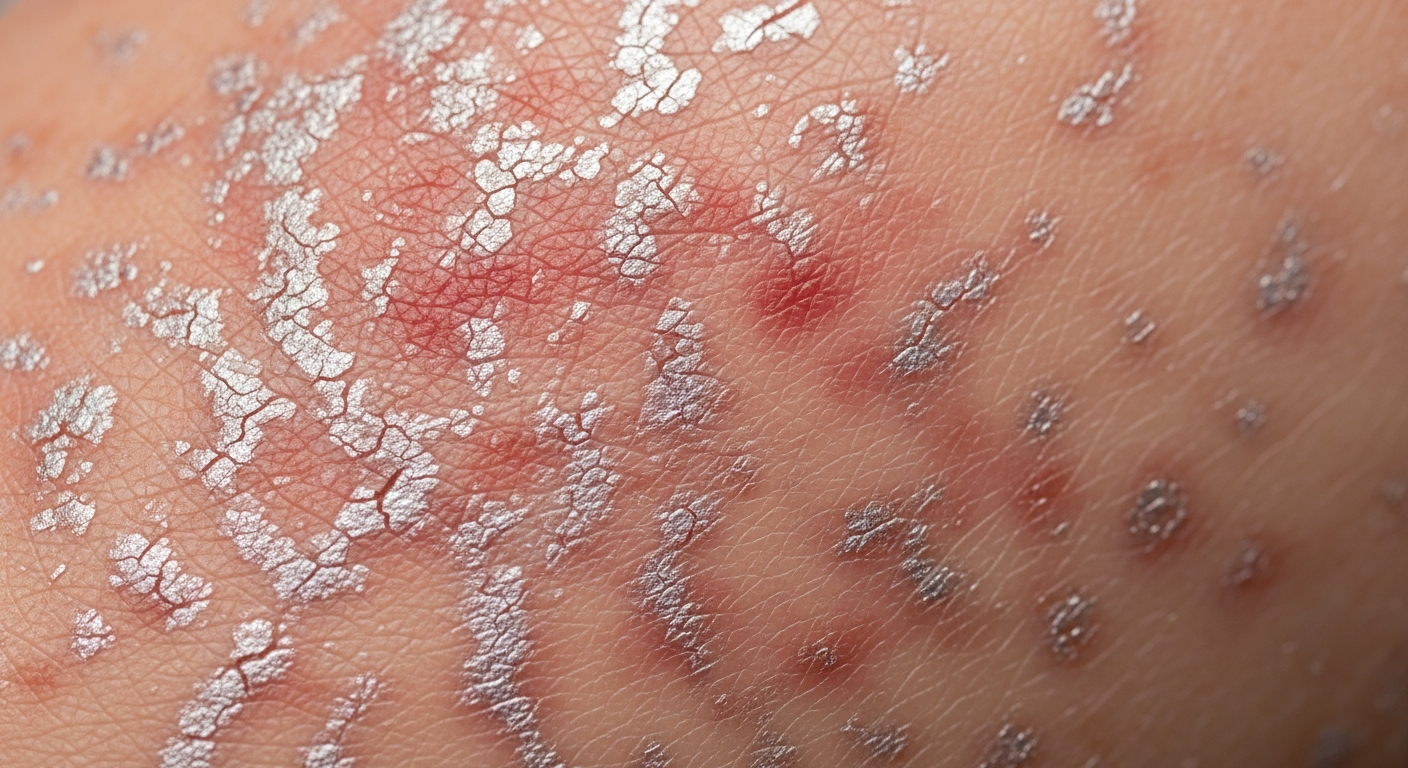
Understanding the diverse visual manifestations is crucial for recognizing skin conditions. This article provides an extensive look at Psoriasis symptoms pictures, detailing the various ways this condition presents on the skin, aiding in visual identification and comprehension of its complex appearances.
Psoriasis Symptoms Pictures
Examining Psoriasis symptoms pictures reveals a spectrum of dermatological presentations, with each type exhibiting distinct visual characteristics crucial for accurate identification. The most common form, plaque psoriasis, typically manifests as raised, inflamed, intensely red patches of skin, often covered with thick, silvery-white scales. These lesions are generally well-demarcated, possessing clear, distinct borders that separate them from surrounding healthy skin. The scales are a hallmark feature, representing an accelerated turnover of skin cells that accumulate on the surface. These plaques can vary significantly in size, from small, coin-sized lesions to extensive areas covering large portions of the body. Common sites for plaque psoriasis include the extensor surfaces of the elbows and knees, the lower back, and the scalp. Patients frequently report significant itching, which can range from mild discomfort to severe, debilitating pruritus that interferes with sleep and daily activities. In some instances, the skin may feel tight, painful, or even crack and bleed, especially in areas subjected to movement or friction. The color of the plaques can vary depending on skin tone; on lighter skin, they often appear bright red or salmon-pink, while on darker skin tones, they might present as purplish, dark brown, or grayish patches, sometimes with less pronounced redness but still retaining the characteristic silvery scales. The texture of these plaques is often rough and uneven due to the build-up of scales, and attempts to scratch or remove these scales can lead to pinpoint bleeding, a phenomenon known as the Auspitz sign, which is a significant diagnostic indicator.
Guttate psoriasis is another distinct subtype, characterized by the sudden appearance of numerous small, teardrop-shaped lesions. These spots are typically less than 1 centimeter in diameter, often pink or salmon-pink, and covered with fine, delicate scales that are less silvery and thick compared to those seen in plaque psoriasis. These lesions commonly erupt over the trunk, arms, legs, and scalp, often following an infection, most notably streptococcal throat infections. The distribution is usually widespread, creating a scattered appearance across the body. The onset is frequently rapid, emerging within days or weeks after the triggering event. The itching associated with guttate psoriasis can also be considerable, though often less intense than the chronic pruritus experienced with plaque psoriasis. The lesions tend to be round or oval, and while they can be numerous, they usually remain discrete and do not coalesce into larger plaques, which differentiates them visually from extensive plaque psoriasis.
Inverse psoriasis, sometimes referred to as flexural psoriasis, presents in a visually distinct manner due to its location in skin folds. Unlike other forms, inverse psoriasis appears as smooth, shiny, intensely red, and inflamed patches that typically lack the characteristic silvery scales. The moist environment of skin folds, such as the armpits (axillae), groin, under the breasts, in the genital area, and within the gluteal cleft, prevents the formation of noticeable scales. The affected skin often looks macerated and can be prone to irritation from rubbing and sweating. Due to its smooth, non-scaly appearance and location, inverse psoriasis can often be mistaken for fungal infections (like candidiasis) or intertrigo. Patients often experience significant discomfort, including burning, itching, and pain, which can be exacerbated by friction and moisture. The sharp, well-defined borders of the lesions remain a key diagnostic feature, even in the absence of scales, allowing for differentiation from other intertriginous dermatoses.
Pustular psoriasis, a less common but often more severe form, is characterized by the presence of sterile, non-infectious pustules (small, pus-filled blisters) on a background of red, inflamed skin. This type is visually striking and can be subcategorized into generalized and localized forms. Generalized pustular psoriasis (GPP), also known as Von Zumbusch psoriasis, is a medical emergency. It involves widespread redness and tenderness of the skin, followed by the rapid eruption of countless sterile pustules that can coalesce into large areas of pus. This eruption is typically accompanied by systemic symptoms such as fever, chills, fatigue, severe itching, and extreme pain. The skin becomes very sensitive, and large sheets of epidermis may shed, resembling a severe burn. The visual impact of GPP pictures is one of acute distress and significant systemic involvement. Localized pustular psoriasis, such as palmoplantar pustulosis, is confined to the palms of the hands and soles of the feet. It presents as recurrent crops of small, deep-seated pustules on erythematous skin, often leading to significant pain, dryness, cracking (fissures), and thickening (hyperkeratosis) of the skin. The pustules eventually dry up, forming brown crusts and scales, which then peel away, only for new pustules to emerge. The visual characteristics of the hands and feet in palmoplantar pustulosis include pronounced redness, numerous yellowish-brown pustules, and deep, painful cracks that can severely impair manual dexterity and ambulation.
Erythrodermic psoriasis is another severe and potentially life-threatening form, characterized by widespread, generalized redness and inflammation covering more than 75-90% of the body surface. The skin appears intensely red, almost scarlet, and often feels hot to the touch. This form typically involves extensive scaling and shedding of the skin in sheets, accompanied by severe itching, burning, and pain. Patients often experience systemic symptoms due to the extensive skin involvement, including widespread swelling (edema), particularly in the ankles and feet, fever, chills, and fatigue. The massive loss of skin cells and damage to the skin barrier can lead to significant fluid and protein loss, electrolyte imbalances, and an increased risk of infection. Visually, erythrodermic psoriasis is dramatic, showing a uniformly red body surface with areas of active peeling and a visibly compromised skin barrier, making it distinct from other forms and signaling a critical medical condition.
Nail psoriasis affects the fingernails and toenails, leading to a variety of visual changes that can be quite distinct in Psoriasis symptoms pictures. Common signs include pitting, which are small, pinpoint depressions on the nail plate, resembling the surface of a thimble. Discoloration, particularly yellowish-brown spots resembling “oil drops” or “salmon patches” beneath the nail plate, is another highly characteristic feature. The nails may also become thick, crumbly, and brittle (onychodystrophy), sometimes separating from the nail bed (onycholysis), creating a space where debris can accumulate. Subungual hyperkeratosis, a build-up of chalky material under the nail, can further lift and thicken the nail. These nail changes can be painful and impact dexterity, and they are often associated with psoriatic arthritis. The visual impact on the nails can range from subtle pitting to severe destruction and malformation, offering key diagnostic clues, especially when other skin manifestations are subtle or absent.
Psoriatic arthritis (PsA) involves joint inflammation and is frequently accompanied by skin psoriasis, although in some cases, joint symptoms may precede skin lesions. The visual cues for PsA in pictures primarily focus on the joints and digits. Swelling and tenderness of the joints are common, often appearing as visibly enlarged or puffy joints. A hallmark feature is dactylitis, characterized by the uniform swelling of an entire finger or toe, giving it a “sausage-like” appearance. This diffuse inflammation affects not only the joint but also the surrounding soft tissues. Enthesitis, inflammation at the sites where tendons or ligaments attach to bone, can also be a visual sign, manifesting as swelling and tenderness, particularly at the Achilles tendon insertion or plantar fascia in the heel. Nail changes, as described above, are frequently observed in individuals with PsA, with up to 80% of PsA patients showing nail involvement. The visual evidence of PsA often extends beyond individual joints, sometimes presenting with visible asymmetry in joint involvement. Early detection of these visual symptoms in Psoriasis symptoms pictures is vital for timely intervention to prevent irreversible joint damage.
Signs of Psoriasis Pictures
Analyzing Psoriasis signs pictures provides deeper insight into the various diagnostic markers and visual cues that distinguish this condition. Beyond the primary lesions, several secondary signs and specific presentations aid in the identification of psoriasis. One such critical sign is the Koebner phenomenon, also known as the isomorphic response. This phenomenon involves the development of psoriatic lesions at sites of skin trauma or injury. Visually, a picture might show linear plaques appearing along a scratch line, a surgical scar, or even areas subjected to repeated friction. This sign is not exclusive to psoriasis but is a strong indicator when observed. It underscores the skin’s heightened sensitivity and inflammatory response in affected individuals. Another classic diagnostic sign is the Auspitz sign, where pinpoint bleeding occurs when the overlying silvery scales of a psoriatic plaque are gently scraped or removed. This bleeding is due to the thinning of the epidermis and the close proximity of dilated capillaries to the surface of the skin, a characteristic histological feature of psoriasis. In pictures, this would manifest as small, red dots appearing immediately after scale removal, a clear indication of compromised superficial vasculature.
The presentation of psoriasis can vary significantly with age. In children, psoriasis pictures might show less extensive lesions, often concentrated on the scalp, face, and in the diaper area (diaper psoriasis), which can sometimes be mistaken for eczema. Childhood psoriasis tends to have thinner plaques and finer scales, and guttate psoriasis is particularly common in pediatric populations, often following a strep infection. In adults, especially older individuals, psoriasis can sometimes be less inflammatory, appearing as thicker, more chronic plaques that may be less erythematous. The signs can also differ based on skin tone. On lighter skin, the vibrant red color of plaques is prominent. On darker skin tones, the erythema can be masked, leading to a more purplish, brownish, or grayish hue, sometimes with post-inflammatory hyperpigmentation (darkening of the skin) after lesions resolve. This variation in presentation means careful examination is needed when interpreting Psoriasis signs pictures across diverse populations.
Specific body areas exhibit unique visual signs of psoriasis. On the scalp, psoriasis pictures reveal thick, adherent, silvery scales that can cover the entire scalp or appear as discrete patches. The underlying skin is often red and inflamed. Severe scalp psoriasis can extend beyond the hairline onto the forehead, neck, and behind the ears (retroauricular area). While psoriasis itself doesn’t typically cause permanent hair loss, vigorous scratching or picking at the scales can lead to temporary hair thinning or breakage. The visual signs of scalp psoriasis are distinct from seborrheic dermatitis, which usually involves greasier, yellowish scales and less intense erythema. For hands and feet, pictures often show significant dryness, thickening of the skin (hyperkeratosis), cracking, and fissuring, especially with palmoplantar psoriasis. These painful cracks can be visually evident, impacting the texture and integrity of the skin. The presence of pustules on the palms and soles in palmoplantar pustulosis also provides a unique visual marker, often with overlying scales and crusts.
Genital psoriasis signs pictures show smooth, well-demarcated, intensely red patches that are typically devoid of scales due to the moist environment of the genital and perianal regions. These lesions can be particularly bothersome, causing significant itching, burning, and soreness. The absence of scales means they can be visually confused with fungal infections or other dermatoses, necessitating careful differentiation. Facial psoriasis is less common but can manifest around the hairline, eyebrows, eyelids, and ears. The plaques tend to be thinner and less scaly than those on other body parts, and the skin in these areas is often more sensitive, making treatment challenging. The visual signs on the face require careful interpretation, as they can mimic other facial rashes. Intergluteal psoriasis, affecting the fold between the buttocks, similarly presents as smooth, red, inflamed patches without scales, sometimes accompanied by fissuring. These specific visual signs across different anatomical locations are crucial for a comprehensive understanding and accurate diagnosis of psoriasis, emphasizing the need for a varied collection of Psoriasis signs pictures for educational and diagnostic purposes.
Early Psoriasis Photos
Early Psoriasis photos capture the initial, often subtle, manifestations of the condition, which can be critical for prompt diagnosis and intervention. The very first signs of psoriasis may not always be the classic, fully developed plaques. Instead, they can begin as small, erythematous papules (red bumps) that gradually enlarge and coalesce. These nascent lesions might first appear as areas of mild redness with very fine, barely noticeable scales. On lighter skin, these initial lesions might be faintly pink or red. On darker skin, they could appear as subtle purplish or brownish discolorations that are slightly raised. The borders might not yet be sharply defined, giving them a less characteristic appearance than mature plaques. These early lesions often emerge in typical psoriatic predilection sites such as the elbows, knees, scalp, or lower back, but their small size and subdued characteristics can make them difficult to distinguish from other common skin conditions. Recognizing these subtle beginnings in Early Psoriasis photos is paramount for early intervention.
A significant challenge in interpreting early Psoriasis photos lies in differentiating it from other dermatological conditions that can mimic its initial presentation. For instance, early psoriatic lesions can often be mistaken for eczema (atopic dermatitis), which also presents with red, itchy patches. However, eczema lesions tend to be less well-demarcated, often with a more eczematous, oozing, or lichenified (thickened, leathery) appearance, particularly in chronic stages, and are more common in flexural areas like the inner elbows and behind the knees. Early psoriasis can also be confused with fungal infections, such as ringworm (tinea corporis), which typically presents as an annular (ring-shaped) lesion with central clearing and a scaly, raised border. Pityriasis rosea, another common rash, also features scaly, oval patches, but its characteristic “herald patch” and “Christmas tree” distribution pattern can help differentiate it from early guttate psoriasis. The scales in early psoriasis might be finer and less silvery, making the distinction from other scaling conditions more challenging without a strong index of suspicion.
The evolution of lesions is a key aspect captured in sequential Early Psoriasis photos. What might start as a single small, pinkish-red papule can gradually expand outwards, developing the characteristic silvery scales as it grows. The scales initially might be thin and white, later thickening and becoming more adherent. Over time, multiple small papules can emerge and then merge to form larger, more extensive plaques. The development of sharp, distinct borders usually becomes more apparent as the lesion matures. In some cases, particularly with guttate psoriasis, the onset can be quite sudden, with numerous small, teardrop-shaped spots appearing rapidly across the body, often a few weeks after a throat infection. These early guttate lesions are typically smaller and less scaly than those of plaque psoriasis and can be misidentified as a viral rash. The visual progression from a mild, almost inconspicuous patch to a more established lesion provides crucial insights into the disease’s natural history.
Subtle signs in Early Psoriasis photos might also include isolated patches on the scalp that are initially mistaken for severe dandruff, or mild redness and scaling on the nails that are attributed to trauma or fungal infections. The presence of itching, even in the absence of prominent lesions, can sometimes be an early indicator. The Koebner phenomenon, as described earlier, can also be an early sign, with lesions developing in areas of minor skin injury before more widespread manifestations appear. For example, a child might develop a linear plaque where they scraped their knee, preceding other psoriatic spots. These early, sometimes isolated or atypical presentations, underscore the importance of careful clinical examination and a thorough patient history. The visual evidence in Early Psoriasis photos serves as a vital educational tool, demonstrating that psoriasis doesn’t always begin with textbook-perfect plaques but often with more nuanced and evolving dermatological changes that demand keen observational skills for accurate early diagnosis and management of the condition.
Skin rash Psoriasis Images
Skin rash Psoriasis images showcase the vast array of inflammatory dermatological presentations, emphasizing the characteristic rashes that define this chronic immune-mediated condition. The most commonly depicted rash in Psoriasis images is that of plaque psoriasis. This rash is universally recognized by its distinct features: well-demarcated, raised, erythematous (red) patches covered with silvery-white scales. The vibrant red color results from increased blood flow and inflammation in the skin. The scales are due to the rapid proliferation and turnover of keratinocytes, leading to an accumulation of immature cells on the skin surface. The term “rash” for plaque psoriasis encompasses these individual lesions, which can appear anywhere on the body but predominantly affect extensor surfaces (elbows, knees), the lower back, and the scalp. Pictures of these rashes often highlight the sharp borders distinguishing psoriatic skin from unaffected areas. The texture can vary from smooth and slightly raised to thick, rugged, and extensively scaled. Severe itching, burning, and pain are frequently associated with these rashes, and excoriations (scratch marks) may be visible in images, indicative of the intense pruritus. In darker skin tones, the erythema of the rash may appear as purplish or dark brown, making the silvery scales the more dominant visual cue.
Guttate psoriasis images display a different type of rash: numerous small, discrete, teardrop-shaped lesions spread across the trunk and limbs. These spots are typically salmon-pink and covered with fine, delicate scales. The rash often appears suddenly, frequently after a streptococcal infection, and can be quite widespread. Unlike plaque psoriasis, the lesions in guttate psoriasis usually remain small and separate, rarely coalescing into larger plaques. The term “guttate” means “drop-like,” accurately describing the appearance of this rash. Visualizing this specific rash in pictures allows for clear differentiation from other conditions like pityriasis rosea, which also features a widespread, scaly rash but with a different morphology and distribution. The onset can be dramatic, with hundreds of these small spots appearing over a short period, creating a very distinct visual pattern on the skin. The inflammation beneath these small scales is typically less pronounced than in plaque psoriasis, leading to less elevation and a more superficial appearance.
Inverse psoriasis rash images focus on lesions found in intertriginous areas, such as the armpits, groin, under the breasts, and in the gluteal cleft. Here, the rash appears as smooth, glossy, deep red, and intensely inflamed patches that typically lack the characteristic silvery scales due to the moist, occluded environment. The absence of scales is a key differentiating feature. The borders of the rash remain well-defined, and the affected skin may appear shiny and macerated. These rashes are highly susceptible to friction and moisture, leading to discomfort, burning, and sometimes fissuring. Recognizing this unique rash morphology in Psoriasis images is crucial, as its appearance often leads to misdiagnosis as a fungal infection (e.g., candidiasis) or bacterial intertrigo, both of which share similar anatomical locations and some visual characteristics, but lack the distinct, sharply demarcated erythematous base of inverse psoriasis.
Pustular psoriasis rash images depict a severe form, characterized by the eruption of sterile pustules on a background of erythematous skin. In generalized pustular psoriasis (GPP), the rash is widespread, starting with large areas of fiery redness that quickly become studded with countless small, non-infectious pustules. These pustules can coalesce into lakes of pus, and the skin often peels in large sheets. The rash is extremely painful and tender to the touch, and it is usually accompanied by systemic symptoms like fever and chills, making it a medical emergency. The dramatic visual presentation in GPP pictures highlights the intensity of the inflammation and the widespread skin involvement. For localized pustular psoriasis, particularly palmoplantar pustulosis, the rash is confined to the palms and soles. Images show recurrent crops of yellowish pustules on red, thickened skin, leading to severe dryness, cracking, and pain. The pustules eventually dry and crust, forming brownish scabs before new crops emerge. The rash on the hands and feet can significantly impair function and quality of life, with the visual evidence clearly demonstrating the chronic and relapsing nature of this specific psoriatic rash.
Erythrodermic psoriasis rash images present a strikingly different and severe picture: near-total body redness and inflammation, often covering 75-90% or more of the skin surface. The skin appears uniformly fiery red, shedding scales in large sheets. This widespread rash is accompanied by intense itching, burning, and pain, as well as systemic symptoms such as fever, chills, and widespread edema (swelling), particularly in the extremities. The skin barrier is severely compromised, leading to significant fluid and heat loss, which can result in dehydration and electrolyte imbalances. The visual impact of this rash is one of profound skin illness, distinctly different from other widespread rashes due to its intensity, generalized nature, and the extensive shedding. Pictures of erythrodermic psoriasis clearly illustrate the severity and urgency of this condition, where the entire skin surface acts as a compromised inflammatory organ, underscoring the critical need for immediate medical attention. The diversity of these Skin rash Psoriasis images underscores the importance of a comprehensive visual library for understanding the varied and complex manifestations of psoriasis.
Psoriasis Treatment
Psoriasis treatment strategies are diverse, aiming to reduce inflammation, slow skin cell growth, and alleviate symptoms, significantly improving the quality of life for individuals with various Psoriasis symptoms pictures. The choice of treatment depends on the severity, type, location of psoriasis, and individual patient factors. A multi-faceted approach often involves topical medications, phototherapy, systemic medications, and biologic therapies, along with lifestyle modifications.
Topical Treatments are often the first line of defense for mild to moderate psoriasis and can be used in conjunction with other therapies for more severe cases. These treatments are applied directly to the skin to target localized lesions.
- Topical Corticosteroids: These are powerful anti-inflammatory agents that reduce redness, swelling, and itching. They come in various strengths (low, medium, high, and super-high potency). Stronger corticosteroids are used for thicker plaques on the body, while milder ones are reserved for sensitive areas like the face, groin, and skin folds. Examples include clobetasol, betamethasone, fluocinonide, triamcinolone, and hydrocortisone. Prolonged or inappropriate use of potent corticosteroids can lead to side effects such as skin thinning (atrophy), stretch marks (striae), telangiectasias (spider veins), and hypopigmentation. Careful application as prescribed is crucial to minimize these risks.
- Vitamin D Analogues: Calcipotriene (calcipotriol) and calcitriol are synthetic forms of vitamin D that help slow down skin cell growth and reduce inflammation. They are effective for plaque psoriasis and can be used alone or in combination with topical corticosteroids, often enhancing efficacy and reducing steroid-related side effects. Calcipotriene is available in creams, ointments, foams, and solutions, while calcitriol is an ointment. Common side effects include skin irritation, burning, and stinging at the application site.
- Topical Retinoids (Tazarotene): This vitamin A derivative normalizes abnormal cell growth and reduces inflammation. Tazarotene is available as a cream or gel and is effective for plaque psoriasis. It can cause skin irritation, redness, and photosensitivity, making sun protection essential during treatment. It is also contraindicated in pregnancy due to potential teratogenic effects.
- Calcineurin Inhibitors (Tacrolimus and Pimecrolimus): These are non-steroidal options primarily used for psoriasis in sensitive areas such as the face, intertriginous regions, and genital areas, where corticosteroids might cause more adverse effects. They work by suppressing the local immune response. Side effects can include temporary burning or itching at the application site.
- Coal Tar: An ancient treatment derived from coal, coal tar has anti-inflammatory, anti-itch, and anti-proliferative properties. It is available in various formulations, including shampoos, creams, lotions, and bath solutions. While effective, it can be messy, have a strong odor, and stain clothing and bedding. Side effects include folliculitis and skin irritation, and it can increase sun sensitivity.
- Anthralin: A potent topical medication used for chronic plaque psoriasis, particularly thicker plaques. It works by inhibiting cell proliferation and reducing inflammation. Anthralin is typically used in a “short-contact” therapy regimen (applied for 10-30 minutes and then washed off) to minimize irritation and staining. It is known to stain skin, hair, and fabric a purplish-brown color and can cause significant irritation if not used correctly.
- Salicylic Acid: A keratolytic agent that helps soften and remove scales, making other topical medications more effective. It is often used in combination with corticosteroids or coal tar. High concentrations can cause irritation, and caution is needed when applying over large body areas due to potential systemic absorption, especially in children.
- Emollients and Moisturizers: While not directly treating the underlying immune process, regular application of thick emollients and moisturizers is crucial for managing psoriasis. They help hydrate the skin, reduce dryness, cracking, itching, and improve the skin barrier function. They can also aid in softening scales, making them easier to remove and enhancing the penetration of other topical treatments.
Phototherapy (Light Therapy) involves exposing the skin to specific wavelengths of ultraviolet (UV) light under medical supervision. It is a common and effective treatment for moderate to severe psoriasis, especially when topical treatments are insufficient or psoriasis is widespread.
- Narrowband UVB (NBUVB): This is the most common form of phototherapy. It uses a specific wavelength of UVB light (311-313 nm) that is very effective at slowing down skin cell growth and reducing inflammation with fewer side effects than broadband UVB. Treatment usually involves 2-3 sessions per week until clearance, followed by maintenance therapy if needed. Side effects include temporary redness, itching, dryness, and potential long-term risks such as photoaging and an increased risk of skin cancer, though this risk is generally considered low with NBUVB.
- Broadband UVB (BBUVB): Uses a wider range of UVB light. While effective, it carries a higher risk of burns and is generally less favored than NBUVB due to a higher erythemogenic (redness-inducing) potential.
- PUVA (Psoralen plus UVA): This therapy combines a light-sensitizing medication called psoralen (taken orally or applied topically via a bath) with exposure to UVA light. Psoralen makes the skin more sensitive to UVA, allowing for deeper penetration and greater efficacy. PUVA is very effective for severe and resistant psoriasis, including palmoplantar psoriasis. However, it carries more significant side effects, including nausea (from oral psoralen), increased photosensitivity (requiring protective eyewear and sun avoidance for 24 hours), and a higher long-term risk of skin aging, cataracts, and skin cancer (especially squamous cell carcinoma) compared to UVB therapy.
- Excimer Laser: This targeted form of phototherapy delivers high-intensity narrowband UVB light to specific psoriatic plaques, sparing healthy skin. It is ideal for localized, resistant patches of psoriasis and can achieve faster clearance with fewer total UV exposures.
Systemic Medications (Oral or Injectable) are prescribed for moderate to severe psoriasis or psoriatic arthritis that has not responded to topical treatments or phototherapy. These medications work throughout the body to suppress the immune system or specific inflammatory pathways.
- Methotrexate: An immunosuppressant that works by inhibiting cell proliferation and having anti-inflammatory effects. It is highly effective for severe plaque psoriasis and psoriatic arthritis. Administered once weekly (oral or injectable), it requires careful monitoring of liver function, kidney function, and blood counts due to potential side effects such as gastrointestinal upset, liver toxicity, bone marrow suppression, and lung toxicity. Folic acid supplementation is usually co-administered to reduce some side effects.
- Cyclosporine: A potent immunosuppressant that rapidly suppresses the immune system. It is often used for severe, acute flares of psoriasis or for patients who require quick clearance. Cyclosporine is highly effective but associated with significant side effects, including nephrotoxicity (kidney damage), hypertension (high blood pressure), and increased risk of infections. Regular blood pressure and kidney function monitoring are essential, and its use is typically limited to shorter courses.
- Acitretin: An oral retinoid (vitamin A derivative) that normalizes skin cell growth and differentiation. It is particularly useful for pustular and erythrodermic psoriasis, but also effective for severe plaque psoriasis. Side effects include dryness of the skin, lips, and eyes, hair thinning, elevated blood lipids (cholesterol and triglycerides), and liver enzyme elevations. Acitretin is highly teratogenic, meaning it can cause severe birth defects, and women of childbearing potential must avoid pregnancy for at least three years after discontinuing the medication.
- Apremilast (Otezla): An oral phosphodiesterase-4 (PDE4) inhibitor that modulates intracellular inflammation. It is used for moderate plaque psoriasis and psoriatic arthritis. Apremilast offers a more favorable safety profile compared to traditional systemic agents, though common side effects include gastrointestinal issues (nausea, diarrhea), headache, and weight loss. It does not require intensive laboratory monitoring.
Biologic Therapies represent a significant advancement in psoriasis treatment, targeting specific components of the immune system that drive inflammation in psoriasis. These are typically administered via injection or intravenous infusion and are reserved for moderate to severe psoriasis and psoriatic arthritis, especially when other treatments have failed or are contraindicated.
- TNF-alpha Inhibitors: This class of biologics blocks tumor necrosis factor-alpha (TNF-alpha), a key inflammatory cytokine. Examples include etanercept (Enbrel), infliximab (Remicade), adalimumab (Humira), and certolizumab pegol (Cimzia). They are highly effective for both skin and joint symptoms. Potential side effects include an increased risk of infections (especially tuberculosis and fungal infections), exacerbation of congestive heart failure, and rare neurological disorders. Screening for latent tuberculosis and hepatitis B is required before starting these medications.
- IL-17 Inhibitors: These biologics specifically block interleukin-17 (IL-17), another critical inflammatory cytokine. Examples include secukinumab (Cosentyx), ixekizumab (Taltz), and brodalumab (Siliq). They provide rapid and often near-complete skin clearance. Side effects may include upper respiratory tract infections and candidiasis (yeast infections).
- IL-12/23 Inhibitors: Ustekinumab (Stelara) targets both interleukin-12 and interleukin-23, modulating the inflammatory pathway. It is highly effective for plaque psoriasis and psoriatic arthritis. Side effects are generally mild but can include infections and headache. Screening for TB is also required.
- IL-23 Inhibitors: A newer class of biologics that selectively blocks interleukin-23. Examples include guselkumab (Tremfya), risankizumab (Skyrizi), and tildrakizumab (Ilumya). These offer high efficacy and prolonged dosing intervals, often achieving high rates of skin clearance. Common side effects include upper respiratory infections and headache, with a similar infection risk profile to other biologics.
Lifestyle Modifications & Complementary Approaches play a supportive role in managing psoriasis symptoms and improving overall well-being.
- Stress Management: Stress is a known trigger for psoriasis flares. Techniques such as meditation, yoga, mindfulness, and regular exercise can help manage stress levels and potentially reduce disease activity.
- Diet and Nutrition: While no specific “psoriasis diet” exists, maintaining a healthy weight through a balanced diet rich in fruits, vegetables, lean proteins, and omega-3 fatty acids can be beneficial. Some individuals report improvement with anti-inflammatory diets or by avoiding certain trigger foods, though scientific evidence is often limited. Weight loss can significantly improve the response to psoriasis treatments in overweight or obese individuals.
- Avoiding Triggers: Identifying and avoiding known triggers such as smoking, excessive alcohol consumption, certain medications (e.g., beta-blockers, lithium, antimalarials), and skin injuries can help prevent flares.
- Regular Moisturizing: Consistent use of emollients and moisturizers, even when the skin is clear, helps maintain skin barrier function, reduce dryness, and minimize itching, supporting overall skin health.
- Controlled Sun Exposure: Brief, controlled exposure to natural sunlight can sometimes improve psoriasis lesions, similar to phototherapy. However, excessive sun exposure can lead to sunburns, which can trigger the Koebner phenomenon and increase skin cancer risk. Consultation with a dermatologist is recommended for appropriate guidance.
The comprehensive Psoriasis treatment landscape offers numerous options, from localized topical applications to advanced biologic therapies, ensuring that individuals with varying Psoriasis symptoms pictures can find an effective management strategy to achieve significant clearance and improve their quality of life.