Exploring genital herpes symptoms pictures can provide crucial visual understanding of this common viral infection. This comprehensive guide will detail the various manifestations, from initial discomfort to the characteristic skin lesions, aiding in recognizing the diverse array of presentations associated with genital herpes outbreaks.
Genital herpes Symptoms Pictures
Understanding the visual progression of genital herpes symptoms is vital for early identification and management. The primary infection, often the most severe, typically manifests with a distinct set of symptoms that evolve over several days or weeks. Initially, individuals may notice a localized tingling, itching, or burning sensation in the genital or anal area, often preceding any visible skin changes. This prodromal phase serves as an important early warning sign of an impending outbreak. Following this, small, red bumps, known as papules, begin to emerge on the skin. These papules are typically firm to the touch and can be distributed in clusters or spread across a wider area depending on the initial site of infection and nerve distribution.
These papules rapidly develop into fluid-filled blisters, or vesicles, which are the hallmark of genital herpes photos. The vesicles are usually small, ranging from pinpoint size to a few millimeters in diameter, and are often grouped together on a red, inflamed base. The fluid inside these blisters is clear or slightly yellowish and contains a high concentration of the herpes simplex virus (HSV). The location of these vesicles can vary widely, including the penis, scrotum, labia, vagina, perineum, buttocks, anus, and inner thighs. In some cases, blisters may also appear on the cervix in women. These lesions are typically painful, tender to the touch, and can cause significant discomfort, especially when in contact with clothing or during urination.
Within a few days, these delicate vesicles rupture, leaving behind shallow, open sores or ulcers. These genital herpes ulcers are typically red at the base and can be intensely painful. The exposed nerve endings make these ulcers highly sensitive to touch, friction, and even air. Multiple ulcers may coalesce to form larger, more irregular lesions. The weeping from these ulcers can lead to a crusting phase as the fluid dries, forming scabs. The scabs are usually yellowish or brownish. As healing progresses, the scabs will eventually fall off, revealing new skin underneath. It is important to note that even after the scabs have fallen off, the area may remain sensitive for some time. The entire cycle from initial prodromal symptoms to complete healing can take anywhere from two to four weeks during a primary infection, although recurrent outbreaks usually resolve much faster.
Beyond the visible lesions, primary genital herpes symptoms often include systemic manifestations due to the body’s initial immune response to the virus. These can be quite debilitating and contribute to significant overall discomfort. Common systemic symptoms include:
- Fever: A generalized increase in body temperature, often accompanied by chills and malaise.
- Headache: A dull or throbbing pain, which can range from mild to severe.
- Muscle aches (myalgia): Generalized body pain, similar to flu-like symptoms.
- Fatigue: Profound tiredness and lack of energy, making daily activities challenging.
- Swollen and tender lymph nodes: Lymphadenopathy, particularly in the groin area (inguinal lymph nodes), as the body fights the infection. These nodes may become noticeably enlarged and painful to touch.
- Dysuria: Pain or difficulty during urination, especially if lesions are near the urethra or inside the urethra itself.
- Vaginal or urethral discharge: An increase in discharge, which may be clear or cloudy, can also occur.
- Meningitis (aseptic): In rare, severe cases, especially with primary infections, HSV can cause inflammation of the meninges, leading to symptoms like stiff neck, severe headache, and photophobia.
The severity of these symptoms can vary widely among individuals, with some experiencing only mild discomfort and others facing significant pain and systemic illness. Recurrent outbreaks, while following a similar pattern of lesion development, are typically less severe, shorter in duration, and may not always present with systemic symptoms. Understanding these detailed visual and systemic cues is fundamental for accurate diagnosis and effective management of genital herpes outbreaks.
Signs of Genital herpes Pictures
Identifying the distinct signs of genital herpes through visual examination is crucial for diagnosis. The progression of lesions provides a clear narrative of the viral activity on the skin and mucous membranes. The initial presentation might be subtle, with areas of redness and mild swelling preceding any prominent lesions. These red patches, often accompanied by localized tenderness, are critical early indicators, even before the characteristic blistering begins. It is essential to look for these subtle changes, especially if a person reports prodromal sensations like itching or tingling.
As the infection progresses, the most definitive visual cues for genital herpes pictures are the vesicles. These small, clear, fluid-filled blisters, typically clustered on an erythematous (red) base, are highly characteristic. The appearance can be likened to a cluster of dewdrops on inflamed skin. These vesicles are fragile and often break easily due to friction, revealing the underlying raw skin. The fluid within the vesicles is infectious and contains high concentrations of the herpes simplex virus, making direct contact with these lesions a high-risk activity for transmission.
Once the vesicles rupture, they transform into shallow, painful ulcers. These genital herpes ulcers are typically round or oval with a red base and can sometimes have a yellowish or grayish exudate. The margins of the ulcers are often well-demarcated but can appear irregular if multiple ulcers coalesce. The intense pain associated with these open sores is a key clinical sign and often prompts individuals to seek medical attention. The location of these ulcers is highly indicative:
- On the penis: Commonly found on the glans, shaft, or foreskin.
- On the vulva: Affecting the labia majora, labia minora, clitoris, or vaginal opening.
- Perianal region: Around the anus, particularly common in individuals engaging in receptive anal intercourse, or due to autoinoculation.
- Buttocks and inner thighs: Lesions can extend to adjacent skin areas.
- Cervix and vagina: Often visible during gynecological examination, sometimes causing internal pain or discharge without external lesions.
- Urethra: Can lead to severe dysuria and sometimes urethral discharge.
After the ulceration phase, the lesions begin to heal by crusting over. A yellowish or brownish crust forms over the open sores as they dry. This protective layer indicates the beginning of the healing process. As the crusts fall off, the skin underneath gradually regenerates. While scarring is uncommon, temporary post-inflammatory hyperpigmentation (darkening of the skin) or hypopigmentation (lightening of the skin) can occur in the affected area, especially after a severe primary infection. These temporary color changes are important to distinguish from active lesions. The entire healing process during a recurrent outbreak is significantly faster than during a primary infection, often resolving within 7-10 days, with crusting appearing much earlier.
Beyond the primary visual signs, other observable symptoms contribute to the overall clinical picture of genital herpes. These include the presence of enlarged, tender inguinal lymph nodes, which are palpable in the groin area. This lymphadenopathy is the body’s immune response to the viral infection. Additionally, individuals may exhibit signs of general malaise, such as looking fatigued or appearing unwell, particularly during a primary outbreak. While these are not direct skin signs, they are crucial indicators that accompany the dermatological manifestations. Examining the patient’s gait might also reveal discomfort, as walking or sitting can be painful with extensive lesions in the perineal or perianal regions. All these visual and systemic signs collectively contribute to a comprehensive understanding of genital herpes symptoms pictures, aiding in accurate clinical assessment.
Early Genital herpes Photos
Recognizing early genital herpes photos is paramount for prompt diagnosis and intervention. The initial stages of a herpes outbreak, particularly during a primary infection, can sometimes be subtle or non-specific, making visual identification challenging without a trained eye. The very first indication, often preceding any visible skin change, is the prodromal phase. This typically involves localized sensations such as itching, tingling, burning, or a shooting pain in the area where the lesions will eventually appear. These symptoms can occur hours or even a day or two before any skin changes become visible. Understanding this pre-eruptive stage is crucial for individuals who experience recurrent outbreaks, as it provides a window for initiating antiviral therapy to potentially abort or significantly lessen the severity of the outbreak.
Following the prodromal symptoms, the skin begins to show its first visible signs. These are typically small, localized areas of redness and slight swelling, often described as an erythematous patch. Within this reddened area, tiny, firm, red bumps, known as papules, start to emerge. These papules are usually only a few millimeters in size and can be mistaken for other common skin conditions such as insect bites, folliculitis, or ingrown hairs. However, their tendency to appear in clusters and their rapid progression are key differentiating factors. These early genital herpes lesions develop quickly, often within hours of the initial redness.
The progression from papules to vesicles is rapid and is a definitive marker in early genital herpes photos. The red bumps soon become topped with small, clear or yellowish fluid-filled blisters (vesicles). These vesicles are typically grouped together on an inflamed, red base. They can appear like small, uniform pearls on the skin. The fluid inside these vesicles is highly infectious, teeming with herpes simplex virus particles. During this stage, the lesions are often quite painful and tender to the touch. The skin surrounding the vesicles may also appear swollen and inflamed, contributing to localized discomfort. For instance, in women, early lesions might appear on the labia minora or majora, presenting as a cluster of small, clear blisters. In men, they could be found on the shaft or glans of the penis, similarly as small, grouped vesicles.
It’s important to differentiate these early lesions from other conditions that might mimic them, emphasizing the need for professional medical evaluation. For example:
- Folliculitis: Presents as red bumps centered around hair follicles, often with a pustular head, usually less painful and not clustered in the same way.
- Candidiasis (yeast infection): Typically presents as widespread redness, itching, and sometimes small pustules, but not the characteristic grouped vesicles of herpes.
- Syphilis (chancre): A syphilitic chancre is usually a single, firm, painless ulcer with a clean base, a stark contrast to the multiple painful vesicles/ulcers of herpes.
- Genital warts (HPV): These are flesh-colored or brownish growths with a cauliflower-like appearance, distinctly different from fluid-filled blisters.
- Contact dermatitis: Can cause redness, itching, and sometimes small blisters, but typically covers a larger area and is associated with exposure to an irritant or allergen, without the typical prodromal symptoms and viral progression.
The early recognition of these grouped vesicles is critical because this is the phase where the viral load on the skin surface is highest, making transmission most likely. Furthermore, early initiation of antiviral medication during this vesicular stage can significantly reduce the duration and severity of the outbreak. Therefore, paying close attention to any new or unusual sensations and quickly examining the affected area for the development of small, clustered, fluid-filled blisters on a red base is key for anyone concerned about early genital herpes symptoms. The pain and discomfort experienced during this early stage are also significant, indicating active viral replication and nerve involvement.
Skin rash Genital herpes Images
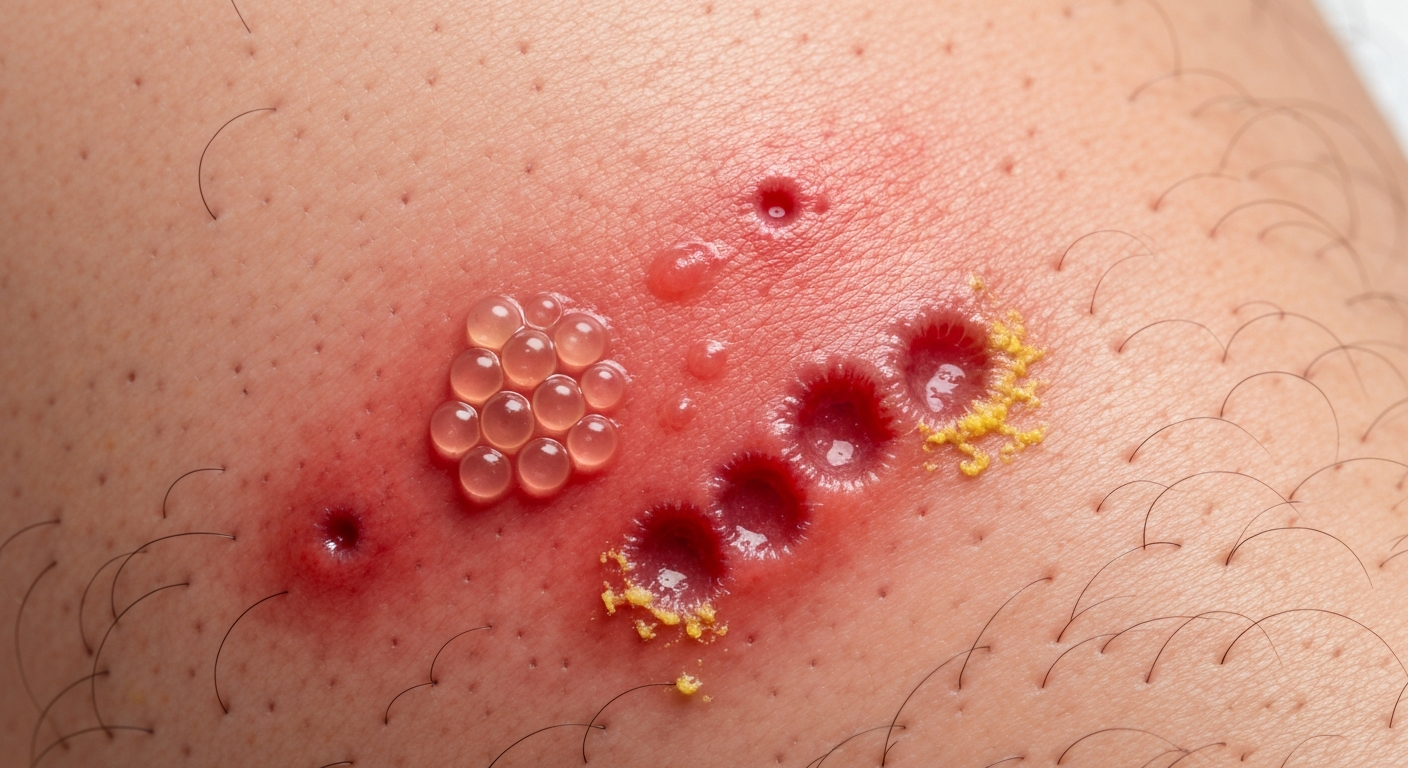
The skin rash of genital herpes presents a very characteristic pattern, making it visually distinct from many other dermatological conditions. The primary visual identifier is the eruption of clustered vesicles on an erythematous base. This “rash” is not diffuse or widespread like eczema, but rather localized to specific areas where the virus has reactivated along nerve pathways. The appearance progresses through several distinct stages, each providing unique visual cues for accurate identification in genital herpes images.
The initial manifestation of the herpes rash, following the prodromal phase, involves localized redness and swelling. This erythema can be intensely inflamed, marking the boundaries of the upcoming lesions. Within this reddened area, small, raised papules quickly form. These tiny bumps are often grouped closely together, creating a palpable texture on the skin. The speed at which these papules transition into fluid-filled vesicles is a key feature of the herpes rash. These vesicles, typically 1-3 mm in diameter, are fragile and contain clear or yellowish serous fluid. Their grouping, often described as a “cluster of grapes,” is highly characteristic and a significant diagnostic sign for genital herpes rash.
When these vesicles rupture, they give rise to painful, shallow ulcers. The open sores reveal a red, raw base, and their margins can be irregular if multiple vesicles have coalesced. The weeping nature of these ulcers, coupled with the exposed nerve endings, contributes to the intense pain and tenderness reported by patients. The location of the rash is consistently in the genital or perianal regions, including:
- Male Genitalia: Penis (glans, shaft, foreskin), scrotum, perineum.
- Female Genitalia: Labia majora, labia minora, clitoris, vaginal introitus, perineum, cervix (often only visible on examination).
- Anal/Perianal Area: Around the anus, buttocks, inner thighs.
- Inguinal Folds: Where the thigh meets the torso.
The progression to crusting is another defining aspect of the genital herpes skin rash. As the ulcers begin to heal, a yellowish-brown crust forms over the lesions. These scabs protect the regenerating skin underneath. Over time, these crusts dry and fall off, usually leaving no permanent scars, though temporary changes in skin pigmentation (lighter or darker spots) can occur. The resolution of the rash is usually complete within 2-4 weeks for a primary infection and 7-10 days for recurrent outbreaks.
Differentiating the herpes rash from other conditions is critical. Conditions that might resemble the herpes rash include:
- Zoster (Shingles): Caused by the varicella-zoster virus, it also presents with vesicular lesions on an erythematous base, but typically follows a dermatomal pattern (a band-like distribution along a single nerve path) and is extremely painful. Herpes rash is usually more localized and clustered without a strict dermatomal pattern.
- Contact Dermatitis: Can cause an itchy, red rash with vesicles, but is usually more diffuse, lacks prodromal symptoms, and has a clear exposure history to an irritant.
- Aphthous Ulcers: These are mouth sores (canker sores) but can sometimes be confused with genital herpes if they appear on mucous membranes. However, aphthous ulcers are not preceded by vesicles and do not typically cluster or recur with the same frequency or pattern as herpes.
- Behçet’s Disease: A rare inflammatory disorder that can cause recurrent genital ulcers, but these are usually larger, deeper, and often accompanied by oral ulcers and eye inflammation.
- Trauma or Friction Blisters: Can be painful but lack the prodromal symptoms, specific grouping pattern, and typical recurrence of herpes.
The distinctive visual characteristics of the lesion clusters, their rapid evolution from papules to vesicles to painful ulcers, and the eventual crusting, along with the consistent anatomical distribution, are the key features to look for in genital herpes images to ensure accurate diagnosis. The recurrent nature of the rash, often in the same location, further aids in identification for individuals with established infections.
Genital herpes Treatment
Effective genital herpes treatment primarily focuses on managing symptoms, accelerating healing, preventing outbreaks, and reducing the risk of transmission. There is currently no cure for herpes, meaning the virus remains dormant in nerve cells indefinitely. However, antiviral medications are highly effective in controlling the virus and significantly improving the quality of life for individuals living with genital herpes. These medications work by interfering with the virus’s ability to replicate, thereby reducing viral load and the severity and frequency of outbreaks.
The primary class of drugs used for genital herpes treatment are antiviral agents. These include:
- Acyclovir (Zovirax): This was the first antiviral specifically developed for herpes. It can be taken orally, intravenously, or topically. Oral acyclovir is commonly prescribed for both initial and recurrent outbreaks, as well as for suppressive therapy. Dosing varies based on the purpose of treatment (e.g., higher doses for initial outbreaks, lower daily doses for suppression).
- Valacyclovir (Valtrex): A prodrug of acyclovir, meaning it is converted to acyclovir in the body. It has improved bioavailability, allowing for less frequent dosing, which can enhance patient adherence. Valacyclovir is a popular choice for treating outbreaks and for daily suppressive therapy due to its convenience.
- Famciclovir (Famvir): A prodrug of penciclovir, similar in action to acyclovir and valacyclovir. Famciclovir also offers convenient dosing schedules and is effective for both episodic treatment and suppressive therapy.
These antiviral medications can be used in two main ways for genital herpes management:
- Episodic Treatment: This involves taking antiviral medication at the first sign of an outbreak (e.g., during the prodromal phase of tingling or itching, or as soon as lesions appear). The goal is to shorten the duration and severity of the outbreak. Starting treatment early is key for maximum effectiveness. For individuals who experience infrequent outbreaks, episodic therapy is a preferred approach.
- Suppressive Therapy: For individuals who experience frequent (e.g., more than six outbreaks per year) or severe recurrent outbreaks, daily suppressive antiviral therapy may be recommended. Taking a low dose of antiviral medication every day can significantly reduce the frequency of outbreaks (by 70-80% or more) and can also decrease the risk of transmitting the virus to partners. This can greatly improve the patient’s physical and psychological well-being.
Beyond antiviral medications, supportive care and adjunctive treatments play a crucial role in managing the symptoms and discomfort associated with genital herpes outbreaks. These measures focus on pain relief, preventing secondary infections, and promoting healing:
- Pain Management: Over-the-counter pain relievers such as ibuprofen, acetaminophen, or naproxen can help alleviate pain and discomfort. Topical anesthetics, such as lidocaine cream or gel, can provide localized relief when applied directly to the lesions.
- Hygiene: Keeping the affected area clean and dry is important to prevent secondary bacterial or fungal infections. Gentle washing with mild soap and water is recommended, followed by patting the area dry.
- Loose Clothing: Wearing loose-fitting cotton underwear and clothing can reduce friction and irritation to the lesions, promoting comfort and healing.
- Sitz Baths: Soaking in warm water (sitz bath) can help soothe painful lesions, especially those in the perianal or genital area, and can aid in cleaning the area.
- Ice Packs: Applying a cold compress or ice pack (wrapped in a cloth) to the affected area can help reduce swelling and numb the pain temporarily.
- Avoiding Irritants: During an outbreak, it is advisable to avoid scented soaps, douches, perfumed products, and tight clothing that can irritate the lesions.
- Stress Reduction: Stress is a known trigger for herpes outbreaks in some individuals. Practices like mindfulness, meditation, yoga, and ensuring adequate sleep can help manage stress levels.
Counseling and education are also integral components of genital herpes treatment. Providing accurate information about the virus, its transmission, and management strategies can empower individuals to manage their condition effectively and reduce associated stigma. Discussing safe sex practices, including consistent condom use and the role of suppressive therapy in reducing transmission risk (known as ‘treatment as prevention’), is vital for preventing the spread of the virus. Regular follow-up with a healthcare provider ensures that treatment plans remain appropriate and effective, especially as new research emerges regarding herpes simplex virus management.