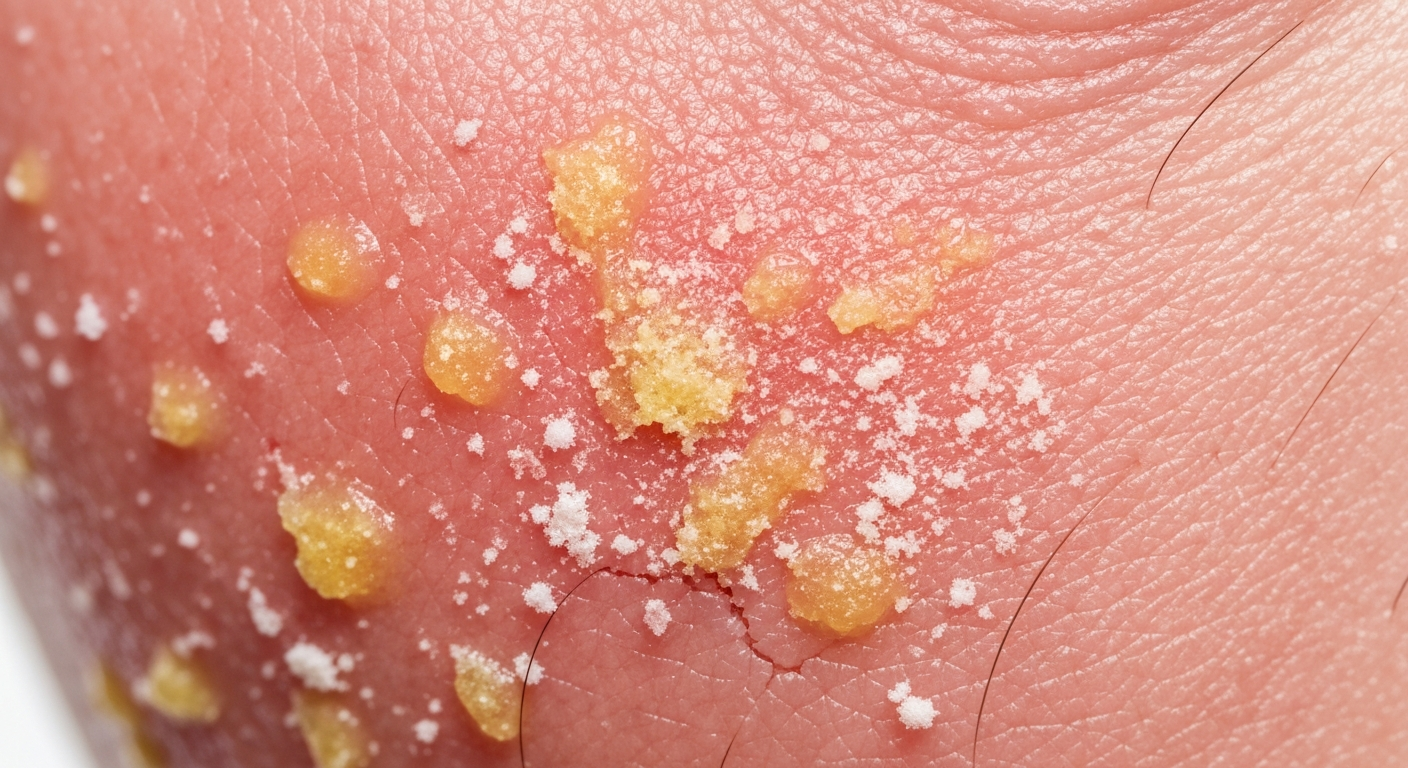
Identifying Seborrheic dermatitis symptoms pictures is crucial for understanding this common skin condition. This article provides a detailed visual guide and symptom descriptions to help in recognizing the various presentations of seborrheic dermatitis across different body areas and stages of development.
Seborrheic dermatitis Symptoms Pictures
Seborrheic dermatitis symptoms pictures often reveal a distinctive pattern of inflammation and scaling on oily areas of the body. These symptoms are not just visual; they are accompanied by specific sensations that patients experience. The presentation can vary significantly based on skin type, location, and the severity of the condition, making a detailed visual and descriptive understanding vital. When examining seborrheic dermatitis pictures, look for consistent features that define this chronic inflammatory disorder, which is intricately linked to the activity of sebaceous glands and the presence of Malassezia yeast.
Key visual seborrheic dermatitis symptoms include:
- Erythematous Patches: These are areas of skin redness, which can range from a faint pink blush in mild cases to a deep, inflamed crimson during active flare-ups. The intensity of the redness in seborrheic dermatitis pictures can be influenced by skin tone, often appearing more pronounced on lighter skin, while on darker skin, it might manifest as subtle purplish or grayish patches, sometimes with post-inflammatory hyperpigmentation after resolution.
- Greasy or Oily Scales: One of the most characteristic features visible in seborrheic dermatitis photos is the presence of scales. These scales are typically yellowish, greasy, and adhere to the skin surface, distinct from the drier, silvery scales seen in conditions like psoriasis. The greasiness is a direct result of the overproduction of sebum, which is a hallmark of areas affected by seborrheic dermatitis.
- Flaking Skin: Beyond the greasy scales, fine, powdery flakes of skin are commonly observed, especially on the scalp, eyebrows, and mustache area. This persistent flaking can be a source of significant distress for individuals, as it is often noticeable on clothing and furniture. The degree of flaking varies, from minimal shedding to abundant, snow-like dandruff.
- Itching (Pruritus): While not directly visible in seborrheic dermatitis symptom pictures, itching is a pervasive and often debilitating symptom. The sensation can range from mild annoyance to intense, persistent pruritus, leading to scratching that can further irritate the skin, cause excoriations, and potentially introduce secondary bacterial infections.
- Burning Sensation: In addition to itching, many individuals report a burning or stinging sensation in the affected areas. This is particularly common during acute flare-ups or when the skin is highly inflamed, indicating significant irritation and discomfort.
- Crusting: In more severe cases, or in areas prone to sweating and friction, the scales and exudate can combine to form thick, adherent crusts. These crusts are often seen on the scalp, behind the ears, or in skin folds, and can be indicative of a more advanced stage of the condition or secondary infection.
- Skin Discoloration: Post-inflammatory changes can lead to temporary changes in skin pigmentation. After the inflammation subsides, some individuals, particularly those with darker skin tones, may experience hypopigmentation (lighter patches) or hyperpigmentation (darker patches) in the affected areas.
Specific body areas often reveal distinct seborrheic dermatitis symptom pictures:
- Scalp Seborrheic Dermatitis: This is arguably the most common presentation, often referred to as dandruff when mild. Symptoms include diffuse or localized patches of redness, covered with greasy, yellowish scales. Hair follicles may appear inflamed, and hair loss can occur in severe, chronic cases due to persistent inflammation and scratching. Patients frequently observe extensive flaking that sheds onto clothing.
- Facial Seborrheic Dermatitis: On the face, symptoms primarily affect the T-zone, including the eyebrows, glabella (between the eyebrows), nasolabial folds (sides of the nose), and forehead. Facial seborrheic dermatitis pictures show redness, fine to greasy scaling, and often a shiny or oily appearance due to increased sebum production. The eyelids can also be affected, leading to seborrheic blepharitis with scaling along the lash line.
- Ear Seborrheic Dermatitis: The external ear canal, retroauricular fold (behind the ears), and within the folds of the ear are common sites. Symptoms include redness, fissures, and greasy scaling, which can sometimes lead to a foul odor if left untreated or complicated by secondary infections. Ear seborrheic dermatitis pictures often show redness and flaking in the ear crease.
- Chest and Upper Back Seborrheic Dermatitis: On the torso, especially the sternal area (center of the chest) and between the shoulder blades, seborrheic dermatitis can manifest as coin-shaped or irregularly shaped patches of redness with greasy scaling. These areas are prone to sweat and friction, which can exacerbate the condition.
- Intertriginous Seborrheic Dermatitis: This form affects skin folds such as the armpits, groin, under the breasts, and abdominal folds. Symptoms are often characterized by well-demarcated patches of redness, sometimes with maceration (softening due to moisture), minimal scaling, and a tendency to fissure or crack. Itching and burning are prominent in these areas.
Signs of Seborrheic dermatitis Pictures
The signs of seborrheic dermatitis pictures provide concrete visual evidence for diagnosis, moving beyond subjective symptoms to observable physical characteristics. These signs are crucial for differentiating seborrheic dermatitis from other dermatological conditions, such as psoriasis, rosacea, or contact dermatitis. Understanding the nuanced presentation of these signs helps in accurate identification and effective management. Seborrheic dermatitis signs are not static; they evolve over time, from subtle initial manifestations to more pronounced and widespread involvement during flare-ups.
Observable seborrheic dermatitis signs typically include:
- Well-Demarcated Erythema: The redness observed in seborrheic dermatitis images is frequently sharply defined, particularly on the face and trunk. This clear border helps distinguish affected skin from unaffected areas. The color might be a faint pink to a fiery red, often with an underlying yellowish tint due to the greasy nature of the scales.
- Yellowish, Greasy Scaling: This is a definitive sign. The scales appear less dry and powdery than typical dandruff and are often more adherent to the skin. In scalp seborrheic dermatitis pictures, these scales can mat the hair, while on the face, they might accumulate in the eyebrows or nasolabial folds, creating a visibly ‘dirty’ or unkempt appearance.
- Follicular Pustules: In some cases, particularly in areas with dense hair follicles like the scalp or beard area, small, inflammatory papules or pustules may be observed. These are often sterile but indicate a heightened inflammatory response around the hair follicles.
- Blepharitis: When seborrheic dermatitis affects the eyelids, it presents as redness, irritation, and scaling along the lash line. This condition, known as seborrheic blepharitis, can cause chronic eye irritation, a gritty sensation, and occasional loss of eyelashes. Eyelid seborrheic dermatitis pictures will show scaly margins.
- Skin Fissuring: In areas of skin folds or where the skin experiences frequent movement and moisture, such as behind the ears or in the nasolabial folds, the inflamed skin can become dry, inelastic, and crack, leading to painful fissures. These open breaks in the skin can increase the risk of secondary bacterial or fungal infections.
- Telangiectasias: Chronic inflammation, especially on the face, can sometimes lead to the development of fine, visible blood vessels (telangiectasias). This sign is more commonly associated with rosacea but can occasionally be seen in long-standing cases of facial seborrheic dermatitis.
- Cradle Cap (Infantile Seborrheic Dermatitis): A specific manifestation in infants, cradle cap pictures show thick, greasy, yellowish-brown scales and crusts primarily on the scalp. It can also extend to the forehead, eyebrows, and behind the ears. Despite its alarming appearance, it is generally benign and non-itchy in infants.
- Diffuse Hair Thinning: While not a direct sign of the skin lesion itself, persistent inflammation on the scalp, combined with scratching, can lead to increased hair shedding and diffuse hair thinning over time. This is a common concern among adults with chronic scalp seborrheic dermatitis.
Variations in seborrheic dermatitis signs based on skin tone and age:
- Skin Tone Differences: On lighter skin tones, erythema is typically more vivid and appears as distinct red patches. On darker skin tones, the redness can be less obvious, appearing as purplish, grayish, or hyperpigmented patches. The presence of scales and flaking remains a consistent sign across all skin types, but the underlying inflammation might be visually subtle, sometimes only apparent as textural changes or hyperpigmented borders.
- Age-Related Manifestations:
- Infants: As mentioned, cradle cap is the primary manifestation, but infants can also develop seborrheic dermatitis in the diaper area (often confused with candidiasis) and skin folds, showing redness with minimal scaling. Infantile seborrheic dermatitis pictures are quite distinctive.
- Children: Less common in early childhood but can appear during puberty. Similar to adult forms, often presenting on the scalp or face.
- Adults: The classic presentation with greasy scales, erythema, and itching on the scalp, face, chest, and intertriginous areas. Flare-ups are often triggered by stress, hormonal changes, or changes in weather.
- Elderly: May present with more chronic, widespread, and persistent forms. Dryness can also be a factor, sometimes masking the greasy scales. Immune compromise in older adults can lead to more severe presentations.
Recognizing these diverse signs of seborrheic dermatitis pictures is paramount for accurate diagnosis and effective management strategies, allowing clinicians to tailor treatments to the specific presentation and patient demographics.
Early Seborrheic dermatitis Photos
Early seborrheic dermatitis photos are invaluable for catching the condition in its nascent stages, allowing for prompt intervention and potentially preventing widespread flare-ups. These initial manifestations are often subtle and can easily be overlooked or mistaken for minor dry skin or simple dandruff. However, discerning these early signs is critical for effective management of early seborrheic dermatitis. The condition typically begins insidiously, with symptoms gradually escalating from mild irritation to more pronounced inflammation and scaling. Paying close attention to persistent, localized skin changes can aid in early detection.
What to look for in early seborrheic dermatitis photos:
- Subtle Scalp Redness: One of the earliest seborrheic dermatitis symptoms on the scalp might be a faint, diffuse redness that isn’t immediately obvious. This redness might be accompanied by a mild, persistent itch or a feeling of tightness. It often precedes visible scaling, especially in individuals with lighter hair or skin.
- Mild Flaking (Dandruff): The initial presentation of early seborrheic dermatitis on the scalp often begins as mild dandruff – small, dry, white flakes that shed from the scalp. While common, persistent dandruff that doesn’t respond to regular shampooing can be an early indicator. Unlike typical dry scalp, these flakes might gradually become slightly more yellowish or greasy over time.
- Slightly Oily or Greasy Patches: On the face, particularly in the nasolabial folds, between the eyebrows, or on the forehead, the first sign might be an area that feels slightly oilier than the surrounding skin, with a very subtle sheen. This oiliness can be accompanied by an imperceptible hint of redness.
- Tiny, Pinpoint Red Dots: In some individuals, particularly those with sensitive skin, early seborrheic dermatitis can start with tiny, almost imperceptible red dots around hair follicles, especially in the beard area or on the scalp. These indicate localized inflammation before larger patches form.
- Minimal Scaling in Eyebrows/Eyelashes: A very fine, almost invisible, powdery scaling might appear in the eyebrows or at the base of the eyelashes. This can cause mild irritation or itching, leading to subtle rubbing of the eyes or brows. Early eyebrow seborrheic dermatitis photos may show just a hint of flaking.
- Persistent Itch without Obvious Rash: Sometimes, an early sign is a persistent, localized itch on the scalp, face, or chest, without any immediately visible rash or significant flaking. This pruritus can be misleading, as individuals might attribute it to dryness or allergies, delaying correct diagnosis of early seborrheic dermatitis.
- Pinkish Hue Behind Ears: The retroauricular folds (behind the ears) are common early sites. A subtle pinkish discoloration, sometimes with a barely perceptible scaling or slight stickiness, can be an initial sign. This area is often overlooked during self-examination.
Progression from early seborrheic dermatitis to more advanced stages:
- Increasing Redness and Inflammation: As the condition progresses, the initial subtle redness intensifies, becoming more clearly defined and possibly spreading. The skin may feel warm to the touch.
- Development of Greasy, Yellowish Scales: The initial dry flakes transition into the more characteristic greasy, yellowish scales, which become thicker and more adherent. This is a crucial visual cue in distinguishing established seborrheic dermatitis.
- Worsening Itching and Burning: The mild pruritus in the early stages can escalate to intense itching and a burning sensation, especially during flare-ups. This increased discomfort often prompts individuals to seek medical attention.
- Spread to Other Areas: From an initial localized patch, the condition may spread to contiguous areas or appear in new, distant sebaceous gland-rich regions of the body. For instance, from the scalp to the forehead, or from the nasolabial folds to the glabella.
- Fissuring and Crusting: In later stages, particularly in skin folds or areas of severe inflammation, the skin can crack (fissure) and thick crusts can form from dried exudate and scales. This indicates a more severe presentation of seborrheic dermatitis and a need for aggressive treatment.
Understanding these early seborrheic dermatitis photos and their associated symptoms is critical for both self-assessment and clinical diagnosis, enabling timely intervention to manage and control the condition effectively.
Skin rash Seborrheic dermatitis Images
The skin rash Seborrheic dermatitis images showcase the distinctive erythematous, scaly rash that defines this condition. This rash is not uniform; it presents with varying degrees of inflammation, scaling, and distribution patterns across different anatomical sites. Recognizing the specific characteristics of the seborrheic dermatitis rash is vital for accurate diagnosis and for differentiating it from other common skin conditions that can mimic its appearance. The interaction of sebum production, fungal proliferation (Malassezia), and the host’s immune response contributes to the unique morphology of this persistent rash. The visual evidence from numerous seborrheic dermatitis rash pictures highlights its chronic and recurrent nature.
Characteristics of the seborrheic dermatitis skin rash:
- Erythematous Patches with Sharply Defined Borders: The rash typically consists of red or pinkish patches. These patches can be oval, round, or irregular in shape, but often possess distinct, well-demarcated borders, especially on the face and trunk. The intensity of redness observed in seborrheic dermatitis rash pictures is highly variable, influenced by the degree of inflammation and the patient’s skin tone.
- Yellowish, Greasy Scales and Flakes: A defining feature of the seborrheic dermatitis rash is the presence of greasy, yellowish scales overlying the erythematous patches. These scales can range from fine, powdery flakes to thick, adherent crusts. The oily quality of these scales helps distinguish seborrheic dermatitis from the dry, silvery scales of psoriasis.
- Distribution Patterns: The rash classically appears in areas rich in sebaceous glands.
- Scalp: The entire scalp or localized patches can be affected. Scalp seborrheic dermatitis rash images typically show diffuse redness with adherent, yellowish, greasy scales, often extending to the hairline.
- Face: Common sites include the T-zone: nasolabial folds (creases from nose to mouth), glabella (between eyebrows), eyebrows themselves, eyelids (seborrheic blepharitis), and the forehead along the hairline. Facial seborrheic dermatitis rash pictures often highlight these symmetric patterns.
- Ears: Behind the ears (retroauricular folds), within the ear canal, and on the outer ear. Redness and scaling with a tendency to fissure are common.
- Trunk: Especially the presternal area (mid-chest) and interscapular region (between shoulder blades). The rash here can be nummular (coin-shaped) or petaloid (flower-shaped) with subtle scaling.
- Skin Folds (Intertriginous Areas): Axillae (armpits), groin, inframammary (under breasts), and umbilical region. The rash in these areas is often red and macerated (moist, softened skin) with less prominent scaling due to moisture, but still distinct borders.
- Symmetry: The seborrheic dermatitis rash often presents symmetrically, particularly on the face (e.g., both nasolabial folds, both eyebrows).
- Itching and Burning: While not a visual characteristic, the rash is almost invariably accompanied by significant pruritus (itching) and often a burning sensation, especially during flare-ups or in areas of intense inflammation. Scratching can lead to excoriations and secondary infections.
- Tendency to Flare and Remit: The seborrheic dermatitis rash is chronic and tends to have periods of exacerbation and remission. Triggers include stress, fatigue, hormonal changes, cold/dry weather, harsh soaps, alcohol use, and certain medications.
Differential diagnosis considerations when viewing skin rash Seborrheic dermatitis images:
- Psoriasis: Psoriasis also causes red, scaly patches, but its scales are typically silvery-white, dry, and thicker, and the rash often affects extensor surfaces (elbows, knees) and nails. Scalp psoriasis often has thicker, more silvery scales and a more defined border compared to seborrheic dermatitis. However, overlap (sebopsoriasis) can occur.
- Rosacea: Primarily affects the central face with redness, flushing, papules, and pustules, but typically lacks the greasy scaling of seborrheic dermatitis. Sometimes, the two conditions can coexist.
- Contact Dermatitis: Often characterized by intense itching, redness, vesicles (small blisters), and swelling, appearing after exposure to an allergen or irritant. The distribution is usually limited to the contact area, unlike the more widespread pattern of seborrheic dermatitis.
- Tinea (Ringworm): A fungal infection that causes annular (ring-shaped) rashes with raised, scaly borders and central clearing. While tinea can be scaly, the scales are not typically greasy, and the morphology is distinct.
- Lupus Erythematosus: Can cause facial rashes (e.g., butterfly rash) but these typically lack the greasy scales and specific distribution of seborrheic dermatitis.
The distinctive features seen in skin rash Seborrheic dermatitis images—the combination of erythema with characteristic yellowish, greasy scales in sebaceous gland-rich areas—are paramount for accurate clinical recognition. A thorough visual examination, combined with patient history, is often sufficient for diagnosis.
Seborrheic dermatitis Treatment
Effective Seborrheic dermatitis treatment aims to control symptoms, reduce inflammation, and manage the proliferation of Malassezia yeast, rather than providing a cure, as the condition is chronic and tends to recur. Treatment strategies for seborrheic dermatitis are multifaceted, encompassing topical medications, lifestyle modifications, and, in severe cases, systemic therapies. The choice of treatment depends on the location, severity, and extent of the condition, as well as individual patient factors. Consistent adherence to a treatment regimen is key to successful long-term management of seborrheic dermatitis symptoms.
Over-the-counter (OTC) Seborrheic dermatitis treatment options:
- Antifungal Shampoos and Cleansers: These are the first line of defense for scalp seborrheic dermatitis and often helpful for facial involvement. They contain active ingredients targeting Malassezia yeast.
- Selenium Sulfide (1%): Works by reducing yeast growth and slowing down cell turnover. Use 2-3 times per week. Common in dandruff shampoos.
- Zinc Pyrithione (1% or 2%): Possesses antifungal and antibacterial properties, effective in reducing scaling and itching. Often used daily or every other day.
- Ketoconazole (1%): A broad-spectrum antifungal that is highly effective against Malassezia. Available as a shampoo and cream. Use 2-3 times per week initially, then less frequently for maintenance.
- Coal Tar: Helps slow skin cell growth and reduce inflammation. Can be messy and has a strong odor, but effective for persistent scaling.
- Salicylic Acid: A keratolytic agent that helps loosen and remove scales, making it easier for other active ingredients to penetrate. Often combined with other agents.
- Topical Hydrocortisone Cream (0.5% or 1%): A mild corticosteroid that reduces inflammation and itching. Suitable for temporary use on facial or body patches, but prolonged use can lead to skin thinning, redness, and acne-like breakouts. It is crucial to use sparingly and under guidance.
- Moisturizers: Non-comedogenic, fragrance-free moisturizers can help soothe dry, irritated skin, especially after using drying antifungal cleansers. Look for ingredients like ceramides or hyaluronic acid.
Prescription Seborrheic dermatitis treatment options:
- Prescription-Strength Antifungal Medications:
- Ketoconazole (2%) Cream or Shampoo: A stronger version of the OTC antifungal, providing more potent yeast reduction. Used for more severe or persistent seborrheic dermatitis.
- Ciclopirox (1%) Cream, Gel, or Shampoo: Another effective antifungal agent, often prescribed when ketoconazole is not sufficient or tolerated.
- Efinaconazole (10%) or Tavaborole (0.5%): Topical antifungals primarily used for fungal nail infections, but can be considered off-label for resistant seborrheic dermatitis due to their broad-spectrum activity.
- Topical Corticosteroids: More potent corticosteroids are prescribed for short-term control of severe inflammation and itching, especially on the scalp or body.
- Desonide (0.05%) Cream or Foam: A low-to-medium potency steroid, often used for facial or intertriginous areas where skin is thinner and more sensitive.
- Fluocinolone Acetonide (0.01% or 0.025%) Solution/Oil/Shampoo: A medium-potency steroid often used for the scalp.
- Clobetasol Propionate (0.05%) Solution/Foam: A high-potency steroid reserved for very severe, resistant patches, used for very short durations due to risk of side effects like skin atrophy and telangiectasias.
Important Note: Topical corticosteroids should always be used under medical supervision due to potential side effects with prolonged use.
- Calcineurin Inhibitors: These are non-steroidal anti-inflammatory agents that can be very effective for facial and intertriginous seborrheic dermatitis, especially for long-term maintenance, as they do not cause skin thinning.
- Pimecrolimus (1%) Cream: Often used for milder cases or as maintenance therapy.
- Tacrolimus (0.03% or 0.1%) Ointment: More potent, used for moderate to severe cases.
- Advantages: Can be used for prolonged periods without the risk of steroid-induced side effects.
- Disadvantages: May cause a temporary burning or stinging sensation upon initial application.
- Oral Antifungal Medications: Systemic antifungals like oral ketoconazole, fluconazole, or itraconazole are reserved for severe, widespread, or resistant seborrheic dermatitis that does not respond to topical treatments. These carry risks of liver toxicity and drug interactions, requiring close medical monitoring.
- Oral Corticosteroids: Rarely used for seborrheic dermatitis due to the risk of rebound flares upon discontinuation and systemic side effects. May be considered for very acute, severe exacerbations for a very short course.
- Isotretinoin: In very rare, severe, and resistant cases, particularly those with significant sebaceous gland involvement, low-dose isotretinoin (an oral retinoid) may be considered to reduce sebum production. This is a powerful drug with many potential side effects and requires strict medical supervision.
Lifestyle and home care strategies for Seborrheic dermatitis management:
- Regular Hair and Skin Washing: Maintain good hygiene to prevent sebum and scale buildup. For the scalp, regular washing with a medicated shampoo as directed is crucial. For facial involvement, gentle cleansing with a mild, non-comedogenic cleanser.
- Avoid Harsh Soaps and Alcohol-Based Products: These can strip the skin of its natural oils, leading to irritation and potentially worsening seborrheic dermatitis symptoms. Opt for gentle, pH-balanced products.
- Moisturize Regularly: Even though seborrheic dermatitis affects oily areas, the skin can still become dry and irritated, especially from medicated treatments. Use a light, oil-free, non-comedogenic moisturizer.
- Manage Stress: Stress is a known trigger for seborrheic dermatitis flares. Incorporate stress-reduction techniques such as meditation, yoga, or regular exercise.
- Dietary Considerations: While direct links are not fully established, some individuals find that reducing intake of sugary foods, processed foods, and dairy, and increasing omega-3 fatty acids, can help manage inflammation. A balanced diet supports overall skin health.
- Sun Exposure: Moderate sun exposure can sometimes improve seborrheic dermatitis, but excessive exposure can cause sunburn and skin damage. Always use sunscreen on unaffected areas.
- Avoid Scrubs and Exfoliants: Mechanical exfoliation can further irritate inflamed skin and should be avoided during flare-ups. Chemical exfoliants like salicylic acid should be used cautiously and as part of a treatment regimen, not as a standalone abrasive scrub.
- Be Gentle with Affected Areas: Avoid scratching or picking at scales and crusts, as this can worsen inflammation, lead to infection, and potentially cause scarring or hair loss.
- Consider Shower Temperature: Hot water can strip skin of its natural oils and exacerbate dryness or irritation. Use lukewarm water for washing.
- Regular Laundry: Wash pillowcases, hats, and scarves frequently to remove yeast and oil buildup, especially if you have scalp seborrheic dermatitis.
Long-term seborrheic dermatitis treatment often involves a maintenance regimen to prevent relapses. This might include using antifungal shampoos once or twice a week, or intermittent application of topical calcineurin inhibitors. Regular follow-up with a dermatologist is recommended to adjust treatment as needed and to manage any potential side effects. Early diagnosis and consistent adherence to treatment are pivotal for effectively controlling seborrheic dermatitis symptoms and improving quality of life.