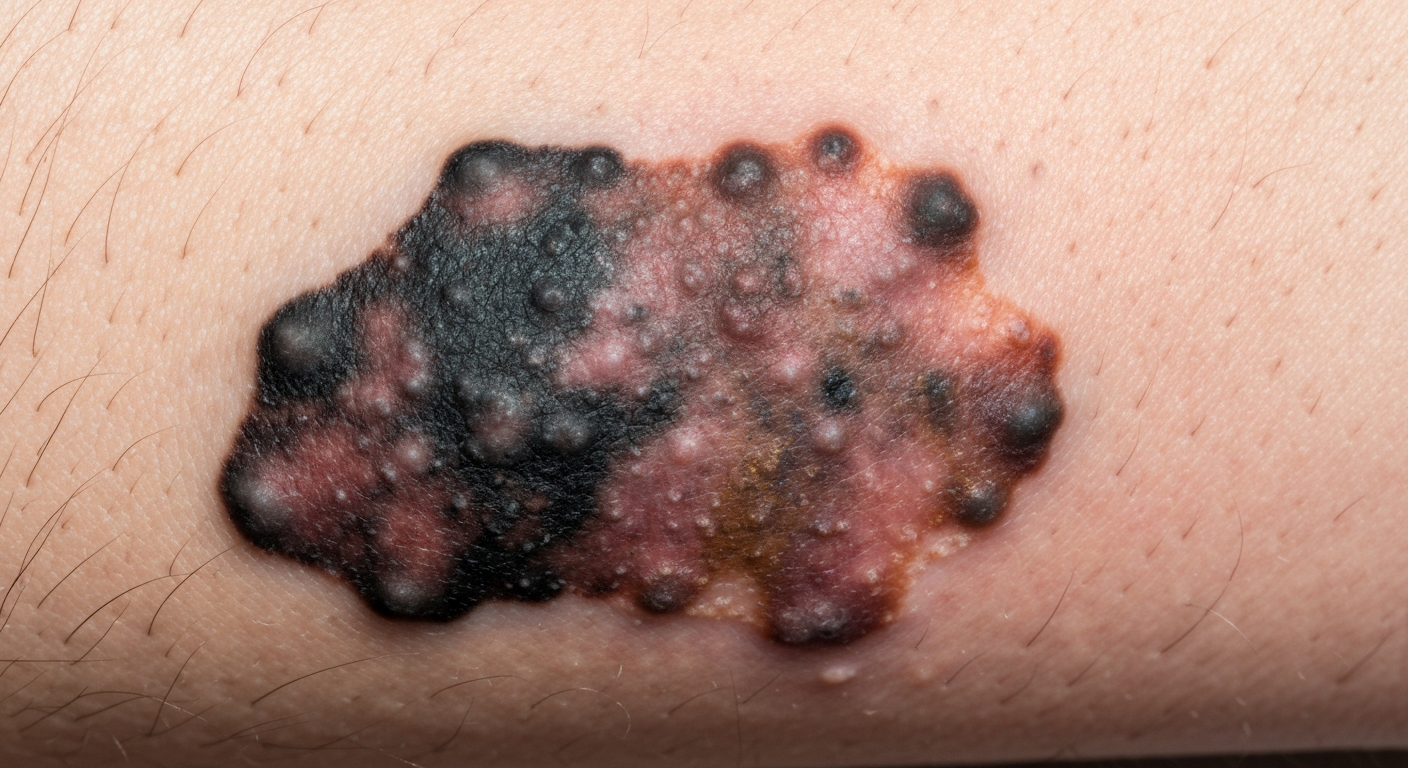
When evaluating skin changes, understanding nevus symptoms pictures is crucial for early detection and peace of mind. These visual guides offer invaluable insight into the varied appearances of moles and other skin lesions, helping individuals identify potential areas of concern that warrant professional medical evaluation. This article will delve into the comprehensive visual aspects of various nevi, assisting in recognizing what to look for.
nevus Symptoms Pictures
Understanding the visual characteristics of nevi, or moles, through nevus symptoms pictures is fundamental for monitoring skin health. Nevi present in a vast array of forms, colors, and textures, and recognizing these attributes can help differentiate between benign lesions and those that may require medical attention. A typical benign nevus is often symmetrical, has regular borders, uniform color, and a diameter generally less than 6 millimeters. However, variations are common, and an awareness of these normal presentations is key.
The color of nevi can range significantly. Common moles are frequently brown, exhibiting shades from light tan to dark chocolate. Some nevi can appear black, especially in individuals with darker skin tones or if they are deeply pigmented. Other benign nevi might present as pink or flesh-colored, particularly dermal nevi which are often raised and can blend with the surrounding skin tone. Blue nevi, a distinct type, typically appear as deep blue or blue-gray macules or papules, often due to melanin located deeper in the dermis. Reddish nevi might suggest vascular components or inflammation, although true melanocytic nevi are usually not red unless irritated or part of a Spitz nevus.
The shape and borders of a nevus are also critical visual cues. Benign nevi commonly display a round or oval shape with smooth, well-defined borders. These borders maintain a consistent edge where the mole meets the surrounding skin. In contrast, irregular or scalloped borders can be a warning sign, suggesting an atypical nevus or potentially melanoma. The surface texture of a nevus can vary from completely flat (macular) to slightly raised (papular) or even dome-shaped. Some nevi may have a velvety or warty texture, while others can be smooth or firm to the touch. The presence of hair within a nevus is common and generally indicates a benign nature, as hair follicles are often intertwined with nevus cells.
Size is another important dimension in nevus symptom pictures. While many benign nevi are small, typically less than 6mm, some can be larger, especially congenital nevi that are present at birth or develop shortly thereafter. These congenital nevi can range from small to giant, covering significant portions of the body. Acquired nevi, which develop later in life, usually remain relatively small. Rapid changes in size, particularly an increase in diameter or elevation over a short period, warrant immediate dermatological evaluation. Any nevus that is greater than 6mm and exhibits other concerning features should be closely monitored.
Beyond visual appearance, some nevi can present with sensory symptoms. While most benign nevi are asymptomatic, itching, tenderness, or bleeding can occasionally occur, especially if the nevus is traumatized or irritated. Persistent itching, unexplained bleeding, or any new sensation associated with a nevus, particularly one that has been stable, should be investigated. Crust formation, ulceration, or non-healing sores on or around a nevus are also significant warning signs that necessitate prompt medical assessment. Inflammatory changes, such as redness or swelling around a nevus without obvious trauma, are also concerning and should be documented and reviewed by a dermatologist.
Detailed characteristics to observe when reviewing nevus symptoms pictures:
- Color Uniformity: Benign nevi typically have a consistent color throughout. Multiple shades of brown, black, red, white, or blue within a single lesion can be a sign of melanoma.
- Symmetry: A benign nevus will often appear symmetrical if divided in half, meaning both halves would largely match. Asymmetry is a common indicator of an atypical nevus or melanoma.
- Border Definition: Look for sharp, regular, and well-defined borders. Blurred, irregular, notched, or scalloped borders are less reassuring.
- Surface Texture: Smooth, uniform surfaces are common for benign nevi. Any areas of rough texture, scaling, crusting, or ulceration that develop warrant concern.
- Elevation: Some nevi are flat (macular), others are raised (papular or nodular). A change in elevation, especially an area becoming significantly more raised or developing new lumps, is important.
- Hair Growth: The presence of hair within a nevus is generally a sign of benignity. Changes in hair growth (e.g., loss of hair) within a nevus can sometimes be a subtle sign of change, though this is less specific than other ABCDE criteria.
- Satellite Lesions: The development of small, pigmented spots around a larger nevus can be a sign of spreading melanoma.
- Inflammation: Redness, swelling, or warmth around a nevus without trauma should be noted.
- Regression: Areas of a nevus appearing to fade or become lighter, sometimes associated with a white halo (halo nevus), can be benign but can also indicate immune system activity against melanoma cells.
The vast spectrum of nevus appearances makes visual assessment complex. This is why professional dermatological evaluation, often involving dermoscopy (a specialized magnifying tool), is crucial for accurately diagnosing and monitoring nevi, especially when any of the above characteristics raise suspicion based on nevus symptoms pictures.
Signs of nevus Pictures
When examining signs of nevus pictures, the primary objective is to differentiate between benign moles and those that exhibit characteristics suspicious for melanoma or other skin cancers. The universally recognized “ABCDE” rule provides a systematic framework for evaluating these signs. This rule is a critical tool for both self-examination and professional screening, highlighting specific features that, when present, increase the likelihood of malignancy.
A – Asymmetry: A key sign of nevus pictures indicative of potential concern is asymmetry. If you draw an imaginary line through the center of the nevus, a benign mole will typically have halves that match each other. In contrast, a suspicious lesion will often be asymmetrical, meaning one half does not mirror the other in shape, size, or elevation. This imbalance suggests uncontrolled growth patterns, a hallmark of malignancy.
B – Border Irregularity: Benign nevi usually have smooth, well-defined, and even borders. When reviewing signs of nevus pictures, look for borders that are ragged, notched, blurred, or scalloped. These irregular edges indicate disorganized growth of pigment-producing cells and are a significant red flag for atypical nevi and melanoma. The borders may also fade into the surrounding skin rather than having a crisp demarcation.
C – Color Variation: One of the most telling signs found in nevus pictures is color variation. A benign nevus will typically have a uniform color throughout. Melanoma, however, often presents with multiple shades of color within the same lesion, including different tones of tan, brown, or black. Furthermore, the presence of red, white, or blue within a pigmented lesion is highly suspicious. Red can indicate inflammation or vascular components, white can suggest areas of regression, and blue indicates deeply situated pigment, all of which are concerning when mixed with other colors.
D – Diameter: The diameter of a nevus is another important consideration. While not an absolute rule, most melanomas are greater than 6 millimeters (about the size of a pencil eraser) when diagnosed. However, it’s crucial to remember that some melanomas can be smaller, especially in their early stages. Therefore, while a large diameter is a warning sign, a smaller lesion with other ABCDE features should not be dismissed. Monitoring for growth is more important than the absolute size alone.
E – Evolving: This is arguably the most critical sign when evaluating nevus pictures. Any change in an existing mole or the appearance of a new, suspicious lesion is a strong indicator for concern. Evolution refers to changes in size, shape, color, elevation, or any new symptoms like bleeding, itching, crusting, or tenderness. A mole that starts to feel different, looks different, or develops new symptoms should be immediately brought to a dermatologist’s attention. This includes changes over weeks, months, or even years. Baseline photographs can be incredibly useful for tracking evolution over time.
Beyond the ABCDEs, other signs can be observed in nevus pictures:
- Elevation Changes: A mole that was previously flat but becomes raised, or develops an uneven surface, should be noted. This could indicate vertical growth.
- Symptomatic Changes: While most benign moles are asymptomatic, persistent itching, tenderness, pain, or a burning sensation within a nevus are significant warning signs.
- Bleeding or Crusting: Any spontaneous bleeding, oozing, or crust formation on a nevus that isn’t due to obvious trauma is highly suspicious.
- Ulceration: The development of an open sore or ulcer within a nevus is a late-stage sign of advanced melanoma.
- Satellite Lesions: The appearance of smaller, new moles or pigmented spots surrounding a primary nevus can indicate metastasis or local spread.
- Halo Phenomenon: While a classic halo nevus (a mole surrounded by a ring of depigmented skin) is usually benign, the development of a halo around an atypical nevus or one with other suspicious features can sometimes indicate an immune response to melanoma.
- Inflammation or Redness: Persistent redness or inflammation around a nevus without an obvious cause (like irritation from clothing) warrants investigation.
- Lack of Uniformity: The overall appearance of a nevus should ideally be uniform in all aspects. Any patchiness, lumpiness, or areas that look distinct from the rest of the lesion can be concerning.
- Hair Loss: While hair in a mole is usually a benign sign, sudden loss of hair within a previously hairy nevus can occasionally be a subtle sign of underlying pathological changes.
Specific types of nevi also have characteristic signs. For example, a Spitz nevus often presents as a rapidly growing, dome-shaped, firm, reddish-pink papule or nodule, especially in children and adolescents. While typically benign, its rapid growth and atypical microscopic features can sometimes mimic melanoma. Blue nevi are usually stable, uniformly blue-gray or blue-black, and often solitary, but any changes should be monitored. Congenital nevi can be large, often hairy, and have a slightly increased lifetime risk of developing melanoma, necessitating careful lifelong monitoring, especially for changes within the lesion.
Regular self-skin exams, coupled with professional dermatological examinations, especially for individuals with numerous moles or a history of atypical nevi, are vital for the early detection of skin cancer based on these signs of nevus pictures. Early detection significantly improves prognosis for melanoma.
Early nevus Photos
Examining early nevus photos provides crucial insights into the initial appearance of moles and the subtle changes that might indicate a developing concern. Early detection is paramount for conditions like melanoma, where prognosis is directly linked to the stage at diagnosis. Therefore, understanding what nascent nevi look like, as well as the very first signs of worrisome transformation, is a vital skill for personal skin surveillance.
Most common acquired nevi appear in early nevus photos as small, uniform, round or oval, flat macules, typically light to medium brown in color. These usually develop during childhood and adolescence. They possess clear, regular borders and a homogenous pigmentation. Over time, some may slightly elevate, becoming papular, but they generally retain their symmetry and uniform appearance. The emergence of new moles, especially after the age of 40, should be noted, though many such new moles are benign. However, new moles are statistically more likely to be atypical or even malignant than changes in existing moles, particularly in older individuals.
When considering early atypical nevus photos, the subtle irregularities become more apparent. These lesions, also known as dysplastic nevi, may initially present as slightly larger than common moles (often >5mm), with somewhat irregular or fuzzy borders, and a mild degree of color variation, perhaps with a darker center and lighter periphery, or vice versa. They might have a slightly pebbly or target-like appearance. While atypical nevi are benign, individuals with many such moles have an increased risk of developing melanoma, both within an existing atypical nevus and on previously clear skin. Therefore, vigilant monitoring of these early atypical lesions is essential.
The most critical aspect of reviewing early nevus photos is identifying the earliest signs of melanoma arising within an existing nevus or as a new lesion. These changes can be extremely subtle initially. One might observe a slight blurring of a previously sharp border, a barely perceptible change in color (e.g., a new shade of brown appearing, or a tiny speck of black or red), or a minor increase in size or elevation. Often, these early melanomas are still quite small, sometimes less than 6mm, which underscores why size alone is not a definitive exclusion criterion. A new, small, dark spot appearing suddenly, especially with any asymmetry or irregular border, even if tiny, warrants attention.
Early congenital nevus photos depict moles present at birth or within the first few weeks of life. These nevi vary widely in size and appearance. Small congenital nevi may look like typical acquired moles, but often have a slightly darker pigmentation and can be hairy. Larger congenital nevi can be quite prominent, sometimes with a velvety or warty surface, and often include coarse hairs. The borders can be irregular, and the color may not be entirely uniform. While most are benign, large congenital nevi carry an increased lifetime risk of developing melanoma, making their early and ongoing surveillance critical.
Early Spitz nevus photos often show a rapidly growing, dome-shaped, firm, pink or reddish-brown nodule, especially on the face or limbs of children and adolescents. Due to their rapid growth, they can sometimes be mistaken for hemangiomas or even melanoma. While histologically complex, most Spitz nevi are benign, but their clinical and pathological similarity to melanoma can make diagnosis challenging, often requiring expert dermatopathological review.
Key features to look for in early nevus photos that might indicate concern:
- New Onset of Pigmentation: The appearance of a completely new pigmented lesion, particularly in adulthood.
- Subtle Border Changes: Edges that were once smooth becoming slightly fuzzy, notched, or indistinct.
- Minor Color Shifts: A previously uniform mole developing a tiny new area of darker pigment, a reddish hue, or a pale spot.
- Slight Elevation: A flat mole becoming minimally raised in one area, or an existing raised mole showing an area of increased elevation.
- Asymmetry in Growth: One part of the mole growing slightly faster or becoming irregularly shaped while the rest remains stable.
- New Sensations: The earliest onset of itching, tenderness, or a feeling of slight irritation in an otherwise stable mole.
- “Ugly Duckling” Sign: A mole that looks noticeably different from all the other moles on an individual’s skin. This concept is extremely useful in early detection, as it flags any lesion that stands out from the typical pattern of a person’s moles.
- Changes in Surface Texture: A previously smooth surface developing a subtle roughness, scaling, or a slight crust.
The importance of taking baseline early nevus photos of your skin, especially if you have many moles or atypical nevi, cannot be overstated. These photos serve as a personal reference point, allowing for objective comparison over time. Regular self-skin examinations, perhaps monthly, combined with annual professional skin checks by a dermatologist, are the cornerstone of early detection. If any of the subtle changes observed in early nevus photos align with personal observations, prompt medical consultation is advised to ensure timely diagnosis and intervention.
Skin rash nevus Images
The concept of “skin rash nevus images” can be interpreted in several ways, as nevi themselves are not typically rashes. However, nevi can interact with the surrounding skin in ways that might resemble or be accompanied by a rash, or they can be part of broader skin conditions that involve both nevi and rash-like symptoms. It’s crucial to distinguish these scenarios to avoid misdiagnosis and ensure appropriate management.
One common scenario where a nevus can be associated with a “rash-like” appearance is an inflamed nevus. This occurs when a benign nevus becomes irritated or traumatized. The inflammation can manifest as redness, swelling, tenderness, and sometimes itching around the mole. This is often due to friction from clothing, scratching, or minor injury. While usually benign and resolving once the irritant is removed, persistent or recurrent inflammation of a nevus should be investigated, as very rarely, melanoma can present with inflammatory features, or inflammation could mask underlying changes.
Another specific condition is a halo nevus, which can be seen in skin rash nevus images. A halo nevus is a benign melanocytic nevus surrounded by a distinct ring of depigmented, white skin. This “halo” is not a rash but rather an autoimmune phenomenon where the body’s immune system attacks the pigment cells (melanocytes) in and around the mole. While halo nevi are generally benign and common in children, the appearance of a halo around an atypical nevus or a rapidly changing lesion can sometimes be associated with melanoma elsewhere on the body, making careful skin examination important.
Sometimes, a nevus can be located within or near an area affected by a common skin condition, leading to what might appear as skin rash nevus images. For instance, a mole within a patch of eczema (atopic dermatitis) or contact dermatitis might display redness, scaling, and itching characteristic of the rash, affecting the surrounding skin and potentially the nevus itself. In such cases, the nevus itself is not the rash, but it is encompassed by it. It’s important to monitor such nevi closely, as prolonged inflammation could theoretically mask or induce changes.
The appearance of satellite lesions around a primary nevus can sometimes be misinterpreted as a spreading rash. Satellite lesions are small, new pigmented spots that emerge close to a larger mole. While benign satellite nevi can occur, particularly with large congenital nevi, the emergence of new satellite lesions around an atypical or suspicious mole is a significant warning sign for melanoma, indicating local spread. These “pepper-like” lesions or small, new dark spots are not a rash but a pattern of malignant dissemination.
Rarely, certain types of nevi or melanoma can present with unusual inflammatory or erysipeloid (resembling erysipelas, a bacterial skin infection) features that might initially be mistaken for a rash. For example, amelanotic melanoma (melanoma without significant pigment) can sometimes appear as a red, inflamed, or non-healing lesion, mimicking various dermatoses or even a granuloma. Similarly, certain aggressive melanomas can spread Lymphatically, causing red, swollen plaques that might resemble inflammatory conditions. These are critical examples where vigilance for subtle changes is vital.
Conditions that may present with features resembling skin rash nevus images include:
- Nevus Spilus: This lesion consists of a large, uniformly pigmented macule (like a birthmark) with multiple smaller, darker pigmented macules or papules scattered within it. While not a rash, the speckled appearance could be visually perplexing.
- Becker’s Nevus: A common acquired lesion, often appearing as a unilaterally distributed, irregular, hyperpigmented patch, usually hairy, and often developing during adolescence. Its large size and diffuse nature might occasionally be confused with a rash, though it is a benign hamartoma.
- Blue nevus: While not a rash, the deep blue-gray color can sometimes be mistaken for a bruise or an unusual vascular lesion, especially by an untrained eye looking at an isolated “skin rash nevus image.”
- Spitz nevus: As mentioned previously, its rapid growth and reddish-pink, dome-shaped appearance can sometimes be confused with hemangiomas or inflammatory lesions, which could be categorized visually as a “rash-like” bump.
- Inflammatory reactions to trauma: Any nevus, especially those in areas of friction or pressure, can become irritated, leading to localized redness, swelling, and tenderness, mimicking a small inflamed rash around the lesion. This is common on the back, shoulders, or feet.
- Pyogenic granuloma on a nevus: While pyogenic granulomas are benign vascular lesions, they can sometimes grow rapidly on an existing mole. They are typically bright red, often bleed easily, and have an inflammatory appearance, which could be seen as a “rash-like” growth.
It is crucial that any new or changing “rash-like” appearance around a nevus, or any nevus that develops unexplained redness, scaling, oozing, or ulceration, be promptly evaluated by a dermatologist. While many such instances will be benign inflammatory reactions, the possibility of an evolving melanoma or a less common skin cancer manifesting with atypical features cannot be overlooked. The context of “skin rash nevus images” therefore emphasizes the importance of careful observation of the skin surrounding a nevus and any symptomatic changes within the nevus itself.
nevus Treatment
Nevus treatment strategies are diverse, ranging from simple observation to surgical excision, and are primarily guided by the nevus’s characteristics, symptoms, patient concerns, and the dermatologist’s assessment of malignancy risk. The decision for nevus treatment often hinges on whether the lesion is suspicious for melanoma, causes discomfort, or poses a cosmetic concern. Understanding these treatment options is vital for informed patient care.
1. Observation and Surveillance:
For most benign nevi that are asymptomatic and do not exhibit any atypical features, the primary “treatment” is regular self-monitoring and periodic professional surveillance. This involves:
- Self-Skin Exams: Patients are educated on the ABCDEs of melanoma and encouraged to perform monthly self-skin exams, noting any changes in existing moles or the appearance of new ones.
- Dermatological Follow-up: Individuals with numerous moles, a history of atypical nevi, a personal or family history of melanoma, or significant sun exposure are recommended for regular full-body skin examinations by a dermatologist, typically annually or semi-annually.
- Dermoscopy: This non-invasive technique uses a specialized handheld microscope to examine pigmented lesions with magnification, allowing dermatologists to visualize subtle structural features not visible to the naked eye. It significantly improves the accuracy of distinguishing benign nevi from melanoma.
- Total Body Photography: For patients with many moles, baseline total body photography can be used to document the location and appearance of all moles, serving as an objective reference for future comparisons and identifying new or changing lesions.
2. Surgical Excision:
Surgical excision is the gold standard for nevus treatment when there is suspicion of melanoma, significant atypical features, or when a definitive diagnosis is required. It is also used for symptomatic nevi (e.g., repeatedly irritated or bleeding) or for cosmetic reasons. The main types of surgical excision include:
- Excisional Biopsy: This involves removing the entire nevus along with a small margin of surrounding healthy skin. The removed tissue is then sent for histopathological examination to determine its exact nature. This method is preferred for suspicious lesions as it allows for a complete assessment and often provides definitive treatment if the lesion is benign or early-stage melanoma. Sutures are typically required, and a scar will result.
- Shave Excision: For raised, benign-appearing nevi (especially dermal nevi) or for cosmetic removal where malignancy is not suspected, a shave excision can be performed. The nevus is “shaved” off level with the surrounding skin using a scalpel. This procedure is less invasive, does not require sutures, and typically results in a flatter, less prominent scar compared to excisional biopsy. However, it only removes the superficial portion of the nevus, which can be problematic if deeper components are atypical or malignant, making it generally unsuitable for suspicious lesions.
- Punch Biopsy: While not a definitive treatment for an entire nevus, a punch biopsy removes a small cylindrical core of tissue from the lesion. It’s often used for diagnostic purposes when a representative sample is needed, particularly for larger lesions where total excision isn’t practical as an initial step, or when the diagnosis is uncertain. If malignancy is confirmed, further excisional surgery may be necessary.
3. Other Removal Techniques (Less Common for Pigmented Nevi):
Other methods for nevus treatment are generally reserved for non-pigmented, benign lesions or specific types of nevi where malignancy is definitively ruled out. They are typically avoided for suspicious pigmented lesions because they destroy the tissue, preventing histopathological examination, which is crucial for melanoma diagnosis.
- Laser Removal: Used primarily for cosmetic removal of non-pigmented or very superficial pigmented lesions (like freckles or lentigines). It is not recommended for suspicious moles due to the inability to obtain a biopsy for pathology and the risk of incomplete removal.
- Cryotherapy (Freezing): Involves using liquid nitrogen to freeze and destroy benign superficial skin lesions. Similar to laser, it is not used for suspicious pigmented nevi because it destroys tissue and prevents histological analysis.
- Electrocautery/Radiofrequency Ablation: Uses heat to destroy tissue. Again, primarily for benign, non-pigmented lesions where no pathology is needed.
4. Specific Nevus Treatments:
Certain types of nevi may have specific treatment considerations:
- Congenital Nevi: Large or giant congenital nevi may be considered for prophylactic removal due to their increased lifetime risk of melanoma, or for cosmetic reasons. This often involves staged excisions or tissue expanders. Small congenital nevi are usually monitored.
- Atypical Nevi (Dysplastic Nevi): These are usually monitored closely. If they show severely atypical features on dermoscopy or clinical examination, or if they have a history of change, excisional biopsy is often performed.
- Spitz Nevi: Due to their histological resemblance to melanoma, many Spitz nevi, especially those with atypical features, are surgically excised to ensure accurate diagnosis and complete removal, particularly in adults.
Post-Treatment Care and Follow-up:
After any nevus removal, it is crucial to follow the dermatologist’s instructions for wound care to promote healing and minimize scarring. If a biopsy reveals melanoma, further treatment, potentially including wider excisions, sentinel lymph node biopsy, or systemic therapies, will be discussed by a multidisciplinary team. For benign lesions, continued regular skin surveillance remains important, as individuals with one nevus requiring removal may be at higher risk for other skin lesions.
In summary, nevus treatment is individualized. The primary goal is always patient safety, with early detection and appropriate intervention for suspicious lesions being paramount. Cosmetic considerations are secondary but valid reasons for removal, provided malignancy has been confidently ruled out.