The visual identification of Liver cirrhosis symptoms pictures can be a critical step in early recognition and intervention for this chronic liver condition. Understanding the diverse spectrum of manifestations, from subtle skin changes to profound systemic alterations, is vital for both medical professionals and individuals seeking to comprehend the implications of advanced liver disease. This comprehensive overview aims to meticulously detail the myriad symptoms and signs observed in liver cirrhosis, emphasizing their visual characteristics.
Liver cirrhosis Symptoms Pictures
Recognizing Liver cirrhosis symptoms pictures involves a keen eye for both subtle and overt physical changes that signal severe hepatic dysfunction. These manifestations stem from the liver’s inability to perform its essential functions, leading to systemic impacts. One of the most frequently observed and visually striking symptoms is jaundice, characterized by a yellowish discoloration of the skin and the whites of the eyes (sclera). This occurs due to the accumulation of bilirubin, a yellow pigment, in the blood, which the damaged liver can no longer process efficiently. In images, jaundice can range from a pale lemon-yellow hue to a deep orange or even greenish tint, particularly noticeable in natural light. The intensity often correlates with the severity of liver impairment. Beyond the skin and eyes, other mucous membranes may also exhibit this discoloration, though less commonly captured in typical photographs.
Another common visual indicator of liver cirrhosis is the presence of spider angiomas, also known as spider nevi or vascular spiders. These are small, bright red lesions characterized by a central arteriole surrounded by numerous radiating, fine capillaries, resembling a spider’s web or a star. They are typically found on the upper body, specifically on the face, neck, upper chest, and arms. In cirrhosis visual signs, spider angiomas develop due to increased estrogen levels, which the cirrhotic liver fails to metabolize. Their size can vary from a pinhead to over a centimeter in diameter, and they blanch upon central pressure, refilling from the center outwards when pressure is released. The presence of multiple spider angiomas often signifies significant liver damage. A high number of these lesions, particularly more than five, can be a strong diagnostic clue, often captured effectively in hepatic dysfunction symptoms imagery.
Palmar erythema is another dermatological manifestation frequently associated with liver cirrhosis, visible in cirrhosis symptoms pictures. This condition presents as a reddening of the palms, particularly affecting the thenar and hypothenar eminences (the fleshy bases of the thumb and little finger) and the fingertips. Unlike a generalized flush, the central part of the palm often remains pale. The redness is typically symmetrical and non-itchy, resulting from altered estrogen metabolism and peripheral vasodilation. While it can also be seen in pregnancy, rheumatoid arthritis, and hyperthyroidism, its occurrence in the context of other liver-related symptoms strongly suggests cirrhosis. The redness can vary in intensity, from a subtle pinkish tinge to a vivid crimson, creating a stark visual contrast that is often evident in photographic documentation.
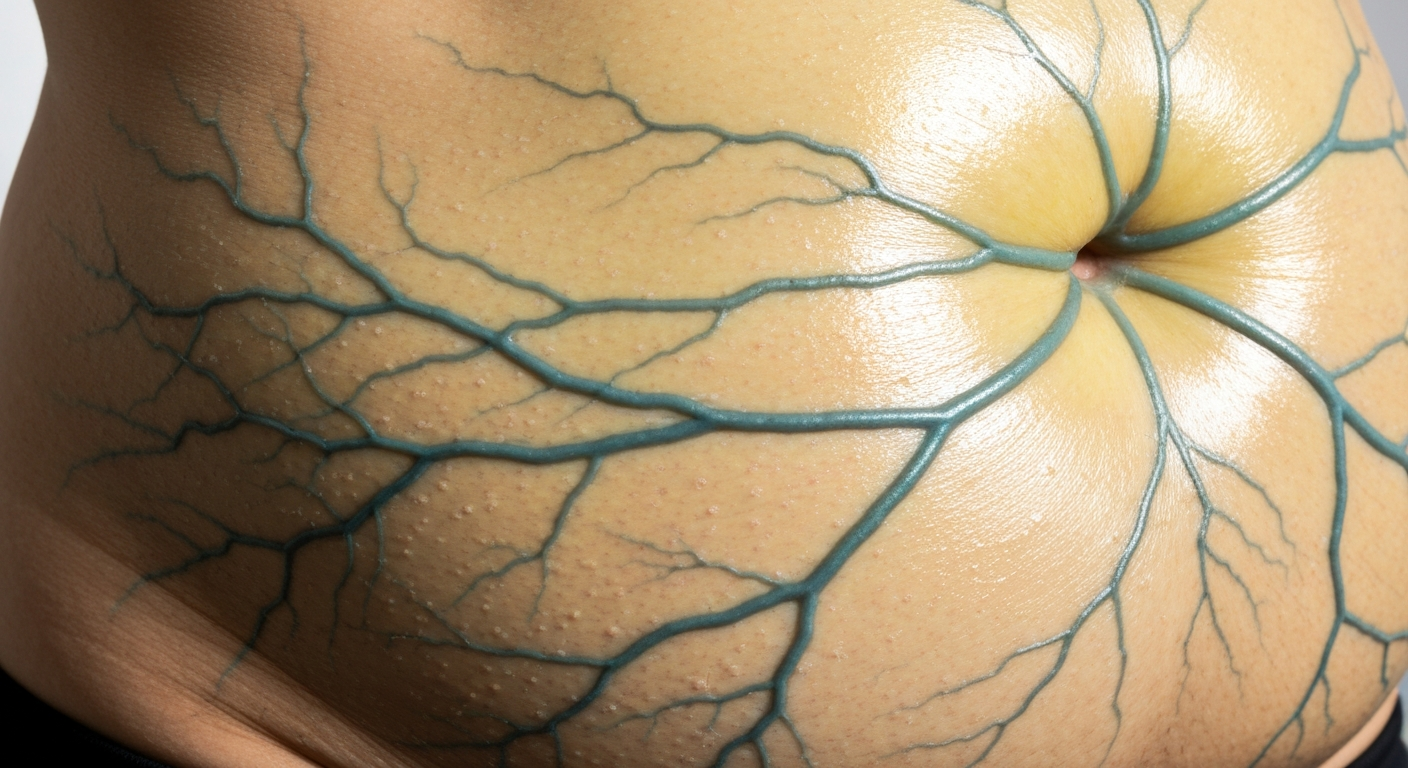
Accumulation of fluid, known as ascites, is a hallmark of decompensated liver cirrhosis and profoundly alters the patient’s physical appearance, making it a prominent feature in liver disease symptoms photos. Ascites manifests as a noticeable distension of the abdomen, which can range from mild bloating to a massively swollen belly, often described as “pot-bellied.” The skin over the distended abdomen may appear taut and shiny. In advanced cases, the abdominal wall might develop visible superficial veins, known as caput medusae, radiating outwards from the umbilicus, due to portal hypertension. Patients with ascites may also experience discomfort, shortness of breath due to diaphragmatic elevation, and weight gain. Visual representation often captures the sheer size difference compared to the limbs, highlighting muscle wasting in other areas of the body. The presence of a fluid wave, though a physical examination finding, can be inferred visually by the degree of abdominal turgidity and symmetry.
Peripheral edema, another form of fluid retention, is commonly observed in the lower extremities, particularly the ankles and feet. This swelling, also known as pitting edema, is caused by low albumin levels (due to impaired liver synthesis) and increased hydrostatic pressure. When pressed, the swollen area temporarily retains an indentation, a characteristic that can sometimes be inferred from the texture and sheen of the skin in cirrhosis visual signs. In images, the affected limbs appear noticeably enlarged and puffy, often lacking definition around the bony prominences. The skin over the edematous areas may look stretched and shiny. In severe cases, edema can extend to the thighs and even the sacral region, particularly in bedridden patients. The combination of ascites and peripheral edema often presents a striking picture of fluid overload in hepatic cirrhosis manifestations.
Muscle wasting or sarcopenia is a significant and often visually apparent symptom of advanced liver cirrhosis. It involves the progressive loss of muscle mass, particularly in the temporal muscles (sides of the head), shoulders, arms, and thighs. This can lead to a gaunt appearance, with prominent bones and sunken features, contrasting sharply with the fluid retention in the abdomen and limbs. In liver cirrhosis symptoms pictures, this catabolic state is evident through visibly reduced muscle bulk, making limbs appear thin and frail. The severity of muscle wasting is an important prognostic indicator and is often exacerbated by malnutrition and altered protein metabolism inherent to severe liver disease. This skeletal muscle atrophy is not just a cosmetic concern but directly impacts strength, mobility, and overall quality of life for individuals grappling with end-stage liver disease.
Changes in the nails can also provide visual clues for cirrhosis visual signs. Terry’s nails are a classic sign, characterized by an opaque, whitish ground-glass appearance of almost the entire nail, with a narrow, distinct reddish-brown band at the tip. This is thought to be due to reduced vascularity and increased connective tissue in the nail bed. While not exclusive to liver disease, they are frequently observed in advanced cirrhosis. Another less common but notable nail change includes clubbing of the fingers, where the fingertips and nails show an increased curvature and bulbous appearance, often accompanied by soft tissue swelling at the base of the nail. This is usually associated with chronic hypoxia but can be seen in advanced cirrhosis. Muehrcke’s lines, characterized by paired, white, transverse lines separated by areas of normal pink nail bed, are also sometimes seen, indicative of hypoalbuminemia. Each of these unique nail presentations contributes to the comprehensive visual assessment in hepatic dysfunction symptoms.
Beyond these primary visual changes, other less frequent but equally impactful symptoms captured in Liver cirrhosis symptoms pictures include purpura and ecchymoses. These manifest as purple-red spots or larger bruises on the skin, resulting from impaired synthesis of clotting factors by the diseased liver and platelet dysfunction. They often appear without significant trauma and highlight the increased bleeding risk associated with advanced chronic liver disease. The discoloration can vary from fresh red-purple to older yellowish-brown, indicating different stages of healing. These visual cues serve as vital indicators for patients and healthcare providers monitoring the progression of liver damage and its systemic complications. The cumulative impact of these symptoms creates a compelling and often somber visual narrative of advanced hepatic cirrhosis.
Signs of Liver cirrhosis Pictures
The Signs of Liver cirrhosis Pictures category delves deeper into the objective findings often identified during a physical examination, many of which have distinct visual characteristics indicative of advanced liver disease. These signs complement the subjective symptoms and provide crucial diagnostic information. As mentioned previously, caput medusae is a pathognomonic sign, visually striking and highly suggestive of severe portal hypertension, a common complication of cirrhosis. It appears as dilated, tortuous superficial veins radiating outwards from the umbilicus across the abdomen, resembling the head of Medusa from Greek mythology. This occurs as collateral circulation develops to bypass the obstructed portal venous system. The presence of this sign is a clear visual marker of significant liver disease progression and is readily captured in clinical photography, emphasizing the severity of portal hypertension in hepatic cirrhosis manifestations.
Scleral icterus refers specifically to the yellowing of the sclera (the white part of the eye). While jaundice describes generalized yellowing, scleral icterus is particularly pronounced and often easier to discern than skin discoloration, especially in individuals with darker skin tones. In liver disease signs pictures, the bright yellow hue of the sclera against the iris is unmistakable and provides a clear visual cue of elevated serum bilirubin levels, directly reflecting the liver’s impaired ability to conjugate and excrete bilirubin. This sign is a critical indicator for healthcare providers and is often among the first visual signs prompting further investigation into potential liver damage.
Clubbing of fingers, also known as digital clubbing, is a condition characterized by a distinctive change in the shape of the fingers and toenails, wherein the nail beds soften, the nails appear to float, and the fingertips become bulbous and enlarged. The angle between the nail and the nail bed increases beyond 180 degrees (Lovibond’s angle). While not exclusive to liver cirrhosis, it is a recognized sign, particularly in advanced stages, and is associated with chronic hypoxemia or other chronic systemic diseases. In cirrhosis physical examination photos, clubbing presents as a distinct rounded and broadened appearance of the distal phalanges, often described as having a “drumstick” appearance. This visual change, when present, can be a subtle but significant indicator of underlying hepatic dysfunction and systemic complications of chronic liver disease.
In male patients with liver cirrhosis, gynecomastia (enlargement of breast tissue) and testicular atrophy are common endocrine manifestations due to the cirrhotic liver’s inability to metabolize estrogen effectively, leading to elevated circulating estrogen levels. Gynecomastia presents as palpable and often visible breast enlargement, which can be unilateral or bilateral. In liver disease signs images, this can range from a subtle increase in breast tissue to a more pronounced, breast-like development. Testicular atrophy, on the other hand, involves a reduction in the size of the testicles, which may be less obvious visually in general photos but is a critical finding during a physical exam and can be inferred from patient posture or specific close-up images if available. These hormonal imbalances underscore the widespread systemic effects of advanced liver disease beyond just metabolism and detoxification, profoundly affecting the patient’s physical appearance and endocrine health.
Terry’s nails, as previously detailed, are significant for their striking visual appearance. The characteristic opaque white nail plate with a distal red-brown band is a strong visual marker. Similarly, Muehrcke’s lines, presenting as double white transverse bands, and leukonychia (whitening of the nails), which can be partial or complete, are also recognized as hepatic cirrhosis manifestations. These nail changes, while often subtle, are important because they can be easily overlooked but offer persistent visual evidence of chronic systemic illness. Documenting these in cirrhosis physical examination photos can aid in diagnosis and monitoring, providing a non-invasive indicator of the body’s response to liver damage. The appearance of these specific nail patterns provides additional layers of visual diagnostic information, critical for a comprehensive assessment of the cirrhotic patient.
Other physical examination signs that can be visually inferred or documented include xanthelasmas or xanthomas. These are yellowish, cholesterol-rich deposits that appear as plaques or nodules on the skin, particularly around the eyelids (xanthelasmas) or on extensor surfaces, palms, soles, and buttocks (xanthomas). They are indicative of hyperlipidemia, often associated with cholestatic liver diseases that can lead to cirrhosis, such as primary biliary cholangitis. In liver disease signs pictures, these lesions are clearly visible as raised, distinct yellowish areas, offering a visual clue to the underlying metabolic disturbances related to hepatic dysfunction. The presence of these lipid deposits, particularly around the eyes, can be a very visible and often aesthetic concern for patients, further highlighting the systemic impact of cirrhosis.
The overall appearance of a patient with advanced cirrhosis often conveys a sense of chronic illness and cachexia. The combination of muscle wasting, ascites, jaundice, and other visible signs can result in a distinctive physical presentation. Facial features may appear gaunt with sunken eyes, and the skin may have a sallow, jaundiced, or even grayish tint. The presence of hepatic fetor, a sweet, musty odor on the breath, while not a visual sign, is a powerful olfactory indicator of severe liver failure and hepatic encephalopathy. Although not picture-based, the sum of these physical findings, often conveyed through general patient photography, paints a compelling picture of the profound impact of decompensated cirrhosis. Each of these objective signs, when compiled, contributes to a comprehensive visual understanding of the complex array of cirrhosis manifestations.
Early Liver cirrhosis Photos
Identifying Early Liver cirrhosis Photos can be challenging because initial symptoms are often subtle, non-specific, and may not present with dramatic visual changes. However, even in the early stages of liver damage, there are nascent signs that, when recognized, can prompt earlier intervention. One of the most common early, though non-visual, symptoms is fatigue. While a picture cannot capture fatigue directly, patients in early stages of cirrhosis might exhibit a generally tired or drawn appearance, with subtle dark circles under their eyes or a lack of vibrancy in their complexion. This general malaise and reduced energy levels are often the first subjective complaints, making the patient look less robust than before. Such subtle shifts in appearance, when viewed in context, can be important in identifying initial liver damage signs.
Unexplained weight loss and a loss of appetite are early systemic indicators that can gradually alter a person’s appearance. As the liver’s metabolic functions begin to decline, individuals may start to lose lean muscle mass, leading to a leaner or more gaunt physique over time. While not as dramatic as the severe muscle wasting seen in advanced disease, early cirrhosis symptoms related to weight loss can be subtle but noticeable to close observers or when comparing serial photographs. Clothes might fit more loosely, and there might be a gradual reduction in body fat and muscle definition. These changes reflect the initial impact on nutritional status and metabolism, providing visual cues for pre-cirrhotic changes or early onset of hepatic fibrosis.
Subtle changes in body fluids can also occur in Early Liver cirrhosis Photos. While pronounced ascites is a late-stage sign, patients in early cirrhosis might experience mild, intermittent abdominal bloating or discomfort due to fluid shifts or mild portal hypertension. This can manifest as a slight distension of the abdomen, which might be more noticeable after meals or towards the end of the day. Such mild bloating might not be dramatic enough for a textbook photo of ascites but can still be an observable visual change for the patient or family members. Coupled with vague abdominal pain or tenderness, this physical sign contributes to the often insidious presentation of early liver disease.
Changes in urine and stool color, while not direct external visual signs on the patient’s body, are crucial early cirrhosis symptoms that can be visually depicted in a clinical setting through sample images. Dark urine, often described as tea-colored or cola-colored, occurs due to the excretion of excess bilirubin through the kidneys when the liver is unable to process it. Conversely, pale stools or clay-colored stools result from the lack of bilirubin in the bile, which normally gives stool its brown color, indicating a blockage or insufficient flow of bile from the liver. Patients may notice these striking color changes in the toilet bowl. These visual changes, though not on the skin, are powerful indicators of impaired bile flow and liver function, making them vital components of early liver damage signs to look out for.
Pruritus, or generalized itching, is another early and often distressing symptom in chronic liver disease, particularly in cholestatic liver conditions that can progress to cirrhosis. While itching itself isn’t directly visual, its consequences are. Persistent scratching can lead to excoriations (scratch marks), skin redness, and sometimes secondary skin infections. In early cirrhosis photos, one might observe subtle linear scratch marks on the skin, particularly on the limbs and trunk. The skin might also appear dry or irritated. These signs, while not pathognomonic, can be visual clues that point towards an underlying liver issue, especially when combined with other subtle symptoms. The presence of these skin changes can signify the initial stages of bile acid accumulation and skin irritation in hepatic fibrosis.
Even mild jaundice can be an early indicator. Unlike the pronounced yellowing of advanced cirrhosis, early jaundice might present as a very faint yellow tinge, particularly noticeable in the sclera or under the tongue. It might be intermittent or only apparent in certain lighting conditions. This subtle coloration can be challenging to capture accurately in a photograph without professional lighting and high resolution but is a crucial observation in initial liver damage signs. Patients or family members might notice a “washed out” or slightly yellow pallor before overt jaundice develops. This subtle discoloration often signifies that the liver’s capacity to process bilirubin is already being compromised, marking a significant step in the progression of liver dysfunction.
Finally, a general feeling of malaise and a decline in overall well-being, though subjective, can manifest in subtle alterations of a person’s demeanor and physical presentation. A lack of usual vibrancy, diminished facial expressions, or a generally less energetic posture can be subtle early cirrhosis symptoms. While these are not distinct lesions or discolorations, they contribute to the overall visual impression of someone who is unwell. Comparing “before and after” photos, if available, can sometimes reveal these gradual, non-specific changes that signal the insidious onset of early chronic liver disease. The challenge in documenting these early signs photographically lies in their subtlety, but their recognition is paramount for early diagnosis and management of hepatic fibrosis.
Skin rash Liver cirrhosis Images
The skin is often a mirror reflecting the internal state of the liver, and Skin rash Liver cirrhosis Images showcase a variety of dermatological manifestations beyond the classical jaundice and spider angiomas. These skin conditions can be diverse, ranging from direct effects of liver dysfunction to secondary complications. As previously mentioned, pruritus (itching) is a pervasive symptom, especially in cholestatic liver diseases. The intense, chronic itching leads to excoriations, which are linear scratch marks, often visible on the limbs and trunk. In cirrhosis skin problems images, these can range from faint red lines to deep, crusted lesions, indicating vigorous scratching. Over time, chronic scratching can also lead to lichenification – a thickening and hardening of the skin with exaggerated skin markings, resembling tree bark – which is clearly visible in affected areas.
Hyperpigmentation is another common dermatological change in patients with liver cirrhosis, particularly in cases of hemochromatosis or primary biliary cholangitis. This appears as a generalized darkening of the skin, often described as a bronzing or grayish-brown discoloration, especially in sun-exposed areas and skin folds. In hepatic dermatological manifestations photography, this change in skin tone can be striking and widespread, distinguishing it from simple tanning. It is believed to be due to increased melanin deposition and can significantly alter a person’s natural complexion, serving as a visual cue for underlying liver disease skin symptoms.
Xanthomas and xanthelasmas are cholesterol-laden deposits that manifest as yellowish papules, plaques, or nodules. Xanthelasmas specifically occur on the eyelids, appearing as soft, yellowish, flat or slightly raised patches. Xanthomas can appear on various parts of the body, including tendons (tuberous xanthomas) or over joints and extensor surfaces. In skin changes in cirrhosis images, these lesions are distinct and yellow, offering a direct visual link to impaired lipid metabolism, often a consequence of cholestasis. Their presence, particularly xanthelasmas, can be an early and visible sign, preceding more severe symptoms of liver failure in conditions like primary biliary cholangitis (PBC).
Purpura and ecchymoses (bruises) are frequently observed in advanced cirrhosis due to coagulopathy resulting from impaired synthesis of clotting factors by the liver and often thrombocytopenia (low platelet count). These appear as reddish-purple to bluish-black skin lesions that do not blanch under pressure. Purpura consists of smaller petechiae (pinpoint spots) or larger ecchymoses. In cirrhosis skin problems images, these can be widespread, occurring spontaneously or with minimal trauma, particularly on the limbs and trunk. The presence of these bleeding manifestations visually underscores the severity of hepatic dysfunction and the increased risk of hemorrhage for the patient, a critical aspect of liver disease symptoms in its advanced stages.
Telangiectasias, commonly known as spider angiomas, are key hepatic dermatological manifestations. Their appearance as central red papules with radiating fine blood vessels is highly characteristic. While they are a direct symptom of altered hormone metabolism in cirrhosis, their specific visual pattern makes them a distinctive ‘rash’ or skin lesion. Multiple, widespread spider angiomas, especially on the upper body, are strong indicators of liver damage. Their visual prominence in skin rash liver cirrhosis images makes them one of the most recognizable dermatological signs of the disease. The dynamic nature, blanching and refilling, if captured in video, further exemplifies their vascular origin.
Other less common but documented skin changes in cirrhosis include conditions that mimic more general dermatoses. For example, some patients may develop pemphigoid-like lesions or erythema multiforme-like eruptions. These are rare, but when they occur, they present as bullae (blisters) or target-like lesions, respectively. These types of skin reactions are typically inflammatory and can be a challenging diagnostic puzzle without considering the underlying liver disease. Their appearance in liver disease skin symptoms photographs would show distinct blister formation or concentric rings of redness, demanding a careful differential diagnosis. The exact mechanisms are not always fully understood but may involve immune dysregulation associated with chronic liver inflammation.
Skin infections are also more prevalent in individuals with liver cirrhosis due to impaired immune function. Cellulitis, erysipelas, and fungal infections are common. Cellulitis presents as a red, swollen, warm, and tender area of skin, often with poorly defined borders, frequently affecting the lower limbs, especially in the presence of edema or ascites. In cirrhosis skin problems images, these infections can be visually concerning, showing signs of acute inflammation and sometimes associated with fever. The skin might appear stretched and shiny due to underlying swelling, and any breaks in the skin from scratching can serve as entry points for bacteria, further complicating the clinical picture of hepatic cirrhosis manifestations.
Finally, leukonychia (whitening of the nails) and clubbing (bulbous fingertips with curved nails) are also skin appendages changes that can be very distinct visually. Leukonychia can be partial (transverse lines) or complete, and clubbing can range from subtle to pronounced. These are chronic changes that develop over time and contribute to the overall visual diagnostic landscape of chronic liver disease. The sheer variety of these dermatological signs underscores the systemic impact of liver dysfunction, making the skin a critical area for visual assessment in patients with or suspected of having cirrhosis.
Liver cirrhosis Treatment
Liver cirrhosis treatment focuses primarily on managing the underlying cause of the liver damage, preventing further progression of fibrosis, and addressing the numerous complications that arise as the disease advances. While this article emphasizes visual symptoms, understanding the treatment strategies is crucial for comprehending the clinical journey of a patient with cirrhosis. The initial and most vital step in cirrhosis management is to eliminate or control the causative agent. This foundational approach seeks to halt or slow down the ongoing liver injury and prevent further hepatic fibrosis.
Key strategies for addressing the underlying cause include:
- Alcohol cessation: For alcoholic liver disease, complete abstinence from alcohol is paramount. This can significantly improve liver function and reduce the risk of further complications.
- Antiviral therapy: For chronic hepatitis B or C, highly effective antiviral medications can eradicate the virus or suppress its replication, thereby preventing further viral-induced liver damage and progression to cirrhosis.
- Weight management and lifestyle changes: For non-alcoholic fatty liver disease (NAFLD) and non-alcoholic steatohepatitis (NASH), weight loss through diet and exercise, along with strict control of diabetes and hyperlipidemia, is crucial. This can lead to regression of steatosis and inflammation, and in some cases, even improvements in fibrosis.
- Immunosuppressive therapy: For autoimmune hepatitis, corticosteroids and other immunosuppressants are used to suppress the autoimmune attack on the liver.
- Chelation therapy: For hemochromatosis, regular phlebotomy (blood removal) helps reduce iron overload. For Wilson’s disease, copper-chelating agents are used to remove excess copper from the body.
- Bile acid therapy: For primary biliary cholangitis (PBC) and primary sclerosing cholangitis (PSC), ursodeoxycholic acid (UDCA) is a common liver disease therapy that can slow disease progression and improve liver enzyme levels, although it is not curative.
Beyond addressing the etiology, treating liver cirrhosis heavily involves managing its life-threatening complications, which are often visually apparent and require prompt intervention:
- Ascites management: This involves a combination of dietary sodium restriction (usually less than 2 grams/day) and diuretic medications (e.g., spironolactone and furosemide). For refractory ascites, therapeutic paracentesis (drainage of fluid from the abdomen) may be performed, which visually reduces abdominal distension. In some severe cases, a transjugular intrahepatic portosystemic shunt (TIPS) procedure or liver transplantation might be considered to divert portal blood flow and reduce pressure.
- Esophageal varices treatment: Enlarged veins in the esophagus (varices) are a major cause of bleeding. Prevention involves non-selective beta-blockers to reduce portal pressure. For active bleeding, endoscopic variceal band ligation (EVL) or sclerotherapy is performed, visually stopping the hemorrhage. Octreotide or terlipressin may also be administered to reduce portal inflow.
- Hepatic encephalopathy (HE) management: This neurological complication affects cognition and can manifest as confusion, disorientation, or coma. Treatment involves reducing ammonia production and absorption from the gut using lactulose and non-absorbable antibiotics like rifaximin. Nutritional support, including adequate protein intake, is also critical.
- Jaundice and pruritus relief: While treating the underlying cause of cholestasis is key, symptomatic relief for severe itching (pruritus) can be achieved with medications like cholestyramine, rifampicin, or naltrexone. UV light therapy can also be employed in some cases. Visually, as bilirubin levels decrease, the yellowing of the skin and sclera will lessen.
- Coagulopathy correction: Impaired clotting due to reduced synthesis of clotting factors. Vitamin K supplementation may be given, but often fresh frozen plasma (FFP) is required before invasive procedures or in cases of active bleeding to supply missing clotting factors. This helps reduce the visual signs of purpura and ecchymoses.
- Infection prevention and treatment: Patients with cirrhosis are highly susceptible to bacterial infections (e.g., spontaneous bacterial peritonitis). Prophylactic antibiotics may be given, and prompt, aggressive treatment with appropriate antibiotics is crucial for any suspected infection.
- Hepatorenal syndrome (HRS) management: A severe form of kidney failure in advanced cirrhosis. Treatment includes vasoconstrictors (e.g., terlipressin) and albumin, aiming to improve renal perfusion.
- Hepatocellular carcinoma (HCC) surveillance: Regular screening (ultrasound, alpha-fetoprotein) is critical as cirrhosis is the leading risk factor for liver cancer. Early detection allows for potentially curative interventions like resection, ablation, or transplantation.
Nutritional support is a cornerstone of cirrhosis management. Patients with cirrhosis often suffer from malnutrition and sarcopenia. Dietary modifications, including adequate calorie and protein intake (often 1.2-1.5 g/kg/day), frequent small meals, and sometimes nocturnal snacks, are essential to combat muscle wasting and improve overall strength and energy levels, contributing to a better physical appearance. Supplements, including fat-soluble vitamins, may also be required. The goal is to reverse or prevent the visible signs of cachexia and maintain body mass.
For patients with decompensated cirrhosis whose disease continues to progress despite optimal medical management, liver transplantation remains the only definitive cure. This major surgical procedure replaces the diseased liver with a healthy donor liver. It significantly improves survival and quality of life for carefully selected candidates. Post-transplant, many of the visual signs of cirrhosis, such as jaundice, ascites, spider angiomas, and muscle wasting, can gradually resolve, allowing patients to regain a healthier appearance and function. The transformation can be quite dramatic in cirrhosis recovery pictures, highlighting the profound impact of successful treatment. Long-term follow-up and immunosuppression are required after transplantation to prevent rejection and other complications, ensuring sustained health benefits from this complex liver disease therapy.