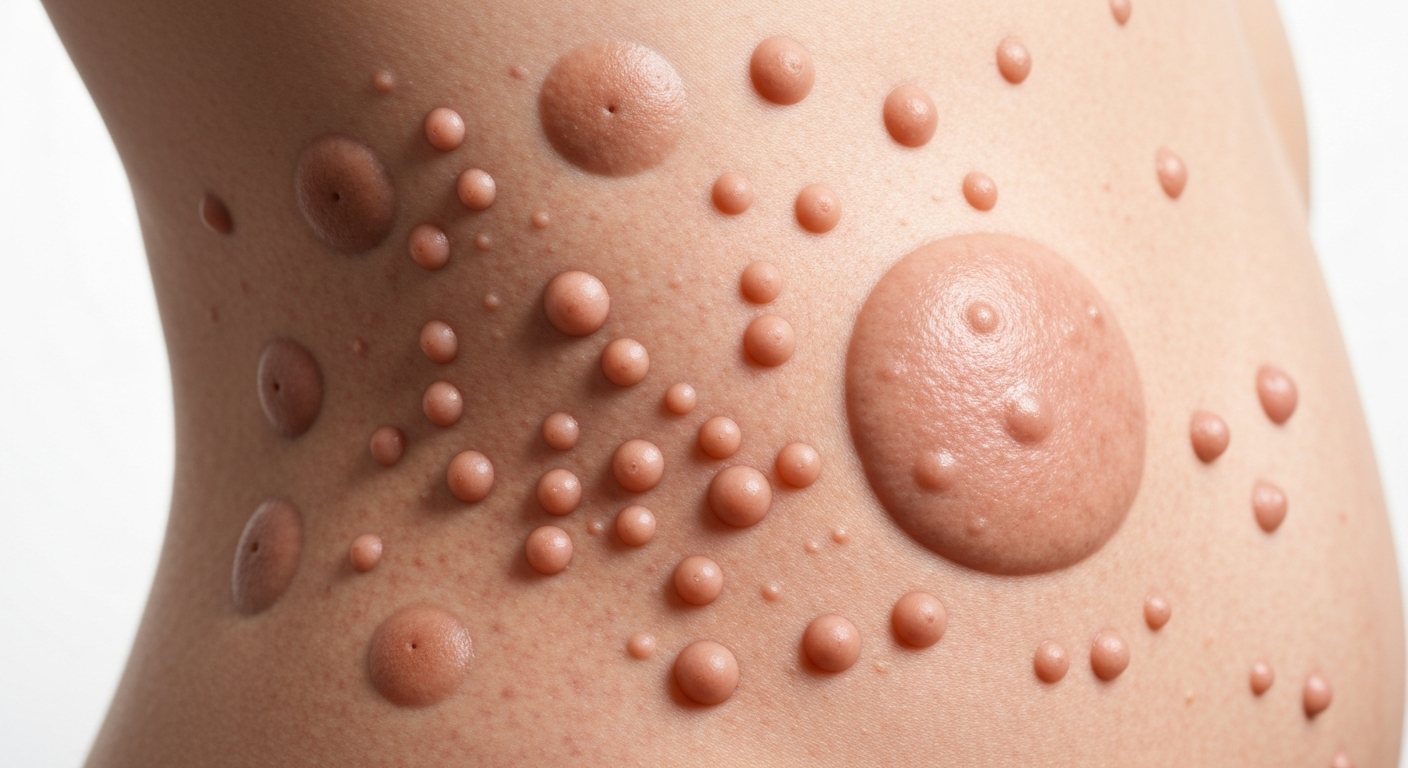
Exploring Neurofibromatosis symptoms pictures provides a critical visual aid for understanding the diverse manifestations of this genetic disorder. These images are invaluable for medical professionals and individuals seeking to identify or comprehend the characteristic skin and physical markers associated with neurofibromatosis, offering a direct look at the progression and presentation of various signs.
Neurofibromatosis Symptoms Pictures
The visual landscape of Neurofibromatosis symptoms pictures is dominated by specific dermatological features that are often the earliest and most recognizable indicators of the condition. These manifestations are not merely cosmetic; they are diagnostic hallmarks that guide clinicians in identifying the disorder. Understanding the appearance and evolution of these symptoms is crucial for an accurate diagnosis and subsequent management of Neurofibromatosis.
One of the most defining Neurofibromatosis symptoms visible in pictures are café-au-lait spots. These are flat, uniformly hyperpigmented macules or patches, ranging in color from light brown to dark brown, resembling the color of coffee with milk. Their borders are typically smooth and regular, though irregular margins can occur. To meet diagnostic criteria for Neurofibromatosis type 1 (NF1), an individual usually presents with six or more such spots, exceeding 5 mm in greatest diameter in prepubertal individuals or 15 mm in postpubertal individuals. These spots are usually present at birth or develop within the first few years of life, increasing in number and size over time. They can appear anywhere on the body but are commonly found on the trunk, buttocks, and extremities, often sparing the face. The presence and distribution of these café-au-lait spots are critical visual clues in Neurofibromatosis diagnosis pictures.
Another prominent feature in Neurofibromatosis symptoms pictures is the development of various types of neurofibromas. These benign tumors arise from the nerve sheath and can manifest in several forms:
- Cutaneous Neurofibromas: These are soft, flesh-colored, pinkish, or brownish bumps that appear on or just beneath the skin’s surface. They can be sessile (broad-based) or pedunculated (stem-like), varying in size from a few millimeters to several centimeters. Their texture can be rubbery or soft, and they may dimple inward when pressed (the “buttonhole sign”). These usually emerge during adolescence and tend to increase in number and size with age. They are often numerous, scattered across the body, and are a key characteristic in Neurofibromatosis images.
- Subcutaneous Neurofibromas: Located deeper under the skin, these feel like firm, mobile nodules. They can be tender or painful when pressed and may appear as subtle elevations on the skin surface. Visualizing these in Neurofibromatosis symptoms pictures might require close inspection or palpation, which photographs can sometimes simulate through shadowing or subtle contour changes.
- Plexiform Neurofibromas: These are more diffuse, often large, and can involve multiple nerve bundles. They grow along nerves and can spread into surrounding tissues, leading to significant disfigurement, functional impairment, or pain. Their appearance in Neurofibromatosis pictures can be striking, presenting as thickened, elongated, or irregularly shaped areas of skin and underlying tissue, often with overlying hyperpigmentation. They can affect any part of the body, including the face, limbs, or trunk, and carry a small risk of malignant transformation. These are particularly important features in advanced Neurofibromatosis photos due to their potential for substantial morbidity.
Axillary and inguinal freckling (Crowe’s sign) is another specific diagnostic criterion and a common finding in Neurofibromatosis symptoms pictures. These are clusters of small, freckle-like spots that appear in the armpits (axilla) and groin (inguinal region), sometimes extending to the submammary folds or neck. Unlike typical sun-induced freckles, these occur in areas not usually exposed to the sun and are much smaller and more numerous than individual café-au-lait spots. Their presence in these specific anatomical locations is highly indicative of NF1 and is a distinct feature captured in Neurofibromatosis photos of affected individuals, especially children.
In summary, the detailed examination of Neurofibromatosis symptoms pictures provides compelling visual evidence of the condition, focusing on the distinct patterns of skin pigmentation, tumor formation, and characteristic freckling that define its presentation. These visual markers are critical for diagnosis and monitoring the progression of Neurofibromatosis.
Key Neurofibromatosis skin manifestations for visual identification include:
- Café-au-lait macules: Flat, light to dark brown spots with well-defined borders.
- Cutaneous neurofibromas: Soft, skin-colored to pinkish bumps, sessile or pedunculated, varying in size.
- Subcutaneous neurofibromas: Firm, palpable nodules beneath the skin surface.
- Plexiform neurofibromas: Diffuse, large, irregular swellings involving skin and deeper tissues, often disfiguring.
- Axillary and inguinal freckling: Small, clustered freckles in skin folds.
- Dysplastic neurofibromas: A less common variant, appearing as firm, deep nodules.
- Mongolian spots: While distinct, sometimes confused, but Neurofibromatosis pictures help differentiate.
- Halo neurofibromas: Neurofibromas surrounded by an area of depigmentation, less common but noteworthy.
Signs of Neurofibromatosis Pictures
Beyond the primary skin lesions, various other signs of Neurofibromatosis can be visually evident or have indirect visual consequences that might be captured in photographs, providing a broader understanding of the systemic nature of the disorder. These signs often point to the involvement of other organ systems, underscoring the complexity of Neurofibromatosis.
One notable ocular sign, while not typically visible in external skin photos, can sometimes have indirect visual implications: Lisch nodules. These are benign hamartomas of the iris, appearing as tan-to-brown dome-shaped elevations. They are usually bilateral and multiple, increasing in number with age. While an ophthalmologist requires a slit-lamp examination to confirm their presence, their diagnostic value in Neurofibromatosis type 1 is significant. Although a direct picture of Lisch nodules isn’t usually an external symptom, their documentation is crucial in the comprehensive assessment of Neurofibromatosis signs.
Skeletal abnormalities are another group of Neurofibromatosis signs that can be striking in pictures. These include:
- Scoliosis: Curvature of the spine, which can range from mild to severe, leading to visible postural changes, uneven shoulders, or a prominent rib cage. Severe scoliosis can be very apparent in Neurofibromatosis images of an individual’s back.
- Tibial bowing and pseudoarthrosis: A characteristic bending or bowing of the long bones, most commonly the tibia (shin bone). In some cases, this can progress to a non-union fracture, known as pseudoarthrosis, which results in a visibly distorted and weakened limb. Neurofibromatosis pictures can clearly show the angulation and deformity of the affected bone.
- Sphenoid wing dysplasia: A malformation of the sphenoid bone in the skull, often leading to pulsatile exophthalmos (protrusion of the eyeball with visible pulsation) if associated with an underlying plexiform neurofibroma or orbital defect. This can be visually prominent in specific Neurofibromatosis patient photos, altering facial symmetry.
- Macrocephaly: An abnormally large head circumference, which can be a subtle but consistent finding in some individuals with NF1. This is a proportional increase in head size and can be observed in Neurofibromatosis images comparing head size to body proportions.
Neurological manifestations, while often internal, can sometimes lead to visible effects. Optic pathway gliomas, tumors affecting the optic nerves, can cause vision problems and, in severe cases, might lead to proptosis (bulging of the eye) or strabismus (misalignment of the eyes), which could be evident in detailed facial Neurofibromatosis pictures. The development of other brain tumors or peripheral nerve tumors, though not directly visible on the skin, contributes to the neurological burden of Neurofibromatosis.
Vascular abnormalities, such as renal artery stenosis, can lead to hypertension, which is not visually apparent but is an important clinical sign. However, other less common vascular lesions, such as arteriovenous malformations, if superficial, could theoretically present with skin changes like warmth or engorgement, though this is rare in Neurofibromatosis skin pictures.
Endocrine issues, such as short stature or precocious puberty, can also occur. While specific endocrine disorders aren’t “pictured” as symptoms, their impact on an individual’s physical development might be observed over time in a series of Neurofibromatosis photos illustrating growth patterns.
Many of these systemic Neurofibromatosis signs are crucial for the overall clinical picture, even if they aren’t always immediately obvious in a casual photograph. Their comprehensive assessment, often guided by imaging techniques like MRI or X-rays, complements the visual diagnosis derived from Neurofibromatosis symptoms pictures, painting a complete portrait of the disease’s impact.
Detailed list of systemic Neurofibromatosis signs and their potential visual implications:
- Ocular findings:
- Lisch nodules (iris hamartomas – internal, but diagnostic).
- Optic pathway gliomas (can lead to proptosis, strabismus – visible in severe cases).
- Glaucoma (less common, but can cause ocular changes).
- Skeletal abnormalities:
- Scoliosis (visible spinal curvature, uneven shoulders/hips).
- Pseudoarthrosis (bowing and non-union of long bones, often tibia).
- Sphenoid wing dysplasia (orbital asymmetry, pulsatile exophthalmos).
- Short stature (general body proportion in comparative photos).
- Macrocephaly (visibly large head circumference).
- Bone cysts and thinning of cortical bone.
- Neurological complications:
- Brain tumors (e.g., optic gliomas, other CNS tumors – indirect visual impact from growth).
- Seizures (no direct visual symptom, but impact on life).
- Hydrocephalus (can contribute to macrocephaly or other cranial changes).
- Learning disabilities (no direct visual manifestation).
- Vascular manifestations:
- Renal artery stenosis (hypertension – not visible).
- Vasculopathy (aneurysms, stenoses – rarely visible externally unless large and superficial).
- Endocrine abnormalities:
- Precocious puberty (visible early secondary sexual characteristics).
- Growth hormone deficiency (impact on stature).
- Malignancies:
- Malignant peripheral nerve sheath tumors (MPNSTs) arising from plexiform neurofibromas (rapid growth, pain – visually concerning changes in a pre-existing lesion).
- Other associated cancers (e.g., pheochromocytoma, leukemia – no direct visual skin signs).
Early Neurofibromatosis Photos
The journey of diagnosing Neurofibromatosis often begins with the recognition of its characteristic features in early Neurofibromatosis photos, particularly those taken during infancy and early childhood. These initial visual cues are paramount for timely diagnosis, intervention, and management. Early identification through Neurofibromatosis pictures allows for proactive monitoring of potential complications and can significantly improve long-term outcomes.
The most common and often the first visible sign of NF1 in early Neurofibromatosis photos are café-au-lait spots. These hyperpigmented macules can be present at birth, or they may appear and increase in number and size during the first few years of life. A child with three or more such spots should prompt suspicion for NF1, with six or more spots fulfilling a major diagnostic criterion. In infant photos, these spots might be subtle, but they become more distinct as the child grows. Parents often notice these spots and may seek medical advice, making these initial Neurofibromatosis images critical for early medical consultation. The color can vary, and they are typically uniform in tone, with smooth borders. Their distribution is often widespread across the trunk and limbs.
Another key indicator in early Neurofibromatosis photos that emerges later in childhood is axillary and inguinal freckling. While café-au-lait spots are often present from birth or soon after, freckling in the armpits and groin typically develops between the ages of three and five years. These small, concentrated clusters of freckles, unlike sun-induced freckles, appear in non-sun-exposed areas. Their characteristic location makes them a highly specific diagnostic sign in early Neurofibromatosis images and a strong indicator for NF1. This sign, often referred to as Crowe’s sign, helps differentiate NF1 from other conditions that might present with café-au-lait spots alone.
The appearance of cutaneous neurofibromas is typically not seen in true early Neurofibromatosis photos of infants or very young children. These benign skin tumors usually begin to manifest during adolescence or early adulthood, although occasionally a few may appear in prepubertal children. However, the early identification of café-au-lait spots and freckling triggers a vigilance for the later development of these neurofibromas. When they do appear, even in younger individuals, they solidify the visual diagnosis of Neurofibromatosis.
Plexiform neurofibromas, though less common than cutaneous neurofibromas, can sometimes be present at birth or develop in early childhood. These larger, diffuse tumors can be quite striking in early Neurofibromatosis photos, causing significant disfigurement, particularly if they affect the face or limbs. They might appear as a soft, thickened area of skin with hyperpigmentation or a palpable mass. Early recognition of plexiform neurofibromas is crucial because of their potential for significant growth, functional impairment, and a small risk of malignant transformation. Images showing these early large lesions are very informative for clinical management.
Other non-dermatological signs that might be inferred or observed in early Neurofibromatosis photos include subtle skeletal abnormalities like mild scoliosis, which can progress over time. Macrocephaly, an enlarged head circumference, can also be noted in comparative childhood photos. While Lisch nodules are internal, their development in early childhood also contributes to the early diagnostic picture, albeit requiring ophthalmological examination rather than simple visual inspection of skin pictures.
The cumulative effect of these visible signs in early Neurofibromatosis photos helps piece together the diagnostic puzzle, allowing for timely medical follow-up, genetic counseling, and symptom management. It emphasizes the importance of regular pediatric check-ups and heightened awareness among parents and clinicians regarding these distinctive early manifestations of Neurofibromatosis.
Key early Neurofibromatosis manifestations for photographic identification:
- Café-au-lait spots: Present at birth or appearing within the first few years, increasing in number and size.
- Axillary freckling: Small, clustered freckles in the armpits, typically appearing between 3-5 years of age.
- Inguinal freckling: Similar freckles in the groin region, also appearing in early childhood.
- Plexiform neurofibromas: Occasionally present at birth or developing in early childhood as diffuse, sometimes large, soft tissue masses.
- Macrocephaly: Visibly enlarged head circumference compared to age and peers.
- Skeletal bowing: Such as tibial bowing, which can be noted as a visible deformity of the limb.
- Subtle facial asymmetry: Potentially indicating underlying plexiform neurofibromas or skeletal dysplasia.
- Developmental delays: While not a visual symptom, often associated with early presentation.
- Early growth patterns: Short stature or accelerated growth could be observed over a series of photos.
Skin rash Neurofibromatosis Images
Distinguishing specific Neurofibromatosis skin manifestations from general skin rashes or other dermatological conditions is a critical aspect of diagnosis, and a careful review of skin rash Neurofibromatosis images highlights these unique features. While the term “rash” often implies an inflammatory, widespread, and transient skin eruption, the characteristic lesions of Neurofibromatosis are typically chronic, distinct, and develop over time, usually lacking the acute inflammatory nature of a true rash.
The primary dermatological feature in skin rash Neurofibromatosis images is the cutaneous neurofibroma. Unlike a typical rash, these are discrete, benign tumors arising from nerve sheaths. They appear as soft, often pedunculated (stem-like) or sessile (broad-based) nodules on the skin surface. Their color can vary from skin-toned to pinkish, reddish-brown, or hyperpigmented. They feel soft and compressible, sometimes invaginating into the skin when pressed (the “buttonhole sign”). A true rash, conversely, is typically flat or mildly elevated, often red, itchy, and symmetrical, and resolves with treatment or time. Neurofibromas, however, persist, gradually increasing in size and number, often becoming very numerous, particularly during and after puberty.
Another key feature in Neurofibromatosis skin images is the plexiform neurofibroma. These are often larger, more diffuse, and deeply situated lesions that involve multiple nerves and surrounding tissues. They present as thickened, overgrown areas of skin, often with a doughy or rubbery consistency and sometimes overlying hyperpigmentation. Their irregular shape and variable size, potentially causing significant disfigurement, differentiate them sharply from any common skin rash. A plexiform neurofibroma is a palpable mass, not a superficial eruption. Pictures showcasing these large, often asymmetrical lesions underscore their unique nature.
Café-au-lait spots, while pigmentary lesions rather than rashes, are fundamental in Neurofibromatosis skin pictures. These are flat, uniformly colored macules with smooth borders, clearly distinct from the patchy, often itchy, or scaly appearance of many rashes. Rashes are often inflammatory, whereas café-au-lait spots are stable pigment alterations. The presence of six or more of these spots is highly diagnostic for NF1, making them crucial elements in a series of Neurofibromatosis skin images.
Similarly, axillary and inguinal freckling (Crowe’s sign) are distinctive. These are clusters of small, punctate hyperpigmented macules in the folds of the armpits and groin. These are not a diffuse rash but rather concentrated, small freckles in specific, non-sun-exposed areas. A general freckling rash would be sun-induced and widespread, lacking the specific anatomical localization of NF1 freckling. The precision of their location in Neurofibromatosis images is key to their diagnostic value.
Differentiation from common skin rashes is essential:
- Eczema/Dermatitis: Typically red, itchy, scaly, sometimes weeping patches; highly inflammatory. Neurofibromas are benign tumors, not inflammatory patches.
- Hives (Urticaria): Transient, raised, itchy welts that appear and disappear rapidly. Neurofibromas are persistent and stable lesions.
- Acne: Follicular papules, pustules, cysts; centered around sebaceous glands. Neurofibromas are nerve sheath tumors, not related to follicles.
- Molluscum Contagiosum: Small, flesh-colored, dome-shaped papules with a central umbilication, caused by a virus. While similar in shape to some small neurofibromas, their consistency and viral origin are distinct.
- Warts (Verrucae): Rough, keratinous growths caused by HPV. Neurofibromas are soft, usually smooth-surfaced, and non-viral.
- Nevus (Mole): Pigmented lesions, usually stable. While some atypical moles can resemble neurofibromas in certain contexts, neurofibromas are distinct in their histology and tendency to grow and multiply.
- Other vascular lesions: Hemangiomas are red or purplish vascular growths; neurofibromas are generally skin-colored or brownish and non-vascular.
The unique morphology, distribution, and non-inflammatory nature of Neurofibromatosis skin lesions are clearly evident when examining skin rash Neurofibromatosis images. They represent a distinct category of skin findings that are central to the diagnosis of this complex genetic disorder, setting them apart from the transient and often irritating presentations of common rashes.
Detailed list of Neurofibromatosis skin features compared to common rashes:
- Neurofibromas (Cutaneous/Subcutaneous/Plexiform):
- Appearance: Discrete, soft to firm, skin-colored to brownish nodules/masses, pedunculated or sessile. Plexiform can be diffuse and disfiguring.
- Feel: Rubbery, soft, doughy, compressible (buttonhole sign).
- Onset/Progression: Develop over years, increasing in number and size, generally stable or slow growing.
- Associated symptoms: Rarely itchy or painful unless traumatized or very large.
- Location: Widespread, any body surface.
- Nature: Benign tumors of nerve sheath origin.
- Café-au-lait spots:
- Appearance: Flat, uniformly light to dark brown macules with smooth borders.
- Feel: Smooth, non-palpable.
- Onset/Progression: Present at birth or early childhood, stable in color, may increase in number/size.
- Associated symptoms: Asymptomatic.
- Location: Widespread, often trunk/limbs.
- Nature: Pigmentary lesions.
- Axillary/Inguinal Freckling:
- Appearance: Small, clustered freckle-like spots.
- Feel: Flat, non-palpable.
- Onset/Progression: Develop in early childhood, persistent.
- Associated symptoms: Asymptomatic.
- Location: Axilla, groin, submammary folds.
- Nature: Specific pigmentary changes.
- Common Rashes (e.g., Eczema, Contact Dermatitis):
- Appearance: Red, inflamed, scaly, crusty, blistering patches or papules.
- Feel: Often rough, raised, sometimes weeping.
- Onset/Progression: Acute or chronic flares, often cyclical, can resolve with treatment.
- Associated symptoms: Intense itching, burning, pain.
- Location: Variable, often symmetrical, can be widespread or localized based on trigger.
- Nature: Inflammatory response to internal or external factors.
Neurofibromatosis Treatment
While Neurofibromatosis symptoms pictures vividly illustrate the manifestations of the disorder, effective Neurofibromatosis treatment goes far beyond visual identification. The management of Neurofibromatosis, particularly NF1, is complex and multidisciplinary, aiming to address the diverse symptoms and complications that can arise. There is no single cure for Neurofibromatosis, but treatments focus on managing symptoms, preventing or mitigating complications, and improving the quality of life for affected individuals. Understanding the available therapeutic options is crucial for anyone involved in the care of a person with Neurofibromatosis.
Medical Management:
Recent advances have introduced targeted therapies for specific Neurofibromatosis manifestations. One significant breakthrough is the approval of MEK inhibitors, such as selumetinib, for the treatment of inoperable plexiform neurofibromas in children. These medications work by targeting a specific signaling pathway (MAPK pathway) that is hyperactive in Neurofibromatosis, leading to tumor growth. In Neurofibromatosis treatment, MEK inhibitors can:
- Reduce the size of plexiform neurofibromas.
- Improve associated symptoms like pain, disfigurement, airway compression, and motor dysfunction.
- Potentially prevent further growth of these problematic tumors.
Other medical treatments might include symptomatic management of pain (e.g., neuropathic pain from neurofibromas), itching, or associated conditions like hypertension. Regular monitoring by specialists (ophthalmologists, neurologists, orthopedists, endocrinologists) is a cornerstone of medical management to detect and address complications early.
Surgical Interventions:
Surgery plays a significant role in Neurofibromatosis treatment, primarily for the removal of problematic neurofibromas or the correction of skeletal deformities. Surgical indications for neurofibromas include:
- Pain or discomfort: Removing neurofibromas that are causing chronic pain or irritation.
- Disfigurement: Excising large or cosmetically bothersome cutaneous or plexiform neurofibromas, especially those affecting the face or other visible areas. Plastic surgery techniques are often employed to minimize scarring.
- Functional impairment: Removing tumors that impinge on nerves, blood vessels, or organs, causing loss of function (e.g., tumors pressing on the spinal cord, bladder, or airways).
- Suspicion of malignancy: Biopsy and surgical removal of neurofibromas that show rapid growth, increased pain, or other concerning changes, as a small percentage of plexiform neurofibromas can transform into malignant peripheral nerve sheath tumors (MPNSTs).
Skeletal complications also frequently require surgical intervention. For example, severe scoliosis may necessitate spinal fusion surgery to correct the curvature and prevent further progression. Pseudoarthrosis of the tibia often requires complex orthopedic surgeries, including bone grafting and internal fixation, to attempt to achieve bone union.
Radiotherapy:
Radiation therapy is generally avoided in Neurofibromatosis treatment due to the increased risk of secondary tumor development in irradiated fields, especially in individuals with NF1. However, in very specific cases, such as inoperable malignant peripheral nerve sheath tumors or certain types of brain tumors, it might be considered as part of a comprehensive treatment plan, always weighing the risks and benefits carefully.
Supportive Care and Monitoring:
Ongoing supportive care and regular surveillance are critical components of Neurofibromatosis treatment. This includes:
- Annual physical examinations: To monitor for new lesions, changes in existing symptoms, and overall health.
- Ophthalmological examinations: Regular eye exams to detect Lisch nodules (for diagnosis) and screen for optic pathway gliomas or glaucoma.
- Neurological evaluations: To monitor for brain tumors, seizures, or other neurological complications.
- Skeletal assessments: Screening for scoliosis, pseudoarthrosis, and other bone abnormalities.
- Developmental and educational support: Addressing learning disabilities, ADHD, and other neurodevelopmental challenges often associated with NF1.
- Psychological and social support: Providing counseling and support for individuals dealing with the physical appearance of neurofibromas, chronic pain, and the general impact of a lifelong condition. Patient support groups are invaluable resources.
- Genetic counseling: For affected individuals and families to understand inheritance patterns and reproductive risks.
The personalized approach to Neurofibromatosis treatment, adapting to the individual’s specific symptoms and complications, ensures the best possible outcomes. Continuous research into the genetic and molecular mechanisms of Neurofibromatosis holds promise for even more targeted and effective therapies in the future.
Comprehensive list of Neurofibromatosis treatment modalities:
- Pharmacological Treatments:
- MEK inhibitors (e.g., Selumetinib) for inoperable plexiform neurofibromas.
- Pain management medications (e.g., neuropathic agents for nerve pain).
- Antihypertensive drugs for associated hypertension.
- Medications for other endocrine abnormalities (e.g., precocious puberty).
- Antiepileptic drugs for seizure management.
- Surgical Interventions:
- Excision of symptomatic cutaneous neurofibromas (for pain, irritation, cosmesis).
- Debulking or complete resection of plexiform neurofibromas (for disfigurement, functional impairment, malignancy risk).
- Spinal surgery (e.g., fusion) for scoliosis.
- Orthopedic surgeries for pseudoarthrosis and other bone deformities.
- Tumor removal from internal organs (e.g., optic pathway gliomas if symptomatic and growing).
- Surgical correction of sphenoid wing dysplasia causing orbital abnormalities.
- Radiotherapy:
- Reserved for specific cases, such as malignant peripheral nerve sheath tumors (MPNSTs) or certain brain tumors, due to concerns about secondary malignancy in NF1.
- Monitoring and Surveillance:
- Annual physical examinations by a specialist (e.g., neurologist, clinical geneticist).
- Regular ophthalmological evaluations (slit-lamp exam, vision testing).
- Neurological assessments, including MRI brain/spine as indicated.
- Orthopedic evaluations for scoliosis and bone lesions.
- Developmental assessments for learning disabilities and ADHD.
- Cardiovascular monitoring for hypertension and vasculopathy.
- Audiological screening for NF2-related hearing loss.
- Supportive Care:
- Psychological counseling and support for body image issues and chronic disease management.
- Educational support services for learning difficulties.
- Physical therapy and occupational therapy for functional limitations.
- Genetic counseling for family planning and understanding inheritance.
- Participation in patient support groups and advocacy organizations.
- Nutritional counseling to promote general health.
- Pain management clinics for chronic pain.