When wondering what does Demodicosis look like symptoms pictures can offer crucial insights into this often perplexing skin condition. The visual manifestations of Demodex mite infestations are diverse, ranging from subtle skin changes to severe inflammatory reactions that mimic other dermatoses. Understanding these visible signs is key to proper identification and management of Demodicosis symptoms.
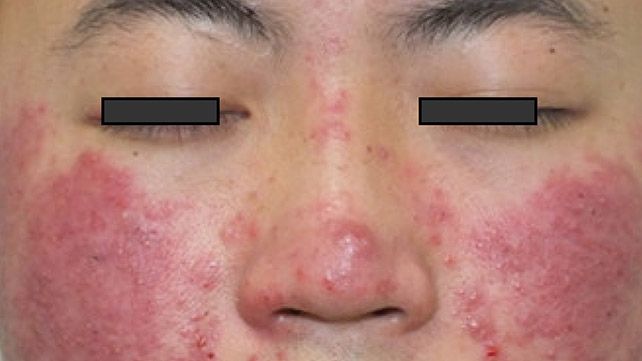
Demodicosis Symptoms Pictures
Demodicosis, a skin condition caused by an overpopulation of Demodex mites, presents a wide array of visual symptoms that can often be observed in Demodicosis symptoms pictures. The appearance is highly variable, influenced by factors such as the individual’s immune response, the density of the mite infestation, and the specific species of Demodex involved (primarily Demodex folliculorum and Demodex brevis). Visually, Demodicosis frequently mimics other common dermatological conditions like rosacea, acne, perioral dermatitis, and seborrheic dermatitis, making accurate diagnosis challenging without clinical examination and sometimes microscopic confirmation.
The primary sites for visible symptoms are typically the face, especially the cheeks, forehead, nose, and chin, but ocular involvement (eyelids) and, less commonly, the neck, scalp, chest, and back can also show signs of Demodex skin infestation. When considering Demodex pictures, one often sees a persistent redness or flushing, accompanied by various types of bumps and skin texture changes. The inflammation is a key component, leading to a chronically irritated appearance.
The visual characteristics commonly seen in Demodicosis symptoms pictures include:
- Erythema (Redness): Often presents as persistent facial redness, sometimes resembling rosacea. This redness can be diffuse or localized to specific areas like the cheeks and nose. In some cases, it can be severe and widespread, giving the skin a flushed or sunburnt appearance.
- Papules: Small, solid, raised bumps that are typically red or skin-colored. These Demodex papules often appear in clusters, particularly on the forehead, cheeks, and around the mouth. They can be tender to the touch.
- Pustules: Small, pus-filled bumps that are superficial and often surrounded by redness. These Demodex pustules are a common feature, mimicking acne vulgaris, but they may lack the comedones typical of true acne.
- Scaling: Fine, flaky skin often present around hair follicles, particularly on the forehead, eyebrows, and nose. This scaling can be subtle or quite pronounced, giving the skin a dry, rough texture.
- Rough or Uneven Skin Texture: The skin may feel gritty or bumpy to the touch, even in areas without overt papules or pustules, due to follicular involvement and inflammation.
- Telangiectasias (Visible Blood Vessels): Fine, thread-like red lines, especially on the cheeks and nose, similar to those seen in rosacea. These are a sign of chronic inflammation and vascular dilation.
- Follicular Pits or Enlarged Pores: Visible openings of hair follicles that may appear more prominent due to inflammation and mite activity within the follicles.
- Perioral Dermatitis-like Eruptions: A rash of small papules and pustules around the mouth, chin, and sometimes extending to the nose and eyes, often misdiagnosed as perioral dermatitis.
- Pruritus (Itching): While not directly visible, intense itching is a common subjective symptom. Scratching can lead to excoriations and secondary infections, altering the visual presentation.
- Burning or Stinging Sensation: Another subjective symptom that contributes to the overall discomfort and can accompany the visible inflammation.
- Increased Skin Sensitivity: Patients often report that their skin feels unusually sensitive to touch, cosmetics, or environmental factors.
- Changes in Skin Pigmentation: Post-inflammatory hyperpigmentation (darker patches) or hypopigmentation (lighter patches) can occur after resolution of active lesions, especially in individuals with darker skin tones.
- Blepharitis (Eyelid Inflammation): When Demodex mites infest the eyelashes and meibomian glands, it leads to redness, itching, scaling, and crusting along the eyelid margins. This is a very distinctive visual sign.
- Madarosis (Eyelash Loss): Chronic Demodex infestation of the eyelids can weaken hair follicles, leading to thinning or loss of eyelashes.
- Cylindrical Dandruff (Collarettes): Waxy, sleeve-like deposits at the base of eyelashes, a highly characteristic sign of ocular demodicosis that can be seen upon close inspection.
When reviewing Demodicosis skin photos, it’s essential to look for these combinations of symptoms rather than relying on a single isolated feature, as the presentation is often multifactorial and can vary significantly from one individual to another.
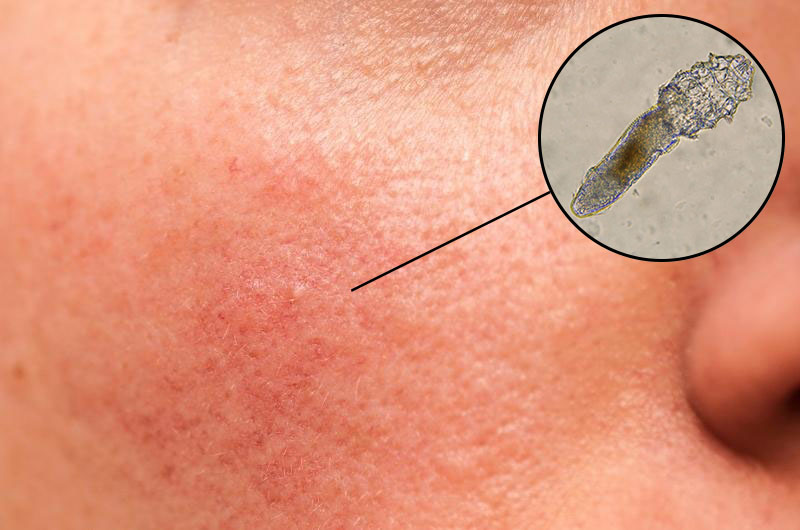
Signs of Demodicosis Pictures
Examining signs of Demodicosis pictures reveals the more specific and often diagnostic visual clues of a Demodex mite infestation. These signs are critical for differentiating Demodicosis from other dermatological conditions. The primary visual manifestations stem from the mites’ activity within hair follicles and sebaceous glands, leading to inflammation, follicular distension, and immune responses. Understanding these precise visual details in Demodex infestation photos is vital for healthcare professionals and individuals seeking to recognize potential symptoms.
Distinctive signs of Demodicosis pictures include:
- Follicular Erythema and Edema: Redness and swelling specifically around hair follicles, giving the skin a speckled or punctate erythematous appearance. This is a direct visual cue of follicular involvement.
- Follicular Scales/Crusting: Fine, often greasy scales or crusts localized at the opening of hair follicles. These can be particularly noticeable on the forehead, T-zone, and around the brows, indicating increased cellular turnover and inflammatory exudate.
- Perifollicular Pustules: Small pustules that are centered around a hair follicle, sometimes appearing as a whitehead with a red base. These can differentiate Demodicosis from general acne, which often has open and closed comedones.
- Rosacea-like Erythema with Papules and Pustules: A common presentation where the facial skin shows persistent redness and outbreaks of small red bumps (papules) and pus-filled lesions (pustules). Unlike classic rosacea, Demodicosis-related papules and pustules often have a more uniform appearance and may respond poorly to traditional rosacea treatments.
- Demodex Granuloma: In rare, severe cases, especially in immunocompromised individuals, Demodex mites can induce a granulomatous reaction, forming firm, persistent nodules or plaques. These represent a deeper, more chronic inflammatory response.
- Ocular Demodicosis Signs:
- Cylindrical Dandruff (Collarettes): One of the most pathognomonic Demodex eye symptoms. These are waxy, tube-like deposits of keratin and lipids that encircle the base of the eyelashes. They are typically seen upon close examination with a magnified view, appearing as tiny sleeves on the lash shafts.
- Eyelid Margin Redness and Swelling (Blepharitis): The edges of the eyelids become inflamed, red, and swollen, often with associated itching and burning sensations. This can be anterior (involving the lash line) or posterior (involving the meibomian glands).
- Crusting and Scaling on Eyelids: Flaky deposits along the lash line, contributing to discomfort and irritation.
- Misdirected Eyelashes (Trichiasis): Eyelashes that grow inwards towards the eye, leading to irritation and potential corneal damage. This can be a consequence of chronic follicular inflammation.
- Loss of Eyelashes (Madarosis): Thinning or complete loss of eyelashes due to sustained mite activity and damage to the hair follicles.
- Conjunctivitis: Chronic irritation of the conjunctiva (the membrane lining the eyelids and covering the white part of the eye), leading to redness and discomfort.
- Scalp Involvement: Less common, but can present as patchy hair loss (alopecia), scalp itching, redness, and folliculitis, with small red bumps or pustules on the scalp.
- Back and Chest Lesions: In some cases, papulopustular lesions can extend to the back and chest, particularly in individuals with a higher mite load or compromised immune systems. These body Demodex signs may resemble truncal acne.
- Hyperpigmentation/Hypopigmentation: Persistent inflammation can lead to post-inflammatory changes in skin color, particularly in individuals with skin of color.
- Skin Thickening and Coarseness: Chronic inflammation can lead to a slight thickening of the skin, making it feel less smooth and supple.
- Excoriations: Scratch marks resulting from intense itching, which can further alter the skin’s appearance and increase the risk of secondary bacterial infections.
Observing these specific Demodex skin signs, especially the characteristic cylindrical dandruff in ocular cases or the perifollicular pustules on the face, significantly aids in a differential diagnosis for skin mite infestation pictures. The distribution patterns and the specific morphology of the lesions are crucial in interpreting Demodicosis photos.
Early Demodicosis Photos
Identifying early Demodicosis photos can be particularly challenging due to the subtle and often non-specific nature of initial symptoms. At this stage, the mite population may not be excessively high, or the host’s immune response might not yet be fully activated, leading to mild or transient skin changes. Patients often attribute these early signs to everyday skin irritation, mild acne breakouts, or sensitive skin reactions. However, recognizing these nascent signs of incipient Demodex infestation is crucial for timely intervention and preventing progression to more severe forms. Early visual cues are frequently confused with the very first signs of rosacea or adult-onset acne, underscoring the importance of a high index of suspicion, especially when symptoms are persistent or unresponsive to standard treatments for those conditions.
Key features to look for in early Demodicosis photos:
- Subtle Redness (Erythema):
- Transient Flushing: Occasional or intermittent redness on the cheeks, nose, or forehead that appears and disappears, often triggered by heat, stress, or spicy foods.
- Mild Persistent Erythema: A very slight, generalized pinkish hue on facial skin, perhaps just enough to make the complexion appear a bit “off” or mildly irritated without overt inflammation.
- Minor Skin Texture Changes:
- Slight Roughness: The skin may feel less smooth than usual, with a subtle grainy or sandpapery texture upon touch. This can be due to mild follicular involvement.
- Barely Noticeable Bumps: Very small, skin-colored or slightly red bumps that are not fully formed papules or pustules, perhaps only visible under certain lighting or close inspection. These early Demodex bumps might be mistaken for clogged pores.
- Follicular Prominence:
- Slightly Enlarged Pores: Pores may appear a fraction more prominent, particularly in the T-zone, though not necessarily blocked. This can be a subtle sign of mite activity within the follicles.
- Subtle Perifollicular Redness: A very faint ring of redness directly around individual hair follicles, noticeable on very close inspection.
- Mild Scaling:
- Fine Flaking: Almost imperceptible, fine, powdery flaking of the skin, especially on the forehead or around the nose. This might be mistaken for dry skin.
- Barely Visible Follicular Scales: Tiny, adherent scales at the base of vellus hairs, requiring magnification to discern.
- Sensory Symptoms (Though Not Visible, Often Reported Early):
- Mild Itching: Occasional, localized itching or tickling sensation on the face, especially in the evenings or when warm. This is a common early Demodex symptom.
- Subtle Burning/Stinging: A mild, intermittent sensation of burning or stinging, particularly after applying products or exposure to environmental factors.
- Increased Sensitivity: The skin may feel more reactive to previously tolerated skincare products or cosmetics.
- Eyelid Changes (Early Ocular Demodicosis):
- Mild Eyelid Itching: Occasional itching of the eyelids, especially along the lash line.
- Subtle Eyelash Thinning: A slight, generalized thinning of eyelashes that might not be immediately obvious but becomes noticeable over time.
- Faint Redness on Eyelid Margins: A very slight pinkish discoloration along the edge of the eyelids, easily missed or dismissed as tired eyes.
- Microscopic Collarettes: While full-blown cylindrical dandruff is a distinct sign, in early stages, microscopic amounts of debris at the lash base might be present, requiring high magnification to observe.
- Lack of Typical Acne Comedones: Unlike early acne, early Demodex rash typically lacks blackheads (open comedones) or whiteheads (closed comedones), even if papules and pustules are present. This can be a differentiating factor when examining photos of early skin conditions.
The challenge with early Demodicosis pictures is that these signs are often so subtle that they don’t immediately suggest a parasitic infestation. A dermatologist or a very observant individual might notice a persistent “something isn’t quite right” with the skin’s texture or tone, especially if the symptoms do not respond to conventional acne or rosacea treatments. The presence of any of these early, persistent visual changes, particularly when accompanied by itching or a burning sensation, should raise suspicion for early Demodex symptoms.
Skin rash Demodicosis Images
The term “skin rash Demodicosis images” refers to the more overt and often widespread inflammatory presentations of Demodex infestation. These rashes are typically characterized by erythema (redness), papules, and pustules, and can vary significantly in intensity and distribution. Unlike a simple allergic rash, Demodex skin rashes are inflammatory and follicular in nature, often presenting with a chronic course and specific patterns that can be seen in various Demodex rash photos. The appearance of the rash is highly dependent on the host’s immune reaction to the mites, their waste products, and the associated bacteria. These rashes are a significant reason for patient discomfort and can have a considerable impact on quality of life, often being misdiagnosed as recalcitrant acne or steroid-induced rosacea.
Common presentations of skin rash Demodicosis images:
- Papulopustular Demodicosis:
- Appearance: Characterized by numerous small, red papules and pus-filled pustules, primarily on the central face (cheeks, forehead, chin, nose). The lesions are often uniform in size and lack the comedones typical of acne.
- Distribution: Commonly affects the convexities of the face, mirroring rosacea patterns. It can extend to the perioral and perinasal areas, resembling perioral dermatitis.
- Distinguishing Features: The lesions tend to be perifollicular, meaning they are centered around hair follicles. Persistent redness underlies the papules and pustules. These Demodex face rash pictures often show a “chicken skin” or “strawberry nose” appearance in severe cases due to follicular prominence and inflammation.
- Erythematous Demodicosis:
- Appearance: Primarily characterized by persistent and diffuse facial redness (erythema), sometimes accompanied by mild scaling and a burning sensation. Telangiectasias may also be present, similar to erythematotelangiectatic rosacea.
- Distribution: Widespread across the face, often worse on the cheeks and nose, but can affect the entire facial area, including the forehead and chin.
- Distinguishing Features: Lack of significant papules or pustules, but the underlying inflammation and erythema are prominent. This form of Demodex redness can be quite disfiguring, giving a constant flushed look.
- Granulomatous Demodicosis:
- Appearance: A rarer and more severe form, presenting as firm, red-brown to violaceous nodules or plaques. These lesions are deeper and more persistent than typical papules.
- Distribution: Can occur anywhere on the face, but sometimes solitary or few lesions, requiring biopsy for definitive diagnosis.
- Distinguishing Features: Histopathology reveals granulomatous inflammation around Demodex mites. This severe Demodex skin rash is often associated with immunocompromised states.
- Perioral/Perinasal Demodicosis:
- Appearance: A cluster of small papules and pustules around the mouth (perioral), nose (perinasal), and sometimes eyes (periocular). The skin in these areas often appears red and slightly scaly.
- Distribution: Concentrated in a horseshoe-like pattern around the mouth and nose, often sparing a narrow border around the lips.
- Distinguishing Features: Often misdiagnosed as perioral dermatitis. The presence of mites is the key differentiator. These Demodex rash photos frequently show a clear distinction from true perioral dermatitis.
- Demodex Folliculitis:
- Appearance: Inflammation of hair follicles, leading to small, red bumps or pustules centered around a hair. This can occur on the face, scalp, neck, or trunk.
- Distribution: Can be localized or widespread depending on the mite load and host response. On the scalp, it may lead to patchy hair loss or general scalp irritation.
- Distinguishing Features: The follicular orientation of the lesions is key. These Demodex folliculitis images show distinct individual inflamed follicles.
- Ocular Demodicosis Rash (Eyelid Rash):
- Appearance: Redness, swelling, itching, and scaling along the eyelid margins. The most definitive visual sign is the presence of cylindrical dandruff (collarettes) at the base of the eyelashes.
- Distribution: Confined to the eyelids and lash line.
- Distinguishing Features: The unique cylindrical dandruff is highly diagnostic. Eyelid Demodex pictures clearly show these white, waxy sleeve-like structures.
- Scalp Demodicosis:
- Appearance: Can manifest as diffuse or patchy hair loss, redness of the scalp, itching, and small perifollicular papules or pustules.
- Distribution: Affects the hair-bearing areas of the scalp.
- Distinguishing Features: Often mistaken for seborrheic dermatitis or other forms of folliculitis. Hair pull test may show increased shedding.
The chronic inflammatory nature of Demodicosis means that these rashes can persist for extended periods, waxing and waning in intensity. The visual appearance of skin rash Demodicosis images highlights the need for a thorough diagnostic approach, often involving microscopic examination of skin scrapings or eyelash samples to confirm the presence of an elevated Demodex mite count. This distinction is crucial because the treatment strategies for Demodicosis differ significantly from those for similar-looking conditions, ensuring effective resolution of the Demodex rash.
Demodicosis Treatment
While the visual aspect of Demodicosis treatment focuses on symptom resolution and skin clearance, understanding the treatments helps interpret the before-and-after Demodicosis treatment pictures. Effective treatment aims to reduce the mite population, quell the inflammatory response, and restore skin barrier function, leading to a visible improvement in redness, papules, pustules, and overall skin texture. The choice of therapy depends on the severity and type of Demodicosis, as well as the patient’s individual response and tolerance. Seeing the progressive improvement in skin with Demodex photos post-treatment is a significant indicator of success. The goal is not just temporary relief but sustained visual and symptomatic improvement, minimizing the recurrence of Demodex rash and associated discomfort.
The visual outcomes and types of Demodicosis treatment typically include:
- Topical Medications: These are often the first-line treatment for localized or mild-to-moderate facial Demodicosis, leading to gradual visual improvement.
- Ivermectin Cream (1%):
- Mechanism: Anthelmintic properties directly target Demodex mites, reducing their numbers. Also has anti-inflammatory effects.
- Visual Outcomes: Significant reduction in erythema, papules, and pustules. Skin appears less inflamed, smoother, and more even-toned. Often shows marked improvement in Demodex before and after pictures within weeks.
- Metronidazole Gel/Cream:
- Mechanism: Primarily anti-inflammatory, helps reduce redness and some inflammatory lesions.
- Visual Outcomes: Reduces general redness and mild papulopustular lesions. Often used for its anti-inflammatory properties, complementing mite-eradicating agents. Skin becomes less sensitive and appears calmer.
- Permethrin Cream:
- Mechanism: A potent scabicide and acaricide that kills mites.
- Visual Outcomes: Effective in reducing mite load, leading to a decrease in itching, papules, and pustules. Often used for body involvement or resistant facial cases.
- Benzoyl Peroxide:
- Mechanism: Has some acaricidal and antibacterial properties, helps with follicular exfoliation.
- Visual Outcomes: Can help reduce mild inflammatory lesions and improve skin texture by unclogging pores. Helps resolve small bumps and general irritation.
- Sulfur Preparations:
- Mechanism: Mild acaricidal and anti-inflammatory properties.
- Visual Outcomes: Can contribute to reducing redness and small bumps, especially in over-the-counter formulations or specialized cleansers.
- Tea Tree Oil (TTO) Products (usually diluted):
- Mechanism: Natural acaricidal properties, particularly for ocular Demodicosis.
- Visual Outcomes: For eyelid Demodicosis, it visibly reduces cylindrical dandruff, eyelid redness, and swelling. Eyelashes appear cleaner and healthier. Strong concentrations used professionally can clear debris effectively, while diluted forms are for home maintenance.
- Ivermectin Cream (1%):
- Oral Medications: Used for more severe, widespread, or resistant cases of Demodex infestation, often providing more rapid and comprehensive visual improvement.
- Oral Ivermectin:
- Mechanism: Systemic acaricide, rapidly kills mites throughout the body.
- Visual Outcomes: Dramatic reduction in widespread papules, pustules, and erythema. Often leads to significant overall facial clearance, visible within days to weeks. Particularly effective for extensive or recalcitrant cases where topical agents alone are insufficient.
- Doxycycline (subantimicrobial dose):
- Mechanism: Anti-inflammatory properties (at low doses), rather than antibiotic. Reduces redness and inflammatory lesions.
- Visual Outcomes: Significant reduction in persistent facial redness and inflammatory papules/pustules, contributing to a calmer, less inflamed appearance. Often used in conjunction with acaricidal treatments.
- Oral Ivermectin:
- Eyelid Hygiene and Ocular Treatment: Specific protocols for ocular Demodex treatment directly address visual signs on the eyelids.
- Lid Scrubs with TTO:
- Visual Outcomes: Immediate and progressive reduction of cylindrical dandruff (collarettes), eyelid margin redness, and crusting. Eyelashes appear cleaner, and eyelid swelling subsides.
- Warm Compresses:
- Visual Outcomes: Reduces swelling and redness, improves comfort, and helps to soften crusts for easier removal.
- Prescription Eye Drops/Ointments:
- Visual Outcomes: Addresses associated dry eye or secondary infections, leading to clearer, less irritated eyes and eyelids.
- Lid Scrubs with TTO:
- Supportive Skincare and Lifestyle Modifications:
- Gentle Cleansing and Moisturizing:
- Visual Outcomes: Helps maintain skin barrier integrity, reducing general redness and irritation. Prevents dryness or excessive oiliness which can exacerbate symptoms. Skin appears healthier and less reactive.
- Avoidance of Triggers:
- Visual Outcomes: Minimizes flare-ups of redness and flushing, contributing to a more stable and consistently clear complexion.
- Gentle Cleansing and Moisturizing:
The effectiveness of Demodicosis treatment is visually evidenced by the progressive fading of erythema, the flattening and resolution of papules and pustules, the reduction in scaling, and the restoration of a smoother, healthier-looking skin texture. For ocular Demodicosis, the disappearance of cylindrical dandruff and the reduction of eyelid inflammation are clear visual markers of successful therapy. Long-term management often involves maintenance therapy to prevent recurrence, ensuring that the visual improvements are sustained and the skin remains clear of Demodex symptoms.
