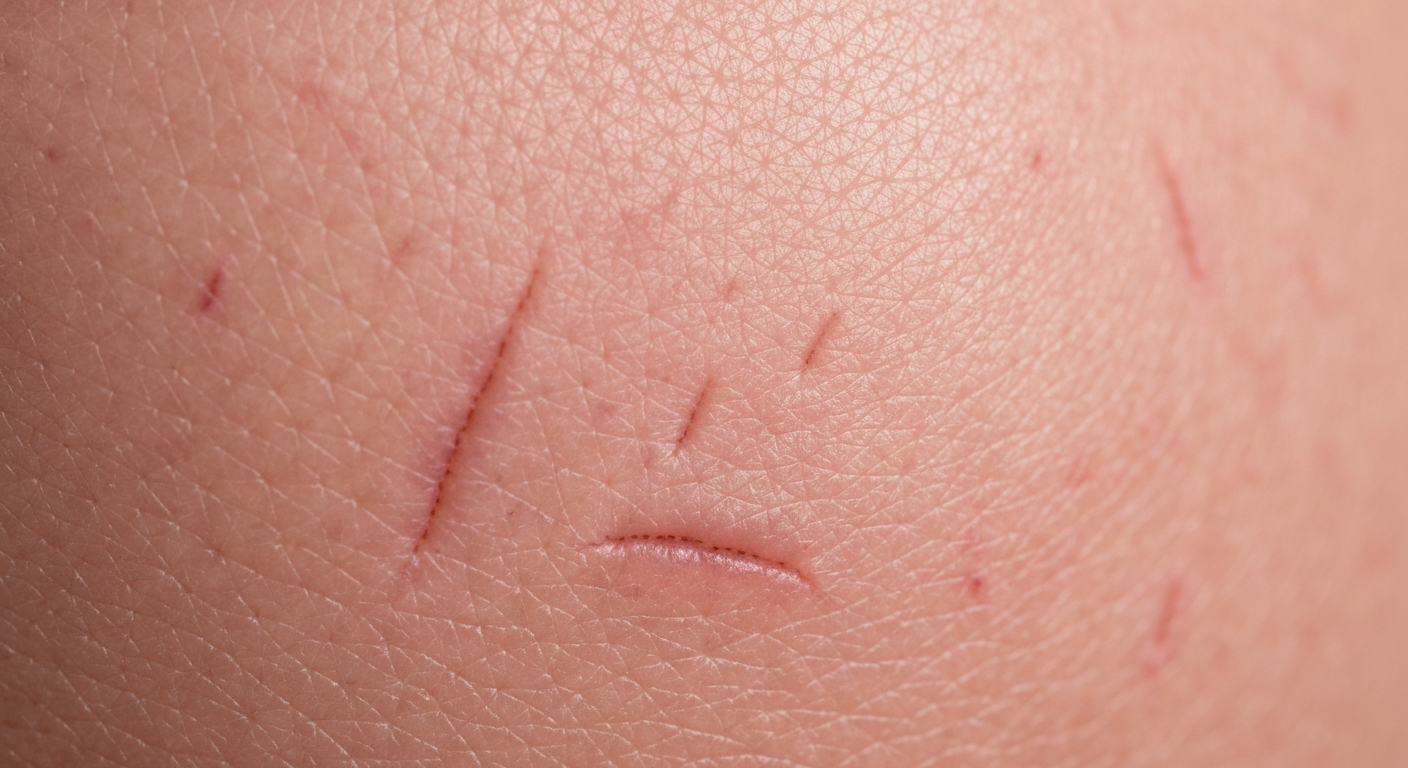
Identifying what does Scabies look like symptoms pictures is crucial for prompt diagnosis and effective treatment. The visual manifestation of scabies can vary, but certain characteristic skin lesions and patterns of distribution are key indicators. Understanding these signs can help differentiate scabies from other dermatological conditions.
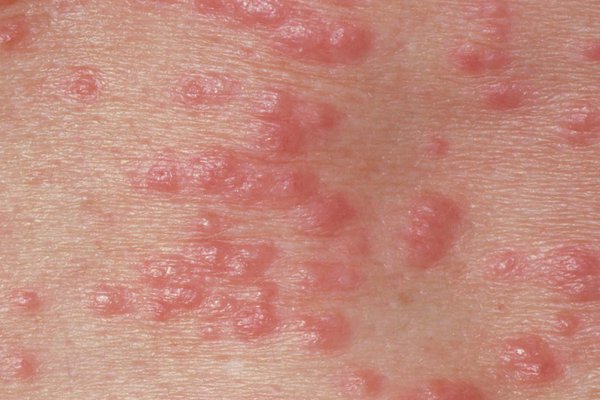
Scabies Symptoms Pictures
When examining scabies symptoms pictures, the most prominent feature is often an intensely itchy skin rash. This itching is typically worse at night or after a hot bath, a hallmark sign of a scabies infestation. The primary skin lesions associated with scabies are polymorphous, meaning they can present in various forms, making visual identification sometimes challenging without proper context. However, several distinct features help in recognizing this parasitic skin condition.
Key visual scabies symptoms to look for include:
- Scabies Burrows: These are arguably the most pathognomonic sign, though often difficult to spot with the naked eye due to their small size and the presence of secondary lesions like excoriations. A scabies burrow appears as a tiny, raised, irregular, grayish or reddish line, typically only a few millimeters to a centimeter in length. It represents the tunnel created by the female scabies mite as it burrows into the outermost layer of the skin (stratum corneum) to lay its eggs.
- Appearance: Fine, thread-like lines, often somewhat zig-zag or serpiginous.
- Color: Can range from skin-colored to grayish-white or reddish.
- Length: Typically 2-15 mm.
- Location: Commonly found on the web spaces between the fingers, sides of the fingers, wrists, elbows, armpits, belt line, nipples, penis, scrotum, and feet. In infants, burrows might be more visible on the palms and soles.
- Contents: The black dot at one end of the burrow is often the mite itself, which can be visualized with magnification.
- Erythematous Papules: These are small, red, raised bumps, usually 1-3 mm in diameter. They are a common inflammatory response to the presence of mites, their eggs, and fecal matter (scybala). These papules are intensely itchy and can be widespread across the body.
- Appearance: Solid, elevated lesions with a distinct reddish hue.
- Size: Generally small, but can coalesce into larger plaques in severe cases.
- Distribution: Widespread, but often concentrated in classic scabies locations like the wrists, elbows, axillae, breasts, waist, genitalia, and gluteal folds.
- Secondary Features: Often topped with tiny crusts or excoriations due to scratching.
- Vesicles: Some individuals, particularly children and infants, may develop small, fluid-filled blisters (vesicles) on the skin. These are usually clear and dome-shaped, and they also contribute to the intense itching.
- Appearance: Tiny, elevated, fluid-filled sacs.
- Size: Typically pinhead to pea-sized.
- Common Sites: Palms, soles, and sometimes the trunk in younger patients.
- Distinction: Important to differentiate from other blistering conditions like eczema or contact dermatitis.
- Pustules: If secondary bacterial infection occurs due to scratching, the papules or vesicles can become infected, leading to the formation of pustules (small, pus-filled bumps). These often indicate impetiginization of the scabies lesions.
- Appearance: Small, elevated lesions containing yellowish-white pus.
- Cause: Secondary bacterial infection, frequently by Staphylococcus aureus or Streptococcus pyogenes.
- Implication: Requires treatment for both scabies and the bacterial infection.
- Nodules: In some cases, particularly in infants and young children, persistent intensely itchy, reddish-brown nodules may develop, especially in covered areas like the armpits, groin, or scrotum. These post-scabetic nodules are often a hypersensitivity reaction to mite antigens and can persist for weeks or months even after successful treatment of the mites.
- Appearance: Firm, raised, dome-shaped lesions.
- Color: Reddish-brown to purple.
- Size: Can range from a few millimeters to over a centimeter.
- Persistence: May remain long after mite eradication, requiring symptomatic treatment.
- Location: Axillae, groin, buttock cleft, male genitalia (scrotum, penis).
The distribution of these scabies lesions is also highly characteristic. While itching can be generalized, the rash tends to concentrate in specific areas of the body where the skin is thin and warm, making it easier for the mites to burrow. These sites include the finger webs, wrists, elbows, armpits, navel, waistline, buttocks, and genital area. In infants and the elderly, the head, neck, palms, and soles may also be affected, areas typically spared in adults. Recognizing these patterns in scabies pictures is key to proper identification.
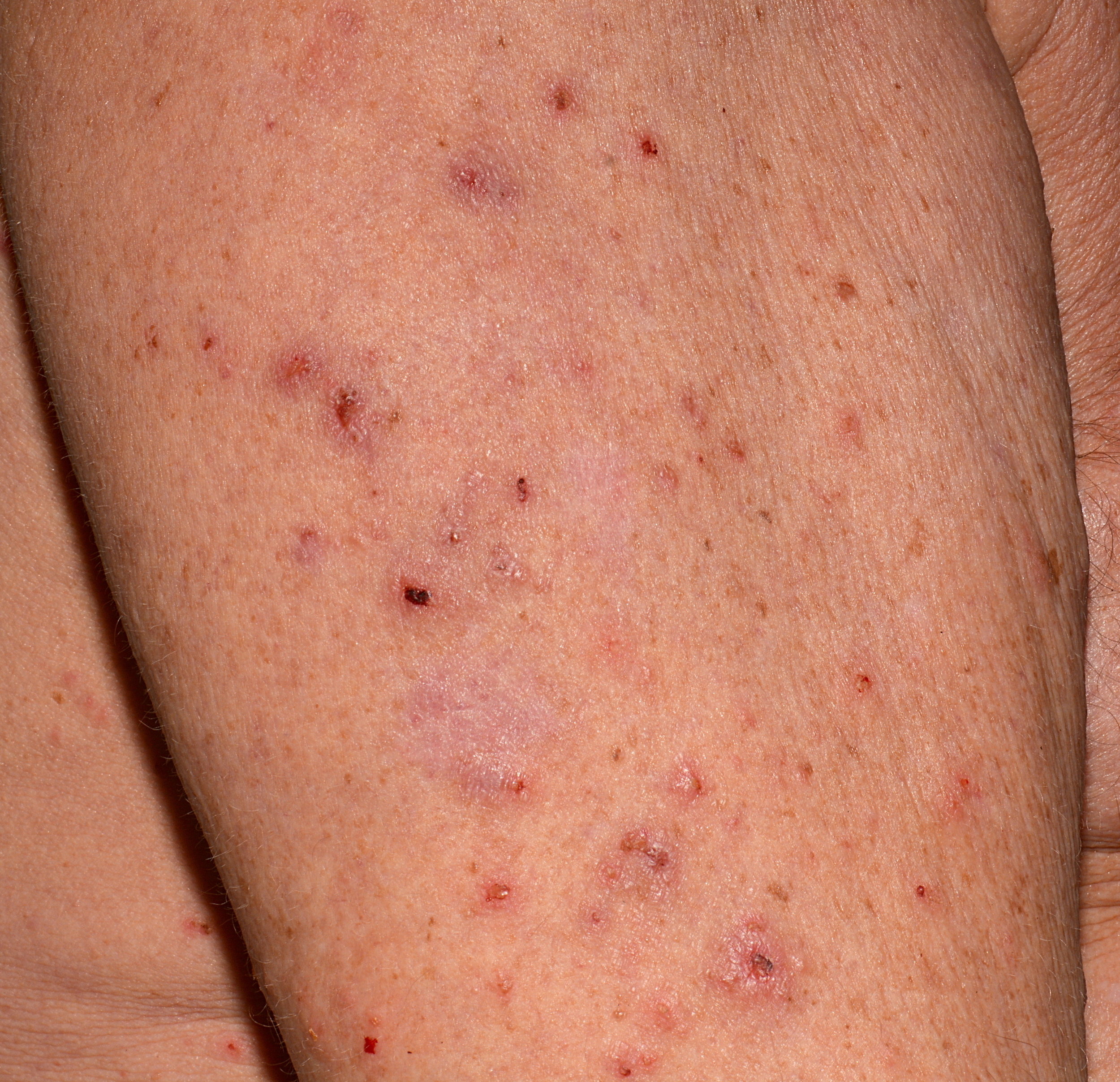
Signs of Scabies Pictures
Beyond the primary lesions, signs of scabies pictures often reveal several secondary changes to the skin caused by the infestation and the patient’s reaction to it. These secondary signs are very common and can sometimes obscure the primary burrows, making diagnosis more challenging for the untrained eye. However, they are integral to the overall clinical picture of scabies.
Common secondary signs visible in scabies pictures include:
- Excoriations: Due to the relentless itching, patients frequently scratch the affected areas, leading to excoriations (scratch marks). These can vary from fine linear marks to deep gouges, often accompanied by crusting and bleeding. Extensive excoriations are a strong indicator of severe pruritus and are almost universally present in symptomatic scabies cases.
- Appearance: Linear erosions, scabs, and sometimes signs of healed wounds.
- Distribution: Coincides with areas of primary rash and intense itching.
- Impact: Can mask primary lesions and increase risk of secondary infection.
- Crusting and Scaling: Chronic scratching and inflammation can lead to thickening of the skin (lichenification) and the formation of crusts and scales. This is particularly noticeable in chronic or severe cases, or in immunocompromised individuals where scabies can present atypically as crusted scabies.
- Lichenification: Thickened, leathery skin with exaggerated skin lines, indicative of chronic rubbing/scratching.
- Crusts: Dried serum, pus, or blood on the skin surface, often from scratched lesions.
- Scaling: Flakes of dead skin cells, especially prominent in crusted scabies.
- Secondary Bacterial Infections: As mentioned, excoriations can break the skin barrier, allowing bacteria (most commonly Staphylococcus aureus or Streptococcus pyogenes) to enter and cause secondary infections. These can manifest as impetigo (honey-colored crusts, pustules), cellulitis (red, swollen, warm skin), or even abscesses. In severe cases, particularly in tropical regions, streptococcal infections can lead to glomerulonephritis.
- Impetigo: Yellowish-brown crusts, often localized.
- Cellulitis: Spreading redness, warmth, and tenderness.
- Lymphadenopathy: Swollen lymph nodes near infected areas.
- Crusted Scabies (Norwegian Scabies): This is a highly contagious and severe form of scabies, primarily seen in immunocompromised individuals (e.g., HIV/AIDS, organ transplant recipients, chemotherapy patients), the elderly, or those with neurological conditions that prevent them from scratching. Signs of crusted scabies pictures are dramatic:
- Appearance: Widespread, thick, hyperkeratotic crusts and scales, often grayish or yellowish, resembling psoriasis or eczema. The skin appears thickened, fissured, and warty.
- Mite Burden: Harbors millions of mites, making it extremely infectious.
- Itching: Surprisingly, itching may be minimal or absent due to nerve damage or immune suppression, making diagnosis challenging if not specifically looked for.
- Distribution: Can affect virtually the entire body surface, including the scalp, face, palms, and soles, which are usually spared in classical scabies. Nails can become dystrophic (thickened, discolored, crumbly).
- Risk: High risk of secondary bacterial infections and sepsis.
- Nodular Scabies: While previously mentioned as a primary lesion type, its persistence and characteristic appearance make it a significant secondary sign. These firm, red-brown, intensely itchy nodules can last for many weeks or months even after successful mite eradication. They represent a persistent immunological reaction.
- Location: Especially common in the axillae, groin, buttocks, and on the male genitalia (scrotum, penis).
- Histology: Shows dense perivascular inflammatory infiltrates with eosinophils.
- Management: Often requires topical corticosteroids or intralesional steroid injections for resolution.
The combination of these signs in typical distribution patterns, especially in a patient with intractable itching, should strongly point towards a diagnosis of scabies. Thorough examination of these visual indicators in pictures is essential for understanding the diverse presentation of this infestation.
Early Scabies Photos
Early scabies photos can be particularly challenging to interpret because the visible signs may be subtle or atypical during the initial stages of infestation. The incubation period, or the time from first exposure to the development of symptoms, can vary significantly. For individuals with no prior exposure to scabies, symptoms may take 4 to 6 weeks to appear. In contrast, re-infestation in someone previously exposed can lead to symptoms within 1 to 4 days due to a pre-sensitized immune system. Understanding what early scabies looks like is crucial for preventing widespread transmission.
In early scabies, the immune response is just beginning, and the mite population is still small. Consequently, the rash may not be as extensive or severe as in later stages. Key features to look for in early scabies photos include:
- Minimal Rash Appearance: The initial rash might consist of only a few scattered, small, reddish papules, often mistaken for insect bites, folliculitis, or mild eczema. These early lesions may not yet have developed the characteristic distribution patterns seen in established scabies.
- Size: Small, discrete lesions, often 1-2 mm.
- Number: Relatively few lesions, sometimes only a handful.
- Location: May appear on single isolated areas before spreading.
- Subtle Burrows: While burrows are the definitive sign, they can be very faint and short in early infestations. They require careful inspection, often with dermoscopy or a magnifying glass, to be identified. They may appear as tiny, slightly elevated, discontinuous lines.
- Visibility: Often difficult to see without magnification.
- Length: Shorter than established burrows, perhaps only a few millimeters.
- Detection: Dermoscopy can reveal the “delta wing” or “jet plane” sign (the mite’s head and front legs) at the end of a burrow.
- Localized Itching: Initially, the itching might be confined to specific areas rather than being generalized. This localized pruritus, particularly if it worsens at night, should raise suspicion even without a widespread rash.
- Intensity: May start as mild to moderate, gradually increasing over time.
- Timing: Characteristic nocturnal exacerbation is often present even in early stages.
- Areas of Early Involvement: Certain areas are more prone to early infestation due to thinner skin and warmth. These include:
- Finger webs: Often one of the first sites to show tiny papules or faint burrows.
- Wrists: Small, red bumps on the flexor aspects of the wrists.
- Elbows: Papules around the elbows, especially on the extensor surfaces.
- Axillae: Small papules or mild irritation in the armpits.
- Belt line/Waist: Irritation or small bumps where clothing is tight.
- Absence of Secondary Changes: In very early scabies, there may be minimal or no excoriations, crusting, or secondary bacterial infections, as these are typically a result of prolonged scratching and inflammation. This can make the rash seem less severe and therefore less alarming.
- Skin texture: May appear relatively normal apart from the specific lesions.
- Infection risk: Lower initially, but increases with continued scratching.
The challenge with early scabies is its non-specific presentation, often leading to misdiagnosis as eczema, allergic reactions, or simple dry skin. A high index of suspicion, especially in cases of persistent, nocturnal itching that doesn’t respond to conventional treatments, is vital. Reviewing early scabies photos can help train the eye to spot these subtle but significant initial clues.
Skin rash Scabies Images
Skin rash scabies images present a wide spectrum, from discreet papules to widespread eczematous changes and severe crusting. The characteristic scabies rash is often described as polymorphous due to the varied types of lesions present simultaneously. The specific appearance of the rash is heavily influenced by factors such as the duration of infestation, the host’s immune response, age, and general health status. Understanding the typical presentation across different demographics and in various locations is key for accurate scabies diagnosis.
Detailed aspects of the scabies skin rash include:
- Typical Distribution Patterns:
- Adults and Older Children: The rash classically affects the interdigital web spaces of the hands, flexor aspects of the wrists, extensor surfaces of the elbows, anterior axillary folds, umbilicus, periareolar areas (especially in women), waistline, buttocks, and external genitalia (scrotum, penis). The head, neck, palms, and soles are usually spared.
- Infants and Young Children: Due to their immature immune systems and softer skin, infants often present with a more widespread and florid rash. The scalp, face, neck, palms, and soles are frequently involved. Vesiculobullous lesions (blisters) are more common in this age group, particularly on the palms and soles. The rash may resemble severe eczema.
- Elderly and Immunocompromised: Atypical presentations are common. The rash may be subtle, or conversely, extremely severe (crusted scabies). Itching may be minimal or absent. The distribution can be widespread, including areas typically spared.
- Morphology of Lesions:
- Papular Eruption: The most common form of the rash consists of multiple, erythematous (red), intensely itchy papules, typically 1-3 mm in diameter. These can be scattered or grouped.
- Vesicular Lesions: Small, clear, fluid-filled blisters (vesicles) can accompany papules, especially in children and on the palms and soles. These are generally discrete but can sometimes rupture, leading to crusting.
- Pustular Lesions: Result from secondary bacterial infection of papules or vesicles, appearing as small, pus-filled bumps. They indicate impetiginization and require antibacterial treatment in addition to scabicidal therapy.
- Nodular Lesions: Persistent, firm, reddish-brown nodules, typically 5-20 mm, often found in intertriginous areas like the groin, axillae, and on the male genitalia. These are a delayed hypersensitivity reaction and can persist for months after successful mite eradication.
- Burrows: As the definitive sign, these are delicate, wavy, thread-like lines, often greyish or skin-colored, 2-15 mm long. They are most commonly found in the web spaces of fingers, wrists, and along the sides of the fingers. Identifying burrows in skin rash scabies images can be diagnostic.
- Secondary Skin Changes:
- Excoriations: Prominent scratch marks, ranging from linear abrasions to deep lacerations, are almost always present due to severe pruritus. These often obscure the primary lesions.
- Lichenification: Chronic scratching and rubbing can lead to thickening of the skin with exaggerated skin markings, particularly in chronic cases.
- Crusting and Scaling: Can range from small, localized scabs over excoriated papules to widespread, thick, hyperkeratotic crusts seen in crusted scabies. The scales may be dry and flaky.
- Post-inflammatory Hyperpigmentation: After the rash resolves, residual dark spots may be left, especially in individuals with darker skin tones.
- Crusted Scabies (Norwegian Scabies) Rash:
- Appearance: Grossly hyperkeratotic plaques and crusts resembling psoriasis or severe eczema. The skin appears thickened, scaly, often with fissures, and can be grayish-yellow.
- Distribution: Widespread, often involving the scalp, face, neck, palms, soles, and nail beds (leading to dystrophic nails).
- Itching: May be absent or mild despite the overwhelming number of mites, making it insidious.
- Contagiousness: Extremely high due to the immense mite burden (millions of mites).
When examining skin rash scabies images, it’s vital to consider the entire clinical context, including the patient’s age, immune status, and the duration of symptoms. The intense pruritus, especially nocturnal, combined with characteristic lesions and their distribution, forms the basis for a presumptive diagnosis, often confirmed by microscopic identification of mites, eggs, or fecal pellets from skin scrapings. These images are powerful tools for recognizing the diverse manifestations of scabies.
Scabies Treatment
Effective scabies treatment involves eradicating the mites and addressing the associated symptoms, particularly the severe itching. Treatment typically consists of topical scabicides or oral medications, often requiring environmental decontamination to prevent re-infestation. It is crucial to treat not only the infested individual but also all close contacts, including household members and sexual partners, even if they are asymptomatic, to break the cycle of transmission. Ignoring treatment for contacts is a common reason for treatment failure and recurrent scabies outbreaks.
Key components of scabies treatment include:
Topical Scabicides:
These are creams or lotions applied directly to the skin to kill the mites. The method of application is critical for successful eradication.
- Permethrin Cream 5%:
- Mechanism: A synthetic pyrethroid that acts as a neurotoxin to mites.
- Application: Apply to all skin surfaces from the neck down to the soles of the feet, including under fingernails and toenails. In infants and the elderly, the scalp and face (avoiding eyes and mouth) should also be treated. Leave on for 8-14 hours (typically overnight), then wash off thoroughly.
- Frequency: A single application is usually sufficient, but a second application 7-10 days later is often recommended to kill newly hatched mites.
- Safety: Considered very safe for most individuals, including children over 2 months of age and pregnant/lactating women (category B).
- Side Effects: Mild transient burning, stinging, itching, or redness.
- Ivermectin Lotion 0.5% (for topical use):
- Mechanism: Causes paralysis and death of mites by interfering with their nervous system.
- Application: Apply to dry skin as a thin layer to all skin surfaces from the neck down. Leave on for 10 minutes, then wash off.
- Frequency: One application; a second application 7 days later may be considered based on clinical judgment.
- Safety: Approved for individuals 6 months of age and older.
- Crotamiton Cream or Lotion 10%:
- Mechanism: Has scabicidal and antipruritic properties, though less effective than permethrin.
- Application: Apply to the entire body from the neck down once daily for 2-5 days.
- Safety: Less commonly used due to lower efficacy compared to permethrin. Not recommended for children or pregnant women.
- Side Effects: Skin irritation, rash.
- Sulfur Ointment 5-10%:
- Mechanism: Directly toxic to mites.
- Application: Applied nightly for 3-7 consecutive nights.
- Safety: An older, safe alternative for infants younger than 2 months and pregnant women. It is messy, has an unpleasant odor, and can stain clothing.
- Side Effects: Skin irritation.
- Benzyl Benzoate Lotion 25%:
- Mechanism: A potent scabicide, but can be highly irritating.
- Application: Apply to the entire body from the neck down for 24 hours, repeat once. Often diluted to 10-12.5% for children.
- Safety: Not recommended for children under 2 years old or in pregnant/lactating women due to irritation.
- Side Effects: Severe skin irritation, especially on inflamed skin.
- Malathion Lotion 0.5%:
- Mechanism: Organophosphate insecticide that inhibits cholinesterase, leading to mite paralysis and death.
- Application: Apply to the entire body from the neck down, leave on for 24 hours, then wash off.
- Safety: Efficacious but has an unpleasant odor and is flammable. Generally reserved for cases resistant to other treatments.
Oral Medications:
Primarily used for crusted scabies, widespread infestations, or cases where topical treatment is impractical or has failed.
- Oral Ivermectin:
- Mechanism: A broad-spectrum antiparasitic agent that paralyzes and kills mites.
- Dosage: Typically a single dose of 200 micrograms/kg body weight, repeated 7-14 days later.
- Indications: Highly effective for crusted scabies (often requiring multiple doses), large outbreaks in institutional settings, or individuals who cannot tolerate or properly apply topical treatments.
- Safety: Not recommended for children weighing less than 15 kg, pregnant women (category C), or lactating women due to limited safety data.
- Side Effects: Dizziness, nausea, headache, transient increase in itching.
Management of Crusted Scabies:
This severe form requires aggressive treatment due to the high mite burden and extreme contagiousness.
- Combination Therapy: Usually involves a combination of oral ivermectin (multiple doses) and a topical scabicide like permethrin cream (daily application for several days or weeks).
- Keratolytics: Topical agents like urea cream or salicylic acid may be used to soften thick crusts and allow better penetration of scabicides.
- Isolation: Patients with crusted scabies should be isolated until successful treatment to prevent widespread outbreaks.
Symptomatic Treatment and Post-Scabies Management:
- Antipruritics: Oral antihistamines (e.g., hydroxyzine, diphenhydramine) can help manage the intense itching.
- Topical Corticosteroids: Mid-potency topical steroids can be used to reduce inflammation and itching, especially for persistent post-scabetic nodules or eczematous reactions, but only after successful mite eradication.
- Antibiotics: If secondary bacterial infection is present, oral or topical antibiotics may be prescribed.
- Post-Scabies Itch: Itching can persist for 2-4 weeks after successful mite eradication as the body clears mite debris and allergens. This is normal and does not necessarily indicate treatment failure or re-infestation. Continued reassurance and symptomatic treatment are important.
Environmental Decontamination:
To prevent re-infestation from mites shed into the environment:
- Laundry: Wash all clothing, bedding, and towels used by the infested person and close contacts within the last 72 hours in hot water (at least 50°C or 122°F) and dry in a hot dryer.
- Items not washable: Items that cannot be washed (e.g., stuffed animals, non-washable shoes) should be sealed in plastic bags for at least 72 hours (3 days) or preferably for a week, as scabies mites cannot survive long off a human host.
- Vacuuming: Vacuum carpets and upholstered furniture, then dispose of the vacuum bag.
- Fumigation: Chemical fumigation of living areas is generally not necessary and is discouraged.
Successful scabies treatment requires adherence to the prescribed regimen, treating all contacts, and understanding that post-treatment itching is common. Close follow-up with a healthcare provider is recommended to ensure complete eradication and address any persistent symptoms or complications.