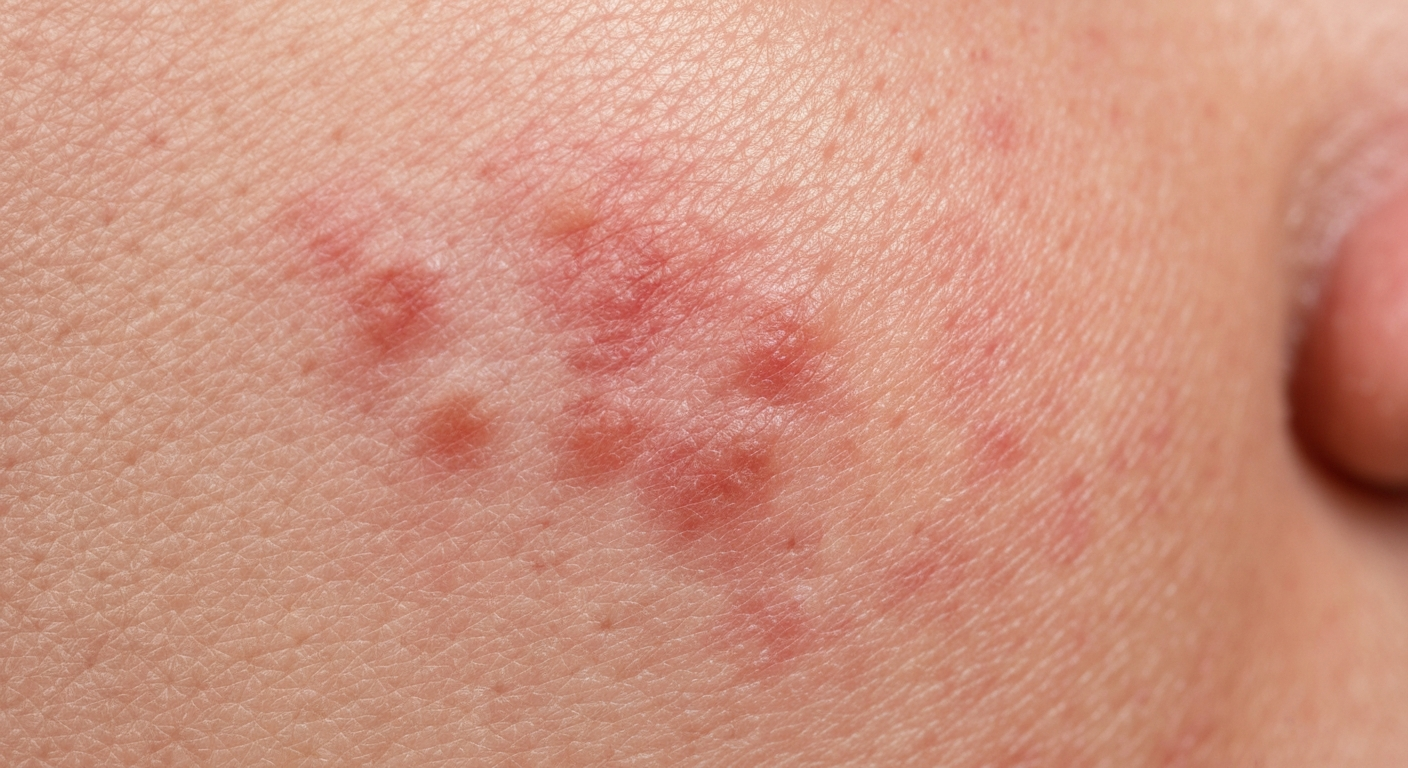
What does Solar Lentigo look like symptoms pictures reveal distinct, often uniform patches of hyperpigmentation on sun-exposed skin. These common skin lesions, widely known as age spots or sun spots, are a clear indicator of chronic ultraviolet radiation exposure, presenting specific visual characteristics that aid in their identification.
Solar Lentigo Symptoms Pictures
Solar lentigines, commonly referred to as age spots or sun spots, are characteristic signs of chronic sun exposure and photoaging. What does Solar Lentigo look like symptoms pictures often display as well-demarcated, flat patches of skin discoloration. These lesions are typically uniform in color, ranging from light brown to dark brown, or occasionally black. Their shape is usually round or oval, but can also be irregular. The size of individual solar lentigo lesions can vary significantly, from a few millimeters to several centimeters in diameter, and they tend to enlarge over time with continued sun exposure. The surface texture of a solar lentigo is smooth, similar to the surrounding skin, meaning it is neither raised nor scaly, which helps differentiate it from other skin conditions like seborrheic keratoses or actinic keratoses. There is typically no associated pain, itching, or tenderness with solar lentigo, making their primary symptom a cosmetic concern related to their visible presence on the skin. These hyperpigmented macules are most prevalent on areas of the body that receive the most intense and prolonged sun exposure throughout a person’s lifetime. Understanding the visual presentation of solar lentigo symptoms is crucial for accurate identification.
The most common locations for observing solar lentigo symptoms pictures include the face, especially the forehead, cheeks, and temples, as well as the dorsal hands (back of the hands), forearms, shoulders, and décolletage (upper chest). These areas are perpetually exposed to ultraviolet (UV) radiation, leading to an accumulation of melanin in the basal layer of the epidermis. Unlike freckles (ephelides), which often darken with sun exposure and fade in its absence, solar lentigines tend to persist once they appear, becoming more numerous and prominent with age. The pigmentation within a solar lentigo is often uniform throughout the lesion, though some may exhibit slight variations in tone. When multiple solar lentigines coalesce, they can form larger, irregularly shaped patches of discoloration, further contributing to an uneven skin tone. Accurate recognition of these pigmented lesions is the first step in managing their appearance or monitoring for any atypical changes that might warrant medical attention. The clinical presentation of solar lentigo is typically benign, but differentiation from more serious pigmented lesions, such as melanoma, is always a critical consideration for dermatologists when reviewing skin symptoms pictures.
Common characteristics of mature solar lentigo lesions:
- Coloration: Uniformly light brown, dark brown, or occasionally black. This consistent pigmentation is a key diagnostic feature in solar lentigo images. The hue is usually even across the entire macule, without the multiple shades or variegated coloring seen in more atypical pigmented lesions.
- Shape: Predominantly round or oval, but irregular shapes can also be observed, especially when lesions coalesce. Their borders are typically distinct and well-defined, making them stand out against surrounding skin.
- Size: Varies from a few millimeters to several centimeters. They can start small and gradually expand over years. The rate of expansion is usually slow, but consistent with ongoing photo-damage.
- Surface: Smooth and flat, flush with the surrounding skin. There is no palpable texture difference, scaling, crusting, or elevation, which distinguishes them from rougher, raised lesions like seborrheic keratoses or actinic keratoses.
- Location: Exclusively found on sun-exposed areas like the face, hands, forearms, shoulders, and upper back. These areas are prone to cumulative UV damage, directly linking their presence to environmental exposure. Rarely found on mucous membranes or non-sun-exposed skin.
- Persistence: Unlike freckles, solar lentigines do not fade significantly during winter months; they are permanent changes in skin pigmentation, indicating a long-term alteration in melanin production and distribution.
- Symptom-Free: Generally asymptomatic, meaning they do not cause itching, pain, tenderness, bleeding, or any other form of physical discomfort. Their primary impact is cosmetic.
- Number: Can appear singly or, more commonly, as multiple lesions scattered across sun-exposed skin, indicating widespread photoaging and chronic sun exposure. The number often increases with age.
- Demarcation: Usually well-defined borders, making them distinct from the surrounding normal skin. This sharp border is often visible in solar lentigo symptoms pictures and aids in clinical diagnosis.
Differentiating features of solar lentigo from other skin conditions (brief overview):
- Freckles (Ephelides): Freckles are smaller, often appear in childhood, tend to darken with sun exposure and significantly lighten or disappear in its absence (e.g., during winter). Solar lentigines are persistent, generally larger, and often appear later in life.
- Seborrheic Keratoses: These are typically raised, have a “stuck-on” or waxy appearance, and can be brown, black, or tan with a crumbly or scaly surface. They often have clear follicular openings. Solar lentigines are consistently flat and smooth.
- Actinic Keratoses: These are precancerous lesions that are typically rough, scaly, and often red, pink, or flesh-colored, though some can be pigmented. They feel like sandpaper to the touch. Solar lentigines are flat, smooth, and benign pigmented spots.
- Melanoma: Melanomas are malignant lesions that often exhibit asymmetry, irregular borders, varied color (multiple shades of brown, black, red, white, or blue), a diameter larger than 6mm, and evolution (changes over time in size, shape, or color). Solar lentigines are typically uniform in color and shape, with regular borders, and generally stable over shorter periods. Any lesion displaying the ABCDE criteria (Asymmetry, Border irregularity, Color variation, Diameter > 6mm, Evolving/Changing) should be evaluated by a dermatologist promptly.
- Lentigo Simplex: Benign macules, often present from birth or early childhood, not necessarily related to sun exposure, and typically smaller and fewer in number than solar lentigines.
Signs of Solar Lentigo Pictures
The visible signs of solar lentigo pictures provide compelling evidence of cumulative sun damage and the broader process of photoaging. These pigmented lesions serve as clinical markers, indicating that the skin has undergone significant exposure to ultraviolet radiation, leading to changes in melanocyte activity and melanin distribution. Dermatologists often observe the distribution and characteristics of solar lentigines as part of a comprehensive skin examination, as they reflect a patient’s historical sun exposure patterns. The presence of numerous solar lentigines, particularly on chronically exposed areas, is a strong indicator of an increased risk for other forms of sun-induced skin damage, including actinic keratoses and skin cancers, although solar lentigines themselves are benign. The development of these spots is a gradual process, often starting in middle age or later, but can appear earlier in individuals with fair skin and a history of excessive sun exposure or sunburns. The consistency in their appearance across different individuals, specifically their flat, uniformly pigmented nature, is a key diagnostic sign that clinicians look for. The sheer volume of solar lentigines can be a significant indicator of long-term sun exposure and serves as a visual warning sign for increased risk of other sun-related skin conditions.
Examining signs of solar lentigo pictures also allows for the assessment of their evolution. Over time, individual solar lentigines can become darker, larger, and more numerous. This progression is a direct sign of ongoing or past sun damage. While they are usually uniform in color, subtle variations can occur, but gross changes in color, size, or shape should prompt a professional evaluation to rule out malignancy. Histopathologically, a solar lentigo is characterized by an increased number of melanocytes at the dermal-epidermal junction and an elongation of the rete ridges (epidermal downgrowths) with increased basal layer pigmentation. These microscopic changes are the underlying reasons for the visible skin discoloration. The commonality of these lesions makes them a frequent subject in discussions about sun-damaged skin and the importance of preventive measures. Their presence is a clear physical manifestation of environmental impact on skin health and appearance, underscoring the need for effective sun protection strategies to prevent further development and worsening of existing lesions. The absence of palpable thickening or inflammation around these lesions is a consistent clinical sign, reinforcing their benign nature. When multiple lesions are present, they often appear randomly distributed across sun-exposed surfaces, highlighting the diffuse nature of UV radiation damage.
Specific signs indicating long-term sun damage manifesting as solar lentigines:
- Presence on Sun-Exposed Areas: The definitive sign is their location on parts of the body that receive the most direct and chronic sunlight, such as the face (forehead, cheeks, temples), neck, upper chest (décolletage), shoulders, dorsal hands, and forearms. This direct correlation with sun exposure is undeniable in solar lentigo imagery, making it the primary diagnostic clue.
- Gradual Onset with Age: While not exclusively tied to advanced age, their prevalence and number significantly increase with age, reflecting cumulative UV exposure over decades. They are often termed age spots for this reason, becoming more noticeable from the 40s onward, though they can appear earlier in susceptible individuals.
- Persistence: Unlike temporary freckles (ephelides), these lesions do not fade with reduced sun exposure. They represent permanent alterations in skin pigmentation due to chronic UV damage, signifying a lasting change in the skin’s melanocyte activity.
- Absence of Inflammation: The lack of redness, swelling, tenderness, itching, or pain around the lesion is a key clinical sign. Solar lentigines are purely pigmentary changes, not inflammatory reactions or infections.
- Associated with Other Photoaging Signs: Often co-exist with other visible signs of sun damage, such as fine lines, wrinkles, skin laxity, telangiectasias (spider veins), poikiloderma of Civatte (a mottled redness with pigmentation and atrophy on the neck), and actinic keratoses. This constellation of signs paints a comprehensive picture of chronic UV damage.
- Histopathological Features: Microscopic examination reveals increased numbers of normal melanocytes in the basal layer of the epidermis, along with elongation and broadening of the epidermal rete ridges and increased melanin within the basal keratinocytes. These findings differentiate them from other pigmented lesions.
- Epidemiological Link: A higher incidence is observed in fair-skinned individuals (Fitzpatrick skin types I-III) who sunburn easily and have a history of significant recreational or occupational sun exposure, correlating directly with individual susceptibility and exposure history.
- Slow, Benign Progression: While they may slowly enlarge or darken over many years, solar lentigines exhibit stable, benign growth patterns without the rapid changes or infiltrative growth characteristic of malignant lesions.
Areas of the body most susceptible to showing solar lentigo signs:
- Face: Forehead, temples, cheeks, nose, and around the eyes are prime locations due to constant, direct, and often unprotected sun exposure. Facial solar lentigo images are among the most commonly observed and cosmetically concerning.
- Dorsal Hands: The back of the hands is a highly vulnerable area, consistently exposed to sun, and often shows some of the earliest and most pronounced signs of solar lentigo, indicating a lifetime of hand exposure.
- Forearms: Especially the extensor surfaces (outer aspect) of the forearms, which are consistently exposed when sleeves are short or absent. The density often increases towards the wrists and elbows.
- Shoulders and Upper Back: Frequently exposed during outdoor activities, particularly in individuals who spend a lot of time shirtless or in swimwear. These areas can accumulate significant sun damage.
- Décolletage (Upper Chest): This area is often exposed by clothing necklines and can accumulate significant sun damage, leading to numerous sun spots, often accompanied by other signs of poikiloderma.
- Scalp (in bald individuals): Unprotected scalps are extremely susceptible to UV radiation and can develop solar lentigines alongside actinic keratoses and basal cell carcinomas.
- Shins: Less common but can occur, particularly in individuals who wear shorts frequently or are exposed to sun while sitting, demonstrating the reach of UV light even on less obvious areas.
- Neck: Especially the sides and back of the neck, areas often overlooked during sunscreen application or covered inadequately by clothing.
Early Solar Lentigo Photos
Examining early solar lentigo photos reveals the incipient stages of these common pigmented lesions, offering insight into their initial appearance before they become more prominent and widespread. Initially, an early solar lentigo may present as a very faint, light brown macule, often barely noticeable to the untrained eye. These early lesions are typically small, perhaps only a few millimeters in diameter, and may have slightly less defined borders compared to more mature lesions. The pigmentation might not yet be perfectly uniform, sometimes appearing somewhat mottled or subtly patchy within the lesion, reflecting the nascent accumulation of melanin. What does Solar Lentigo look like symptoms pictures in its early phase often show a subtle darkening that occurs gradually over months or years, often unnoticed until several lesions have developed or an existing one has visibly darkened. These early manifestations are direct results of localized increases in melanocyte activity and melanin production in response to cumulative, though perhaps not immediately severe, UV exposure. They are not inflammatory and do not cause any physical symptoms like itching or pain, making their detection purely visual.
The development of early solar lentigo is usually linked to a history of intermittent or chronic sun exposure, rather than a single acute sunburn, although severe sunburns can predispose individuals to earlier onset. Individuals with lighter skin types (Fitzpatrick types I-III) are particularly susceptible to developing these incipient lesions, often beginning in their 30s or 40s. In its earliest stages, solar lentigo can sometimes be confused with nascent freckles, but a key differentiator is the persistence of the pigmentation even after sun exposure has ceased or diminished. Freckles tend to fade significantly in winter, whereas early solar lentigines, once formed, typically remain throughout the year. Monitoring changes in these faintly pigmented spots is important, although they are overwhelmingly benign. The appearance of multiple small, light brown spots on areas like the back of the hands or the face in individuals in their 30s or 40s often represents the start of widespread solar lentigines. Recognizing these early stage solar lentigo signs can prompt individuals to enhance their sun protection habits, potentially mitigating the development of more numerous and darker lesions in the future. Preventative measures are most effective when applied at this early stage of photoaging signs, making early identification a valuable tool for patient education and proactive skincare. These initial signs are critical for understanding the progression of sun-induced skin damage and reinforcing the need for lifelong sun protection.
Characteristics of early-stage solar lentigo:
- Subtle Pigmentation: Very light brown or tan, often barely darker than the surrounding skin. The pigmentation in these early solar lentigo photos is usually subdued, making them easy to overlook in their initial phase.
- Small Size: Typically only 1-3 millimeters in diameter, though they can slowly expand. They are generally smaller than mature lesions and are less likely to coalesce with adjacent spots.
- Faint Borders: May have less distinct or slightly irregular borders compared to more established lesions, making them harder to perceive and differentiate from minor skin variations.
- Slow Progression: Develop gradually over time, often becoming more noticeable as they darken and enlarge. This slow, insidious evolution is characteristic of early lesions, often taking years to become prominent.
- Appearance on Sun-Exposed Skin: Always localized to areas regularly exposed to UV radiation, reinforcing their origin from sun damage. Common sites include the face and back of hands, even in younger individuals with significant sun exposure history.
- Asymptomatic: No associated itching, pain, or inflammation. Their presence is purely a visual skin change, posing no physical discomfort.
- Persistence: Unlike juvenile freckles, these initial lentigines do not disappear or significantly lighten during periods of reduced sun exposure. They mark a permanent, albeit subtle, change in the skin.
- First Signs of Photoaging: Often among the first visible indicators of chronic sun damage, preceding more severe forms of photoaging like deeper wrinkles or significant skin textural changes.
- Number: May appear singly at first, but with continued sun exposure, multiple early lesions will often develop, indicating a broader predisposition to sun damage.
Factors influencing the early development of solar lentigo:
- Cumulative UV Exposure: The most significant factor. Even moderate, consistent sun exposure over years can trigger early solar lentigo. This is not necessarily about severe sunburns but the total lifetime dose of UV radiation.
- Skin Type: Individuals with lighter skin tones (Fitzpatrick types I-III) who burn easily and tan poorly are genetically more prone to developing lentigines earlier in life due to less protective melanin.
- Genetics: A familial predisposition to freckling or hyperpigmentation can increase the likelihood of developing solar lentigines, suggesting a genetic component to susceptibility.
- Sunburn History: While chronic exposure is key, a history of severe sunburns, especially during childhood or adolescence, can accelerate the process, triggering localized damage that manifests as early lesions.
- Lack of Sun Protection: Inconsistent or absent use of sunscreen, protective clothing, and shade significantly contributes to early onset by allowing unchecked UV penetration. This is a crucial modifiable factor in preventing early sun spots.
- Geographic Location: Living in regions with high UV index, such as tropical or high-altitude areas, naturally increases UV exposure and thus the risk of early development.
- Outdoor Hobbies/Occupations: Lifestyles or professions that involve prolonged time outdoors (e.g., farming, construction, sports, gardening) without adequate protection significantly increase exposure and risk of early lesions.
- Age: While early development can occur, the incidence and prevalence increase significantly with age, indicating the cumulative nature of the damage.
Skin rash Solar Lentigo Images
While solar lentigo is not typically classified as a “skin rash” in the conventional sense, as it lacks inflammatory components like redness, swelling, or itching, the term skin rash solar lentigo images might be used to describe the widespread distribution and numerous lesions that can cover significant areas of sun-exposed skin. Instead of an inflammatory eruption, solar lentigines present as a proliferation of distinct, non-inflammatory pigmented macules that, when numerous, can create a mottled or “speckled” appearance on the skin, resembling a diffuse pattern. This pattern, particularly on areas like the chest, shoulders, or back of the hands, can sometimes be visually interpreted as a “rash” of spots, rather than individual isolated lesions. What does Solar Lentigo look like symptoms pictures in this context highlights the cumulative effect of sun damage resulting in multiple, often coalescing, hyperpigmented areas that contribute to an uneven skin tone and texture perception. The lack of itching, burning, or discomfort associated with these spots is a key differentiator from true dermatological rashes, which are typically characterized by these symptoms of inflammation or irritation. The appearance of multiple, seemingly randomly distributed brown spots can visually overwhelm the skin, leading to the mischaracterization as a form of “rash.”
The appearance of multiple solar lentigines distributed across a broad skin surface strongly correlates with a history of chronic and unprotected sun exposure. This widespread presence serves as a visual testament to significant cumulative ultraviolet radiation damage, often signifying years of inadequate sun protection. Unlike allergic rashes, viral rashes, or fungal infections, solar lentigines are purely pigmentary changes that do not involve an immune response or infectious agent. Their smooth, flat surface and stable nature further distinguish them from inflammatory skin conditions that are often raised, scaly, vesicular, or rapidly evolving. When viewing skin rash solar lentigo images, one will notice the consistent brown to dark brown coloration of the lesions, often varying slightly in size and shape but maintaining their characteristic benign appearance and non-inflammatory nature. The term “rash” in this context refers to the sheer number and widespread scattering of these pigmented macules across a broad area of skin, creating a pattern of discoloration, rather than an acute inflammatory process. Understanding this distinction is vital for proper diagnosis and reassurance, as solar lentigines are benign, while many rashes require specific medical intervention. The prevalence of these lesions is a strong indicator of the extent of photoaging and should prompt a discussion about sun protection and skin cancer screening with a healthcare provider, even if the lesions themselves are harmless. The chronic, non-tender nature is a crucial diagnostic feature.
Differences between solar lentigo and common skin rashes:
- Inflammation: Rashes typically involve clear signs of inflammation such as redness (erythema), swelling (edema), heat, and sometimes tenderness. Solar lentigines are distinctly non-inflammatory; they appear as flat, pigmented spots without any surrounding erythema or palpable changes.
- Symptoms: Rashes often cause subjective symptoms like itching (pruritus), burning, stinging, pain, or tenderness. Solar lentigines are almost uniformly asymptomatic, causing no physical discomfort whatsoever.
- Texture: Rashes can be raised, bumpy (papules, nodules), scaly (desquamation), vesicular (blister-like), pustular, or weeping. The surface may feel rough, uneven, or wet. Solar lentigines are consistently flat (macular) and smooth, flush with the surrounding skin, with no textural irregularities.
- Color: While rashes can be red, pink, purplish, or varied due to inflammation or vascular involvement, solar lentigines are consistently brown to dark brown, reflecting melanin accumulation. The color is typically uniform within each lesion.
- Cause: Rashes can be caused by a multitude of factors, including allergies (contact dermatitis), infections (bacterial, viral, fungal), autoimmune conditions (psoriasis, eczema), irritants, or systemic diseases. Solar lentigines are solely caused by chronic exposure to ultraviolet (UV) radiation.
- Evolution: Rashes can appear rapidly (acute onset) and resolve or change significantly over days to weeks. Solar lentigines develop slowly over years and are persistent, showing only gradual changes in size or color over prolonged periods.
- Contagion: Rashes, especially infectious ones (e.g., viral exanthems, impetigo), can be contagious. Solar lentigines are non-infectious and therefore not contagious in any way.
- Associated Features: Rashes may be accompanied by fever, malaise, or other systemic symptoms. Solar lentigines are isolated skin findings, typically not associated with general health complaints.
Visual patterns of multiple solar lentigo spots on sun-exposed skin:
- Scattered Distribution: Often appear as individually distinct spots scattered across an entire sun-exposed area, like the back of the hands or forearms. This diffuse pattern can be quite widespread, giving the impression of numerous, separated spots.
- Coalescence: In areas of intense chronic exposure, multiple smaller lentigines can merge or grow into one another, forming larger, irregularly shaped patches of hyperpigmentation. This creates a broader, more continuous area of discoloration rather than discrete spots.
- Density in High-Exposure Zones: The concentration of lentigines is typically highest on the most sun-exposed convexities of the body, such as the cheekbones, bridge of the nose, tops of shoulders, and dorsal hands, indicating areas of maximal UV impact.
- Symmetry: While not perfectly symmetrical in individual lesion placement, solar lentigines often appear on both sides of the body (e.g., both hands, both forearms, both cheeks) if sun exposure has been relatively balanced over time.
- Non-Uniform Skin Tone: The collective presence of numerous solar lentigines leads to an overall non-uniform or mottled skin tone, particularly noticeable against areas less exposed to the sun. This contributes to the aged appearance of sun-damaged skin.
- “Speckled” Appearance: Many small, brown spots can give the skin a “speckled” or “peppered” appearance, which some might loosely associate with a benign pigmented rash, particularly on the chest or arms.
- Associated with Other Photoaging: These patterns often occur alongside other signs of aging skin, such as fine lines, deeper wrinkles, telangiectasias (spider veins), skin laxity, and a generally dull or leathery skin texture, completing the visual picture of extensive environmental damage.
- Clear Demarcation: Despite their numbers, individual lesions often retain clear, distinct borders, even when closely spaced, which helps to differentiate them from diffuse post-inflammatory hyperpigmentation.
Solar Lentigo Treatment
While solar lentigines are benign and do not require treatment for medical reasons, many individuals seek solar lentigo treatment for cosmetic purposes to improve skin uniformity and reduce the visible signs of sun damage. A variety of effective treatments are available, ranging from topical creams to light-based therapies and cryotherapy. The choice of treatment for solar lentigo removal depends on several factors, including the number and size of the lesions, skin type, patient preference, the clinician’s expertise, and the available technology. What does Solar Lentigo look like symptoms pictures often guides the treatment approach, as darker, more pronounced lesions may respond better to certain modalities, while widespread, lighter lesions might benefit from other options. Regardless of the chosen treatment, strict adherence to sun protection measures post-treatment is crucial to prevent the recurrence of existing lesions and the development of new ones. Comprehensive hyperpigmentation treatment plans often incorporate both active lesion removal and long-term preventive strategies to achieve optimal and lasting results. It’s essential to consult with a board-certified dermatologist to determine the most appropriate and safest treatment plan for individual cases of solar lentigo, ensuring the chosen method is suitable for your skin type and specific concerns.
Effective solar lentigo treatment aims to reduce or eliminate the excess melanin responsible for the pigmentation. Non-invasive and minimally invasive options are preferred due to the benign nature of the lesions and the desire to minimize recovery time and potential side effects. Topical therapies are often the first line for widespread or less prominent solar lentigines, offering a gradual reduction in pigmentation. For more stubborn or localized spots, procedures like laser therapy, intense pulsed light (IPL), or cryotherapy offer more targeted and often quicker results. Each treatment modality carries its own set of considerations regarding efficacy, potential side effects (e.g., temporary redness, swelling, blistering, or changes in pigmentation), recovery time, and cost. Patients should be fully informed about what to expect before, during, and after any procedure, including potential downtime and necessary aftercare. Post-treatment care is vital, typically involving rigorous sun protection and gentle skin care, to facilitate proper healing, prevent complications, and maintain the cosmetic improvements. The goal of any lentigo removal strategy is not only to diminish the visible spots but also to improve overall skin health, achieve a more even complexion, and encourage healthier, lifelong skin habits, with an emphasis on continuous sun protection as the foundation of long-term success, irrespective of whether active treatment is pursued.
Overview of medical treatments for solar lentigo:
- Laser Therapy:
- Q-switched Lasers (e.g., Q-switched Nd:YAG, Ruby, Alexandrite): These highly specialized lasers emit very short, high-energy pulses of light that are specifically absorbed by melanin pigments in the solar lentigo, breaking them down into smaller particles. These particles are then naturally cleared by the body’s immune system. Highly effective for individual, well-demarcated solar lentigines. Often requires 1-3 sessions, spaced several weeks apart. Side effects can include temporary redness, swelling, bruising, blistering, or post-inflammatory hyperpigmentation (PIH), especially in darker skin types, or less commonly, hypopigmentation (lightening of the treated area).
- Picosecond Lasers: Represent a newer generation of laser technology, delivering ultra-short pulses (picoseconds, trillionths of a second). These lasers shatter melanin particles even more effectively and with less heat generation than Q-switched lasers, potentially offering faster melanin clearance with fewer treatment sessions and a reduced risk of heat-related side effects like PIH, making them particularly suitable for stubborn hyperpigmentation and darker skin types.
- Fractional Lasers (ablative and non-ablative): These lasers create microscopic treatment zones in the skin, stimulating collagen production and promoting turnover of pigmented cells. They are effective for widespread solar lentigines and overall skin rejuvenation, improving texture and tone alongside pigmentation. Multiple sessions are typically needed. Ablative fractional lasers have more downtime but greater efficacy for severe photoaging, while non-ablative ones have less downtime.
- Intense Pulsed Light (IPL):
- IPL is not a laser but uses broad-spectrum light delivered in pulses. It targets melanin (and hemoglobin for redness in blood vessels), making it highly effective for widespread solar lentigines and overall signs of photoaging, including textural improvements and reduction of redness. Multiple sessions (typically 3-5, spaced 3-4 weeks apart) are usually required. Side effects are generally milder than Q-switched lasers, including temporary redness, swelling, and darkening of the spots before they flake off. It is excellent for improving overall skin tone and texture, making it a popular choice for diffuse pigmentation.
- Cryotherapy:
- Involves applying liquid nitrogen (a very cold gas) to the solar lentigo, freezing the melanocytes and causing cellular damage. This leads to the formation of a blister, which then scabs over and peels off, taking the pigmented cells with it. Effective for individual or small clusters of lesions. Can cause temporary redness, swelling, blistering, and sometimes hypopigmentation (lightening of the skin) or hyperpigmentation, particularly in darker skin types. Requires precision to avoid damage to surrounding healthy skin and typically involves a healing period of 1-2 weeks.
- Chemical Peels:
- Involves the application of a chemical solution (e.g., glycolic acid, salicylic acid, trichloroacetic acid (TCA), Jessner’s solution) to exfoliate the top layers of skin, including the pigmented epidermal cells. Effective for superficial and widespread solar lentigines, simultaneously improving overall skin texture and tone. The depth of the peel determines its efficacy and recovery time. Multiple sessions are usually needed, depending on the peel’s strength. Side effects can include redness, peeling, temporary sensitivity, and a risk of PIH, especially with deeper peels or in darker skin.
- Topical Agents:
- Hydroquinone: A gold-standard depigmenting agent that inhibits the enzyme tyrosinase, which is crucial for melanin production. Available in various strengths (2% over-the-counter, 4% or higher by prescription). Effective for gradual lightening of solar lentigines but requires consistent, long-term use (often several months). Can cause irritation, dryness, or, rarely, a bluish discoloration (exogenous ochronosis) with prolonged high-concentration use. Often used in combination with retinoids and corticosteroids.
- Retinoids (e.g., Tretinoin, Retinol, Adapalene): Derivatives of vitamin A that promote rapid cell turnover (exfoliation) and can help distribute melanin more evenly in the epidermis. Used for overall skin rejuvenation, improving fine lines, and gradual lightening of lentigines. Can cause redness, peeling, dryness, and increased sun sensitivity, especially during the initial weeks of use.
- Alpha Hydroxy Acids (AHAs) and Beta Hydroxy Acids (BHAs): Exfoliate the skin and promote cell turnover (e.g., glycolic acid, lactic acid, salicylic acid). Milder than professional chemical peels, often found in over-the-counter creams, serums, and cleansers. They aid in the reduction of superficial pigmentation by shedding pigmented cells and can improve skin texture.
- Other Brightening Agents: Ingredients like kojic acid, azelaic acid, vitamin C (ascorbic acid), niacinamide, arbutin, licorice extract, and tranexamic acid can help lighten solar lentigines by inhibiting melanin production, acting as antioxidants, or interfering with pigment transfer. Often used in combination with other treatments for enhanced and synergistic results.
Essential preventative measures against solar lentigo development:
- Daily Sunscreen Use: This is the single most important and effective step in preventing new solar lentigo lesions and stopping existing ones from worsening. Apply broad-spectrum sunscreen with an SPF of 30 or higher (preferably SPF 50+) every single day, regardless of weather or season, to all exposed skin. Reapply every two hours when outdoors, or more frequently if swimming, sweating heavily, or after towel drying. Ensure it provides protection against both UVA and UVB rays.
- Protective Clothing: Wear long-sleeved shirts, long pants, wide-brimmed hats (at least 3-inch brim all around), and UV-protective clothing (UPF-rated apparel). This physically blocks UV radiation more effectively than sunscreen alone and offers consistent protection without reapplication.
- Seek Shade: Avoid direct sun exposure, especially during peak hours (typically 10 a.m. to 4 p.m. in most regions) when UV radiation is strongest. Utilize natural shade from trees or structures, or carry an umbrella.
- Avoid Tanning Beds: Tanning beds emit harmful UV radiation (primarily UVA, which penetrates deeper) that significantly accelerates the development of solar lentigines, photoaging, and drastically increases the risk of all forms of skin cancer, including melanoma.
- Regular Skin Self-Exams: Conduct monthly head-to-toe skin self-exams to monitor your skin for any new or changing spots, including the appearance of new solar lentigines or any changes in size, shape, or color of existing ones. Early detection of suspicious lesions is key for better outcomes.
- Annual Dermatological Check-ups: Schedule professional skin exams with a board-certified dermatologist, particularly if you have a history of significant sun exposure, multiple solar lentigines, a personal or family history of skin cancer, or any concerning lesions. Dermatologists can identify suspicious spots that laypeople might miss.
- Antioxidant Skincare: Incorporate topical antioxidants like Vitamin C, Vitamin E, ferulic acid, and green tea extract into your daily skincare routine. These ingredients can help neutralize free radicals generated by UV exposure, potentially reducing oxidative stress, skin damage, and the formation of pigmentation.
- Awareness of UV Index: Pay attention to the daily UV index report from weather forecasts. Take extra precautions and intensify sun protection efforts when the UV index is high (e.g., 3 or higher).
- Sunglasses: Wear UV-blocking sunglasses to protect the delicate skin around the eyes and reduce the risk of eye damage from UV radiation.