Explore detailed allergic dermatitis symptoms pictures to identify common reactions and understand various manifestations across different skin types and locations. This comprehensive guide provides visual insights into the diverse presentation of contact dermatitis and other allergic skin conditions.
Allergic dermatitis Symptoms Pictures
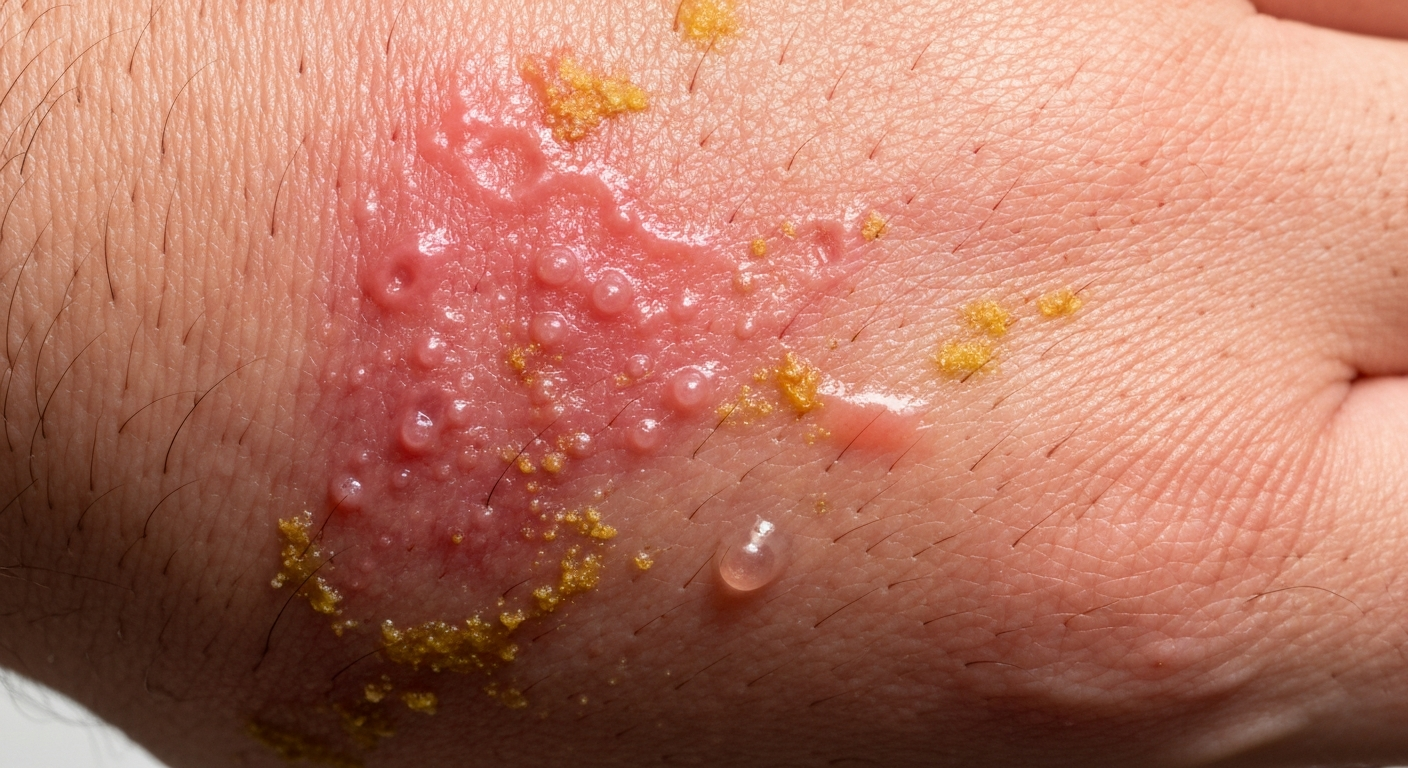
When examining allergic dermatitis symptoms pictures, a prominent feature is often intense pruritus, or itching, which can be severe enough to disrupt sleep and daily activities. The skin reaction frequently presents as erythema, a noticeable redness, particularly in the affected areas. This redness can range from a faint pink blush to a vivid, fiery red, often with ill-defined borders that spread beyond the immediate contact point in cases of contact allergic dermatitis. Swelling, or edema, is also a common visual cue, making the skin appear puffy or raised. This swelling can sometimes be subtle, a slight thickening of the skin, or quite pronounced, especially around the eyes or on the hands and feet. Vesicles, small fluid-filled blisters, are characteristic, particularly in acute presentations. These tiny blisters may coalesce to form larger bullae, and when they rupture, they can ooze clear or yellowish fluid, leading to a moist, glistening appearance on the skin surface. This oozing is a key indicator of acute inflammatory activity in many allergic dermatitis images.
The morphology of the rash in allergic dermatitis pictures can vary significantly based on the allergen, the individual’s sensitivity, and the duration of exposure. Common presentations include:
- Erythematous Papules: Small, red, raised bumps that can appear individually or in clusters. These are often the first visible signs in many allergic skin reactions.
- Vesicles and Bullae: Fluid-filled lesions. Vesicles are typically less than 0.5 cm, while bullae are larger. Their presence indicates an acute, often intense, inflammatory response.
- Oozing and Crusting: As vesicles and bullae rupture, they release serous fluid, which then dries to form yellowish or brownish crusts. This stage is highly indicative of active inflammation and can be seen clearly in many diagnostic dermatitis symptom photos.
- Scaling: Flakes of dead skin cells that can be white, gray, or yellowish. This often appears as the inflammation subsides or in more subacute/chronic phases, indicating ongoing skin turnover due to irritation.
- Lichenification: Thickening of the skin with exaggerated skin markings, resembling tree bark. This is a sign of chronic scratching and rubbing, common in long-standing cases of chronic allergic dermatitis.
- Fissures: Cracks in the skin, especially in areas of movement or where the skin is thick and dry (e.g., fingertips, heels). These can be painful and may bleed, highlighting the damage to the skin barrier.
- Hyperpigmentation/Hypopigmentation: Darkening or lightening of the skin in affected areas, often post-inflammatory. This can be a lingering visual sign after the acute symptoms have resolved, particularly noticeable in certain skin tones.
The distribution of the rash in allergic dermatitis images is crucial for diagnosis. It often mirrors the pattern of contact with the allergen. For instance, a rash on the wrist might suggest a watchband allergy, while a rash on the earlobes could point to nickel in earrings. Rashes on the eyelids might be due to nail polish or airborne allergens settling there. Hands are a very common site for contact dermatitis pictures due to frequent exposure to various substances, showing reactions from detergents, gloves, or industrial chemicals. Feet can react to shoe materials (rubber, leather dyes) or socks. Understanding these patterns is key to identifying the offending agent, making detailed visual analysis of allergic skin rash photos indispensable for clinical assessment.
Signs of Allergic dermatitis Pictures
Delving deeper into the specific signs of allergic dermatitis pictures reveals a spectrum of visual cues that indicate an immune response in the skin. Beyond the general redness and swelling, particular morphologies and secondary changes provide more nuanced diagnostic information. One prominent sign is the presence of sharply demarcated erythema with papules and vesicles, often distributed in a linear or geometric pattern, strongly suggesting an exogenous contactant. For example, a streaky rash observed in poison ivy allergic dermatitis photos clearly illustrates this contact pattern, following where the plant brushed against the skin. In contrast, airborne contact dermatitis might present with a more diffuse rash on exposed areas like the face, neck, and upper chest, sparing areas covered by clothing.
Chronic scratching and rubbing, which are direct consequences of intense itching, lead to several secondary signs clearly visible in allergic dermatitis visual documentation. These include:
- Excoriations: Linear erosions or scratches on the skin surface, often evidence of the patient attempting to relieve the pruritus. These can sometimes become infected.
- Lichenification: As previously mentioned, this severe thickening and hardening of the skin is a hallmark of chronic allergic dermatitis. The skin texture becomes leathery and coarse, with exaggerated skin lines, giving it a distinctive appearance in chronic dermatitis pictures. This change signifies a long-standing inflammatory process and repeated mechanical trauma from scratching.
- Post-inflammatory hyperpigmentation: Darkening of the skin, often brown or purplish, that occurs after the inflammation has resolved. This is particularly common in individuals with darker skin tones and can persist for months or even years, leaving a visible reminder of previous flares in allergic skin condition photos.
- Fissuring: Deep cracks in the skin, especially on palms, soles, and joints, due to dryness and chronic inflammation. These are not only painful but also potential entry points for bacterial infections.
- Plaques: Raised, flat-topped lesions that are larger than papules, often formed by the coalescence of multiple papules. These frequently exhibit scaling and lichenification in chronic cases.
In certain presentations, particularly acute episodes, clinicians will look for the presence of widespread edema and erythema, sometimes accompanied by a “weeping” or “wet” appearance due to ruptured vesicles. This wet stage is a critical visual sign indicating an active, highly inflammatory process. The distribution of these lesions often helps differentiate between various types of allergic dermatitis. For example, nickel allergy from a belt buckle will produce a localized rash around the navel, while a reaction to an adhesive plaster will leave a rectangular imprint of the allergic reaction. The symmetry or asymmetry of the rash can also provide clues; asymmetrical patterns often point to direct contact with an allergen on one side of the body. Examining allergic skin reaction pictures with a keen eye for these specific signs and their patterns is vital for accurate diagnosis and management, helping to pinpoint the underlying cause of the skin irritation and allergic response.
Early Allergic dermatitis Photos
Observing early allergic dermatitis photos is crucial for understanding the initial phase of the skin’s immune response to an allergen. In its nascent stages, allergic dermatitis may appear subtle, making early identification challenging but vital for timely intervention. Typically, the very first visual manifestation is a mild, localized erythema, or redness, often confined to the area of contact. This redness might be accompanied by a sensation of warmth to the touch, though this is not always visually apparent. The skin might feel slightly irritated or itchy before any prominent rash develops. This initial itching is often a key subjective symptom, preceding visible changes by hours or even a day.
Within the first 6-48 hours post-exposure, depending on the individual’s sensitivity and the allergen’s potency, more distinct signs begin to emerge. These include:
- Faint Redness (Erythema): The skin area where the allergen made contact becomes noticeably pink or light red. This might be diffuse and not yet sharply demarcated, but it represents the initial inflammatory response. This is a common feature in many initial allergic rash images.
- Subtle Swelling (Edema): A very slight puffiness or elevation of the skin may become apparent. This early edema is often non-pitting and can be difficult to discern without close inspection, but it indicates fluid accumulation in the dermal layer.
- Minute Papules: Tiny, pinprick-sized raised bumps may start to form. These papules represent early cellular infiltration and fluid accumulation within the epidermis and dermis. They are often the precursors to more prominent vesicles. These can be seen in high-resolution early contact dermatitis pictures.
- Increased Itching: The pruritus intensifies from a mild irritation to a more persistent and bothersome itch. While not a visual sign, it’s a critical accompanying symptom in the early stages that often drives patients to seek examination of their “itchy spots.”
- Warmth to the touch: The affected skin area might feel warmer than the surrounding skin, indicating increased blood flow and inflammation.
The distribution of these early changes in early allergic dermatitis photos is highly indicative. For instance, if an individual reacts to a new cosmetic, the early redness and small papules might appear specifically on the eyelids, around the mouth, or on the neck, depending on the product’s application. A reaction to jewelry might show a faint red ring under a watch or earring. The edges of the early rash might not yet be distinct but will usually follow the general contour of contact. There might be some minimal scaling or dryness beginning to appear as the initial acute inflammation subsides slightly and skin cells start to turn over faster. These very early stages, sometimes referred to as the “prodromal” phase of the rash, are characterized by a developing inflammation that hasn’t yet progressed to full-blown vesiculation or widespread crusting. Recognizing these initial subtle changes in first signs of allergic reaction pictures allows for prompt removal of the allergen and initiation of appropriate therapy, which can prevent the rash from worsening significantly and becoming more extensive or chronic. Thus, careful observation of any new or unusual skin changes, even minor ones, is paramount for early diagnosis and effective management of allergic skin conditions.
Skin rash Allergic dermatitis Images
Examining skin rash allergic dermatitis images reveals the full spectrum of inflammatory skin changes that arise from an allergic reaction. The appearance of the rash is highly variable, influenced by the specific allergen, the intensity of exposure, individual susceptibility, and the anatomical location. Acute allergic dermatitis often presents as erythematous, edematous plaques with numerous vesicles and bullae. These fluid-filled lesions are hallmark features, and when they rupture, they lead to weeping and serous crusting, giving the skin a moist, often yellowish appearance. The surrounding skin may also be red and swollen. For example, poison ivy rash pictures frequently show this acute, linear, vesicular eruption, clearly outlining the plant’s contact path.
In subacute phases, as the initial exudation subsides, the vesicles may become less prominent, replaced by more papules, erythema, and fine scaling. The skin starts to dry out, and crusts may still be present from previous weeping. Pruritus remains a significant symptom, driving further scratching which can exacerbate the rash. Chronic allergic dermatitis, on the other hand, presents a different visual landscape in chronic dermatitis rash images. Here, prolonged inflammation and repeated scratching lead to profound structural changes in the skin:
- Lichenification: Thickened, leathery skin with exaggerated skin markings, often appearing dull or hyperpigmented.
- Excoriations: Numerous scratch marks, which may be fresh or healed, indicating persistent itching.
- Fissures: Deep cracks, particularly common on the palms and soles, which are painful and can bleed.
- Hyperpigmentation: Darkening of the skin in previously inflamed areas, a common aftermath, especially in individuals with darker skin tones, creating a mottled appearance in some allergic skin disease photos.
- Dryness and Scaling: The skin becomes dry, rough, and sheds fine scales, indicating impaired barrier function.
The distribution of the rash provides critical diagnostic clues when analyzing allergic rash images. Common patterns include:
- Hands and Wrists: Frequent sites due to contact with detergents, solvents, chemicals, jewelry (nickel, chrome), gloves (latex, rubber accelerators), and plants.
- Face and Neck: Often affected by cosmetics (fragrances, preservatives), hair products (dyes, perms), airborne allergens (pollen, dust mites, plant resins), and transferred allergens from hands (nail polish). Eyelids are particularly sensitive and can react to airborne particles or products applied elsewhere.
- Feet: Common reactions to shoe materials (dyes, adhesives, leather treatments), socks (fabric softeners, dyes), and topical medications.
- Body Folds (Axillae, Groin): Reactions to deodorants, clothing, or topical medications applied to these areas.
- Generalized Eruption: While less common for contact dermatitis, severe widespread reactions can occur, making the primary site of contact harder to identify. This can sometimes be seen in severe systemic allergic reactions that manifest on the skin, though allergic contact dermatitis is typically localized.
The morphology of the rash, whether macular, papular, vesicular, or lichenified, tells a story about the stage and chronicity of the allergic reaction. A careful review of high-quality allergic dermatitis rash pictures, considering these detailed morphological and distributional characteristics, is indispensable for dermatologists and patients alike in understanding and managing this prevalent skin condition, guiding both diagnostic patch testing and effective treatment strategies for skin allergy symptoms.
Allergic dermatitis Treatment
Effective allergic dermatitis treatment focuses on alleviating symptoms, reducing inflammation, promoting skin healing, and, most importantly, identifying and avoiding the causative allergen. While our focus here is on the visual symptoms, understanding the treatment helps to understand how these visual cues are managed and ultimately resolve. The first and most critical step is the immediate removal and future avoidance of the allergen. This often requires careful detective work to pinpoint the exact trigger, which may involve environmental assessment, review of product ingredients, and potentially patch testing conducted by a dermatologist. Once the allergen is identified and removed, the visual signs of allergic skin inflammation will typically begin to improve.
Medical interventions for managing the visual and subjective symptoms include:
- Topical Corticosteroids: These are the cornerstone of treatment for reducing inflammation and itching. Available in various potencies (mild to very strong), they are applied directly to the affected skin. Visually, topical steroids effectively diminish erythema, reduce swelling, and help dry up weeping vesicles, leading to a smoother, less inflamed appearance in allergic dermatitis photos after treatment. Long-term use or use of high-potency steroids on sensitive areas must be managed carefully to avoid side effects like skin thinning or hypopigmentation.
- Oral Corticosteroids: For severe, widespread, or highly symptomatic allergic dermatitis, a short course of oral corticosteroids (e.g., prednisone) may be prescribed. These rapidly suppress the immune response, leading to a dramatic reduction in generalized redness, swelling, and itching. The visual improvement can be significant, rapidly clearing widespread skin allergy rashes.
- Antihistamines: Oral antihistamines, particularly sedating ones like diphenhydramine or hydroxyzine, can help alleviate itching, especially at night, thereby reducing scratching and preventing further excoriations and lichenification. While they don’t directly change the rash’s appearance, they indirectly aid healing by minimizing mechanical trauma.
- Topical Calcineurin Inhibitors (TCIs): Medications like tacrolimus and pimecrolimus are steroid-free alternatives that reduce inflammation and itching. They are often used for sensitive areas like the face and eyelids where steroids might be problematic, or for long-term maintenance. Visually, they help maintain a clearer skin appearance and prevent flares of allergic contact dermatitis symptoms.
- Emollients and Moisturizers: Regular application of thick, fragrance-free moisturizers is crucial for restoring the skin barrier function, which is often compromised in allergic dermatitis. They help reduce dryness, scaling, and cracking (fissures), making the skin appear smoother and healthier. This is a vital supportive measure in all phases of dermatitis management.
- Wet Dressings: For acute, weeping lesions, cool, wet compresses (e.g., with tap water or Burrow’s solution) can provide soothing relief, reduce oozing, and help debride crusts. This visually reduces the “wet” appearance and promotes drying, making the affected skin look cleaner and less inflamed.
- Antibiotics: If secondary bacterial infection (impetiginization) occurs, characterized by pus, honey-colored crusts, or increasing pain and swelling, oral or topical antibiotics may be necessary. This helps clear the infection, which would otherwise complicate the visual presentation of the allergic skin reaction.
Preventive strategies are paramount for long-term management of allergic dermatitis. This includes educating patients on common allergens (e.g., nickel, fragrances, preservatives, rubber chemicals), recommending hypoallergenic products, using protective clothing or gloves when handling irritants, and practicing good skin hygiene without harsh soaps. For chronic cases, consistent skin care, stress management, and ongoing allergen avoidance are critical to prevent recurrence of distressing allergic dermatitis symptoms pictures and maintain skin health. Regular follow-up with a healthcare provider ensures that the treatment plan remains effective and adapted to the patient’s changing needs, targeting both acute relief and long-term remission of allergic skin disease manifestations.