Recognizing the visual cues of onycholysis is paramount for timely identification and appropriate management. This comprehensive guide provides an in-depth look at onycholysis symptoms pictures, detailing the varied presentations of nail plate detachment to aid in understanding this common nail disorder. Understanding these visual characteristics is crucial for individuals and healthcare professionals alike.
onycholysis Symptoms Pictures
Onycholysis, characterized by the separation of the nail plate from the nail bed, presents with a diverse range of visual symptoms. These symptoms can vary in severity, location, and associated features, making a detailed understanding of onycholysis symptoms pictures essential for accurate recognition. The primary visual characteristic is the lifting of the nail, typically beginning at the distal (free edge) or lateral (sides) margins and progressing proximally. This separation creates a visible gap between the nail plate and the underlying nail bed.
The appearance of the separated area is often striking and can indicate underlying causes. Common visual symptoms include:
- Discoloration of the Nail Plate:
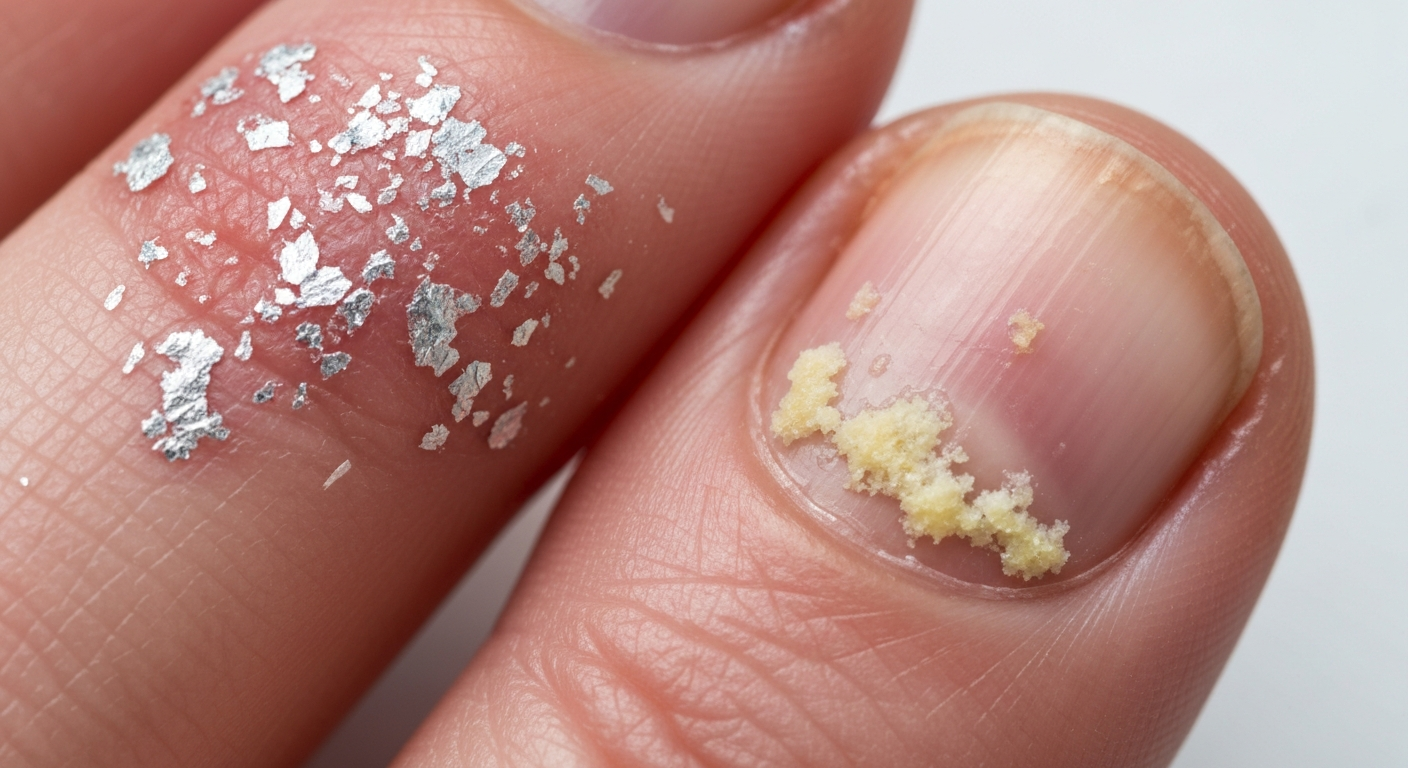
- White Onycholysis: Often seen in initial stages or when the underlying cause is trauma, fungal infection (distal subungual onychomycosis), or simple idiopathic separation. The detached area appears opaque and whitish due to air trapped beneath the nail.
- Yellow Onycholysis: Frequently associated with fungal infections (onychomycosis), psoriasis, or prolonged exposure to certain chemicals. The yellowish hue can range from pale straw to deep amber.
- Green Onycholysis: A strong indicator of a secondary bacterial infection, most commonly caused by Pseudomonas aeruginosa. This distinct green-black discoloration is due to pyocyanin pigment produced by the bacteria, often accompanied by a foul odor.
- Brown Onycholysis: Can result from chronic trauma, certain medications (e.g., tetracyclines, psoralens), or subungual hemorrhage. It can also be seen in severe cases of fungal infection.
- Black Onycholysis: Typically signifies subungual hematoma (blood trapped under the nail, often from severe trauma), but less commonly can be associated with certain medications or even subungual melanoma, requiring careful differentiation.
- Irregular Border of Separation: The line where the nail plate detaches from the nail bed is rarely perfectly straight. It can be jagged, wavy, or arc-shaped, reflecting the pattern of detachment.
- Accumulation of Subungual Debris: Underneath the lifted nail plate, a white, chalky, or yellowish substance often accumulates. This debris is a mixture of keratinous material, skin cells, and sometimes fungal elements or bacterial colonies. The volume of debris can vary greatly.
- Transparency or Opacity Changes: The detached portion of the nail often loses its normal pinkish transparency, becoming opaque, white, or discolored. The intact portion of the nail may retain its normal appearance.
- Texture Changes of the Nail Plate: While the primary issue is separation, the nail plate itself might become brittle, crumbly, or thickened, particularly in cases of onychomycosis or psoriasis. It may also feel softer or more pliable in the detached area.
- Partial or Complete Detachment: Onycholysis can affect a small portion of one nail or involve extensive detachment of multiple nails, reflecting the widespread nature of some underlying conditions.
- Absence of Pain (Initially): In many cases, onycholysis itself is painless, especially in its early stages. Pain typically arises if there’s secondary infection, significant trauma, or inflammation of the nail bed.
- Pitting or Ridging: Especially when associated with psoriasis, the nail plate might exhibit small indentations (pitting) or horizontal/vertical ridges in addition to the onycholysis.
Understanding these visual elements within onycholysis symptoms pictures is foundational for recognizing the condition and guiding further diagnostic steps.
Signs of onycholysis Pictures
Beyond the primary symptom of nail plate detachment, several specific signs observed in signs of onycholysis pictures provide crucial clues regarding the etiology and severity of the condition. These signs are often subtle but important for differentiating between various causes, from fungal infections to systemic diseases. Recognizing these specific visual markers is key for comprehensive assessment of onycholysis signs.
Detailed examination of the nail and surrounding tissues can reveal the following significant signs:
- Proximal Spread of Separation: While onycholysis often starts distally or laterally, its progression towards the nail root (proximal spread) is a common sign. The extent of this spread can indicate the duration and severity of the underlying issue.
- Subungual Hyperkeratosis: This refers to the excessive accumulation of keratinous material underneath the nail plate in the separated area. In signs of onycholysis pictures, it appears as a thick, crumbly, white-to-yellowish mass, often lifting the nail even further. It is a hallmark sign of conditions like psoriasis and onychomycosis.
- Oil Spot or Salmon Patch: Pathognomonic for psoriatic onycholysis, these signs appear as yellowish-red or salmon-colored translucent areas within the nail plate, typically observed beneath the detached portion or at the border of separation. They represent psoriatic plaques in the nail bed.
- Splinter Hemorrhages: Small, thin, reddish-brown lines running longitudinally under the nail plate. While not exclusive to onycholysis, they can be seen in psoriatic nails, endocarditis, or after trauma, and may coexist with nail detachment.
- Onycholysis with Erythema and Swelling of the Proximal Nail Fold: This can suggest a paronychia (inflammation of the nail fold) that has extended to cause onycholysis, or it can be a sign of inflammatory conditions affecting the nail matrix and fold, such as lupus or dermatomyositis.
- Beau’s Lines: Transverse depressions across the nail plate, often indicating a temporary arrest of nail growth due to systemic illness, severe trauma, or medication. If onycholysis develops after a Beau’s line, it might suggest the event that caused the Beau’s line also contributed to the nail separation.
- Leukonychia (White Spots/Lines): While sometimes benign, extensive or unusual patterns of leukonychia (white discoloration within the nail plate) can accompany onycholysis in some systemic conditions or genetic disorders.
- Pitting of the Nail Plate: Small, punctate depressions on the surface of the nail, most commonly associated with psoriasis, but also seen in alopecia areata. When present with onycholysis, it strongly points towards these dermatological conditions.
- Nail Plate Thickening (Onychauxis) or Thinning: Thickening is very common with onychomycosis and psoriasis. Conversely, some inflammatory conditions or severe nutritional deficiencies might lead to a thinner, more brittle nail plate that easily separates.
- Nail Bed Changes: In some cases, careful observation might reveal changes in the exposed nail bed, such as erythema (redness), atrophy, or an irregular surface, particularly after the detached nail plate has been removed.
- Perionyx Discoloration or Inflammation: Discoloration or inflammation of the skin immediately surrounding the nail (perionyx) can be a secondary sign, indicating a broader dermatological condition affecting both skin and nails.
These specific signs, when observed in signs of onycholysis pictures, are critical for a clinician to build a differential diagnosis and guide further laboratory investigations, such as fungal cultures or biopsies, to pinpoint the underlying cause of the nail separation.
Early onycholysis Photos
Early detection of onycholysis is crucial for preventing progression and initiating effective treatment, making the study of early onycholysis photos highly valuable. At its onset, onycholysis can be subtle and easily overlooked, yet prompt recognition can significantly impact the outcome. The initial stages often involve minimal detachment, which may be mistaken for minor nail damage or simply a cosmetic issue. However, understanding the characteristics of early separation can lead to timely intervention.
Key features to look for in early onycholysis photos include:
- Minimal Distal or Lateral Separation: The very first sign is typically a small area of detachment at the free edge (distal onycholysis) or along the side (lateral onycholysis) of the nail plate. This separation may be no more than a millimeter or two.
- Subtle White Opaque Area: The newly detached area will often appear slightly opaque and whitish, differing from the normal pinkish, translucent appearance of the nail plate firmly attached to the nail bed. This color change is due to air trapping.
- Slight Irregularity of the Free Edge: Instead of a clean, sharp edge, the border of separation might appear slightly ragged or uneven at its very beginning.
- No Significant Discoloration (Initially): In its earliest stages, significant yellow, green, or brown discoloration might not be present. These often develop as the condition progresses or secondary infections set in.
- Absence of Subungual Debris: Early onycholysis may not yet have significant accumulation of keratinous debris or fungal elements underneath. This debris often builds up over time as the separation widens.
- Lack of Pain or Inflammation: Often, early onycholysis is asymptomatic in terms of pain or visible inflammation of the surrounding skin. Pain or redness typically indicates progression, trauma, or secondary infection.
- Focus on a Single Nail: Early onycholysis might affect only one or a couple of nails before spreading to others, especially if the cause is localized trauma or a nascent fungal infection.
- History of Minor Trauma: In some cases, the patient may recall a recent minor trauma (e.g., impact, prolonged pressure from footwear, excessive manicuring) that precipitated the initial separation, which then fails to reattach.
- Water Ingress: Patients might notice water collecting under the nail more easily, leading to a temporary darkening or softening of the detached area after bathing or washing hands. This can be an early indicator of separation.
- Relatively Intact Nail Plate Texture: The nail plate itself may not show signs of thickening, crumbling, or significant surface changes in the very early stages, maintaining its normal texture outside the separated zone.
The importance of identifying these nascent signs from early onycholysis photos cannot be overstated. When onycholysis is recognized early, interventions aimed at addressing underlying causes (e.g., avoiding irritants, targeted antifungal treatment, managing inflammatory conditions) can often prevent extensive nail damage, reduce the risk of secondary infections, and shorten recovery time. Educating individuals on what to look for at the first sign of nail plate lifting is a critical step in proactive nail health management and can prevent the condition from becoming chronic or severely debilitating.
Skin rash onycholysis Images
When onycholysis is accompanied by a skin rash, it often points to an underlying dermatological condition that affects both the skin and the nails. Examining skin rash onycholysis images is vital for identifying these associated conditions, as the characteristics of the rash can provide direct clues to the etiology of the nail separation. Several skin diseases are known to manifest with both cutaneous lesions and nail involvement, including onycholysis. The appearance of the rash, its location, and its specific features are crucial for diagnosis.
Common skin conditions causing or associated with onycholysis and their characteristic rashes include:
- Psoriasis:
- Rash Description: Psoriatic rashes are typically well-demarcated, erythematous (red) plaques covered with silvery scales. They commonly appear on extensor surfaces (elbows, knees), scalp, and lower back.
- Nail Involvement: Psoriatic onycholysis can be very distinctive, often accompanied by oil spots (salmon patches), nail pitting, subungual hyperkeratosis, and crumbling of the nail plate. The nail bed itself may appear red or inflamed beneath the separated area.
- Visual Clues in Images: Look for classic psoriatic plaques on the skin alongside the specific nail changes (pitting, oil spots, significant subungual debris) that accompany the onycholysis.
- Eczema (Dermatitis):
- Rash Description: Eczematous rashes are characterized by erythema, pruritus (itching), scaling, vesicles, crusting, and thickening (lichenification) of the skin. They can be acute or chronic, often affecting the hands and fingers.
- Nail Involvement: Chronic hand eczema, especially allergic contact dermatitis or atopic dermatitis, can severely impact nail growth and health, leading to onycholysis. Nails may also become rough, ridged, discolored, or brittle. Inflammation of the nail folds is common.
- Visual Clues in Images: Observe the inflamed, often vesiculated or lichenified skin around the fingers and nail folds, coexisting with nail separation and possible nail dystrophy.
- Lichen Planus:
- Rash Description: Lichen planus typically presents as pruritic, polygonal, purple, planar papules and plaques. It can affect skin, mucous membranes, hair, and nails.
- Nail Involvement: Nail lichen planus is rarer but can cause significant damage, including onycholysis, longitudinal ridging, thinning of the nail plate, pterygium formation (fusion of the proximal nail fold to the nail bed), and even complete nail loss (anonychia).
- Visual Clues in Images: Look for the characteristic purplish, flat-topped papules on the skin, particularly on the flexor surfaces of wrists and ankles, in conjunction with onycholysis and other nail dystrophies.
- Fungal Infections (Tinea Corporis, Tinea Pedis leading to Onychomycosis):
- Rash Description: Fungal skin infections often present as annular (ring-shaped) patches with raised, erythematous, and scaly borders (tinea corporis), or scaling, maceration, and itching, particularly between the toes (tinea pedis).
- Nail Involvement: While onychomycosis is a fungal infection of the nail itself, skin infections on the hands or feet can be a source or an accompanying sign. Onychomycosis commonly causes distal subungual onycholysis, accompanied by yellowing, thickening, and crumbly debris.
- Visual Clues in Images: Observe the classic “ringworm” pattern on the skin of the body, or scaling and redness on the feet, alongside the characteristic discolored and separated nails.
- Alopecia Areata:
- Rash Description: Not a rash in the typical sense, but an autoimmune condition causing patchy hair loss, usually on the scalp.
- Nail Involvement: While less common than psoriasis or eczema, alopecia areata can cause nail dystrophy, including fine pitting, trachyonychia (rough, sand-papered nails), and occasionally onycholysis.
- Visual Clues in Images: Look for smooth, round patches of hair loss on the scalp or body, co-occurring with onycholysis and other subtle nail surface changes.
The presence of a skin rash alongside onycholysis requires a careful dermatological assessment. The patterns seen in skin rash onycholysis images are invaluable for distinguishing between conditions that necessitate different diagnostic tests and treatment regimens, from antifungal medications to immunosuppressants or corticosteroids.
onycholysis Treatment
Effective onycholysis treatment fundamentally depends on accurately identifying and addressing its underlying cause. Since onycholysis is a symptom rather than a disease in itself, management strategies are highly individualized. A comprehensive treatment plan often combines specific medical interventions with general nail care practices. The goal of onycholysis treatment is to promote reattachment of the nail plate, prevent recurrence, and manage any associated pain or infection. Understanding the various therapeutic approaches is critical for successful outcomes.
Treatment modalities for onycholysis can be broadly categorized as:
1. Identification and Elimination of the Cause:
This is the most critical step. Without addressing the root cause, onycholysis is likely to persist or recur.
- Trauma:
- Management: Avoidance of further trauma. This includes cutting nails short to prevent leverage, wearing protective footwear, and being gentle during manicures/pedicures.
- Prevention: Education on proper nail care and protective measures in occupational or recreational settings.
- Fungal Infections (Onychomycosis):
- Diagnosis: Confirmed by microscopy (KOH prep) and fungal culture of subungual debris.
- Treatment:
- Topical Antifungals: Lacquers (e.g., ciclopirox, efinaconazole, tavaborole) applied daily. Effective for mild-to-moderate cases or as adjunctive therapy. Requires long-term application (months to a year).
- Oral Antifungals: (e.g., terbinafine, itraconazole, fluconazole). Reserved for more extensive or recalcitrant cases. Higher cure rates but carry risks of systemic side effects, requiring liver function monitoring. Treatment duration typically 6-12 weeks for fingernails, longer for toenails.
- Combination Therapy: Often more effective, using both oral and topical agents.
- Psoriasis:
- Treatment: Nail psoriasis is challenging.
- Topical Steroids: High-potency corticosteroids (e.g., clobetasol propionate) applied to the nail folds and under the nail.
- Topical Calcipotriol/Calcitriol: Vitamin D analogues, often combined with steroids.
- Intralesional Injections: Corticosteroids injected into the nail matrix or bed. Effective but painful.
- Systemic Therapies: For severe cases, methotrexate, cyclosporine, oral retinoids (acitretin), or biologics (e.g., adalimumab, ustekinumab) used to treat skin psoriasis can also improve nail involvement.
- Phototherapy: PUVA (psoralen plus UVA light) can be effective.
- Treatment: Nail psoriasis is challenging.
- Bacterial Infections (e.g., Pseudomonas):
- Treatment: Topical antibiotics (e.g., gentamicin solution, ciprofloxacin solution, mupirocin cream) often with debridement. Soaks in diluted white vinegar can also be helpful.
- Oral Antibiotics: Rarely needed unless there is significant cellulitis.
- Thyroid Disease:
- Treatment: Management of the underlying thyroid disorder (hypothyroidism or hyperthyroidism) with appropriate hormone replacement or antithyroid medications. Nail changes typically resolve as thyroid function normalizes.
- Drug-Induced Onycholysis:
- Management: Discontinuation of the causative medication (if clinically feasible and with physician approval). Psoralens, tetracyclines, and some chemotherapeutic agents are common culprits.
- Photoprotection: For photosensitizing drugs, strict sun protection of the nails.
- Allergic Contact Dermatitis:
- Diagnosis: Patch testing to identify specific allergens (e.g., nail glue, formaldehyde, acrylates, nail polish ingredients).
- Treatment: Strict avoidance of identified allergens. Topical corticosteroids to manage inflammation.
2. General Nail Care and Supportive Measures:
These practices are universally beneficial for managing onycholysis, regardless of the cause.
- Keep Nails Short: Trim the detached portion of the nail back to where it is firmly attached to the nail bed. This prevents further leverage, reduces the area for debris accumulation, and minimizes the risk of secondary trauma or infection.
- Avoid Moisture: Keep the nails dry. Prolonged immersion in water can worsen separation and promote bacterial/fungal growth. Wear gloves for wet work.
- Avoid Irritants and Chemicals: Protect nails from harsh soaps, detergents, solvents, and nail polish removers.
- Gentle Cleaning: Gently clean under the nail with a soft brush, avoiding sharp instruments that can cause further trauma or lift the nail plate.
- Protection: Wear gloves for manual tasks or activities where nails might be exposed to trauma.
- Avoid Nail Polish: While nail polish itself doesn’t cause onycholysis, it can trap moisture and chemicals, and make it difficult to monitor the nail or apply topical treatments. Some individuals may also develop an allergic reaction to polish components.
- Moisturize Nail Folds: Keeping the surrounding skin hydrated can prevent cracking and inflammation, particularly beneficial for conditions like eczema.
3. Management of Complications:
- Secondary Infections: If bacterial (green discoloration, pain, pus) or severe fungal infections develop, specific antibacterial or antifungal treatments are initiated, often in conjunction with debridement.
- Pain Management: For painful onycholysis, over-the-counter analgesics and addressing the underlying inflammatory cause are key.
Successful onycholysis treatment requires patience, as nails grow slowly (fingernails replace in 4-6 months, toenails in 12-18 months). Consistent adherence to the treatment plan and ongoing preventive measures are essential for nail reattachment and the restoration of healthy nails. Regular follow-up with a dermatologist is often recommended to monitor progress and adjust treatment as needed.