Recognizing the diverse presentations of Pulpitis is crucial for timely intervention and preserving dental health. This article offers an in-depth look at Pulpitis symptoms pictures, guiding readers through the various manifestations of this common dental condition. Understanding these signs and symptoms is the first step towards effective treatment and preventing further complications.
Pulpitis Symptoms Pictures
Pulpitis, the inflammation of the dental pulp, presents with a wide array of symptoms, primarily centered around pain and sensitivity. These symptoms can range from mild and transient to severe and debilitating, significantly impacting daily life. The characteristics of the pain are key indicators for differentiating between reversible and irreversible forms of pulpitis, guiding both diagnosis and subsequent treatment strategies. Early recognition of these
Detailed Pain Characteristics:
- Pain Intensity: The severity of pain is highly variable and can escalate as the pulpitis progresses.
- Mild Pain: Often described as a dull ache or slight sensitivity, typically associated with reversible pulpitis. It might be noticeable only with specific stimuli like cold drinks.
- Moderate Pain: A more pronounced and persistent discomfort. It can be sharp or throbbing, interfering with concentration or light activities.
- Severe Pain: Intense, often excruciating pain that can be constant or come in waves. This level of pain is characteristic of irreversible pulpitis and can be debilitating, making eating, speaking, or even resting difficult.
- Excruciating Pain: The highest level of pain, often described as unbearable, requiring immediate professional attention. It can radiate widely and disrupt sleep profoundly.
- Pain Duration: How long the pain lasts after a stimulus is removed is a critical diagnostic factor.
- Momentary Pain: Pain that subsides almost immediately after the removal of the trigger (e.g., cold air, sweet food). This is typical of reversible pulpitis or dentin hypersensitivity.
- Lingering Pain: Pain that persists for several seconds to minutes after the stimulus is removed. This is a strong indicator of irreversible pulpitis, signaling significant pulpal damage.
- Constant Pain: Pain that is present continuously, with or without external stimuli. This often suggests advanced irreversible pulpitis or pulpal necrosis with periapical involvement.
- Pain Triggers: Specific stimuli often provoke or exacerbate pulpitis pain.
- Cold: Sensitivity to cold drinks, food, or air is a common early symptom. In reversible pulpitis, the pain is sharp and brief. In irreversible pulpitis, the pain is often intense and lingers.
- Heat: Sensitivity or pain triggered by hot drinks or food typically indicates more advanced, irreversible pulpitis, often associated with a necrotic or partially necrotic pulp. Heat can cause expansion of gases within the pulp chamber, leading to increased pressure.
- Sweet: Sugary foods can draw fluid out of the dentinal tubules, stimulating nerve endings and causing pain, particularly in cases of exposed dentin or early caries.
- Pressure/Biting: Pain upon biting or chewing indicates inflammation has spread beyond the pulp to the periapical tissues (periodontal ligament). This is a sign of periapical periodontitis, which often accompanies irreversible pulpitis or necrotic pulp.
- Spontaneous Pain: Pain that occurs without any apparent external stimulus. This is a hallmark of irreversible pulpitis, indicating a high degree of pulpal inflammation.
- Pain Nature: The descriptive quality of the pain provides further clues.
- Sharp Pain: Often described as a sudden, acute, piercing sensation, frequently associated with reversible pulpitis or early irreversible pulpitis to specific triggers.
- Dull Ache: A persistent, low-grade, non-specific pain. Can be present in chronic forms of pulpitis or after initial acute phases.
- Throbbing Pain: A pulsatile pain sensation, often synchronized with the heartbeat, indicating increased blood flow and pressure within an inflamed, confined space like the pulp chamber. This is very characteristic of irreversible pulpitis and acute periapical abscesses.
- Shooting Pain: Pain that rapidly extends or radiates along a nerve pathway.
- Radiating Pain: Pain that spreads from the affected tooth to other areas, such as the jaw, ear, temple, or neck. This makes localization difficult for the patient and is common in irreversible pulpitis.
- Pain Localization:
- Localized Pain: The patient can precisely point to the offending tooth. More common in early or reversible pulpitis.
- Diffuse Pain: The patient has difficulty pinpointing the exact tooth. This is common in irreversible pulpitis, especially in the mandibular molars where pain can refer across the midline.
- Referred Pain: Pain perceived in an area distant from the actual source. Pulpitis can cause referred pain to the ear, temple, sinuses, or opposing jaw.
- Sleep Disruption: Pain severe enough to wake a patient from sleep is a strong indicator of irreversible pulpitis or acute periapical infection.
- Headache, Earache, Jaw Pain: These can be secondary or referred pains originating from a pulpitis-affected tooth, particularly in the posterior regions of the mouth.
- Bad Taste or Smell: If the infection has progressed to form an abscess with a draining sinus tract, a foul taste or odor might be present in the mouth.
- Swelling: While not a direct pulpitis symptom, swelling of the gums or face indicates that the infection has spread beyond the tooth’s root apex into the surrounding soft tissues, potentially forming an abscess or cellulitis. This is a serious complication stemming from untreated pulpitis.
Signs of Pulpitis Pictures
Beyond the subjective symptoms, there are objective signs that a dental professional can observe or elicit during an examination. These signs, coupled with patient history and radiographic findings, form the basis for a definitive diagnosis of pulpitis. Identifying these
Objective Clinical and Diagnostic Signs:
- Visual Signs (Oral Examination):
- Deep Dental Caries (Cavities): The most common cause of pulpitis. Visibly deep cavities, often dark brown or black, that have progressed close to or into the pulp chamber.
- Cracked Tooth Syndrome (Fractures/Craze Lines): Hairline cracks or visible fractures in the enamel or dentin, particularly common in posterior teeth with large restorations or under heavy occlusal stress. These cracks can allow bacteria to penetrate the pulp or cause hydromechanical irritation.
- Discolored Tooth: A tooth affected by pulp necrosis may appear grayish, yellowish-brown, or darker than adjacent teeth due to blood breakdown products within the dentinal tubules.
- Swelling of Gums Around the Affected Tooth: Redness, tenderness, and swelling (erythema and edema) of the gingiva and oral mucosa adjacent to the involved tooth can indicate periapical inflammation or abscess formation.
- Fistula/Sinus Tract (Gum Boil): A small, raised lesion on the gum tissue (or rarely, facial skin) with a central opening, through which pus may drain from an underlying chronic abscess. This indicates a long-standing infection.
- Large or Defective Restorations: Old, leaky, or deep fillings can contribute to pulpal irritation or allow bacterial ingress.
- Palpation Signs:
- Tenderness to Palpation over the Apex: Sensitivity or pain when gentle pressure is applied to the gum tissue over the root tip of the affected tooth. This indicates inflammation of the periapical tissues.
- Tenderness to Palpation of Surrounding Soft Tissues: Pain upon touching adjacent facial or neck soft tissues, suggesting a spread of infection into fascial spaces (e.g., cellulitis).
- Percussion Signs:
- Tenderness to Percussion: Pain elicited when the tooth is gently tapped with the handle of a dental mirror. This is a key sign of inflammation in the periodontal ligament, indicating periapical involvement (periapical periodontitis). A vital pulp with periapical periodontitis suggests irreversible pulpitis, while a non-vital pulp with periapical periodontitis indicates pulpal necrosis.
- Thermal Tests: These tests assess the pulp’s response to temperature changes.
- Exaggerated or Lingering Response to Cold: A sharp, intense pain that lingers for more than a few seconds after the cold stimulus (e.g., ice, Endo-Ice) is removed, strongly suggests irreversible pulpitis. A brief, sharp pain that quickly subsides is characteristic of reversible pulpitis or dentin hypersensitivity.
- Exaggerated or Lingering Response to Heat: Pain triggered by heat (e.g., hot gutta-percha, heated water) that is intense and lingers is highly indicative of irreversible pulpitis, often suggesting liquefaction necrosis or an inflamed pulp attempting to drain. Heat pain can be more difficult to localize.
- No Response to Thermal Tests: The absence of any sensation or pain in response to both hot and cold stimuli indicates a necrotic (dead) pulp.
- Electric Pulp Test (EPT):
- Lower Threshold (Hypersensitivity): The tooth responds to a very low electrical stimulus, indicating a hyper-reactive or inflamed pulp.
- Higher Threshold or No Response: The tooth requires a very strong stimulus or shows no response at all, indicating a compromised or necrotic pulp. EPT only indicates pulp vitality (presence of nerve fibers) but not its health or inflammatory state definitively.
- Mobility:
- Increased Tooth Mobility: While not a primary sign of pulpitis itself, increased tooth looseness can occur if the periapical infection has led to significant bone destruction around the root, or if the tooth has experienced trauma.
- Radiographic Signs (X-rays): Radiographs provide crucial diagnostic information, though early pulpitis may not show any radiographic changes.
- Deep Caries Approaching the Pulp: Visual evidence of cavities extending very close to or into the pulp chamber.
- Periapical Radiolucency: A darkened, well-demarcated or diffuse area at the apex of the root, indicating bone destruction due to chronic inflammation or abscess formation. This is a key sign of periapical periodontitis or an abscess.
- Widening of the Periodontal Ligament Space (PDL): The space between the root and the surrounding bone appears thicker than normal, indicating inflammation of the ligament. This can be an early sign of periapical involvement.
- Internal or External Resorption: Less common, but visible loss of tooth structure either from the inside (internal resorption, often due to chronic pulpitis) or outside (external resorption, due to various factors including periapical infection).
- Presence of Large or Faulty Restorations: Radiographs can show the depth and quality of existing fillings, which might be contributing factors.
Early Pulpitis Photos
Early pulpitis, particularly in its reversible form, often presents with subtle signs and symptoms that can be easily overlooked or mistaken for routine sensitivity. However, prompt identification of these initial manifestations, including characteristic
Characteristics of Early Pulpitis:
- Reversible Pulpitis: This is the initial, mildest form of pulp inflammation where the pulp is still capable of healing once the irritant is removed.
- Pain Description:
- Brief, Sharp Pain to Cold or Sweet: The hallmark symptom. Pain is acute and piercing but lasts only a few seconds after the stimulus (e.g., ice cream, cold air, sugary drink) is removed. It does not linger.
- No Spontaneous Pain: Pain does not occur without an external trigger.
- No Lingering Pain: Once the stimulus is gone, the pain dissipates quickly.
- No Pain on Percussion: Tapping the tooth does not elicit pain, indicating that the inflammation has not yet spread to the periodontal ligament.
- Common Causes:
- Early or Moderate Caries: Cavities that have not yet deeply penetrated the dentin or exposed the pulp.
- Exposed Dentin: Due to gum recession, abrasion (wear from aggressive brushing), erosion (acid wear), or abfraction (stress lesions at the gumline).
- New Restorations: Sometimes, after a new filling is placed, transient sensitivity can occur due to the preparation process or material irritation.
- Minor Cracks or Fractures: Fine craze lines in enamel that cause sensitivity without significant structural compromise.
- Trauma: A mild concussion to the tooth.
- Visual Signs (early stage):
- Small to Moderate Sized Cavities: Often visible as dark spots or small openings on the tooth surface.
- Visible Root Surface: Due to gingival recession.
- Fine Craze Lines or Hairline Fractures: Sometimes only visible under magnification or transillumination.
- Intact Tooth: In cases of trauma, the tooth may appear externally sound but present with sensitivity.
- Radiographic Findings (early stage):
- Often no significant changes on X-rays. Caries may be visible, but no periapical radiolucency or widening of the PDL space.
- Pain Description:
- Early Irreversible Pulpitis: This is the transitional phase where the pulp inflammation is severe enough that it’s unlikely to heal, but the necrotic process may not be fully established.
- Pain Description:
- More Intense, Lingering Pain to Cold/Heat: The pain is sharper and, crucially, lingers for more than a few seconds after the stimulus is removed.
- Spontaneous Pain Episodes: Pain can occur without any external trigger, often at night, disrupting sleep.
- Pain May Radiate: Difficulty in localizing the pain; it may spread to adjacent teeth, the jaw, or ear.
- Pain Worsens When Lying Down: Increased intrapulpal pressure when horizontal can exacerbate the pain.
- Possible Pain with Biting or Chewing Pressure: This indicates early inflammation of the periodontal ligament (early periapical periodontitis).
- Visual Signs:
- Moderate to Deep Cavities: Caries is likely closer to the pulp.
- Visible Cracks or Fractures: May be more pronounced than in reversible pulpitis.
- Large or Failing Restorations: Cracked or leaky fillings can be evident.
- Radiographic Findings:
- Caries approaching the pulp is often visible.
- Periapical changes (e.g., widening of the PDL space) may begin to appear, especially in response to percussion sensitivity.
- Pain Description:
Skin rash Pulpitis Images
It is critical to clarify that pulpitis itself, an inflammation of the dental pulp within the tooth, does not directly cause skin rashes. The symptoms of pulpitis are primarily confined to the tooth and its immediate surrounding structures. However, severe, untreated dental infections originating from pulpitis can spread beyond the tooth, leading to serious complications that
Indirect Skin Manifestations and Complications of Untreated Pulpitis:
When pulpitis progresses to pulpal necrosis and subsequent periapical infection, bacteria can exit the tooth apex and spread into the surrounding bone and soft tissues. This can lead to various types of infections that may present with external, visible signs on the skin of the face or neck. These require immediate medical and dental attention.
- Cellulitis:
- Description: A rapidly spreading bacterial infection of the skin and subcutaneous tissues. It is a serious complication of untreated dental infections.
- Appearance:
- Redness (Erythema): The affected skin area becomes visibly red, often with ill-defined borders, spreading outwards.
- Swelling (Edema): Significant swelling of the facial or neck tissues, which can be firm and warm to the touch.
- Warmth and Tenderness: The area feels hot and painful when touched.
- Shiny or Stretched Skin: The skin over the swollen area may appear taut and shiny.
- Pitting Edema: In some cases, pressing on the swollen area may leave a temporary indentation.
- Location: Depending on the affected tooth and the fascial spaces involved, cellulitis can appear on the cheek (buccal space), under the jaw (submandibular space), around the eye (periorbital cellulitis, extremely dangerous), or in the neck.
- Associated Systemic Symptoms: Fever, chills, malaise, and lymphadenopathy (swollen lymph nodes) are common with cellulitis.
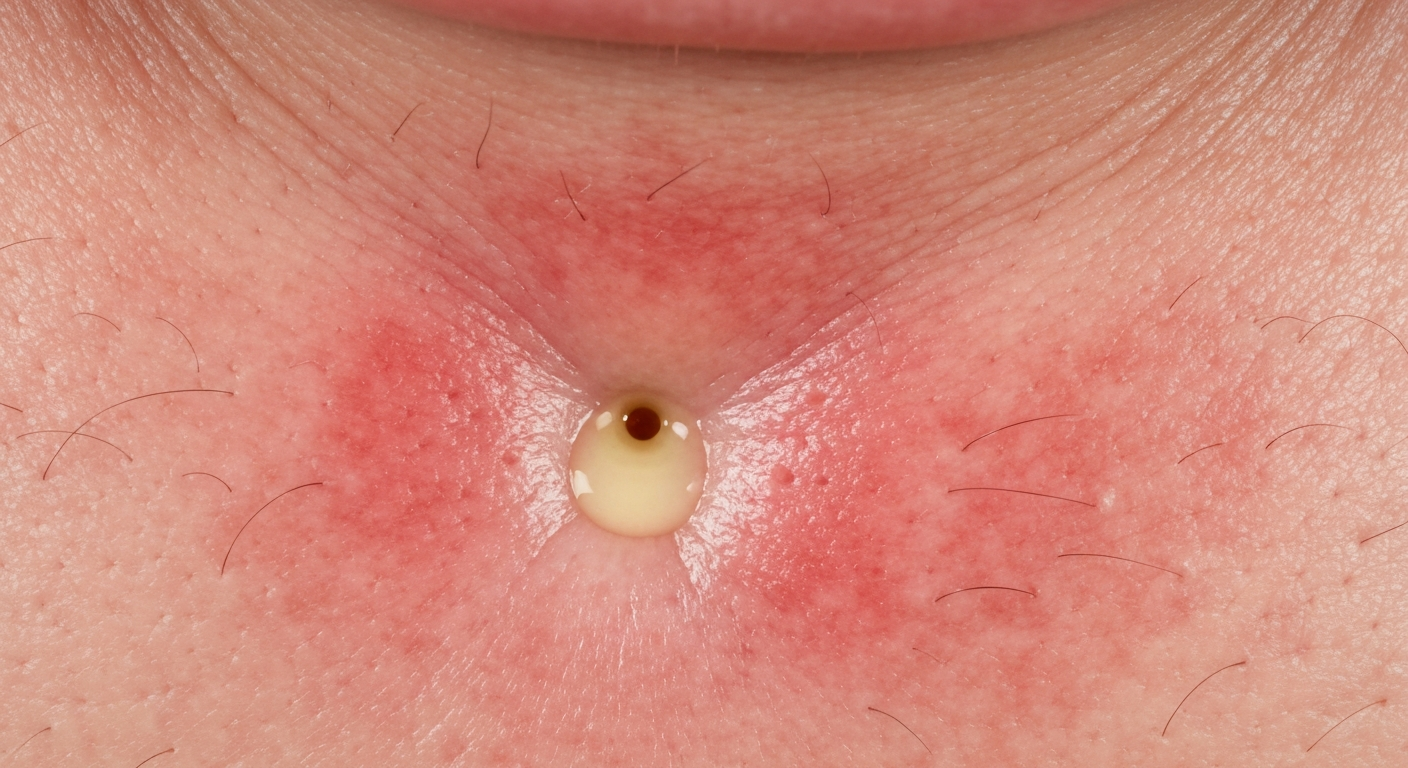
- Fistula/Sinus Tract (Cutaneous or Oral):
- Description: A pathological channel that forms from an infected tooth root to an external surface, allowing pus to drain. While often intraoral (a “gum boil” or parulis), it can occasionally track through bone and soft tissue to the facial skin.
- Appearance:
- Small, Raised Lesion: Appears as a small, pimple-like bump or nodule on the skin (or gum).
- Central Opening: Often has a tiny opening through which pus or serosanguinous fluid may intermittently discharge. This discharge can relieve pressure, sometimes leading to a reduction in pain.
- Healing and Scarring: Once the underlying infection is treated, the tract usually closes and heals, sometimes leaving a small scar or dimple.
- Location: If cutaneous, it typically appears on the chin, cheek, or submandibular area, often directly overlying the apex of the infected tooth. Patients might initially mistake it for an acne lesion or an insect bite.
- Abscess (Cutaneous/Subcutaneous):
- Description: A localized collection of pus in the skin or subcutaneous tissues, often as a result of a spreading dental infection. This is distinct from cellulitis, which is a diffuse infection.
- Appearance:
- Swollen, Tender Lump: A distinct, raised, often red and warm mass under the skin.
- Fluctuant: As the abscess matures, it becomes soft and compressible to the touch, indicating the presence of fluid (pus).
- Pain: Often accompanied by significant localized pain.
- Location: Similar to cellulitis, can form on the face or neck if the dental infection tracks externally and becomes walled off.
- Ludwig’s Angina:
- Description: A rare, but extremely severe and life-threatening form of cellulitis involving the submandibular, sublingual, and submental spaces. It typically originates from infected mandibular molars.
- Appearance:
- Massive Brawny Edema: Severe, firm swelling of the floor of the mouth and neck, which may cause elevation of the tongue.
- Dysphagia (Difficulty Swallowing) and Dyspnea (Difficulty Breathing): Due to airway compromise.
- Fever, Chills, Malaise: Systemic signs of severe infection.
- Skin Changes: The skin overlying the affected areas (e.g., under the jaw, anterior neck) becomes red, tense, and warm, but usually lacks the characteristic fluctuance of an abscess.
- Systemic Reactions (Rare, Severe Sepsis):
- Description: In extremely rare and severe cases where an uncontrolled dental infection leads to sepsis (a life-threatening response to infection), generalized skin manifestations can occur.
- Appearance:
- Petechiae: Small, pinpoint, non-blanching red spots on the skin due to capillary bleeding.
- Purpura: Larger areas of hemorrhage into the skin.
- Diffuse Erythema or Rash: Non-specific skin reactions that can accompany severe systemic inflammation.
- Significance: These are signs of a critical medical emergency requiring immediate hospitalization and aggressive treatment. They are not direct pulpitis symptoms but indicate a catastrophic failure to contain the dental infection locally.
In summary, while pulpitis primarily affects the tooth, these external skin signs underscore the critical importance of treating dental infections promptly to prevent severe, potentially life-threatening complications. Any such skin manifestation in conjunction with dental pain warrants urgent evaluation.
Pulpitis Treatment
The treatment for pulpitis depends critically on its classification – whether it is reversible or irreversible – and the extent of pulpal and periapical involvement. The primary goal of
Treatment for Reversible Pulpitis:
The aim is to remove the irritant and allow the pulp to heal. This is the most conservative form of intervention.
- Removal of Irritant:
- Caries Removal: The most common intervention. All decayed tooth structure is meticulously removed.
- Replacement of Defective Restorations: Leaky or poorly contoured fillings that cause chronic irritation are replaced.
- Addressing Exposed Dentin:
- Fluoride Application: Professional fluoride varnishes or gels can help remineralize exposed dentin and reduce sensitivity.
- Desensitizing Agents: Various over-the-counter or professional agents containing ingredients like potassium nitrate or strontium chloride can block dentinal tubules.
- Bonding or Fillings: To cover areas of severe abrasion, erosion, or exposed root surfaces due to recession.
- Treatment of Cracked Tooth:
- Bonding/Sealants: For superficial craze lines.
- Occlusal Adjustment: To reduce excessive biting forces on the affected tooth.
- Crown Placement: A full coverage crown can bind the fractured tooth segments together, preventing further propagation of the crack and protecting the pulp.
- Deep Fillings with Protective Liner/Base:
- When caries is deep but not yet exposed the pulp, a protective liner (e.g., calcium hydroxide, glass ionomer) is placed on the deepest portion of the cavity preparation before the final filling material. This aims to stimulate tertiary dentin formation and insulate the pulp.
Treatment for Irreversible Pulpitis / Necrotic Pulp:
When the pulp is irreversibly damaged or necrotic, it cannot heal and must be removed to prevent further infection spread and alleviate pain. The primary treatments are root canal therapy or extraction.
- Root Canal Treatment (Endodontic Therapy): This is the preferred method to save a tooth with irreversible pulpitis or necrosis.
- Steps Involved:
- Access Cavity Preparation: An opening is made through the crown of the tooth to gain access to the pulp chamber and root canals.
- Pulp Extirpation: The inflamed or infected pulp tissue is completely removed from the pulp chamber and root canals.
- Cleaning and Shaping: The root canals are meticulously cleaned and shaped using specialized endodontic files (manual or rotary) to remove bacteria, debris, and infected dentin.
- Disinfection: Irrigation solutions (e.g., sodium hypochlorite, EDTA) are used throughout the cleaning process to disinfect the canals. Intra-canal medications (e.g., calcium hydroxide) may be placed between appointments for continued disinfection.
- Obturation (Filling the Canal): Once thoroughly cleaned and disinfected, the canals are filled and sealed with a biocompatible material, typically gutta-percha, combined with a sealer. This prevents reinfection.
- Coronal Restoration: After root canal treatment, the access cavity is sealed with a permanent filling, and often a full-coverage crown is recommended to protect the treated tooth from fracture, as endodontically treated teeth can become more brittle.
- Purpose: To eliminate bacteria and inflammation from the root canal system, save the natural tooth, preserve chewing function, and maintain the aesthetic appearance.
- Steps Involved:
- Pulp Capping (Direct and Indirect): These are vital pulp therapies aimed at preserving the health and function of the dental pulp.
- Indirect Pulp Cap (IPC):
- Indication: When deep caries is removed, a thin layer of affected (but not infected) dentin is left immediately over the pulp to avoid pulp exposure.
- Procedure: A biocompatible material (e.g., calcium hydroxide, MTA, glass ionomer) is placed over this remaining dentin, and then the tooth is restored. The goal is to promote remineralization and formation of tertiary dentin.
- Direct Pulp Cap (DPC):
- Indication: When a small, mechanical (traumatic) or carious exposure of a healthy or reversibly inflamed pulp occurs.
- Procedure: A biocompatible material (e.g., MTA, calcium hydroxide) is placed directly onto the exposed pulp tissue, followed by a permanent restoration. The goal is to stimulate a dentin bridge formation and maintain pulp vitality. More successful in young, vital permanent teeth.
- Indirect Pulp Cap (IPC):
- Pulpotomy:
- Description: The removal of the inflamed or infected coronal (crown portion) pulp, while leaving the vital radicular (root portion) pulp intact and attempting to preserve its vitality.
- Indication: Primarily used in primary (baby) teeth with reversible or early irreversible pulpitis, or in immature permanent teeth with carious pulp exposure where root formation is incomplete.
- Procedure: The inflamed coronal pulp is removed, hemostasis is achieved, and a medicament (e.g., MTA, calcium hydroxide, formocresol) is placed over the radicular pulp stumps before final restoration.
- Extraction (Tooth Removal):
- Indication: When the tooth is severely damaged, unrestorable (e.g., extensive fracture below the gum line, severe periodontal disease), or if root canal treatment is not feasible, desired, or has failed. It is the last resort for irreversible pulpitis or necrotic pulp.
- Follow-up Options: After extraction, options to replace the missing tooth include dental implants, fixed bridges, or removable partial dentures to maintain function and aesthetics.
Pain Management During Treatment:
- Local Anesthesia: Essential for pain control during all dental procedures, ensuring patient comfort.
- Systemic Analgesics: Over-the-counter pain relievers (e.g., NSAIDs like ibuprofen, acetaminophen) or prescription medications may be recommended to manage pain post-procedure or while awaiting definitive treatment.
- Antibiotics:
- Not for Pulpitis Itself: Antibiotics are generally not effective for pain or infection strictly confined within the pulp chamber, as the compromised blood supply limits their delivery.
- Indication: They are prescribed only if the infection has spread beyond the tooth’s confines, causing systemic signs (fever, malaise), localized swelling (abscess, cellulitis), or in immunocompromised patients.
Prevention of Pulpitis:
Preventative measures are critical for maintaining oral health and avoiding pulpitis.
- Good Oral Hygiene: Regular brushing with fluoride toothpaste and flossing removes plaque and prevents caries formation.
- Regular Dental Check-ups and Cleanings: Allows for early detection and treatment of cavities and other dental issues before they progress to pulpitis.
- Prompt Treatment of Cavities: Addressing cavities when they are small prevents them from deepening and reaching the pulp.
- Use of Mouthguards: For individuals who grind their teeth (bruxism) or participate in contact sports, mouthguards can protect teeth from cracks and fractures.
- Dietary Control: Limiting sugary and acidic foods and drinks reduces the risk of dental decay and erosion.
More from my site: