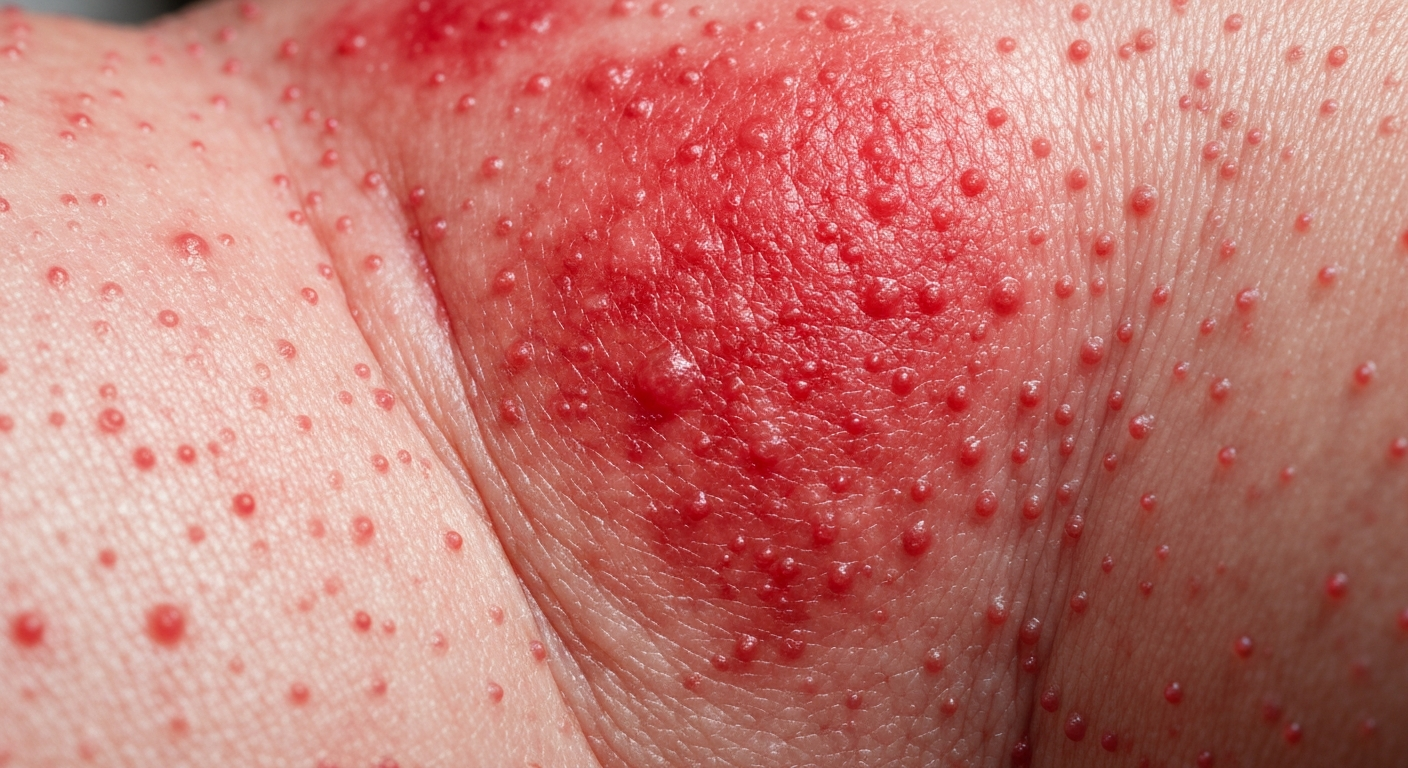
When identifying fungal infections, visualizing the affected areas is crucial. This article provides comprehensive descriptions of candidiasis symptoms pictures, helping to understand the diverse manifestations across different body parts. Focusing on specific visual cues can greatly aid in early recognition and appropriate intervention for candidal infections.
candidiasis Symptoms Pictures
candidiasis, a common fungal infection caused by various species of Candida, predominantly Candida albicans, manifests with a wide array of visual symptoms depending on the affected body site. Understanding these candidiasis symptoms pictures is vital for accurate identification.
Oral candidiasis (Thrush) Visual Manifestations:
- Creamy White Patches: The most characteristic sign of oral candidiasis is the presence of distinctive creamy white, slightly raised lesions or patches on the tongue, inner cheeks, roof of the mouth, tonsils, and sometimes the back of the throat. These patches often resemble cottage cheese or milk curds.
- Underlying Redness and Tenderness: When these white patches are scraped off, which can be difficult, the underlying tissue typically appears fiery red, tender, or even bleeds slightly. This distinguishes candidiasis from simple milk residue.
- Angular Cheilitis (Perleche): Often co-occurring with oral thrush, this involves redness, cracking, and scaling at the corners of the mouth. The skin here may appear macerated and can be quite painful.
- Erythematous Candidiasis: Less common but identifiable, this form presents as flat, red areas on the tongue or palate, often associated with a burning sensation rather than prominent white plaques. The tongue may appear smoothed or atrophic in areas.
- Denture Stomatitis: In individuals wearing dentures, candidiasis can manifest as a chronic redness and inflammation beneath the denture, primarily affecting the palate. The mucosa appears shiny, often granular, and consistently inflamed, often without overt white patches.
Vaginal candidiasis (Vaginal Yeast Infection) Visual Manifestations:
- Vulvar and Vaginal Redness: A prominent visual symptom is intense redness and inflammation of the vulva and vaginal tissues. This erythema can be widespread and severe, contributing to significant discomfort.
- Swelling (Edema): The labia and vaginal opening may appear swollen and puffy due to inflammation. This edema can be quite noticeable in candidiasis symptoms pictures.
- Thick, White, Cottage Cheese-Like Discharge: The hallmark sign is a characteristic vaginal discharge that is thick, white, lumpy, and often described as resembling cottage cheese. This discharge may cling to the vaginal walls and labia.
- Vaginal Fissures and Cracks: Due to intense itching and inflammation, small fissures or cracks may develop in the sensitive skin of the vulva. These can be painful and may bleed.
- Excoriations: Persistent scratching can lead to skin abrasions and excoriations in the perivaginal area, further complicating the visual presentation.
- Satellite Lesions: In severe cases, the rash can extend to the groin folds, presenting with the characteristic red, scaly patches and tiny pustules known as satellite lesions, which are crucial for identifying candidiasis.
Cutaneous candidiasis (Skin Fold candidiasis/Intertrigo) Visual Manifestations:
- Bright Red Rash: candidiasis in skin folds (e.g., armpits, groin, under breasts, abdominal folds) typically presents as a bright red, glistening rash. The color is often intensely vivid.
- Well-Defined Borders with Satellite Lesions: A key diagnostic visual feature is the presence of well-demarcated borders of the primary rash, with smaller, separate pustules or papules (satellite lesions) extending outwards from the main lesion. These satellite lesions are highly indicative of a candidal infection.
- Maceration and Erosion: Due to moisture retention, the skin within the folds often appears macerated (softened and whitish), and in severe cases, superficial erosions or peeling of the skin may be visible.
- Small Pustules: Tiny, pus-filled bumps or pustules may be present, particularly at the periphery of the rash or as part of the satellite lesions.
- Scaling: Fine scaling may be observed, though the prominent feature is often the moist, erythematous base.
Diaper Rash candidiasis Visual Manifestations:
- Intense Redness and Shininess: Diaper candidiasis typically appears as an intensely red, shiny rash in the diaper area, covering the perineum, inner thighs, and buttocks.
- Well-Demarcated Edges: Similar to other cutaneous candidiasis, the rash often has sharp, clear borders where the infected skin meets healthy skin.
- Satellite Lesions: The presence of small, red bumps or pustules (satellite lesions) scattered outside the main area of the rash is a definitive visual clue for candidiasis in the diaper area.
- Pustules and Papules: Tiny pustules and red papules are frequently observed within the rash, particularly in more severe cases.
Nail candidiasis (Onychomycosis or Paronychia) Visual Manifestations:
- Chronic Paronychia: This involves redness, swelling, and tenderness of the nail folds, often affecting multiple digits. The cuticle may be absent or retracted, creating a space for moisture and yeast accumulation. Pus may sometimes be expressed from the nail fold.
- Nail Plate Changes: The nail plate itself may become thickened, discolored (yellowish or brownish), and distorted. In some cases, the nail may lift off the nail bed (onycholysis).
- Horizontal Ridges: Chronic inflammation can lead to the formation of horizontal ridges (Beau’s lines) on the nail plate.
Esophageal candidiasis Visual Manifestations (indirect through endoscopy):
- White Plaques and Ulcerations: Endoscopic images of esophageal candidiasis reveal white, adherent plaques or pseudomembranes on the esophageal lining. These plaques can be discrete or confluent.
- Erythema and Friability: The underlying esophageal mucosa appears red (erythematous) and can be friable, meaning it bleeds easily upon contact.
- Ulcerations: In more severe cases, ulcerations may be present alongside the plaques.
These detailed descriptions of candidiasis symptoms pictures provide a foundational understanding of how this common yeast infection presents visually across different anatomical sites, aiding in recognition and subsequent treatment strategies.
Signs of candidiasis Pictures
Identifying the visual signs of candidiasis is paramount for prompt diagnosis and effective treatment. These observable signs, when viewed (even descriptively, as pictures), offer clear indications of a fungal infection.
Observable Signs of Oral candidiasis (Thrush):
- Visualized White Patches: The hallmark sign is the distinct appearance of creamy white, elevated patches or lesions on the mucous membranes of the mouth. These patches are highly visible on the tongue, inner cheeks, gums, or palate.
- Difficulty in Removal: An important diagnostic sign is that these white patches are typically challenging to scrape off. Unlike food debris, they adhere firmly to the underlying tissue.
- Erythematous Base: Upon successful, albeit difficult, removal of the white patches, the underlying tissue exhibits pronounced redness (erythema) and often appears raw or inflamed. Minor bleeding can also be an observable sign.
- Cracked Mouth Corners (Angular Cheilitis): Observation of red, cracked, and sometimes weeping lesions at the corners of the mouth is a strong indicator, especially when co-occurring with intraoral white patches. The skin may look macerated and irritated.
- Red or Smooth Tongue Areas: In erythematous candidiasis, the tongue may appear unusually red or smooth in certain areas, reflecting atrophy of the papillae, rather than the typical white coating.
Observable Signs of Vaginal candidiasis:
- Vulvar and Vaginal Erythema: A prominent visual sign is intense redness and inflammation of the vulva (external genital area) and the vaginal walls. This erythema can range from a mild pink to a fiery red.
- Swelling of Labia: The labia majora and minora may appear visibly swollen or edematous, contributing to discomfort and an altered appearance.
- Characteristic Vaginal Discharge: The most recognizable sign is the presence of a thick, white, curd-like or cottage cheese-like vaginal discharge. This discharge is typically odorless and may adhere to the vaginal walls.
- Skin Excoriations: Due to severe itching, scratch marks (excoriations) and small abrasions may be visible on the skin of the vulva and surrounding perineal area.
- Fissures: Small, painful cracks or fissures can be observed in the sensitive vulvar skin, often indicating significant inflammation and dryness.
Observable Signs of Cutaneous candidiasis:
- Intertriginous Rash: In skin folds, a highly visible sign is a bright red, intensely erythematous rash that often has a glistening or moist appearance. This candidiasis rash is typically confined to the fold but may extend slightly beyond.
- Satellite Lesions: Crucially, the presence of small, discrete pustules or papules (satellite lesions) located a short distance away from the main, confluent rash is a definitive diagnostic sign of candidiasis. These are often seen at the periphery of the main lesion.
- Well-Demarcated Borders: The main candidal rash usually has sharp, clear borders, distinguishing it from surrounding healthy skin.
- Maceration: The affected skin within the fold may appear softened, whitish, and somewhat wrinkled due to moisture (maceration).
- Superficial Erosion or Peeling: In more chronic or severe cases, the surface of the skin may exhibit peeling or superficial erosions.
Observable Signs of Diaper candidiasis:
- Shiny Red Rash: A very noticeable sign is an intensely red, shiny rash covering the entire diaper area, including the skin folds. Unlike simple irritant diaper rash, candidiasis often affects the creases.
- Distinct Satellite Pustules: The presence of small, scattered red bumps or pustules (satellite lesions) beyond the main area of redness is a key visual sign differentiating candidal diaper rash from other forms.
- Raised Border: The rash may have a slightly raised and somewhat scaly border.
Observable Signs of Nail candidiasis (Paronychia):
- Inflamed Nail Folds: The skin around the nail (nail folds) appears visibly red, swollen, and tender. This inflammation can be chronic.
- Loss of Cuticle: The cuticle may be absent or noticeably retracted, creating a gap between the nail plate and the proximal nail fold, which can be an entry point for yeast.
- Nail Plate Changes: The nail itself may show signs such as thickening, discoloration (yellow-brown), and distortion or ridging. The nail surface may also become brittle.
- Pus Formation: In some instances, particularly with acute flares, pus may be observed or expressed from the inflamed nail fold.
Understanding these distinct visual signs across various forms of candidiasis is essential for healthcare professionals and individuals seeking to recognize and address these common fungal infections effectively. The detailed descriptions aim to emulate the visual information gained from candidiasis pictures.
Early candidiasis Photos
Recognizing candidiasis in its initial stages is critical for preventing widespread infection and facilitating quicker recovery. Early candidiasis photos would typically capture subtle yet distinct visual cues before the infection becomes deeply established or extensively spread. Here, we describe what those early signs might look like.
Early Oral candidiasis (Thrush) Signs:
- Pinpoint White Spots: Initially, oral thrush may present as a few small, isolated, pinpoint white spots or flecks on the tongue or inner cheeks, rather than extensive plaques. These might be mistaken for milk residue.
- Subtle Redness: Before obvious white patches form, there might be a general, subtle redness or mild inflammation of the oral mucosa, possibly accompanied by a feeling of mild discomfort or burning.
- Slightly Creamy Coating: A very thin, almost translucent creamy or yellowish-white coating might be observed on the tongue, which is easily overlooked but represents early yeast colonization.
- Mild Angular Cheilitis: The corners of the mouth might show very early signs of slight redness, dryness, or a barely perceptible crack, without significant scaling or pain. This early angular cheilitis can precede full-blown intraoral thrush.
Early Vaginal candidiasis Signs:
- Mild Vulvar Redness: One of the earliest visual signs is a slight, localized redness or pinkish hue on the labia or vaginal opening, often accompanied by mild itching. This redness may not be widespread initially.
- Minimal Swelling: There might be a very subtle puffiness or slight swelling of the vulvar tissues, not yet extensive edema.
- Thin, Watery Discharge with Flecks: Instead of the thick, cottage cheese-like discharge, early vaginal candidiasis might present with a thin, watery discharge that contains small, sparse white flecks or tiny clumps. The discharge volume may not be significantly increased at this stage.
- Mild Irritation/Itchiness: Though not a visual symptom, a sensation of mild vaginal irritation or itchiness often precedes the more pronounced visual signs. Visually, this might manifest as barely perceptible skin changes from rubbing.
Early Cutaneous candidiasis (Skin Folds) Signs:
- Patchy Redness: The first visual sign in skin folds might be an area of faint, patchy redness or erythema, often irregular in shape, within the deepest part of the fold. It may not yet be glistening or intensely red.
- Scattered Pinpoint Papules: Very early candidiasis may present as a few scattered, tiny red bumps or pinpoint papules at the edges of an area that is beginning to show mild redness. These are the precursors to satellite lesions.
- Slight Maceration: The skin might show only a minimal degree of softening or a whitish tinge (maceration) due to prolonged moisture, without overt peeling or erosion.
- Lack of Clear Borders: In the very earliest stages, the rash may not have the sharp, well-demarcated borders characteristic of more established candidiasis. The redness might blend more subtly into the surrounding healthy skin.
Early Diaper candidiasis Signs:
- Red Spots in Folds: Unlike simple irritant diaper rash which spares folds, early candidal diaper rash might show small, isolated red spots or a faint, diffuse redness specifically within the skin creases of the groin or upper thighs.
- Few Satellite Lesions: The presence of just a few, very small, widely spaced red bumps (incipient satellite lesions) outside the main area of irritation can be an early indicator, even if the primary rash is not yet severe.
- Mild Shiny Appearance: The affected skin area might begin to show a slight shininess or glossy appearance, indicating increased moisture and inflammation.
Early Nail candidiasis (Paronychia) Signs:
- Mild Nail Fold Redness: The earliest sign is often a subtle, localized redness and very slight swelling of one nail fold, typically around the base or sides of the nail. It may be intermittent.
- Minimal Tenderness: Gentle pressure on the nail fold might elicit a mild tenderness, without overt pain or pus.
- Intact Cuticle (but vulnerable): At this stage, the cuticle may still appear intact but might be slightly lifted or less adherent, creating an early opportunity for moisture and yeast invasion.
- Very Subtle Nail Plate Change: The nail plate itself might show only a barely perceptible change in texture or a very faint yellowish tinge at the base, not yet widespread discoloration or thickening.
These descriptions aim to guide recognition of candidiasis at its nascent stages, allowing for timely intervention based on early candidiasis photos, even when only described. Early detection of these candidiasis symptoms is crucial for effective management and preventing the condition from worsening or spreading.
Skin rash candidiasis Images
Skin rash candidiasis, also known as cutaneous candidiasis, presents with distinctive visual characteristics that are crucial for accurate diagnosis. These images, described in detail, highlight the specific appearance of candidal rashes in various body locations. The appearance of these candidiasis rashes is highly indicative of the underlying yeast infection.
Intertriginous candidiasis (Skin Fold Rash) Visual Details:
- Fiery Red and Glistening Erythema: The most striking feature is an area of intensely red, often glistening or shiny erythema located within skin folds. These folds commonly include the axillae (armpits), groin, inframammary (under breasts), web spaces between fingers/toes, and abdominal folds. The color is typically a vibrant, almost angry red.
- Well-Demarcated Borders: The main patch of candidal rash usually has sharp, clear, and often slightly raised borders, creating a distinct line between infected and healthy skin. This clear demarcation is a key visual clue.
- Satellite Lesions: A definitive characteristic visible in candidiasis images is the presence of smaller, discrete papules (red bumps) or pustules (pus-filled bumps) scattered outside the main rash. These “satellite lesions” are typically a few millimeters away from the main erythematous area and are highly specific to candidiasis.
- Maceration and Moist Appearance: Due to continuous moisture, the skin often appears macerated, soft, whitish, and wrinkled within the deepest part of the fold. The surface may look perpetually moist.
- Scaling and Peeling: Fine, white scaling can sometimes be observed, particularly at the periphery or where the skin is less macerated. In chronic cases, superficial peeling or exfoliation may be present.
- Fissures: Cracks or fissures can sometimes develop within the deep folds, especially if the skin is stretched or subjected to friction, leading to pain and further discomfort.
Diaper candidiasis Rash Visual Details:
- Intense Erythema Across Diaper Area: The rash is typically characterized by an area of bright red, often confluent (merged) erythema covering the skin surfaces that come into contact with a diaper. This includes the perineum, inner thighs, buttocks, and lower abdomen.
- Involvement of Skin Creases: Unlike simple irritant diaper rash, candidal diaper rash characteristically involves the skin folds and creases (inguinal folds, labial folds in girls), which appear equally red and often glistening. This is a critical differentiating feature in candidiasis images.
- Prominent Satellite Pustules/Papules: Similar to intertrigo, numerous small, raised red bumps or pustules (satellite lesions) are scattered beyond the main, confluent rash. These are highly diagnostic for diaper candidiasis.
- Shiny Surface: The entire rash often has a shiny or glazed appearance due to the moist environment and inflammation.
- Raised, Slightly Scaly Borders: The edges of the main rash can sometimes appear slightly raised and may show fine scaling.
Erosio Interdigitalis Blastomycetica (candidiasis of Finger/Toe Webs) Visual Details:
- Macerated and Whitened Skin: This specific form of candidiasis manifests as pronounced maceration and whitish discoloration of the skin in the web spaces between fingers (most commonly 3rd and 4th) or toes.
- Central Erosion: A key visual feature is a central erosion or ulceration within the macerated area, often appearing raw, red, and sometimes weeping.
- Well-Demarcated Border: The lesion usually has a clear, often slightly undermined, border separating it from healthy skin.
- Redness and Surrounding Inflammation: Beyond the central erosion, the surrounding skin in the web space appears red and inflamed.
Chronic Mucocutaneous candidiasis (CMC) Skin Manifestations:
- Diverse and Persistent Lesions: In CMC, the skin lesions are often widespread, persistent, and can be highly disfiguring. Visuals would show a variety of presentations.
- Hyperkeratotic and Crusted Plaques: Skin can develop thick, scaly, and crusted plaques, often resembling psoriasis or other chronic dermatoses. These can be particularly prominent on the face, scalp, and nails.
- Granulomatous Lesions: In severe cases, especially in those with underlying immune deficiencies, thick, nodular, or granulomatous lesions can form, particularly on the face, indicating deep tissue involvement.
- Dystrophic Nails: Nails are often severely affected, becoming thickened, discolored, and severely dystrophic, often with associated chronic paronychia.
These detailed descriptions of skin rash candidiasis images provide a comprehensive visual guide for understanding the diverse presentations of candidal skin infections, from common intertrigo to more severe forms. Recognizing these specific visual characteristics is crucial for accurate diagnosis and initiating appropriate candidiasis treatment.
candidiasis Treatment
Effective candidiasis treatment involves a range of antifungal medications and supportive measures, tailored to the location and severity of the infection. The primary goal is to eliminate the Candida yeast and alleviate symptoms. Treatment for candidiasis symptoms varies, but generally relies on antifungal agents.
Topical Antifungal Treatments:
These are typically the first line of candidiasis treatment for superficial infections of the skin, mouth, and vagina.
- Azole Antifungals:
- Clotrimazole: Available as creams (for skin and vaginal candidiasis), lozenges or troches (for oral candidiasis/thrush). Applied 2-3 times daily for skin, once daily vaginally for 3-7 days. Oral troches are dissolved slowly in the mouth 5 times daily.
- Miconazole: Available as creams, powders, sprays (for skin candidiasis), and vaginal suppositories or creams. Applied 1-2 times daily for skin; vaginal preparations typically used for 3-7 days.
- Ketoconazole: Available as creams, shampoos, and oral tablets (though oral use is reserved for severe cases due to liver toxicity concerns). Cream applied once daily for skin candidiasis.
- Econazole: Primarily used as a cream for cutaneous candidiasis, applied once daily.
- Tioconazole: Available as a single-dose vaginal ointment for vaginal candidiasis.
- Polyene Antifungals:
- Nystatin: Highly effective for candidiasis. Available as creams, ointments, powders (for skin candidiasis, especially diaper rash and intertrigo), and oral suspensions (for oral thrush). Skin preparations are applied 2-3 times daily. Oral suspension is swished in the mouth and swallowed (or spit out for infants/children) 4 times daily.
- Other Topical Agents:
- Ciclopirox: Available as cream, gel, or lacquer (for nail candidiasis). Applied 2 times daily for skin.
- Terbinafine: While primarily effective against dermatophytes, it can have some activity against Candida and is available as a cream or spray.
Oral Antifungal Treatments:
These are typically reserved for more severe, widespread, recurrent, or systemic candidiasis infections, or when topical treatments are ineffective. Oral medications are crucial for deep-seated or disseminated candidiasis symptoms.
- Fluconazole: The most commonly prescribed oral antifungal for candidiasis.
- Vaginal candidiasis: A single oral dose of 150 mg is often sufficient for uncomplicated cases. For recurrent infections, a longer course (e.g., 150 mg once weekly for 6 months) may be prescribed.
- Oral thrush (Oropharyngeal candidiasis): Typically 100-200 mg once daily for 7-14 days.
- Esophageal candidiasis: Higher doses, typically 200-400 mg once daily for 14-21 days.
- Cutaneous candidiasis: May be used for extensive or refractory skin infections.
- Systemic candidiasis: Higher doses and longer durations are used, often intravenously initially.
- Itraconazole: Available in capsules or oral solution.
- Used for oropharyngeal and esophageal candidiasis, as well as some forms of cutaneous and nail candidiasis, particularly when fluconazole is not suitable or effective. Dosage varies based on indication.
- Oral solution has better bioavailability for oral/esophageal candidiasis.
- Amphotericin B: A powerful antifungal, typically reserved for severe, life-threatening systemic candidiasis, often administered intravenously. Due to significant side effects, it’s used with caution.
- Caspofungin, Micafungin, Anidulafungin (Echinocandins): These are newer classes of antifungals, primarily used intravenously for severe invasive candidiasis, especially in critically ill patients or those resistant to azoles.
Supportive Measures and Lifestyle Modifications:
These complement antifungal candidiasis treatment and help prevent recurrence.
- Maintain Dryness: For cutaneous candidiasis, keeping affected skin areas dry is paramount.
- Use moisture-absorbing powders (e.g., cornstarch, but avoid if active infection to prevent trapping yeast) or antifungal powders.
- Wear loose-fitting, breathable clothing made of cotton or natural fibers.
- Ensure proper hygiene and drying of skin folds after bathing.
- Oral Hygiene: For oral candidiasis, meticulous oral hygiene is important.
- Brush teeth regularly with a soft toothbrush.
- Sterilize or replace toothbrushes and dentures to prevent reinfection.
- Rinse mouth with saltwater or non-alcoholic mouthwash.
- Vaginal Hygiene: For vaginal candidiasis.
- Avoid douching, scented feminine hygiene products, and harsh soaps, as these can disrupt the natural vaginal flora.
- Wear cotton underwear and avoid tight-fitting synthetic clothing.
- Change out of wet swimsuits or sweaty exercise clothes promptly.
- Dietary Considerations: While evidence is limited, some individuals find that reducing sugar intake or consuming probiotics (e.g., yogurt with live cultures) can help prevent recurrent candidiasis.
- Addressing Underlying Conditions: Treatment of underlying conditions that predispose to candidiasis is crucial.
- Diabetes: Strict glycemic control can significantly reduce the risk of candidiasis.
- Immunosuppression: Managing the underlying immune deficiency or adjusting immunosuppressive medications when possible.
- Antibiotic Use: Minimizing unnecessary antibiotic use or taking prophylactic antifungals if long-term antibiotics are unavoidable.
- Nail Care: For nail candidiasis, keep nails trimmed and clean. Avoid prolonged water exposure.
The choice of candidiasis treatment regimen depends on various factors including the patient’s age, immune status, location and severity of the infection, and presence of any underlying medical conditions. Always consult a healthcare professional for diagnosis and treatment of candidiasis symptoms pictures.