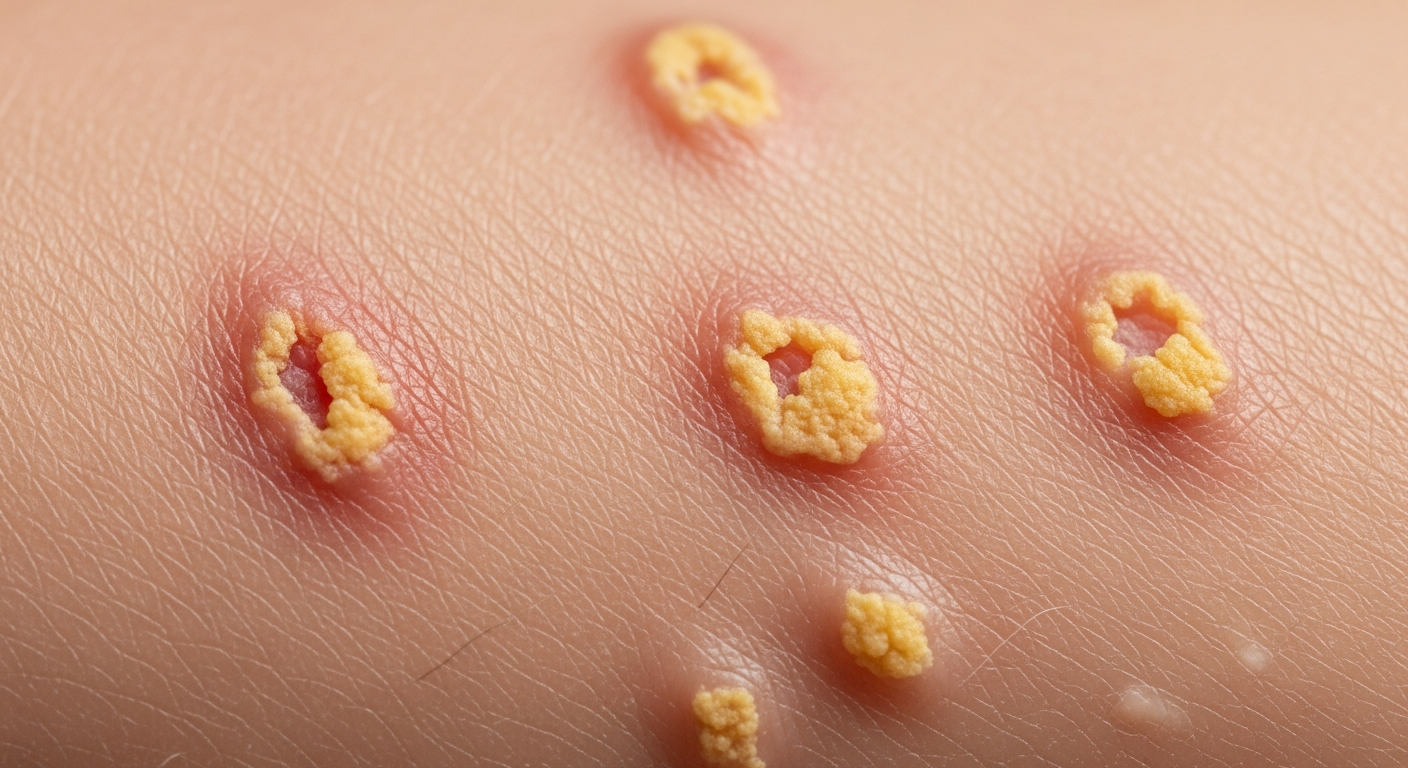
This article provides a detailed visual guide to Streptoderma symptoms pictures, focusing on the various manifestations of this common bacterial skin infection. Understanding these visual cues is crucial for timely identification and appropriate management, preventing the spread and potential complications. Examine the comprehensive descriptions accompanying these Streptoderma symptoms pictures to enhance recognition.
Streptoderma Symptoms Pictures
When observing Streptoderma symptoms pictures, a range of distinct dermatological features become apparent, reflecting the diverse clinical presentations of streptococcal skin infections. The primary lesions often begin as small macules or papules, rapidly evolving into characteristic vesicles, bullae, or pustules. These initial formations typically exhibit a clear to yellowish serous fluid, which quickly becomes turbid due to the accumulation of neutrophils and bacteria. The surrounding skin frequently displays varying degrees of erythema, indicating an active inflammatory process. A key visual hallmark in many streptoderma symptom images is the development of a thick, adherent crust, often described as “honey-colored” due to its distinctive golden-yellow hue. This crust forms as the seropurulent exudate dries, creating a protective but highly contagious covering over the eroded skin beneath.
The distribution of these lesions in streptoderma symptoms pictures is often localized, with a strong predilection for exposed areas of the body, particularly the face (perioral, perinasal regions), neck, and extremities such as the hands, forearms, and lower legs. In children, the diaper area or areas subjected to minor trauma, insect bites, or existing dermatoses (like eczema) are also common sites for initial infection. The lesions can vary in size from a few millimeters to several centimeters, sometimes coalescing to form larger, more irregular patches of crusted skin. The edges of the lesions, especially in conditions like erysipelas, might be sharply demarcated and raised, presenting a distinctive “peau d’orange” (orange peel) texture due to lymphatic involvement and swelling. Deeper forms of streptoderma, such as ecthyma, will show punched-out ulcers beneath the crusts, leaving scars upon healing. Pruritus, or itching, is a common accompanying symptom, leading to scratching that can further spread the infection to new sites, creating satellite lesions that are visually identical to the primary infection points. Pain and tenderness can also be observed, particularly in deeper or more extensive infections. Systemic symptoms, while not always visually apparent in a static image, often accompany these dermatological signs, including fever, malaise, and regional lymphadenopathy, which may manifest as visible swelling in the lymph node areas proximal to the infected skin. Detailed observation of these diverse features in streptoderma symptoms pictures is crucial for accurate diagnosis.
- Non-bullous Impetigo (Impetigo Contagiosa):
- Initial appearance: Small, red macules or papules that quickly progress to thin-walled vesicles.
- Evolution: Vesicles rupture within hours, releasing serous fluid.
- Crust formation: Characteristic golden-yellow to honey-colored crusts develop as the exudate dries. These crusts are typically sticky and loosely adherent.
- Underlying skin: Moist, erythematous, and superficially eroded skin is revealed when crusts are removed.
- Location: Most commonly seen on the face (around the nose and mouth), but also on hands, arms, and legs.
- Size and spread: Lesions are typically 0.5 to 2 cm in diameter, but can coalesce. Satellite lesions may appear due to autoinoculation.
- Associated symptoms: Mild itching (pruritus) is common, leading to scratching and further spread. Minimal pain.
- Bullous Impetigo:
- Initial appearance: Larger, flaccid bullae (blisters) ranging from 1 to 5 cm in diameter, often containing clear yellow fluid that later becomes cloudy.
- Crust formation: Bullae rupture, leaving a moist, erythematous base that forms a thin, varnish-like crust. The crust is less thick and less honey-colored than in non-bullous impetigo.
- Location: Often found on the trunk, buttocks, and extremities, but can occur anywhere. More common in infants and young children.
- Distinguishing features: Lack of surrounding erythema compared to non-bullous impetigo; lesions often appear more localized and discrete.
- Pathogen: Primarily caused by Staphylococcus aureus, but sometimes co-infection with Streptococcus or secondary staphylococcal infection can occur in streptoderma.
- Ecthyma:
- Definition: A deeper form of streptococcal skin infection that extends through the epidermis into the dermis.
- Initial appearance: Vesicles or pustules that evolve into a characteristic “punched-out” ulcer.
- Crust formation: A thick, adherent, dark brown to black crust covers the ulcer.
- Ulcer characteristics: Removing the crust reveals a deep, necrotic ulcer with raised, erythematous margins. The base of the ulcer often has a purulent exudate.
- Healing: Heals slowly and typically leaves a scar.
- Location: Most common on the lower extremities (shins, ankles) in individuals with poor hygiene, diabetes, or immunocompromise.
- Associated symptoms: More painful than impetigo, often accompanied by significant regional lymphadenopathy.
- Erysipelas:
- Definition: A superficial form of cellulitis with significant lymphatic involvement.
- Appearance: A bright red, fiery, well-demarcated plaque that is raised and often has an “orange peel” texture (peau d’orange). The borders are distinctively sharp and palpable.
- Progression: Spreads rapidly, often with a “tongue-like” extension.
- Location: Most commonly affects the face (malar area, bridge of nose, ears) and lower extremities.
- Systemic symptoms: High fever, chills, malaise, headache, and vomiting are common, often preceding the skin lesions. Significant regional lymphadenopathy is typical.
- Pain: The affected skin is exquisitely tender and warm to the touch.
- Cellulitis:
- Definition: A deeper bacterial infection of the dermis and subcutaneous tissue.
- Appearance: An erythematous, warm, swollen, and tender area of skin without the sharp demarcation seen in erysipelas. The borders are typically diffuse and poorly defined.
- Progression: Can spread rapidly and lead to systemic toxicity.
- Location: Can occur anywhere on the body, but most commonly affects the lower extremities.
- Associated features: May be accompanied by vesicles, bullae, pustules, or abscess formation.
- Systemic symptoms: Fever, chills, malaise, and regional lymphadenopathy are common.
- Distinguishing from Erysipelas: Lack of sharp borders and deeper tissue involvement.
Signs of Streptoderma Pictures
Observing signs of streptoderma pictures reveals the objective evidence of the infection as it manifests on the skin and potentially systemically. Beyond the primary lesions, several key indicators help in identifying streptoderma. One of the most prominent signs is erythema, a redness of the skin resulting from increased blood flow due to inflammation. This can range from a faint pink blush around early lesions to an intense, fiery red in more severe conditions like erysipelas. The degree and pattern of erythema are critical in distinguishing different forms of streptoderma; for instance, erysipelas presents with a uniquely bright red, sharply demarcated plaque, while cellulitis exhibits a more diffuse and poorly defined redness. Another significant sign is edema, or swelling, which occurs due to the accumulation of fluid in the interstitial spaces. This can cause the skin to appear puffy and taut, sometimes giving it a glossy sheen. In erysipelas, the edema can contribute to the characteristic “peau d’orange” texture, making the affected area feel firm and raised. These signs of swelling are often accompanied by a palpable warmth over the infected area, indicating heightened local metabolic activity and inflammation.
The progression of lesions is another crucial set of signs of streptoderma pictures. The transformation from fluid-filled vesicles (small blisters) to pustules (pus-filled blisters) to eventually crusts provides a dynamic visual timeline of the infection. The presence of seropurulent exudate, visible as clear, yellowish, or cloudy fluid oozing from ruptured lesions, is a strong indicator of bacterial activity and is highly contagious. When this exudate dries, it forms the characteristic honey-colored crusts of impetigo, or darker, more adherent crusts in ecthyma. The removal of these crusts often reveals an underlying erosion or ulceration, which may be moist, red, and sometimes bleeding. For deeper infections, such as ecthyma, a “punched-out” ulcer with necrotic tissue at its base is a definitive sign, indicating significant tissue destruction. Regional lymphadenopathy, manifested as visibly swollen and tender lymph nodes in the drainage area proximal to the infection, is a common systemic sign, suggesting the body’s immune response to the spreading bacteria. In severe cases, particularly with erysipelas and cellulitis, systemic signs like fever, chills, and general malaise can be inferred from the overall appearance of a patient, even if not directly visible in a static image. The patient might appear unwell, fatigued, and exhibit a flushed complexion due to fever. Careful examination of these visible and inferred signs in streptoderma pictures is essential for accurate diagnosis and assessment of disease severity.
- Erythema:
- Appearance: Redness of the skin, varying from a light pink to an intense, fiery red.
- Significance: Indicates inflammation and increased blood flow to the infected area.
- Variations:
- Erysipelas: Bright red, sharply demarcated, raised plaque.
- Cellulitis: Diffuse, poorly defined redness.
- Impetigo: Erythematous base beneath vesicles and crusts, often less extensive than in erysipelas/cellulitis.
- Edema (Swelling):
- Appearance: Puffy, swollen skin, sometimes glossy or taut.
- Significance: Accumulation of fluid in tissues due to inflammation and lymphatic obstruction.
- Variations:
- Erysipelas: Contributes to the “peau d’orange” texture and palpable induration.
- Cellulitis: Significant swelling, often pitting on pressure.
- Vesicles and Bullae:
- Vesicles: Small (up to 1 cm) fluid-filled blisters with clear or yellowish fluid.
- Bullae: Larger (over 1 cm) fluid-filled blisters, typically flaccid in bullous impetigo.
- Significance: Early stages of infection, indicating superficial epidermal involvement and bacterial toxin production.
- Pustules:
- Appearance: Vesicles or bullae that become filled with pus (a milky, opaque fluid containing neutrophils and cellular debris).
- Significance: Direct evidence of bacterial proliferation and immune response.
- Exudate and Crusting:
- Seropurulent Exudate: Oozing of clear, yellow, or cloudy fluid from ruptured lesions. Highly contagious.
- Honey-colored Crusts: Characteristic golden-yellow, sticky crusts formed when exudate from impetigo lesions dries.
- Dark, Adherent Crusts: Thicker, often dark brown or black crusts seen in ecthyma, covering a deeper ulcer.
- Significance: Hallmark of impetigo; indicates active infection and bacterial growth.
- Erosion and Ulceration:
- Erosion: Superficial loss of epidermis, often revealed after crust removal in impetigo. Heals without scarring.
- Ulceration: Deeper loss of tissue extending into the dermis, characteristic of ecthyma. Heals with scarring.
- Significance: Indicates tissue destruction, with ulcers signifying a more severe, deeper infection.
- Warmth and Tenderness:
- Appearance: Affected skin feels noticeably warmer to the touch.
- Tenderness: Pain upon palpation of the infected area.
- Significance: Localized inflammation and active infection. Prominent in erysipelas and cellulitis.
- Regional Lymphadenopathy:
- Appearance: Swollen, sometimes visibly enlarged, and tender lymph nodes in the area draining the infection.
- Significance: Immune response to bacterial dissemination from the primary site. A common systemic sign.
- Systemic Symptoms:
- Fever and Chills: Elevated body temperature and shivering, particularly common in erysipelas and cellulitis.
- Malaise: General feeling of discomfort, illness, or uneasiness.
- Headache: May accompany fever and systemic inflammation.
- Significance: Indicates systemic involvement and a more severe infection requiring prompt attention.
Early Streptoderma Photos
Examining early streptoderma photos is vital for recognizing the initial manifestations of this bacterial skin infection, facilitating prompt intervention. The very first signs often appear subtle, starting with an innocuous-looking red spot or a small, raised bump. Typically, the infection begins as a small macule, a flat, red discolored area of the skin, or a slightly elevated papule, often measuring just a few millimeters in diameter. These initial lesions are frequently located on areas of skin that have experienced minor trauma, such as scrapes, insect bites, or existing dermatoses, which serve as portals of entry for the bacteria. The redness around these nascent lesions might be minimal at first, easily overlooked as a common skin irritation. However, the rapidity of progression is a key characteristic to look for in early streptoderma photos. Within a matter of hours, or at most a day or two, these macules and papules quickly evolve into distinct, fluid-filled lesions.
The next discernible stage in early streptoderma photos involves the development of vesicles or pustules. Vesicles are small, clear or yellowish fluid-filled blisters, usually thin-walled and fragile. These can appear individually or in clusters. It’s crucial to note that the fluid within these vesicles rapidly becomes cloudy, transforming into pustules as neutrophils and bacteria accumulate. This transition from a clear vesicle to a pus-filled pustule is a definitive early sign of bacterial proliferation. The surrounding erythema also tends to become more pronounced as the inflammatory response intensifies. The initial localization often targets the perioral and perinasal regions on the face, where minor abrasions or irritations from nose-wiping or lip-licking are common. On the extremities, early streptoderma photos might show lesions developing around fingernails or on the dorsal surfaces of hands, especially in children. These early lesions are highly contagious, and even a slight scratch or touch can transfer bacteria to adjacent or distant skin sites, leading to the formation of new, discrete lesions. This autoinoculation process means that multiple lesions in various stages of development can often be observed simultaneously. Recognizing these subtle yet rapidly progressing signs in early streptoderma photos is paramount for early diagnosis and treatment, preventing widespread skin involvement and potential complications.
- Initial Macules and Papules:
- Appearance: Small (1-5 mm) flat red spots (macules) or slightly raised red bumps (papules).
- Color: Typically light to medium red, sometimes with a faint pinkish hue.
- Location: Often begin at sites of minor skin trauma (scratches, insect bites, abrasions) or existing skin conditions. Common on the face (around the nose and mouth) and extremities.
- Feeling: May be mildly itchy or asymptomatic initially.
- Significance: The very first visible sign of infection, representing the initial inflammatory response to bacterial colonization.
- Rapid Vesicle Formation:
- Appearance: Within hours to a day, macules/papules rapidly transform into small, thin-walled, fluid-filled blisters (vesicles).
- Fluid content: Initially clear or serous (yellowish), often appearing translucent.
- Size: Typically 1-5 mm in diameter.
- Surrounding skin: May have a faint erythematous halo.
- Fragility: These vesicles are very fragile and often rupture easily.
- Significance: Marks the rapid progression of bacterial replication within the superficial epidermis.
- Pustule Development:
- Appearance: Vesicles quickly become opaque and filled with pus (a cloudy, yellowish-white fluid).
- Progression: This stage often occurs very quickly after vesicle formation, sometimes within a few hours.
- Distinction: The pus indicates a significant accumulation of white blood cells (neutrophils) fighting the bacterial infection.
- Significance: A clear sign of active bacterial infection and immune response.
- Early Crusting:
- Appearance: As vesicles/pustules rupture, the seropurulent fluid dries to form a crust.
- Color: Initially light yellow to golden, often described as “honey-colored.”
- Texture: Sticky and somewhat loosely adherent to the underlying skin.
- Underlying skin: Moist and erythematous erosion is visible when the crust is gently lifted.
- Significance: The earliest stage of crust formation, indicative of ruptured superficial lesions.
- Erythematous Halo:
- Appearance: A ring of redness surrounding the nascent vesicles or pustules.
- Significance: Localized inflammation and increased blood flow in response to the infection.
- Progression: May become more pronounced as the infection progresses.
- Satellite Lesions:
- Appearance: New lesions, often in the same early stages (macules, papules, vesicles), appearing adjacent to or at a distance from the primary infection site.
- Cause: Autoinoculation due to scratching or touching the primary lesions and then touching unaffected skin.
- Significance: Demonstrates the highly contagious nature of streptoderma and its potential for rapid spread.
- Mild Pruritus:
- Feeling: Mild itching may be present even in the earliest stages.
- Consequence: Contributes to scratching, which exacerbates autoinoculation and spread.
- Significance: An important subjective symptom that can alert individuals to a developing skin issue.
Skin rash Streptoderma Images
When reviewing skin rash streptoderma images, the visual patterns and distribution of the lesions provide critical clues for diagnosis. Streptoderma manifests as a highly variable rash, primarily depending on the specific clinical type. The most common presentation in skin rash streptoderma images is impetigo, which typically appears as a localized or multifocal rash characterized by rapidly evolving vesicles and pustules that soon transform into golden-yellow, honey-colored crusts. This crusting rash often forms discrete patches that can coalesce, creating larger areas of involvement. The borders of these impetigo lesions are usually irregular and somewhat ill-defined, differing significantly from the sharp demarcation seen in other forms. The distribution often favors exposed areas, particularly the face (around the nose, mouth, and cheeks), hands, and extremities. In children, it’s common to see this impetiginous rash spreading through autoinoculation, where scratching one lesion leads to new lesions appearing on previously unaffected skin. This results in a rash composed of lesions at various stages of development – some still vesicular, others already crusted – creating a dynamic and patchy appearance across the skin surface.
In contrast, skin rash streptoderma images displaying erysipelas show a distinctly different rash pattern. Erysipelas presents as a rapidly spreading, intensely red, fiery, and sharply demarcated plaque. The rash is elevated above the surrounding normal skin, and its borders are typically palpably warm and indurated, giving it a distinctive raised margin. The surface of this rash often has a characteristic “peau d’orange” texture due to significant dermal edema and lymphatic involvement. Facial erysipelas commonly affects the bridge of the nose and cheeks, sometimes forming a “butterfly” distribution. On the lower extremities, it can involve a large area of the limb. Cellulitis, another form of streptoderma, also appears as an erythematous rash, but unlike erysipelas, its borders are typically diffuse and poorly defined, blending into the surrounding skin. The cellulitic rash is also warm, tender, and swollen, often affecting deeper subcutaneous tissues. Ecthyma, the ulcerative form, appears as a localized rash of deeply crusted lesions that, when the crust is removed, reveal “punched-out” ulcers. These deep ulcers are typically surrounded by an erythematous and indurated border, and they are more commonly found on the lower legs. Understanding the distinct visual characteristics, patterns, and preferred anatomical sites in skin rash streptoderma images is fundamental for differentiating the various forms of this bacterial infection and guiding appropriate treatment strategies. The rash is often accompanied by itching, which further contributes to its spread and the presence of satellite lesions.
- Non-bullous Impetigo Rash (Honey-Crusted Rash):
- Appearance: Characterized by multiple, discrete or coalescing patches of golden-yellow to honey-colored crusts.
- Underneath the crusts: Moist, erythematous, superficially eroded skin.
- Distribution: Primarily on the face (perioral, perinasal, cheeks), but also common on hands, arms, and legs.
- Spread: Autoinoculation causes satellite lesions, resulting in a rash with lesions at various stages (vesicles, pustules, crusts).
- Contagiousness: Highly contagious through direct contact with the exudate from the rash.
- Associated symptoms: Mild itching, leading to scratching and further spread.
- Bullous Impetigo Rash (Blistering Rash):
- Appearance: Flaccid, clear to cloudy bullae (large blisters) that rupture to leave a thin, varnish-like crust on an erythematous base.
- Distribution: More common on the trunk, buttocks, and extremities; can be widespread in infants.
- Distinctive features: Lesions often appear more localized and discrete, with less surrounding erythema than non-bullous impetigo.
- Pathogen association: Often associated with Staphylococcus aureus, but clinically important to consider within the broader streptoderma context, especially with mixed infections.
- Erysipelas Rash (Fiery Red Plaque):
- Appearance: A bright red, intensely erythematous, warm, and tender plaque with sharply demarcated, raised, and often palpably firm borders.
- Texture: May have an “orange peel” (peau d’orange) appearance due to edema and lymphatic involvement.
- Distribution: Most commonly on the face (cheeks, bridge of nose) and lower extremities.
- Spread: Rapidly spreading with characteristic “tongue-like” extensions.
- Systemic symptoms: Often accompanied by high fever, chills, and malaise, which may precede the rash.
- Cellulitis Rash (Diffuse Redness):
- Appearance: An area of erythema, warmth, swelling, and tenderness with poorly defined, diffuse borders that gradually merge with the surrounding healthy skin.
- Depth: Affects deeper dermis and subcutaneous tissues.
- Distribution: Can occur anywhere, but most frequent on the lower extremities.
- Associated features: May include vesicles, bullae, or purulent discharge; can lead to systemic toxicity.
- Distinction from Erysipelas: Lack of sharp borders and deeper tissue involvement.
- Ecthyma Rash (Ulcerative Rash):
- Appearance: Begins as vesicles or pustules that evolve into a characteristic “punched-out” ulcer covered by a thick, adherent, dark brown to black crust.
- Underneath the crust: A deep, necrotic ulcer with raised, erythematous margins and a purulent base.
- Distribution: Most common on the lower extremities, especially shins and ankles.
- Healing: Heals slowly and leaves a scar.
- Associated symptoms: More painful than impetigo, often with significant regional lymphadenopathy.
- Perianal Streptoderma Rash:
- Appearance: Sharply demarcated, intensely red, glazed-looking erythema around the anus.
- Symptoms: Intense itching (pruritus ani), pain, and sometimes fissures or blood-streaked stools.
- Distribution: Localized to the perianal area, often extending a few centimeters outward.
- Clinical context: Commonly seen in children, often recurrent, and may be associated with strep throat.
- Angular Cheilitis (Perlèche):
- Appearance: Fissuring, erythema, and crusting at the corners of the mouth.
- Cause: Often multifactorial, but streptococcal infection can be a component, especially in children with lip-licking habits or orthodontic appliances.
- Symptoms: Pain, tenderness, and difficulty opening the mouth widely.
Streptoderma Treatment
Effective streptoderma treatment hinges on prompt diagnosis, often guided by the visual symptoms discussed, and the appropriate administration of antibiotics. The primary goal of treatment is to eradicate the bacterial infection, prevent local spread and autoinoculation, reduce the risk of transmission to others, and avert potential complications such as acute post-streptococcal glomerulonephritis (APSGN) or, less commonly, rheumatic fever. Antibiotic therapy is the cornerstone of streptoderma treatment. The choice between topical and systemic antibiotics depends on the extent and severity of the infection. For localized, non-bullous impetigo, topical antibiotics are often sufficient, while more widespread, bullous, or deeper infections like ecthyma, erysipelas, or cellulitis necessitate systemic oral or intravenous antibiotics. Furthermore, strict hygiene measures are an integral part of streptoderma treatment, crucial for controlling the spread of the highly contagious bacteria. Regular cleaning of the affected areas and adherence to hand hygiene protocols are paramount.
Topical antibiotics commonly used in streptoderma treatment include mupirocin 2% ointment or cream, fusidic acid 2% cream, and retapamulin 1% ointment. These are typically applied two to three times daily for 5 to 7 days. These agents are effective against both Streptococcus pyogenes and Staphylococcus aureus, which are the most common causative organisms. For more extensive or recalcitrant infections, or when there are signs of systemic involvement (fever, lymphadenopathy), oral systemic antibiotics are indicated. Penicillin V is often the first-line choice for streptococcal infections, given its efficacy and narrow spectrum. Alternatives for penicillin-allergic patients include erythromycin or clindamycin. Other commonly used oral antibiotics for streptoderma treatment include cephalexin, dicloxacillin, and amoxicillin/clavulanate. The duration of oral antibiotic therapy typically ranges from 7 to 10 days to ensure complete eradication and minimize recurrence and complication risks. In severe cases of erysipelas or cellulitis, particularly with widespread involvement, significant systemic symptoms, or immunocompromise, intravenous antibiotics such as penicillin G, ceftriaxone, or clindamycin may be required. Beyond antibiotics, supportive care is crucial. This includes gently cleaning crusts with soap and water or antiseptic solutions (e.g., chlorhexidine) to facilitate topical medication penetration and remove infectious material. Keeping nails short can prevent further autoinoculation and skin trauma from scratching. Covering lesions with loose dressings can reduce spread. Patient education regarding the contagious nature of streptoderma and the importance of completing the full course of antibiotics is essential. Follow-up is important, especially to monitor for resolution of symptoms and potential signs of complications, such as changes in urine output or color indicative of APSGN. Early and appropriate streptoderma treatment is key to achieving full recovery and preventing long-term sequelae.
- Topical Antibiotics:
- Mupirocin 2% Ointment/Cream:
- Mechanism: Inhibits bacterial protein synthesis.
- Usage: Applied 2-3 times daily for 5-7 days for localized impetigo. Effective against both S. pyogenes and S. aureus.
- Advantages: Low systemic absorption, low risk of resistance for topical use.
- Fusidic Acid 2% Cream/Ointment:
- Mechanism: Inhibits bacterial protein synthesis.
- Usage: Applied 2-3 times daily for 7 days. Also effective against S. pyogenes and S. aureus.
- Availability: More common in some regions than others.
- Retapamulin 1% Ointment:
- Mechanism: Inhibits bacterial protein synthesis at a different ribosomal site.
- Usage: Applied twice daily for 5 days. Specific for Gram-positive bacteria, including resistant strains.
- Indication: Approved for impetigo caused by susceptible S. pyogenes or S. aureus.
- Mupirocin 2% Ointment/Cream:
- Oral Systemic Antibiotics:
- Indications:
- Widespread or bullous impetigo.
- Ecthyma, erysipelas, cellulitis.
- Signs of systemic infection (fever, lymphadenopathy).
- Failure of topical treatment.
- High risk of post-streptococcal complications.
- First-Line Agents:
- Penicillin V (Phenoxymethylpenicillin):
- Mechanism: Cell wall synthesis inhibitor.
- Usage: Typically 250-500 mg 2-4 times daily for 7-10 days. Effective for streptococcal infections.
- Advantages: Narrow spectrum, less prone to resistance compared to broad-spectrum drugs.
- Dicloxacillin or Flucloxacillin:
- Mechanism: Penicillinase-resistant penicillins, effective against penicillin-producing S. aureus.
- Usage: Typically 250-500 mg 4 times daily for 7-10 days.
- Cephalexin (First-generation Cephalosporin):
- Mechanism: Cell wall synthesis inhibitor.
- Usage: Typically 250-500 mg 2-4 times daily for 7-10 days. Effective against both S. pyogenes and methicillin-susceptible S. aureus.
- Advantages: Good safety profile, well-tolerated.
- Penicillin V (Phenoxymethylpenicillin):
- Alternatives for Penicillin Allergy:
- Erythromycin (Macrolide):
- Mechanism: Inhibits bacterial protein synthesis.
- Usage: Typically 250-500 mg 4 times daily for 7-10 days.
- Considerations: Potential for gastrointestinal side effects and increasing resistance.
- Clindamycin (Lincosamide):
- Mechanism: Inhibits bacterial protein synthesis.
- Usage: Typically 150-300 mg 3-4 times daily for 7-10 days.
- Advantages: Good tissue penetration, effective against many Gram-positive bacteria and some anaerobes.
- Considerations: Risk of Clostridioides difficile infection.
- Doxycycline (Tetracycline):
- Mechanism: Inhibits bacterial protein synthesis.
- Usage: Typically 100 mg twice daily for 7-10 days.
- Considerations: Not for children under 8 years due to tooth discoloration, photosensitivity. Useful for some resistant strains.
- Erythromycin (Macrolide):
- Indications:
- Intravenous Antibiotics (for Severe Cases):
- Indications: Severe erysipelas or cellulitis, rapidly spreading infection, systemic toxicity (sepsis), immunocompromised patients, or failure of oral therapy.
- Common Agents:
- Penicillin G: For severe streptococcal infections.
- Ceftriaxone: Broad-spectrum cephalosporin, often used empirically.
- Clindamycin: For severe cases, especially if MRSA is suspected or penicillin allergy.
- Vancomycin or Daptomycin: For suspected or confirmed MRSA (Methicillin-resistant Staphylococcus aureus) infections.
- Hygiene and Supportive Care:
- Gentle Cleaning: Wash affected areas daily with mild soap and water or an antiseptic solution (e.g., chlorhexidine) to remove crusts and exudates.
- Nail Trimming: Keep fingernails short to prevent scratching, which can spread the infection (autoinoculation) and cause further skin damage.
- Covering Lesions: Loosely cover lesions with gauze or bandages to prevent further spread and protect the infected skin.
- Hand Hygiene: Frequent and thorough hand washing with soap and water or an alcohol-based hand sanitizer.
- Avoid Sharing: Do not share towels, clothing, bedding, or personal items to prevent transmission.
- Symptomatic Relief: Acetaminophen or ibuprofen for fever and pain, if present.
- Prevention of Complications:
- Acute Post-Streptococcal Glomerulonephritis (APSGN): Though rare, it’s a serious renal complication, primarily following infection with nephritogenic strains of S. pyogenes. Prompt antibiotic treatment does not reliably prevent APSGN, but it’s still crucial for other reasons.
- Rheumatic Fever: Less commonly associated with skin streptococcal infections compared to pharyngitis, but prevention is still a goal.
- Cellulitis/Abscess Formation: Early treatment prevents deeper tissue involvement and localized pus collections.
- Patient Education:
- Emphasize the importance of completing the full course of antibiotics, even if symptoms improve.
- Educate on contagion and measures to prevent spread.
- Advise on signs of worsening infection or complications requiring medical attention.