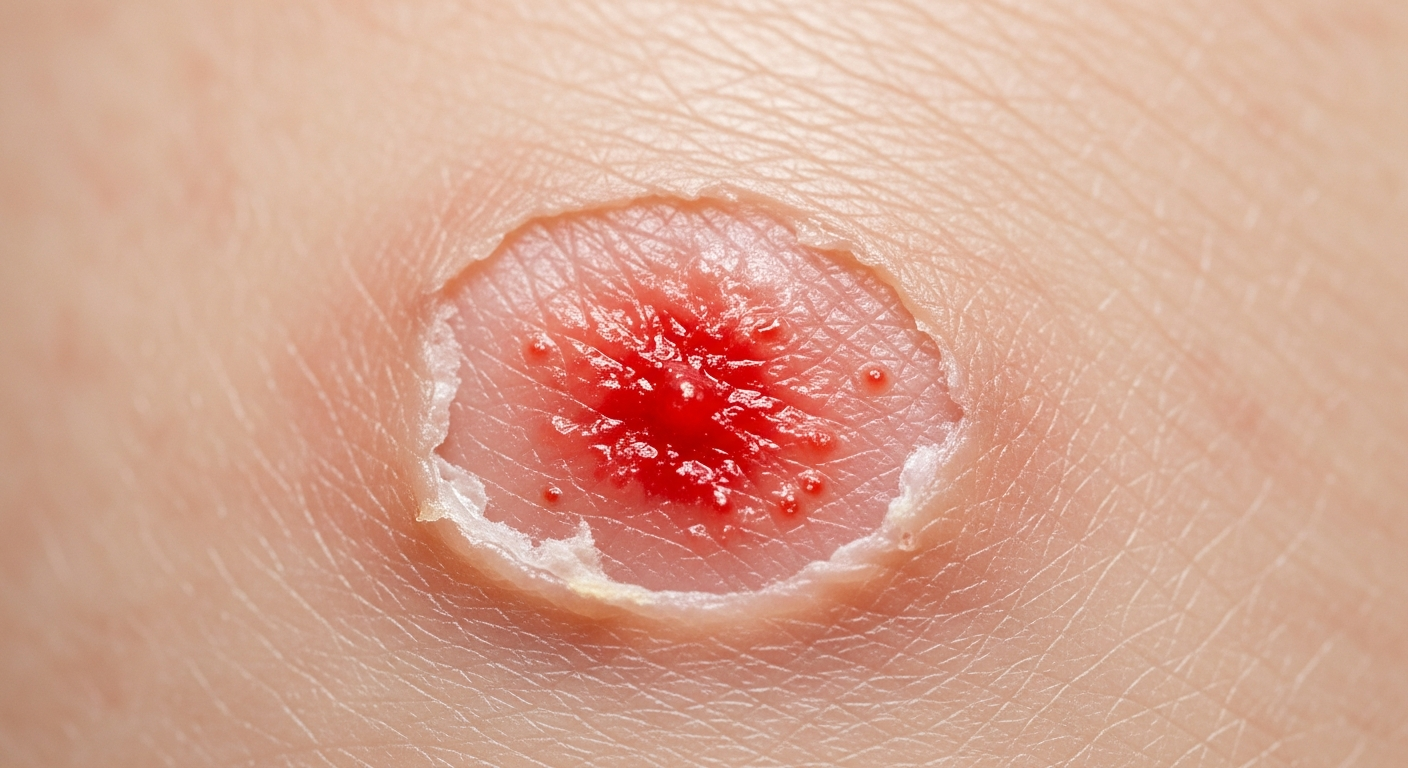
Navigating the visual indicators of a fungal infection is crucial for timely recognition and intervention. This detailed guide offers an extensive look at thrush in men symptoms pictures, providing a comprehensive visual and descriptive reference for identifying this common condition. Understanding these specific manifestations is the first step towards seeking appropriate care and relief from penile candidiasis.
Thrush in men Symptoms Pictures
Identifying Thrush in men symptoms pictures involves recognizing a distinct set of visual and physical indicators that often present on the penis, groin, and surrounding skin. The clinical presentation of male candidiasis can vary in intensity and extent, but several key features are consistently observed. These manifestations are crucial for understanding and diagnosing penile thrush symptoms and male yeast infection pictures, which typically involve inflammation of the glans penis (balanitis) and potentially the foreskin (balanoposthitis).
- Redness and Inflammation (Erythema): One of the most prominent signs in Thrush in men symptoms pictures is significant redness, often appearing as an intense, fiery hue on the glans penis and/or foreskin. This erythema can be widespread, covering the entire tip of the penis, or localized in patches. The inflamed skin often looks shiny or glazed, indicating a heightened inflammatory response. In some cases, the redness extends to the shaft of the penis or the groin folds, presenting as a broader area of irritation.
- Clinical Appearance: The affected area may appear vividly red, sometimes with a purplish tinge, especially in individuals with darker skin tones. The redness is often accompanied by swelling, making the glans appear puffy or distended.
- Associated Discomfort: This inflammation is almost invariably associated with significant discomfort, including burning and itching sensations, particularly after urination or sexual activity.
- Progression: In early stages, the redness might be subtle, but it typically intensifies rapidly as the infection progresses, becoming a hallmark feature in balanitis candida photos.
- Itching (Pruritus): An overwhelming and persistent itch is a cardinal symptom of male thrush. This pruritus is typically localized to the penis, particularly the glans and under the foreskin, but can radiate to the scrotum and groin. The intensity of the itch can range from mild annoyance to severe and debilitating, often leading to scratching, which can further irritate the skin and potentially introduce secondary bacterial infections.
- Pattern of Itching: The itching may be constant or intermittent, often worsening at night or when the area is warm and moist, such as after showering or during sleep.
- Impact on Daily Life: Severe itching can disrupt sleep, concentration, and overall quality of life, becoming a primary complaint among men seeking treatment for male genital candidiasis.
- Burning Sensation: A distinct burning sensation is commonly reported by men with thrush, particularly during and after urination (dysuria) or sexual intercourse. This symptom can be quite distressing and is a direct result of the inflammation and irritation of the delicate skin of the glans and urethra.
- Post-Urination Burn: The acidic nature of urine can exacerbate the burning sensation when it comes into contact with inflamed or broken skin, leading to significant discomfort during micturition.
- Sexual Discomfort: Friction during sexual activity can intensify the burning, making intercourse painful and often discouraging sexual intimacy.
- White, Thick Discharge: A characteristic sign visible in Thrush in men symptoms pictures is the presence of a white, often thick and lumpy discharge from under the foreskin or around the tip of the penis. This discharge is typically odorless or may have a yeasty smell and is often described as resembling cottage cheese or curds.
- Appearance: The discharge can vary in consistency from a thin, milky film to thick, adherent plaques. It may accumulate in the coronal sulcus (the groove behind the glans) and under the foreskin in uncircumcised men.
- Quantity: The amount of discharge can range from minimal to abundant, depending on the severity and duration of the infection.
- Distinction: It is crucial to differentiate this discharge from other penile discharges, such as those associated with sexually transmitted infections (STIs), which may have different colors, consistencies, and odors.
- Small Red Spots or Bumps (Papules and Pustules): In addition to generalized redness, the skin of the glans and shaft may develop small, pinpoint red spots (papules) or fluid-filled bumps (pustules). These lesions are indicative of localized inflammatory responses and can be scattered or clustered.
- Distribution: These spots often appear on the glans itself, around the opening of the urethra, or along the inner surface of the foreskin.
- Evolution: Papules can sometimes evolve into pustules, which may then rupture, leading to small, superficial erosions or ulcers. These features are common in detailed candida balanitis images.
- Pain during Urination or Intercourse (Dysuria and Dyspareunia): The intense inflammation and irritation of the penile skin can lead to significant pain during both urination (dysuria) and sexual intercourse (dyspareunia). This pain is directly related to the contact of urine or friction from sexual activity with the inflamed or excoriated skin.
- Dysuria Specifics: The pain during urination is typically a burning or stinging sensation that occurs as urine passes over the irritated mucous membranes.
- Dyspareunia Specifics: Painful intercourse can be so severe that it discourages sexual activity, further impacting relationships and quality of life.
- Cracked Skin or Fissures: In more severe or prolonged cases of thrush, particularly when the skin is dry or subjected to repeated scratching, the skin on the glans or foreskin can become cracked, leading to small, painful fissures. These tiny cuts can bleed easily and are entry points for secondary bacterial infections.
- Location: Fissures are most commonly seen on the foreskin, especially at the tip or where it retracts, due to the constant movement and stretching.
- Healing: These cracks can be slow to heal without appropriate antifungal treatment, contributing to persistent discomfort.
Signs of Thrush in men Pictures
Delving deeper into the observable signs of Thrush in men pictures reveals specific visual cues that clinicians and individuals can use for diagnosis. These signs often manifest as distinct patterns and textures on the skin, providing critical information beyond just generalized symptoms. Understanding these specific visual pathologies is key to recognizing male candidiasis signs and distinguishing them from other dermatological conditions affecting the genital area. The detailed examination of the affected skin, especially in groin yeast infection pictures and scrotal thrush symptoms, highlights the characteristic presentation of Candida infection.
- Glistening or Shiny Appearance of the Glans: The glans penis, when infected with Candida, often takes on a strikingly glistening or shiny appearance. This is due to the acute inflammation and edema (swelling) of the epidermal layers, which alters the light reflection properties of the skin surface.
- Visual Characteristic: Instead of the usual matte or slightly textured surface, the glans appears taut, stretched, and excessively reflective, often resembling a glazed or varnished surface.
- Underlying Cause: This shininess is a direct result of the inflammatory process, where fluid accumulates in the superficial skin layers, making them appear swollen and smooth.
- White Patches or Plaques: In contrast to the general white discharge, specific white patches or plaques can adhere firmly to the glans or under the foreskin. These are typically composed of accumulated yeast cells, inflammatory exudate, and desquamated epithelial cells.
- Texture: These plaques can be thick, cheesy, and difficult to wipe away, often leaving an erythematous (red) and tender surface underneath if dislodged.
- Distribution: They are commonly found in the coronal sulcus, on the glans, or on the inner surface of the foreskin, especially in uncircumcised men. These are frequently visible in penile yeast infection photos.
- Differentiation: It is important to differentiate these from smegma, which is a natural accumulation of dead skin cells, oils, and moisture that can be easily washed away. Candida plaques are typically more tenacious.
- Satellite Lesions: A highly characteristic sign of candidal skin infections, including those affecting the penis and groin, is the presence of “satellite lesions.” These are small, isolated papules or pustules that appear some distance away from the main, confluent area of redness and rash.
- Appearance: Satellite lesions are typically small, discrete red bumps or pustules, often with a slightly raised border, scattered around the periphery of the primary rash.
- Diagnostic Value: Their presence is a strong indicator of a fungal infection, helping to differentiate candidiasis from other causes of dermatitis or rash. These are crucial details in male thrush image galleries.
- Foreskin Involvement (Balanoposthitis): For uncircumcised men, the foreskin (prepuce) is frequently affected alongside the glans, leading to a condition known as balanoposthitis. The foreskin may become swollen, red, tender, and difficult to retract (phimosis) or to return to its original position after retraction (paraphimosis).
- Swelling: Edema of the foreskin can be significant, causing it to appear puffy and making it challenging or painful to retract.
- Cracking and Fissures: The chronic inflammation and dryness can lead to small cracks or fissures on the foreskin, which are painful and can bleed.
- Discharge Accumulation: The space under the foreskin provides an ideal warm, moist environment for yeast growth, leading to significant accumulation of white discharge.
- Groin and Scrotal Involvement: While penile involvement is primary, the infection can spread to adjacent areas, including the groin folds (inguinal creases) and the scrotum. This manifests as a red, itchy rash, often with distinct borders, and sometimes with the classic satellite lesions. This is particularly relevant when observing groin candidiasis pictures.
- Appearance: The rash in the groin and on the scrotum tends to be intensely red, moist, and often has macerated (softened and whitish from moisture) edges.
- Pruritus: Itching in these areas can be extremely severe, often more so than on the glans itself, due to constant friction and warmth.
- Moisture: The natural folds of the skin in the groin and the warmth of the scrotum create a perfect breeding ground for yeast, exacerbating symptoms.
- Erosions or Superficial Ulcers: In more advanced or neglected cases, the inflamed skin may break down, leading to small, superficial erosions or even shallow ulcers. These represent areas where the integrity of the skin barrier has been compromised.
- Pain: These lesions are typically quite painful, especially upon contact or friction.
- Risk of Secondary Infection: Erosions increase the risk of secondary bacterial infections, complicating the clinical picture and requiring broader treatment.
Early Thrush in men Photos
Recognizing early Thrush in men photos is paramount for prompt treatment and preventing the escalation of symptoms. Initial manifestations of penile candidiasis can be subtle, often mimicking minor irritation or friction. However, understanding these nascent signs can lead to quicker intervention, minimizing discomfort and the potential for complications. Looking for these early indicators, whether it’s the first hint of redness or a slight change in sensation, is key in identifying initial penile yeast infection pictures and understanding the very first signs of male thrush. Early detection can prevent the full-blown inflammatory response often depicted in more advanced mild candidiasis in men presentations.
- Subtle Redness (Mild Erythema): The very first visual sign of thrush is often a mild, barely noticeable redness on parts of the glans penis or under the foreskin. This initial erythema might be localized to a small area, perhaps around the urethral opening or in the coronal sulcus.
- Appearance: Unlike the intense, fiery redness of advanced thrush, early redness is a faint pink or light red, which might be mistaken for normal skin variation or temporary irritation from clothing or hygiene products.
- Consistency: This redness might be intermittent at first, appearing after activities like exercise or sexual intercourse, and then fading, only to return with greater persistence.
- Slight Itching or Tingling Sensation: Before visible signs become prominent, many men report a subtle itching, tingling, or unusual sensation on the glans or foreskin. This feeling might be mild and easily dismissed as minor irritation.
- Description: It’s often described as a tickle, a mild “crawling” sensation, or an infrequent, non-intense itch.
- Timing: This sensation might be more noticeable at specific times, such as in the evening or when the area is warm.
- Dryness or Mild Flakiness: In some instances, early thrush can present as localized dryness or a very fine, subtle flakiness on the skin of the glans or foreskin. This can be easily overlooked or attributed to general skin dryness.
- Texture: The skin might feel slightly rougher to the touch than usual, or small, nearly invisible flakes of skin may be present, particularly after showering.
- Distinction: Unlike common dry skin, this dryness often precedes the development of other, more classic candidal symptoms and may be accompanied by a very mild itch.
- Minimal Discharge or White Film: At the earliest stages, the characteristic thick, lumpy discharge may not be evident. Instead, there might be a very thin, almost translucent white film or a minimal amount of white residue, often only visible upon careful inspection, especially under the foreskin.
- Consistency: This early discharge is usually less curdy and more like a thin, milky coating or a slight accumulation of whitish material in the skin folds.
- Odor: It is typically odorless or has only a very faint, almost imperceptible yeasty smell at this stage.
- Minor Swelling or Puffiness: A very slight degree of swelling or puffiness of the glans or foreskin might be an early indicator. This edema is often subtle and might only be noticeable by touch, making the skin feel slightly firmer or fuller than usual.
- Visual Cue: The glans might appear subtly more rounded or less defined at its edges, without overt signs of acute inflammation.
- Associated Feeling: This minor swelling can contribute to a feeling of tightness or mild pressure, especially if the foreskin is involved.
- Increased Sensitivity or Tenderness: The skin of the glans or foreskin may become unusually sensitive to touch, friction, or temperature changes. This heightened sensitivity can be an early sign that inflammation is beginning.
- Reaction to Stimuli: Patients might notice discomfort with tight underwear, friction during walking, or contact with soap and water during hygiene.
- Early Pain: While not yet full-blown dysuria or dyspareunia, there might be a hint of discomfort during urination or mild sensitivity during sexual activity.
- Isolated Small Red Spots: Sometimes, the very first visible signs are one or two isolated, tiny red spots (papules) on the glans. These are often less than a millimeter in size and can be easily mistaken for minor skin blemishes or folliculitis.
- Distribution: These initial spots might be scattered and not yet form a confluent rash, making them difficult to attribute specifically to thrush without other accompanying symptoms.
- Progression: If untreated, these small spots often multiply and coalesce, forming the more characteristic candidal rash.
Skin rash Thrush in men Images
The skin rash Thrush in men images distinctly illustrate the characteristic dermatological presentation of penile candidiasis. This rash is often the most visually striking and diagnostic feature of the infection, providing clear evidence of yeast proliferation on the skin surface. Understanding the morphology, distribution, and associated features of this rash is crucial for accurate identification, especially when distinguishing it from other types of dermatitis or sexually transmitted infections. The specific appearance of a male yeast infection rash pictures or candida rash on penis photos often involves specific colors, textures, and patterns that are indicative of a fungal etiology. Furthermore, observing groin candidiasis rash images helps to understand the spread and presentation in intertriginous areas.
- Bright Red, Well-Demarcated Rash: The hallmark of a candidal rash on the penis and surrounding areas is its vivid, often fiery red color, with a clear, well-defined border. This distinct border helps to separate the infected skin from healthy skin, although satellite lesions may extend beyond this main perimeter.
- Color Intensity: The redness is typically intense, often described as a vibrant crimson or scarlet, especially in areas of friction or moisture.
- Border Definition: The sharp, clear edges of the rash are a key diagnostic feature, signifying the fungal spread.
- Shiny or Glazed Appearance: The surface of the rash, particularly on the glans penis, frequently appears shiny, glistening, or glazed. This is due to the acute inflammation, epidermal edema, and sometimes a thin, moist exudate on the skin surface.
- Texture: The skin feels taut and stretched, losing its normal texture and appearing unusually smooth and reflective.
- Moisture: The shininess is often more pronounced in warm, moist environments, which are conducive to yeast growth.
- Presence of Satellite Lesions: As previously mentioned, satellite lesions are small, disconnected papules or pustules that “orbit” the main rash. They are a highly characteristic feature of candidal skin infections and are almost pathognomonic when seen with the primary rash.
- Distribution: These smaller lesions are scattered peripherally, often a few millimeters or centimeters away from the main erythematous patch.
- Appearance: They typically start as tiny red bumps (papules) and can sometimes develop into small pus-filled spots (pustules) before resolving or merging into the main rash.
- Erosions and Maceration: In areas where skin rubs against skin (e.g., under the foreskin, in groin folds), the rash can exhibit maceration—a softening and whitening of the skin due to constant moisture. This macerated skin is prone to breakdown, leading to superficial erosions or small ulcerations.
- Appearance of Maceration: The skin takes on a pale, whitish, soggy appearance, often with a wrinkled or boggy texture.
- Erosions: When macerated skin breaks down, it exposes raw, weeping surfaces that are particularly painful and susceptible to secondary infections. These features are prominent in intertriginous candidiasis images.
- Pustules or Vesicles: While not always present, the rash can sometimes include small pustules (pus-filled bumps) or vesicles (small fluid-filled blisters). These typically rupture quickly, leaving behind shallow erosions.
- Content: Pustules contain a yellowish or whitish exudate, signifying an inflammatory response.
- Significance: Their presence indicates a more active inflammatory process and potentially a higher fungal load.
- Fine Scaling at the Edges: As the rash progresses or begins to heal, fine, dry scaling may be observed, particularly at the periphery of the erythematous patches. This indicates epidermal turnover and is a common feature of fungal dermatoses.
- Texture: The scales are usually fine and white, not thick and silvery like those seen in psoriasis.
- Location: While the central part of the rash may remain shiny or moist, the edges might show subtle desquamation.
- Location-Specific Presentations:
- Glans Penis: Often shows the most intense redness, shininess, and potentially white plaques.
- Foreskin: May be significantly swollen, red, and show white discharge or plaques underneath. Fissures are common.
- Coronal Sulcus: A common site for accumulation of white, cheesy discharge and intense redness.
- Shaft of the Penis: The rash may extend to the penile shaft, often as discrete red patches with possible satellite lesions.
- Scrotum and Groin Folds: In these intertriginous areas, the rash is typically very red, moist, well-demarcated, and often features prominent maceration and satellite lesions, indicative of candidal intertrigo. Itching here is often severe.
Thrush in men Treatment
Effectively treating Thrush in men treatment requires a multi-pronged approach, primarily focusing on eliminating the fungal overgrowth and managing associated symptoms. While visual identification from Thrush in men symptoms pictures can be highly suggestive, a medical consultation is always recommended for definitive diagnosis and personalized treatment plans. Early intervention with appropriate antifungal medications, coupled with crucial hygiene and lifestyle adjustments, is key to successful outcomes and preventing recurrence. This section details common and effective strategies for male yeast infection cure, including pharmaceutical options, self-care measures, and preventative steps. Understanding how to manage balanitis candida treatment is essential for long-term relief.
Over-the-Counter (OTC) Antifungal Treatments
For mild to moderate cases of thrush, several readily available OTC antifungal creams and ointments can be highly effective. These products work by directly applying antifungal agents to the affected skin, inhibiting yeast growth. Always follow the product instructions carefully regarding application frequency and duration.
- Clotrimazole (e.g., Canesten, Lotrimin AF):
- Mechanism: An azole antifungal that disrupts the cell membrane of Candida fungi.
- Application: Typically applied thinly to the affected area (glans, foreskin, groin) 2-3 times a day.
- Duration: Treatment usually lasts for 7-14 days, even if symptoms improve earlier, to ensure complete eradication of the fungus.
- Formulations: Available as creams, lotions, and powders. Creams are generally preferred for penile thrush.
- Miconazole (e.g., Daktarin, Desenex):
- Mechanism: Another azole antifungal with similar action to clotrimazole.
- Application: Apply 2-3 times daily.
- Duration: Typically a 7-14 day course.
- Considerations: Some formulations are available as powders which can be useful for moist areas like the groin, but creams are better for direct penile application.
- Tioconazole (e.g., Monistat 1-Day treatment for women, but cream is applicable for men):
- Mechanism: An azole antifungal.
- Application: Often available in higher concentrations for single or short-course applications, but for men, daily application of the cream for 7 days is more common.
- Note: While often marketed for vaginal thrush, the active ingredient in cream form is effective for male candidiasis.
- Terbinafine (e.g., Lamisil):
- Mechanism: An allylamine antifungal that works by interfering with sterol synthesis in the fungal cell membrane.
- Application: Typically once or twice daily.
- Duration: Often a shorter course (e.g., 7 days) may be effective for some cases, but longer use may be needed depending on severity.
- Note: While effective against many fungi, some Candida species may be less susceptible to terbinafine compared to azoles.
Prescription Medications
If OTC treatments are ineffective, or for more severe, recurrent, or widespread infections, a healthcare provider may prescribe stronger topical or oral antifungal medications. These are particularly important for ensuring a complete antifungal cream for men regimen or systemic treatment when needed.
- Stronger Topical Antifungals:
- Nystatin Cream: Often prescribed for candidiasis, particularly effective for mucocutaneous infections. Applied 2-3 times daily for 10-14 days.
- Econazole Cream: Another potent azole antifungal, often used in cases unresponsive to milder OTC options. Applied once or twice daily.
- Topical Corticosteroids (e.g., Hydrocortisone): Sometimes combined with antifungals (e.g., hydrocortisone/clotrimazole combination creams) to reduce severe inflammation and itching. These should only be used for short durations as prescribed, as prolonged use can thin the skin and worsen fungal infections.
- Oral Antifungal Medications:
- Fluconazole (Diflucan): This is the most common oral medication for thrush.
- Dosage: A single dose of 150 mg of fluconazole is often sufficient for uncomplicated male thrush. For recurrent or more severe cases, a doctor might prescribe a longer course or repeated doses.
- Mechanism: Works systemically to kill fungi throughout the body.
- Side Effects: Generally well-tolerated, but can cause nausea, headache, or abdominal pain. Liver function should be monitored with prolonged use.
- Itraconazole: Another oral azole antifungal, used for more resistant or widespread fungal infections. Requires a prescription and careful monitoring.
- Fluconazole (Diflucan): This is the most common oral medication for thrush.
General Hygiene and Self-Care Measures
Complementary self-care practices are vital for both treating an active infection and preventing thrush in men, especially for those prone to recurrence. These measures help to maintain a hostile environment for Candida growth.
- Maintain Excellent Genital Hygiene:
- Washing: Gently wash the penis daily with warm water. Uncircumcised men should carefully retract the foreskin and clean underneath it thoroughly to remove any smegma or yeast build-up.
- Soap: Avoid harsh, perfumed soaps, shower gels, or strong antiseptics, as these can irritate the skin and disrupt the natural flora, making candidiasis worse. Use a mild, pH-balanced cleanser if necessary, or just water.
- Drying: Ensure the genital area is completely dry after washing, especially under the foreskin and in skin folds. Moisture creates an ideal environment for yeast. Pat dry gently with a clean towel.
- Wear Loose-Fitting, Breathable Underwear:
- Material: Opt for cotton underwear, which is breathable and absorbs moisture better than synthetic fabrics.
- Fit: Loose-fitting underwear reduces friction and allows for air circulation, preventing the buildup of heat and moisture that yeast thrives on.
- Change Regularly: Change underwear daily, or more frequently if it becomes damp or sweaty.
- Avoid Irritants:
- Chemicals: Steer clear of perfumed products, bubble baths, spermicides, and lubricants that may contain irritants or allergens.
- Tight Clothing: Avoid tight jeans, trousers, or cycling shorts for prolonged periods, especially if prone to thrush.
- Dietary Considerations:
- Sugar Intake: Some evidence suggests that a high-sugar diet can contribute to yeast overgrowth. Reducing sugar intake may be beneficial, though this is not a primary treatment.
- Probiotics: Consuming probiotic-rich foods (yogurt with live cultures, kefir) or probiotic supplements may help restore a healthy balance of gut flora, potentially indirectly impacting systemic yeast levels.
- Manage Underlying Health Conditions:
- Diabetes: Poorly controlled diabetes is a major risk factor for thrush. Managing blood sugar levels effectively is crucial for preventing recurrence.
- Weakened Immune System: Conditions that compromise the immune system (e.g., HIV, corticosteroid use, chemotherapy) increase susceptibility to candidiasis. Addressing the primary condition is vital.
- Sexual Health Practices:
- Partner Treatment: If your sexual partner has vaginal thrush, they should also be treated to prevent re-infection (ping-pong effect). Using condoms during treatment can also help prevent transmission.
- Sexual Activity: Avoid sexual activity during an active infection to prevent irritation, pain, and transmission to a partner.
When to See a Doctor
While many cases of thrush in men respond well to OTC treatments, it’s important to seek medical advice in certain situations:
- First-Time Symptoms: To confirm the diagnosis and rule out other, potentially more serious conditions (like STIs, bacterial infections, or other dermatological issues).
- No Improvement with OTC Treatment: If symptoms do not improve after 7-14 days of using OTC antifungal creams, stronger treatment or a re-evaluation of the diagnosis may be necessary.
- Recurrent Infections: If you experience thrush frequently (e.g., more than twice in six months), it warrants investigation into underlying causes (e.g., diabetes, immune compromise, re-infection from a partner).
- Severe Symptoms: If the pain, swelling, or redness is severe, or if open sores, ulcers, or fissures develop, prompt medical attention is advised.
- Difficulty Retracting Foreskin (Phimosis) or Returning it (Paraphimosis): These can be complications of severe balanoposthitis and require urgent medical care.
- Other Concerning Symptoms: Any unusual discharge, odor, lumps, or rashes that do not fit the typical description of thrush should be evaluated by a healthcare professional.