Understanding the visual manifestations of eyelid inflammation is crucial for accurate self-assessment and professional diagnosis. This article offers an in-depth exploration of blepharitis symptoms pictures, guiding you through the visible signs and characteristics of this common eye condition. Observing these signs can help in recognizing the severity and type of blepharitis.
blepharitis Symptoms Pictures
When examining blepharitis symptoms pictures, several key visual indicators stand out, ranging from subtle irritation to pronounced inflammation. The appearance can vary significantly depending on whether the blepharitis is anterior (affecting the outside front of the eyelid, where the eyelashes attach) or posterior (affecting the inner eyelid margin, where the meibomian glands are located). Both types of blepharitis often present with overlapping symptoms, making comprehensive visual analysis essential for effective management. Recognizing these blepharitis symptoms through detailed visual descriptions is the first step toward understanding the condition.
Here are some of the most common blepharitis symptoms visible in pictures:
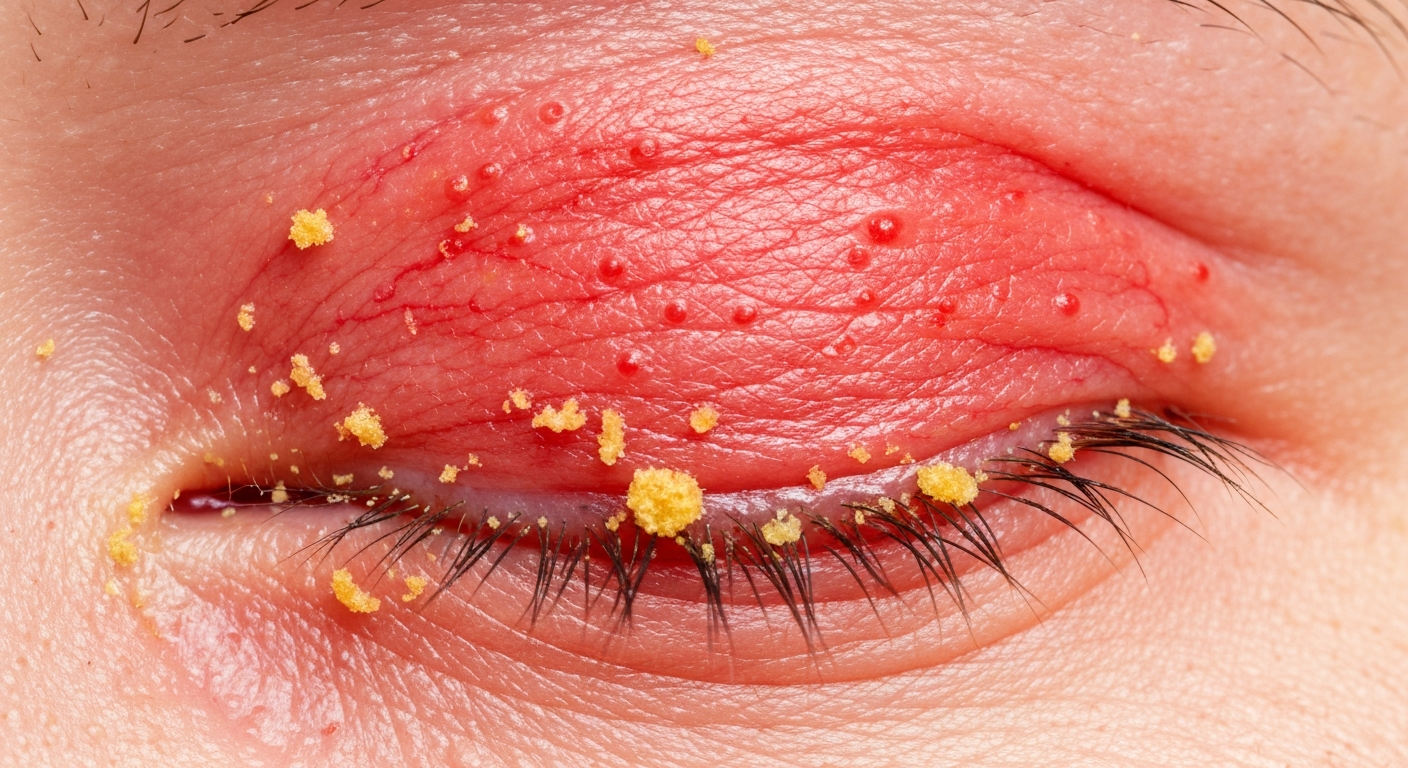
- Redness of the Eyelid Margins (Erythema): This is one of the most consistent blepharitis symptoms. The edges of the eyelids, particularly where the eyelashes emerge, appear visibly red or inflamed. This redness can range from a faint pink blush to an intense, fiery red, often indicating active inflammation. In blepharitis symptoms pictures, this erythema is a prominent feature, often presenting symmetrically on both upper and lower eyelids. The redness may extend slightly onto the adjacent skin or involve the conjunctiva, making the eyes appear bloodshot. Chronic redness is a hallmark sign of persistent blepharitis, signaling ongoing irritation and inflammation of the delicate eyelid tissues. This visible eyelid inflammation is a primary indicator for a blepharitis diagnosis.
- Swollen Eyelids (Edema): Eyelids affected by blepharitis frequently appear puffy or swollen. This swelling can be mild, making the eyelids look slightly heavier, or severe, causing significant discomfort and affecting vision. The edema is typically more pronounced in the morning due to fluid accumulation overnight. Observing swollen eyelids in blepharitis symptoms pictures helps to gauge the extent of the inflammatory response. This swelling, or edema, is a direct result of inflammation and can contribute to a feeling of tightness or pressure around the eyes. Chronic eyelid swelling is a strong indicator of blepharitis severity.
- Crusting or Flakes on Eyelashes: A definitive sign in blepharitis symptoms pictures is the presence of crusty deposits or flakes along the eyelashes and eyelid margins. These crusts are often yellowish or grayish and can resemble dandruff. They are composed of dried oil, skin cells, and sometimes bacteria, accumulating overnight. Upon waking, these crusts can make eyelids stick together, requiring warm compresses for removal. These flakes are a key diagnostic indicator for various forms of blepharitis, particularly anterior blepharitis, and their appearance is crucial for identification. The texture and color of the crusting can also provide clues about the underlying cause, such as seborrheic or staphylococcal blepharitis. Severe crusty eyelashes are a common blepharitis symptom.
- Greasy Eyelids: Particularly characteristic of posterior blepharitis or seborrheic blepharitis, the eyelids may appear shiny or greasy due to excessive oil production from dysfunctional meibomian glands. This oily sheen is often visible along the eyelid margins and can contribute to the formation of frothy tears. blepharitis symptoms pictures highlighting this greasy appearance indicate a problem with lipid secretion and distribution, which in turn affects tear film stability. This excessive oiliness can lead to blurred vision and discomfort. This greasy eyelid texture is a key visual sign of blepharitis, especially Meibomian Gland Dysfunction (MGD).
- Frothy Tears or Bubbles at Eyelid Margins: Dysfunction of the meibomian glands, common in posterior blepharitis, can lead to an unstable tear film. This instability often manifests as foamy or frothy tears accumulating at the eyelid margins, or small bubbles visible along the lash line. These bubbles are evidence of altered lipid composition in the tear film. Observing frothy tears in blepharitis symptoms pictures is a strong indicator of meibomian gland dysfunction (MGD), a common underlying cause of chronic blepharitis. This visual of foamy eye discharge is a crucial blepharitis sign.
- Misdirected Eyelashes (Trichiasis): Chronic inflammation associated with blepharitis can lead to scarring and distortion of the eyelash follicles. This can cause eyelashes to grow inwards, rubbing against the cornea and conjunctiva, leading to significant irritation and discomfort. This condition is known as trichiasis. Visual evidence of misdirected eyelashes in blepharitis symptoms pictures underscores the long-term impact of the disease on ocular health and can indicate a more advanced or persistent form of the condition. Trichiasis is a serious blepharitis complication.
- Loss of Eyelashes (Madarosis): In more severe or chronic cases of blepharitis, inflammation can damage eyelash follicles, leading to the thinning or complete loss of eyelashes. This can affect specific sections of the eyelid or lead to a more generalized reduction in lash density. Madarosis is a visible sign of chronic inflammatory damage to the eyelid margin. The absence or sparsity of eyelashes in certain areas in blepharitis symptoms pictures is a clear indicator of the severity and chronicity of the inflammation. Eyelash loss is a notable blepharitis symptom.
- Scaly Patches on Eyelid Skin: Especially in seborrheic blepharitis, the skin around the eyelids can develop fine, whitish or yellowish scales, similar to dandruff found on the scalp. These scaly patches are a result of excessive skin cell turnover and oil production. blepharitis symptoms pictures may reveal these discrete or diffuse areas of scaling on the eyelid skin, often extending beyond the lash line. This scaly appearance often accompanies itching and can be quite irritating. Scaly eyelid skin is a common blepharitis presentation.
- Itching or Burning Sensation: While not directly visible in blepharitis symptoms pictures, the physical manifestation of patients rubbing their eyes or signs of chronic irritation (like excoriation marks from scratching) can sometimes be inferred. Patients frequently report an intense itching or burning sensation, which contributes to the visible signs of irritation and redness. Chronic eye irritation is a persistent blepharitis complaint.
- Dry Eye Symptoms: Blepharitis frequently coexists with or causes dry eye syndrome due to its impact on the tear film. While dry eye itself isn’t a direct visual symptom in pictures, signs of chronic ocular surface irritation, such as diffuse redness of the conjunctiva (the white part of the eye), can be indirect indicators. The eyes may appear less lubricated, or tear film breakup time can be inferred by rapid evaporation. Dry, gritty eyes are often associated with blepharitis.
Signs of blepharitis Pictures
Beyond the primary symptoms, there are specific signs of blepharitis that are often more evident upon close inspection and are frequently captured in clinical blepharitis pictures. These signs offer deeper insights into the underlying pathology and help differentiate types of blepharitis. Understanding these observable characteristics is crucial for ophthalmologists and optometrists in making an accurate diagnosis and formulating an appropriate treatment plan for eyelid inflammation. These signs of blepharitis pictures are vital for precise clinical assessment.
Key signs of blepharitis that are frequently visualized in diagnostic blepharitis pictures include:
- Telangiectasia on Eyelid Margins: This refers to the dilation of small blood vessels, appearing as fine, spider-like red lines on the eyelid margins. Telangiectasia is a common sign of chronic inflammation and is particularly prevalent in individuals with ocular rosacea or long-standing posterior blepharitis. In blepharitis pictures, these visible blood vessels are a clear indication of ongoing vascular changes and chronic irritation of the delicate eyelid tissues. Their presence suggests a persistent inflammatory state that requires careful management. Eyelid margin telangiectasia is a key sign of chronic blepharitis.
- Collerettes (Cuffing of Lashes): These are cylindrical flakes or scales that encircle the base of the eyelashes. Collerettes are highly indicative of staphylococcal blepharitis, a bacterial form of anterior blepharitis. They are distinct from general crusting and appear as tight, sleeve-like formations around individual lash shafts. Seeing collerettes in blepharitis pictures is a strong diagnostic sign for bacterial involvement, requiring targeted antimicrobial treatment. The precise cuffing around the lash follicles differentiates them from simple, loose flakes. Cylindrical cuffing is a specific sign of staphylococcal blepharitis.
- Meibomian Gland Capping or Pouting: In posterior blepharitis, the meibomian glands along the inner eyelid margin may appear capped with thick, inspissated (thickened) oil, or the orifices may be pouting (everted). When pressure is applied to the eyelid, the meibomian glands may express toothpaste-like or granular secretions instead of clear oil. These visual changes in the meibomian gland orifices are key diagnostic signs of meibomian gland dysfunction (MGD). Blepharitis pictures often focus on these specific changes in the eyelid’s inner structure, revealing the extent of gland blockage and dysfunction, which directly impacts tear film quality and stability. Meibomian gland dysfunction is often seen in signs of blepharitis pictures.
- Notching of the Eyelid Margin: Long-term, severe blepharitis, especially if left untreated, can lead to scarring and permanent changes in the eyelid architecture. This can manifest as notching or irregularities along the eyelid margin, where parts of the margin may appear eroded or uneven. This sign in blepharitis pictures indicates chronic damage to the eyelid tissue and may suggest a more advanced stage of the disease, potentially requiring more intensive intervention. Eyelid notching indicates chronic blepharitis damage.
- Conjunctival Hyperemia: While blepharitis primarily affects the eyelids, the inflammation can extend to the conjunctiva, the membrane lining the inside of the eyelids and covering the white part of the eye. This results in generalized redness of the conjunctiva, known as conjunctival hyperemia. Observing bloodshot eyes alongside eyelid symptoms in blepharitis pictures suggests involvement of the ocular surface and may indicate a secondary conjunctivitis or dry eye component. Conjunctival redness is a common blepharitis sign.
- Formation of Chalazia or Styes (Hordeola): Blepharitis, particularly posterior blepharitis and MGD, can predispose individuals to recurrent chalazia (non-infectious cysts caused by blocked meibomian glands) and styes (infectious lumps caused by blocked and infected lash follicles or meibomian glands). The presence of these localized lumps or bumps on the eyelids in blepharitis pictures is a strong indicator of underlying blepharitis, as the inflammation and gland dysfunction create an environment conducive to their formation. Recurrent styes and chalazia are often linked to blepharitis.
- Demodex Mites: While not directly visible to the naked eye, the presence of Demodex mites can often be inferred by specific visual signs in blepharitis pictures, such as cylindrical sleeves or scales (similar to collerettes) at the base of the eyelashes, often referred to as “Demodex sleeves.” These sleeves are characteristic debris around the lash follicles caused by the mites. Microscopic examination is needed for definitive diagnosis, but their characteristic visual signs are important for clinical suspicion in blepharitis pictures. Demodex blepharitis often presents with these specific signs.
- Scarring of the Eyelid Margin: Chronic inflammation can lead to permanent fibrotic changes. In advanced cases, blepharitis pictures might show subtle or overt scarring along the eyelid margin, which can alter its contour and function. This scarring can contribute to trichiasis or ectropion/entropion over time. Eyelid scarring is a late-stage blepharitis sign.
- Punctal Stenosis or Occlusion: In some chronic forms of blepharitis, particularly with rosacea, the lacrimal puncta (small openings on the inner corner of the eyelids that drain tears) can become inflamed and stenosed (narrowed) or even occluded (blocked). This can lead to epiphora (excessive tearing) and is sometimes observable in blepharitis pictures as visibly inflamed or narrowed punctal openings. Punctal narrowing can be a blepharitis complication.
- Corneal Involvement: In severe or untreated blepharitis, the inflammation can extend to the cornea, leading to corneal infiltrates, ulcers, or vascularization. While these are typically observed with magnification, subtle signs of corneal irritation or redness around the limbus (the junction of the cornea and sclera) might be visible in detailed blepharitis pictures, indicating a more serious complication requiring immediate attention. Corneal complications are a severe sign of blepharitis.
Early blepharitis Photos
Identifying early blepharitis photos is critical for prompt intervention and preventing the condition from becoming chronic or more severe. In its initial stages, blepharitis symptoms can be subtle and easily overlooked or mistaken for simple eye irritation or fatigue. However, recognizing these incipient signs of eyelid inflammation is key to effective management. Early blepharitis photos provide valuable insights into the nascent presentation of this common ocular surface disease, highlighting the first subtle changes in the eyelid margin and associated structures. Understanding these initial visual cues is paramount for both patients and healthcare providers to identify early blepharitis symptoms.
Here are the early signs and symptoms of blepharitis as they would appear in early blepharitis photos:
- Mild Redness Along the Eyelid Margins: One of the earliest visual indicators in early blepharitis photos is a very subtle, almost imperceptible pinkish hue along the rim of the eyelids, particularly near the base of the eyelashes. This is a faint erythema, not yet a deep, angry red, but enough to suggest mild inflammation. It might be patchy or uniform, but it’s not severe. This initial redness is often dismissed as minor irritation, making it crucial to look for this subtle coloration. Early eyelid redness is a primary indicator.
- Fine, Sparse Flakes on Eyelashes: Unlike the heavy crusting of established blepharitis, early blepharitis photos might show only a few, very fine, almost dust-like flakes clinging to the base of the eyelashes. These flakes are often whitish or clear and can be easily dislodged. They are not yet forming thick, cohesive crusts, but their presence indicates an early accumulation of epithelial cells and possibly oil. This mild flaking is a precursor to more significant crusting. Sparse eyelash flakes are a subtle early blepharitis sign.
- Slightly Greasy Eyelid Appearance: In the early stages, particularly with incipient posterior or seborrheic blepharitis, the eyelid margins might exhibit a very slight sheen or a barely perceptible greasy texture. This isn’t overt oiliness, but a subtle change in the reflectivity of the eyelid skin. Early blepharitis photos can sometimes capture this subtle alteration in the visual texture of the eyelid surface, hinting at early meibomian gland dysfunction. Subtle greasy eyelids can indicate early blepharitis.
- Subtle Eyelid Swelling or Puffiness: There might be a very slight, almost imperceptible puffiness of the eyelids, especially noticeable in the morning. This swelling is not dramatic but gives the eyelids a slightly heavier appearance. Early blepharitis photos may show this minimal edema, often mistaken for sleepiness or mild allergies. This minor swelling indicates the initial stages of fluid retention due to inflammation. Minimal eyelid puffiness is an early blepharitis symptom.
- Increased Tear Film Instability (Implied): While not directly visible as a physical sign, early blepharitis photos might indirectly suggest increased tear film instability through observations like reflections on the eye surface or slight blurriness. Patients might report occasional blurring of vision, especially after blinking, due to the compromised tear film. This instability is a hallmark of early meibomian gland involvement. Unstable tear film is an early sign of blepharitis.
- Mild Irritation or Foreign Body Sensation: Patients in the early stages might report a vague feeling of irritation, grittiness, or a sensation as if something is in their eye. While not visible in early blepharitis photos, this subjective symptom often accompanies the minimal objective signs. It’s important to correlate patient symptoms with even the slightest visual changes. Gritty eye sensation is a common early complaint.
- Occasional Itching or Burning: Similar to irritation, mild, intermittent itching or a slight burning sensation can be an early indicator. These sensations are often sporadic and might not be constant, making them easy to dismiss. However, when paired with even subtle visual changes in early blepharitis photos, they become significant. Intermittent eye itching can indicate early blepharitis.
- Subtle Changes in Eyelash Orientation: In very early stages, some eyelashes might show a barely noticeable deviation from their normal growth pattern. This isn’t full-blown trichiasis but a slight disarray that hints at inflammation affecting the follicles. Early blepharitis photos might capture these minor shifts in eyelash alignment. Slight eyelash disarray can be an early sign.
- Minimal Loss of Eyelashes (Localized): Rarely, early blepharitis photos might reveal one or two isolated eyelashes that have fallen out, or a very slight thinning in a highly localized area. This is not widespread madarosis but a subtle sign of early follicular damage from localized inflammation. Localized eyelash thinning is an early blepharitis indicator.
- Absence of Severe Symptoms: Crucially, early blepharitis photos are characterized by the absence of severe signs like heavy crusting, significant scarring, extensive telangiectasia, or recurrent chalazia/styes. The absence of these more advanced symptoms helps to confirm an early-stage presentation, emphasizing that prompt recognition of the subtle signs is key to preventing progression. The lack of severe symptoms is key for early blepharitis identification.
Skin rash blepharitis Images
When blepharitis presents with more pronounced skin involvement, often resembling a dermatological rash, the visual presentation in skin rash blepharitis images becomes distinct. This typically occurs when blepharitis is associated with underlying skin conditions such as seborrheic dermatitis, rosacea, or contact dermatitis affecting the periocular area. These skin rash blepharitis images highlight not only the eyelid margin inflammation but also the broader inflammatory and scaling patterns on the surrounding skin. Understanding these specific visual cues is vital for a differential diagnosis and for tailoring treatment to both the ocular and dermatological aspects of the condition. A blepharitis rash indicates more extensive skin involvement.
Here are the detailed characteristics observed in skin rash blepharitis images:
- Diffuse Erythema Extending Beyond Eyelid Margins: Unlike isolated eyelid margin redness, skin rash blepharitis images often show a more widespread redness (erythema) that extends from the eyelid margins onto the surrounding facial skin, including the upper and lower eyelids, and sometimes the periorbital area. This diffuse redness is indicative of a broader inflammatory process involving the skin beyond the immediate lash line, frequently seen in conditions like rosacea blepharitis or contact dermatitis. Widespread facial redness accompanying eyelid inflammation is a strong indicator of skin rash blepharitis.
- Scaly Patches and Flaking on Adjacent Skin: A hallmark of seborrheic blepharitis presenting as a rash is the presence of greasy, yellowish, or whitish scales on the eyelid skin itself and often extending to the eyebrows, glabella (area between the eyebrows), and nasolabial folds. Skin rash blepharitis images will clearly depict these scaly patches, which can be fine and powdery or thicker and more adherent, distinguishing them from the simpler flakes found directly on eyelashes. This scaly skin is a key feature in seborrheic dermatitis-associated blepharitis. Greasy, scaly patches on periocular skin define seborrheic blepharitis rash.
- Greasy or Oily Skin Texture: The entire periocular skin, not just the eyelid margins, may appear noticeably oily or greasy in skin rash blepharitis images, especially in seborrheic forms. This is due to hyperactivity of sebaceous glands in the facial skin, contributing to the overall dermatological manifestation. The combination of redness and oiliness with scales is highly characteristic. Oily skin around the eyes often accompanies this blepharitis skin rash.
- Papules and Pustules on Eyelids and Periocular Skin: In blepharitis associated with ocular rosacea, skin rash blepharitis images might reveal small, red bumps (papules) or pus-filled lesions (pustules) on the eyelids and surrounding skin. These lesions are similar to those seen in facial rosacea and indicate a inflammatory response within the skin itself. The presence of these acneiform lesions near the eyes is a strong indicator of rosacea-related blepharitis. Eyelid papules and pustules are specific to rosacea blepharitis.
- Telangiectasia on Facial Skin (Beyond Eyelids): While telangiectasia can appear on the eyelid margins, in skin rash blepharitis images related to rosacea, these dilated blood vessels might also be visible on the cheeks, nose, and forehead, extending towards the eyes. This broader pattern of vascular changes reinforces the systemic nature of rosacea affecting the ocular area. Facial telangiectasia extending from eyelids suggests rosacea blepharitis.
- Edema and Induration of Periocular Skin: The skin around the eyes may not only be swollen (edematous) but also feel thickened and hardened (indurated) in chronic or severe cases of skin rash blepharitis. This change in skin texture is often visible in images, suggesting long-standing inflammation that has led to structural changes in the dermal layers. Thickened, hardened periocular skin indicates chronic skin rash blepharitis.
- Lichenification: In chronic itching and rubbing associated with severe skin involvement, the skin around the eyes can become thickened and develop exaggerated skin lines, a process called lichenification. Skin rash blepharitis images might capture these changes, indicating prolonged irritation and mechanical trauma to the skin. Skin lichenification around the eyes is a sign of chronic blepharitis with scratching.
- Excoriation Marks: Due to intense itching, patients might scratch the periocular skin, leading to visible scratch marks (excoriations) or skin breaks. These can appear as linear abrasions or areas of raw, irritated skin in skin rash blepharitis images, pointing to the severity of pruritus experienced. Scratch marks are clear indicators of severe itching in skin rash blepharitis.
- Contact Dermatitis-like Presentation: If the blepharitis is exacerbated by an allergic reaction (e.g., to cosmetics, eye drops, or contact lens solutions), skin rash blepharitis images might show signs typical of contact dermatitis:
- Intense Redness and Swelling: Often more acute and severe than other forms.
- Vesicles or Blisters: Small fluid-filled blisters can form on the eyelid skin, often breaking to form crusts.
- Oozing and Weeping: The affected skin may appear moist and ooze clear fluid, followed by crusting.
- Sharp Margins of Involvement: The rash might have clearer boundaries, corresponding to the area of contact with the allergen.
Contact dermatitis can mimic or worsen blepharitis with distinct skin rash images.
- Psoriasis-like Plaques: While less common, blepharitis can be associated with psoriasis. In such cases, skin rash blepharitis images might display well-demarcated, erythematous plaques covered with silvery scales on the eyelids or surrounding skin, characteristic of psoriatic lesions. Psoriasis can present as a blepharitis skin rash with silvery scales.
blepharitis Treatment
Effective blepharitis treatment is often multifaceted, aiming to alleviate symptoms, reduce inflammation, control bacterial load, and manage underlying conditions. Since blepharitis is frequently a chronic condition, treatment strategies emphasize long-term management and patient education on eyelid hygiene. The goal is not just symptomatic relief but also to prevent exacerbations and complications. Understanding the various components of blepharitis treatment is crucial for sustained ocular health and comfort. This section provides a comprehensive overview of the different approaches to managing blepharitis effectively, focusing on practical steps for blepharitis relief and long-term care.
Here are the primary components of blepharitis treatment:
- Eyelid Hygiene (Warm Compresses and Eyelid Scrubs): This is the cornerstone of all blepharitis treatment regimens. Consistent and proper eyelid hygiene helps to remove crusts, debris, and excess oil from the eyelid margins, and to unblock meibomian glands.
- Warm Compresses: Applying a clean, warm compress (such as a washcloth soaked in warm water or a specialized heated eye mask) to closed eyelids for 5-10 minutes, 1-2 times daily, is essential. The heat helps to loosen crusts, melt thickened oils in the meibomian glands, and improve circulation. Following the compress, gentle massage of the eyelids can further aid in expressing the softened oils from the glands. This crucial step in blepharitis treatment promotes better meibomian gland function.
- Eyelid Scrubs/Cleansing: After the warm compress, gently scrub the eyelid margins with a diluted baby shampoo solution (one drop of baby shampoo in a small cup of warm water) or a commercially available eyelid cleanser (foam, gel, or pre-moistened wipes). Use a clean fingertip, cotton swab, or lint-free pad to gently scrub along the base of the eyelashes. This physically removes bacteria, debris, and flakes. For posterior blepharitis, cleaning the inner eyelid margin can also be beneficial. This routine for blepharitis treatment must be performed diligently to reduce eyelid inflammation.
- Topical Antibiotics: For blepharitis with a significant bacterial component (e.g., staphylococcal blepharitis), topical antibiotic ointments or drops may be prescribed to control bacterial overgrowth.
- Ointments (e.g., Bacitracin, Erythromycin): Applied thinly to the eyelid margins, usually at bedtime. The ointment helps to reduce bacterial load and can also act as a protective barrier overnight, preventing crust formation. They are particularly effective for anterior blepharitis. This antibiotic eye ointment is a common blepharitis treatment.
- Drops (e.g., Azithromycin, Tobramycin): Used when there’s associated conjunctivitis or corneal involvement. Azithromycin, specifically, has anti-inflammatory properties in addition to its antibiotic effect, which can be beneficial in chronic blepharitis treatment. Antibiotic eye drops can treat blepharitis bacterial infections.
- Oral Antibiotics: In more severe or unresponsive cases, especially with posterior blepharitis, meibomian gland dysfunction, or rosacea-associated blepharitis, oral antibiotics may be used for their anti-inflammatory properties at sub-antimicrobial doses.
- Tetracyclines (e.g., Doxycycline, Minocycline): These are commonly prescribed due to their ability to reduce inflammation and modify meibomian gland secretions, making the oils thinner and less likely to block glands. They are often given at low doses for an extended period. Oral doxycycline for blepharitis is a widely used long-term treatment.
- Macrolides (e.g., Azithromycin): An alternative for those who cannot tolerate tetracyclines. It also has anti-inflammatory effects and can improve meibomian gland function. Oral azithromycin is another option for blepharitis management.
- Topical Anti-inflammatory Medications: These are used to control the inflammatory response directly and reduce discomfort.
- Corticosteroid Eye Drops/Ointments: Short-term use may be prescribed for acute exacerbations or severe inflammation. These reduce redness and swelling quickly but require careful monitoring due to potential side effects like increased intraocular pressure. Steroid eye drops offer rapid relief for severe blepharitis.
- Cyclosporine Eye Drops (e.g., Restasis, Cequa): Used for chronic blepharitis, especially when associated with dry eye. Cyclosporine helps to increase natural tear production and reduces inflammation on the ocular surface and within the meibomian glands. It’s a long-term blepharitis treatment option for persistent inflammation.
- Lifitegrast Eye Drops (e.g., Xiidra): Another anti-inflammatory agent that targets specific pathways of inflammation involved in dry eye and may be beneficial in blepharitis associated dry eye. Lifitegrast can aid in blepharitis-related dry eye treatment.
- Artificial Tears and Lubricating Eye Drops: Blepharitis often causes or exacerbates dry eye symptoms due to tear film instability. Regular use of preservative-free artificial tears helps to lubricate the eyes, rinse away irritants, and stabilize the tear film, providing symptomatic relief. Lubricating eye drops are essential for blepharitis symptom relief.
- Omega-3 Fatty Acid Supplements: Oral omega-3 supplements (found in fish oil, flaxseed oil) have been shown to improve meibomian gland function and reduce inflammation in some individuals, particularly those with posterior blepharitis and dry eye. This is a supportive blepharitis treatment that targets underlying meibomian gland health.
- Management of Underlying Conditions: Addressing coexisting conditions is vital for successful blepharitis treatment, as these often contribute to its chronicity.
- Seborrheic Dermatitis: Management of scalp and facial seborrheic dermatitis with medicated shampoos and creams can significantly improve seborrheic blepharitis. Treating underlying seborrheic dermatitis is crucial for blepharitis.
- Ocular Rosacea: Treatment for facial rosacea (e.g., oral doxycycline, topical metronidazole) often improves ocular symptoms. Managing ocular rosacea directly impacts blepharitis.
- Demodex Infestation: If Demodex mites are identified as a contributing factor, specific treatments like tea tree oil preparations (e.g., eyelid wipes containing terpinen-4-ol) or topical ivermectin creams (off-label for eyelids) may be used to eradicate the mites. Demodex blepharitis treatment targets mite eradication.
- In-office Procedures: For chronic or severe meibomian gland dysfunction that is unresponsive to home care, several in-office procedures can provide additional relief by targeting the root cause.
- LipiFlow/TearScience/iLux/MGD Express: Thermal pulsation treatments that apply heat and pressure to the eyelids to melt and express blockages from the meibomian glands. These devices can significantly improve gland function. In-office MGD treatment devices offer advanced blepharitis care.
- BlephEx: A microblepharoexfoliation device used by an ophthalmologist to mechanically remove debris, biofilm, and Demodex mites from the eyelid margins. BlephEx for blepharitis effectively removes eyelid debris.
- Intense Pulsed Light (IPL) Therapy: Can be effective for rosacea-associated blepharitis and MGD by reducing inflammation and improving meibomian gland function. IPL therapy is an emerging blepharitis treatment option.
- Environmental and Lifestyle Modifications: These adjustments can help minimize triggers and support the overall blepharitis treatment plan.
- Avoidance of Irritants: Minimize exposure to smoke, dust, wind, and allergens that can exacerbate eyelid irritation.
- Contact Lens Care: If wearing contact lenses, ensure proper hygiene and consider temporary discontinuation during flare-ups of blepharitis symptoms.
- Cosmetics: Avoid eye makeup during active inflammation and ensure thorough removal of all cosmetics, which can clog glands and trap bacteria.
Lifestyle changes are crucial for long-term blepharitis management.