Understanding the visual manifestations of Pityriasis versicolor is critical for accurate identification and effective management. This article provides a comprehensive guide to Pityriasis versicolor symptoms pictures, focusing on the various ways this common fungal infection presents on the skin. By examining the distinct characteristics of the lesions, individuals and healthcare providers can better recognize Pityriasis versicolor symptoms pictures and pursue appropriate care.
Pityriasis versicolor Symptoms Pictures
The visual presentation of Pityriasis versicolor symptoms pictures is highly variable, reflecting the “versicolor” aspect of its name, meaning “of various colors.” This common superficial fungal infection, caused by an overgrowth of Malassezia yeast on the skin, leads to distinct skin discoloration and texture changes. Recognizing these Pityriasis versicolor symptoms is the first step towards proper diagnosis and treatment of this prevalent fungal skin infection.
Key visual characteristics often seen in Pityriasis versicolor symptoms pictures include:
- Discoloration: The hallmark symptom. Patches can be lighter than the surrounding skin (hypopigmented), darker (hyperpigmented), or reddish-brown (erythematous).
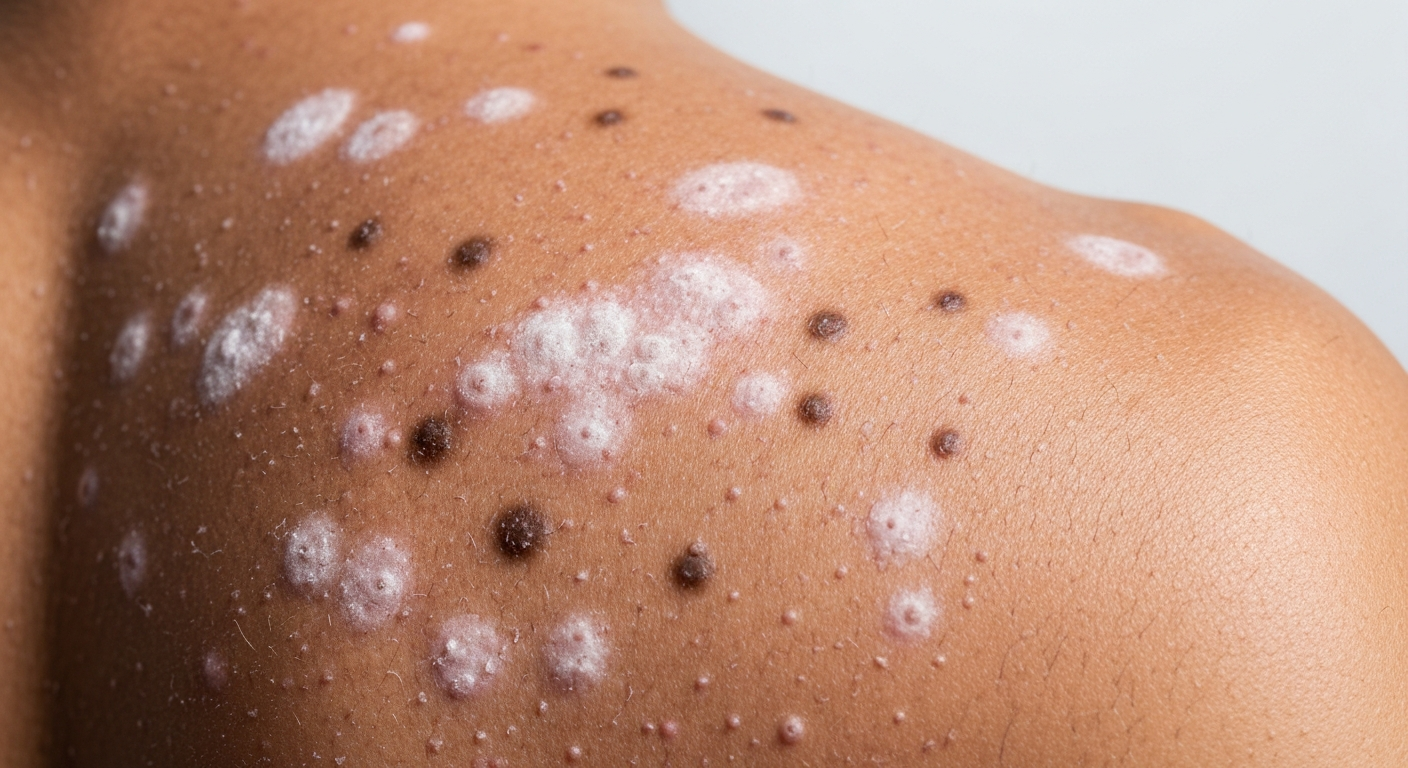
- Hypopigmentation: The most common presentation, especially in individuals with darker skin tones or after sun exposure. The yeast produces azelaic acid, which inhibits melanin production, leading to areas that fail to tan. These white spots are highly characteristic.
- Hyperpigmentation: Often seen in individuals with lighter skin tones. The patches may appear light brown, dark brown, or even pinkish-tan. This can be due to an inflammatory response or the presence of yeast pigment.
- Erythema: Reddish or pinkish patches, particularly noticeable in early stages or in areas with active inflammation. These can sometimes be confused with other forms of skin rash.
- Fine Scaling: A subtle but consistent feature. The affected skin often has fine, powdery scales that are more evident when the skin is stretched or lightly scraped (the “chip sign”). This scaling is a result of the yeast disrupting the normal desquamation process of the epidermis.
- Distribution: Pityriasis versicolor typically affects areas of the body rich in sebaceous glands, where the Malassezia yeast thrives. Common locations include:
- Upper back
- Chest
- Neck and shoulders
- Upper arms
- Abdomen (less common but can occur)
- Face (especially in children or immunocompromised individuals)
- Groin and flexures (rare)
- Shape and Size: Lesions usually start as small, round or oval macules (flat spots) and gradually enlarge, coalescing into larger, irregular patches. The borders are often well-defined, though they can sometimes be more diffuse.
- Sensation: While often asymptomatic, some individuals report mild itching (pruritus), especially when sweating or in warm environments. The itching associated with Pityriasis versicolor rash is generally less intense than that of other fungal infections like tinea corporis.
Environmental factors significantly influence the appearance of Pityriasis versicolor symptoms pictures. Warm, humid climates, excessive sweating, oily skin, and immunosuppression are known to exacerbate the condition and promote yeast overgrowth. Sun exposure, in particular, highlights the hypopigmented areas as the surrounding skin tans, making the affected patches more noticeable. This contrast is a key diagnostic feature often observed in tinea versicolor symptoms pictures.
Understanding these diverse visual cues is essential for differentiating Pityriasis versicolor from other skin conditions such as vitiligo, post-inflammatory hypopigmentation, pityriasis alba, or other forms of fungal rash. Accurate identification through careful observation of Pityriasis versicolor symptoms pictures guides appropriate management strategies.
The progression of the condition, from subtle initial spots to widespread confluent patches, is also a critical aspect seen in Pityriasis versicolor photos. The lesions tend to be chronic and recurrent, especially without consistent preventive measures, and their appearance can fluctuate with seasonal changes and individual lifestyle factors. For many, the aesthetic concern over the skin discoloration is the primary reason for seeking treatment for this common yeast infection skin condition.
The texture of the lesions is also a notable feature. While the primary lesions are macules (flat), the fine scaling adds a slightly rough or powdery feel to the affected areas. This characteristic scaling, though sometimes subtle, is consistently present and is a key indicator for diagnosis when examining Pityriasis versicolor images. Stretching the skin can often make these scales more apparent, revealing a fine, branny desquamation that helps distinguish Pityriasis versicolor from conditions that do not typically present with such scaling. This is particularly useful when the discoloration is less pronounced.
Signs of Pityriasis versicolor Pictures
When examining signs of Pityriasis versicolor pictures, specific objective findings are consistently observed, providing crucial diagnostic clues. These signs, visible to the eye, help differentiate this common skin discoloration from other dermatological conditions. The primary observable signs revolve around color changes, surface texture, and lesion morphology, all indicative of Malassezia furfur overgrowth.
Detailed analysis of signs of Pityriasis versicolor pictures reveals:
- Color Variances (Versicolor Effect):
- Hypopigmented Macules and Patches: These appear as areas significantly lighter than the patient’s normal skin tone. In fair-skinned individuals, they might appear as faint white or off-white spots. In individuals with darker complexions or those who have been sun-tanned, these areas stand out strikingly as bright white patches because the yeast interferes with melanocyte function. These white spots on skin are highly characteristic.
- Hyperpigmented Macules and Patches: These manifest as light brown, dark brown, tan, or sometimes slightly reddish-brown spots. This darker pigmentation is more common in individuals with lighter skin types and can be due to inflammatory changes or the presence of fungal pigments. The margins of these dark spots on skin are often well-demarcated.
- Erythematous Lesions: Pink or reddish macules, particularly in active or early stages of the infection. These can sometimes be mildly inflammatory, though significant erythema is less common than with other fungal infections. The redness typically precedes the more chronic hypo or hyperpigmented changes.
- Fine, Branny Scaling: This is a very consistent objective sign. The affected areas, regardless of their color, exhibit a superficial, flaky texture.
- “Chip Sign” or “Scratch Sign”: Lightly scraping the lesion with a fingernail or tongue depressor often accentuates the fine scaling, causing tiny flakes to become visible. This is a highly specific diagnostic maneuver when evaluating potential tinea versicolor lesions.
- The scales are typically small, dry, and powdery, resembling fine bran, hence the term “branny.” They are not typically large, greasy, or adherent like scales seen in conditions such as psoriasis.
- Morphology and Configuration:
- Discrete Macules: Lesions often begin as small, round or oval, flat macules, typically 1-3 mm in diameter.
- Coalescing Patches: As the infection progresses, these discrete macules tend to merge, forming larger, irregularly shaped patches with polycyclic or geographic borders. These larger patches can cover significant areas of the upper trunk.
- Follicular Pattern: Sometimes, the lesions can present as small, perifollicular papules or macules, particularly in areas like the chest or back, suggesting involvement around hair follicles.
- Sharp Demarcation: The borders between affected and unaffected skin are usually distinct, making the spread of the fungal rash clearly visible in Pityriasis versicolor skin pictures.
- Distribution Pattern: The lesions preferentially localize to sebaceous areas, which are oil-producing zones of the skin.
- Upper chest and back are the most common sites.
- Neck, shoulders, and upper arms are also frequently involved.
- Less commonly, the abdomen, scalp margin, and face (especially forehead and perinasal areas) can be affected.
- Lack of Significant Inflammation: Unlike many other fungal infections or eczematous rashes, Pityriasis versicolor typically does not present with significant redness, swelling, blistering, or oozing. Any erythema present is usually mild. This relative absence of acute inflammatory signs helps distinguish it from more inflammatory conditions when viewing skin rash pictures.
Observing these specific signs in Pityriasis versicolor pictures allows for a high degree of diagnostic accuracy. The interplay of color variations, the subtle but characteristic scaling, and the typical anatomical distribution collectively form a unique clinical picture. The chronic and often recurrent nature of these signs further emphasizes the need for a comprehensive approach to both treatment and prevention of this yeast infection skin rash. Patients often present due to the cosmetic disfigurement caused by the prominent skin discoloration, especially after sun exposure, which highlights the hypopigmented areas.
Under Wood’s lamp examination, a less common but definitive sign, Malassezia furfur often exhibits a characteristic yellowish-green fluorescence. This glow is due to a metabolite produced by the yeast and can confirm the presence of the active infection, although it may not always be positive, particularly after a patient has used a topical antifungal. However, in the absence of recent treatment, this fluorescent sign is a strong indicator when evaluating Pityriasis versicolor under UV light.
The morphology of individual lesions and their confluence are also key signs. The small, often circular or oval initial macules can merge seamlessly, creating large, sprawling areas of affected skin. These larger patches often retain the distinct colors and scaling, giving a mosaic appearance. The borders can sometimes be somewhat irregular, especially when multiple smaller lesions have coalesced. This morphological progression is a critical diagnostic element when reviewing a series of Pityriasis versicolor rash pictures.
Early Pityriasis versicolor Photos
Identifying early Pityriasis versicolor photos can be challenging due to the often subtle nature of the initial symptoms. However, recognizing these nascent signs is crucial for prompt diagnosis and intervention, potentially preventing the widespread proliferation of the Malassezia yeast and extensive skin discoloration. Early lesions typically appear in areas predisposed to yeast overgrowth, such as the upper trunk, and gradually evolve over time.
Common characteristics observed in early Pityriasis versicolor photos include:
- Small, Discrete Macules: The infection usually begins as isolated, small, round or oval macules, often only a few millimeters in diameter. These are flat and typically do not present with significant elevation or inflammation.
- Subtle Color Changes:
- Faint Hypopigmentation: In early stages, especially in individuals with lighter skin, the hypopigmented spots may be very subtle, barely lighter than the surrounding skin. They might only become noticeable after mild sun exposure when the surrounding skin begins to tan.
- Mild Hyperpigmentation: For some, early lesions might appear as slightly darker tan or light brown spots. These can sometimes be mistaken for freckles or minor sun damage.
- Pinkish or Reddish Tinge: Very early lesions, particularly in fair-skinned individuals, might have a faint pink or reddish hue, indicating minimal inflammatory activity. This erythema is usually mild and diffuse, not sharply demarcated.
- Minimal Scaling: The fine, branny scaling characteristic of Pityriasis versicolor may be very minimal or almost imperceptible in early lesions. It often becomes more apparent as the lesions mature or upon careful stretching or scraping of the skin.
- Asymptomatic Nature: Many individuals with early Pityriasis versicolor report no symptoms. There is typically no itching or discomfort, which often leads to delayed presentation until the lesions become more widespread or cosmetically noticeable.
- Common Initial Locations:
- Upper Chest: This is a very frequent starting point, often near the sternum or clavicles.
- Upper Back: Especially between the shoulder blades, where sweating is common.
- Neck: Often seen extending from the chest or back onto the lower neck.
- Shoulders: Isolated spots on the shoulders are also common early findings.
- Slow Progression: Early lesions typically enlarge slowly over weeks or months, gradually coalescing to form larger patches. This slow, insidious onset contributes to the delay in seeking medical advice.
Distinguishing early Pityriasis versicolor from other subtle skin changes is vital. For instance, very faint hypopigmented patches might resemble early vitiligo, but the presence of fine scaling (even if minimal) and the characteristic distribution help differentiate it. Similarly, slightly hyperpigmented spots could be confused with solar lentigines, but their texture and potential for scaling are key differentiators. The absence of significant inflammation or pain is another hallmark when viewing early Pityriasis versicolor photos.
The role of environmental factors in the onset of early Pityriasis versicolor cannot be overstated. Individuals residing in or visiting hot, humid climates, or those who engage in activities leading to excessive sweating, are more prone to developing the condition. The increased moisture and warmth provide an ideal environment for the Malassezia yeast to transition from its commensal (normal inhabitant) to pathogenic (disease-causing) form. This environmental trigger often initiates the subtle changes seen in early tinea versicolor photos.
Regular skin self-examinations, especially after sun exposure when hypopigmented areas become more obvious, can aid in early detection. If a person notices new, subtly discolored spots, particularly on the chest or back, that do not tan and show very fine scaling, these could be early signs of Pityriasis versicolor. Early treatment with a topical antifungal agent can often prevent the lesions from spreading and becoming more prominent, reducing the need for more intensive therapies and improving cosmetic outcomes.
The morphology of these early lesions is often quite uniform; small, circular macules are the predominant form. They may present as a scattering of a few isolated spots before they begin to merge. This initial presentation is critical for understanding the natural history of the fungal skin infection. Any changes in color, even subtle ones, accompanied by a slightly altered texture, especially in areas prone to sweating, should raise suspicion for early Pityriasis versicolor and prompt a professional evaluation to confirm the diagnosis and initiate timely Pityriasis versicolor treatment.
Skin rash Pityriasis versicolor Images
The term “skin rash Pityriasis versicolor images” broadly encompasses the various ways this fungal infection manifests across larger areas of the skin, emphasizing its widespread nature and characteristic appearance. Unlike some inflammatory rashes that are acutely red and itchy, Pityriasis versicolor often presents as a chronic, spreading discoloration with subtle textural changes. The “versicolor” aspect is particularly prominent in these images, showing the dynamic color shifts that define the condition.
When analyzing skin rash Pityriasis versicolor images, look for:
- Widespread Discoloration: The rash typically involves extensive patches rather than isolated spots. These patches can be uniformly hypopigmented, hyperpigmented, or a mixture of both, leading to a mottled or variegated appearance on the skin surface.
- Large Hypopigmented Patches: Often the most striking feature, particularly in individuals with tanned skin. These white patches on skin can cover significant areas of the upper back, chest, and shoulders, creating a stark contrast against tanned skin.
- Confluent Hyperpigmented Patches: Brownish or tan patches that merge into large, irregular areas, particularly in individuals with lighter skin tones or those with less sun exposure. These dark skin patches might be more noticeable against pale skin.
- Erythematous Overlays: In some cases, particularly in active or more inflammatory presentations, large areas of the rash may have a pinkish or reddish tint, although this is usually less pronounced than in other common inflammatory rashes.
- Characteristic Scaling: The entire affected area of the rash will exhibit fine, branny scaling. This scaling can be diffuse across the large patches, making the skin appear dry or somewhat dusty. The “chip sign” (accentuated scaling upon scraping) remains a key diagnostic feature even in widespread lesions.
- Irregular and Serpiginous Borders: As individual lesions coalesce, the overall borders of the rash often become irregular, polycyclic, or even serpiginous (snake-like). These sprawling patterns are highly characteristic in Pityriasis versicolor pictures.
- Typical Distribution: The rash predominantly affects seborrheic areas:
- Chest: Often spreads widely across the sternum, breasts, and lateral chest walls.
- Back: Can cover the entire upper and mid-back, extending onto the shoulders and sometimes down the arms.
- Neck: Frequently involves the sides and back of the neck, creating a visible line at the collar.
- Abdomen: While less common, the central abdomen can be affected, often in a scattered pattern.
- Asymptomatic to Mildly Pruritic: While often visually prominent, the Pityriasis versicolor rash is frequently asymptomatic. When itching occurs, it is usually mild and often exacerbated by sweating, heat, or exercise. It does not typically cause the intense, debilitating itch associated with conditions like eczema or scabies.
- Lack of Other Inflammatory Signs: Generally, the rash does not present with significant blistering, crusting, weeping, or deep inflammation. Any redness is usually superficial. This differentiates it from many bacterial skin infections or acute eczematous flare-ups.
The term “versicolor” truly comes to life when observing widespread skin rash Pityriasis versicolor images, where different hues can be present simultaneously across the body. For instance, an individual might have hypopigmented patches on the back contrasting with mildly erythematous or hyperpigmented areas on the chest. This mosaic of colors is a strong indicator of the presence of Malassezia overgrowth. Sun exposure plays a critical role in how the rash appears. Areas of hypopigmentation become strikingly visible against tanned skin, often leading individuals to seek treatment for the noticeable cosmetic alteration.
Chronic and recurrent presentations are common, meaning the rash can persist for long periods if untreated, and frequently recurs even after successful treatment, especially if predisposing factors (like warm, humid environments or oily skin) persist. The cumulative effect of these recurrences can lead to more widespread and visually complex rashes. Understanding these patterns is essential for effective Pityriasis versicolor treatment and long-term management.
When differentiating Pityriasis versicolor rash from other skin conditions like fungal infections (e.g., tinea corporis), psoriasis, or eczema, the absence of prominent inflammation, the characteristic fine scaling, and the diverse color changes are crucial. Tinea corporis typically presents with annular (ring-shaped) lesions with raised, erythematous, and often intensely itchy borders. Psoriasis typically features thicker, silvery scales on sharply demarcated erythematous plaques. Eczema is often intensely pruritic, poorly demarcated, and can involve significant weeping or crusting. The subtle, branny scaling and the distinct color variability of Pityriasis versicolor make it unique when viewed in skin rash Pityriasis versicolor images.
The psychological impact of a visible, widespread skin discoloration should not be underestimated. Patients often feel self-conscious about their appearance, especially in social settings or when wearing certain clothing. This cosmetic concern is a primary driver for seeking medical help and underscores the importance of accurate diagnosis and effective Pityriasis versicolor management. Regular use of specific anti-fungal soaps or cleansers can sometimes mitigate the severity and recurrence of such widespread rashes.
Pityriasis versicolor Treatment
Effective Pityriasis versicolor treatment focuses on eradicating the overgrowth of Malassezia yeast on the skin and preventing recurrence. While the symptoms, particularly skin discoloration, can be cosmetically distressing, Pityriasis versicolor is generally not a harmful condition. Treatment aims to restore normal skin pigmentation and reduce scaling and itching. It’s crucial to understand that even after successful antifungal therapy, the changes in skin pigmentation (especially hypopigmentation) may take weeks or even months to resolve as the skin gradually repigments with sun exposure or natural cell turnover.
Treatment modalities for Pityriasis versicolor are broadly categorized into topical and oral therapies, chosen based on the extent and severity of the infection.
Topical Pityriasis versicolor Treatment
Topical treatments are typically recommended for localized or less severe cases of fungal skin infection. These agents directly target the yeast on the skin surface.
- Antifungal Shampoos/Cleansers:
- Selenium Sulfide 2.5% (e.g., Selsun Blue Rx): Applied to affected areas for 10-15 minutes daily for 7-14 days, then weekly for maintenance. It’s often lathered, left on, and rinsed off.
- Ketoconazole 2% Shampoo: Similar application as selenium sulfide, typically once daily for 5-7 days, followed by monthly maintenance. This is a very effective antifungal shampoo for skin.
- Zinc Pyrithione (e.g., Head & Shoulders): A milder option available over-the-counter, used daily as a cleanser for affected areas.
- Topical Antifungal Creams/Gels/Lotions: Applied directly to the affected skin.
- Azole Antifungals:
- Ketoconazole cream 2%: Applied once or twice daily for 2-4 weeks. Very effective for localized tinea versicolor lesions.
- Clotrimazole cream 1%: Applied twice daily for 2-4 weeks.
- Miconazole cream 2%: Applied twice daily for 2-4 weeks.
- Econazole cream 1%: Applied once daily for 2-4 weeks.
- Allylamine Antifungals:
- Terbinafine cream 1%: While primarily effective against dermatophytes, it can be used for Pityriasis versicolor, typically once or twice daily for 1-2 weeks.
- Ciclopirox cream/gel/suspension 0.77%: Applied twice daily for 2-4 weeks. Offers broad-spectrum antifungal activity.
- Azole Antifungals:
- Propylene Glycol 50% in Water: An older but effective treatment, applied twice daily for 2 weeks. It has fungistatic properties.
When using topical agents, consistent application over the entire affected area and slightly beyond is crucial for successful clearance of the yeast infection skin rash. It is also important to continue treatment for the full prescribed duration, even if symptoms appear to improve sooner, to prevent recurrence.
Oral Pityriasis versicolor Treatment
Oral antifungals are reserved for widespread, recalcitrant, or frequently recurring cases of Pityriasis versicolor, or when topical treatments are impractical or ineffective. They offer systemic coverage but come with potential side effects and drug interactions.
- Ketoconazole (Oral):
- Typically 200 mg daily for 5-7 days.
- Alternatively, a single dose of 400 mg can be used, often with the patient advised to sweat heavily (e.g., exercise) 1-2 hours after taking the medication to help distribute the drug to the skin surface.
- Caution: Due to potential hepatotoxicity and drug interactions, oral ketoconazole is less commonly prescribed for Pityriasis versicolor unless other options fail or contraindications exist for other oral antifungals.
- Fluconazole (Oral):
- A common regimen is 300 mg once weekly for 2-4 weeks.
- Alternatively, a single dose of 400 mg can be effective.
- Fluconazole has good penetration into the stratum corneum and is generally well-tolerated.
- Itraconazole (Oral):
- Often prescribed as 200 mg daily for 5-7 days, or 200 mg daily for 7 days then 200 mg once monthly for 6 months as prophylaxis.
- Similar to ketoconazole, patients may be advised to exercise and sweat after taking the dose to enhance delivery to the skin.
Oral medications require careful monitoring for side effects, especially liver function, and consideration of drug-drug interactions. They are usually prescribed by a physician after evaluating the patient’s overall health and the severity of their Pityriasis versicolor symptoms.
Maintenance and Prevention of Pityriasis versicolor
Pityriasis versicolor is prone to recurrence, especially in predisposed individuals (oily skin, warm climates, sweating). Maintenance therapy and preventive measures are crucial for long-term control.
- Regular Use of Antifungal Cleansers: Using selenium sulfide, ketoconazole, or zinc pyrithione shampoos as body washes 1-2 times a week can help keep yeast populations in check. This is particularly useful in warm, humid months or for individuals who sweat heavily.
- Good Skin Hygiene: Regular showering, especially after sweating, helps remove excess oil and yeast from the skin surface.
- Loose-Fitting Clothing: Wearing breathable, loose-fitting clothing made of natural fibers can reduce moisture and heat buildup on the skin, which discourages yeast overgrowth.
- Management of Predisposing Factors: Addressing underlying conditions such as immunosuppression (if present) or managing oily skin with appropriate skincare products can also help.
Post-Treatment Expectations
Patients should be advised that even after successful antifungal treatment, the skin discoloration, especially hypopigmentation (white spots on skin), will not immediately disappear. It can take several weeks to months for the skin to repigment naturally, often requiring sun exposure to stimulate melanin production in the previously affected areas. This is why patients may still see Pityriasis versicolor symptoms pictures of discoloration even when the active infection is gone. Continued sun protection is important for the repigmenting skin to avoid sunburn while it recovers its natural tone.
The successful management of Pityriasis versicolor involves not only clearing the current infection but also implementing strategies to prevent its return, thereby improving both the aesthetic appearance and overall skin health of the individual. Regular follow-ups with a dermatologist can help tailor treatment plans and provide guidance on long-term prevention for this common Malassezia furfur skin infection.