Navigating the journey of pregnancy involves a dynamic array of physiological changes, each bringing new sensations and sometimes, visible alterations. This comprehensive guide delves into pregnancy by week symptoms pictures, offering an in-depth look at what to expect as your body transforms to support new life, including specific attention to skin manifestations.
pregnancy by week Symptoms Pictures
The experience of pregnancy is unique for every individual, yet a common spectrum of symptoms emerges as the weeks progress, each signaling profound hormonal and physiological shifts. Understanding these changes can help manage expectations and recognize potential concerns, often providing visual cues that align with your gestational stage.
First Trimester Symptoms (Weeks 1-12):
- Nausea and Vomiting (Morning Sickness): Often beginning around week 4-6, this common symptom can occur at any time of day or night. It’s thought to be primarily due to rising levels of human chorionic gonadotropin (hCG) and estrogen. Visual cues might include pallor or fatigue.
- Breast Changes: Sore, tender, and swollen breasts are among the earliest signs, usually noticeable by week 4. The areolae may darken and enlarge, and veins may become more prominent. Nipple sensitivity is also common.
- Fatigue: Profound tiredness is a hallmark of early pregnancy, driven by increased progesterone levels, lower blood sugar, lower blood pressure, and increased blood production. This often appears as extreme exhaustion, not simply sleepiness.
- Frequent Urination: Starting around week 6-8, the growing uterus puts pressure on the bladder, and increased blood volume leads to more fluid processing by the kidneys.
- Food Aversions and Cravings: Hormonal shifts can dramatically alter taste and smell, leading to strong preferences or dislikes for certain foods.
- Mood Swings: Rapidly fluctuating hormones, especially estrogen and progesterone, can cause heightened emotional sensitivity, leading to periods of irritability, joy, anxiety, or sadness.
- Light Spotting (Implantation Bleeding): A small amount of pinkish or brownish discharge may occur around 6-12 days after conception as the fertilized egg implants in the uterine lining. This is typically lighter and shorter than a menstrual period.
- Headaches: Hormonal changes, fatigue, and increased blood volume can contribute to tension headaches in early pregnancy.
- Dizziness or Lightheadedness: Lower blood pressure and changes in blood volume can lead to feelings of faintness, especially when standing up quickly.
Second Trimester Symptoms (Weeks 13-28):
- Growing Uterus and Baby Bump: The abdomen visibly expands as the baby grows. The fundus (top of the uterus) can typically be felt just below the navel by week 20.
- “Pregnancy Glow”: Increased blood volume and hormonal changes can lead to improved circulation, often giving the skin a radiant appearance.
- Braxton Hicks Contractions: Irregular, mild uterine contractions that feel like a tightening in the abdomen, often starting mid-second trimester. They are usually painless and don’t occur at regular intervals.
- Leg Cramps: Common due to the added weight, changes in circulation, and sometimes mineral deficiencies (e.g., magnesium, calcium).
- Heartburn and Indigestion: The growing uterus displaces organs, and progesterone relaxes the esophageal sphincter, allowing stomach acid to reflux.
- Sciatica: Pressure from the growing uterus and changes in posture can compress the sciatic nerve, causing pain in the lower back, buttock, and leg.
- Nasal Congestion and Nosebleeds: Increased blood volume and estrogen can cause swelling of mucous membranes, leading to stuffiness and occasional nosebleeds.
- Stretch Marks (Striae Gravidarum): Pink, red, or purple lines may appear on the abdomen, breasts, hips, and thighs as the skin stretches rapidly. These often fade to silvery-white after birth.
- Linea Nigra: A dark line running vertically down the abdomen from the navel to the pubic bone, often appearing around week 20. It results from increased melanin production.
- Chloasma (Mask of Pregnancy): Darkening of skin on the face, particularly on the forehead, cheeks, and upper lip, due to increased melanin. Sun exposure can worsen it.
Third Trimester Symptoms (Weeks 29-40+):
- Increased Fatigue: Similar to the first trimester, but now due to the increased physical demands of carrying a larger baby, sleep disturbances, and the body preparing for labor.
- Shortness of Breath: The enlarged uterus pushes up against the diaphragm, reducing lung capacity.
- Swelling (Edema): Especially in the ankles, feet, and hands, due to increased blood volume and pressure from the uterus on pelvic veins.
- Backache: The growing belly shifts the center of gravity, straining back muscles and ligaments.
- Pelvic Pressure: As the baby “drops” or engages in the pelvis, increased pressure on the bladder, pelvis, and perineum is common.
- Varicose Veins and Hemorrhoids: Increased blood volume and pressure on pelvic veins can lead to dilated veins in the legs, vulva, and rectum.
- Frequent Urination: Intensifies as the baby’s head puts more direct pressure on the bladder.
- Sleep Disturbances: Discomfort, frequent urination, leg cramps, and anxiety can disrupt sleep patterns.
- Nipple Leakage (Colostrum): The breasts may begin to produce and leak colostrum, a yellowish pre-milk fluid, as early as week 20, but more commonly in the third trimester.
- Heartburn and Indigestion: Can worsen as the uterus continues to grow and push stomach contents upwards.
Signs of pregnancy by week Pictures
Beyond subjective symptoms, several objective signs of pregnancy become apparent over the weeks, often providing visual confirmation of the developing life within. These signs are frequently observed during clinical examinations or are visible physical changes that become more pronounced as gestation progresses.
Early Physical Signs (Pre-clinical/Self-observed):
- Missed Menstrual Period: The most common initial sign, often leading to a pregnancy test.
- Positive Home Pregnancy Test: Detects hCG in urine, typically reliable a week after a missed period.
- Darkening Areolae and Nipples: Increased pigmentation around the nipples and areolae due to hormonal changes, often noticeable by week 6-8.
- Montgomery’s Tubercles: Small, raised bumps on the areolae that become more prominent. These are sebaceous glands that lubricate the nipple and areola.
- Prominent Veins: Increased blood volume causes veins to become more visible, particularly across the breasts and abdomen.
- Quickening (Fetal Movement): The first perception of fetal movement, usually described as flutters or gas bubbles, typically occurs between week 16-25 (earlier for multiparous women, later for primiparous).
Clinical Signs (Observed by Healthcare Provider):
- Chadwick’s Sign: A bluish discoloration of the cervix, vagina, and labia due to increased blood flow, visible around week 6-8.
- Goodell’s Sign: Softening of the cervix, typically detectable by a doctor around week 4-6.
- Hegar’s Sign: Softening of the lower uterine segment, making the uterus feel disconnected from the cervix, palpable around week 6-12.
- Enlarged Uterus: Palpable uterine enlargement during a pelvic exam. The uterus grows from the size of a pear to the size of a grapefruit by the end of the first trimester.
- Fetal Heartbeat: Can be detected by Doppler ultrasound as early as week 10-12, sometimes earlier with transvaginal ultrasound.
- Ultrasound Visualization:
- Gestational Sac: Visible as early as 4.5 to 5 weeks gestational age.
- Yolk Sac: Visible at 5 weeks, provides nourishment to the embryo.
- Fetal Pole: The first visual sign of a developing embryo, seen around 5.5 to 6 weeks.
- Embryo with Heartbeat: Usually visible and detectable by 6 weeks.
- Crown-Rump Length (CRL): Used to accurately date the pregnancy in the first trimester.
- Ballottement: A technique used in later pregnancy where the examiner taps the uterus, causing the fetus to float upwards and then rebound, confirming the presence of a floating object.
Visible Body Changes Throughout Pregnancy:
- Abdominal Protuberance: The most obvious visual sign, the “baby bump” becomes increasingly prominent from the second trimester onwards. The shape and size vary based on individual body type, muscle tone, and fetal position.
- Postural Changes: As the center of gravity shifts forward, many women adopt a swayback posture (lordosis) to compensate, leading to a more pronounced curve in the lower back.
- Gait Changes (“Pregnancy Waddling”): Relaxin hormone loosens pelvic joints, combined with increased weight, can lead to a wider, waddling gait in the third trimester.
- Facial Edema: Swelling in the face, especially around the eyes, can be a sign of preeclampsia if accompanied by high blood pressure, but mild facial puffiness can also be normal due to increased fluid retention.
- Hair and Nail Changes: Hormonal changes often lead to thicker, shinier hair (reduced shedding phase) and stronger or sometimes more brittle nails.
- Spider Veins (Telangiectasias): Small, red, web-like veins may appear on the face, neck, chest, and arms due to increased estrogen levels.
Early pregnancy by week Photos
The initial weeks of pregnancy, often before many even realize they are pregnant, are a period of rapid and profound transformation at a cellular level. While few external signs are immediately apparent, internal changes lay the groundwork for the entire gestation. Understanding these early shifts is key to appreciating the earliest pregnancy by week photos, even if they’re mainly conceptual until visible symptoms emerge.
Week 1-2 (Conception Period):
- No immediate symptoms: These weeks are counted from the first day of your last menstrual period (LMP) and include ovulation and fertilization. Therefore, no pregnancy symptoms are present.
- Focus: Preparation of the uterine lining, ovulation, and eventual fertilization if conception occurs.
Week 3 (Implantation):
- Fertilization and travel: The fertilized egg (zygote) travels down the fallopian tube, dividing rapidly to become a morula, then a blastocyst.
- Implantation: The blastocyst implants into the uterine wall. This can sometimes cause mild implantation bleeding, which is a key early visual sign that might be mistaken for a light period.
- Early hormonal surge: hCG production begins, though levels are often too low for a positive home pregnancy test.
Week 4 (First Missed Period):
- Missed Period: The most common first sign.
- Positive Pregnancy Test: hCG levels are usually high enough for a positive result.
- Subtle Symptoms:
- Breast tenderness: Mild discomfort or sensitivity.
- Fatigue: A feeling of unusual tiredness.
- Mild cramping: Similar to menstrual cramps but typically less intense.
- Increased vaginal discharge: Often thin, milky-white, due to increased estrogen.
- Embryonic development: The embryo is tiny, about the size of a poppy seed. The neural tube, which will become the brain and spinal cord, starts to form.
Week 5 (Rapid Development):
- Intensified Symptoms:
- Nausea and vomiting (morning sickness): Often begins to appear.
- Increased urination: Kidneys start processing more fluid.
- Heightened sense of smell: Leading to food aversions.
- Mood swings: Hormonal fluctuations become more pronounced.
- Embryonic development: The heart tube is forming and may begin to beat. Arm and leg buds appear. The embryo is about the size of an orange seed.
Week 6 (Heartbeat Detectable):
- Stronger Symptoms: Morning sickness peaks for many. Fatigue remains a dominant symptom.
- Physical signs: Chadwick’s sign (bluish tint to cervix/vagina) may be present. Breasts continue to swell and become more tender.
- Embryonic development: A heartbeat is usually detectable by transvaginal ultrasound. Major organs are beginning to form. The embryo is about the size of a lentil. Neural tube closes.
Week 7 (Visual Growth):
- Continued Symptoms: Nausea, fatigue, and frequent urination persist.
- Early belly changes: While not a visible “bump,” some women may feel slight bloating or a feeling of fullness in the abdomen.
- Embryonic development: The embryo doubles in size. Tiny hands and feet begin to sprout webbed fingers and toes. The brain is developing rapidly. The embryo is about the size of a blueberry.
Week 8 (Facial Features Develop):
- Symptoms remain strong: Many continue to experience morning sickness, food aversions, and fatigue.
- Physical changes: Breasts are visibly larger and heavier. Areolae may be darkening.
- Embryonic development: Eyelids and ears are forming. Limbs are growing longer. The embryo is about the size of a kidney bean.
Week 9 (Transition to Fetus):
- Decreasing Nausea for some: Some women may find morning sickness starts to subside, though it can continue for weeks.
- Embryonic development: All major body parts are in place. The tiny tail is disappearing. The embryo is now officially considered a fetus. The fetus is about the size of a grape.
Week 10 (Organ Systems Refine):
- Visible abdominal changes: For some, the waistline might begin to thicken, requiring looser clothing.
- Symptoms: Heartburn may begin as progesterone relaxes the digestive system. Varicose veins might start to appear for some.
- Fetal development: Vital organs like the kidneys, intestines, brain, and liver are beginning to function. The fetus is about the size of a kumquat.
Week 11 (Refining Features):
- Fetal development: Fingers and toes are fully separated. External genitalia are forming. The fetus is about the size of a lime.
Week 12 (End of First Trimester):
- Symptoms often improve: Many women experience a decrease in first-trimester symptoms like nausea and fatigue, leading to increased energy.
- Visible bump: The uterus is now growing out of the pelvis, and a small baby bump may become noticeable.
- Fetal development: All organ systems are formed and continue to mature. The fetus is about the size of a plum.
Skin rash pregnancy by week Images
Pregnancy brings a myriad of hormonal and immunological changes that can significantly impact the skin, leading to a range of dermatological conditions. While some skin changes like the “pregnancy glow” or linea nigra are physiological, others manifest as itchy rashes, known as pruritic dermatoses of pregnancy, which can be distressing and sometimes indicate underlying health issues. These skin rash pregnancy by week images represent a diverse spectrum of conditions.
Common Physiological Skin Changes:
- Hyperpigmentation:
- Chloasma (Melasma/Mask of Pregnancy): Irregular patches of dark skin on the face (forehead, cheeks, upper lip). Often appears in the second or third trimester. Caused by increased estrogen, progesterone, and melanocyte-stimulating hormone (MSH). Worsened by sun exposure.
- Linea Nigra: A dark vertical line from the navel to the pubic bone. Typically appears from the second trimester. Fades after delivery.
- Areola and Genital Darkening: Nipple and areolae darken significantly. Skin in the genital area and inner thighs also often darkens.
- Stretch Marks (Striae Gravidarum): Pink, red, or purple lines on the abdomen, breasts, hips, and thighs. They occur as the skin stretches rapidly and connective tissues break down. Most common in the third trimester. They eventually fade to silvery-white, but rarely disappear entirely.
- Spider Angiomas (Spider Nevi) and Palmar Erythema: Small, red, spider-like blood vessels on the face, neck, and upper chest, and redness of the palms, respectively. Caused by increased estrogen and blood volume. Usually resolve after delivery.
- Increased Sweating and Oiliness: Hormonal shifts and increased metabolic rate can lead to increased perspiration and sebaceous gland activity, potentially exacerbating acne.
Specific Pruritic Dermatoses of Pregnancy (Itchy Rashes):
1. Pruritic Urticarial Papules and Plaques of Pregnancy (PUPPP) / Polymorphic Eruption of Pregnancy (PEP):
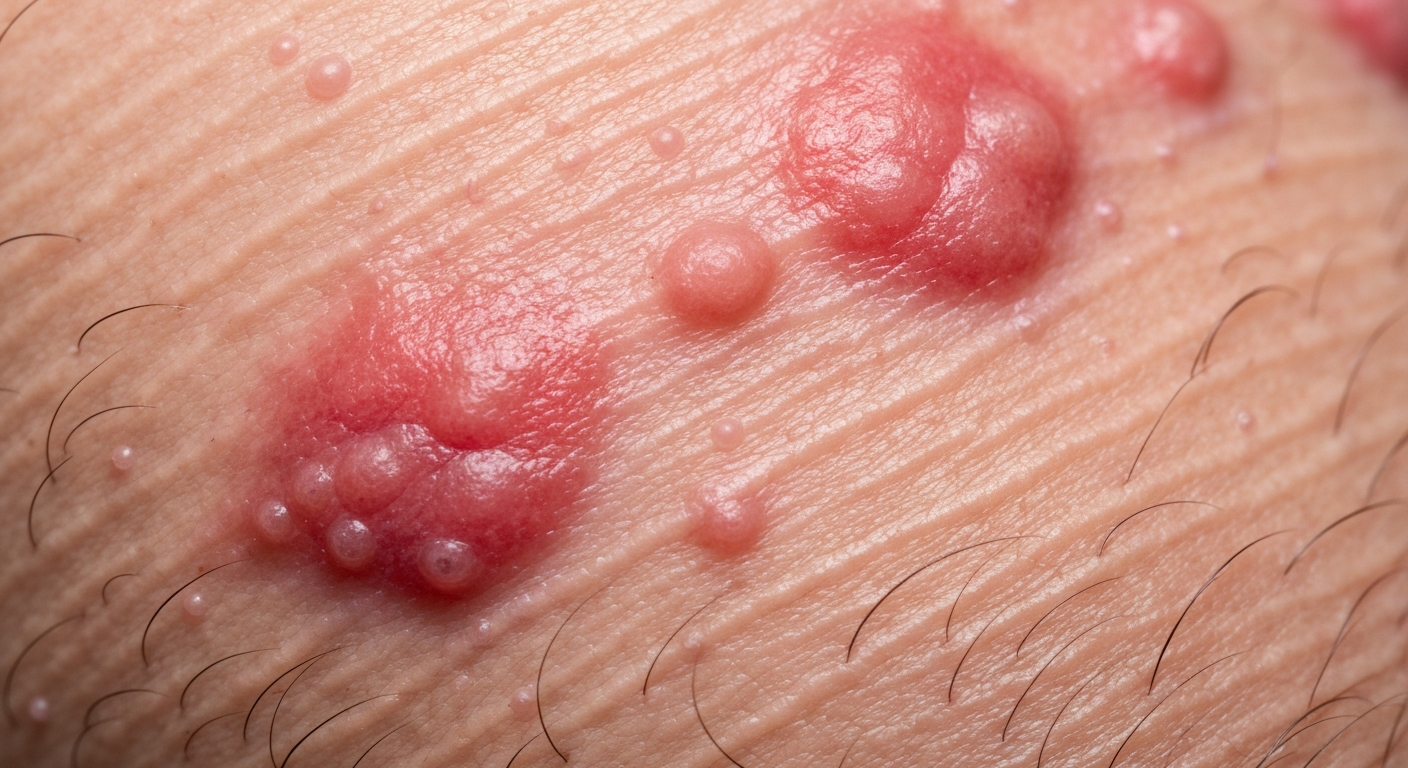
- Description: This is the most common specific dermatosis of pregnancy, affecting about 1 in 160 pregnancies. It typically starts as small, intensely itchy, red papules (hives-like bumps) that coalesce into larger plaques. The lesions may be surrounded by a pale halo. They can evolve into vesicles (small blisters).
- Location: Almost always begins in the stretch marks on the abdomen, especially around the umbilicus, often sparing the periumbilical area itself. It can then spread to the thighs, buttocks, and arms, but rarely involves the face, palms, or soles.
- Onset: Most commonly appears in the late third trimester (around week 35-36) or immediately postpartum. More frequent in first pregnancies and in multiple gestations.
- Associated Symptoms: Extremely pruritic (itchy), often disrupting sleep. No systemic symptoms.
- Cause: Unknown, but theorized to be related to stretching of the abdominal skin and possibly fetal cells invading maternal skin.
- Prognosis: Resolves spontaneously within 1-2 weeks postpartum. Tends not to recur in subsequent pregnancies, or if it does, it’s usually milder.
- Risks: No known risks to mother or fetus.
2. Pemphigoid Gestationis (PG) / Herpes Gestationis (HG):
- Description: A rare but serious autoimmune blistering disease. Starts with intensely itchy urticarial papules and plaques, which rapidly progress to tense blisters (bullae) and vesicles. The lesions are polymorphic.
- Location: Often begins around the navel (periumbilical region), then spreads to the trunk, back, arms, and legs. Face, palms, and soles can be involved. Oral mucosa is usually spared.
- Onset: Most commonly in the second or third trimester, but can appear any time during pregnancy or immediately postpartum. It often flares with subsequent pregnancies, menstruation, or use of oral contraceptives.
- Associated Symptoms: Severe pruritus. Malaise, fever, and headache can occur in severe cases. Diagnosed by immunofluorescence studies showing C3 deposition at the dermal-epidermal junction.
- Cause: Autoimmune, mediated by IgG autoantibodies targeting a component of the basement membrane (BP180, also known as type XVII collagen).
- Prognosis: Typically resolves spontaneously weeks to months postpartum, but can recur in future pregnancies.
- Risks: Associated with increased risk of premature birth and small for gestational age (SGA) infants. Neonatal PG can occur in about 5-10% of cases, presenting as a transient rash on the baby.
3. Intrahepatic Cholestasis of Pregnancy (ICP) / Obstetric Cholestasis (OC):
- Description: While not a primary skin rash, intense generalized pruritus is its hallmark symptom, without a primary skin lesion. The itching can be so severe that excoriations (scratch marks) may be the only visible skin signs. The pruritus is worse at night and often starts on the palms and soles before becoming generalized. Jaundice may develop in about 10-20% of cases.
- Location: Generalized, but often starts on palms and soles.
- Onset: Typically in the late second or third trimester (after week 25).
- Associated Symptoms: Diagnosed by elevated serum bile acids (the key diagnostic marker) and liver enzymes. Fatigue, dark urine, and light-colored stools can also occur.
- Cause: A liver disorder of pregnancy characterized by impaired bile flow. Genetic predisposition and hormonal factors play a role.
- Prognosis: Resolves spontaneously within days to weeks postpartum. Recurrence rate in subsequent pregnancies is high (45-90%).
- Risks: Significant risks to the fetus, including increased rates of spontaneous preterm birth, meconium-stained amniotic fluid, fetal distress, and sudden intrauterine fetal demise (stillbirth). Maternal risks include vitamin K deficiency and postpartum hemorrhage.
4. Atopic Eruption of Pregnancy (AEP):
- Description: A broad term encompassing worsening of pre-existing atopic dermatitis (eczema) or new-onset eczema-like lesions during pregnancy. Presents as dry, itchy, red patches or papules, sometimes with vesicles, crusting, and lichenification (thickening of the skin from chronic scratching).
- Location: Can be diffuse, but often affects the flexural areas (elbow and knee creases), neck, face, and trunk.
- Onset: Can appear any time, but most commonly in the first or second trimester. It is the most common specific skin condition in pregnancy, accounting for about 50% of pregnancy dermatoses.
- Associated Symptoms: Intense itching. Often occurs in women with a personal or family history of atopy (eczema, asthma, hay fever).
- Cause: Believed to be related to immunological changes in pregnancy, particularly a shift towards a Th2 immune response.
- Prognosis: Typically improves after delivery, but can persist. Often recurs in subsequent pregnancies.
- Risks: Generally considered benign for mother and fetus, though severe cases can cause significant discomfort.
5. Prurigo of Pregnancy (PP):
- Description: Characterized by scattered, intensely itchy, excoriated papules or nodules. There are typically no primary urticarial lesions or blisters.
- Location: Most commonly on the extensor surfaces of the limbs (arms and legs) and trunk, but can be generalized.
- Onset: Can occur at any time, but often in the second or third trimester.
- Associated Symptoms: Pruritus leading to scratching and secondary skin lesions (excoriations).
- Cause: Exact cause unknown, sometimes considered a variant of AEP or chronic idiopathic prurigo.
- Prognosis: Usually resolves spontaneously after delivery, but can persist for weeks to months. Often recurs.
- Risks: No known risks to mother or fetus.
6. Impetigo Herpetiformis (IH):
- Description: A rare and severe pustular psoriasis of pregnancy. Presents as widespread, intensely erythematous (red) plaques with sterile pustules (small pus-filled bumps) at the periphery, often coalescing to form polycyclic or annular (ring-shaped) patterns. Lesions are usually painful and burning rather than itchy.
- Location: Typically starts in flexural areas (groin, axillae, under breasts) and spreads to the trunk and limbs. Oral mucosa can be involved.
- Onset: Most commonly in the third trimester, but can occur earlier. Recurrence in subsequent pregnancies is common and often more severe.
- Associated Symptoms: Systemic symptoms are common and severe, including fever, chills, nausea, vomiting, diarrhea, generalized weakness, and hypocalcemia (low calcium). It can also lead to secondary infections.
- Cause: Considered a variant of generalized pustular psoriasis triggered by pregnancy.
- Prognosis: Typically remits spontaneously postpartum, but can be life-threatening if untreated.
- Risks: Significant risks to mother (sepsis, fluid/electrolyte imbalance, acute kidney injury) and fetus (placental insufficiency, fetal distress, stillbirth). Requires urgent medical attention.
It is crucial for any pregnant person experiencing a new or worsening skin rash, especially one that is intensely itchy, painful, or accompanied by systemic symptoms, to seek immediate medical advice. Accurate diagnosis is essential to rule out conditions like ICP or Pemphigoid Gestationis which carry fetal risks, or severe maternal conditions like Impetigo Herpetiformis.
pregnancy by week Treatment
Managing the symptoms of pregnancy by week, including specific skin rashes, requires a careful approach that prioritizes both maternal and fetal well-being. Treatment strategies often involve a combination of lifestyle adjustments, home remedies, and in some cases, safe pharmacological interventions, always under the guidance of a healthcare provider. The goal is to alleviate discomfort, prevent complications, and ensure a healthy pregnancy journey.
General Symptom Management:
- Nausea and Vomiting:
- Eat small, frequent meals to avoid an empty stomach.
- Opt for bland, dry foods (crackers, toast).
- Avoid trigger foods and strong smells.
- Stay hydrated with small sips of water, ginger ale, or clear broths.
- Acupressure wristbands.
- Vitamin B6 (pyridoxine) supplements, sometimes combined with doxylamine (Unisom SleepTabs), under medical supervision.
- For severe cases (Hyperemesis Gravidarum), prescription antiemetics may be necessary.
- Fatigue:
- Prioritize rest and aim for 7-9 hours of sleep per night.
- Take short naps during the day if possible.
- Listen to your body and avoid overexertion.
- Maintain a balanced diet and stay hydrated.
- Gentle exercise, such as walking, can sometimes boost energy.
- Frequent Urination:
- Reduce fluid intake before bedtime, but ensure adequate hydration during the day.
- Avoid diuretics like caffeine.
- Ensure complete bladder emptying when urinating.
- Always mention to your doctor if accompanied by pain or burning, as it could indicate a UTI.
- Heartburn and Indigestion:
- Eat smaller, more frequent meals.
- Avoid trigger foods (spicy, fatty, acidic foods, chocolate, caffeine).
- Stay upright for at least an hour after eating.
- Elevate your head while sleeping.
- Over-the-counter antacids (e.g., calcium carbonate) are generally safe; consult your doctor.
- Backache and Pelvic Pain:
- Maintain good posture.
- Wear supportive, low-heeled shoes.
- Use a maternity support belt.
- Apply warm compresses or take warm baths (not too hot).
- Prenatal yoga or swimming for gentle exercise and stretching.
- Sleep on your side with a pillow between your knees.
- Physical therapy may be recommended for severe cases.
- Swelling (Edema):
- Elevate your feet and legs whenever possible.
- Avoid prolonged standing or sitting.
- Wear comfortable, non-constricting shoes and clothing.
- Stay well-hydrated.
- Compression stockings can help reduce leg swelling.
- Report sudden, severe swelling to your doctor immediately, especially if accompanied by headaches, vision changes, or right upper quadrant pain, as it could be a sign of preeclampsia.
- Leg Cramps:
- Stretch calf muscles before bedtime.
- Stay hydrated.
- Ensure adequate intake of magnesium and calcium through diet or supplements, under medical advice.
- Massage the affected muscle.
- Walk around to improve circulation.
Treatment for Specific Skin Rashes in Pregnancy:
1. Pruritic Urticarial Papules and Plaques of Pregnancy (PUPPP/PEP) Treatment:
- Topical Corticosteroids: Mid-potency corticosteroids (e.g., triamcinolone) are the mainstay for reducing inflammation and itch. Stronger corticosteroids may be used for severe cases under medical supervision.
- Oral Antihistamines: Non-sedating (e.g., loratadine, cetirizine) or sedating (e.g., diphenhydramine) antihistamines can help alleviate pruritus, especially at night.
- Emollients and Moisturizers: Frequent application of plain, unscented moisturizers can soothe dry, irritated skin.
- Cool Compresses and Baths: Lukewarm colloidal oatmeal baths can provide temporary relief from itching.
- Oral Corticosteroids: For very severe, widespread cases, a short course of oral corticosteroids (e.g., prednisone) may be prescribed by a dermatologist, with careful consideration of gestational age and potential side effects.
- Dietary Considerations: Some anecdotal reports suggest a gluten-free diet may help, though scientific evidence is lacking.
2. Pemphigoid Gestationis (PG/HG) Treatment:
- Systemic Corticosteroids: Oral prednisone is the primary treatment for active disease, often started at moderate to high doses and tapered as symptoms improve. This is essential to control blistering and intense itching, and to potentially reduce fetal risks.
- Topical Corticosteroids: High-potency topical steroids can be used for localized lesions or as an adjunct to systemic therapy.
- Oral Antihistamines: For symptomatic relief of itching.
- Immunosuppressants: In very rare, severe, or steroid-refractory cases, other immunosuppressants (e.g., azathioprine, cyclosporine) might be considered postpartum or in cases where risks outweigh benefits for the fetus, but this is highly specialized management.
- Monitoring: Close monitoring of both mother and fetus is crucial due to potential for preterm birth and SGA infants.
3. Intrahepatic Cholestasis of Pregnancy (ICP/OC) Treatment:
- Ursodeoxycholic Acid (UDCA): This is the first-line and most effective treatment. It helps improve liver function, reduces bile acid levels, and significantly alleviates itching. It also improves fetal outcomes.
- Antihistamines: Can offer some symptomatic relief from itching, though often less effective than UDCA for ICP-related pruritus.
- Topical Agents: Calamine lotion or menthol creams might provide temporary soothing.
- Vitamin K Supplementation: Recommended for the mother (and sometimes the newborn) to prevent hemorrhagic complications due to impaired fat-soluble vitamin absorption.
- Fetal Monitoring: Intensive fetal surveillance is critical, including non-stress tests, biophysical profiles, and regular ultrasounds, due to the increased risk of adverse fetal outcomes. Early induction of labor is often considered around 36-37 weeks depending on bile acid levels and other factors.
- Dietary Adjustments: A low-fat diet may be recommended.
4. Atopic Eruption of Pregnancy (AEP) / Prurigo of Pregnancy (PP) Treatment:
- Emollients and Moisturizers: Regular and generous application to maintain skin barrier function and reduce dryness and itch.
- Topical Corticosteroids: Low to mid-potency topical steroids are generally safe and effective for treating inflamed areas.
- Oral Antihistamines: For symptomatic relief of itching.
- Wet Wraps: Applying wet dressings over corticosteroid-treated areas can enhance penetration and reduce itching.
- Avoid Triggers: Identify and avoid irritants (e.g., harsh soaps, synthetic fabrics, specific allergens).
- Phototherapy (UVB): Narrowband UVB phototherapy can be considered for widespread or refractory cases, under specialist guidance.
5. Impetigo Herpetiformis (IH) Treatment:
- Systemic Corticosteroids: Oral prednisone is the cornerstone of treatment and should be initiated promptly and at high doses to control the disease and prevent life-threatening complications.
- Calcium and Vitamin D Supplementation: Crucial to correct hypocalcemia, which is common and potentially dangerous.
- Fluid and Electrolyte Management: Essential due to systemic inflammation and potential for dehydration.
- Antibiotics: For secondary bacterial infections of the skin.
- Monitoring: Close maternal and fetal monitoring in a hospital setting is often required due to the severity of the condition and potential for complications.
General Skincare and Prevention during Pregnancy:
- Gentle Cleansing: Use mild, unscented soaps and lukewarm water.
- Moisturize Regularly: Apply thick, emollient creams or lotions, especially after bathing. This can help prevent dryness and reduce the appearance of stretch marks, though not entirely.
- Sun Protection: Use broad-spectrum sunscreen with an SPF of 30 or higher daily, wear protective clothing, and seek shade to minimize hyperpigmentation (chloasma) and protect against UV damage.
- Avoid Harsh Chemicals: Steer clear of retinoids (retinol, tretinoin), hydroquinone, and salicylic acid in high concentrations, as these are generally not recommended during pregnancy. Consult your dermatologist for pregnancy-safe alternatives.
- Stay Hydrated: Drinking plenty of water helps maintain skin elasticity and overall health.
- Nutritious Diet: A diet rich in vitamins, minerals, and antioxidants supports healthy skin and overall well-being.
- Consult Your Healthcare Provider: Always discuss any new or worsening symptoms, especially skin rashes, with your obstetrician or dermatologist. Self-treating can be risky during pregnancy, and proper diagnosis is paramount for appropriate and safe management.