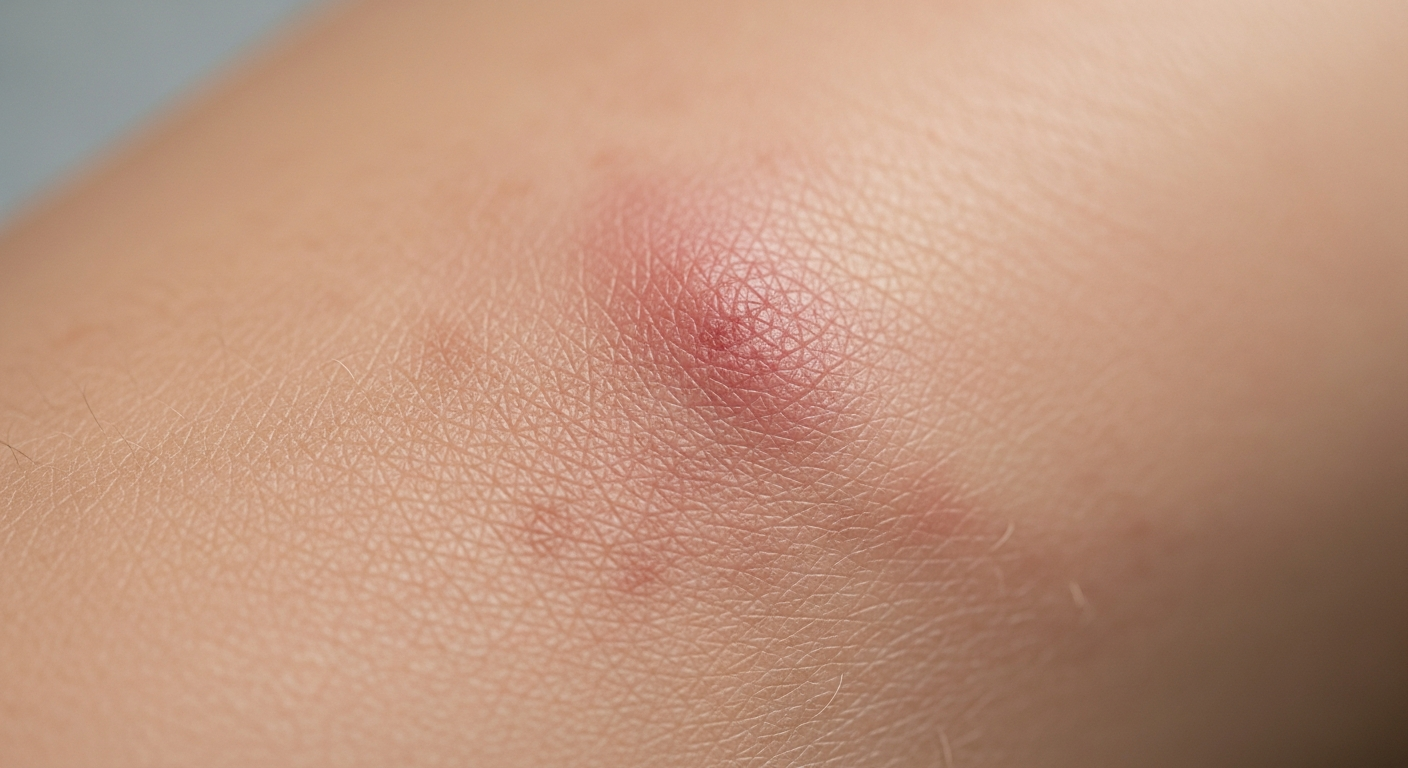
This article provides detailed descriptions of Atopic dermatitis symptoms pictures, helping to visually identify the condition through its diverse manifestations. We delve into observable signs and the progression of eczema, offering insight into what these skin conditions look like at various stages.
Atopic dermatitis Symptoms Pictures
Understanding Atopic dermatitis symptoms pictures involves recognizing the primary visual cues that characterize this chronic inflammatory skin condition. The skin’s appearance in Atopic dermatitis can vary significantly depending on the patient’s age, skin tone, and the chronicity of the condition. However, certain hallmark features are consistently observed across eczema pictures and clinical presentations. These symptoms are often intensely itchy, leading to a vicious cycle of scratching, further inflammation, and skin damage. Patients frequently report sensations ranging from mild irritation to excruciating, persistent itch that disrupts sleep and daily activities. The distribution of these symptoms is also crucial for identification, typically favoring flexural areas in older children and adults, while presenting on the face and extensor surfaces in infants. The presence of these visual symptoms in Atopic dermatitis images is essential for accurate diagnosis and management planning.
Key Visual Symptoms in Atopic Dermatitis Pictures:
- Erythema (Redness): One of the most common and earliest visible symptoms. Affected skin areas appear red or reddish-brown due to inflammation. In lighter skin tones, this redness can be quite vivid, appearing as bright pink or fiery red patches. In darker skin tones, erythema might manifest as violaceous (purple) or ashen-gray patches, making it sometimes challenging to discern without careful examination under proper lighting. This redness is indicative of active inflammation in the dermis and epidermis.
- Dry Skin (Xerosis): Almost universally present, dry skin is a foundational symptom of Atopic dermatitis. The skin often looks scaly, rough, and feels tight, lacking the normal suppleness and moisture. This dryness contributes significantly to the barrier dysfunction characteristic of AD, allowing irritants and allergens to penetrate more easily. Dry skin eczema pictures prominently display this scaling and dullness, often with fine lines and cracks.
- Itching (Pruritus): While not directly visible in a static picture, the effects of intense itching are paramount. Evidence of scratching such as excoriations (scratch marks), erosions, and secondary infections can be seen. The chronic nature of the itch leads to frequent scratching, which further damages the skin barrier and exacerbates inflammation, creating a persistent itch-scratch cycle.
- Edema (Swelling): During acute flares, the skin can become swollen and puffy, indicating increased fluid in the tissues. This swelling is particularly noticeable around the eyes or on the hands and feet. The inflamed areas may appear raised and thickened due to this underlying edema.
- Papules and Vesicles: In acute phases, especially in infants and young children, small, raised bumps (papules) and tiny fluid-filled blisters (vesicles) may appear. These vesicles can rupture, leading to weeping and crusting. Acute eczema pictures frequently show these vesicular lesions.
- Lichenification (Skin Thickening): A classic sign of chronic Atopic dermatitis, resulting from prolonged scratching and rubbing. The skin becomes thickened, leathery, and often develops exaggerated skin lines, resembling the bark of a tree. This change indicates long-standing inflammation and mechanical trauma. Lichenified skin images clearly show this coarse texture and prominent skin folds.
- Crusting: Yellowish or honey-colored crusts can form on the skin surface, often indicating secondary bacterial infection (e.g., Staphylococcus aureus) on weeping lesions. These crusts are dried serum or pus.
- Scales and Flakes: Shedding of epidermal cells resulting in visible flakes on the skin surface. This is particularly noticeable in areas of chronic dryness and inflammation. The degree of scaling can range from fine, powdery flakes to thick, adherent scales.
- Hyperpigmentation/Hypopigmentation: Post-inflammatory changes can lead to darkening (hyperpigmentation) or lightening (hypopigmentation) of the skin in affected areas, especially in individuals with darker skin tones. These dyspigmentation issues can persist long after the active inflammation has subsided and are often a source of cosmetic concern. Eczema hyperpigmentation pictures illustrate these varied color changes.
- Fissures: Cracks in the skin, particularly in areas of movement or severe dryness, such as around joints or on the palms and soles. These fissures can be painful and may bleed, increasing the risk of infection.
Identifying these diverse features in Atopic dermatitis symptoms pictures is key to understanding the disease’s presentation and progression. The appearance is dynamic, changing from acute inflammatory stages with redness and weeping to chronic stages with lichenification and pigmentary changes. Consistent observation of these features aids in differential diagnosis from other dermatological conditions.
Signs of Atopic dermatitis Pictures
The signs of Atopic dermatitis pictures encompass observable objective findings that a clinician can identify, often reflecting the severity and chronicity of the disease. While closely related to symptoms, signs focus on the physical manifestation rather than the subjective experience. These visual signs provide critical evidence for diagnosis and monitoring the effectiveness of treatment. Examining eczema signs across different age groups and body parts reveals a spectrum of presentations, from subtle changes to pronounced dermatological lesions. The interplay of genetic predisposition, environmental triggers, and immune dysregulation culminates in these visible skin changes. Recognition of these specific signs in various skin inflammation photos is fundamental for accurate assessment.
Observable Signs in Atopic dermatitis Pictures:
- Location and Distribution:
- Infantile Eczema (0-2 years): Typically affects the face (cheeks, forehead, scalp), and extensor surfaces of the arms and legs. The diaper area is usually spared. Often presents as red, weeping, crusted patches. Baby eczema pictures commonly show these facial and scalp lesions.
- Childhood Eczema (2 years-puberty): Commonly found in flexural areas (antecubital fossae, popliteal fossae), neck, wrists, and ankles. Lesions are often drier, more lichenified, and less exudative than in infants.
- Adult Eczema: Similar distribution to childhood eczema (flexural areas) but can also involve hands, feet, eyelids, and nipples. Lichenification is prominent, and patients may present with nummular (coin-shaped) or discoid eczema patterns.
- Generalized Eczema: In severe cases, Atopic dermatitis can affect large areas of the body, leading to widespread erythema, scaling, and lichenification.
- Xerosis Cutis (Dry Skin): The skin often appears dull, fine-scaled, and feels rough. This widespread dryness is a characteristic background feature upon which flares develop. Chronic eczema images often highlight the persistent dry, lacklustre appearance of the skin.
- Excoriations: Linear scratch marks of varying depths and stages of healing, resulting from intense pruritus. These marks are a direct consequence of scratching and indicate active or recent itching. They can range from superficial epidermal abrasions to deeper dermal wounds.
- Lichenification: Thickened, leathery skin with accentuated skin markings, appearing as a result of chronic rubbing and scratching. This sign is a strong indicator of long-standing Atopic dermatitis and is particularly prominent in flexural areas, neck, and extremities. The texture is coarse and indurated, distinct from normal skin.
- Erythroderma: In severe cases, especially during widespread flares, the entire skin surface may become red, scaly, and inflamed. This condition, known as erythroderma or exfoliative dermatitis, is a medical emergency requiring urgent attention.
- Dennie-Morgan Folds: Extra folds or creases below the lower eyelids, which are non-specific but often associated with Atopic dermatitis. These folds are thought to be related to chronic inflammation or lymphatic changes in the periorbital area.
- Allergic Shiners: Darkening or discoloration under the eyes, resembling “black eyes.” This sign is often attributed to venous congestion secondary to chronic inflammation or allergies, common in Atopic individuals.
- Hyperlinear Palms and Soles: Exaggerated skin lines on the palms of the hands and soles of the feet. This sign reflects a tendency towards skin thickening and dryness, part of the atopic diathesis.
- Pityriasis Alba: Hypopigmented (lighter) patches, usually on the face, neck, and upper trunk, which are more visible in darker skin tones or after sun exposure. These areas often represent post-inflammatory changes following mild eczema. Pityriasis alba pictures show these characteristic lighter patches, which can sometimes be confused with fungal infections.
- Perioral Pallor: Paleness around the mouth, in contrast to the surrounding erythema of the face, can sometimes be observed.
- Cheilitis: Inflammation and cracking of the lips, particularly at the corners of the mouth, often due to lip licking or local inflammation.
- Hand and Foot Eczema: Specific patterns of Atopic dermatitis affecting the hands and feet, characterized by dryness, scaling, fissures, vesicles, and lichenification. These areas are prone to irritation and can be particularly debilitating. Hand eczema pictures frequently display these challenging manifestations.
- Nipple Eczema: Inflammation, redness, scaling, and itching of the nipples, which can be an isolated manifestation of AD or part of more generalized disease.
- Follicular Accentuation (Keratosis Pilaris-like): Small, pointed papules at the hair follicles, particularly on the outer aspects of the arms and thighs, which can indicate follicular involvement in AD.
The careful examination of these physical signs of Atopic dermatitis pictures enables a comprehensive understanding of the patient’s condition, guiding treatment strategies and prognosis. The observable changes range from acute weeping lesions to chronic lichenified plaques, each providing clues about the disease’s activity and history. Documenting these signs, especially through visual means, is invaluable in tracking the patient’s response to interventions.
Early Atopic dermatitis Photos
Early Atopic dermatitis photos are crucial for identifying the condition in its initial stages, particularly in infants and young children, where the presentation can be distinct. Recognizing these initial signs allows for prompt intervention, potentially altering the disease course and minimizing discomfort. The earliest manifestations often involve acute inflammatory reactions, appearing as red, oozing patches before progressing to drier, more chronic forms. These early presentations are frequently triggered by factors such as changes in diet, exposure to irritants, or allergens. Understanding what to look for in infant eczema pictures and baby eczema symptoms is vital for parents and caregivers. The skin barrier is particularly vulnerable in infants, making them susceptible to rapid development of symptoms. The precise appearance can be subtle at first, evolving quickly into more noticeable lesions. Early identification in acute eczema images helps distinguish AD from other common childhood rashes.
Characteristics in Early Atopic dermatitis Photos:
- Infantile Onset (First few months of life):
- Facial Eczema: Most commonly starts on the cheeks and forehead. Lesions are typically erythematous (red), often symmetrical, and can be intensely itchy, leading to rubbing against bedding or clothing. Baby eczema on face pictures clearly show these characteristic red patches.
- Scalp Involvement: Similar red, scaly, and sometimes greasy patches on the scalp, which can be mistaken for cradle cap but are typically itchier and more inflamed.
- Extensor Surfaces: Lesions can appear on the outer aspects of the arms and legs (elbows, knees). These areas are more prone to irritation from movement and clothing in infants.
- Acute Inflammation: The skin often appears bright red, swollen (edematous), with tiny papules and vesicles.
- Weeping and Crusting: The vesicles can rupture, leading to serous exudation (weeping) and the formation of yellowish or honey-colored crusts. This indicates an active inflammatory process and sometimes secondary infection. Weeping eczema images are often characteristic of acute flares in infancy.
- Dryness and Scaling: While weeping is prominent, areas might also show underlying dryness and fine scaling.
- Childhood Onset (Late infancy to early childhood):
- Flexural Involvement: As children grow, the distribution shifts from extensor to flexural areas. The creases of the elbows (antecubital fossae) and knees (popliteal fossae) are prime locations for early childhood AD. The neck, wrists, and ankles are also frequently affected.
- Less Weeping, More Dryness: Lesions tend to be less exudative than in infancy, with more prominent dryness, scaling, and mild thickening (lichenification) developing due to repeated scratching.
- Papular Eczema: Small, raised bumps (papules) may be more evident, sometimes coalescing into plaques.
- Prurigo Nodularis-like Lesions: In some children, persistent scratching can lead to firm, itchy nodules.
- Post-inflammatory Hypopigmentation: After inflammation subsides, areas may appear lighter than the surrounding skin, especially in children with darker skin tones. This is a common finding in childhood eczema photos.
- Subtle Early Signs:
- Generalized Dry Skin: Even before distinct rashes appear, infants and children with atopic tendencies often have unusually dry skin.
- Early Itching: While infants cannot verbalize itch, excessive fussiness, restless sleep, and attempts to rub against surfaces can be early indicators of pruritus.
- Sensitivity to Irritants: Early reactions to soaps, detergents, wool, or certain foods can signal a developing Atopic dermatitis predisposition.
Early diagnosis based on early Atopic dermatitis photos and clinical observation is critical. It allows for timely implementation of preventative measures, such as intense moisturization, trigger avoidance, and mild topical treatments, which can help manage flares and reduce the long-term impact of the disease. Observing the progression from initial redness and weeping to eventual dryness and thickening provides valuable insights into the natural history of AD. Recognizing these early visual cues facilitates prompt action, aiming to break the itch-scratch cycle before it becomes deeply entrenched.
Skin rash Atopic dermatitis Images
Skin rash Atopic dermatitis images showcase the diverse morphology of the eczematous lesions that are the hallmark of this condition. The appearance of the rash is highly variable, influenced by the age of the patient, the duration of the flare, and individual skin characteristics. From acute, intensely red, and weeping patches to chronic, thickened, and hyperpigmented plaques, the rash of Atopic dermatitis presents a complex visual spectrum. The relentless itching associated with these rashes often leads to secondary changes, such as excoriations and lichenification, which are also evident in eczema rash types. Understanding these various presentations is essential for accurate diagnosis and differentiating AD from other dermatological conditions that may mimic its appearance. Red itchy rash pictures are frequently sought by those trying to identify their symptoms, highlighting the need for detailed visual descriptions.
Variations in Skin Rash Atopic dermatitis Images:
- Acute Eczematous Rash:
- Erythema: Bright red, inflamed patches that are often sharply demarcated. This redness signifies active inflammation.
- Papules and Vesicles: Small, raised bumps and tiny fluid-filled blisters are characteristic. These can be pinpoint or slightly larger and are often intensely itchy.
- Edema: Swelling of the skin, making the affected areas appear puffy and raised.
- Weeping and Oozing: Ruptured vesicles or eroded skin surfaces release clear to yellowish fluid. This exudation can be profuse in severe acute flares.
- Crusting: Dried serum or pus forming yellowish or honey-colored crusts over the weeping areas, often indicative of secondary bacterial infection.
- Locations: Common in infants on the face and extensor surfaces; in adults, can occur anywhere but often signals a severe flare.
- Subacute Eczematous Rash:
- Less Weeping: The acute exudation subsides, and the rash becomes drier.
- Scaling: Fine to moderate flaking and shedding of skin cells become more prominent.
- Milder Erythema: Redness may be less intense, shifting from bright red to a duller reddish-brown hue.
- Mild Lichenification: Early signs of skin thickening may appear due to persistent scratching.
- Locations: Often seen as a transitional phase, or in mild flares, commonly in flexural areas in children and adults.
- Chronic Eczematous Rash:
- Lichenification: The most prominent feature, with thickened, leathery skin and accentuated skin markings due to prolonged rubbing and scratching. The skin’s texture becomes coarse.
- Hyperpigmentation/Hypopigmentation: Areas can appear darker (hyperpigmented) or lighter (hypopigmented) than surrounding healthy skin, especially after inflammation has subsided. These changes are more noticeable in individuals with darker skin tones. Eczema hyperpigmentation pictures often highlight this persistent discoloration.
- Dryness and Scaling: Persistent xerosis with prominent scaling and a dull, sometimes ashen, appearance.
- Fissures: Painful cracks in the skin, particularly in areas of movement or severe dryness.
- Excoriations: Ongoing scratch marks, indicating persistent itch.
- Locations: Predominantly in flexural areas (antecubital, popliteal fossae), neck, wrists, ankles, and often involving hands and feet.
- Specific Rash Presentations in Atopic Dermatitis Images:
- Nummular (Discoid) Eczema: Coin-shaped or oval patches of inflammation, often intensely itchy, with vesicles, crusts, and scales. Can appear anywhere but commonly on the trunk and limbs.
- Hand and Foot Eczema: Distinct patterns affecting these high-use areas, characterized by dryness, cracking, scaling, and sometimes deep, painful fissures or vesicles (dyshidrotic eczema component).
- Follicular Eczema: Involvement of hair follicles, presenting as small, itchy papules around the follicles, often with follicular hyperkeratosis.
- Perioral/Periocular Eczema: Rash around the mouth or eyes, which can be particularly sensitive and prone to irritation.
- Eczema Herpeticum: A severe complication where the eczematous skin becomes infected with herpes simplex virus, leading to widespread monomorphic (similar-sized) punched-out erosions, vesicles, and pustules. This is a medical emergency and looks distinctly different from typical eczema.
Analyzing skin rash Atopic dermatitis images allows for a deeper understanding of the disease’s varied presentations. The morphology of the rash is a dynamic entity, changing with age, disease activity, and the impact of the itch-scratch cycle. Careful observation of these detailed features in eczema images is paramount for differential diagnosis and for tailoring effective treatment strategies. Each type of rash carries specific implications for management, whether it’s acute weeping lesions requiring antiseptic care or chronic lichenified plaques needing potent anti-inflammatory agents.
Atopic dermatitis Treatment
While this article focuses on Atopic dermatitis symptoms pictures, a discussion on treatment is essential as it directly addresses and aims to alleviate the visible symptoms described. Atopic dermatitis treatment is multifaceted, focusing on symptom control, reducing inflammation, restoring the skin barrier, and preventing flares. The approach is highly individualized, considering the patient’s age, disease severity, affected body areas, and response to previous therapies. Effective management involves a combination of topical medications, systemic treatments for severe cases, phototherapy, and crucial lifestyle modifications. The goal is to improve the quality of life by reducing itching, clearing skin lesions, and prolonging remission periods. Consistent adherence to treatment protocols is vital for long-term success in managing eczema management. Addressing the underlying immune dysregulation and skin barrier defects is key to preventing the recurrence of visible symptoms.
Key Pillars of Atopic dermatitis Treatment:
- Skin Barrier Restoration and Hydration:
- Emollients and Moisturizers: The cornerstone of AD treatment. Daily and liberal application of thick, fragrance-free creams or ointments helps repair the skin barrier, lock in moisture, and reduce dryness. They should be applied multiple times a day, especially after bathing. Examples include petrolatum-based products, ceramides, and humectants. This helps reduce the scaling and roughness seen in dry skin eczema pictures.
- Lukewarm Baths/Showers: Short, lukewarm baths (avoiding hot water) followed immediately by patting dry and applying moisturizer (“soak and seal”) are recommended to hydrate the skin.
- Wet Wrap Therapy: Applying damp bandages or clothing over medicated creams, which helps to hydrate the skin, enhance absorption of topical medications, and reduce scratching by providing a physical barrier.
- Anti-Inflammatory Medications:
- Topical Corticosteroids (TCS): The primary treatment for active flares. Available in various potencies (mild to very potent) and formulations (creams, ointments, lotions). They reduce redness, swelling, and itching by suppressing the immune response in the skin. Used intermittently to control flares, not for continuous long-term use due to potential side effects like skin thinning. Selecting the appropriate potency and duration is crucial to avoid adverse effects.
- Topical Calcineurin Inhibitors (TCIs): Non-steroidal alternatives (e.g., tacrolimus, pimecrolimus) that suppress inflammation by inhibiting calcineurin, thereby reducing T-cell activation. They can be used on sensitive areas (face, eyelids, skin folds) where corticosteroids might cause thinning, and are suitable for long-term maintenance therapy to prevent flares.
- Topical PDE4 Inhibitors: (e.g., crisaborole) A newer class of non-steroidal topical medications that reduce inflammation by inhibiting phosphodiesterase-4. Used for mild to moderate Atopic dermatitis.
- Anti-Itch Therapies:
- Oral Antihistamines: Sedating antihistamines (e.g., hydroxyzine, diphenhydramine) can be used at night to help with sleep disruption caused by severe itching. Non-sedating antihistamines are generally not effective for the itch of Atopic dermatitis.
- Cool Compresses: Applying cool, damp cloths to itchy areas can provide temporary relief.
- Menthol or Pramoxine-containing Lotions: Can provide immediate, temporary itch relief.
- Infection Control:
- Antibiotics: Oral or topical antibiotics are used to treat secondary bacterial infections (e.g., Staphylococcus aureus) which often colonize eczematous skin and contribute to flares (impetiginization, seen as crusting in weeping eczema images).
- Antiviral Agents: If eczema herpeticum (HSV infection) is suspected, oral antiviral medications are critical.
- Antifungal Agents: Used if concurrent fungal infections are present, particularly in skin folds.
- Systemic Therapies (for severe/refractory AD):
- Oral Corticosteroids: Used for severe, widespread flares, but typically for short courses due to significant side effects with prolonged use. They rapidly reduce inflammation.
- Immunosuppressants: (e.g., cyclosporine, methotrexate, azathioprine, mycophenolate mofetil) Used for long-term control of severe Atopic dermatitis that is unresponsive to topical therapies. These medications suppress the overall immune response.
- Biologics: (e.g., dupilumab, tralokinumab) Injectable medications that target specific components of the immune system responsible for the inflammation in Atopic dermatitis. They offer effective and targeted treatment for moderate to severe AD and have revolutionized management for many patients.
- JAK Inhibitors: (e.g., upadacitinib, abrocitinib) Oral medications that target Janus kinase pathways involved in inflammation. Also used for moderate to severe Atopic dermatitis.
- Phototherapy:
- Narrowband Ultraviolet B (NB-UVB): Exposure to specific wavelengths of UV light under medical supervision can reduce inflammation and itching. It is an option for moderate to severe Atopic dermatitis when topical treatments are insufficient.
- Trigger Avoidance and Lifestyle Modifications:
- Identify and Avoid Triggers: Common triggers include certain foods (in some individuals, especially infants), dust mites, pet dander, pollen, harsh soaps, detergents, fragrances, wool, cigarette smoke, and stress. Trigger avoidance is crucial in preventing flares.
- Stress Management: Stress can exacerbate Atopic dermatitis; techniques like mindfulness, meditation, and exercise can be beneficial.
- Protective Clothing: Wearing soft, breathable cotton clothing can prevent irritation.
- Maintain Comfortable Room Temperature and Humidity: Extreme temperatures and low humidity can dry out the skin.
The comprehensive management of Atopic dermatitis treatment requires a tailored approach that integrates these various strategies. Regular follow-up with a dermatologist is essential to adjust treatments based on the patient’s response and evolving symptoms. Education about the condition, proper skin care techniques, and medication use empowers patients to effectively manage their disease and improve their skin’s appearance, moving beyond the challenging visuals seen in eczema symptoms pictures to healthier, more comfortable skin.