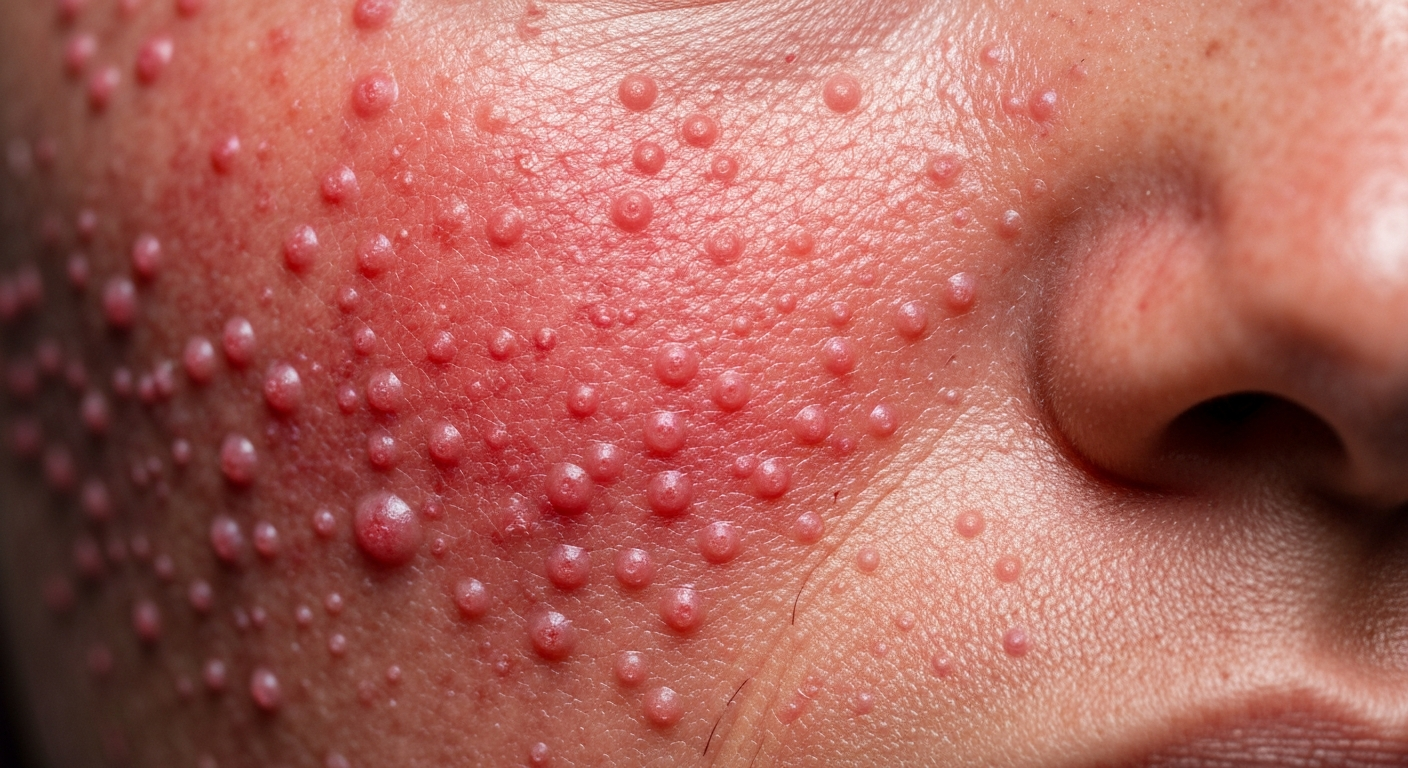
Recognizing the distinct visual characteristics of demodicosis is crucial for accurate diagnosis. This article provides detailed descriptions of various demodicosis symptoms pictures, guiding you through the often subtle yet significant changes observed on the skin, focusing on what to look for when examining photographic evidence of this condition.
demodicosis Symptoms Pictures
Understanding the full spectrum of demodicosis symptoms pictures is paramount for healthcare professionals and individuals seeking information on this skin condition. Demodicosis, caused by an overpopulation of Demodex mites, manifests with a wide array of visual signs that can often mimic other dermatological issues, making precise identification challenging without detailed knowledge. The symptoms are largely a result of the mites, their waste products, and the host’s immune response within the hair follicles and sebaceous glands.
One of the most common presentations visible in demodicosis symptoms pictures is persistent facial redness, often concentrated around the T-zone (forehead, nose, chin) and cheeks. This erythema can range from a mild, diffuse pinkish hue to a more intense, fiery red. The redness may be transient initially, appearing after hot showers, exercise, or consumption of spicy foods, similar to rosacea. However, with chronic demodicosis, the redness often becomes fixed and more prominent. Accompanying this redness, individuals frequently report a burning or stinging sensation, which may not always be visible but contributes to the patient’s discomfort. The skin surface might also appear slightly rough or uneven due to subtle scaling and follicular changes.
Another key visual symptom found in demodicosis pictures includes the presence of small, red papules and pustules. These lesions are typically small, solid bumps (papules) or pus-filled bumps (pustules) that are often clustered. Unlike typical acne vulgaris, demodicosis papules and pustules tend to lack comedones (blackheads or whiteheads) and are often more uniformly sized. They frequently occur on the cheeks, nose, and forehead, but can also extend to the scalp, neck, and chest. The pustules may be sterile or contain secondary bacterial infection, further complicating the visual presentation. In severe cases, these lesions can become confluent, forming larger, inflamed plaques, particularly on the nose, leading to tissue hypertrophy in a condition resembling rhinophyma, albeit often milder.
Intense itching, medically termed pruritus, is a hallmark symptom, even if not directly visible in a static picture. However, the consequences of scratching – excoriations, lichenification (skin thickening), and post-inflammatory hyperpigmentation – are frequently observed in demodicosis symptoms pictures. The itching is often worse at night when the mites are more active. This nocturnal exacerbation is a crucial diagnostic clue. Patients may present with generalized facial itchiness or localized itching, particularly around the eyes or scalp. The constant urge to scratch can lead to skin barrier disruption, making the skin more susceptible to irritation and secondary infections. Furthermore, a gritty sensation in the eyes, often accompanied by crusting of the eyelashes, can be a symptom of ocular demodicosis.
Detailed examination of demodicosis symptoms pictures might reveal a unique phenomenon known as “Demodex frost” or “follicular scaling.” This refers to fine, often white or grayish, powdery scales that adhere to the base of the eyelashes or to the follicular openings on the face. These scales are essentially collections of mite debris, keratin, and sebum, indicative of high mite activity within the follicles. This scaling is particularly noticeable under magnification and is a strong indicator of demodicosis. In addition to scaling, patients may experience a sensation of crawling or tingling on the skin, known as formication, although this is more subjective and not directly visible.
Common Types of Skin Lesions in demodicosis Pictures:
Erythema: Diffuse or patchy redness, often persistent and exacerbated by triggers like heat or exercise. Can range from a light pink blush to a deep, angry red. Visible prominently on the central face.
Papules: Small, solid, raised bumps (typically 1-3 mm in diameter) that are red or flesh-colored. They frequently appear in clusters and are often tender or itchy. Unlike acne, they usually lack a central pore (comedo).
Pustules: Small, pus-filled bumps, often with a red base. They are superficial and can rupture, leading to crusting. These are distinct from typical acne pustules in their distribution and lack of associated comedones.
Follicular Scales/Frost: Fine, often whitish or grayish, powdery scales adhering to the base of hairs (especially eyelashes) or around follicular openings on the face. This is a direct sign of mite activity and accumulation of debris.
Telangiectasias: Fine, visible blood vessels (spider veins) that often appear on the cheeks and nose, particularly in chronic cases or demodicosis mimicking rosacea. These are permanent dilations of superficial capillaries.
Oedema (Swelling): Mild to moderate swelling, especially around the eyes or on the central face, contributing to a generalized puffy appearance. This can be more pronounced in inflammatory forms of demodicosis.
Excoriations: Linear erosions or scabs resulting from scratching due to intense pruritus. These are secondary lesions but are highly indicative of symptomatic demodicosis.
Lichenification: Thickening of the skin with exaggerated skin markings, often due to chronic scratching or rubbing. The skin may appear leathery and rough to the touch.
Hyperpigmentation/Hypopigmentation: Darker or lighter patches of skin, respectively, can occur post-inflammation, especially in individuals with darker skin tones, as a residual effect of persistent lesions.
Signs of demodicosis Pictures
The observable signs of demodicosis pictures offer critical insights into the severity and chronicity of the condition. While symptoms are what a patient experiences, signs are what a clinician observes. These visual clues are essential for distinguishing demodicosis from other dermatoses that share similar presentations. A meticulous examination of the skin can reveal characteristic findings indicative of a high Demodex mite burden and the subsequent host inflammatory response.
One prominent sign observed in demodicosis pictures is generalized facial erythema, which is often persistent and may have a patchy or diffuse distribution. This redness is typically more pronounced on the cheeks, nose, and forehead. Unlike flushing, which is transient, the erythema in chronic demodicosis tends to be fixed. Coupled with this, the skin texture might appear rough or gritty upon palpation, an observation that can sometimes be inferred from close-up photographs showing irregular skin topography. Pores may also appear dilated or more prominent due to follicular inflammation and keratin plugging, especially around the nose and central face.
Follicular prominence is another key diagnostic sign. In signs of demodicosis pictures, one might notice that individual hair follicles appear more distinct or slightly raised, sometimes exhibiting a reddish halo around them. This is particularly evident on the forehead and cheeks. This sign reflects the inflammation and distension of the pilosebaceous units by accumulating mites, dead skin cells, and sebum. In certain cases, especially on the forehead, the entire texture of the skin can take on a granular or cobblestone-like appearance due to the widespread involvement of numerous follicles.
The presence of fine scales, often described as branny or pityriasiform, is a common sign. These delicate scales may be difficult to discern without magnification but can give the skin a dull or somewhat frosted appearance in good lighting. These scales are indicative of increased epidermal turnover and follicular dysfunction. In more severe cases, particularly in immunocompromised individuals, a more generalized scaling or crusting may be present, extending beyond the typical facial distribution to the neck, chest, and back. These severe presentations often represent a different form known as pityriasis folliculorum or generalized demodicosis.
For ocular demodicosis, specific signs are paramount in demodicosis pictures focusing on the eye area. These include erythema and swelling of the eyelid margins (blepharitis), often with associated crusting and cylindrical scales at the base of the eyelashes. These scales, known as “collarettes,” are pathognomonic for ocular demodicosis. Additionally, loss of eyelashes (madarosis) or misdirected eyelashes (trichiasis) can be observed due to chronic inflammation and follicular damage. The conjunctiva may also appear hyperemic (red) in severe cases, indicating a secondary conjunctivitis.
In chronic or neglected cases, more severe and disfiguring signs can develop. These include localized skin thickening (lichenification), especially on areas subject to repeated scratching. Persistent inflammation can also lead to lymphoedema, visible as persistent swelling and puffiness of the affected areas, contributing to a coarser facial appearance. Rarely, granulomatous demodicosis can occur, presenting as firm, skin-colored to reddish nodules or plaques, which require histological confirmation. These are significant findings that impact both appearance and function, necessitating prompt and effective treatment strategies.
Specific Visual Signs to Look for in demodicosis Pictures:
Fixed Erythema: Persistent redness of the skin, not just transient flushing. Often concentrated on the central face, giving a “rosacea-like” appearance. Can vary in intensity and distribution.
Follicular Prominence: Hair follicles appear more distinct, slightly raised, or surrounded by a subtle reddish ring. This indicates inflammation and distension of the pilosebaceous units.
Dilated Pores: Enlarged or more visible pores, especially on the nose, forehead, and cheeks, often a result of follicular blockage and inflammation. Skin may appear somewhat orange-peel like.
Cylindrical Scales (Collarettes): Characteristic waxy, cylindrical scales at the base of eyelashes, a hallmark sign of ocular demodicosis. These are composed of keratin, sebum, and mite debris.
Madarosis/Trichiasis: Loss of eyelashes (madarosis) or misdirection of eyelashes (trichiasis), indicating chronic inflammation and damage to the eyelash follicles. Visible as sparse or irregularly growing lashes.
Rough or Gritty Skin Texture: Palpable unevenness of the skin surface, often due to micro-papules, scales, and follicular changes. This can sometimes be inferred from textured appearance in close-up images.
Perioral/Periorbital Involvement: Redness, scaling, or papules specifically around the mouth (perioral) or eyes (periorbital) areas. This distribution can be a clue to demodicosis, distinguishing it from general acne.
Inflammatory Nodules/Plaques: In more severe or granulomatous forms, larger, firm, persistent bumps or flat-topped lesions may be present. These indicate a deeper and more intense inflammatory reaction.
Pigmentary Changes: Post-inflammatory hyperpigmentation (darkening) or hypopigmentation (lightening) can occur as a residual sign, particularly in individuals with darker skin tones, marking previous inflammatory lesions.
Rhinophyma-like Changes: While true rhinophyma is associated with severe rosacea, chronic demodicosis can, in rare instances, contribute to mild nasal enlargement or distortion due to persistent inflammation and tissue hypertrophy.
Early demodicosis Photos
Identifying early demodicosis photos requires a keen eye for subtle changes that might easily be overlooked or attributed to other common skin irritations. The initial manifestations of demodicosis are often mild and non-specific, making early diagnosis challenging but crucial for preventing progression to more severe forms. These early signs represent the very beginning of the host’s reaction to an increased mite population.
In early demodicosis photos, one might first observe a very mild, sometimes intermittent, redness on the central face. This erythema may not be constant and could be mistaken for slight blushing or a reaction to environmental factors. It often presents as a diffuse pinkish hue rather than distinct red patches. The skin might feel slightly warmer to the touch in these affected areas, though this tactile sensation is not visible in photographs. This initial redness is usually the body’s first inflammatory response to the proliferation of Demodex mites within the hair follicles.
Subtle changes in skin texture are another early indicator. Close-up early demodicosis photos might show a very fine, almost imperceptible roughness or a slight dullness to the skin’s surface. This can be due to minimal scaling that is not yet obvious but contributes to a less smooth appearance. Patients might describe their skin as feeling “gritty” or “less smooth than usual.” There might also be a very slight increase in follicular prominence, where the individual pore openings appear marginally more noticeable, particularly around the nose and forehead.
The earliest form of papules can be extremely small, almost micro-papules, which may be skin-colored or very faintly red. These tiny bumps are often best appreciated by touch rather than sight initially, but in good lighting, they might be visible as a textural unevenness in early demodicosis photos. They tend to be non-pustular at this stage and are often confined to a smaller area, such as the cheeks or forehead. These early papules represent localized inflammation around individual hair follicles reacting to the mite infestation.
Mild itching or a sensation of crawling (formication) on the skin is frequently reported as an early symptom, although it’s not directly visible in early demodicosis photos. However, if the itching is persistent enough to cause even minor scratching, subtle excoriations or very fine, linear abrasions might be seen. These are often transient and heal quickly, but their presence indicates ongoing skin irritation. The itching often follows a pattern of being worse at night, correlating with the nocturnal activity of Demodex mites as they emerge from follicles to mate.
For ocular involvement, early signs in early demodicosis photos of the eyelids might include minimal redness along the eyelid margins and a very subtle irritation at the base of the eyelashes. The characteristic cylindrical scales (collarettes) may not yet be fully formed or obvious, appearing as just a slight accumulation of whitish debris. Patients might experience mild eye irritation, dryness, or a foreign body sensation. Early detection of these subtle changes is vital as ocular demodicosis can lead to chronic blepharitis and visual discomfort if left untreated.
Characteristics of Early demodicosis Manifestations in Photos:
Mild, Intermittent Erythema: Subtle, transient redness, often resembling blushing or mild irritation, primarily on the central face. Not yet fixed or intense.
Subtle Skin Roughness: A very fine, almost imperceptible unevenness or textural change on the skin’s surface, indicating early follicular involvement or minimal scaling.
Micro-papules: Extremely small, skin-colored or faintly red bumps that are often best seen in excellent lighting or by touch. They represent initial inflammatory responses in individual follicles.
Slight Follicular Prominence: Hair follicles may appear marginally more distinct or slightly raised, particularly on the forehead and nose, preceding overt inflammation.
Localized Mild Itching: While not visible, early photos might show very faint signs of rubbing or minimal, superficial excoriations if the itching is sufficient. Itching is often worse at night.
Minimal Perifollicular Scaling: Very fine, powdery scales that are barely noticeable around hair follicles or at the base of eyelashes (in ocular cases), indicating early mite activity.
Increased Skin Sensitivity: Patients may report their skin becoming more easily irritated or reactive to products, though this is a subjective symptom.
Faint “Dullness” to Skin: The skin might lose some of its natural luminosity or appear slightly dull due to the accumulation of mite debris and minor scaling, especially when observed closely.
Isolated Eyelid Margin Redness: In early ocular demodicosis, a very faint pinkish hue along the edges of the eyelids, possibly with minimal crusting, before full-blown blepharitis.
Absence of Comedones: Crucially, unlike early acne, early demodicosis typically lacks blackheads or whiteheads, which helps differentiate it from other common follicular disorders.
Skin rash demodicosis Images
The appearance of a skin rash demodicosis images is one of the most common and visually impactful presentations of this condition. Demodex mites can trigger a variety of rash types, often leading to misdiagnosis due to their resemblance to acne, rosacea, or perioral dermatitis. Understanding the specific characteristics of these rashes in demodicosis images is vital for accurate identification and appropriate treatment.
One prevalent type of skin rash demodicosis is the erythematous-papulopustular rash. This rash is characterized by widespread redness (erythema) punctuated by numerous small, red bumps (papules) and sometimes pus-filled lesions (pustules). In demodicosis images, this can look strikingly similar to rosacea. The distribution is typically on the central face—cheeks, nose, forehead, and chin. The papules are usually symmetrical, monomorphic (similar in size and shape), and lack comedones, which differentiates them from acne. The pustules are often superficial and can be very numerous, contributing to a “bumpy” texture of the skin. Patients often report an intense burning or stinging sensation associated with this inflammatory rash, which further contributes to discomfort.
Another distinct presentation in skin rash demodicosis images is the pityriasis folliculorum-like rash. This form is characterized by diffuse redness and fine, branny, or dusty scaling over the affected areas. Unlike the papulopustular form, the prominent feature here is the scaling and a rough, sandpaper-like texture rather than distinct papules or pustules, though scattered small bumps may still be present. The scales are often adherent to follicular openings. This type of rash can be more subtle but widespread, covering larger areas of the face, and sometimes extending to the neck and chest. It often gives the skin a dull, desquamating appearance, and the itching can be a significant symptom, leading to visible excoriations.
Granulomatous demodicosis, while rarer, presents a more severe form of skin rash demodicosis. In demodicosis images, this rash consists of firm, reddish-brown to violaceous nodules or plaques. These lesions are deeper and more persistent than typical papules and pustules. They often result from a profound foreign body giant cell reaction to the Demodex mites or their chitinous exoskeletons, particularly in immunocompromised individuals. These nodules can be disfiguring and may require more aggressive diagnostic and therapeutic approaches. Their appearance can sometimes mimic sarcoidosis or other granulomatous dermatoses.
In cases of ocular demodicosis, the rash is confined to the eyelids and surrounding periorbital area. Skin rash demodicosis images of the eyes will show chronic blepharitis, characterized by redness, swelling, and thickening of the eyelid margins. The most characteristic sign is the presence of cylindrical dandruff or “collarettes” – waxy, sleeve-like scales that encircle the base of the eyelashes. Loss of eyelashes (madarosis) and misdirection of eyelashes (trichiasis) are also common. This specific rash pattern around the eyes is highly indicative of Demodex infestation.
Less commonly, a perioral or periorbital distribution of papules and pustules can be observed in skin rash demodicosis images, mimicking perioral dermatitis. Here, the rash is concentrated around the mouth (sparing a narrow strip around the vermilion border) or around the eyes. While the lesions are similar to the papulopustular type, their specific localization suggests demodicosis when other causes of perioral dermatitis have been ruled out. The constant itching and burning in these areas are also key symptomatic indicators.
Different Types of demodicosis Rashes to Identify in Images:
Erythematous-Papulopustular Rash: The most common type, characterized by diffuse redness, small red papules, and superficial pustules, often concentrated on the central face. Resembles rosacea but typically lacks telangiectasias in early stages and comedones of acne. Papules are usually monomorphic.
Pityriasis Folliculorum-like Rash: Features fine, branny or dusty scales overlying red or hyperpigmented skin. The skin texture often appears rough or sandy. Papules may be subtle or absent. Common on the forehead, temples, and cheeks. Often accompanied by intense itching.
Granulomatous demodicosis Rash: A rarer, more severe form presenting with firm, persistent reddish-brown to violaceous nodules or plaques. These are deeper lesions, often indicative of a profound inflammatory response and can be disfiguring. Requires careful differentiation from other granulomatous conditions.
Ocular demodicosis Rash (Blepharitis): Involves the eyelids, characterized by redness, swelling, and thickening of the eyelid margins. Key features include “collarettes” (cylindrical scales at eyelash base), madarosis (eyelash loss), and trichiasis (misdirected eyelashes). Leads to chronic eye irritation.
Perioral/Periorbital Rash: Papules and pustules concentrated specifically around the mouth (sparing the vermilion border) or around the eyes. This localized rash pattern can mimic perioral dermatitis, but the presence of mites confirms demodicosis.
Scaly Patches with Follicular Spines: Less common, but sometimes observed as discrete patches with prominent follicular openings plugged with keratinaceous material, giving a spiny or prickly feel. This can be more common on the scalp or neck.
Urticarial Rash: In rare instances, individuals can develop a hives-like rash (urticaria) as an allergic reaction to Demodex mites or their byproducts. This appears as itchy, raised, red welts that can be transient.
Lichenoid demodicosis Rash: Characterized by flat-topped, polygonal, purple papules or plaques, often intensely itchy, resembling lichen planus. This indicates a lymphocyte-mediated immune response to the mites.
Eczematous demodicosis Rash: Can present as patches of red, itchy, sometimes weeping or crusting skin, similar to eczema. This may be a result of chronic irritation and barrier dysfunction exacerbated by mites.
demodicosis Treatment
Effective demodicosis treatment aims to reduce the mite population, alleviate symptoms, and restore skin health. Given the diverse presentations of demodicosis, treatment strategies often involve a combination of topical and oral medications. The goal of demodicosis treatment is not necessarily to eradicate all Demodex mites, as they are a normal part of the skin microbiome, but rather to reduce their numbers to a level where they no longer trigger an inflammatory response or cause symptoms.
Topical medications form the cornerstone of demodicosis treatment, especially for mild to moderate cases. These agents directly target the mites on the skin surface and within follicles. The duration of topical treatment typically ranges from several weeks to months, depending on the severity and response. Patients are often advised to continue treatment for a period even after symptoms improve to prevent recurrence. Adherence to the treatment regimen is crucial for successful outcomes. Proper skin hygiene, including gentle cleansing, is also an important adjunct to topical therapy, helping to remove dead skin cells and mite debris.
For more severe, widespread, or recalcitrant cases, oral medications may be prescribed as part of demodicosis treatment. These systemic therapies work from within the body to combat the mite infestation and reduce inflammation. Oral treatments are often used in conjunction with topical agents to achieve a more rapid and comprehensive response. The choice of oral medication depends on the specific presentation, patient health status, and potential drug interactions. It is essential for patients to follow their healthcare provider’s instructions carefully when taking oral medications, especially regarding dosage and duration.
Beyond specific medications, supportive measures are also important in demodicosis treatment. These include avoiding triggers that exacerbate inflammation, such as excessive heat, spicy foods, alcohol, and certain cosmetics. Using gentle, non-comedogenic, and fragrance-free skincare products can help soothe irritated skin and prevent further irritation. Regular cleansing of bedding, towels, and makeup brushes can also help reduce environmental mite load, though the primary source of reinfestation is typically from close human contact rather than environmental reservoirs. Sun protection is also important, as UV exposure can sometimes worsen inflammatory skin conditions.
Ocular demodicosis requires specialized demodicosis treatment focusing on the eyelids. This often involves specific eyelid hygiene practices, such as daily cleansing with tea tree oil-based solutions or wipes. These products have demonstrated significant miticidal effects. In some cases, topical ophthalmic medications may be prescribed. For severe ocular cases, systemic oral medications might be considered. Long-term management of ocular demodicosis is often necessary to prevent chronic blepharitis and associated eye discomfort and vision problems. Patients with ocular symptoms should be managed by an ophthalmologist or a dermatologist experienced in ocular conditions.
Monitoring treatment effectiveness is a continuous process. Clinical improvement in symptoms and signs, such as reduced redness, papules, pustules, and itching, indicates successful demodicosis treatment. In some cases, repeat microscopic examination of skin scrapings or epilated eyelashes may be performed to confirm a reduction in mite density. Education on the chronic nature of demodicosis and the potential for recurrence is essential, empowering patients to recognize early signs and seek timely intervention, thus maintaining long-term control of their condition.
Common Treatment Approaches and Medications for demodicosis:
Topical Ivermectin Cream (1%): A highly effective, first-line topical treatment. It targets Demodex mites directly by interfering with their nervous system. Applied once daily, it significantly reduces mite density and inflammation, leading to substantial improvement in papulopustular and erythematous lesions. Generally well-tolerated.
Topical Metronidazole Cream or Gel (0.75-1%): An antimicrobial and anti-inflammatory agent commonly used in rosacea treatment, also effective in demodicosis. It helps reduce redness and papulopustules. Applied once or twice daily. Less potent against mites than ivermectin but useful for its anti-inflammatory properties.
Topical Permethrin Cream (5%): An insecticide traditionally used for scabies, it can also be effective against Demodex mites. Applied overnight, typically once or twice a week for several weeks. Can sometimes be irritating for facial use.
Topical Benzyl Benzoate Lotion/Emulsion (10-25%): An acaricide used to kill mites. Applied to affected areas, usually for several consecutive nights. Can be drying and irritating to the skin, so caution is advised for facial application.
Topical Crotamiton Cream/Lotion (10%): An antipruritic and scabicidal agent that also has some acaricidal properties against Demodex. Applied to alleviate itching and reduce mite populations.
Topical Sulfur Preparations (5-10%): Sulfur has mild antiseptic, antifungal, and acaricidal properties. Available in various forms (creams, washes, masks). Can be effective for mild cases but may have an unpleasant odor and be drying.
Oral Ivermectin: Reserved for more severe, widespread, or refractory cases. Administered orally, typically in a single dose, repeated after 7-14 days. Highly effective systemically against Demodex mites. Dosing is weight-dependent and requires medical supervision.
Oral Metronidazole: Used for its anti-inflammatory properties, particularly in papulopustular demodicosis resembling rosacea. Administered daily for several weeks. Often used when topical treatments are insufficient, though less directly miticidal than ivermectin.
Oral Tetracyclines (Doxycycline, Minocycline): These antibiotics have anti-inflammatory effects independent of their antimicrobial action, making them useful in reducing the redness and papulopustules of inflammatory demodicosis. Low-dose doxycycline is often favored to minimize side effects.
Tea Tree Oil (TTO) Eyelid Cleansers (5-50%): Specifically for ocular demodicosis. Available as wipes, foams, or solutions. TTO is a potent miticide. Used daily for eyelid hygiene to reduce mite load on eyelashes and eyelid margins. Concentrations above 5% should be used cautiously around the eyes and often diluted.
Gentle Skincare: Use of mild, non-comedogenic, and fragrance-free cleansers and moisturizers. Avoiding harsh scrubs or irritating products that can further compromise the skin barrier and exacerbate inflammation. This is supportive but crucial for skin health.
Sun Protection: Regular use of broad-spectrum sunscreen. UV radiation can worsen inflammation in some skin conditions, including those that mimic demodicosis, and can be a trigger for some forms of rosacea-like demodicosis.