infection.
- Localized Itching or Burning Sensation: Patients may report a peculiar itching, tingling, or burning sensation at the exact site where the erysipelas lesion will subsequently erupt, serving as an early, localized warning sign.
- Myalgia (Muscle Aches): Generalized muscle aches can be part of the initial febrile illness.
Initial Visual Manifestations in Early Erysipelas Photos:
- Small Red Patch: The lesion often begins as a relatively small, localized area of erythema, sometimes only a few centimeters in diameter, which rapidly begins to expand.
- Slightly Raised: Even in its nascent stage, the lesion will typically exhibit a subtle elevation compared to the surrounding healthy skin, indicating early dermal edema.
- Tender to Touch: Palpation of this early red patch usually elicits tenderness or pain, distinguishing it from non-infectious rashes. This localized pain is a critical early symptom.
- Rapid Spread: A defining characteristic of erysipelas is its expeditious centrifugal expansion. What appears as a minor lesion in the morning can significantly enlarge and intensify over the course of a day.
- Warm to Touch: The affected area feels noticeably warmer than adjacent healthy skin, a direct result of localized inflammation and increased blood flow.
- Ill-Defined Initially, Then Sharpening: While the hallmark sharp border develops quickly, the very earliest presentation might have a slightly less distinct edge that rapidly becomes well-demarcated and raised as the infection progresses.
- Common Initial Sites: Early lesions are frequently observed on the face (near the nose or eye) or on the lower extremities (shin or foot), correlating with typical entry points for the bacteria.
- Absence of Blistering/Purpura: In the very early stages, vesicles, bullae, or purpura are typically absent, but these more severe manifestations can develop rapidly as the infection intensifies.
- Shiny Appearance: As edema develops, the skin can begin to look stretched and shiny, even in early stages, hinting at the fluid accumulation beneath the surface.
Skin rash erysipelas Images
Skin rash erysipelas images consistently highlight the aggressive nature of this acute bacterial skin infection. The “rash” of erysipelas is distinctively characterized by its intense red color, sharp, raised border, and significant edema. This is not a diffuse, patchy rash, but rather a well-demarcated, rapidly spreading lesion that signals a clear inflammatory front. The color itself is often described as bright red or fiery, a result of marked vasodilation and inflammation in the superficial dermal and lymphatic layers. In many images, the skin appears stretched and shiny due to underlying swelling, and the texture may be uneven, sometimes exhibiting the classic peau d’orange appearance if lymphatic involvement is pronounced. The lesion is invariably warm and tender to the touch, features that are often visually implied by the swollen, taut appearance of the skin in photographs.
Variations in the presentation of the erysipelas rash can also be observed in specific skin rash erysipelas images. For instance, bullous erysipelas photos show the formation of clear or hemorrhagic blisters (bullae) on the surface of the erythematous skin, indicating a more severe inflammatory response and epidermal detachment. In cases of hemorrhagic erysipelas, petechiae or purpura (small blood spots or bruises) are visible within the red rash, signifying capillary damage and extravasation of red blood cells. These variations underscore the severity and depth of the infection. Furthermore, lymphangitic streaking, appearing as thin, red lines extending proximally from the main rash, can be seen in some images, indicating the spread of infection through the lymphatic channels. The rapid expansion of this dermatological condition, often described as having a ‘geographic’ pattern due to its distinct borders, makes it a visually compelling and clinically urgent presentation. Understanding these visual cues is paramount for accurate identification of this acute streptococcal skin infection.
Variations in Erysipelas Rash Presentation in Images:
- Erysipelas Bullosum (Bullous Erysipelas): Pictures of this variant show the formation of vesicles (small blisters) or bullae (large blisters) on the surface of the intensely erythematous and edematous skin. These blisters can contain clear, serous, or sometimes hemorrhagic fluid, indicating a more severe inflammatory reaction and epidermal separation.
- Erysipelas Haemorrhagicum (Hemorrhagic Erysipelas): This form is characterized by the presence of petechiae (pinpoint red spots) or purpura (larger red/purple blotches) within the erythematous rash. These hemorrhagic signs result from microvascular damage and extravasation of blood into the dermis, suggesting a more aggressive infection or coagulopathy.
- Erysipelas Gangrenosum (Gangrenous Erysipelas): A rare and severe variant where areas of tissue necrosis (gangrene) develop within the erysipelas rash. Photos would show dark, necrotic patches or eschars developing in the center of the inflamed skin, signaling extensive tissue destruction and requiring urgent intervention.
- Erysipelas Migrans (Migratory Erysipelas): This refers to an erysipelas rash that appears to “migrate” or spread across the skin in an unusual pattern, sometimes leaving behind a resolution at the initial site while advancing at the periphery. This is less common but visually distinct.
- Erysipelas Recidivans (Recurrent Erysipelas): While not a distinct visual type, this describes repeated episodes of erysipelas in the same anatomical location. Pictures of recurrent cases might show subtle residual changes in skin texture or pigmentation, or areas of chronic lymphedema, which predispose to recurrence.
- Facial Erysipelas: Often presents with a characteristic “butterfly” distribution involving the bridge of the nose and cheeks, leading to significant periorbital edema and facial distortion in images.
- Lower Extremity Erysipelas: Commonly affects the shins and feet, often presenting as extensive, fiery-red patches that can cover large areas of the limb, frequently associated with underlying lymphedema or venous insufficiency.
Distinguishing Features of Erysipelas Rash in Images:
- Well-Demarcated Border: The defining feature, a sharply defined and often elevated border that clearly distinguishes the infected skin from the healthy surrounding tissue. This distinct margin is a crucial visual cue in erysipelas pictures.
- Intensely Red (Fiery Erythema): The color is typically a vivid, bright red or scarlet, indicating a robust inflammatory response in the superficial dermis.
- Edematous and Swollen: The affected area is visibly raised, swollen, and thickened due to significant fluid accumulation (edema) in the dermal layers.
- Warm to Touch: The inflammatory process causes a noticeable increase in local skin temperature, making the rash feel significantly warmer than adjacent skin.
- Palpable Raised Edge: The border is not just visually distinct but also palpable, feeling firm and elevated upon touch, a key physical sign corroborated by visual cues.
- Rapid Progression: A critical characteristic is the speed at which the rash spreads and intensifies. Photos taken over a short period can dramatically illustrate its rapid expansion.
- Shiny Surface: Due to the underlying edema stretching the skin, the surface of the rash often appears smooth, glossy, or shiny.
- Lymphangitic Streaking: Red linear streaks extending proximally from the main rash are visual indicators of bacterial spread along the lymphatic vessels, often towards regional lymph nodes.
- Absence of Central Clearing: Unlike some fungal rashes, erysipelas typically maintains a uniform redness across the lesion, without central clearing.
- Tenderness and Pain: The rash is typically very tender and painful to touch, a symptom that can be inferred from a patient’s expression or posture in clinical images.
- Associated Systemic Symptoms: The presence of fever, chills, and malaise, while not directly visible on the skin, contributes to the overall clinical picture of a severe infection.
erysipelas Treatment
While this article focuses on erysipelas symptoms pictures, understanding the visual changes associated with erysipelas treatment is crucial for monitoring progress and recovery. The primary aim of erysipelas treatment is to eradicate the underlying bacterial infection and alleviate symptoms. This is achieved predominantly through antibiotic therapy. Once appropriate antibiotics are initiated, early signs of improvement can often be observed within 24-48 hours. Visually, the intense fiery redness typically begins to fade, transitioning to a duller red or pink. The distinct sharp, raised border may start to soften and become less pronounced as the acute inflammation subsides. Swelling (edema) in the affected area will also noticeably decrease, reducing the tautness and shininess of the skin. The warmth and tenderness upon palpation will diminish, indicating a reduction in the inflammatory process. Any associated vesicles, bullae, or purpura will begin to resolve; blisters may dry and crust over, and petechiae will gradually fade.
Supportive care measures also play a significant role in managing erysipelas symptoms and can influence the visual resolution seen in erysipelas pictures during treatment. Elevating the affected limb, especially for lower extremity erysipelas, helps to reduce swelling and improve lymphatic drainage, visually contributing to a faster decrease in edema. Cool compresses can offer symptomatic relief from burning and pain, potentially reducing the visual signs of distress. For patients with bullae, sterile dressings are applied to prevent secondary infection and promote healing, and images might show these dressings covering the affected skin. As the infection resolves, the skin will gradually return to its normal color and texture, though some post-inflammatory hyperpigmentation (darkening of the skin) may persist for weeks or months, especially in recurrent cases or those with more severe initial inflammation. Prophylactic measures to prevent recurrence, such as treating underlying lymphedema or tinea pedis, are also important, as repeated episodes can lead to chronic skin changes and thickening, visible in long-term follow-up erysipelas pictures.
Primary Treatment Modalities for Erysipelas and Their Visual Impact:
- Systemic Antibiotics (Penicillin-based): Penicillin V or penicillin G are the first-line agents due to their efficacy against Streptococcus pyogenes. Visually, effective antibiotic therapy leads to a rapid decrease in erythema (from fiery red to duller pink), softening of the sharp border, and reduction in swelling within 24-48 hours.
- Systemic Antibiotics (Cephalosporins): For penicillin-allergic patients, cephalexin or ceftriaxone can be used. Their visual impact mirrors penicillin, with noticeable de-escalation of inflammatory signs.
- Systemic Antibiotics (Macrolides): Clindamycin or erythromycin are alternatives for severe penicillin allergies. Their initiation targets the bacterial cause, leading to the visual resolution of the intense skin inflammation.
- Intravenous Antibiotics for Severe Cases: For extensive or rapidly progressing erysipelas, or for patients with systemic toxicity, IV antibiotics (e.g., penicillin G, ceftriaxone) are administered. This faster delivery can lead to a more rapid initial visual improvement of the lesion and systemic symptoms.
- Oral Antibiotics for Mild-Moderate Cases: Once stabilized or for less severe presentations, oral antibiotics are sufficient, continuing the process of visual resolution of the skin lesion and prevention of complications.
- Duration of Antibiotic Treatment: Typically 7-14 days. Continued treatment ensures complete eradication of the infection, preventing relapse and allowing for full visual resolution of the lesion without scarring, unless deep tissue damage occurred.
- Monitoring for Improvement: Clinical assessment focuses on the reduction of erythema, edema, pain, warmth, and resolution of systemic symptoms. This visual and symptomatic improvement confirms effective erysipelas treatment.
Supportive Care and Symptom Management Affecting Visual Erysipelas Resolution:
- Analgesics for Pain: Over-the-counter pain relievers (e.g., ibuprofen, acetaminophen) help manage the significant localized pain associated with erysipelas, contributing to patient comfort and potentially reducing visible signs of distress.
- Antipyretics for Fever: Medications to reduce fever improve systemic well-being, which, while not directly altering the skin lesion, supports the overall recovery process.
- Elevation of Affected Limb: For erysipelas on the lower or upper extremities, elevating the limb above heart level significantly reduces edema and swelling. Visually, this leads to a faster decrease in the bulk and tautness of the lesion.
- Cool Compresses: Applying cool, moist compresses to the affected area can provide symptomatic relief from the burning sensation and reduce local inflammation, potentially aiding in the visual calming of the fiery redness.
- Sterile Dressings for Bullae/Ulcerations: If vesicles or bullae form, they should be managed with sterile dressings to prevent rupture, secondary infection, and promote healing, often seen as a covered lesion in treatment photos.
- Adequate Hydration: Maintaining good hydration supports overall physiological function and recovery from systemic illness.
- Rest: Physical rest helps the body conserve energy for fighting the infection, contributing to the overall healing process and symptom resolution.
- Skin Care: Gentle cleansing and moisturizing of the recovering skin can help prevent dryness and cracking as the inflammation subsides.
Prevention of Erysipelas Recurrence and Its Long-Term Visual Implications:
- Addressing Predisposing Factors: Identifying and managing underlying conditions like venous insufficiency, chronic lymphedema, tinea pedis (athlete’s foot), skin breaks, and wounds is critical for preventing future episodes. For instance, treating fungal infections of the feet (tinea pedis) eliminates a common portal of entry for bacteria, preventing visual recurrences.
- Meticulous Skin Care: Regular moisturizing, prompt treatment of cuts or abrasions, and maintaining good hygiene, especially in areas prone to infection, can visually reduce the risk of new erysipelas episodes.
- Compression Therapy for Lymphedema: For patients with lymphedema, wearing compression garments or undergoing manual lymphatic drainage can prevent fluid accumulation that makes the limb susceptible to erysipelas. This visibly reduces chronic swelling and skin thickening.
- Prophylactic Antibiotics: In individuals with frequent recurrent erysipelas (e.g., more than 2-3 episodes per year), long-term low-dose antibiotics (e.g., penicillin V, erythromycin) may be prescribed. This prevents the characteristic red, swollen lesions from reappearing.
- Managing Chronic Wounds: Proper wound care and infection control for chronic skin lesions (e.g., leg ulcers) are essential to prevent erysipelas from developing at these vulnerable sites.
- Post-Inflammatory Hyperpigmentation: After severe or recurrent episodes, the skin may show persistent darkening or discoloration (hyperpigmentation) in the affected area, a visual marker of previous inflammation.
- Chronic Skin Thickening: Repeated bouts of erysipelas, especially in the lower extremities, can lead to chronic lymphatic damage and fibrosis, resulting in permanent skin thickening (elephantiasis nostras verrucosa), a significant visual sequela.
- Education on Early Symptom Recognition: Patients are educated to recognize early signs of recurrence (e.g., new redness, warmth, tenderness) to seek prompt treatment, which can limit the extent of the visible lesion.