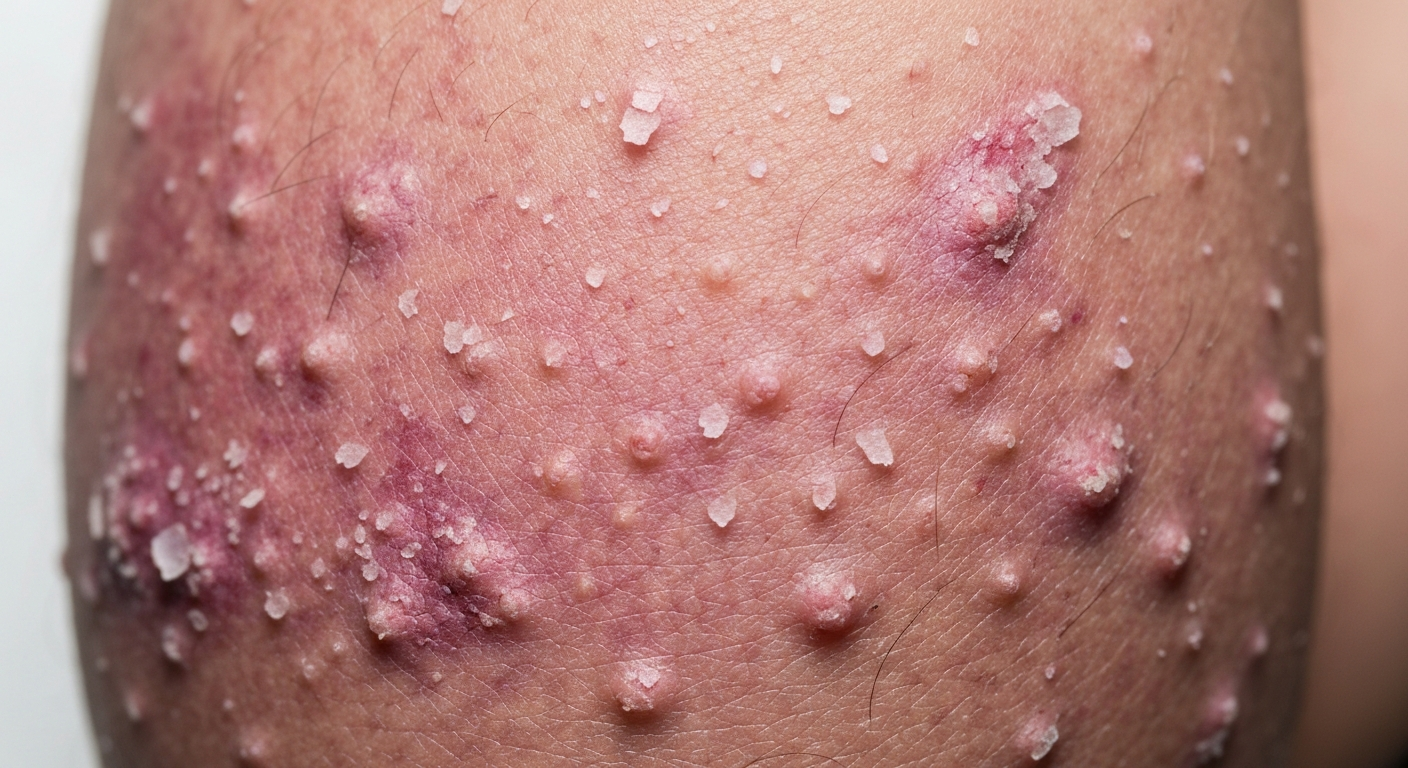
Identifying various skin conditions is crucial for timely management, and understanding Dermatosis symptoms pictures provides invaluable visual guidance. This resource is designed to aid in recognizing common dermatological manifestations through detailed descriptions of visual cues. Explore comprehensive insights into diverse presentations of skin issues and their potential implications.
Dermatosis Symptoms Pictures
Recognizing Dermatosis symptoms pictures involves a thorough understanding of various cutaneous manifestations that can affect the skin’s appearance and texture. These visible signs are critical for initial assessment and differentiating between numerous dermatological conditions. Understanding the spectrum of these symptoms is the first step in identifying specific dermatoses, ranging from common irritations to more complex systemic diseases with skin involvement. Each symptom provides clues about the underlying pathological process, guiding further diagnostic steps.
The primary visual symptoms of dermatosis often include changes in:
- Skin Color: Erythema (redness), hyperpigmentation (darkening), hypopigmentation (lightening), pallor (paleness), or cyanosis (bluish tint). These color alterations can be diffuse, patchy, or localized, offering insights into inflammatory processes, melanin disruption, or vascular changes.
- Skin Texture: Roughness, smoothness, thickening (lichenification), thinning (atrophy), or induration (hardening). Textural changes reflect cellular proliferation, collagen alterations, or epidermal damage.
- Lesion Morphology: The specific shape, size, and character of individual skin lesions are fundamental in dermatosis identification.
- Distribution Pattern: Whether lesions are localized to a specific area, generalized across the body, symmetrical, asymmetrical, or follow particular anatomical lines or patterns.
Common Primary Lesions Observable in Dermatosis Symptoms Pictures:
Primary lesions are the initial pathological changes directly related to the disease process.
- Macules: Small, flat, discolored spots less than 1 cm in diameter, such as freckles or early rashes. They represent a change in skin color without elevation or depression.
- Patches: Larger macules, greater than 1 cm, like vitiligo or large birthmarks. Patches are also flat areas of changed skin color.
- Papules: Small, solid, elevated lesions less than 1 cm, palpable to the touch, such as warts or insect bites. They arise from epidermal or dermal proliferation or infiltration.
- Plaques: Elevated, flat-topped lesions greater than 1 cm, often formed by the coalescence of papules, characteristic of psoriasis or eczema. Plaques suggest widespread epidermal thickening or dermal inflammation.
- Nodules: Solid, elevated lesions greater than 1 cm that extend deeper into the dermis or subcutaneous tissue, feeling firm, like lipomas or cysts. Their depth distinguishes them from papules and plaques.
- Wheals (Urticaria): Transient, elevated, compressible, pruritic lesions caused by dermal edema, typically seen in hives. They are often pink or red and disappear within hours.
- Vesicles: Small, fluid-filled blisters less than 1 cm, containing serous fluid, often seen in herpes simplex or allergic contact dermatitis. They indicate epidermal separation and fluid accumulation.
- Bullae: Large, fluid-filled blisters greater than 1 cm, such as those caused by severe burns or bullous pemphigoid. Bullae signify more extensive epidermal or dermal-epidermal separation.
- Pustules: Small, circumscribed elevations of the skin filled with pus, indicative of bacterial infection or sterile inflammation, like acne or folliculitis.
- Cysts: Sac-like lesions containing fluid or semi-solid material, often encapsulated and extending into the dermis or subcutaneous tissue, such as epidermal cysts.
Common Secondary Lesions Observable in Dermatosis Symptoms Pictures:
Secondary lesions evolve from primary lesions or are caused by external factors like scratching or infection.
- Scales: Flakes of stratum corneum, representing excessive proliferation or abnormal shedding, common in psoriasis, eczema, or tinea infections. They can be fine, greasy, or silvery.
- Crusts: Dried serum, blood, or pus on the skin surface, forming a scab, as seen in impetigo or healing wounds. Crusts indicate exuded fluids that have dried.
- Erosions: Superficial breaks in the epidermis that do not extend into the dermis, healing without scarring, like ruptured vesicles. They appear as moist, depressed areas.
- Ulcers: Deep erosions that extend into the dermis, often healing with scarring, such as venous stasis ulcers or pressure sores. Ulcers signify significant tissue loss.
- Fissures: Linear cracks in the epidermis that may extend into the dermis, often painful, seen in severely dry skin or athlete’s foot. They are deep, narrow openings.
- Excoriations: Linear abrasions caused by scratching, indicating pruritus, frequently seen in eczema or scabies.
- Lichenification: Thickening of the epidermis with exaggerated skin lines, typically due to chronic scratching or rubbing, giving a leathery appearance.
- Atrophy: Thinning of the skin, which may appear shiny and translucent, often seen with prolonged corticosteroid use or aging.
- Scars: Fibrous tissue that replaces normal skin after injury or disease, varying in color and texture. They are permanent changes indicating dermal damage.
- Keloids: Elevated, enlarged scars that extend beyond the original wound boundaries, resulting from abnormal collagen production.
Observing these specific Dermatosis symptoms pictures and understanding their nomenclature is crucial for accurate communication among healthcare professionals and for patients seeking to describe their condition. Detailed descriptions of these visual cues significantly enhance the diagnostic process for various skin conditions.
Signs of Dermatosis Pictures
Delving deeper into Signs of Dermatosis Pictures, we explore the specific observable characteristics that differentiate various skin conditions and provide critical information for diagnosis. Beyond basic lesion types, signs encompass a broader range of visual cues, including skin color changes, specific patterns, and the presence of associated features like hair or nail involvement. These signs, when combined with patient history, paint a comprehensive picture of the dermatological issue at hand, aiding clinicians in pinpointing the exact nature of the dermatosis.
Specific Visual Signs and Associated Conditions:
Detailed analysis of Dermatosis symptoms pictures often reveals nuances that are key to distinguishing between similar-looking conditions. These specific signs include:
- Erythema: Redness caused by capillary dilation, a hallmark of inflammation.
- Diffuse Erythema: Widespread redness, often seen in sunburn or drug reactions.
- Localized Erythema: Confined redness, typical of localized infections like cellulitis or insect bites.
- Blanching Erythema: Redness that temporarily disappears when pressure is applied, indicating vascular dilation, distinguishing it from petechiae/purpura.
- Hyperpigmentation: Increased melanin deposition, leading to darker skin areas.
- Post-inflammatory Hyperpigmentation: Darkening after inflammation or injury (e.g., healing acne lesions, eczema).
- Melasma: Symmetrical, patchy brown hyperpigmentation on the face, often hormone-related.
- Café-au-lait Spots: Light brown, uniformly pigmented macules, sometimes indicative of neurofibromatosis.
- Hypopigmentation/Depigmentation: Decreased or absent melanin, resulting in lighter or white skin areas.
- Vitiligo: Autoimmune condition causing complete loss of melanocytes, resulting in sharply demarcated white patches.
- Tinea Versicolor: Fungal infection causing patchy hypopigmentation or hyperpigmentation, often with fine scales.
- Post-inflammatory Hypopigmentation: Temporary lightening after inflammatory conditions.
- Vascular Signs: Indicators of blood vessel involvement.
- Petechiae: Tiny, pinpoint non-blanching red or purple spots, < 1 cm, due to capillary hemorrhage, indicative of vasculitis or clotting disorders.
- Purpura: Larger non-blanching red or purple patches, > 1 cm, also due to hemorrhage, seen in trauma, vasculitis, or coagulation defects.
- Telangiectasias: Dilated superficial blood vessels appearing as fine, red lines, often seen in rosacea, sun damage, or systemic sclerosis.
- Ecchymoses: Bruises, larger areas of extravasated blood, often purplish or bluish.
- Texture Changes: Alterations in the skin surface.
- Lichenification: Thickening and accentuation of skin lines due to chronic rubbing or scratching, creating a leathery texture, common in chronic eczema.
- Induration: Hardening or firming of the skin, often associated with inflammation or deep infiltration, as in cellulitis or scleroderma.
- Atrophy: Thinning of the epidermis or dermis, making the skin appear shiny, wrinkled, and translucent, often due to aging or corticosteroid use.
- Hair and Nail Changes: Dermatosis can manifest in adnexal structures.
- Alopecia: Hair loss, which can be patchy (e.g., alopecia areata, tinea capitis) or diffuse (e.g., telogen effluvium).
- Onycholysis: Separation of the nail plate from the nail bed, often seen in psoriasis, fungal infections (onychomycosis), or trauma.
- Nail Pitting: Small depressions on the nail surface, highly characteristic of psoriasis.
- Subungual Hyperkeratosis: Thickening of the nail bed beneath the nail plate, common in psoriasis and onychomycosis.
- Beau’s Lines: Transverse grooves across the nail plate, indicating a temporary halt in nail growth due to systemic illness or severe stress.
- Specific Lesion Patterns and Configurations:
- Annular: Ring-shaped lesions with a clear center, typical of tinea corporis or granuloma annulare.
- Arcuate: Arc-shaped lesions.
- Serpiginous: Wavy or snake-like lesions.
- Linear: Lesions arranged in a line, often due to external contact (e.g., contact dermatitis from poison ivy) or Koebner phenomenon.
- Reticular: Net-like or lace-like pattern, as seen in livedo reticularis.
- Target Lesions: Concentric rings of color resembling a target, characteristic of erythema multiforme.
- Grouped Lesions: Lesions clustered together, like vesicles in herpes simplex.
- Dermatomal/Zosteriform: Lesions following a nerve distribution, characteristic of herpes zoster (shingles).
- Perifollicular: Lesions surrounding hair follicles.
Analyzing these diverse Signs of Dermatosis Pictures allows for a more refined diagnosis, helping to narrow down the possibilities among numerous skin conditions. Each sign, whether subtle or prominent, contributes to the overall clinical picture and guides further investigation and management of dermatological issues.
Early Dermatosis Photos
Catching Early Dermatosis Photos is paramount for effective treatment and preventing progression or complications of various skin conditions. Early detection often leads to simpler, more successful interventions and can significantly improve patient outcomes. Recognizing the subtle initial manifestations requires a keen eye and familiarity with how different dermatoses typically begin. These early signs can often be less distinct than advanced lesions, making their identification particularly challenging yet crucial for prompt management of skin health. The initial stages may involve faint discoloration, minor textural changes, or mild itching, which can easily be dismissed as insignificant without proper knowledge.
Initial Manifestations and Subtle Cues in Early Dermatosis:
When examining Dermatosis symptoms pictures focusing on early stages, look for:
- Subtle Erythema: A faint pink or red blush on the skin, often preceding a full-blown rash. This might be localized or present as diffuse mild redness.
- Early Eczema (Dermatitis): May begin as a small patch of mild redness, dryness, and slight itching, often in skin folds or on extensor surfaces. The skin might feel slightly rough or warm.
- Early Psoriasis: Can manifest as small, discrete reddish papules covered with fine, silvery scales, often on elbows, knees, or scalp. Initially, these might be very small and easily overlooked.
- Early Fungal Infections (Tinea): Might appear as a faintly red, slightly scaly patch with a barely raised border, often starting as a small macule or papule that slowly expands.
- Minor Texture Changes: Slight roughness, dryness, or a subtle change in skin elasticity.
- Xerosis (Dry Skin): Initial stages present as dull, tight-feeling skin with fine scales, sometimes accompanied by mild pruritus. This can be a precursor to asteatotic eczema.
- Early Actinic Keratosis: A small, rough, sandpaper-like patch on sun-exposed skin, often easier felt than seen initially. It may be slightly red or flesh-colored.
- Isolated or Few Primary Lesions: Rather than widespread involvement, early dermatosis often starts with a single lesion or a small cluster.
- Early Acne Vulgaris: Characterized by isolated comedones (blackheads or whiteheads) or a few inflammatory papules/pustules.
- Early Rosacea: May begin with transient facial redness or flushing, occasionally accompanied by a few scattered papules or pustules without comedones.
- Early Herpes Simplex: Characterized by a tingling or burning sensation followed by the development of a small cluster of vesicles on an erythematous base.
- Mild Pruritus (Itching): Often the first symptom, sometimes preceding any visible skin changes.
- Early Urticaria (Hives): Can start with localized itching before the characteristic wheals fully develop.
- Early Scabies: Intense itching, especially at night, often precedes the visible burrow lines or excoriated papules.
- Faint Discoloration: Subtle changes in pigmentation that are not yet pronounced.
- Early Melasma: Very light brown patches on the face that become darker with sun exposure.
- Early Vitiligo: Small, poorly demarcated hypopigmented macules that slowly expand and become more distinct over time.
Importance of Recognizing Early Dermatosis:
- Preventing Progression: Treating skin conditions in their nascent stages can halt their development into more severe or widespread forms. For instance, early treatment of eczema can prevent lichenification.
- Minimizing Complications: Early intervention can prevent secondary infections, scarring, or chronic pain associated with advanced dermatosis. Treating early tinea infections prevents spread and deeper invasion.
- Improving Prognosis: Many dermatoses respond more favorably to treatment when caught early. Early diagnosis of skin cancers like basal cell carcinoma or squamous cell carcinoma is critical for complete cure.
- Reducing Discomfort: Addressing symptoms like itching, burning, or pain in their initial stages significantly improves the patient’s quality of life.
- Cost-Effectiveness: Early, simpler treatments are often less expensive and less invasive than interventions required for chronic or advanced conditions.
Encouraging self-examination and providing clear examples of Early Dermatosis Photos can empower individuals to seek professional medical advice promptly. Education on recognizing these nascent signs of dermatological issues is a cornerstone of preventative skin health and effective disease management. Paying close attention to any persistent or unusual skin changes, however subtle, is crucial.
Skin rash Dermatosis Images
Exploring Skin rash Dermatosis Images provides a critical visual guide to understanding the diverse manifestations of skin rashes, which are among the most common presentations of dermatological conditions. A rash refers to any change in the skin that affects its appearance or texture, encompassing a wide range of types, patterns, and underlying causes. Analyzing these images helps in differentiating between inflammatory, infectious, allergic, and autoimmune etiologies, which is fundamental for accurate diagnosis and appropriate treatment. The morphology, distribution, and associated symptoms of a rash are key elements to consider when reviewing visual evidence of dermatosis.
Categorization of Rashes Based on Morphology and Pattern:
When examining Dermatosis symptoms pictures specifically featuring rashes, attention to detail regarding their appearance is vital.
- Macular Rashes: Flat, non-palpable areas of changed skin color.
- Morbilliform Rash: Macular or maculopapular rash resembling measles, often viral exanthem (e.g., rubella, roseola, viral drug eruptions). Characterized by discrete red spots that may coalesce.
- Erythema Infectiosum (Fifth Disease): “Slapped cheek” appearance followed by a lacy, reticular rash on the body.
- Drug Eruptions: Can present as diffuse macular erythema, sometimes pruritic.
- Papular Rashes: Elevated, solid lesions less than 1 cm.
- Lichen Planus: Pruritic, purple, polygonal, planar papules and plaques (the 6 P’s), often with Wickham’s striae (fine white lines).
- Molluscum Contagiosum: Small, dome-shaped, flesh-colored papules with a central umbilication.
- Folliculitis: Small, erythematous papules or pustules centered around hair follicles.
- Insect Bites (Papular Urticaria): Itchy, red papules that may appear in clusters.
- Vesicular/Bullous Rashes: Fluid-filled blisters.
- Herpes Simplex/Zoster: Grouped vesicles on an erythematous base, often painful or itchy, following a dermatomal pattern in zoster.
- Contact Dermatitis: Erythematous, intensely pruritic vesicles and bullae in a localized pattern, often linear from allergen exposure (e.g., poison ivy).
- Chickenpox (Varicella): Generalized rash starting as macules, progressing to papules, then vesicles, and finally crusts, often in different stages of healing simultaneously (“dewdrop on a rose petal”).
- Bullous Pemphigoid: Large, tense bullae on an erythematous or normal skin base, typically in older adults.
- Pustular Rashes: Lesions filled with pus.
- Acne Vulgaris: Polymorphous eruption of comedones, papules, pustules, and cysts primarily on the face, chest, and back.
- Pustular Psoriasis: Widespread erythema with numerous sterile pustules, often accompanied by fever.
- Rosacea: Erythema, telangiectasias, and recurrent papules and pustules on the central face.
- Urticarial Rashes (Hives): Transient, migratory, erythematous, and pruritic wheals.
- Acute Urticaria: Develops suddenly, usually lasting less than six weeks, often triggered by allergies, infections, or drugs.
- Chronic Urticaria: Persists for more than six weeks, often idiopathic but can be autoimmune or trigger-induced.
- Scaling Rashes: Characterized by the presence of loose epidermal cells (scales).
- Psoriasis: Well-demarcated, erythematous plaques with thick, silvery scales, typically on extensor surfaces, scalp, and nails.
- Eczema (Atopic Dermatitis): Erythematous, itchy, and scaly patches, often with excoriations and lichenification, typically in flexural areas (e.g., antecubital and popliteal fossae).
- Seborrheic Dermatitis: Greasy, yellow scales on an erythematous base, commonly affecting the scalp, face (nasolabial folds, eyebrows), and chest.
- Tinea Corporis (Ringworm): Annular or arcuate erythematous plaques with raised, scaly borders and central clearing.
- Pityriasis Rosea: Oval, erythematous, finely scaly patches, often starting with a “herald patch” and spreading in a “Christmas tree” pattern on the trunk.
- Purpuric Rashes: Non-blanching red/purple lesions due to bleeding into the skin.
- Vasculitis: Palpable purpura, often with associated symptoms like fever, joint pain, and kidney involvement.
- Henoch-Schönlein Purpura: Palpable purpura on lower extremities and buttocks, associated with abdominal pain, joint pain, and renal disease, often in children.
Each type of rash provides invaluable visual information that, when combined with patient history and other clinical findings, guides the diagnostic process. Understanding the characteristics visible in Skin rash Dermatosis Images is essential for both medical professionals and individuals seeking to identify and describe their dermatological concerns accurately. These visual distinctions are crucial for differentiating conditions and ensuring appropriate management of skin diseases.
Dermatosis Treatment
While Dermatosis symptoms pictures are crucial for identification, understanding Dermatosis Treatment is the ultimate goal of diagnosis. Treatment strategies for dermatoses are highly varied, depending on the specific condition, its severity, the patient’s overall health, and potential triggers. Effective treatment aims to alleviate symptoms, heal lesions, prevent recurrence, and improve the patient’s quality of life. It often involves a combination of topical medications, systemic therapies, lifestyle adjustments, and, in some cases, specialized procedures. A thorough understanding of treatment options is vital for managing chronic skin diseases and acute dermatological issues effectively.
General Principles of Dermatosis Treatment:
- Accurate Diagnosis: The cornerstone of effective treatment. Without a precise identification of the dermatosis, therapies may be ineffective or even harmful.
- Symptom Relief: Alleviating immediate discomforts like itching, pain, or burning.
- Eliminating/Controlling Cause: Addressing the underlying trigger, whether it’s an allergen, infection, autoimmune process, or genetic predisposition.
- Restoring Skin Barrier Function: Many dermatoses compromise the skin barrier, making barrier repair (e.g., emollients) a key component of treatment.
- Preventing Complications: Reducing the risk of secondary infections, scarring, or long-term damage.
- Patient Education: Empowering patients with knowledge about their condition, triggers, and self-care strategies.
Common Treatment Modalities for Various Dermatoses:
1. Topical Therapies:
Applied directly to the skin, these are often the first line of defense for localized dermatoses, minimizing systemic side effects.
- Corticosteroids: (e.g., hydrocortisone, betamethasone)
- Mechanism: Potent anti-inflammatory and immunosuppressive effects.
- Uses: Eczema, psoriasis, contact dermatitis, lichen planus, insect bites.
- Considerations: Available in various strengths (mild to super potent). Long-term use or use of potent steroids on sensitive areas can lead to skin thinning, striae, telangiectasias, or rebound flares.
- Calcineurin Inhibitors: (e.g., tacrolimus, pimecrolimus)
- Mechanism: Immunomodulators that block T-cell activation, reducing inflammation without corticosteroid side effects.
- Uses: Atopic dermatitis, especially on sensitive areas like the face and skin folds.
- Considerations: May cause transient burning or stinging upon application.
- Antifungals: (e.g., clotrimazole, terbinafine, ketoconazole)
- Mechanism: Inhibit fungal growth.
- Uses: Tinea infections (ringworm, athlete’s foot, jock itch), candidiasis, tinea versicolor.
- Considerations: Ensure complete treatment course to prevent recurrence.
- Antibiotics: (e.g., mupirocin, clindamycin)
- Mechanism: Combat bacterial infections.
- Uses: Impetigo, folliculitis, infected eczema.
- Considerations: Resistances are a concern; use judiciously.
- Emollients and Moisturizers: (e.g., petroleum jelly, ceramides, hyaluronic acid)
- Mechanism: Hydrate the skin, repair the skin barrier, reduce transepidermal water loss.
- Uses: Dry skin (xerosis), eczema, psoriasis, any condition with barrier dysfunction.
- Considerations: Essential for maintenance therapy in chronic dry skin conditions.
- Keratolytics: (e.g., salicylic acid, urea, lactic acid)
- Mechanism: Exfoliate dead skin cells, soften scales, reduce hyperkeratosis.
- Uses: Psoriasis, acne, keratosis pilaris, warts.
- Considerations: Can cause irritation if too concentrated or used excessively.
- Retinoids: (e.g., tretinoin, adapalene)
- Mechanism: Regulate cell growth and differentiation, reduce inflammation, unclog pores.
- Uses: Acne, photoaging, psoriasis.
- Considerations: Can cause dryness, redness, and photosensitivity; use sunscreen.
2. Systemic Therapies:
Taken orally or by injection, these are used for widespread, severe, or recalcitrant dermatoses that do not respond to topical treatments.
- Oral Corticosteroids: (e.g., prednisone)
- Mechanism: Potent systemic anti-inflammatory and immunosuppressive effects.
- Uses: Severe allergic reactions, acute exacerbations of eczema/psoriasis, bullous diseases.
- Considerations: Short-term use preferred due to numerous side effects (weight gain, osteoporosis, hypertension, diabetes, immunosuppression).
- Immunosuppressants: (e.g., methotrexate, cyclosporine, azathioprine)
- Mechanism: Suppress the immune system to reduce inflammation and autoimmune responses.
- Uses: Severe psoriasis, severe eczema, bullous diseases, autoimmune connective tissue diseases.
- Considerations: Require close monitoring for side effects (liver toxicity, kidney damage, increased infection risk).
- Biologics: (e.g., adalimumab, ustekinumab, secukinumab)
- Mechanism: Target specific components of the immune system involved in disease pathogenesis (e.g., TNF-alpha, IL-17, IL-23).
- Uses: Moderate to severe psoriasis, psoriatic arthritis, severe atopic dermatitis.
- Considerations: Administered via injection, high cost, potential for increased infection risk, need for careful patient selection and monitoring.
- Systemic Antibiotics: (e.g., doxycycline, cephalexin)
- Mechanism: Treat bacterial infections or their inflammatory components.
- Uses: Moderate to severe acne, cellulitis, erysipelas, severe folliculitis.
- Considerations: Risk of resistance, gastrointestinal side effects, photosensitivity.
- Systemic Antihistamines: (e.g., cetirizine, fexofenadine, hydroxyzine)
- Mechanism: Block histamine receptors, reducing itching and allergic reactions.
- Uses: Urticaria, severe pruritus associated with eczema or other itchy dermatoses.
- Considerations: Sedating vs. non-sedating options.
- Oral Retinoids: (e.g., isotretinoin)
- Mechanism: Potent modulator of sebaceous gland function and keratinization.
- Uses: Severe, recalcitrant nodulocystic acne.
- Considerations: Significant side effects (teratogenicity, dryness, elevated lipids, mood changes); strict monitoring required.
3. Phototherapy:
Controlled exposure to ultraviolet (UV) light to treat inflammatory skin conditions.
- UVB (narrowband UVB, broadband UVB):
- Mechanism: Suppresses inflammation and slows excessive skin cell growth.
- Uses: Psoriasis, eczema, vitiligo, cutaneous T-cell lymphoma.
- Considerations: Requires multiple sessions, risk of sunburn and long-term skin cancer.
- PUVA (Psoralen plus UVA):
- Mechanism: Psoralen sensitizes the skin to UVA light, enhancing its therapeutic effects.
- Uses: Severe psoriasis, vitiligo, cutaneous T-cell lymphoma.
- Considerations: Higher risk of side effects, including nausea, photosensitivity, and increased risk of skin cancer compared to UVB.
4. Lifestyle Modifications and Adjunctive Therapies:
- Trigger Avoidance: Identifying and avoiding allergens (e.g., in contact dermatitis), irritants, or stress that exacerbate conditions.
- Proper Skin Care: Gentle cleansing, regular moisturizing, avoidance of harsh soaps.
- Dietary Adjustments: While controversial for many dermatoses, some patients report improvement with specific diets (e.g., gluten-free for some with dermatitis herpetiformis).
- Stress Management: Stress can exacerbate many inflammatory dermatoses like psoriasis and eczema. Techniques like mindfulness, yoga, or meditation can be beneficial.
- Protective Measures: Sun protection for photosensitive conditions, wearing appropriate clothing.
Successful Dermatosis Treatment often requires a holistic approach, tailored to the individual, combining various therapeutic strategies. Regular follow-up with a dermatologist is essential to monitor progress, adjust treatments as needed, and manage any potential side effects of medications. Understanding both the visual cues from Dermatosis symptoms pictures and the available treatment options empowers patients and healthcare providers in managing these prevalent skin conditions effectively.