Understanding what does Necrobiosis Lipoidica look like symptoms pictures is crucial for early identification and appropriate management. This article provides an in-depth visual guide to the manifestation of this chronic dermatological condition, focusing on its distinctive presentation across various stages.
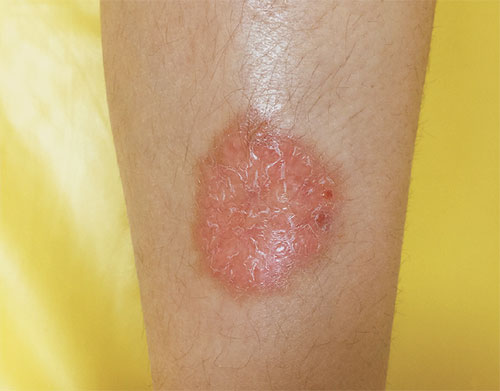
Necrobiosis Lipoidica Symptoms Pictures
The visual characteristics of Necrobiosis Lipoidica are often striking and evolve significantly over time, making detailed descriptions vital for recognizing its presence. Typically affecting the shins, the lesions present a complex array of symptoms that are best understood through a chronological and morphological lens. Patients and healthcare providers frequently seek to understand the progression of these unique skin changes.
Here are the primary visual symptoms and features commonly observed:
- Initial Appearance: The earliest manifestation of Necrobiosis Lipoidica often begins as one or more small, firm, reddish-brown papules or nodules. These initial lesions are typically discrete and may be slightly raised, sometimes resembling an insect bite or a minor trauma. Their color can vary from a pale pink to a more pronounced reddish hue.
- Progression to Plaques: Over weeks to months, these initial papules or nodules gradually expand and coalesce to form well-demarcated, irregularly shaped plaques. These plaques are the hallmark of developed Necrobiosis Lipoidica. The borders are often slightly raised and erythematous (reddish), indicating active inflammation.
- Central Atrophy and Discoloration: A distinctive feature of mature Necrobiosis Lipoidica plaques is the development of central atrophy. The skin in the center of the plaque becomes thinned, shiny, and often takes on a yellowish, waxy, or translucent appearance due to the loss of subcutaneous fat and dermal collagen. This central yellow discoloration is a key diagnostic sign for necrobiosis lipoidica appearance. The underlying blood vessels may become visible through the atrophic skin, giving a telangiectatic appearance.
- Color Spectrum: The color profile of Necrobiosis Lipoidica lesions is highly variable, reflecting different stages of inflammation and tissue damage.
- Reddish-Brown Periphery: The outer edges of the plaques often maintain an active, reddish-brown, or violaceous (purplish) hue, signifying ongoing inflammation and progression.
- Yellowish-Brown Center: As the lesion matures, the central area typically develops a characteristic yellowish, waxy, or even orange-brown tint. This is attributed to lipid deposition and granulomatous inflammation within the dermis and subcutaneous tissue, representing the `necrobiosis` component.
- Telangiectasia: Fine, dilated blood vessels (telangiectasias) are frequently visible within the atrophic, yellowish center, contributing to the variegated appearance of the necrobiosis lipoidica lesions.
- Texture Changes: The texture of the skin within the plaque undergoes significant alteration:
- Shiny and Smooth: The atrophic center often appears remarkably shiny and smooth, almost glazed, due to the thinning of the epidermis and loss of adnexal structures.
- Waxy or Indurated: The skin can feel firm or indurated, especially at the borders, due to granulomatous inflammation and fibrous tissue deposition.
- Fragility: The thinned, atrophic skin in the center is exceedingly fragile and prone to trauma, which can easily lead to ulceration, a significant complication.
- Ulceration: One of the most severe complications and a common symptom of advanced Necrobiosis Lipoidica is ulceration. The fragile, atrophic skin, particularly on the shins, is highly susceptible to minor trauma, leading to chronic, often painful, and slow-healing ulcers. These ulcers can be shallow or deep, sometimes exposing subcutaneous tissue or even bone, and are a major source of morbidity. Recognizing necrobiosis lipoidica ulceration is critical for wound care planning.
- Pain and Discomfort: While some patients experience no pain, many report tenderness, itching, burning, or a dull ache associated with the lesions, especially when they are inflamed or ulcerated. Ulcers are particularly noted for their pain.
- Bilateral but Asymmetrical: Necrobiosis Lipoidica often affects both legs but usually in an asymmetrical pattern, meaning the lesions may be different in size, number, or stage of progression on each leg.
- Location: While typically found on the anterior aspects of the lower legs (shins), lesions can occasionally occur on other body parts, including the arms, trunk, scalp, or face, although these presentations are rarer.
Understanding these detailed visual cues is paramount for correct identification of necrobiosis lipoidica skin changes and distinguishing it from other dermatological conditions.
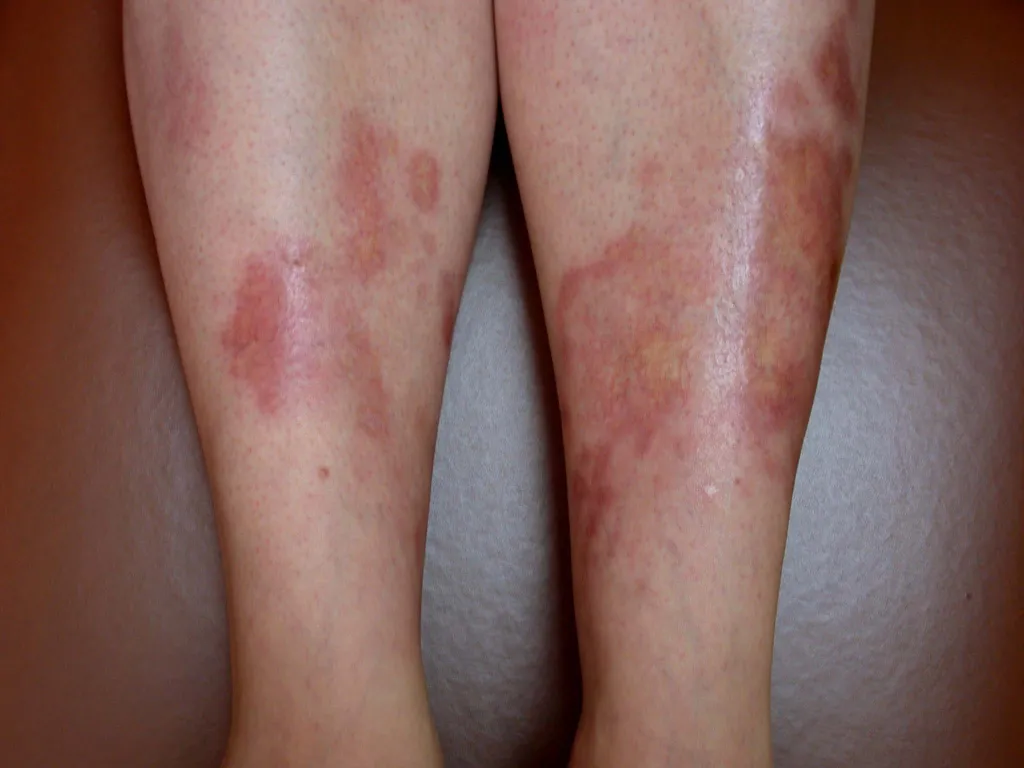
Signs of Necrobiosis Lipoidica Pictures
The observable signs of Necrobiosis Lipoidica are distinct and evolve through various phases, providing a clear visual narrative of the disease progression. These signs are crucial for clinical diagnosis and monitoring the efficacy of treatment. The characteristic features often seen in necrobiosis lipoidica photos include specific color patterns, textural changes, and the presence of associated vascular alterations.
Detailed signs that characterize Necrobiosis Lipoidica include:
- Well-Demarcated Borders: The plaques of Necrobiosis Lipoidica typically have distinct, often slightly raised, and sometimes erythematous or violaceous borders. These borders clearly separate the affected skin from the surrounding healthy tissue, making the lesions easily identifiable. This well-defined edge is a key `necrobiosis lipoidica plaque` sign.
- Central Yellowish Atrophy: The most pathognomonic sign is the central area of the plaque, which appears sunken (atrophic), shiny, and characteristically yellowish-brown. This atrophic skin necrobiosis lipoidica is a direct result of fat necrosis and collagen degradation in the dermis and subcutaneous tissue. The yellow hue is often described as waxy or porcelain-like.
- Telangiectasias (Visible Blood Vessels): Within the atrophic, translucent center of the lesion, fine, dilated blood vessels become readily apparent. These `telangiectasias necrobiosis lipoidica` are a consequence of epidermal thinning and dermal atrophy, allowing superficial capillaries to become visible. They contribute to the variegated appearance of the plaque.
- Epidermal Thinning and Fragility: The overlying epidermis in the atrophic center is significantly thinned, making the skin fragile and susceptible to breakdown. This fragility is a major factor contributing to ulceration and makes the skin very vulnerable to even minor trauma.
- Peripheral Erythema and Induration: The active, growing edge of the plaque is often characterized by a reddish (erythematous) or purplish (violaceous) hue, indicating ongoing inflammation. This peripheral area may also feel firm (indurated) to the touch due to granulomatous infiltration.
- Loss of Hair Follicles and Sweat Glands: Within the atrophic areas, there is often a noticeable reduction or complete loss of hair follicles and sweat glands. This contributes to the smooth, sometimes anhydrous (dry) appearance of the central lesion.
- Variable Size and Shape: Necrobiosis Lipoidica plaques can vary significantly in size, ranging from a few centimeters to extensive areas covering much of the lower leg. Their shape can be oval, round, irregular, or sometimes annular (ring-shaped) with central clearing.
- Absence of Epidermal Scaling: Unlike many eczematous or psoriasiform rashes, Necrobiosis Lipoidica typically does not exhibit significant scaling on its surface, especially in the central atrophic areas. While some dryness may occur, prominent flaking or silvery scales are generally absent.
- Chronic and Progressive Nature: The signs of Necrobiosis Lipoidica demonstrate its chronic and progressive nature. Lesions tend to expand slowly over time, and new lesions may appear. The atrophic changes and potential for ulceration signify a long-standing process.
- Predilection for Lower Extremities: Although rare, instances of Necrobiosis Lipoidica lesions appearing on areas other than the shins are documented. These atypical locations might include the forearms, scalp, face, or trunk. The appearance, however, maintains the core characteristics of atrophy and yellowish discoloration.
These specific necrobiosis lipoidica visual signs collectively paint a comprehensive picture of the condition, guiding clinicians toward an accurate diagnosis and appropriate management strategies for this challenging skin disorder.
Early Necrobiosis Lipoidica Photos
The early stages of Necrobiosis Lipoidica are crucial for prompt recognition, as intervention during this phase may help mitigate progression and reduce complications. Early Necrobiosis Lipoidica photos typically show subtle yet distinct changes that, while not always immediately alarming, possess characteristics that differentiate them from more common dermatological issues. Understanding these initial presentations is key for any thorough assessment of `necrobiosis lipoidica initial symptoms`.
Here’s a detailed breakdown of what to look for in the early phases:
- Small, Reddish Papules or Nodules: The very first visible signs of Necrobiosis Lipoidica often manifest as small, firm, raised lesions. These can be:
- Papules: Elevated, solid lesions less than 1 cm in diameter. They may feel slightly firm to the touch.
- Nodules: Larger, deeper, and firmer lesions, often extending into the dermis or subcutaneous tissue.
- The color is usually reddish, ranging from a light pinkish-red to a more saturated red or reddish-brown. This initial redness can sometimes be mistaken for an inflammatory reaction to a minor injury or insect bite. This is the `initial necrobiosis lipoidica lesion`.
- Slightly Raised and Indurated: Even at an early stage, the lesion may feel slightly firm or indurated (hardened) when palpated. The edges might be subtly elevated above the surrounding healthy skin. This firmness is due to early inflammatory infiltrates and granuloma formation.
- Discrete and Localized: Initially, lesions tend to be discrete and localized, rather than widespread. They may appear as a single papule or a cluster of a few small papules in close proximity, most commonly on the anterior lower legs.
- Asymptomatic or Mildly Pruritic/Tender: In the early stages, the lesions might be entirely asymptomatic, meaning the patient feels no pain, itching, or discomfort. However, some individuals may report mild itching (pruritus) or slight tenderness, especially if the lesion is inflamed or subjected to pressure.
- Gradual Expansion: A hallmark of early progression is the slow, insidious expansion of these initial papules. They gradually increase in size and may begin to coalesce with adjacent lesions, forming larger patches or plaques. This gradual spread is often over weeks to months, not days.
- Subtle Central Changes: As the lesion begins to expand, very subtle changes may start to appear in the center. The initial redness might begin to fade slightly, or a very faint yellowish tint might emerge. The skin may also start to appear a little shinier or smoother compared to the surrounding healthy skin, indicating very early `necrobiosis lipoidica skin changes`.
- Absence of Ulceration: Ulceration is extremely rare in the earliest stages of Necrobiosis Lipoidica. The skin is typically intact, although its underlying structure is undergoing changes. Ulcers are a feature of more advanced, atrophic disease.
- Often Misdiagnosed: Due to their relatively non-specific appearance, early Necrobiosis Lipoidica lesions are frequently misdiagnosed as other common dermatological conditions like granuloma annulare, insect bites, or even simple areas of trauma. This underscores the importance of a biopsy for definitive diagnosis if there is clinical suspicion.
Recognizing these nuanced features in early necrobiosis lipoidica pictures is critical for timely diagnosis. The presence of a persistent, reddish-brown, slightly raised and indurated papule or nodule, especially on the shins, that slowly expands and shows subtle central shininess or discoloration, should raise suspicion for this condition. Early detection allows for consideration of interventions aimed at controlling inflammation and preventing the more severe atrophic and ulcerative phases.
Skin rash Necrobiosis Lipoidica Images
While often described as plaques rather than a typical “rash,” the diverse cutaneous manifestations of Necrobiosis Lipoidica can indeed present a pattern that might initially be perceived as a persistent skin eruption. Exploring skin rash Necrobiosis Lipoidica images reveals a spectrum of presentations, from individual lesions to coalesced patches covering significant areas of the lower limbs. The key is to understand the unique characteristics that differentiate this specific “rash” from other inflammatory or infectious dermatoses.
Here are detailed aspects of the Necrobiosis Lipoidica “rash”:
- Erythematous to Yellow-Brown Patches: The primary characteristic of the `necrobiosis lipoidica rash` is the formation of patches that display a distinctive color transition.
- Peripheral Redness: The active, expanding edges of the patches are often reddish, purplish, or reddish-brown due to inflammatory cell infiltration and vascular changes. This is often the initial appearance before central changes set in.
- Central Yellowing: As the rash matures, the center of the patches develops a classic yellowish, waxy, or translucent appearance, characteristic of lipid deposition and necrobiosis. This is highly diagnostic and sets it apart from many other rashes.
- Shiny, Atrophic Skin: Within the central, yellowish areas of the rash, the skin becomes remarkably thin, shiny, and atrophic. This gives the appearance of stretched or glazed skin, through which underlying blood vessels (telangiectasias) are often visible. This atrophic skin necrobiosis lipoidica is a hallmark feature.
- Well-Demarcated Borders: The “rash” typically has clear, often slightly elevated, and sometimes undulating borders, sharply distinguishing the affected skin from the surrounding healthy tissue. These well-defined edges help in identifying the discrete nature of the lesions, even when they coalesce.
- Induration: The skin within and at the borders of the rash can feel firm or hardened (indurated) upon palpation, particularly in actively inflamed areas. This firmness is due to granulomatous tissue formation.
- Location Predominance: Overwhelmingly, the `necrobiosis lipoidica patches` are found on the anterior aspects of the lower legs, particularly the shins. While other locations can be affected (e.g., forearms, trunk), a `leg rash necrobiosis lipoidica` on the shins is the most common presentation. Bilateral involvement is common, though often asymmetrical.
- Absence of Scale or Vesicles: Unlike many common rashes (e.g., eczema, fungal infections), Necrobiosis Lipoidica typically does not present with significant scaling, crusting, or fluid-filled blisters (vesicles). The surface is usually smooth, especially in the atrophic areas.
- Fragility and Ulceration: A critical aspect of the Necrobiosis Lipoidica rash is the extreme fragility of the affected skin. Minor trauma can easily lead to the development of painful, chronic ulcers within the atrophic areas. These ulcers can be shallow or deep and are a significant complication. The development of ulcers completely changes the visual appearance of the `skin rash necrobiosis lipoidica images`.
- Variable Morphology: The “rash” can vary in its specific morphology:
- Single Plaque: A solitary, well-defined plaque.
- Multiple Plaques: Several distinct plaques scattered across the shins.
- Confluent Patches: Multiple plaques that have expanded and merged to form larger, irregular patches, sometimes covering extensive areas.
- Annular or Serpiginous: Occasionally, the lesions may form ring-shaped (annular) or snake-like (serpiginous) patterns, with central clearing and active borders.
- Slow Progression: The development and expansion of this “rash” are typically slow and chronic, evolving over months to years rather than rapidly appearing and resolving like acute rashes. This chronic nature is an important diagnostic clue for necrobiosis lipoidica images.
- Associated Symptoms: While the primary focus is on visual appearance, it’s important to note that the rash can be associated with symptoms such as itching, burning, tenderness, or pain, particularly when inflammation is active or ulcers are present.
The distinctive combination of peripheral erythema, central yellowish atrophy, shininess, telangiectasias, and extreme fragility makes the skin rash of Necrobiosis Lipoidica visually unique. Careful observation of these features in various presentations is essential for accurate diagnosis and for guiding treatment strategies for this often challenging chronic skin condition.
Necrobiosis Lipoidica Treatment
While Necrobiosis Lipoidica has no definitive cure, management focuses on symptom control, preventing disease progression, reducing inflammation, promoting healing of ulcers, and improving the cosmetic appearance of the lesions. Understanding the available Necrobiosis Lipoidica treatment options is critical for improving patient quality of life and preventing complications. Treatment strategies are often multi-faceted and tailored to the individual patient’s disease severity and progression, particularly focusing on the `managing necrobiosis lipoidica` aspects.
Here are the common therapeutic approaches for Necrobiosis Lipoidica:
- Topical Corticosteroids:
- Mechanism: Potent topical corticosteroids are a first-line treatment, aiming to reduce inflammation, especially at the active, erythematous borders of the lesions. They can help flatten raised areas and prevent further expansion.
- Application: Applied directly to the skin, sometimes under occlusion (e.g., with plastic wrap) to enhance penetration.
- Goals: To control the inflammatory phase, reduce redness, and potentially slow down lesion progression. However, prolonged use on atrophic skin must be carefully monitored due to the risk of further skin thinning.
- Intralesional Corticosteroids:
- Mechanism: Injections of corticosteroids directly into the active, raised borders of the plaques can deliver a high concentration of anti-inflammatory medication locally, minimizing systemic side effects.
- Application: Performed by a dermatologist, these injections target specific areas of inflammation.
- Goals: Highly effective for localized, inflamed plaques, helping to flatten them and reduce erythema, thus improving the visual appearance.
- Systemic Corticosteroids:
- Mechanism: Oral corticosteroids (e.g., prednisone) are potent anti-inflammatory agents used for widespread, rapidly progressing, or severely inflamed lesions that are unresponsive to topical or intralesional therapy.
- Considerations: Used with caution due to systemic side effects and typically for short durations to control acute flares.
- Goals: To bring systemic inflammation under control, especially in severe cases, as a bridge to other therapies or for significant symptom relief.
- Wound Care for Ulcerations:
- Critical Importance: Ulceration is a major complication and requires diligent `necrobiosis lipoidica ulcer care`. This involves protecting the wound, preventing infection, and promoting healing.
- Methods:
- Non-Adherent Dressings: To protect the fragile wound bed.
- Moist Wound Healing Principles: Using hydrocolloids, foams, or alginates to maintain a moist environment conducive to healing.
- Debridement: Removal of necrotic tissue to facilitate healing.
- Antibiotics: For secondary bacterial infections, either topical or systemic.
- Compression Therapy: To manage edema, if present, which can impede healing.
- Goals: To prevent infection, reduce pain, and facilitate re-epithelialization of the ulcer. This is crucial for both functional and cosmetic outcomes.
- Immunomodulators/Immunosuppressants:
- Topical Calcineurin Inhibitors (e.g., tacrolimus, pimecrolimus): Can be used as a steroid-sparing option, particularly for inflammatory lesions, reducing redness and inflammation without the risk of skin atrophy associated with long-term steroid use.
- Systemic Agents (e.g., cyclosporine, mycophenolate mofetil, azathioprine): Reserved for severe, recalcitrant cases or rapidly progressing disease. These agents suppress the immune response that drives the inflammation.
- Biologic Agents: Emerging therapies, such as TNF-alpha inhibitors, have shown promise in some severe cases, targeting specific inflammatory pathways.
- Goals: To modulate the immune response, reduce chronic inflammation, and prevent disease progression in cases not responding to conventional therapies.
- Phototherapy (PUVA, UVB):
- Mechanism: Exposure to specific wavelengths of ultraviolet light (UVA with psoralen, or narrowband UVB) can have immunomodulatory effects on the skin, reducing inflammation and potentially inducing repigmentation.
- Application: Administered in a clinical setting under medical supervision.
- Goals: To control inflammation, reduce lesion activity, and potentially improve the appearance of discolored areas, although results are variable.
- Anti-platelet Aggregation Agents (e.g., aspirin, dipyridamole):
- Rationale: Necrobiosis Lipoidica is thought to involve microangiopathy (small blood vessel disease). These agents may improve blood flow and oxygenation to the affected tissues.
- Usage: Sometimes considered as an adjunctive therapy, particularly if there’s evidence of vascular compromise.
- Goals: To improve vascular supply and potentially prevent ulceration or promote healing.
- Laser Therapy:
- Types: Pulsed dye laser (PDL) for telangiectasias, fractional lasers for texture improvement.
- Goals: Primarily cosmetic, to reduce the appearance of visible blood vessels (telangiectasias) and improve skin texture in atrophic areas, which can significantly enhance the `necrobiosis lipoidica cosmetic improvement`.
- Diabetes Control:
- Crucial Link: Given the strong association with diabetes, meticulous control of blood glucose levels is paramount.
- Impact: Poor glycemic control can exacerbate Necrobiosis Lipoidica and impair wound healing, especially for ulcers.
- Goals: To stabilize existing lesions, prevent new ones, and optimize healing conditions by managing the underlying metabolic disorder.
- Surgical Excision:
- Limited Role: Generally discouraged for active, inflammatory plaques due to the risk of poor wound healing and recurrence in the surgical scar.
- Indications: May be considered for very small, stable, non-inflamed lesions, or for chronic, non-healing ulcers that are not responding to conventional wound care, sometimes with skin grafting.
- Goals: To remove problematic lesions or to close chronic ulcers, but recurrence risk is high.
In summary, the necrobiosis lipoidica treatment strategy is individualized, often requiring a combination of approaches. Regular follow-up with a dermatologist is essential to monitor disease activity, adjust treatments, and manage any complications, particularly ulceration, thereby striving for the best possible outcomes in `managing necrobiosis lipoidica lesions`.