This comprehensive guide offers detailed insights into identifying various Tick bite symptoms pictures, providing essential information to understand and address potential health concerns. Focusing on visual cues and associated medical conditions, we aim to equip you with the knowledge to recognize early signs and seek appropriate care for tick bite reactions.
Tick bite Symptoms Pictures
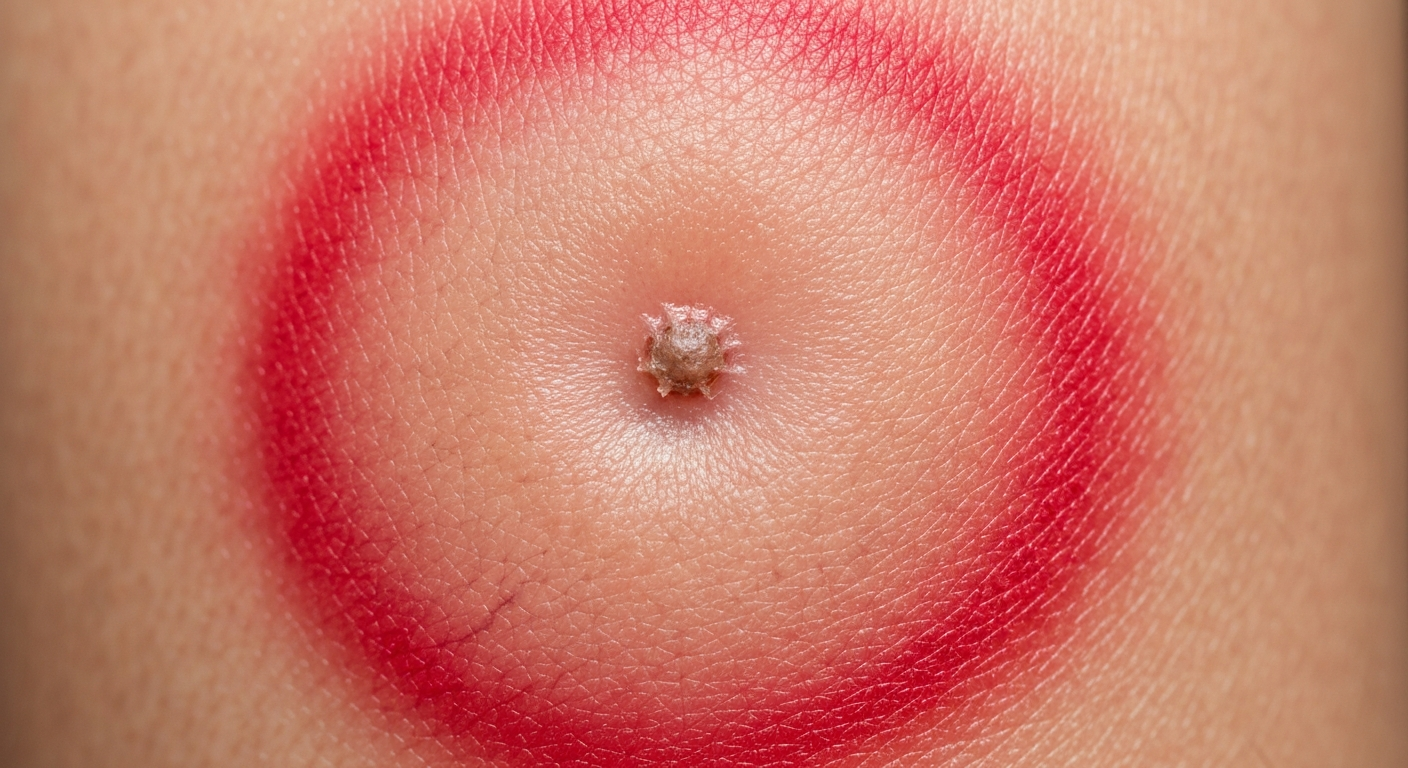
Understanding the immediate and evolving Tick bite symptoms pictures is crucial for early detection and intervention. A tick bite often presents initially as a small, red bump at the site of attachment, which can sometimes be confused with other insect bites. However, the progression and specific characteristics of a tick bite can differentiate it. The local reaction typically involves erythema, which is redness of the skin, swelling, and sometimes itching or a burning sensation. In some individuals, a small, firm papule may form, akin to a mosquito bite but often more persistent. The severity of these localized symptoms can vary significantly based on the individual’s immune response, the type of tick, and the duration of attachment.
Beyond the immediate bite site, systemic Tick bite symptoms pictures can develop if a tick-borne pathogen has been transmitted. These symptoms are not always immediately apparent and can manifest days to weeks after the initial bite. Key systemic indicators to watch for include:
- Fever and Chills: Often a generalized response to infection, these can range from mild to high-grade.
- Headache: Persistent and unexplained headaches, especially if accompanied by other symptoms.
- Muscle Aches (Myalgia) and Joint Pain (Arthralgia): Widespread body aches or specific joint pain, which may migrate.
- Fatigue: Profound tiredness or malaise that is disproportionate to activity levels.
- Swollen Lymph Nodes: Lymphadenopathy, particularly near the bite area or generalized.
- Nausea or Vomiting: Gastrointestinal disturbances, although less common as primary symptoms for all tick-borne illnesses.
- Loss of Appetite: A general feeling of not wanting to eat, contributing to weakness.
- Neck Stiffness: Indicative of meningeal irritation, potentially seen in advanced stages of some diseases.
- Sensitivity to Light (Photophobia): Another symptom that can suggest central nervous system involvement.
- Rash Development: While specific rashes like Erythema migrans are distinct, non-specific rashes can also occur.
The type of tick plays a significant role in the symptoms observed. For instance, a Lone Star tick bite can cause a specific localized rash called Southern Tick-Associated Rash Illness (STARI), which closely resembles Lyme disease’s bull’s-eye rash but is caused by a different pathogen. Deer ticks (blacklegged ticks) are primarily responsible for transmitting Lyme disease, Anaplasmosis, and Babesiosis, each with its own set of potential symptoms. Rocky Mountain wood ticks and American dog ticks can transmit Rocky Mountain Spotted Fever (RMSF), known for its characteristic petechial rash. Accurate identification of these various Tick bite symptoms pictures is paramount for effective diagnosis and management.
Factors influencing the severity and presentation of tick bite reactions and symptoms include:
- Tick Species: Different ticks carry different pathogens and can cause varying local reactions.
- Duration of Attachment: The longer a tick is attached, the higher the risk of pathogen transmission.
- Individual Immune Response: Some individuals may have more pronounced inflammatory reactions or be more susceptible to infection.
- Bite Location: Bites on sensitive areas may cause more discomfort or be harder to detect.
- Presence of Allergies: Some people can develop allergic reactions to tick saliva.
- Concurrent Health Conditions: Underlying health issues can influence symptom expression and severity.
- Age of the Host: Children and the elderly might experience different symptom profiles.
- Pathogen Load: The amount of infectious agent transmitted can influence disease progression.
Vigilance in monitoring Tick bite symptoms pictures after a known or suspected tick exposure is key. If any systemic symptoms develop, or if the local reaction appears concerning or persists, medical consultation is strongly advised to prevent potential complications from tick-borne diseases. Early recognition of these crucial signs can significantly impact treatment outcomes.
Signs of Tick bite Pictures
Observing the specific Signs of Tick bite Pictures is critical for distinguishing tick exposures from other dermatological concerns and for initiating timely removal and monitoring. The most direct sign is the presence of an attached tick itself. Ticks vary in size, from a poppy seed (nymphs) to a pencil eraser (engorged adults), and can appear brown, black, or reddish. When attached, they often embed their mouthparts into the skin, making them difficult to dislodge. The body of an engorged tick will appear swollen and grayish or bluish due to the blood meal. It is essential to look for the distinct shape of the tick’s body and legs protruding from the skin, as opposed to a simple scab or mole.
Upon tick removal, or if the tick detaches on its own, the bite site will present with specific visual signs. These localized Signs of Tick bite Pictures include:
- Red Macule or Papule: An immediate red spot or raised bump where the tick was attached. This is a common inflammatory response to the tick’s saliva.
- Erythema: A halo of redness surrounding the central bite point, which can vary in diameter.
- Induration: The skin around the bite may feel firm or hardened to the touch.
- Pruritus (Itching): Intense itching is a common complaint, though some bites may be painless.
- Minor Swelling: Localized edema around the bite site, usually mild.
- Ecchymosis (Bruising): In some cases, a small bruise may form if there was local tissue damage during attachment or removal.
- Central Punctum: A tiny scab or scabbed over pinpoint mark at the exact site where the tick’s mouthparts penetrated the skin.
- Persistent Lesion: Unlike many insect bites that fade quickly, a tick bite lesion might persist for several days to weeks, especially if an inflammatory reaction is ongoing.
- Formation of a Nodule: Sometimes, a persistent, firmer lump or granuloma can form weeks or months after the bite, especially if mouthparts were left behind.
Distinguishing Signs of Tick bite Pictures from other insect bites requires careful observation. Mosquito bites are typically softer, itchier, and fade within a day or two. Spider bites often present with two distinct puncture marks and can be more painful or blister. Flea bites typically appear in clusters or lines and are usually very itchy. Tick bites, particularly those that transmit pathogens, require a more cautious approach due to their potential health implications.
Red flag signs indicating potential complications or the transmission of a tick-borne illness include:
- Expanding Red Rash: Especially if it forms a bull’s-eye pattern or grows over several days (e.g., Erythema migrans from Lyme disease).
- Fever, Chills, Body Aches: Systemic symptoms appearing days to weeks post-bite.
- Neurological Symptoms: Weakness, numbness, tingling, or paralysis (rare, but can occur with tick paralysis).
- Persistent Swelling or Pain: If the local reaction worsens instead of improves after tick removal.
- Pus or Purulence: Signs of a secondary bacterial infection at the bite site.
- Difficulty Breathing or Swallowing: Rare, but severe allergic reactions or complications like tick paralysis can manifest this way.
- Blistering or Ulceration: Indicating a more severe local tissue reaction.
- Lymphangitis: Red streaks extending from the bite site, indicating a spreading infection.
- Petechiae or Purpura: Small, non-blanching red or purple spots, potentially seen in conditions like Rocky Mountain Spotted Fever.
The progression of Signs of Tick bite Pictures over time is also important. An initial small red spot might transform into a larger rash, indicating the onset of a tick-borne disease. Therefore, continuous monitoring of the bite site and the individual’s overall health for several weeks following a tick bite is strongly recommended. Documenting changes with photos can be helpful for medical professionals when seeking diagnosis.
Early Tick bite Photos
Identifying Early Tick bite Photos is paramount for prompt intervention, especially since many tick-borne diseases respond best to treatment initiated soon after infection. The initial reaction to a tick bite is often subtle and can easily be overlooked or mistaken for a common insect bite. Typically, within a few hours to a day after the tick has attached or detached, the bite site will begin to show its first visual cues. These early manifestations are primarily localized to the point of skin penetration.
Key features to look for in Early Tick bite Photos include:
- Pinpoint Redness: A very small, often barely perceptible red dot or macule at the exact point of the bite. This is the immediate inflammatory response to the tick’s saliva and the mechanical puncture.
- Mild Erythema: A slight reddish discoloration of the skin immediately surrounding the central bite mark. This redness is usually faint and may not be warm to the touch.
- Minimal Swelling: A barely raised bump or papule, often no larger than a small pimple. This swelling is due to localized fluid accumulation.
- Faint Pruritus or Tenderness: A mild itching sensation or slight tenderness when touched, which might not be constant.
- Absence of a Large Rash: In the very early stages (first 24-48 hours), the characteristic rashes associated with tick-borne diseases like Erythema migrans are typically not present. Their development usually takes days.
- Presence of the Tick Itself: The most definitive early sign is often finding the tick still attached, partially engorged, or just starting to embed. Ticks can be very small, especially nymphs, making them hard to spot.
The timeline of early symptom development for Early Tick bite Photos is critical. Most localized reactions become visible within a few hours to a day. If the tick has been removed, the bite mark might remain as a small red spot for several days. However, the absence of an immediate, severe reaction does not rule out the possibility of a tick-borne illness, as systemic symptoms and specific rashes often have a delayed onset. For example, the Erythema migrans rash of Lyme disease typically appears 3 to 30 days after the bite, with an average of 7-14 days.
Common locations for Early Tick bite Photos, reflecting where ticks most frequently attach, include:
- Lower Extremities: Ankles, calves, and behind the knees, as ticks are often encountered in tall grass or brush.
- Groin Area: A warm, protected area ticks favor.
- Armpits: Another warm and moist location.
- Waistline: Where clothing often provides a barrier and ticks might crawl underneath.
- Hairline and Scalp: Especially in children, ticks can be difficult to spot here.
- Behind the Ears: A less obvious, hidden spot.
- Back of the Neck: Often unnoticed until a lump is felt.
What to look for immediately after a suspected bite or outdoor activity:
- Thorough Body Check: Conduct a full-body tick check immediately after returning indoors, paying close attention to hidden areas.
- Small Dark Spots: Any new, small, dark, raised spots that don’t easily brush off could be a tick.
- Irritation or Itching: Any localized skin irritation or persistent itching in a specific area.
- “Seed-like” Bumps: Engorged nymphal ticks can feel like small seeds under the skin.
Variations in Early Tick bite Photos presentations can occur. Some individuals may experience a more pronounced immediate allergic reaction, leading to a larger, more intensely itchy welt. Conversely, some people may have almost no immediate reaction, making early detection solely reliant on physically finding the tick. It is this variability that underscores the importance of a diligent approach to tick checks and monitoring for any subsequent changes. Early detection and removal of a tick within 24-48 hours significantly reduce the risk of transmitting many tick-borne pathogens, making these early visual cues critically important.
Skin rash Tick bite Images
The appearance of a Skin rash Tick bite Images is often the most definitive and concerning symptom of a tick-borne illness, signaling the dissemination of pathogens within the body. While not all tick bites result in a rash, several significant tick-borne diseases are characterized by distinct dermatological manifestations. Recognizing these rashes is crucial for timely diagnosis and treatment, as many have specific patterns and progressions.
The most iconic Skin rash Tick bite Images is the Erythema migrans (EM) rash, a hallmark of early localized Lyme disease. Its characteristics include:
- Target or Bull’s-eye Appearance: A central red spot or clearing surrounded by an expanding red ring, with healthy skin in between. This classic appearance is seen in about 20-30% of cases.
- Homogeneous Redness: A uniformly red, expanding patch without central clearing, which is a more common presentation of EM (often seen in 50-60% of cases).
- Atypical Shapes: EM can also appear as an oval, triangular, or linear patch, especially if the bite occurred in a skin fold.
- Size: Typically greater than 5 cm in diameter, often expanding over days or weeks to reach sizes exceeding 12-30 cm.
- Texture: Usually flat, but can be slightly raised or bumpy, especially at the edges.
- Symptoms: May be itchy, warm, or slightly painful, but often asymptomatic. It is rarely blistering or crusting.
- Migration: The rash slowly expands outwards from the bite site over several days to weeks.
- Multiple Lesions: In disseminated early Lyme disease, multiple EM lesions can appear on different parts of the body, indicating widespread infection.
Atypical Erythema migrans presentations can make diagnosis challenging. These might include:
- Vesicular or Necrotic Centers: Rare, but sometimes observed, particularly in young children.
- Absence of Clear Borders: The edges of the rash might be indistinct.
- Location on Face or Scalp: Especially in children, EM can appear in these less common areas.
- Blue-Red Hue: Some rashes might have a more violaceous color rather than bright red.
Other important Skin rash Tick bite Images associated with specific tick-borne diseases include:
- Southern Tick-Associated Rash Illness (STARI) Rash: Caused by the Lone Star tick, this rash is clinically indistinguishable from the EM rash of Lyme disease, often presenting as a bull’s-eye. However, STARI is not caused by the Lyme bacterium Borrelia burgdorferi and is generally a milder illness.
- Rocky Mountain Spotted Fever (RMSF) Rash:
- Onset: Typically appears 2-5 days after the onset of fever.
- Appearance: Initially small, flat, pink, non-itchy spots (macules) on the wrists, forearms, and ankles.
- Progression: Spreads to the trunk, palms, and soles. Within a few days, the macules become raised (papules) and then petechial (small, non-blanching red or purple spots caused by bleeding under the skin).
- Severity: The petechial rash indicates more severe disease and is a late sign. Absence of a rash does not rule out RMSF.
- Ehrlichiosis and Anaplasmosis Rashes: While a rash is uncommon in these diseases (occurring in less than 10-20% of cases), when present, it can be non-specific, maculopapular, or petechial, and often affects the trunk. It does not typically have the classic EM appearance.
- Tularemia Rash: If the infection is acquired through a tick bite, an ulceroglandular form can develop, where a painful skin ulcer forms at the bite site, often with swollen lymph nodes.
- Tick-borne Relapsing Fever (TBRF) Rash: Can sometimes present with a transient maculopapular rash on the trunk and extremities, particularly during febrile episodes.
- Powassan Virus Disease: This severe tick-borne viral infection typically does not cause a rash.
Features differentiating tick-borne rashes from other rashes:
- Geographic Location and Exposure: History of outdoor activity in endemic areas is a strong indicator.
- Associated Symptoms: Rashes accompanied by fever, headache, myalgia, and fatigue strongly suggest a tick-borne illness.
- Pattern and Progression: The characteristic expansion of EM, or the centripetal spread and petechial nature of RMSF, are key differentiators.
- Lack of Pruritus: Many tick-borne rashes, especially EM, are less itchy than allergic reactions or other insect bites.
Any new or unusual Skin rash Tick bite Images appearing after a tick bite warrants immediate medical evaluation. Early diagnosis based on these visual cues, combined with a patient’s exposure history and other symptoms, is vital for successful treatment and preventing potential long-term complications associated with tick-borne diseases.
Tick bite Treatment
Effective Tick bite Treatment encompasses immediate first aid, medical intervention for potential infections, and robust prevention strategies. The approach to treatment is multi-faceted, ranging from proper tick removal to pharmacological management of tick-borne diseases. Understanding the various stages of treatment is crucial for mitigating risks and ensuring optimal health outcomes.
Step-by-Step Tick Removal Guide: The first and most critical step in Tick bite Treatment is the prompt and correct removal of the attached tick.
- Gather Supplies: Use fine-tipped tweezers, rubbing alcohol, and an antiseptic wipe.
- Grasp Close to the Skin: Use tweezers to grasp the tick as close to the skin’s surface as possible. Avoid grasping the tick’s body, as this can squeeze fluids into the skin.
- Pull Upward with Steady Pressure: Pull upward with steady, even pressure. Do not twist or jerk the tick, which can cause the mouthparts to break off and remain in the skin.
- Inspect the Bite Site: After removing the tick, examine the bite site to ensure that no mouthparts were left behind. If mouthparts remain, try to remove them with tweezers. If you cannot remove them easily, leave them alone and let the skin heal.
- Clean the Area: Thoroughly clean the bite area and your hands with rubbing alcohol or soap and water.
- Dispose of the Tick: Place the live tick in a sealed bag or container, wrap it tightly in tape, or flush it down the toilet. Do not crush the tick with your fingers.
- Document: Note the date, location of the bite, and consider taking a photo of the tick for potential identification by a healthcare provider.
When to Seek Medical Attention After a Tick Bite: While not every tick bite requires medical intervention beyond proper removal, certain circumstances warrant a doctor’s visit.
- Inability to Remove the Tick: If you cannot safely remove the tick yourself.
- Symptoms of Tick-Borne Illness: Development of fever, rash (especially a bull’s-eye rash), headache, muscle aches, joint pain, or fatigue within several weeks of the bite.
- Concerns About Tick Species: If the tick is identified as a species known to transmit severe diseases (e.g., deer tick in endemic areas).
- Prolonged Tick Attachment: If the tick was attached for more than 36-48 hours, increasing the risk of pathogen transmission.
- Local Reaction Worsens: If the bite site becomes increasingly red, swollen, painful, or shows signs of infection (pus).
- Immunocompromised Individuals: People with weakened immune systems may require closer monitoring.
- Severe Allergic Reaction: Although rare, difficulty breathing or widespread rash indicates a severe allergic response.
Medical Treatments for Specific Tick-Borne Illnesses: Timely diagnosis and antibiotic therapy are critical for bacterial tick-borne diseases.
- Lyme Disease Treatment:
- Early Localized Disease (Erythema migrans): Typically treated with oral antibiotics such as doxycycline (first choice for adults and children > 8 years old), amoxicillin, or cefuroxime axetil for 10-21 days.
- Early Disseminated Disease (Neurological, Cardiac, or Multiple EM): May require longer courses of oral antibiotics or intravenous antibiotics (e.g., ceftriaxone) depending on severity.
- Late Lyme Disease (Arthritis, Chronic Neurological): Often necessitates extended courses of oral or intravenous antibiotics.
- Rocky Mountain Spotted Fever (RMSF) Treatment:
- Primary Treatment: Doxycycline is the drug of choice for all ages, including young children. Treatment should be initiated immediately upon clinical suspicion, even before laboratory confirmation.
- Duration: Typically 7-14 days or for at least 3 days after fever subsides and clinical improvement is noted.
- Anaplasmosis and Ehrlichiosis Treatment:
- Primary Treatment: Doxycycline is the first-line antibiotic for both anaplasmosis and ehrlichiosis, effective for both adults and children.
- Duration: Usually 10-14 days, or until the patient is afebrile for at least 3 days.
- Babesiosis Treatment:
- Treatment Regimen: Often a combination of atovaquone and azithromycin, or clindamycin and quinine, for 7-10 days.
- Severity: Treatment depends on the severity of the illness; severe cases may require red blood cell exchange transfusion.
- STARI Treatment: Generally treated with oral doxycycline, similar to Lyme disease, for a shorter duration (e.g., 10-14 days).
- Tick Paralysis Treatment: Simply removing the tick typically resolves symptoms within hours to days.
- Alpha-gal Syndrome (Meat Allergy): There is no specific treatment for the allergy itself, beyond avoiding red meat and certain mammalian products. Symptoms of allergic reaction are managed with antihistamines, corticosteroids, or epinephrine for severe reactions.
Post-Exposure Prophylaxis (PEP) for Lyme Disease:
- A single dose of oral doxycycline (200 mg for adults, 4.4 mg/kg up to 200 mg for children ≥8 years old) may be offered in certain circumstances:
- The attached tick is an identified Ixodes scapularis (deer tick).
- The tick is estimated to have been attached for ≥36 hours (based on degree of engorgement or likely exposure time).
- Prophylaxis can be started within 72 hours of tick removal.
- Lyme disease is highly prevalent in the area.
- The individual is not pregnant or lactating, and has no contraindications to doxycycline.
Home Care and Symptomatic Relief for Tick bites:
- Pain and Itch Relief: Over-the-counter pain relievers (acetaminophen, ibuprofen) and topical anti-itch creams (hydrocortisone, calamine lotion) can alleviate discomfort.
- Cold Compress: Applying a cold compress to the bite site can reduce swelling and itching.
- Avoid Scratching: Prevent scratching the bite to reduce the risk of secondary bacterial infection.
Comprehensive Tick bite Prevention Strategies: Prevention is the most effective form of Tick bite Treatment.
- Use Insect Repellents: Apply EPA-registered insect repellents containing DEET, picaridin, IR3535, oil of lemon eucalyptus (OLE), para-menthane-diol (PMD), or 2-undecanone on exposed skin.
- Treat Clothing and Gear: Use products containing permethrin on clothing, boots, tents, and camping gear. Do not apply permethrin directly to skin.
- Wear Protective Clothing: When in wooded or grassy areas, wear long-sleeved shirts, long pants tucked into socks, and light-colored clothing to make ticks more visible.
- Perform Thorough Tick Checks: Conduct full-body tick checks on yourself, children, and pets after spending time outdoors, paying attention to hair, ears, armpits, groin, navel, and behind knees.
- Shower After Outdoor Activity: Showering within two hours of coming indoors can help wash off unattached ticks.
- Tumble Dry Clothes: Tumble dry clothes on high heat for 10 minutes to kill ticks on dry clothing after coming indoors.
- Landscape for Tick Control: Maintain a tick-safe yard by keeping lawns mowed, removing leaf litter, clearing tall grasses and brush, and creating a barrier of wood chips or gravel between wooded areas and lawns.
- Avoid Tick Habitats: Stay on cleared trails and avoid walking through dense brush, tall grass, and heavily wooded areas.
By implementing these comprehensive Tick bite Treatment and prevention measures, individuals can significantly reduce their risk of tick-borne diseases and manage tick exposures effectively.