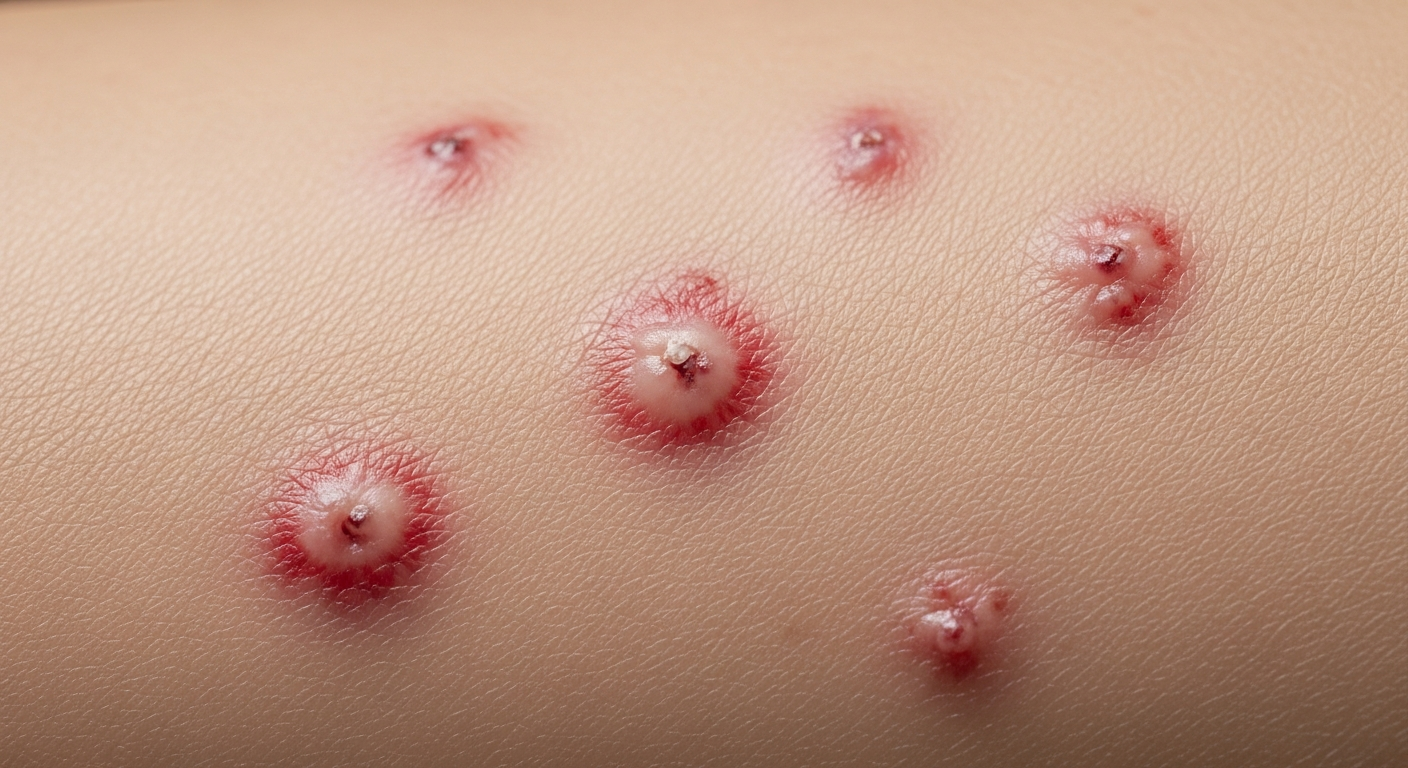
For individuals seeking to identify or understand the visual presentation of varicella-zoster virus infection, a detailed examination of Chickenpox symptoms pictures is crucial. These images depict the various stages of the characteristic rash, offering invaluable insights into disease progression and manifestation across the skin and mucous membranes. Understanding these visual cues is paramount for accurate diagnosis and timely intervention.
Chickenpox Symptoms Pictures
Understanding the visual chickenpox symptoms pictures is essential for identifying this common viral infection. The hallmark of chickenpox, caused by the varicella-zoster virus (VZV), is its distinctive rash, which progresses through several stages, often simultaneously present on the body. This asynchronous development is a key diagnostic feature.
Key Visual Indicators of Chickenpox:
- Prodromal Symptoms (Often Not Visible in Pictures but Precedes Rash): While not directly visible in a photo, it’s important to note that many individuals, particularly adults and adolescents, may experience a prodrome of symptoms 1-2 days before the rash appears. These can include:
- Mild fever (typically 100-102°F or 37.8-38.9°C)
- General malaise or feeling unwell
- Headache
- Loss of appetite
- Body aches or muscle pain
- Fatigue
- Irritability (especially in young children)
- Macules (Red Spots):
- Appearance: These are the very first lesions to emerge. They appear as small, flat, red spots on the skin. They are non-raised and might initially be mistaken for insect bites or a generic allergic reaction.
- Size: Typically 2-4 mm in diameter.
- Distribution: They usually begin on the face, scalp, and trunk (chest, back, abdomen), often appearing first on areas covered by clothing. They then spread to the extremities.
- Progression: Macules are transient and quickly evolve into papules, often within hours.
- Papules (Small Bumps):
- Appearance: Macules rapidly transform into slightly raised, red bumps. These papules are solid to the touch.
- Sensation: The itching often begins or intensifies at this stage.
- Number: New papules can continue to appear for 3-5 days.
- Evolution: Within a day or two, these papules develop into fluid-filled blisters (vesicles).
- Vesicles (Fluid-Filled Blisters):
- Appearance: This is the most characteristic stage, often described as “dewdrops on a rose petal.” The vesicles are small, clear, fluid-filled blisters that sit on a red base. The fluid is initially clear but can become cloudy.
- Size: Generally 2-5 mm in diameter.
- Fragility: The vesicle walls are very thin and fragile, making them prone to rupture, either spontaneously or due to scratching.
- Location: They are found all over the body, including mucous membranes (mouth, throat, genitals, eyelids), which can be particularly painful and lead to difficulty eating or urinating. Vesicles on the scalp are also very common and can be intensely itchy.
- Itching: The itching at this stage is typically severe and relentless.
- Pustules (Pus-Filled Lesions):
- Appearance: As vesicles mature, the clear fluid often becomes cloudy and may turn yellowish, indicating the presence of pus. These are pustules. This is a natural progression and doesn’t necessarily mean a secondary bacterial infection, though it can precede one.
- Texture: They are still raised but may feel more firm than early vesicles.
- Evolution: Pustules eventually dry out and form scabs.
- Scabs/Crusts:
- Appearance: Once vesicles or pustules rupture or dry, they form crusts or scabs. These are typically yellowish-brown and eventually fall off.
- Healing: The scabs usually heal without scarring unless there has been significant scratching or secondary bacterial infection.
- Contagion: An individual is considered contagious until all lesions have crusted over, meaning there are no new blisters forming and all existing ones have scabbed.
- Timeline: This process from macule to scab typically takes about 7-10 days for any individual lesion, but since new lesions appear daily, the total duration of the rash can be up to 2 weeks.
- “Crops” of Lesions: A crucial visual aspect is the simultaneous presence of lesions at different stages of development (macules, papules, vesicles, pustules, and scabs) in the same area of the body. This phenomenon is highly indicative of chickenpox.
Signs of Chickenpox Pictures
Analyzing signs of chickenpox pictures goes beyond just the individual lesions; it involves observing the overall pattern, distribution, and associated physical manifestations that can be captured visually or inferred from a comprehensive photographic series. These signs help differentiate chickenpox from other common skin conditions.
Observable Signs in Chickenpox Photography:
- Rash Distribution Patterns:
- Centripetal Spread: The rash typically starts on the trunk (chest, back, abdomen) and face, then spreads outward to the arms and legs. This “centripetal” distribution, where the rash is densest on the torso and less so on the extremities, is a classic sign.
- Scalp Involvement: One of the strongest indicators is the presence of lesions on the scalp, often hidden by hair. These can be intensely itchy and lead to scratching.
- Mucous Membrane Involvement: Ulcers or blisters in the mouth, throat, eyes, and genital area are common. Oral lesions can make eating and drinking painful, appearing as small, shallow ulcers with a red base. Pictures might show redness and small white or yellow spots inside the mouth.
- Axillary and Groin Areas: Lesions are frequently found in skin folds, such as the armpits and groin.
- Evolutionary Asynchrony:
- Simultaneous Stages: As mentioned, the presence of various lesion types—red spots, bumps, fresh blisters, cloudy blisters, and crusts—all at once in one photographic frame or across the body is a definitive sign of chickenpox. This “polymorphism” is a powerful diagnostic clue that helps distinguish it from other viral rashes (like measles or rubella, which tend to have rashes at a uniform stage).
- Ongoing Appearance: Pictures taken over several days would show new crops of lesions appearing while older ones progress, demonstrating the continuous cycle of eruption.
- Associated Skin Manifestations:
- Erythema: General redness of the skin around the lesions due to inflammation.
- Scratch Marks/Excoriations: Due to intense itching, individuals, especially children, often scratch, leading to linear abrasions, scabs, and potential signs of secondary bacterial infection (e.g., honey-colored crusting indicating impetigo). Pictures may show these visible signs of scratching.
- Post-Inflammatory Pigmentation: After scabs fall off, some individuals, particularly those with darker skin tones, may develop temporary hyperpigmentation (darker spots) or hypopigmentation (lighter spots) at the site of healed lesions.
- Scarring: While most chickenpox lesions heal without scarring, deep scratching, secondary bacterial infections, or lesions that are picked can lead to permanent, pitted scars.
- General Appearance (Inferred from Photographs):
- Distress/Discomfort: Although not a direct rash sign, a child’s facial expression in a photo might convey discomfort, irritability, or fatigue, which are common non-specific symptoms.
- Dehydration: In severe cases, especially with painful oral lesions, a child might appear listless or signs of dehydration (e.g., dry lips, sunken eyes) could be inferred in pictures.
- Atypical Presentations (Less Common but Important):
- Hemorrhagic Chickenpox: A rare, severe form where vesicles contain blood, appearing darker, and can be accompanied by bleeding from other sites. This is a medical emergency.
- Bullous Chickenpox: Larger, blister-like lesions (bullae) may form.
- Congenital Varicella Syndrome: In infants whose mothers contracted chickenpox during pregnancy, specific birth defects can be observed, though these are not typical rash pictures of a developing infection.
- Varicella in Immunocompromised Individuals: The rash can be much more severe, extensive, hemorrhagic, and prolonged, with lesions appearing in atypical areas and healing poorly.
Early Chickenpox Photos
Early chickenpox photos focus on the initial eruption, providing a critical window into the very first manifestations of the rash. Identifying chickenpox at this nascent stage can facilitate prompt management and isolation, helping to prevent further spread of the highly contagious varicella-zoster virus. These early images capture the subtle yet distinct changes on the skin before the full-blown vesicular rash develops.
Characteristics to Look for in Early Chickenpox Photos:
- Initial Presentation – The Macule Stage:
- Appearance: The very first lesions are small, flat, red spots (macules). They are often indistinct and can be easily overlooked or mistaken for other minor skin irritations. They lack elevation.
- Color: Typically bright red or reddish-pink.
- Size: Usually pinhead-sized, growing to 2-4 mm in diameter.
- Feeling: They are not usually itchy at this precise stage, though the itching sensation often begins shortly after they appear or as they evolve.
- Distribution: Early photos will likely show these macules predominantly on the trunk (chest, back), face, and scalp. They tend to appear in clusters rather than a single isolated spot.
- Rapid Progression to Papules:
- Appearance: Within hours of the macules appearing, they quickly become slightly raised, firm, red bumps (papules). This elevation differentiates them from the earlier flat spots.
- Feel: When touched, these papules have a palpable texture.
- Itching Onset: This is often the stage where the characteristic intense itching of chickenpox truly begins, prompting discomfort.
- Number: Early photos might show a sparse distribution initially, with only a few dozen lesions, but their number rapidly increases over the next 24-48 hours.
- First Appearance of Vesicles:
- Timing: The transformation from papule to vesicle (fluid-filled blister) is remarkably fast, often occurring within 12-24 hours after the initial macule appears. Early photos might capture this transition where some lesions are still papules, while others have just developed a clear fluid center.
- “Dewdrop” Appearance: Look for the classic “dewdrop on a rose petal” description – a tiny, clear, superficial blister sitting on a slightly reddened base. This is a definitive sign.
- Transparency: In early vesicles, the fluid is clear and translucent. Cloudiness or pus-like appearance indicates a later stage.
- Fragility: The walls of these fresh vesicles are very thin and easily rupture.
- Early Locations: The first vesicles are most likely to be seen on the trunk and face. Areas like the scalp and inside the mouth might also show early vesicular lesions.
- Limited Spread:
- Concentration: Early chickenpox photos usually show a higher concentration of lesions on the central parts of the body (trunk and face), with fewer or no lesions yet on the arms and legs.
- Absence of Crusting: Crucially, in early chickenpox, there should be no scabs or crusts. The presence of scabs would indicate that the infection has been present for several days and is no longer in its absolute early stage. The earliest images capture only the initial eruptions, which are predominantly macules, papules, and nascent vesicles.
- Prodromal Clues (If Available):
- While photos primarily show visible symptoms, if accompanying information describes prodromal symptoms (fever, malaise) preceding the photographed rash by a day or two, this strongly supports an early chickenpox diagnosis. For instance, a photo of a child with a few early macules and a slightly flushed face could visually imply a fever.
Skin rash Chickenpox Images
Skin rash chickenpox images encompass the full spectrum of morphological changes, from the initial eruption to the final stages of healing. This section delves into the detailed visual characteristics of the chickenpox rash, emphasizing its unique evolution and distribution, which are key to accurate identification.
Detailed Morphology and Evolution of the Chickenpox Rash:
- Maculopapular Stage: The Genesis of the Rash
- Initial Macules: Appear as small, flat, reddish spots (erythematous macules), typically 2-4 mm in diameter. They are non-blanching under pressure, indicating underlying inflammation.
- Progression to Papules: Within a few hours, these macules become elevated, forming small, firm, red bumps (papules). The skin around them may also be slightly reddened, forming an erythematous halo.
- Distribution: Primarily concentrated on the trunk, face, and scalp. They are often sparse on the extremities in the earliest stages.
- Onset of Itching: The characteristic pruritus (itching) often begins as lesions transition from macules to papules.
- Vesicular Stage: The Iconic “Dewdrop” Blisters
- Rapid Transformation: Papules quickly evolve into vesicles, typically within 12-24 hours. These are the most distinctive feature of chickenpox.
- Appearance: Small (2-5 mm), clear, fluid-filled blisters that are superficial and delicate. They possess a characteristic “dewdrop on a rose petal” appearance, meaning a clear, glistening vesicle resting on a reddish, inflamed base.
- Fluid Content: Initially, the fluid is clear and serous. Over 1-2 days, it often becomes cloudy or turbid as inflammatory cells accumulate, leading towards the pustular stage.
- Fragility: The vesicle walls are extremely thin and easily rupture, either spontaneously or due to scratching. This rupture releases fluid, which can then spread the virus.
- Intense Pruritus: Itching is at its peak during the vesicular stage, leading to significant discomfort and the potential for secondary bacterial infections from scratching.
- Mucosal Involvement: Vesicles are common on mucous membranes, including the oral cavity (buccal mucosa, palate, tongue), pharynx, conjunctiva, and genital regions. Oral lesions appear as shallow, painful ulcers.
- Scalp Lesions: Often numerous and hidden by hair, scalp vesicles contribute significantly to the overall discomfort and itching.
- Pustular Stage: Cloudy Blisters and Infection Risk
- Appearance: Vesicles become pustules when their fluid turns opaque and yellowish, indicative of pus formation. This transformation is a natural part of the disease progression for many lesions, not always a sign of bacterial infection.
- Size: Slightly larger and more elevated than early vesicles.
- Risk of Secondary Infection: While natural, these lesions are more susceptible to secondary bacterial infections, especially if scratched. Signs of bacterial infection include increasing redness, warmth, swelling, pain around the lesion, and thicker, honey-colored crusts.
- Crusting Stage: Healing and Contagion End
- Formation: As vesicles and pustules dry up, they form yellowish-brown, irregular crusts or scabs. This typically happens 3-7 days after eruption for an individual lesion.
- Falling Off: These scabs gradually detach and fall off over 1-2 weeks.
- Resolution of Contagion: A person is no longer considered contagious once all lesions have crusted over, and no new blisters are forming.
- Scarring: Most chickenpox scabs heal without permanent scarring, especially if they are not scratched or picked. However, deep scratching, bacterial superinfection, or lesions on particular areas (e.g., face) can lead to pitted, permanent scars.
- Pigmentary Changes: Post-inflammatory hyperpigmentation (darkening) or hypopigmentation (lightening) can occur, especially in individuals with darker skin tones, but these usually resolve over time.
- Asynchronous Crops – The Definitive Visual Hallmark:
- Polymorphism: The most distinctive visual characteristic of the chickenpox rash is the simultaneous presence of lesions in all stages of development—macules, papules, fresh clear vesicles, cloudy vesicles, pustules, and crusts—all visible on the body at the same time. This “polymorphic” rash is almost pathognomonic for chickenpox.
- Continuous Eruption: New crops of lesions continue to appear for 3-5 days, while older ones progress through their stages, leading to this mixed appearance.
- Extent and Severity of Rash:
- Mild Cases: May have only a few dozen lesions, predominantly on the trunk.
- Moderate to Severe Cases: Can involve hundreds to thousands of lesions covering most of the body surface, including the scalp, face, trunk, and extremities, as well as mucous membranes.
- Age-Related Severity: The rash tends to be more extensive and severe in adults and immunocompromised individuals.
Differential Diagnosis Considerations (What Chickenpox is NOT):
- Measles: Characterized by a uniform, maculopapular rash that starts on the head and spreads downwards, often coalescing, without vesicles. Koplik spots in the mouth precede the rash.
- Rubella (German Measles): A milder maculopapular rash, often starting on the face and spreading quickly, also without vesicles.
- Herpes Zoster (Shingles): Caused by reactivation of the same VZV, but presents as a painful, vesicular rash confined to a dermatome (a single nerve path), typically unilateral.
- Hand, Foot, and Mouth Disease: Caused by coxsackievirus, features vesicles and ulcers in the mouth, and non-itchy lesions on the palms, soles, and sometimes buttocks.
- Impetigo: A bacterial skin infection causing honey-colored crusts, usually without preceding macules or papules across the body.
- Insect Bites: Can cause itchy bumps but are usually localized and don’t progress through the distinct stages or widespread distribution of chickenpox.
- Scabies: Characterized by intensely itchy papules and burrows, often in webs of fingers, wrists, and beltline, with distinct patterns different from chickenpox.
Chickenpox Treatment
Chickenpox treatment primarily focuses on managing symptoms, preventing complications, and, in certain high-risk groups, using antiviral medications. The goal is to alleviate discomfort, reduce itching, and promote healing without scarring. It’s crucial to consult a healthcare provider for personalized advice, especially for severe cases or at-risk individuals.
Symptomatic Relief and Home Care:
- Relieving Itching (Pruritus Management):
- Antihistamines: Oral antihistamines (e.g., diphenhydramine, loratadine, cetirizine) can help reduce itching and improve sleep, especially at night. Non-drowsy options are available for daytime use.
- Calamine Lotion: Topical calamine lotion provides a cooling sensation and helps dry out lesions, reducing itching. Apply liberally to affected areas.
- Oatmeal Baths: Colloidal oatmeal baths can soothe irritated and itchy skin. Avoid scrubbing; gently pat dry afterward. Lukewarm water is preferred over hot water, which can intensify itching.
- Cool Compresses: Applying cool, wet cloths to particularly itchy spots can offer temporary relief.
- Loose-Fitting Clothing: Dress in loose, soft, cotton clothing to minimize irritation to the skin.
- Keep Fingernails Trimmed: Short fingernails reduce the risk of scratching, which can lead to secondary bacterial infections and scarring. Consider mittens for infants and young children, especially during sleep.
- Fever Reduction:
- Acetaminophen (Paracetamol): Can be used to manage fever and body aches. Follow dosing instructions carefully.
- Avoid Aspirin: Crucially, do not give aspirin or aspirin-containing products to children or adolescents with chickenpox. This can lead to Reye’s syndrome, a serious and potentially fatal condition affecting the brain and liver. Always check medication labels for aspirin content.
- Hydration and Nutrition:
- Fluids: Encourage plenty of fluids to prevent dehydration, especially if fever is present.
- Soft Foods: If oral lesions are present and painful, offer soft, bland foods that are easy to swallow. Avoid acidic, salty, or spicy foods that can irritate mouth sores. Cool foods like yogurt or ice cream can be soothing.
- Hygiene:
- Regular Bathing: Gentle, daily bathing (short, lukewarm showers or oatmeal baths) can help keep skin clean and prevent bacterial infections. Use mild, unscented soap.
- Avoid Rubbing: Pat skin dry with a clean towel instead of rubbing, to prevent rupturing blisters and causing irritation.
Antiviral Medications:
- Acyclovir: An antiviral drug that can reduce the severity and duration of chickenpox if started within 24 hours of the rash onset.
- Indications:
- Immunocompromised individuals (e.g., those with HIV, on chemotherapy, or organ transplant recipients).
- Adults and adolescents (who tend to have more severe disease).
- Individuals with chronic skin or lung conditions (e.g., eczema, asthma).
- Household contacts of immunocompromised individuals or pregnant women.
- Sometimes considered for children over 12 years old.
- Mechanism: Acyclovir works by inhibiting the replication of the varicella-zoster virus.
- Other Antivirals: Famciclovir and valacyclovir are also used, often in adults, and have similar efficacy with different dosing schedules.
- Indications:
Prevention of Complications:
- Secondary Bacterial Infections:
- Signs: Increased redness, warmth, swelling, pain, pus-filled lesions, or honey-colored crusts around lesions.
- Treatment: If a bacterial infection is suspected, a healthcare provider may prescribe oral antibiotics.
- Prevention: Good hygiene and avoiding scratching are key preventive measures.
- Scarring:
- Minimize Scratching: Preventing scratching is the best way to avoid pitted scars.
- Moisturizers: Once lesions have scabbed and fallen off, gentle, unscented moisturizers can help skin heal.
- Isolation:
- Contagious Period: Individuals with chickenpox are contagious from 1-2 days before the rash appears until all lesions have crusted over (typically 5-10 days after rash onset).
- School/Work Exclusion: Stay home from school, daycare, or work during the contagious period to prevent spreading the virus, especially to unvaccinated or vulnerable individuals.
Post-Exposure Prophylaxis:
- Varicella-Zoster Immune Globulin (VZIG): Can be administered to high-risk individuals (e.g., immunocompromised, pregnant women, neonates) who have been exposed to chickenpox and are susceptible, to prevent or modify the disease.
- Varicella Vaccine: The chickenpox vaccine can also be given post-exposure (within 3-5 days) to susceptible individuals to prevent or significantly lessen the severity of the disease.
Long-Term Considerations:
- Shingles (Herpes Zoster): The varicella-zoster virus remains dormant in nerve cells after chickenpox. It can reactivate later in life, causing shingles. Vaccination against shingles is available for adults aged 50 and older to prevent this reactivation.
- Vaccination: The chickenpox vaccine is highly effective in preventing chickenpox and is recommended as part of routine childhood immunization. Two doses are typically given.