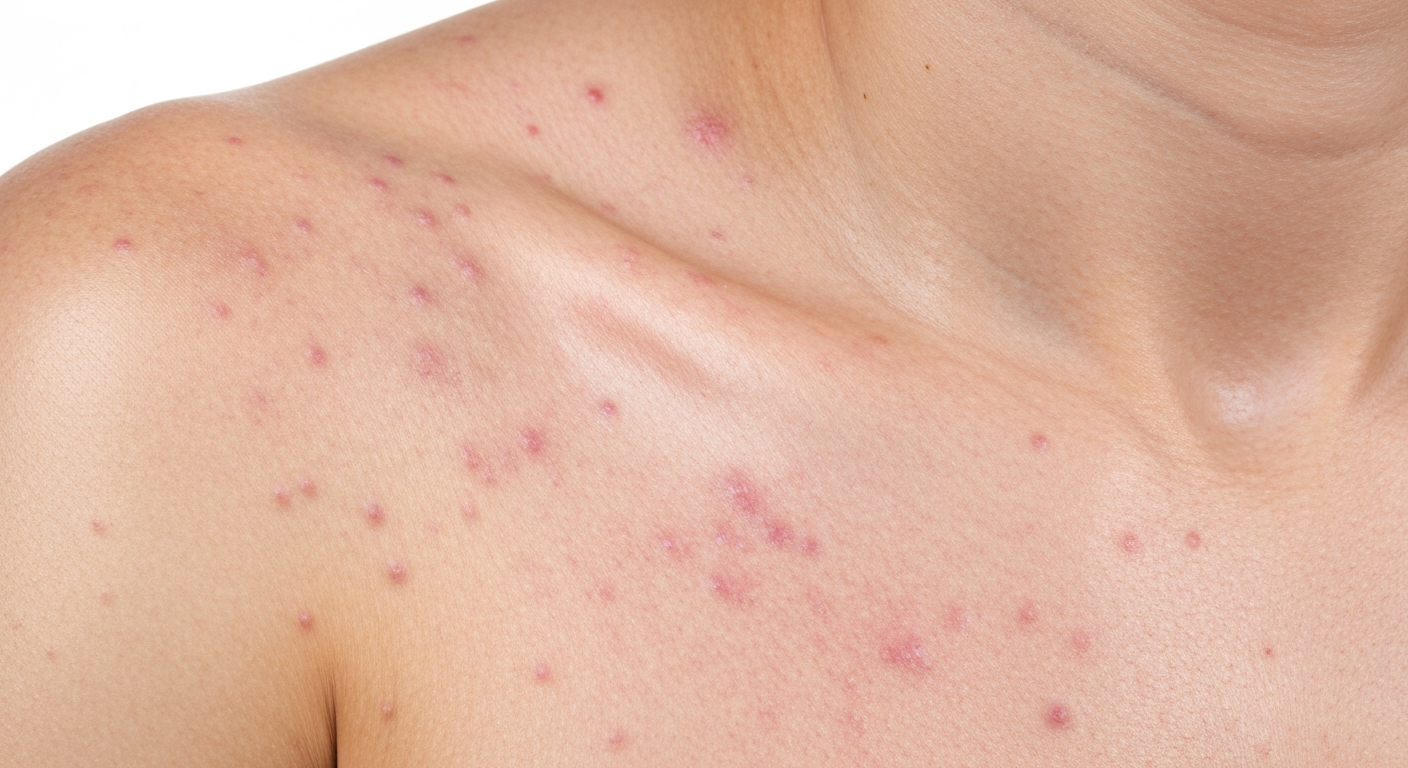
For those seeking to understand the visual presentation of this viral infection, our comprehensive guide provides detailed descriptions that complement Rubella symptoms pictures. Explore the characteristic rash and other diagnostic signs to aid in early recognition and management of Rubella.
Rubella Symptoms Pictures
Rubella, also widely known as German measles, presents with a distinct set of symptoms, many of which are visually identifiable and crucial for early diagnosis. When reviewing Rubella symptoms pictures, one typically observes a mild, often transient rash that is the hallmark of the infection. The rash, which is maculopapular in nature, tends to be lighter in color and less prominent than that of measles (rubeola), making careful observation essential. Visual documentation through Rubella pictures often highlights the generalized nature of the rash, starting on the face and spreading downwards to the trunk and extremities within a short period, usually 24 hours. Accompanying the rash, other tell-tale signs such as enlarged lymph nodes, particularly behind the ears (postauricular) and at the back of the neck (occipital), are frequently visible or palpable and are important diagnostic indicators. These palpable lymph nodes, often referred to as lymphadenopathy, contribute significantly to the overall clinical picture of Rubella. Fever, typically low-grade, may also be evident, though it is usually not a prominent feature in adults and children compared to more severe viral illnesses. Identifying these characteristic features in Rubella symptom images can significantly assist healthcare professionals and parents in understanding the progression and presentation of the disease.
Detailed observation of Rubella rash pictures reveals the evolution of the lesions. Initially, the rash consists of discrete, small, pinkish-red spots. Over time, particularly on the trunk, these spots may become more confluent, giving the skin a flushed or sandpaper-like appearance, although this is less common than in scarlet fever. The overall impression from pictures of Rubella symptoms is often one of a relatively benign rash, which typically fades within three days without pigmentation or desquamation (peeling). This transient nature is a key differentiating factor. Furthermore, careful scrutiny of Rubella infection pictures might also reveal subtle signs such as mild conjunctivitis (redness of the eyes) or a general malaise that precedes the rash. Understanding the full spectrum of these visual cues is paramount for accurate identification of Rubella, especially given its potential complications, particularly for pregnant individuals.
Key visual characteristics often captured in Rubella symptoms photos include:
- Maculopapular Rash: The primary visual symptom, appearing as flat (macular) or slightly raised (papular) pinkish-red spots. These lesions are typically small, ranging from 1 to 4 mm in diameter.
- Cephalocaudal Spread: The distinctive pattern where the rash begins on the face and neck, then rapidly spreads downwards to the trunk, arms, and legs within 24 hours.
- Transient Nature: The rash typically lasts for 1 to 3 days, fading quickly without leaving marks or peeling skin. This rapid resolution is a critical visual sign.
- Lymphadenopathy: Swollen and tender lymph nodes, most notably in the postauricular (behind the ears), occipital (back of the head), and posterior cervical (back of the neck) regions. These swellings are often palpable and sometimes visible in profile.
- Mild Conjunctivitis: A subtle reddening of the whites of the eyes (sclera) may be present, indicating inflammation of the conjunctiva.
- Faintness of Rash: Compared to measles, the Rubella rash is often described as lighter, less vibrant, and more dispersed, making it less striking in some visuals of Rubella.
- Absence of Koplik’s Spots: Unlike measles, Rubella does not feature the characteristic Koplik’s spots on the buccal mucosa, which is an important negative visual sign.
The overall presentation in Rubella disease images highlights the milder nature of the infection in many cases, though the potential for severe complications, especially in specific populations, underscores the importance of vaccination and accurate diagnosis. Visual aids are invaluable in distinguishing Rubella from other exanthematous illnesses, such as roseola, scarlet fever, or parvovirus B19 infection, all of which can present with similar skin manifestations.
Signs of Rubella Pictures
Delving deeper into the observable signs of Rubella, beyond just the rash, can provide a more comprehensive understanding when examining signs of Rubella pictures. These images often capture the subtle yet diagnostic cues that accompany the infection. One of the most consistent and diagnostically significant signs, frequently observed even before or concurrently with the rash, is generalized lymphadenopathy. Pictures showing Rubella signs will often feature individuals with noticeable swelling in specific lymph node areas. The postauricular (behind the ears) and occipital (at the base of the skull, back of the neck) lymph nodes are almost invariably enlarged, firm, and often tender to the touch. These can sometimes be visibly swollen, particularly in children with thinner necks, and their prominence in Rubella clinical photos is a key diagnostic feature of German measles.
Another important sign, though not always visually striking in typical photographs unless specifically highlighted, is the presence of Forchheimer spots. These are small, pinpoint red lesions or petechiae that can be seen on the soft palate. While not unique to Rubella, their presence in conjunction with other symptoms strongly supports a diagnosis. When viewing Rubella oral cavity pictures, these ephemeral spots might be glimpsed, often appearing just before or concurrent with the cutaneous rash. Additionally, mild inflammation of the eyes, known as conjunctivitis, often presents as a subtle reddening of the conjunctiva. This ocular sign, while not always the focus of general Rubella symptom images, can be an important contributing factor to the overall clinical picture, and sometimes captured in close-up facial shots.
Beyond external visual signs, patients infected with Rubella often exhibit systemic symptoms that, while not directly captured in still images, contribute to the ‘picture’ of the illness. These include a low-grade fever, typically below 38.5°C (101.3°F), and general malaise. In adolescents and adults, especially women, arthralgia (joint pain) or even frank arthritis (joint inflammation) can be a prominent symptom, affecting the small joints of the hands, wrists, and knees. Although not a direct visual sign on the skin, a person demonstrating discomfort or guarding of joints in patient Rubella images could indirectly suggest this symptom. The combination of these specific signs – the characteristic rash, distinctive lymphadenopathy, and other systemic findings – creates a unique clinical pattern for Rubella, making careful observation of all available Rubella diagnostic images crucial.
Key observable signs of Rubella often highlighted in clinical photography include:
- Postauricular Lymphadenopathy: Swollen and tender lymph nodes located directly behind the ears. This is one of the most reliable and early signs of Rubella infection. In some Rubella patient images, this swelling can be visibly apparent, causing a slight protrusion.
- Occipital Lymphadenopathy: Enlargement of lymph nodes at the base of the skull, often felt or seen as subtle bumps in the posterior neck region. This is highly characteristic of German measles.
- Posterior Cervical Lymphadenopathy: Swollen lymph nodes along the back of the neck. These, along with postauricular and occipital nodes, are part of the generalized lymphadenopathy often associated with Rubella.
- Forchheimer Spots: Small, red petechial spots observed on the soft palate. These are transient and can be difficult to capture in general Rubella symptom photos but are a specific mucosal finding. They typically appear before or with the rash.
- Mild Conjunctivitis: Redness and irritation of the conjunctiva, often subtle. Close-up facial Rubella images might show slightly bloodshot eyes.
- Exanthematous Rash: As detailed previously, the maculopapular rash itself is a primary sign, distinguished by its pink color, fine texture, and characteristic cephalocaudal spread. Its transient nature is also a key visual indicator in sequential Rubella rash progression pictures.
- Malaise and Low-Grade Fever: While not directly visual, a patient’s overall appearance of mild illness and flushed cheeks from a fever can be indirectly inferred from general Rubella patient photographs.
The constellation of these signs helps healthcare providers confirm a suspected Rubella diagnosis, especially in the absence of laboratory testing, relying heavily on the careful interpretation of visual Rubella presentations. The absence of more severe symptoms typical of other viral exanthems, such as high fever or profound prostration, further refines the diagnostic accuracy when reviewing Rubella signs and symptoms images.
Early Rubella Photos
Understanding what to look for in early Rubella photos is crucial for timely identification, particularly as the initial symptoms can be subtle or mistaken for other common childhood illnesses. The incubation period for Rubella typically ranges from 12 to 23 days, and the prodromal phase, which precedes the characteristic rash, often lasts for 1 to 5 days. During this prodromal phase, early Rubella pictures might capture non-specific symptoms such as low-grade fever, malaise, and mild upper respiratory symptoms like a runny nose or sore throat. These are often difficult to differentiate from common colds without the context of impending rash or known exposure.
The most distinctive feature in early Rubella photos, marking the transition from the prodromal phase to the acute phase, is the onset of the maculopapular rash. This rash typically first appears on the face, often around the hairline and behind the ears, before spreading rapidly. First appearance of Rubella rash photos will show small, discrete, pinkish-red spots that are generally non-itchy or only mildly pruritic. These initial lesions are macular (flat) but can sometimes have a slightly raised, papular component. The rapid progression of this rash from the face downwards is a hallmark of Rubella, and sequential Rubella rash progression images would beautifully illustrate this cephalocaudal spread.
Another key indicator visible in early stages of Rubella pictures is the onset of lymphadenopathy. Enlarged postauricular and occipital lymph nodes often become palpable, and sometimes subtly visible, before the rash fully erupts. Early Rubella lymph node pictures might show slight swelling or tenderness in these areas, even when the rash is just beginning to manifest or is very faint. This early lymphadenopathy is often considered a more reliable early sign than the rash itself, especially given the variable presentation of the rash. For adolescents and adults, especially women, early symptoms can also include arthralgia (joint pain) or stiffness, which, while not visually captured in photos of skin symptoms, might be inferred from body language in early Rubella patient portraits showing discomfort or limited movement.
The mildness of these early symptoms in some individuals can lead to asymptomatic or very mild infections, especially in young children, making identification solely based on early Rubella photos challenging without additional clinical context. However, for those exhibiting clearer signs, the combination of mild fever, distinctive lymph node swelling, and the initial facial rash forms a characteristic pattern. It is critical for healthcare providers to be aware of these subtle early presentations to prevent further spread and protect vulnerable populations, particularly pregnant women at risk of Congenital Rubella Syndrome.
Key features to look for in early Rubella photos include:
- Initial Facial Rash: The very first visible sign of the rash typically appears on the face, often around the forehead, hairline, and behind the ears. These are usually discrete, faint, pink macules.
- Early Lymph Node Swelling: Noticeable swelling or prominence of the lymph nodes behind the ears (postauricular) and at the back of the head (occipital). These may appear slightly enlarged or cause a subtle change in the contour of the neck and head in profile Rubella pictures.
- Mild Conjunctivitis: A slight redness or irritation of the eyes may be visible in close-up early facial Rubella images.
- Subtle Body Language: While not a direct visual sign of the rash, a child or adult in early Rubella photographs might appear slightly unwell, irritable, or have a flushed appearance consistent with low-grade fever or general malaise.
- Prodromal Symptoms (indirectly): Although not directly pictured, the history accompanying early Rubella photos would often include reports of mild fever, sore throat, or runny nose preceding the rash onset.
- Absence of Significant Distress: Unlike more severe exanthems, individuals in early Rubella pictures typically do not appear to be in significant distress, reinforcing the often mild nature of the initial infection.
Careful attention to these early visual cues, combined with clinical history and epidemiological context, is vital for diagnosing Rubella. The information gleaned from early Rubella symptom pictures aids in understanding the disease progression and in differentiating it from other viral rashes that might present similarly in their nascent stages.
Skin rash Rubella Images
The skin rash of Rubella is arguably the most recognizable and frequently photographed symptom of the infection, making skin rash Rubella images an invaluable resource for visual diagnosis. This maculopapular rash is characterized by its distinct appearance, distribution, and transient nature, setting it apart from other viral exanthems. Upon examining Rubella rash pictures, one typically observes small, flat (macular) or slightly raised (papular) lesions that are pink or light red in color. The size of these lesions usually ranges from 1 to 4 mm, and they are initially discrete, meaning they do not merge together.
The evolution and spread of the Rubella skin rash are highly characteristic. It generally begins on the face, often around the forehead and behind the ears, within 1 to 5 days after the onset of prodromal symptoms. Facial Rubella rash images will clearly show this initial presentation. Within 24 hours of its facial onset, the rash rapidly spreads downwards, affecting the trunk, arms, and legs in a cephalocaudal progression. This rapid full-body spread, captured in sequential full-body Rubella rash photos, is a key diagnostic feature. On the trunk, the individual lesions may become more confluent, giving a more generalized flushed appearance, though this is often less pronounced and widespread than in measles.
A critical characteristic evident in Rubella rash visuals is its short duration. The rash typically fades within 1 to 3 days, disappearing in the same order it appeared, often leaving no residual pigmentation or desquamation (peeling). This rapid resolution is a strong indicator of Rubella and helps differentiate it from conditions like measles, where the rash is darker, more confluent, and lasts longer, sometimes with subsequent desquamation. The overall impression from Rubella skin rash pictures is often one of a relatively faint or “washed out” rash compared to the vibrant, blotchy rash of measles. This subtlety requires careful observation, especially in individuals with darker skin tones where the pinkish-red hue might be less obvious, requiring palpation to detect the papular component or textural changes.
In some cases, particularly in older children and adults, the rash may be more prominent, but typically it remains less severe than other viral rashes. The absence of intense itching is also a common feature, though mild pruritus can occur. The presence of generalized lymphadenopathy, especially affecting the postauricular and occipital nodes, consistently accompanies the Rubella rash, and careful examination of Rubella images should look for these concurrent signs. The visual pattern of the Rubella rash, combined with the context of other symptoms and epidemiological factors, forms the cornerstone of clinical diagnosis.
Detailed characteristics of the Rubella skin rash as seen in images:
- Appearance: Maculopapular, consisting of small (1-4 mm), flat or slightly raised, pink to light red spots. The color is often described as “rose-pink.”
- Distribution: Starts on the face (forehead, hairline, behind ears) and rapidly spreads to the trunk, arms, and legs within 24 hours. This cephalocaudal spread is highly characteristic in Rubella rash patterns.
- Confluence: While initially discrete, lesions on the trunk may become confluent, giving a more uniform reddish appearance in some Rubella body rash pictures, but usually less intensely so than in measles.
- Duration: Typically lasts 1 to 3 days, fading quickly without leaving any skin discoloration or peeling. Sequential Rubella rash fading images would show this rapid resolution.
- Texture: Can feel slightly rough, described sometimes as a “sandpaper” texture, particularly when the papular component is more pronounced.
- Itchiness: Usually non-itchy or only mildly pruritic, unlike conditions such as chickenpox or eczema.
- Faintness: Often appears fainter and less prominent than the rash of measles (rubeola), sometimes described as “washed out” in comparison. This subtlety is important in distinguishing Rubella pictures from those of measles.
- Absence of Pigmentation/Desquamation: The skin returns to its normal appearance once the rash resolves, without any residual staining or peeling, which can be observed in post-rash Rubella skin images.
- Associated Lymphadenopathy: Often accompanied by visible or palpable enlargement of postauricular and occipital lymph nodes, reinforcing the diagnosis alongside the rash.
The meticulous examination of skin rash Rubella images provides invaluable insights into the typical presentation of this exanthematous disease, aiding both in education and clinical recognition. Understanding these visual nuances is paramount for distinguishing Rubella from other similar conditions and for appropriate public health interventions.
Rubella Treatment
While Rubella symptoms pictures and diagnostic signs are crucial for identification, understanding the appropriate treatment and management strategies is equally important. It is vital to state upfront that there is no specific antiviral treatment for Rubella virus infection. The infection is generally self-limiting in otherwise healthy individuals, and management primarily focuses on supportive care and symptomatic relief. However, the most critical aspect of Rubella management lies in prevention through vaccination, particularly to protect vulnerable populations from the severe consequences of Congenital Rubella Syndrome (CRS).
Supportive Care for Rubella:
For individuals presenting with classic Rubella symptoms, including the characteristic rash, lymphadenopathy, and low-grade fever, the treatment approach is largely supportive. The aim is to alleviate discomfort until the immune system clears the virus. Key aspects of supportive care include:
- Rest: Encouraging adequate rest can help the body recover more effectively, especially during the febrile and symptomatic phases.
- Hydration: Maintaining good hydration is important, particularly if there is a low-grade fever. Oral fluids such as water, clear broths, and electrolyte solutions are recommended.
- Antipyretics and Analgesics: Over-the-counter medications can be used to manage fever and pain.
- Acetaminophen (Paracetamol): Effective for reducing fever and alleviating general aches and pains.
- Nonsteroidal Anti-inflammatory Drugs (NSAIDs) like Ibuprofen: Can help reduce fever, pain, and inflammation, particularly useful for arthralgia (joint pain) or arthritis, which can be prominent in adolescents and adults, especially women.
It is important to avoid aspirin in children and adolescents due to the risk of Reye’s syndrome.
- Isolation: To prevent further transmission, individuals with Rubella should avoid contact with non-immune individuals, especially pregnant women. They are typically considered contagious from 7 days before to 7 days after the rash appears.
- Topical Treatments for Itching (if present): While the Rubella rash is typically not intensely itchy, if mild pruritus occurs, over-the-counter anti-itch creams containing hydrocortisone or oral antihistamines can provide relief.
- Eye Care: If mild conjunctivitis is present, warm compresses can soothe the eyes. Avoiding eye strain may also be beneficial.
Management of Specific Symptoms:
While Rubella is often mild, some symptoms might require more focused attention:
- Arthritis/Arthralgia: Joint pain or inflammation is more common in adult women. Treatment involves rest, application of warm or cold packs, and the use of NSAIDs. In rare cases of severe or persistent arthritis, rheumatology consultation might be considered, though symptoms usually resolve completely within a few weeks.
- Neurological Complications: Extremely rare complications like encephalitis or post-infectious encephalopathy are medical emergencies. Management would involve intensive supportive care in a hospital setting, tailored to the specific neurological manifestations.
- Hemorrhagic Complications: Very rarely, Rubella can lead to thrombocytopenic purpura, which might manifest as petechiae or bruising. Management would involve close monitoring and, in severe cases, treatment with corticosteroids or intravenous immunoglobulin (IVIG).
Prevention: The Cornerstone of Rubella Control:
The most effective strategy against Rubella is prevention through vaccination. The Measles, Mumps, and Rubella (MMR) vaccine is a live attenuated vaccine that provides highly effective and long-lasting immunity against Rubella. Global vaccination programs have dramatically reduced the incidence of Rubella and, more importantly, Congenital Rubella Syndrome (CRS).
- MMR Vaccine Schedule:
- First Dose: Typically administered at 12 to 15 months of age.
- Second Dose: Usually given at 4 to 6 years of age, before school entry.
Catch-up vaccination is recommended for non-immune individuals, especially women of childbearing age, to prevent potential infection during pregnancy.
- Targeting Pregnant Women: Screening for Rubella immunity (serology for IgG antibodies) is a routine part of prenatal care. Women found to be non-immune should be advised to get vaccinated postpartum, to protect future pregnancies. Vaccination during pregnancy is contraindicated due to the theoretical risk (though never confirmed) to the fetus from the live attenuated vaccine.
- Congenital Rubella Syndrome (CRS) Prevention: The primary goal of Rubella vaccination programs is to eliminate CRS, which occurs when a pregnant person contracts Rubella, especially during the first trimester. The virus can cross the placenta, leading to severe and often permanent birth defects in the developing fetus.
Management of Congenital Rubella Syndrome (CRS):
For infants born with CRS, treatment is entirely supportive and focuses on managing the various birth defects caused by the infection. There is no specific treatment to reverse the damage caused by the virus during fetal development. The manifestations of CRS can be wide-ranging and include:
- Ocular Defects: Cataracts, glaucoma, retinopathy, microphthalmia. Surgical correction may be necessary for cataracts.
- Cardiac Defects: Patent ductus arteriosus, pulmonary artery stenosis. Surgical intervention may be required for severe cardiac anomalies.
- Auditory Defects: Sensorineural hearing loss. Hearing aids and other supportive measures are used.
- Neurological Defects: Microcephaly, developmental delay, intellectual disability. Early intervention programs and special education are crucial.
- Other Manifestations: Growth retardation, hepatosplenomegaly, thrombocytopenia (often seen in pictures of neonates with CRS as purpuric rash or “blueberry muffin” lesions), bone lesions. Management is symptom-specific.
Children with CRS often require lifelong multidisciplinary care involving pediatricians, ophthalmologists, cardiologists, audiologists, neurologists, and developmental specialists. Early identification of these defects and appropriate interventions can significantly improve the quality of life for affected individuals. The immense burden of CRS underscores the paramount importance of universal Rubella vaccination.
In conclusion, while Rubella infection itself in healthy individuals typically requires only symptomatic and supportive care due to its mild, self-limiting nature, the focus of medical and public health efforts is heavily placed on prevention through vaccination. The consequences of Rubella, particularly for an unborn child, are severe and largely preventable. Therefore, public health campaigns emphasizing the MMR vaccine and maintaining high vaccination rates are the most effective forms of “treatment” against the devastating impact of Rubella.