Recognizing potential changes in your skin is crucial for early detection. This article provides detailed descriptions of various skin cancer symptoms pictures, offering guidance on what to look for when examining your skin for any suspicious growths or lesions.
Skin cancer Symptoms Pictures
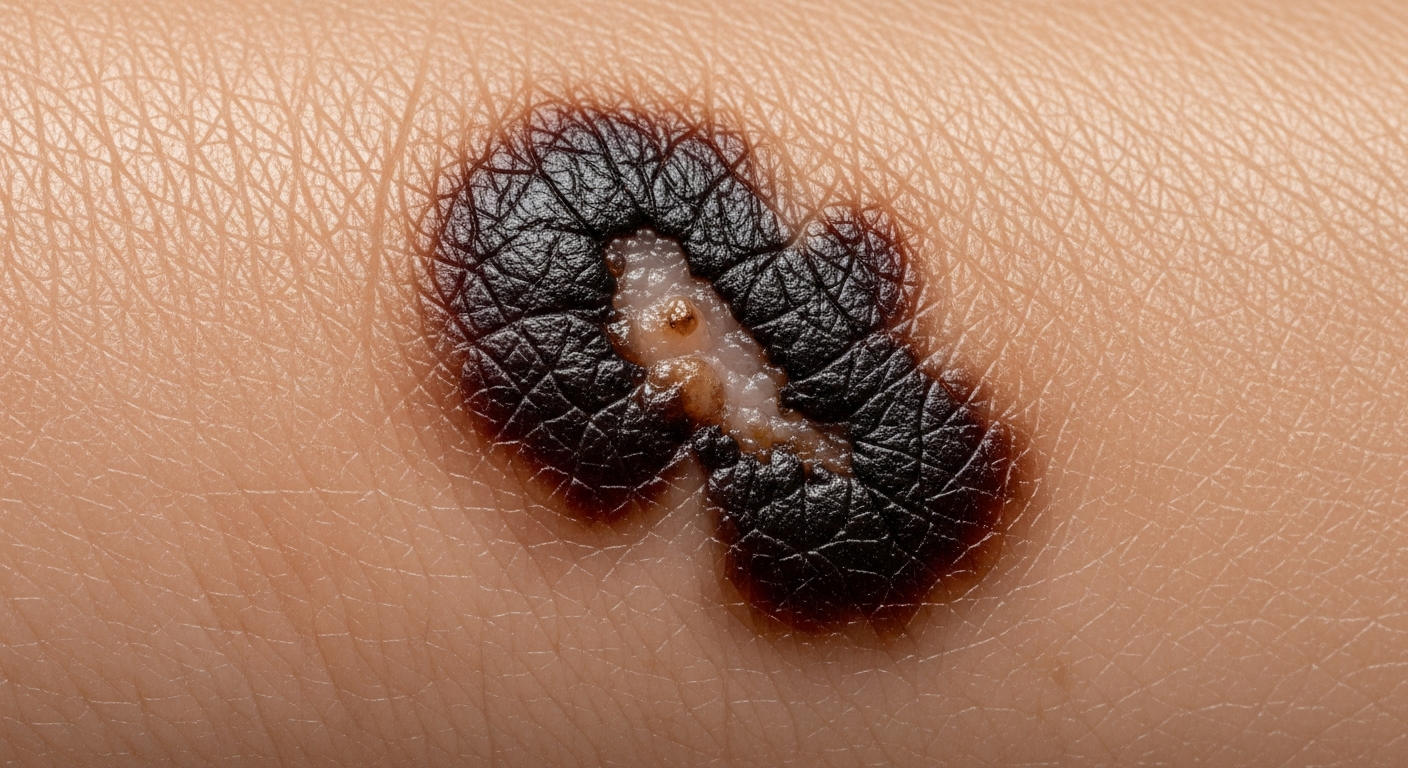
Understanding the visual characteristics of skin cancer is paramount for early identification. When reviewing skin cancer symptoms pictures, it’s vital to pay close attention to the details of any new or changing lesions on your skin. These symptoms can vary significantly depending on the type of skin cancer, including melanoma, basal cell carcinoma (BCC), and squamous cell carcinoma (SCC), but common visual cues often provide critical warning signs.
For melanoma symptoms pictures, the primary focus is on moles or new pigmented growths that exhibit asymmetry, irregular borders, varied color, a diameter greater than 6mm, or evolution over time (the ABCDEs). Detailed observation of these characteristics is essential:
- Asymmetry: If you draw a line through the middle of the lesion, the two halves do not match. One side may be noticeably larger, a different shape, or have distinct color variations compared to the other.
- Border Irregularity: The edges of the lesion are often jagged, notched, blurred, or scalloped, rather than smooth and well-defined. This unevenness is a strong indicator.
- Color Variation: The lesion displays multiple colors within a single mole, such as shades of brown, black, tan, white, red, or blue. Patches of lighter or darker pigmentation within the same lesion are highly suspicious.
- Diameter: Melanomas are typically larger than 6 millimeters (about the size of a pencil eraser) when diagnosed, though they can be smaller. Rapid growth in size is also a significant concern.
- Evolution: Any change in size, shape, color, elevation, or any new symptom like bleeding, itching, or crusting. This is arguably the most important sign, as it indicates a dynamic process. The mole may also become noticeably firmer or bumpier.
In addition to the ABCDEs, other visual melanoma warning signs include:
- New pigmented lesion appearing spontaneously.
- Existing mole that starts to itch, bleed, or become tender without trauma.
- A lesion that feels different to the touch, such as becoming scaly, crusty, or oozing.
- A dark streak under a fingernail or toenail (subungual melanoma) not caused by trauma.
- A dark spot on the palm of the hand or sole of the foot (acral lentiginous melanoma), especially in individuals with darker skin tones where it’s more common.
- A lesion that looks like an open sore but doesn’t heal within a few weeks.
- A firm, raised, and dome-shaped lesion that may be black, blue, or red (nodular melanoma).
For basal cell carcinoma (BCC) pictures, the visual symptoms often present differently. BCC is the most common type of skin cancer and typically grows slowly. Key visual indicators of BCC include:
- Pearly or Waxy Bump: A small, dome-shaped growth that is often translucent, appearing pearly white or pink. Blood vessels (telangiectasias) may be visible within the bump.
- Open Sore: A lesion that bleeds, oozes, or crusts and remains open for weeks, failing to heal, or healing and then recurring. This can be particularly indicative of an ulcerated BCC.
- Reddish Patch: A flat, scaly, reddish patch that may be itchy or slightly tender. This presentation is common in superficial BCC, often mistaken for eczema or psoriasis.
- Pink Growth with Rolled Border: A slightly elevated growth with a rolled, pearly border and an indented center. This often resembles a classic nodular BCC.
- Scar-Like Area: A white, waxy, scar-like lesion without a clearly defined border (morpheaform BCC). This type is often subtle and can be more invasive beneath the skin’s surface.
- Dark Lesion: Less commonly, BCCs can be pigmented, appearing brown, black, or blue, sometimes resembling melanoma, especially in darker skin types.
Squamous cell carcinoma (SCC) visual symptoms are also distinct and crucial to identify. SCC is the second most common type of skin cancer and can be more aggressive than BCC if left untreated. Look for:
- Firm, Red Nodule: A firm, red, often scaly or crusted lump that can grow rapidly. This is a common presentation for invasive SCC.
- Flat, Scaly Patch: A flat, reddish patch with an irregular border that is prone to bleeding and crusting. This can represent Bowen’s disease (SCC in situ).
- Open Sore: A persistent sore that doesn’t heal, or heals and reopens, often with a raised, firm edge.
- Wart-like Growth: A rough, wart-like lesion that may bleed easily, especially in sun-exposed areas. These can sometimes be painful.
- Crusted or Ulcerated Area: A lesion with a central depression that may be crusted or ulcerated, surrounded by a raised border.
It’s important to remember that these skin cancer pictures and descriptions are guidelines. Any new growth, mole, bump, patch, or sore that doesn’t heal, or any change in an existing skin lesion, warrants immediate medical evaluation by a dermatologist. Early detection is a cornerstone of successful skin cancer treatment outcomes.
Signs of Skin cancer Pictures
Identifying the distinct signs of skin cancer through visual inspection is a critical step in preventing advanced disease. When looking at signs of skin cancer pictures, one must be attuned to subtle differences in skin texture, color, and growth patterns. These visual cues are often the first indication that something is amiss, prompting further investigation. It is not just about identifying a “spot” but understanding the specific characteristics that elevate a lesion from benign to suspicious.
For melanoma warning signs, the “ugly duckling” sign is often as important as the ABCDE criteria. This refers to a mole that looks distinctly different from the surrounding moles on an individual’s skin. If a particular mole stands out as unique in its color, size, or shape compared to others, it should be considered suspicious. Specific visual hallmarks of melanoma, often seen in diagnostic images, include:
- Multicolor Presentation: Lesions exhibiting a mosaic of colors such as varying shades of brown, black, red, white, or blue. For example, a mole might have a very dark black center, a lighter brown periphery, and a reddish hue at one edge.
- Irregularity in Shape: Rather than a round or oval shape, melanomas often present with an unpredictable, uneven outline. This could involve projections, indentations, or a generally chaotic shape.
- Surface Changes: A previously flat mole that begins to become raised, bumpy, scaly, or crusty. The texture may feel different to touch, rougher or harder than surrounding skin.
- Bleeding or Oozing: Any mole that spontaneously bleeds, oozes fluid, or develops a scab without being scratched or injured is a significant warning sign.
- Itching or Tenderness: Persistent itching, burning, or tenderness in a mole that was previously asymptomatic. These sensory changes often accompany structural changes.
- Inflammation: Redness or swelling surrounding a mole, indicating irritation or an inflammatory response.
- Ulceration: The formation of an open sore or crater within a mole, which may or may not heal.
- Satellite Lesions: Small, new moles or dark spots that appear around an existing larger mole, suggesting spread.
- Rapid Growth: A mole that shows a noticeable increase in size over a period of weeks or months. Measuring and tracking moles can be very useful.
For basal cell carcinoma signs, the visual clues are often related to surface characteristics and the lesion’s interaction with the surrounding skin. These lesions rarely metastasize but can be locally destructive if not treated. Common presentations include:
- Pearly Nodule with Rolled Border: This is the classic presentation. A small, shiny, firm nodule, often with a raised, translucent border and fine blood vessels (telangiectasias) visible on its surface. The center may be slightly depressed or crusted.
- Non-Healing Sore: A lesion that looks like a cut, scratch, or sore that refuses to heal, or repeatedly heals and breaks open again. It might be slightly tender or itchy.
- Shiny Patch or Scar-like Area: Particularly for morpheaform BCC, the lesion may appear as a flat, firm, pale yellow or white patch that resembles a scar. These lesions often have ill-defined borders and can be more extensive below the surface.
- Reddish, Dry Patch: For superficial BCC, a slightly scaly, reddish-brown patch that may appear similar to eczema or a persistent dry skin patch. It often has a fine, thread-like border.
- Pigmented Basal Cell Carcinoma: A less common variant that appears dark brown, black, or blue, often with irregular pigmentation and a pearly border, potentially mimicking melanoma.
- Erosion or Ulceration: The central part of the lesion may break down, forming an ulcer, particularly in larger or older lesions.
Squamous cell carcinoma signs are diverse and can range from subtle to overtly aggressive. These growths often occur on sun-exposed areas. Key visual indicators include:
- Crusted, Scaly Patch: A persistent, reddish, scaly patch that may be tender or bleed easily, particularly when scraped or bumped. This can be an early form (Bowen’s disease) or more invasive.
- Firm, Red Nodule: A raised, firm, often tender or painful bump that can be red or flesh-colored. The surface may be rough, scaly, or wart-like.
- Open Sore with Raised Border: A sore that doesn’t heal, often with a crusty surface and an elevated, firm margin. These ulcers can become quite deep.
- Wart-like Growth: A rough, lumpy growth that resembles a wart, often with a central depression or ulceration. These can be particularly concerning if they grow rapidly.
- Horny Projections: In some cases, SCC can present as a cutaneous horn, a conical projection of keratinized material that can be quite pronounced.
- Induration: The area around the lesion feels hard or firm to the touch, indicating deeper tissue involvement.
- Rapid Growth: Unlike many BCCs, SCCs can grow quite quickly, sometimes doubling in size over a few months.
When examining skin cancer pictures for diagnostic purposes, it’s crucial to look for combinations of these signs rather than relying on a single symptom. Self-examinations, coupled with regular professional skin checks, are vital for detecting these signs early. Remember, persistent changes or any new, unusual growth should always be evaluated by a dermatologist promptly to ensure accurate diagnosis and timely treatment.
Early Skin cancer Photos
Detecting early skin cancer symptoms through images is often challenging but profoundly important for treatment success. Early skin cancer photos highlight the subtle initial manifestations of these diseases, which can easily be overlooked or mistaken for benign conditions. Recognizing these initial visual cues requires a keen eye and an understanding of what distinguishes a nascent cancerous lesion from ordinary skin blemishes. The focus in early detection is on identifying changes at their smallest and least invasive stages.
When observing early melanoma pictures, the changes are often subtle evolutions of existing moles or the appearance of new, slightly atypical pigmented lesions. These early signs might not yet fully satisfy all the ABCDE criteria but should still raise suspicion:
- Subtle Asymmetry: One half of a mole might be slightly larger or a different shape than the other, without being overtly asymmetrical.
- Slightly Irregular Border: The edges may have very slight notching or be somewhat fuzzy rather than perfectly smooth and round.
- Minor Color Variation: A mole might show only two shades of brown or the beginning of a darker speck within a uniformly colored lesion.
- Small but Changing Diameter: A mole that is still under 6mm but has shown a measurable increase in size over a few weeks or months.
- New Onset Itching or Tenderness: A mole that recently started to itch mildly or feel slightly sensitive, even without noticeable visible changes.
- New, Small Pigmented Spot: The appearance of a new dark spot on the skin that wasn’t there before, even if it’s small and appears benign initially. These should always be monitored closely.
- Changes in Texture: A previously smooth mole developing a very fine, granular texture or becoming slightly elevated in one area.
- “Ugly Duckling” in Miniature: A new mole that, despite its small size, simply looks different or more suspicious than your other moles.
Early basal cell carcinoma (BCC) photos often reveal very small, often barely noticeable lesions that can be subtle. They typically appear on sun-exposed areas like the face, neck, and hands. Key early indicators include:
- Tiny, Pearly Bump: A very small (1-2mm), shiny, translucent bump, often mistaken for a pimple that won’t go away. It might have a faint pink or flesh tone and a hint of a rolled edge.
- Small, Persistent Sore: A tiny sore or scratch that appears, might scab over, and then reopens repeatedly, failing to heal within a few weeks. It might bleed easily with minor trauma.
- Flat, Reddish Spot: A small, slightly scaly, pink or red patch that might be asymptomatic or slightly itchy. This is particularly relevant for superficial BCC and can be confused with dry skin or a benign rash.
- Scar-like Pinprick: A very small, white or yellowish, slightly depressed area that looks like a miniature scar, even without any previous injury. This is a subtle sign of morpheaform BCC.
- Visible Micro-Vessels: The appearance of one or two very fine, thread-like blood vessels (telangiectasias) on the surface of a small, slightly raised lesion.
Early squamous cell carcinoma (SCC) images can show lesions that are also deceptively innocent-looking, often resembling common benign skin conditions. SCC typically arises on areas with significant sun exposure or chronic inflammation. Early signs include:
- Small, Rough Patch: A small, persistent red or brownish-red scaly patch or plaque that feels rough to the touch. It may resemble actinic keratosis (a precancerous lesion).
- Tender, Firm Bump: A small, firm, red bump that might be slightly tender or painful when touched. It may have a central depression or be covered by a crust.
- Non-Healing Pimple or Wart: A lesion that looks like an inflamed pimple or a small wart that doesn’t resolve with standard treatments and continues to persist or grow.
- Persistent Sore: A small, ulcerated lesion that bleeds easily and doesn’t heal, often with a firm, slightly raised border.
- Actinic Keratosis Progression: An existing actinic keratosis that becomes noticeably thicker, more inflamed, or begins to ulcerate. While AKs are precancerous, some can evolve into SCC.
- Small Cutaneous Horn: A small, conical projection of hard, keratinized skin, often sitting on a reddish base.
The term “precancerous lesions” is also vital in early detection, as these are conditions that can develop into skin cancer over time. The most common precancerous lesion is actinic keratosis (AK). Early pictures of AKs typically show:
- Small, rough, dry, or scaly patches on sun-exposed skin.
- Color can range from skin-colored to red or brown.
- Often feel like sandpaper when rubbed.
- Can be easier to feel than to see.
- Multiple lesions are common.
Early identification of these lesions allows for simpler and less invasive treatments, often preventing the progression to full-blown skin cancer. Regular self-skin exams, knowing your skin, and consulting a dermatologist for any suspicious changes are the most effective strategies for catching skin cancer at its earliest, most treatable stages. Pay close attention to any changes in existing moles or the appearance of new, unusual spots, especially on sun-exposed skin.
Skin rash Skin cancer Images
Distinguishing between a benign skin rash and a potentially malignant skin cancer lesion is a significant diagnostic challenge, even for experienced dermatologists. Many skin cancers, especially in their early stages, can visually mimic common inflammatory skin conditions, making the interpretation of skin rash skin cancer images particularly complex. Understanding the nuanced differences and red flag signs is critical for correct diagnosis and timely intervention. The key lies in observing persistence, evolution, and specific morphological features that differentiate cancer from inflammation.
Some skin cancers can present with a rash-like appearance. These include, but are not limited to:
- Superficial Basal Cell Carcinoma (sBCC): Often appears as a flat, reddish, scaly patch, resembling eczema, psoriasis, or a fungal infection. It may be slightly itchy or asymptomatic. Unlike a typical rash, an sBCC patch tends to persist in one spot, resist standard rash treatments, and may have a fine, thread-like, pearly border if examined closely. It can also have subtle erosions or fine crusting.
- Bowen’s Disease (Squamous Cell Carcinoma in situ): This is an early, non-invasive form of SCC confined to the epidermis. It typically presents as a slowly enlarging, persistent, reddish-brown, scaly patch or plaque with an irregular border. It often mimics eczema, psoriasis, or ringworm. Key differentiating features include its chronicity in a single location, lack of response to anti-inflammatory creams, and sometimes a slightly indurated or raised feel at the periphery.
- Cutaneous T-cell Lymphoma (CTCL), specifically Mycosis Fungoides: This is a rare form of non-Hodgkin lymphoma that primarily affects the skin. Early stages can be highly polymorphic and rash-like.
- Patches: Reddish-brown, scaly patches that can be itchy, often appearing on sun-protected areas like the buttocks or inner thighs. These patches might wax and wane but rarely disappear completely.
- Plaques: Thicker, raised, scaly lesions that can be linear or annular. These can mimic psoriasis or chronic eczema.
- Erythroderma: In advanced stages, widespread redness and scaling affecting most of the body, resembling severe eczema or psoriasis.
Differentiating CTCL from benign rashes relies on biopsy and specialized staining, as visual distinction alone is often impossible. The chronicity, unusual locations for common rashes, and resistance to standard therapies are red flags.
- Amelanotic Melanoma: While less common, this aggressive form of melanoma lacks pigment, making it appear pink, red, or flesh-colored. It can be mistaken for a benign rash, a cyst, a pimple, or a patch of dermatitis. Amelanotic melanoma is characterized by its rapid growth, potential for bleeding or ulceration, and often an irregular shape and border, though these might be subtle without pigment. Its evolutionary nature is a key indicator.
- Merkel Cell Carcinoma: A rare but aggressive neuroendocrine skin cancer. It can sometimes present as a rapidly growing, firm, flesh-colored to red or purplish nodule that may be asymptomatic. While not typically “rash-like,” its initial presentation can be subtle and mistaken for a cyst or an inflamed area before rapid growth becomes apparent.
When encountering rash-like skin lesions, consider the following differentiating factors:
- Persistence: Benign rashes typically respond to treatment (e.g., topical steroids, antifungals) or resolve on their own within a few weeks. Skin cancers, particularly those mimicking rashes, persist indefinitely in one spot, despite appropriate management for common skin conditions.
- Location: While rashes can occur anywhere, certain skin cancers have predilections for sun-exposed areas (BCC, SCC, melanoma) or sun-protected areas (CTCL patches).
- Evolution: Rashes typically have a more generalized or spreading pattern. Cancerous lesions are usually fixed in one location and may show subtle but continuous changes in size, shape, color, or texture over time.
- Symptoms: While itching is common in rashes, persistent, localized itching, burning, or tenderness in a single lesion that doesn’t fit a typical rash pattern should raise suspicion. Bleeding or oozing without trauma is a significant red flag for cancer.
- Texture: Cancerous lesions, even when rash-like, may have a subtle induration (firmness) or thickening compared to the surrounding skin, which is less common with most benign rashes.
- Border Definition: While some rashes have distinct borders, many cancerous lesions, especially superficial BCC or Bowen’s disease, can have irregular or slightly raised borders that are not typical of inflammatory conditions.
- Absence of Symmetry/Conformity: Benign inflammatory rashes often appear symmetrically or conform to skin folds. Cancerous lesions are often solitary or present in an asymmetrical pattern.
The interpretation of skin cancer vs. rash images requires a high index of suspicion. Any persistent, non-healing, or evolving skin lesion, especially one that doesn’t respond to conventional treatments for rashes, must be evaluated by a dermatologist. Biopsy remains the gold standard for definitive diagnosis when there is uncertainty, providing clarity where visual assessment alone is insufficient. Do not self-diagnose based solely on skin cancer symptom pictures; professional medical evaluation is essential.
Skin cancer Treatment
Once a diagnosis of skin cancer has been confirmed through biopsy, a comprehensive treatment plan is developed, tailored to the specific type of cancer, its stage, location, and the patient’s overall health. Skin cancer treatment strategies aim to remove or destroy cancerous cells while preserving as much healthy tissue as possible and minimizing scarring. The choice of treatment modality is influenced by whether it is melanoma, basal cell carcinoma (BCC), or squamous cell carcinoma (SCC), and whether the cancer is early-stage, advanced, or metastatic. Understanding the various options for skin cancer treatment is crucial for patients and caregivers.
Treatment for Basal Cell Carcinoma (BCC) and Squamous Cell Carcinoma (SCC)
BCC and SCC are generally treated with local therapies, as they are less likely to metastasize than melanoma, especially when detected early. Common BCC and SCC treatment options include:
- Surgical Excision: This is a very common and highly effective treatment. The surgeon cuts out the cancerous tumor along with a surrounding margin of healthy skin (called the surgical margin). The removed tissue is then examined under a microscope to ensure all cancer cells have been removed. This procedure is performed under local anesthesia for most cases.
- Mohs Micrographic Surgery: Considered the gold standard for high-risk BCCs and SCCs, especially those on the face, ears, neck, hands, feet, or genitals, or those that are large, recurrent, or aggressive. In Mohs surgery, the surgeon removes thin layers of skin containing cancer, one layer at a time. Each layer is immediately examined under a microscope until no cancer cells remain. This method spares the maximum amount of healthy tissue and has very high cure rates.
- Curettage and Electrodesiccation (C&E): Often used for superficial BCCs and small, low-risk SCCs. The tumor is scraped away with a sharp, spoon-shaped instrument (curette), and the base of the wound is then cauterized with an electric needle to destroy remaining cancer cells and stop bleeding. This process is usually repeated multiple times.
- Radiation Therapy: Used for patients who cannot undergo surgery due to age, poor health, or the location of the tumor (e.g., eyelids, nose, or ears). It can also be used for large tumors or when surgery might result in unacceptable cosmetic outcomes. Radiation therapy uses high-energy beams to destroy cancer cells. It typically involves multiple sessions over several weeks.
- Cryosurgery (Freezing): Involves applying liquid nitrogen to the tumor to freeze and destroy the cancer cells. This is suitable for small, superficial BCCs and SCCs, and precancerous lesions like actinic keratoses. It often results in a blister that eventually scabs and falls off.
- Topical Chemotherapy (e.g., 5-Fluorouracil cream): Applied directly to the skin, this cream is effective for superficial BCCs and widespread actinic keratoses. It works by killing rapidly dividing cancer cells. Treatment typically lasts several weeks and causes inflammation, redness, and crusting.
- Photodynamic Therapy (PDT): Involves applying a light-sensitizing medication to the skin, which is then activated by a specific type of light. This process creates oxygen radicals that destroy cancer cells. PDT is effective for superficial BCCs and actinic keratoses, often causing temporary redness and swelling.
- Imiquimod Cream: An immune-modulating cream that stimulates the body’s immune system to attack cancer cells. It is approved for superficial BCCs and some actinic keratoses. It is applied several times a week for an extended period, leading to an inflammatory response.
- Systemic Therapy (for advanced BCC/SCC): For very advanced or metastatic BCC or SCC (which is rare), targeted therapies like hedgehog pathway inhibitors (e.g., vismodegib, sonidegib for BCC) or immunotherapy (e.g., pembrolizumab, cemiplimab for SCC) may be used. These treatments target specific molecular pathways in cancer cells or boost the body’s immune response against the cancer.
Treatment for Melanoma
Melanoma is potentially more aggressive and requires a more extensive treatment approach, often involving a combination of therapies. Melanoma treatment options are determined by the stage of the cancer and its spread:
- Surgical Excision: The primary treatment for most melanomas. The tumor is removed with a wider margin of healthy-appearing skin compared to BCC/SCC, the width of which depends on the melanoma’s thickness (Breslow depth).
- Wide Local Excision: Standard surgical procedure to remove the melanoma and a safety margin of normal-looking skin.
- Lymph Node Biopsy: For thicker melanomas, a sentinel lymph node biopsy may be performed to check if cancer cells have spread to nearby lymph nodes. If the sentinel node is positive, a complete lymph node dissection might be recommended.
- Immunotherapy: A revolutionary treatment that harnesses the body’s immune system to fight cancer. These drugs (e.g., nivolumab, pembrolizumab, ipilimumab) are used for advanced or metastatic melanoma and sometimes as adjuvant therapy after surgery to reduce the risk of recurrence. They work by blocking “checkpoint” proteins that normally keep immune cells from attacking cancer.
- Targeted Therapy: For melanomas with specific genetic mutations (e.g., BRAF mutations, common in about half of all melanomas), targeted drugs (e.g., dabrafenib, vemurafenib, encorafenib, trametinib, cobimetinib, binimetinib) can block the activity of these abnormal proteins, leading to tumor shrinkage. These are used for advanced or metastatic melanoma.
- Radiation Therapy: May be used after surgery to kill any remaining cancer cells, especially if lymph nodes were involved or there’s a high risk of recurrence. It can also be used to treat metastatic melanoma in specific areas, such as the brain or bones, to alleviate symptoms.
- Chemotherapy: Less commonly used for melanoma now due to the effectiveness of immunotherapy and targeted therapy, but it may be considered for certain advanced cases or when other treatments are not suitable. It uses powerful drugs to kill cancer cells throughout the body.
- Oncolytic Virus Therapy (e.g., Talimogene Laherparepvec – T-VEC): This involves injecting a modified virus directly into melanoma tumors, causing the cancer cells to burst and also stimulating an immune response against the cancer. It is approved for certain unresectable melanomas that have not spread widely.
General Considerations for Skin Cancer Treatment
- Staging: Before treatment, the cancer is staged (0-IV) to determine its extent and guide treatment decisions.
- Multidisciplinary Approach: Treatment planning often involves a team of specialists, including dermatologists, surgical oncologists, radiation oncologists, and medical oncologists.
- Follow-up Care: Regular follow-up appointments are crucial after treatment to monitor for recurrence, detect new primary cancers, and manage any long-term side effects. This includes frequent skin self-examinations and professional skin checks.
- Sun Protection: Regardless of the type of skin cancer, strict sun protection measures (sunscreen, protective clothing, seeking shade) are vital to prevent new cancers and recurrences.
- Clinical Trials: For advanced cases or when standard treatments are ineffective, participation in clinical trials offering novel therapies may be an option.
The choice of skin cancer treatment is highly individualized and depends on numerous factors, including the patient’s age, overall health, the specific characteristics of the tumor, and the potential side effects of treatment. A thorough discussion with a healthcare provider is essential to determine the most appropriate and effective course of action for each unique situation.