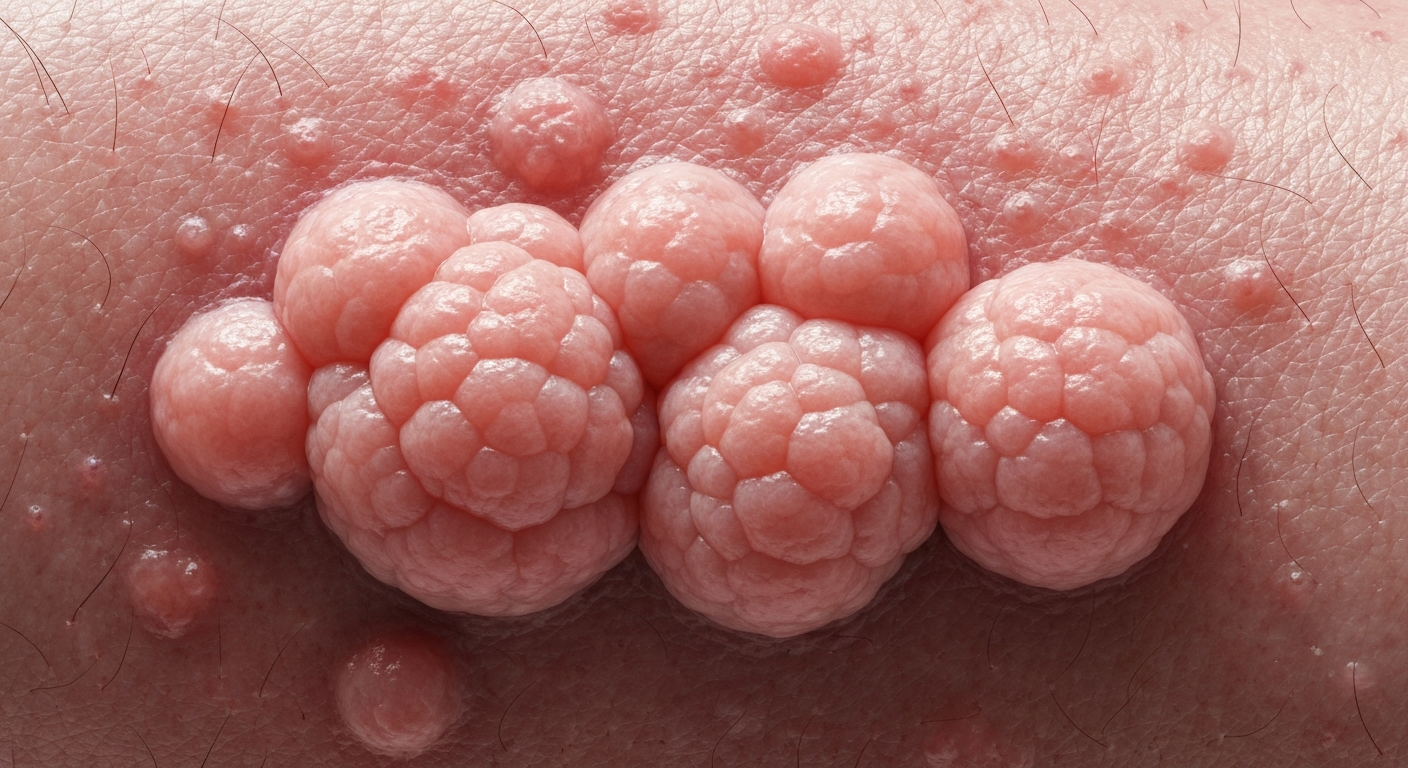
This article presents a comprehensive visual guide to HPV symptoms pictures, detailing the varied dermatological manifestations of human papillomavirus. Understanding these visual cues is crucial for early identification and appropriate medical consultation regarding HPV symptoms.
HPV Symptoms Pictures
Visualizing HPV symptoms pictures is paramount for recognizing the diverse presentations of human papillomavirus. The symptoms primarily manifest as warts, which can vary significantly in appearance, location, and severity. These lesions are caused by specific strains of HPV and can appear on various parts of the body, leading to distinct clinical classifications.
Genital Warts Pictures: These are arguably the most recognized HPV wart photos. They typically appear as small, flesh-colored bumps or groups of bumps in the anogenital area. Their texture can range from smooth and pearly to rough and cauliflower-like. Key characteristics often seen in genital warts pictures include:
- Location: In males, common sites include the penis, scrotum, groin, inner thighs, and around the anus. In females, they can appear on the vulva, in and around the vagina, on the cervix, and around the anus. Both sexes can develop them in the perineal area.
- Appearance:
- Condylomata acuminata: These are the classic cauliflower-like lesions, often soft and moist, ranging from a few millimeters to several centimeters in diameter. Their irregular surface is a key identifying feature in HPV symptoms pictures.
- Papular warts: Small, raised, dome-shaped lesions.
- Flat warts: Less common in the genital area but can appear as slightly raised, flesh-colored or brownish patches that are difficult to see without acetic acid application.
- Keratotic warts: Hard, thickened lesions, often more common on external genitalia.
- Color: Typically flesh-colored, but can be white, pink, or brownish.
- Size: Can be very small, almost undetectable, or coalesce into larger masses.
- Symptoms: Often asymptomatic, but can cause itching, discomfort, bleeding during intercourse, or obstruction in severe cases.
Common Warts (Verruca Vulgaris) Pictures: These are primarily found on the hands, fingers, and around nails, but can appear anywhere on the body. HPV symptoms pictures of common warts show:
- Appearance: Rough, grainy texture, often raised, with tiny black dots (thrombosed capillaries) visible when scraped.
- Shape: Round or irregular, firm to the touch.
- Color: Greyish, brownish, or flesh-colored.
- Size: Can vary from a pinhead to over a centimeter.
- Distribution: Can appear singly or in clusters.
Plantar Warts Pictures (Verruca Plantaris): These warts occur on the soles of the feet and are often confused with calluses. Distinctive features in HPV symptoms pictures of plantar warts include:
- Location: Soles of the feet, especially weight-bearing areas.
- Appearance: Grow inwards due to pressure, often flat or slightly raised, rough surface.
- Color: Flesh-colored, yellowish, or brownish, often surrounded by thickened skin.
- Key identifying feature: Presence of tiny black dots (petechiae from clotted blood vessels) visible after paring down the lesion, which differentiates them from calluses.
- Symptoms: Can be painful when walking or standing, especially if on a pressure point.
Flat Warts (Verruca Plana) Pictures: These are smoother and flatter than common warts and are often numerous. HPV symptoms pictures of flat warts typically display:
- Location: Commonly on the face, neck, hands, wrists, and shins.
- Appearance: Small, slightly raised, smooth-topped papules.
- Color: Flesh-colored, light brown, or pinkish.
- Size: Usually 1-5 mm in diameter.
- Distribution: Often appear in lines due to scratching (Koebner phenomenon).
Understanding these specific visual cues from human papillomavirus symptoms is essential for proper identification and subsequent medical guidance, emphasizing why clear HPV symptoms pictures are invaluable educational tools for patients and healthcare providers alike.
Signs of HPV Pictures
Delving deeper into signs of HPV pictures reveals further nuances in how human papillomavirus manifests visually. Beyond the general wart categories, specific locations and HPV strains can lead to distinct appearances, making detailed visual recognition crucial. These visual HPV symptoms can range from highly conspicuous lesions to more subtle changes requiring careful examination.
Anal Warts Pictures: Warts occurring in or around the anus deserve special attention. Anal warts pictures often show:
- Location: Perianal skin, within the anal canal, or both.
- Appearance: Similar to genital warts, they can be solitary or multiple, ranging from small, flesh-colored bumps to large, coalesced, cauliflower-like masses (condylomata acuminata). They may be external or internal.
- Texture: Can be soft, moist, or more firm and keratotic depending on location and chronicity.
- Symptoms: Often asymptomatic, but can cause itching, bleeding, discharge, pain during defecation, or a feeling of a lump or mass. Internal anal warts may be more difficult to detect without an anoscopy.
- Specific considerations: Anal warts are associated with higher-risk HPV types (e.g., HPV 16, 18) more frequently than external genital warts, increasing the risk of anal cancer, particularly in immunocompromised individuals.
Oral HPV Symptoms Pictures: HPV can also affect the oral cavity and throat, with varying appearances depending on the specific location and HPV type. Oral HPV symptoms pictures may include:
- Squamous papillomas: These are benign, solitary, exophytic (outward-growing) lesions with a warty, cauliflower-like, or finger-like surface. They are typically flesh-colored or white and are most commonly found on the tongue, lips, and soft palate.
- Verruca vulgaris (oral): Similar to common warts on the skin, these are rough-surfaced, raised lesions that can occur anywhere in the mouth, but particularly on the lips and gingiva.
- Focal epithelial hyperplasia (Heck’s disease): Caused by low-risk HPV types (e.g., HPV 13, 32), this presents as multiple, discrete, flattened papules or nodules with a cobblestone or pebbly appearance, usually on the labial, buccal, and lingual mucosa.
- Recurrent Respiratory Papillomatosis (RRP): While not strictly an “oral” symptom, it’s related to HPV in the aerodigestive tract. Laryngeal papillomas pictures show multiple wart-like growths in the larynx, often leading to hoarseness, difficulty breathing, or chronic cough. It is caused by HPV 6 and 11 and can be debilitating.
- High-risk oral HPV: While typically asymptomatic, persistent infection with high-risk HPV types (e.g., HPV 16) in the oropharynx is a leading cause of oropharyngeal cancer. Visible lesions are usually not present in the early, pre-cancerous stages.
Differential Diagnosis in Visual HPV Symptoms: It’s crucial to differentiate HPV signs images from other conditions that may mimic warts. This requires careful examination and sometimes biopsy. Conditions that can be confused with HPV include:
- Molluscum contagiosum: Small, flesh-colored, dome-shaped papules with a central umbilication.
- Skin tags (acrochordons): Small, soft, flesh-colored growths that are typically peduculated (stalk-like).
- Seborrheic keratoses: Benign, waxy, “stuck-on” appearing lesions, often brown or black.
- Lichen planus: Can cause purplish, itchy, flat-topped papules, sometimes with a lacy white pattern in the mouth (Wickham’s striae).
- Pearly penile papules: Small, dome-shaped or filiform papules arranged circumferentially around the corona of the glans penis, a normal anatomical variant.
- Vestibular papillomatosis: Small, pink, finger-like projections found on the vulvar vestibule in females, also considered a normal anatomical variant.
Careful evaluation of differentiating HPV lesions through high-quality signs of HPV pictures is vital for accurate diagnosis and management of the human papillomavirus.
Early HPV Photos
The challenge with identifying HPV often lies in its insidious onset. Early HPV photos reveal that initial lesions can be remarkably subtle, easily overlooked, or even entirely absent, making detection difficult. The incubation period for HPV can range from weeks to months, or even years, before any visible symptoms appear. This latency period means that by the time initial HPV lesions become noticeable, the infection may have been present for a significant duration.
Characteristics of Early Stage Genital Warts: When visible, early stage genital warts often begin as:
- Pinpoint Papules: Very small, barely perceptible bumps that are flesh-colored or slightly lighter/darker than surrounding skin. They may feel rougher to the touch than they appear.
- Slight Texture Changes: The skin may feel slightly bumpy or granular in an area where it was previously smooth. This can be especially true for early flat warts which are often more easily felt than seen.
- Subtle Discoloration: A faint pinkish, whitish, or brownish discoloration may be the only sign, often blending in with the surrounding skin tone.
- Single or Few Lesions: Initially, there may be only one or a very small cluster of these nascent warts, rather than the extensive cauliflower-like growths seen in later stages.
- Locations: Often found in areas of friction or moisture, such as the frenulum of the penis, labial folds, or perianal region.
Challenges in Spotting Early HPV Signs:
- Asymptomatic Nature: Many individuals with HPV, particularly those with high-risk types, never develop visible warts or any symptoms. This makes subtle HPV signs extremely difficult to detect without specific screening.
- Microscopic Lesions: Some early lesions are microscopic and only become visible under magnification (e.g., colposcopy for cervical lesions) or after the application of acetic acid, which turns HPV-infected tissue white (acetowhite changes). However, acetowhite changes are not specific to HPV and can be seen in other conditions, necessitating expert interpretation.
- Mimicking Normal Anatomy: Very small warts can be mistaken for normal skin variations, hair follicles, or benign skin tags.
- Internal Lesions: Warts on the cervix, inside the vagina, or in the anal canal are not externally visible and require speculum examination or anoscopy. Early HPV photos of cervical lesions might show only minor surface irregularities or acetowhite changes during a colposcopic examination, which are crucial in screening for pre-cancerous changes.
Progression from Latent HPV to Visible Warts:
- The HPV virus can remain in a latent HPV state for extended periods, integrated into the host cell DNA without causing any visible changes.
- Factors like weakened immune function, stress, or other infections can trigger the virus to become active, leading to cell proliferation and the formation of visible warts.
- Even once active, the initial growth of warts can be slow, with nascent warts gradually increasing in size and number over weeks or months.
Due to the elusive nature of early HPV photos and the often asymptomatic course, regular screenings (such as Pap tests for cervical HPV) and heightened awareness of subtle skin changes are critical for early detection and management of human papillomavirus.
Skin rash HPV Images
While HPV is most commonly associated with distinct wart formations, certain manifestations can present more diffusely, resembling a skin rash HPV images show. This is particularly true for extensive flat warts or confluent lesions that cover a larger area, or in conditions where the virus causes widespread epidermal changes rather than isolated papules. Differentiating these HPV-related rashes from other dermatological conditions is essential for accurate diagnosis.
Flat Warts Resembling a Rash:
- Widespread Distribution: Flat warts (verruca plana) can be numerous and spread across an area, appearing as a cluster of small, slightly raised, smooth-topped papules. On areas like the face, neck, or shins, these collections can give the impression of a patchy or diffuse rash.
- Coloration: These lesions are often flesh-colored, light brown, or pinkish, which can blend into the skin, making them easily mistaken for other types of irritations or minor rashes.
- Koebner Phenomenon: A characteristic feature of flat warts is their tendency to appear in lines or clusters following scratching or minor trauma. This linear arrangement can make the lesion pattern resemble a dermatographic rash or an allergic contact dermatitis.
- Differential from inflammatory rashes: Unlike inflammatory rashes, flat warts typically do not itch intensely, are not usually red, and do not present with vesicles or crusting unless secondarily infected.
Confluent HPV Lesions:
- In some cases, especially in immunocompromised individuals, individual warts can grow very large or merge together, forming large plaques or sheets of papillomatous tissue. Extensive HPV lesions like these can cover significant surface areas, such as the entire anogenital region, resembling a broad, verrucous rash.
- Giant Condyloma (Buschke-Löwenstein tumor): This is a rare but aggressive form of genital wart that grows into a massive, cauliflower-like tumor, invading local tissues. Its large size and spreading nature can appear as an overwhelming, destructive “rash” that obliterates normal skin architecture.
HPV-Related Skin Changes and Differential Diagnosis: When evaluating HPV-related skin changes that look like a rash, several conditions must be considered for accurate differential diagnosis:
- Fungal Infections (Tinea): Ringworm can cause red, scaly, itchy patches with raised borders, which can sometimes be confused with the perimeter of a spreading wart cluster.
- Psoriasis: This chronic autoimmune condition causes red, scaly plaques, often with silvery scales, commonly found on elbows, knees, and scalp. Psoriasis can sometimes appear in intertriginous areas and be mistaken for widespread flat warts.
- Lichen Planus: Characterized by purplish, polygonal, pruritic papules that can coalesce into plaques. Oral lichen planus, in particular, can have a white lacy pattern that might be confused with oral HPV lesions.
- Contact Dermatitis: An allergic reaction or irritation can cause red, itchy, sometimes blistering rashes that can appear anywhere on the skin. The distribution pattern might sometimes overlap with areas where flat warts commonly appear.
- Molluscum Contagiosum: Although typically discrete papules with central umbilication, extensive molluscum lesions in certain areas can be misidentified in a rapid visual assessment as a viral rash.
- Seborrheic Dermatitis: Causes red, greasy, scaly patches, particularly on the scalp, face, and chest, which typically do not resemble warts but can be part of a broader “rash” differential.
The ability to distinguish between these conditions through careful examination of flat wart photos and other skin rash HPV images is critical for ensuring that patients receive the correct diagnosis and appropriate treatment for their specific dermatological condition, whether it is HPV or another skin ailment.
HPV Treatment
HPV treatment primarily focuses on managing the visible symptoms, such as warts, rather than directly eradicating the virus itself. The immune system often clears the HPV infection over time, but treatments are available to remove bothersome or high-risk lesions. The choice of wart removal options depends on the type, size, location, and number of warts, as well as patient preference and immune status. A key aspect of HPV management is addressing both current lesions and reducing the risk of transmission or progression to cancer for high-risk types.
Medical Treatments (Topical Applications): These are often the first-line therapies for external warts.
- Podofilox (Condylox):
- Mechanism: An antimitotic agent that destroys wart tissue.
- Application: Applied by the patient twice daily for three days, followed by four days of no treatment, for up to four cycles.
- Efficacy: Effective for small to medium-sized external genital warts.
- Side Effects: Local irritation, burning, pain, inflammation.
- Imiquimod (Aldara, Zyclara):
- Mechanism: An immune response modifier that stimulates the body’s immune system to fight the HPV virus.
- Application: Applied by the patient, typically 3 times per week at bedtime for Aldara, or daily for Zyclara, for up to 16 weeks.
- Efficacy: Effective for external genital and perianal warts.
- Side Effects: Local skin reactions (redness, itching, burning, erosion), flu-like symptoms.
- Sinecatechins (Veregen):
- Mechanism: A green tea extract with antioxidant and antiviral properties.
- Application: Applied by the patient three times daily for up to 16 weeks.
- Efficacy: Effective for external genital and perianal warts.
- Side Effects: Local skin reactions (erythema, itching, burning), pain.
- Trichloroacetic Acid (TCA) / Bichloroacetic Acid (BCA):
- Mechanism: Caustic agents that chemically destroy wart tissue.
- Application: Applied by a healthcare provider weekly until warts resolve.
- Efficacy: Effective for small, moist genital warts, often used for flat warts.
- Side Effects: Local irritation, pain, ulceration, scarring. Requires careful application to avoid damage to surrounding healthy tissue.
- Salicylic Acid:
- Mechanism: Keratolytic agent that gradually dissolves wart tissue.
- Application: Applied by the patient daily for common and plantar warts.
- Efficacy: Over-the-counter option for common and plantar warts.
- Side Effects: Local irritation, skin discoloration.
Surgical and Destructive Treatments: These methods are performed by healthcare professionals for larger, more persistent, or internal warts, or when topical treatments fail.
- Cryotherapy:
- Mechanism: Freezing warts with liquid nitrogen, causing cellular destruction.
- Procedure: Applied by a healthcare provider every 1-3 weeks.
- Efficacy: Widely used for various types of warts, including genital, common, and plantar warts.
- Side Effects: Pain, blistering, temporary discoloration, scarring (rare).
- Electrocautery and Surgical Excision:
- Mechanism: Burning warts with an electric current (electrocautery) or physically cutting them out with a scalpel (excision).
- Procedure: Performed under local anesthesia.
- Efficacy: Effective for single, larger, or persistent warts.
- Side Effects: Pain, scarring, risk of infection, recurrence if not completely removed.
- Laser Treatment (CO2 Laser):
- Mechanism: Using a focused beam of light to vaporize wart tissue.
- Procedure: Performed under local or general anesthesia for extensive or hard-to-reach warts.
- Efficacy: Effective for large, widespread, or recurrent warts, including those in difficult anatomical locations (e.g., anal canal, urethra).
- Side Effects: Pain, scarring, delayed healing, potential for plume inhalation if not properly managed.
- Curettage:
- Mechanism: Scraping the wart off with a curette, often followed by electrocautery or cryotherapy.
- Procedure: Performed under local anesthesia.
- Efficacy: Commonly used for common and plantar warts.
- Side Effects: Pain, bleeding, scarring.
HPV Vaccine and Prevention:
- Gardasil 9: Protects against nine types of HPV, including low-risk types (6 and 11) that cause about 90% of genital warts, and high-risk types (16, 18, 31, 33, 45, 52, 58) that cause about 90% of cervical cancers and a majority of other HPV-related cancers.
- Recommendation: Recommended for both males and females, ideally before exposure to HPV (i.e., before sexual activity), typically starting at age 11 or 12.
- Other prevention methods: Consistent and correct condom use can reduce the risk of HPV transmission but does not provide complete protection as HPV can infect areas not covered by a condom. Regular screening (Pap tests, HPV tests) is crucial for early detection of cervical changes caused by high-risk HPV types.
Successful genital wart treatment and overall HPV management involve a personalized approach, often combining different therapies and emphasizing preventative measures like vaccination and safe sex practices to reduce the burden of human papillomavirus.