This detailed guide explores what does Dermatofibroma look like symptoms pictures, offering an in-depth visual and descriptive overview of this common benign skin lesion. Understanding its characteristic appearance and associated symptoms is crucial for proper identification and effective management strategies for dermatofibroma patients.
Dermatofibroma Symptoms Pictures
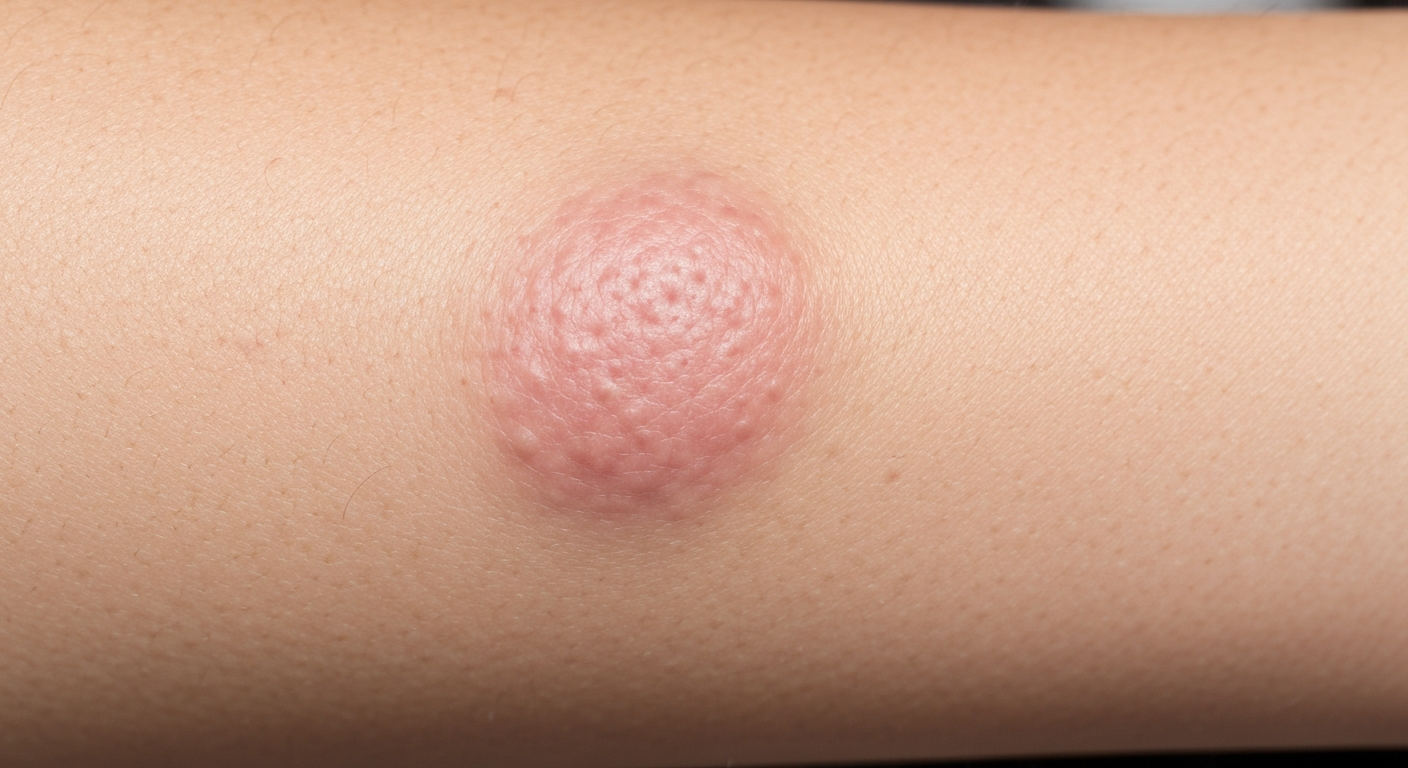
Dermatofibroma is a prevalent, benign skin growth, typically presenting as a firm, raised bump that can vary significantly in its exact visual characteristics and accompanying symptoms. When seeking to understand what dermatofibroma looks like, it’s essential to consider a range of presentations across different individuals and skin types. These lesions, also known as fibrous histiocytomas, are most frequently observed on the lower legs, but can emerge anywhere on the body, including the arms, upper back, and less commonly, the trunk or head.
The primary visual characteristics of dermatofibroma often include:
- Size: Typically, a dermatofibroma measures between 0.5 to 1.5 centimeters in diameter, though smaller or larger variants are not uncommon. Some may be as small as a pencil eraser, while others can reach the size of a thumbnail or even larger, creating a more prominent skin lesion.
- Shape: Most dermatofibromas are dome-shaped, resembling a small, firm button embedded within or on top of the skin. They can also appear somewhat flattened or slightly raised, with well-defined borders that separate them from the surrounding healthy skin. The surface can sometimes be slightly irregular, but is generally smooth.
- Coloration: The color of a dermatofibroma is highly variable, making it one of the most intriguing aspects for those examining dermatofibroma pictures. Common colors include:
- Flesh-toned: Some dermatofibromas may blend in with the surrounding skin, appearing as a slightly raised, firm bump without significant color deviation, especially in lighter skin tones.
- Pink to Red: Inflamed or recently developed dermatofibromas often present with a reddish or pinkish hue, which can sometimes lead to confusion with other inflammatory skin conditions.
- Brown to Dark Brown: This is a very common presentation, particularly in individuals with darker skin tones or those exposed to significant sun. The brown pigmentation can range from light tan to a very dark, almost black appearance, raising concerns about melanocytic lesions.
- Purple to Grey: Less frequently, dermatofibromas can have a purplish or grayish tint, especially if there’s an older lesion or if it contains hemosiderin deposits from previous microtrauma.
- Mottled Appearance: Some lesions may exhibit a combination of these colors, presenting with a mottled or variegated appearance that adds to their diagnostic complexity.
- Texture: A defining characteristic visible in dermatofibroma photos is their texture. They are almost invariably firm to hard when palpated, often described as feeling like a small pebble or rubbery knot beneath the skin. This firmness is due to the dense fibrous tissue and histiocytes that compose the lesion.
- Surface: The surface of a dermatofibroma is typically smooth and shiny. However, it can sometimes become slightly scaly or crusted if subjected to repeated irritation, scratching, or trauma, which might alter its initial characteristic appearance.
Beyond the visual cues, dermatofibromas can also be associated with a range of subjective symptoms:
- Asymptomatic: Many dermatofibromas cause no symptoms at all and are discovered incidentally. They are simply a cosmetic concern for the individual. This lack of symptoms can sometimes make early detection challenging, as they might go unnoticed until they reach a more prominent size or color.
- Itching (Pruritus): Itching is one of the most common symptoms reported. The sensation can range from a mild, occasional itch to persistent and bothersome pruritus, especially if the lesion is located in an area prone to friction or irritation from clothing. The exact mechanism for itching in dermatofibromas is not fully understood, but it may be related to inflammatory cells within the lesion.
- Tenderness or Pain: Some individuals experience tenderness or localized pain when pressure is applied to the dermatofibroma, or even spontaneously. This symptom can become more pronounced if the lesion is irritated, bumped, or in a high-friction area. The presence of nerve endings within the fibrous tissue can contribute to this discomfort.
- Bleeding: While uncommon unless traumatized, a dermatofibroma can bleed if scratched vigorously, picked at, or if it experiences significant friction. This bleeding is usually minor and localized but can be a source of concern.
- Changes with Temperature: Some patients report that their dermatofibroma feels more prominent or symptomatic in cold weather or changes slightly in appearance with temperature fluctuations, though this is less commonly reported.
Understanding these comprehensive symptoms and visual characteristics is key to recognizing a dermatofibroma, especially when reviewing various dermatofibroma pictures or examining a suspected lesion on the skin.
Signs of Dermatofibroma Pictures
Recognizing the specific signs of dermatofibroma involves not only observing its static appearance but also understanding how it reacts to manipulation and its typical behavior over time. These dynamic signs are often crucial for clinical diagnosis, even before considering advanced imaging or biopsy. The characteristic features consistently observed in dermatofibroma images and during physical examination greatly aid in distinguishing this benign entity from more concerning skin growths.
Key diagnostic signs frequently highlighted in examinations include:
- The Dimple Sign (Fitzpatrick’s Sign): This is arguably the most classic and reliable clinical sign of a dermatofibroma. When lateral pressure is applied to the edges of the lesion, or when the skin surrounding the dermatofibroma is squeezed between the thumb and forefinger, the central portion of the lesion often invaginates or “dimples” inwards. This unique phenomenon occurs because the fibrous tissue of the dermatofibroma is tethered to the underlying dermis, pulling the surface skin inwards when compressed. The dimple sign is a strong indicator, frequently visible in dermatofibroma photos specifically demonstrating this maneuver, and serves as a critical differentiator from other skin lesions that typically protrude when squeezed.
- Firmness and Immovability: Unlike cysts or lipomas which might feel softer or more mobile, a dermatofibroma feels distinctly firm and rubbery, almost like a cartilaginous mass. It often feels like it’s firmly anchored within the skin layers, rather than being superficial or easily movable. This deep-seated firmness is a consistent sign across various dermatofibroma types.
- Well-Demarcated Borders: Despite being embedded, dermatofibromas usually have relatively clear and distinct borders when palpated or closely inspected. While not always sharply raised like a wart, the edge of the lesion often feels discernible from the surrounding healthy skin. This helps in understanding the lesion’s extent.
- Location Predilection: While dermatofibromas can appear anywhere, a strong predilection for the lower legs and arms is a significant diagnostic sign. If a firm, pigmented nodule is found in these areas, especially in adults, dermatofibroma should be high on the differential diagnosis list. Observing the lesion in context of its common anatomical sites enhances diagnostic accuracy when reviewing dermatofibroma pictures.
- Slow Growth and Stability: Dermatofibromas are typically slow-growing lesions. Once they appear, they often grow slowly over months or years to a certain size and then remain stable for an extended period, sometimes for decades. Rapid growth or significant changes in shape or color are uncommon and should prompt further investigation to rule out other conditions. This stability is a reassuring sign for patients and clinicians alike.
- Multiple Lesions: While usually solitary, some individuals may develop multiple dermatofibromas. This is more common in individuals with compromised immune systems, autoimmune diseases (e.g., lupus, Crohn’s disease), or those receiving certain medications (e.g., immunosuppressants). The presence of numerous similar lesions can be a diagnostic clue, pointing towards a systemic association, which is an important consideration for specialists examining extensive skin rash dermatofibroma images or widespread presentations.
Further elaborations on appearance variations that act as key signs:
- Hypopigmented Halo (rare): Occasionally, a dermatofibroma might be surrounded by a thin rim of lighter skin, a phenomenon less common but observed. This can contribute to its unique visual fingerprint.
- Hyperkeratotic Surface (less common): While typically smooth, some dermatofibromas, especially those subjected to chronic rubbing or irritation, can develop a slightly scaly or thickened (hyperkeratotic) surface. This can alter their typical smooth texture seen in most dermatofibroma pictures.
- Epidermal Changes: Histologically, the epidermis overlying a dermatofibroma often shows changes such as basal layer hyperpigmentation, hyperplasia, and elongation of rete ridges, which can contribute to the lesion’s varied surface pigmentation and texture. These micro-level signs inform the macroscopic appearance.
- Vascular Component: Some dermatofibromas have a more pronounced vascular component, making them appear redder or violaceous. This can be a sign of increased blood supply within the lesion, which might make them more prone to bleeding if traumatized.
The combination of these visual and palpable signs, especially the dimple sign and the firm, tethered nature of the lesion, provides a strong basis for the clinical diagnosis of dermatofibroma. When these characteristic signs are present, the need for further invasive diagnostics like biopsy can sometimes be minimized, though it remains an option for atypical or symptomatic lesions.
Early Dermatofibroma Photos
Identifying dermatofibroma in its early stages can sometimes be challenging due to its often subtle initial presentation, which can mimic a variety of other minor skin imperfections. Unlike a full-blown, characteristic lesion often seen in diagnostic textbooks, early dermatofibroma photos might show a much less pronounced skin alteration. Understanding these nascent signs is crucial for both self-assessment and clinical vigilance. The evolution from an indistinct spot to a clearly identifiable nodule occurs gradually, and recognizing the preliminary phases can provide peace of mind or prompt timely consultation if warranted.
Typical appearances of an early dermatofibroma include:
- Small, Indistinct Spot: Initially, a dermatofibroma may begin as a very small, almost unnoticeable bump or discolored area, often only a few millimeters in size. It might be mistaken for:
- An insect bite that never fully resolves.
- A small pimple or acne lesion that persists.
- An ingrown hair bump that feels unusually firm.
- A minor bruise or a localized patch of hyperpigmentation.
The lack of immediate growth or significant symptoms often means these initial lesions go unnoticed.
- Subtle Discoloration: In its earliest phase, the lesion might present as a faint reddish, pinkish, or light brown spot. The color can be very mild and blend in with the surrounding skin, making it difficult to discern without close inspection. This initial pigmentation can gradually darken over time as the fibrous tissue proliferates and melanocytes become more active in the overlying epidermis.
- Slightly Raised or Flat Papule: Rather than a pronounced dome, an early dermatofibroma might just be a slightly elevated papule that barely breaks the skin’s surface. In some cases, it may initially feel more like a small, firm area within the skin rather than a distinctly raised bump, making it more palpable than visible. This subsurface firmness is a key early clue.
- Lack of Prominent Symptoms: At its onset, an early dermatofibroma is typically asymptomatic. There’s usually no itching, pain, or tenderness associated with it, which can contribute to its delayed discovery. Any symptoms, such as mild itching, usually develop as the lesion becomes more established and larger.
- Slow, Gradual Development: The progression from an early, subtle lesion to a more characteristic dermatofibroma is often very slow. It might take months or even years for the lesion to reach its typical size and develop its hallmark firmness and dimple sign. This gradual nature is a key feature distinguishing it from rapidly evolving skin cancers or inflammatory reactions.
Factors that influence the appearance of early dermatofibroma:
- Skin Type: In lighter skin tones, an early dermatofibroma might appear as a faint pink or reddish spot, whereas in darker skin types, it might manifest as a subtle brown or hyperpigmented patch. The contrast against the surrounding skin can vary significantly.
- Location: Lesions in areas of frequent friction or sun exposure (e.g., lower legs) might develop more distinct pigmentation or slight irritation earlier than those in protected areas.
- Underlying Factors: While not fully understood, some theories suggest that early dermatofibromas might develop in response to minor trauma, insect bites, or even folliculitis. Therefore, an early lesion might appear at the site of a resolving inflammatory reaction.
When examining early dermatofibroma photos, one should look for these nascent characteristics – the subtle bump, the initial discoloration, and the firm feel upon gentle palpation. While these early signs are often non-specific, their persistence and slow progression, especially if they begin to develop the characteristic dimple sign, are strong indicators of a developing dermatofibroma. Any rapidly changing, bleeding, or painful early lesion should always be evaluated by a healthcare professional to rule out more serious conditions.
Skin rash Dermatofibroma Images
It is crucial to clarify that a dermatofibroma is fundamentally a solitary, benign nodule or papule, and not a generalized “skin rash.” The term “rash” implies a widespread eruption of lesions, often inflammatory, itchy, or spreading across a larger skin area, characteristic of conditions like eczema, psoriasis, or allergic reactions. A dermatofibroma, by contrast, is a localized growth. However, there are scenarios where individuals might associate a dermatofibroma with a “rash,” or its presentation might, in rare circumstances, be misinterpreted as part of a broader skin condition when viewing skin rash dermatofibroma images.
Understanding why a dermatofibroma might be confused with or appear in the context of a “rash”:
- Multiple Dermatofibromas: While typically solitary, some individuals, particularly those with underlying autoimmune conditions (e.g., systemic lupus erythematosus, Crohn’s disease), immunosuppression, or certain genetic predispositions, can develop multiple dermatofibromas. If these multiple lesions are numerous and spread across a body area, they might superficially resemble a widespread eruption or a chronic inflammatory skin condition, leading to the impression of a “rash.” However, even in such cases, each individual lesion retains the characteristic features of a dermatofibroma (firmness, dimple sign, typical coloration).
- Inflamed or Irritated Dermatofibroma: A dermatofibroma can become inflamed, especially if it’s located in an area prone to friction (e.g., waistline, bra line, lower legs where clothing rubs), or if it’s repeatedly scratched, picked, or traumatized. An inflamed dermatofibroma will present with:
- Increased Redness: The lesion becomes noticeably redder or more erythematous than its baseline color.
- Tenderness and Pain: It may become exquisitely tender or painful to touch, mimicking the acute pain of an inflamed rash lesion.
- Swelling: There might be localized swelling around the lesion, making it appear more prominent.
- Itching: Pre-existing itching might intensify, or new itching might develop.
- Crusting or Ulceration: In cases of severe trauma or persistent irritation, the surface of the dermatofibroma can become excoriated, crusted, or even ulcerated, resembling an infected or severely inflamed patch of skin.
These inflammatory signs can cause a single dermatofibroma to stand out dramatically against the surrounding skin, and if multiple lesions are inflamed, the overall impression could be confused with a localized “rash-like” reaction.
- Coexistence with Other Skin Conditions: It is possible for a dermatofibroma to simply coexist on the skin of an individual who also has a genuine skin rash (e.g., eczema, contact dermatitis, psoriasis). In such scenarios, the distinct dermatofibroma might be inadvertently captured within skin rash dermatofibroma images or described as part of the wider skin problem. Clinicians must differentiate between the two entities to ensure proper diagnosis and treatment of both.
- Post-Inflammatory Hyperpigmentation: Occasionally, a dermatofibroma might develop in an area that previously experienced inflammation or trauma, leading to post-inflammatory hyperpigmentation around or on the lesion. This could contribute to a mottled, discolored appearance that might be superficially misconstrued as part of a generalized pigmentary rash.
Differentiating Dermatofibroma from True Rashes:
- Consistency: Rashes are typically soft, pliable, or flaky, whereas a dermatofibroma is consistently firm or hard.
- Dimple Sign: The dimple sign is exclusive to dermatofibromas; true rashes do not exhibit this characteristic retraction upon squeezing.
- Evolution: Rashes tend to evolve rapidly, often with spreading patterns or new lesions appearing over days to weeks. Dermatofibromas are slow-growing and stable for long periods.
- Surface Characteristics: Rashes often have characteristic surface changes like vesicles, pustules, papules, plaques, scaling, or weeping, which are not typical for an untouched dermatofibroma.
Therefore, while you might encounter skin rash dermatofibroma images that show a dermatofibroma alongside other skin changes, it is critical to remember that the dermatofibroma itself is a distinct, benign fibrous tumor, not a spreading inflammatory rash. Any concerning skin lesion, particularly if it’s rapidly changing, bleeding spontaneously, or painful, should always be examined by a dermatologist to ensure accurate diagnosis and appropriate management.
Dermatofibroma Treatment
The management of dermatofibroma typically revolves around observation, symptomatic relief, or removal, depending on the patient’s concerns, the lesion’s characteristics, and diagnostic certainty. Since dermatofibromas are benign skin tumors and pose no health risk, active treatment is often not medically necessary. However, various factors lead individuals to seek dermatofibroma treatment, and understanding the available options is crucial for informed decision-making.
Reasons for Seeking Dermatofibroma Treatment:
- Cosmetic Concerns: This is by far the most common reason for treatment. Patients may find the appearance of the dermatofibroma visually unappealing, especially if it’s large, dark, or located on a prominent area like the face or lower legs. The desire for aesthetic improvement often drives the decision for removal.
- Symptomatic Lesions: If the dermatofibroma is persistently itchy, tender, or painful, particularly due to irritation from clothing, shaving, or repeated trauma, treatment becomes more medically indicated to alleviate discomfort and improve quality of life.
- Diagnostic Uncertainty: In some cases, the clinical appearance of a dermatofibroma may be atypical, making it difficult to definitively distinguish from other, potentially more serious skin lesions (e.g., melanoma, basal cell carcinoma, atypical fibroxanthoma). In such instances, excisional biopsy (complete removal with subsequent pathological examination) is performed primarily for diagnostic confirmation. This ensures that a correct diagnosis is made and appropriate follow-up, if any, is established.
- Recurrent Trauma/Bleeding: If the dermatofibroma is frequently traumatized or bleeds due to its location or individual habits, removal can prevent ongoing issues.
Common Dermatofibroma Treatment Options:
1. Observation (Watchful Waiting):
- Description: For asymptomatic and diagnostically straightforward dermatofibromas that are not causing any bother, observation is the most common and often recommended approach. No intervention is necessary.
- Benefits: Avoids scars, risks of surgery, and recovery time.
- Considerations: Requires patients to be comfortable with the lesion’s presence and appearance. Regular self-checks for any changes are advisable, although significant changes are rare.
2. Surgical Excision:
- Description: This involves surgically cutting out the entire dermatofibroma with a small margin of surrounding healthy skin. The wound is then closed with sutures. This is considered the definitive treatment for complete removal and provides tissue for histological confirmation.
- Procedure Details:
- Performed under local anesthesia in an outpatient setting.
- Involves precise removal of the lesion and a small amount of underlying tissue to prevent recurrence.
- Requires suturing to close the wound, leading to a linear scar.
- Benefits:
- Complete Removal: Ensures the entire lesion, including its deeper components, is removed, minimizing recurrence risk.
- Histological Confirmation: Provides tissue for microscopic examination by a pathologist, offering a definitive diagnosis, which is particularly important for atypical lesions or when diagnostic uncertainty exists.
- Symptom Resolution: Effectively eliminates symptoms like itching or pain.
- Considerations:
- Scarring: Will inevitably leave a permanent linear scar, which might be more noticeable than the lesion itself, especially on areas with tension or poor healing. Scar appearance varies by individual, location, and surgical technique.
- Recovery Time: Requires wound care, suture removal (if non-dissolvable), and avoidance of strenuous activities for a period.
- Potential Complications: Minor risks include infection, bleeding, nerve damage (rare), and keloid or hypertrophic scar formation.
3. Shave Excision:
- Description: Involves using a surgical blade to “shave” off the raised portion of the dermatofibroma, leaving the deeper parts of the lesion in situ. This technique aims to flatten the lesion.
- Benefits:
- Minimally Invasive: Less invasive than full excision, resulting in a flatter, less prominent scar (often a flat, round, hypopigmented or hyperpigmented patch).
- Quicker Healing: The wound typically heals by secondary intention (like an abrasion), often faster than a sutured wound.
- Cosmetic Improvement: Can significantly improve the lesion’s prominence for cosmetic reasons.
- Considerations:
- Higher Recurrence Risk: Since the deeper parts of the dermatofibroma are not removed, there is a higher chance of recurrence or regrowth of the lesion.
- Diagnostic Limitations: The removed tissue may not be fully representative for comprehensive histological assessment if diagnostic uncertainty is high.
- Scarring: While flatter, a discoloration or textural change will still be present.
4. Cryotherapy (Freezing):
- Description: Involves applying liquid nitrogen to freeze and destroy the cells of the dermatofibroma. This method is generally used to flatten the lesion and reduce symptoms.
- Benefits:
- Non-Invasive: Does not involve cutting or sutures.
- Minimal Downtime: Generally quick procedure with little to no recovery time beyond blister care.
- Reduces Size and Symptoms: Can flatten the lesion and alleviate itching or tenderness.
- Considerations:
- Limited Efficacy for Full Removal: Seldom achieves complete destruction of the lesion, leading to a high rate of recurrence or persistence.
- Hypopigmentation/Hyperpigmentation: Can cause temporary or permanent lightening (hypopigmentation) or darkening (hyperpigmentation) of the treated skin, which can be more noticeable in darker skin types.
- Blistering: The freezing process causes a blister, which needs to be managed during healing.
- Multiple Sessions: May require several treatment sessions to achieve desired results.
5. Laser Therapy:
- Description: Various lasers (e.g., CO2 laser, pulsed dye laser) can be used to treat dermatofibromas, primarily targeting vascular components, ablating tissue, or improving texture and color.
- Benefits:
- Precision: Allows for very precise tissue removal or modification.
- Reduced Bleeding: Some lasers coagulate blood vessels, minimizing bleeding during the procedure.
- Improved Cosmesis: Can improve the color and texture of the lesion, especially for reddish or purplish variants.
- Considerations:
- Limited Penetration: Deeply embedded dermatofibromas may not be fully amenable to laser treatment for complete removal.
- Cost: Can be more expensive than other methods.
- Potential Side Effects: Risks include scarring, dyspigmentation, and prolonged redness.
- Recurrence: Similar to shave excision and cryotherapy, complete eradication of the deep fibrous component can be challenging.
6. Intralesional Corticosteroid Injections:
- Description: Injecting corticosteroids directly into the dermatofibroma can sometimes help to reduce its size, flatten it, and alleviate symptoms like itching or inflammation, especially for tender or inflamed lesions.
- Benefits:
- Non-Surgical: A less invasive approach.
- Symptomatic Relief: Effective for reducing inflammation, itching, and tenderness.
- Considerations:
- Temporary Effect: The effects are often temporary, and the lesion may return to its original state once the steroid wears off.
- Skin Atrophy: Repeated injections can lead to skin thinning (atrophy) or hypopigmentation at the injection site.
- Not for Complete Removal: Does not remove the lesion but rather reduces its prominence and symptoms.
Important Considerations for Dermatofibroma Treatment:
- Consultation with a Dermatologist: Always seek advice from a qualified dermatologist. They can accurately diagnose the lesion, discuss the pros and cons of each treatment option in relation to your specific dermatofibroma, and help set realistic expectations regarding scarring and recurrence.
- Scarring: It is crucial to understand that any invasive treatment of a dermatofibroma will result in some form of scar. The goal is often to replace the dermatofibroma with a less noticeable or more cosmetically acceptable scar.
- Recurrence: While surgical excision offers the lowest recurrence rate, it’s not zero. For less invasive methods like shave excision or cryotherapy, the recurrence rate is higher because the entire fibrous base is often not removed.
In conclusion, while dermatofibromas are benign, their management options are diverse and should be chosen based on individual patient needs, cosmetic desires, symptom severity, and diagnostic requirements. A clear understanding of dermatofibroma treatment pathways empowers patients to make the best decisions for their skin health and well-being.