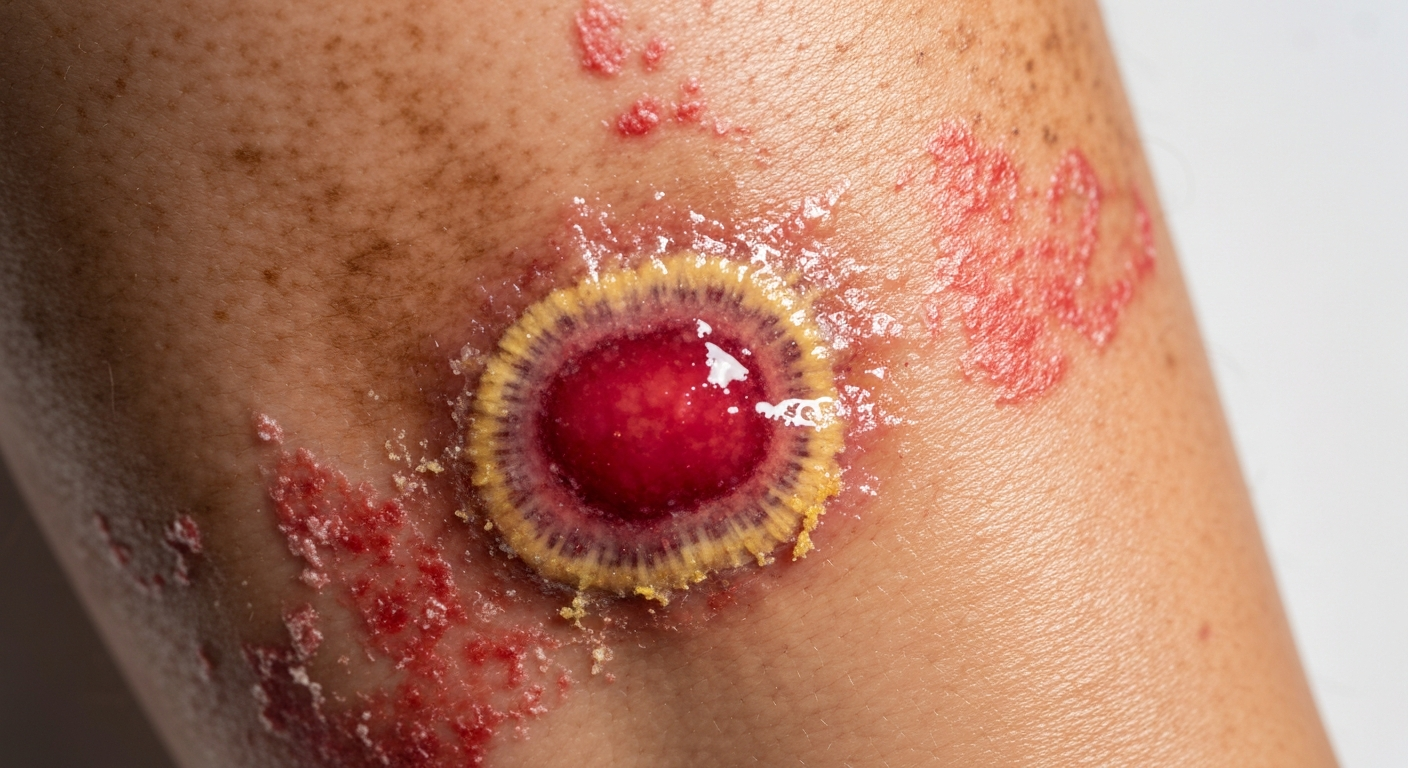
When examining various `trophic ulcer symptoms pictures`, it is critical to understand the diverse visual manifestations of these chronic wounds. This comprehensive guide details the observable characteristics, progression, and associated skin changes, crucial for accurate identification and management of `trophic ulcer images`.
trophic ulcer Symptoms Pictures
Analyzing `trophic ulcer symptoms pictures` reveals a complex array of visual cues indicative of deep tissue damage and impaired healing. These images typically showcase open wounds, often irregularly shaped, that penetrate into the dermis and deeper subcutaneous tissues. The appearance can vary significantly based on the underlying etiology, but common features include a necrotic base, slough, granulation tissue, and variable exudate. The wound edges may be ill-defined or sharply demarcated, sometimes undermined, and the surrounding skin often presents with distinct changes reflecting chronic inflammation or ischemia. Pain levels associated with these `chronic wound images` are also highly variable, ranging from excruciating in arterial ulcers to minimal in neuropathic ulcers due to nerve damage. Understanding these visual distinctions is paramount for healthcare professionals and patients alike when confronted with `skin lesion photos` or `wound deterioration pictures` requiring intervention.
The morphology of a trophic ulcer in `trophic ulcer photos` often depends on its origin:
- Venous Ulcers: Commonly found on the medial aspect of the lower leg, particularly around the malleolus. These `venous ulcer signs` often present as shallow, irregularly shaped wounds with a ruddy, granulating base. The surrounding skin typically shows signs of chronic venous insufficiency, including hemosiderin staining (a brownish discoloration), lipodermatosclerosis (hardening and tightening of the skin), edema, and sometimes eczema or dermatitis. Exudate is usually moderate to high, often serous or seropurulent. Pain is generally moderate and often relieved by elevation.
- Arterial Ulcers: These ulcers, depicted in `arterial ulcer appearance` images, are frequently located on the toes, heels, and anterior tibial area. They are typically “punched-out” in appearance with regular, well-demarcated borders and a pale, often necrotic or fibrinous base. The surrounding skin is usually cool to the touch, shiny, hairless, and atrophic, often appearing pale or cyanotic. `Ischemic wound photos` will highlight pallor and absence of granulation tissue. Pain is often severe, especially at night or with leg elevation, and is a hallmark symptom of `peripheral artery disease ulcers`.
- Neuropathic Ulcers (Diabetic Foot Ulcers): Predominantly found on the plantar surface of the foot, especially under pressure points like the metatarsal heads or heels, these `diabetic ulcer symptoms` are typically painless due to neuropathy. They are often surrounded by thick calluses, which can mask the underlying ulcer. The ulcer itself may be deep, sometimes extending to bone, and can have a clean, granulating base or a sloughy, infected appearance. `Diabetic foot lesion pictures` often show characteristic deep, round wounds with minimal surrounding inflammation unless infected.
- Pressure Ulcers (Decubitus Ulcers): Occur over bony prominences subject to prolonged pressure, such as the sacrum, ischium, greater trochanter, and heels. Their appearance in `pressure ulcer stages photos` varies greatly by stage, from intact skin with non-blanchable erythema (Stage 1) to full-thickness tissue loss with exposed bone or muscle (Stage 4). The ulcer base can be sloughy, necrotic, or granulating, and the shape often reflects the pressure point.
- Mixed Etiology Ulcers: Many `leg ulcer visual signs` are a combination of the above, presenting complex features that make diagnosis challenging without a thorough clinical assessment.
When observing `trophic ulcer symptoms pictures`, specific details related to the wound bed composition are crucial. The types of tissue present within the ulcer base directly inform the wound’s healing trajectory and guide treatment strategies:
- Necrotic Tissue (Eschar): This appears as dark, leathery, often black tissue, representing dead tissue. Its presence in `necrotic wound images` indicates non-viable tissue that impedes healing and often harbors bacteria. Removal of eschar is typically a primary goal in wound management to facilitate granulation.
- Slough: Often yellow, tan, gray, or green, slough is soft, moist, devitalized tissue composed of fibrin, pus, and cellular debris. It can be stringy or gel-like. `Sloughy wound pictures` show this material adhering to the wound bed, often indicating an impediment to granulation and a potential nidus for infection.
- Granulation Tissue: This is healthy, beefy red, moist, and shiny tissue comprised of new capillaries, fibroblasts, and collagen. It is a sign of healing and fills the wound defect from the bottom up. `Granulation tissue photos` signify a positive healing response, although excessive granulation (hypergranulation) can also occur.
- Epithelial Tissue: Appears as light pink or pearly white tissue, usually originating from the wound edges or hair follicles. This is the final stage of wound closure. `Epithelialization pictures` show the wound margins advancing inward, signaling successful re-epithelialization.
- Hypergranulation (Proud Flesh): An overgrowth of granulation tissue that extends above the wound margins, preventing epithelialization. It is often moist and friable. `Hypergranulation images` demonstrate an imbalance in the healing process requiring intervention.
- Undermining and Tunneling: These are extensions of the ulcer under the wound edges or into deeper tissues, respectively. `Undermining wound photos` show the skin lip overhanging the wound bed, suggesting a more extensive wound beneath the surface. Tunneling indicates deeper, narrower tracts.
Signs of trophic ulcer Pictures
Distinct `signs of trophic ulcer pictures` go beyond the immediate wound bed, encompassing changes in the periwound skin and the affected limb that provide vital diagnostic clues. These visual indicators help differentiate ulcer types and guide targeted interventions. Identifying these subtle yet significant `skin damage images` is crucial for understanding the overall impact of the underlying disease process on the integumentary system. For instance, `wound infection signs` are often present in the periwound area before systemic symptoms manifest, making visual assessment paramount. The characteristics of the surrounding skin often tell a story about the ulcer’s etiology and its chronicity, making `leg ulcer visual signs` a critical part of the diagnostic process.
Key observable signs in `trophic ulcer photos` include:
- Periwound Skin Discoloration:
- Hemosiderin Staining: A brownish or reddish-brown discoloration, particularly prominent in `venous ulcer signs photos`. This results from the breakdown of hemoglobin in red blood cells that have leaked out of incompetent veins, staining the skin. It indicates chronic venous hypertension.
- Pallor or Cyanosis: A pale or bluish discoloration of the skin, common in `arterial ulcer images`. This indicates poor arterial blood flow and tissue ischemia. The affected limb may appear lifeless.
- Erythema: Redness around the wound, which can indicate inflammation, infection (`wound infection signs`), or early pressure damage. Spreading erythema with warmth and tenderness suggests cellulitis.
- Livedo Reticularis: A net-like, purplish discoloration, sometimes seen in severe arterial disease or vasculitic conditions. It indicates impaired microcirculation.
- Skin Temperature Changes:
- Cool to Cold Skin: Associated with `arterial insufficiency ulcers` due to reduced blood flow. The limb distal to the ulcer will often feel noticeably cooler than the unaffected limb.
- Warm to Hot Skin: Common in infected ulcers or those with significant inflammation, such as cellulitis around a `diabetic foot lesion`. This indicates an active inflammatory response or bacterial proliferation.
- Skin Texture and Integrity:
- Induration: Hardening or thickening of the periwound skin, often palpable. In venous disease, this can lead to lipodermatosclerosis, where the skin becomes tough and wood-like. `Lipodermatosclerosis images` show a characteristic “inverted champagne bottle” appearance of the lower leg.
- Atrophy: Thinning and loss of elasticity of the skin, making it fragile and shiny. Common in areas of chronic arterial insufficiency or prolonged steroid use. `Atrophic skin photos` highlight the delicate, easily damaged nature of the epidermis.
- Hair Loss: Absence of hair on the toes and dorsum of the foot is a common `peripheral vascular disease sign`, indicating poor arterial perfusion.
- Nail Changes: Thickened, brittle, slow-growing nails, often discolored, are seen in chronic arterial insufficiency and fungal infections. `Ischemic nail changes pictures` illustrate this dystrophy.
- Maceration: Softening and whitening of the skin, particularly around wounds with high exudate. This makes the skin fragile and susceptible to further breakdown. `Macerated skin images` show wrinkled, often pale tissue surrounding the wound.
- Callus Formation: Thickened areas of hardened skin, particularly around `neuropathic ulcer signs` on the plantar surface of the foot. These calluses often obscure underlying ulcers and increase pressure.
- Edema:
- Pitting Edema: Swelling that retains an indentation after pressure is applied. Common in venous insufficiency and systemic fluid overload. `Pitting edema photos` clearly show the persistent indentation.
- Non-Pitting Edema: Swelling that does not indent. Can be associated with lymphedema or severe lipodermatosclerosis.
- Pulses and Capillary Refill:
- Diminished or Absent Pulses: A critical sign in `arterial ulcer assessment`. Palpation of dorsalis pedis and posterior tibial pulses provides insight into arterial flow. `Doppler ultrasound images` can confirm pulse presence and flow.
- Prolonged Capillary Refill Time (CRT): If the toenail bed takes longer than 3 seconds to return to its normal color after being blanched, it indicates poor arterial perfusion, a key `peripheral ischemia sign`.
- Pain Characteristics:
- Severe Rest Pain: A hallmark of `critical limb ischemia` and arterial ulcers, often worse at night or with elevation.
- Minimal or Absent Pain: Characteristic of `diabetic neuropathic ulcers` due to nerve damage, which unfortunately contributes to delayed presentation and increased severity.
- Dull, Aching Pain: Typically associated with `venous stasis ulcers`, often worse with prolonged standing and relieved by elevation.
Early trophic ulcer Photos
Identifying `early trophic ulcer photos` is crucial for preventing progression to chronic, complex wounds. These initial stages often present subtly, making early detection challenging but vital for timely intervention and improved outcomes. `Initial ulcer formation photos` may not always show an open wound but rather pre-ulcerative skin changes that signal impending tissue breakdown. Understanding these nascent signs can help differentiate a minor skin irritation from a developing `incipient ulcer image`. Early detection can significantly reduce the morbidity associated with `trophic ulcer development` and prevent the severe complications often seen in advanced stages.
The progression from intact skin to an early trophic ulcer involves several distinct visual changes:
- Stage 1: Non-blanchable Erythema (Pre-ulcerative skin changes):
- Persistent Redness: The earliest sign, especially for pressure ulcers, is a localized area of intact skin with persistent non-blanchable redness. This means the skin does not turn white when pressed, indicating underlying tissue damage. `Non-blanchable erythema pictures` show this discoloration, which may appear differently in darkly pigmented skin (e.g., persistent purple or blue tint).
- Skin Warmth or Coolness: The area might feel warmer or cooler to the touch compared to adjacent skin, signaling altered circulation or inflammation.
- Edema and Induration: Localized swelling or hardening of the skin may be present before any visible break in skin integrity.
- Pain or Itching: Patients may report discomfort, tingling, or itching in the affected area, indicating sensory changes.
- Stage 2: Partial-Thickness Skin Loss:
- Shallow Open Ulcer: At this stage, `minor skin breaks` occur, manifesting as a shallow open ulcer with a red-pink wound bed, without slough or bruising. This indicates partial-thickness loss of the dermis.
- Blister Formation: May also present as an intact or ruptured serum-filled blister, which is a key `early skin breakdown image`. Blood-filled blisters suggest deeper tissue damage.
- Abrasion or Tear: Superficial abrasions or skin tears can also be early presentations, particularly in fragile skin. These are often seen in `skin tear photos` on the lower extremities.
- Epidermal Peeling: The superficial layer of the skin may peel away, revealing the tender underlying dermis.
- Early Neuropathic Changes:
- Callus Formation: For `diabetic foot ulcer images`, early signs often include the development of thick calluses over pressure points. These calluses can initially protect the skin but also mask underlying tissue necrosis or can become the site of hemorrhage, leading to ulceration. `Callus development pictures` show the progression of hardened skin.
- Fissures within Callus: Cracks or fissures within a thick callus can be a precursor to deeper ulceration, allowing pathogens to enter.
- Localized Redness or Bruising: Subtle redness or discoloration beneath a callus can indicate localized trauma or pressure, an early `pressure point damage sign`.
- Absence of Pain: Due to neuropathy, the patient may not feel any discomfort, allowing the ulcer to progress undetected until significant damage has occurred.
- Early Arterial Changes:
- Intermittent Claudication: While not directly visible, patients experience leg pain during exertion that is relieved by rest. This is an early `peripheral arterial disease symptom`.
- Dependent Rubor: Redness that appears when the leg is in a dependent position and fades with elevation, indicating severe arterial insufficiency. `Dependent rubor pictures` capture this color change.
- Delayed Wound Healing: Any minor cut or abrasion that fails to heal within a normal timeframe should raise suspicion for underlying arterial disease. `Non-healing wound photos` can represent an early arterial issue.
- Small, Painful Pustules or Blisters: These can sometimes precede a punched-out arterial ulcer, signaling localized ischemia.
- Early Venous Changes:
- Ankle Flare (Corona Phlebectatica): A fan-shaped pattern of small veins on the medial or lateral aspect of the ankle. This is an early `venous insufficiency sign`.
- Eczematous Skin Changes: Red, scaly, itchy patches, or `stasis dermatitis pictures`, often around the ankles, indicating chronic venous hypertension and inflammation.
- Edema: Swelling of the lower leg and ankle, especially after prolonged standing, which resolves with elevation. This `pitting edema picture` can be an early indicator of venous dysfunction.
- Hyperpigmentation: Subtle brownish discoloration (hemosiderin staining) that begins to appear around the ankles before overt ulceration.
Skin rash trophic ulcer Images
While a trophic ulcer itself is not a “skin rash,” the periwound skin, or skin surrounding the ulcer, frequently exhibits a variety of inflammatory and reactive changes that can resemble or be mistaken for a rash. These `trophic ulcer associated skin changes` are crucial to identify as they can exacerbate the wound, impede healing, or signal infection. Understanding the appearance of `periwound dermatitis images` and other reactive skin conditions around `leg ulcer rash photos` is vital for comprehensive assessment and management. These manifestations are often a direct consequence of chronic inflammation, edema, infection, or contact reactions related to wound care products, making the differential diagnosis in `skin irritation around wound` scenarios complex.
Common “rash-like” appearances and skin changes observed around `trophic ulcer images` include:
- Stasis Dermatitis (Venous Eczema):
- Appearance: Red, scaly, itchy, and sometimes weeping patches of skin, typically located around the ankles and lower legs. `Stasis dermatitis pictures` often show inflamed, thickened skin with crusting and excoriations from scratching.
- Association: Primarily associated with `venous insufficiency ulcers`. It results from chronic venous hypertension, leading to inflammation and breakdown of skin barrier function.
- Impact: Can significantly increase discomfort and itching, potentially leading to secondary skin breakdown or infection due to scratching.
- Contact Dermatitis:
- Appearance: Erythematous, pruritic, sometimes blistering or weeping rash, localized to areas where a topical agent or dressing material has been applied. `Allergic contact dermatitis photos` show clear patterns conforming to the application area.
- Association: Can occur around any `chronic wound image` due to sensitivity to wound care products (e.g., antiseptics, adhesives, preservatives in creams, dressing components).
- Impact: Causes significant irritation and discomfort, requiring identification and removal of the offending agent. Can delay wound healing if not addressed.
- Cellulitis / Erysipelas:
- Appearance: A rapidly spreading area of redness, warmth, swelling, and tenderness, often with ill-defined borders (cellulitis) or sharply demarcated, raised borders (erysipelas). `Cellulitis leg ulcer pictures` highlight the spreading erythema radiating from the wound.
- Association: A common bacterial infection of the skin and subcutaneous tissue, often originating from `wound infection signs` or skin breaks near the ulcer.
- Impact: Requires urgent antibiotic treatment as it can lead to systemic infection (sepsis) and further tissue damage.
- Folliculitis:
- Appearance: Small, red bumps or pustules centered around hair follicles. `Folliculitis images` show localized inflammation often associated with hair growth areas.
- Association: Can occur in the periwound area, especially in areas of chronic moisture or irritation from dressings.
- Impact: Can be itchy or tender and, if left untreated, can progress to abscesses.
- Fungal Infections (e.g., Candidiasis, Tinea Pedis):
- Appearance: Red, itchy, scaly patches, sometimes with satellite lesions (candidiasis), or interdigital scaling and maceration (tinea pedis). `Fungal infection skin images` show characteristic patterns of infection.
- Association: Common in moist, macerated periwound skin, especially under occlusive dressings or in patients with diabetes.
- Impact: Causes itching and discomfort, can contribute to skin breakdown, and must be treated with antifungals.
- Livedo Reticularis:
- Appearance: A mottled, purplish, net-like pattern on the skin. `Livedo reticularis images` clearly show this reticulated discoloration.
- Association: Not a rash in the typical sense, but a vascular pattern indicative of compromised microcirculation. It is often seen in conditions causing `arterial insufficiency`, vasculitis, or cold exposure.
- Impact: A visual sign of underlying vascular pathology that contributes to poor wound healing.
- Hemosiderin Staining:
- Appearance: Diffuse brownish or reddish-brown discoloration, particularly in the lower leg, often referred to as “brawny edema” when combined with induration. `Hemosiderin staining pictures` reveal the chronic discoloration.
- Association: A classic sign of `chronic venous insufficiency`, resulting from the extravasation of red blood cells and deposition of iron pigment (hemosiderin) in the dermis.
- Impact: While not a rash, it is a persistent cosmetic concern and a marker of long-standing venous disease, indicating a high risk for `venous ulcer development`.
- Purpura/Ecchymoses:
- Appearance: Purple or reddish-brown non-blanchable patches or spots due to bleeding into the skin. `Purpuric lesions images` vary in size and distribution.
- Association: Can be seen in various conditions, including vasculitis, anticoagulant therapy, or severe trauma, and may precede skin breakdown in fragile skin.
- Impact: Indication of vascular fragility or bleeding disorders, potentially leading to increased wound exudate or impaired healing.
trophic ulcer Treatment
Effective `trophic ulcer treatment` demands a multifaceted approach, directly informed by the visual cues observed in `trophic ulcer symptoms pictures` and a thorough understanding of the underlying etiology. The primary goals are to promote healing, manage infection, alleviate pain, and prevent recurrence. Successful `wound care management` involves not only local wound treatment but also systemic interventions to address the root cause, ensuring that the visual signs of improvement in `wound healing progression photos` are sustained. A comprehensive `ulcer healing strategy` integrates debridement, appropriate dressing selection, and management of the periwound skin, which may show `trophic ulcer associated skin changes`.
Key components of `trophic ulcer therapy` include:
- Addressing the Underlying Cause: This is the most critical step and varies by ulcer type:
- Venous Ulcers: `Venous insufficiency ulcer treatment` primarily involves compression therapy (e.g., compression bandages, stockings) to counteract venous hypertension and reduce edema. Leg elevation and exercise are also important. Surgical interventions like vein ablation may be considered.
- Arterial Ulcers: `Arterial ulcer interventions` focus on improving blood flow to the affected limb. This often involves revascularization procedures such as angioplasty, stenting, or bypass surgery. Risk factor modification (smoking cessation, diabetes control, hypertension management) is vital.
- Neuropathic Ulcers (Diabetic Foot Ulcers): `Diabetic ulcer therapy` centers on offloading pressure from the ulcerated area (e.g., total contact casts, specialized footwear, crutches). Strict glycemic control is essential. Regular foot inspections and protective footwear are crucial for prevention.
- Pressure Ulcers: `Pressure ulcer prevention and treatment` involves frequent repositioning, pressure-relieving support surfaces, meticulous skin care, and nutritional support.
- Wound Bed Preparation: This aims to create an optimal environment for healing, often guided by visual assessment of `wound bed images`:
- Debridement: Removal of necrotic tissue and slough, which can impede healing and harbor bacteria.
- Surgical Debridement: Rapid removal of non-viable tissue, often necessary for heavily necrotic or infected wounds.
- Enzymatic Debridement: Application of topical enzymes to chemically digest necrotic tissue and slough over time.
- Autolytic Debridement: Using the body’s own enzymes, facilitated by moisture-retentive dressings, to break down non-viable tissue.
- Mechanical Debridement: Use of wet-to-dry dressings or pulsed lavage (less common now).
- Biological Debridement (Maggot Therapy): Application of medical-grade maggots to selectively consume necrotic tissue and bacteria.
- Infection Control: Management of bacterial load within the ulcer and surrounding skin.
- Topical Antimicrobials: Used for localized infection (e.g., silver dressings, iodine-impregnated dressings), particularly when `wound infection signs` are present.
- Systemic Antibiotics: Indicated for spreading cellulitis, deep tissue infection, osteomyelitis, or systemic signs of infection (fever, malaise), identified from `cellulitis leg ulcer pictures`.
- Antifungals: For periwound fungal infections identified by `fungal infection skin images`.
- Moisture Balance: Maintaining a moist wound environment is crucial for healing.
- Exudate Management: Use of absorbent dressings (e.g., foam, alginate, hydrofiber) for highly exuding `venous ulcers` to prevent maceration of the periwound skin.
- Moisture Provision: Use of hydrating dressings (e.g., hydrogel, hydrocolloid) for dry wounds, such as some `arterial ulcers`, to prevent desiccation.
- Debridement: Removal of necrotic tissue and slough, which can impede healing and harbor bacteria.
- Dressing Selection: Based on the wound characteristics (exudate level, presence of infection, tissue type in the wound bed) visible in `wound dressing photos`.
- Alginates and Hydrofibers: Highly absorbent, ideal for wounds with heavy exudate.
- Foam Dressings: Moderate absorption, provide cushioning, good for `pressure ulcers`.
- Hydrocolloids: Provide a moist environment, autolytic debridement, moderate absorption, good for superficial `chronic wounds`.
- Hydrogels: Donate moisture to dry wounds, promote autolytic debridement.
- Transparent Films: Allow visualization, minimal absorption, ideal for superficial wounds or as secondary dressings.
- Antimicrobial Dressings: Contain silver, iodine, or PHMB for infected or critically colonized wounds.
- Collagen Dressings: Promote granulation tissue formation.
- Pain Management: Addressing ulcer-related pain (especially in `arterial ulcer appearance` scenarios) is critical for patient comfort and compliance.
- Systemic Analgesics: NSAIDs, acetaminophen, or opioids as needed.
- Topical Anesthetics: Applied to the wound prior to painful procedures like debridement.
- Neuropathic Pain Medications: For `diabetic neuropathic ulcers` (e.g., gabapentin, pregabalin).
- Nutritional Support: Adequate protein, vitamins (especially C and A), and minerals (zinc, iron) are essential for `wound healing acceleration`. Nutritional deficiencies can significantly impede `ulcer healing progress`.
- Adjunctive Therapies: For chronic, non-healing ulcers.
- Negative Pressure Wound Therapy (NPWT): Applies controlled suction to the wound bed, promoting granulation, reducing edema, and managing exudate, often visible in `NPWT application images`.
- Hyperbaric Oxygen Therapy (HBOT): Delivers 100% oxygen under increased atmospheric pressure, improving oxygenation to ischemic tissues and enhancing healing, particularly in severe `diabetic foot ulcers` or `arterial ulcers`.
- Growth Factors: Topical application of bioengineered growth factors (e.g., platelet-derived growth factor) to stimulate cell proliferation.
- Bioengineered Skin Substitutes: Application of living cellular products or acellular matrices to assist in wound closure, for `complex wound reconstruction`.
- Patient Education and Prevention: Empowering patients with knowledge about `trophic ulcer prevention` and self-care significantly reduces recurrence.
- Foot Care: Daily inspection, proper hygiene, and appropriate footwear for `diabetic foot ulcer prevention`.
- Leg Care: Elevation, compression, and regular exercise for `venous ulcer prevention`.
- Skin Protection: Moisturizing dry skin, protecting fragile areas from trauma.
- Lifestyle Modifications: Smoking cessation, blood glucose control, blood pressure management, healthy diet, and regular exercise.