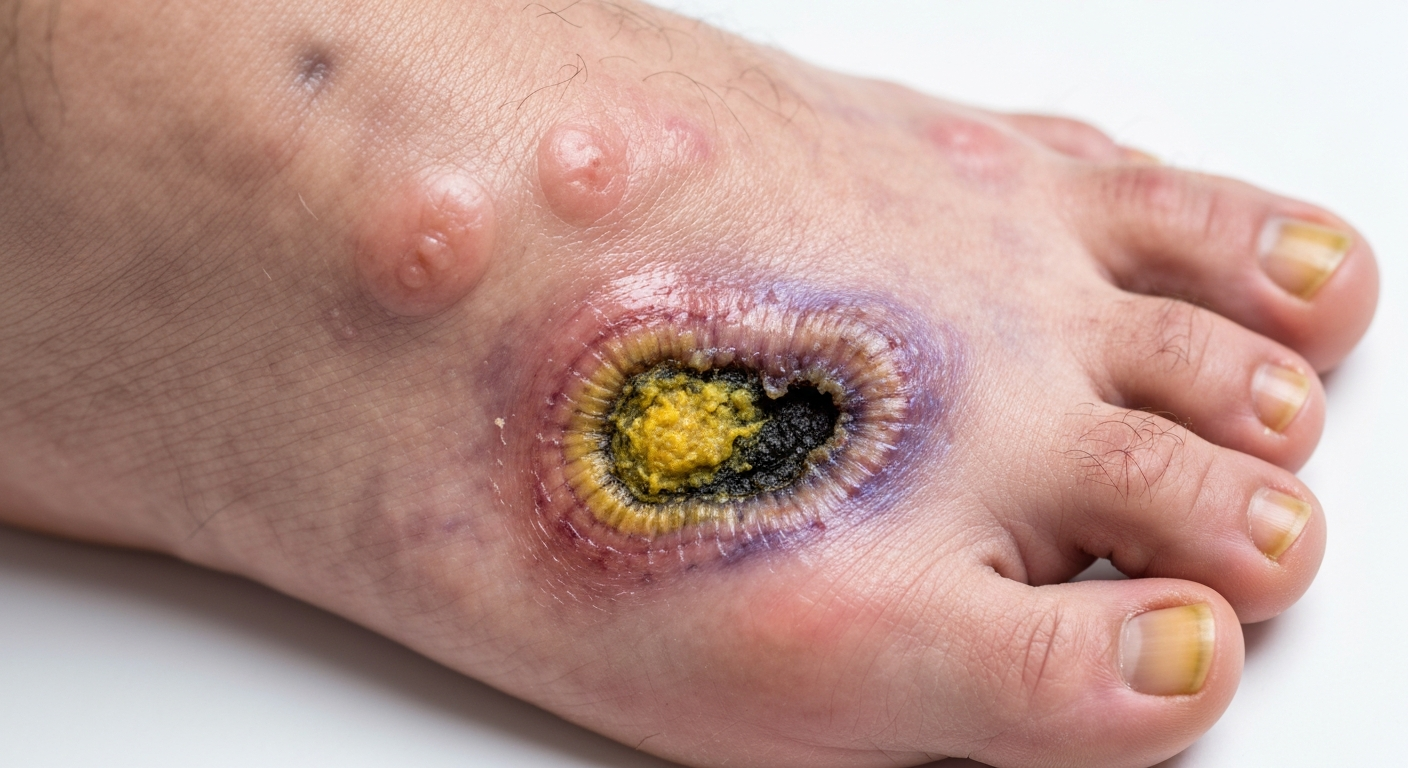
Recognizing the visual cues of diabetic foot is paramount for preventing severe complications. This detailed article explores various
Diabetic foot Symptoms Pictures
Understanding the visual manifestations of diabetic foot is crucial for early detection and intervention. This section provides detailed descriptions of various
Key
- Diabetic Foot Ulcers: These are open sores or wounds that commonly develop on the feet of individuals with diabetes.
Diabetic foot ulcers are a hallmark symptom and are often precipitated by peripheral neuropathy, leading to loss of protective sensation, and peripheral artery disease, which impairs healing. Ulcers can vary significantly in appearance but frequently present as a ‘punched-out’ lesion with a necrotic base, surrounded by hyperkeratotic tissue (callus). They most often occur on pressure points such as the balls of the feet, the heels, or the tips of the toes, where constant friction and pressure, combined with reduced sensation, can lead to unnoticed injury. The depth can range from superficial skin breaks to deep wounds exposing tendons, bones, and joints. These ulcers are highly susceptible to infection, which can rapidly spread and escalate the severity of the condition. Visual cues include drainage (serous, purulent, sanguineous), surrounding redness, warmth, and the presence of foul odor indicating infection. The edges may be rolled or calloused, providing a visual border to the lesion. - Neuropathic Pain and Sensory Loss: While ‘pain’ might not be a direct visual symptom, its absence or presence can influence the presentation of other visual signs.
Diabetic neuropathy often leads to a diminished ability to feel pain, temperature changes, or pressure. This sensory loss means minor cuts, blisters, or pressure sores can go unnoticed and worsen significantly without the patient realizing. Visually, this can manifest as unrecognized trauma, such as foreign objects embedded in the foot, or unexplained blistering and rubbing injuries from ill-fitting shoes. Conversely, some patients may experience neuropathic pain, described as burning, tingling, sharp, or shooting pains, which are not directly visible but can lead to patient behaviors (e.g., limping, favoring a foot) that may contribute to visible signs of stress or injury on other parts of the foot. The loss of protective sensation is a critical factor in the development ofdiabetic foot complications . - Skin Changes and Discoloration: Changes in
skin appearance on the feet are criticaldiabetic foot symptoms pictures . These can indicate underlying vascular or neurological compromise.- Redness (Erythema): Often a sign of inflammation or infection, particularly around an ulcer or an area of increased pressure. Localized redness, warmth, and swelling can signal cellulitis, a bacterial skin infection that requires prompt treatment to prevent deeper tissue involvement. Diffuse redness can also indicate the acute phase of
Charcot foot . - Blueness/Purpleness (Cyanosis): Suggests severe ischemia (lack of blood flow). This discoloration indicates critical limb ischemia and a high risk of tissue death. It is often accompanied by a cold sensation and can be a precursor to
gangrene . - Pallor (Pale Skin): An indicator of reduced blood supply, especially when the leg is elevated (Buerger’s sign). The foot might appear excessively pale or waxy. This points to insufficient arterial flow, characteristic of
peripheral artery disease (PAD). - Darkening/Blackening (Gangrene): The most severe form of tissue necrosis, resulting from a complete lack of blood flow or overwhelming infection.
Gangrene can be ‘dry’ (mummified, shriveled, cold, and numb, often black or dark brown, with a clear line of demarcation) or ‘wet’ (swollen, blistered, oozing, foul-smelling, and rapidly spreading due to bacterial infection, often purplish-black). Both are dire signs requiring urgent medical intervention, often involving surgical debridement or amputation. - Shiny, Taut Skin: Often seen in areas with poor circulation, indicative of reduced tissue perfusion and skin elasticity. The skin may appear thin and translucent. Hair loss on the lower legs and feet often accompanies this sign, reinforcing the diagnosis of vascular insufficiency.
- Thickened, Scaly Skin: Can be a result of chronic edema or underlying fungal infections, leading to a leathery appearance.
- Redness (Erythema): Often a sign of inflammation or infection, particularly around an ulcer or an area of increased pressure. Localized redness, warmth, and swelling can signal cellulitis, a bacterial skin infection that requires prompt treatment to prevent deeper tissue involvement. Diffuse redness can also indicate the acute phase of
- Swelling (Edema): While not always specific to
diabetic foot , localized or generalized swelling in the foot or ankle can be a significant indicator.- Localized Swelling: Around an infected wound or ulcer, indicating inflammation and fluid accumulation. This can be accompanied by warmth and tenderness.
- Generalized Swelling: Can be due to systemic issues like heart failure or kidney disease, but in the context of
diabetic foot , it might suggest earlyCharcot neuropathic osteoarthropathy (Charcot foot) or deep vein thrombosis (DVT). The swelling associated with Charcot foot is typically unilateral and often accompanied by intense warmth.
- Temperature Changes: The skin temperature of the foot can provide crucial diagnostic clues for
diabetic foot problems .- Increased Warmth: Localized warmth can indicate inflammation, infection (e.g., cellulitis, osteomyelitis), or the acute phase of
Charcot foot , where bone destruction and inflammatory processes lead to increased blood flow to the affected area. This warmth can be striking, often several degrees Fahrenheit higher than the contralateral foot. - Decreased Coolness: A cold foot, especially in contrast to the unaffected limb, strongly suggests
peripheral artery disease and poor circulation. This symptom is often accompanied by pallor or cyanosis and delayed capillary refill time, signifying inadequate blood flow to the extremities.
- Increased Warmth: Localized warmth can indicate inflammation, infection (e.g., cellulitis, osteomyelitis), or the acute phase of
- Foot Deformities: Long-standing neuropathy can lead to muscle weakness and imbalances, resulting in structural changes to the foot. These
diabetic foot deformities create new pressure points that are highly susceptible to ulceration.- Hammertoes and Claw Toes: Toes that are bent abnormally, increasing pressure on the tips of the toes and the balls of the feet, making them prone to ulcers and calluses. These deformities result from intrinsic muscle weakness caused by neuropathy.
- Bunions (Hallux Valgus): Bony bumps at the base of the big toe, often caused by abnormal mechanics and exacerbated by ill-fitting footwear. These are also a common site for ulceration due to friction and pressure.
- Rocker-Bottom Foot (Charcot Foot): A severe deformity where the arch of the foot collapses, creating a convex sole. This is a progressive and destructive arthropathy associated with severe neuropathy. The foot becomes warm, red, and swollen in its acute phase, followed by eventual collapse and deformity, creating new pressure points susceptible to ulceration and subsequent infection. Early detection of acute Charcot is critical to prevent irreversible deformity.
- Calluses and Corns: While common in the general population, in diabetic patients, thick calluses (hyperkeratosis) frequently form over pressure points. These are significant because they can conceal underlying ulcers, and the pressure beneath them can contribute to ulcer formation. They often appear yellow or brownish, are very hard, and can be quite thick. Regular reduction of calluses by a podiatrist is crucial to prevent
diabetic foot ulcers from forming beneath them. - Nail Changes:
Diabetic foot problems can also manifest in the nails.- Thickened, Brittle, or Discolored Nails: Often indicative of fungal infections (onychomycosis), which are more common and harder to treat in diabetic patients due to compromised immunity and circulation. The nails may appear yellow, brown, or black and can crumble easily.
- Ingrown Toenails: Can lead to infections, especially in patients with neuropathy who may not feel the initial irritation or pressure from the nail growing into the surrounding skin. This can quickly escalate to cellulitis or osteomyelitis.
- Loss of Hair on Toes and Feet: A classic sign of poor circulation (
peripheral artery disease ), where reduced blood flow diminishes nutrient supply to hair follicles. The skin may also appear atrophic. This is an important visual clue for underlying vascular compromise. - Muscle Atrophy: Thinning of the muscles in the foot, particularly noticeable in the intrinsic foot muscles, can be a visual sign of long-standing neuropathy. This contributes to foot deformities and altered biomechanics, increasing pressure on specific areas.
Signs of Diabetic foot Pictures
Observing the specific
Key
- Active Ulceration and Wound Characteristics:
- Location:
Diabetic foot ulcers typically occur on pressure points. Plantar aspect of metatarsal heads, heels, tips of toes (from hammertoes), sides of feet (from ill-fitting shoes). - Appearance: A ‘punched-out’ look with clearly defined borders, often surrounded by a hyperkeratotic rim (callus). The base of the ulcer can be pink and granular (healthy healing tissue), pale (poor perfusion), yellow/sloughy (necrotic tissue), or black (eschar/gangrene).
- Depth: Can range from superficial epidermal loss to deep tissue involvement, exposing tendons, bones, or joint capsules. Deeper ulcers carry a higher risk of osteomyelitis.
- Drainage (Exudate): The type and amount of fluid draining from an ulcer provide crucial information.
- Serous: Clear, watery fluid, often indicating a clean wound or blister.
- Sanguineous: Red, bloody drainage, suggesting fresh bleeding or highly vascularized tissue.
- Seropurulent: Pinkish-yellow, thin and cloudy, often an early sign of infection.
- Purulent: Thick, opaque, yellow, green, or brown fluid with a foul odor, strongly indicative of bacterial infection.
- Peri-wound Skin: The skin surrounding the ulcer. Look for redness (erythema), warmth, swelling (edema), or induration (hardening), which are all signs of infection or inflammation. Maceration (softening due to excessive moisture) can also be observed.
- Location:
- Signs of Infection:
- Cellulitis: Diffuse redness, warmth, swelling, and tenderness of the skin, often spreading rapidly. The borders are typically ill-defined. This is a common
diabetic foot infection . - Abscess Formation: A localized collection of pus within tissues, often presenting as a tender, fluctuant (fluid-filled) lump. May be accompanied by surrounding cellulitis.
- Lymphangitis: Red streaks extending proximally from the infected area, indicating bacterial spread along lymphatic channels.
- Osteomyelitis: While not directly visible, signs like persistent deep ulcers that probe to bone, chronic pain, and recurrent infections in the same area suggest underlying bone infection, which often manifests through non-healing wounds.
- Cellulitis: Diffuse redness, warmth, swelling, and tenderness of the skin, often spreading rapidly. The borders are typically ill-defined. This is a common
- Signs of Ischemia (Peripheral Artery Disease – PAD):
- Dependent Rubor: A dusky red discoloration of the foot when in a dependent position (hanging down), which turns pale on elevation. This is a classic sign of severe arterial insufficiency.
- Pallor on Elevation: The foot becomes excessively pale when elevated above heart level, due to reduced blood flow struggling against gravity.
- Delayed Capillary Refill: When pressure is applied to the toe and released, the time it takes for color to return is prolonged (greater than 3 seconds), indicating poor microcirculation.
- Absence or Diminished Pulses: While a physical palpation sign, the absence of pedal pulses (dorsalis pedis, posterior tibial) is a critical indicator of PAD, which has direct visual consequences on the skin.
- Atrophy of Skin and Subcutaneous Tissue: Thin, shiny, hairless skin on the lower leg and foot, often accompanied by reduced muscle mass.
- Trophic Changes: Thickened, brittle toenails (onychomycosis is common but not always ischemic), slow nail growth, and loss of hair.
- Charcot Neuropathic Osteoarthropathy (Charcot Foot):
- Acute Phase: Characterized by unilateral warmth, redness, and swelling in the foot or ankle, often without significant trauma. It can be mistaken for infection. The foot is often very painful initially, but due to neuropathy, pain perception may be diminished.
- Chronic Deformity: The most recognizable sign is the “rocker-bottom” deformity, where the midfoot arch collapses, creating a convex sole. This leads to new pressure points and a high risk of ulceration. Bone displacement and joint dislocation are also visible on imaging, contributing to the external deformity.
- Foot Deformities (General):
- Hammertoes/Claw Toes: Visibly bent toes, where the joint closer to the nail (distal interphalangeal) or the middle joint (proximal interphalangeal) is flexed.
- Bunions: A visible bony protrusion at the base of the big toe, often pushing the big toe towards the other toes.
- Prominent Metatarsal Heads: Due to fat pad atrophy and muscle imbalance, the ball of the foot appears bony and prominent, increasing pressure and callus formation.
- Talipes Equinovarus (Clubfoot-like deformity): Less common in adult diabetic foot but can occur secondary to severe Charcot or chronic contractures.
- Skin Breakdowns and Pre-ulcerative Lesions:
- Blisters (Bullae): Fluid-filled lesions caused by friction or pressure, especially common in neuropathic feet that don’t feel the irritation. Can be clear or blood-filled.
- Fissures and Cracks: Especially on heels and between toes, often due to dry skin or fungal infections, providing entry points for bacteria.
- Ingrown Toenails: Redness, swelling, and sometimes pus around the nail border where the nail has grown into the skin.
- Hyperkeratosis (Callus): Thickened, hardened skin, typically yellow or brown, over pressure points. While protective to a degree, excessive callus harbors pressure and can hide underlying ulcers.
Early Diabetic foot Photos
Early detection of
Key
- Dry, Cracking Skin (Xerosis): One of the earliest and most common
early diabetic foot symptoms . Due to autonomic neuropathy, the sweat glands in the feet may not function properly, leading to excessively dry skin. This can make the skin flaky, itchy, and prone to cracking, especially around the heels and soles. These cracks (fissures) can serve as entry points for bacteria, leading to infections.Diabetic foot care includes daily moisturizing to combat this. - Minor Calluses and Corns: While calluses are common, in diabetic individuals, even minor calluses can indicate areas of increased pressure. In a neuropathic foot, these can quickly progress to deeper tissue damage and ulceration beneath the hardened skin. Early calluses are often yellowish and localized to pressure points.
- Subtle Skin Discoloration:
- Mild Pallor: A slightly paler appearance of the foot, especially when elevated, which may indicate early, less severe peripheral artery disease.
- Subtle Redness: Localized, mild redness, particularly around a callus or an area of minor irritation, could be the first sign of inflammation or developing pressure. This should not be ignored.
- Bluish Tint: A very faint bluish or purplish tint, especially on the toes, can indicate reduced oxygenation due to early vascular compromise.
- Changes in Foot Temperature:
- Mild Warmth: A localized area of the foot feeling slightly warmer than other areas or the contralateral foot could be an early sign of inflammation, a forming ulcer, or the very beginning of acute
Charcot foot . - Mild Coolness: A foot that consistently feels slightly cooler than the other, or generally cool, could indicate subtle reduction in blood flow, suggesting early peripheral artery disease.
- Mild Warmth: A localized area of the foot feeling slightly warmer than other areas or the contralateral foot could be an early sign of inflammation, a forming ulcer, or the very beginning of acute
- Hair Loss on the Toes and Dorsum of the Foot: This is a very important, though often overlooked,
early sign of peripheral artery disease . Reduced blood flow deprives hair follicles of necessary nutrients, leading to thinning or complete absence of hair on the feet and lower legs. - Shiny, Thin Skin: The skin on the lower legs and feet may appear unnaturally shiny and thin, indicating reduced blood supply and atrophy of the skin layers. This is an
early visual symptom of vascular compromise . - Nail Changes:
- Thickening or Discoloration of Toenails: While often fungal,
onychomycosis is more prevalent and harder to treat in diabetics. Early signs include yellowing, slight thickening, or brittleness of the nails. - Slow Nail Growth: Another subtle sign of reduced peripheral circulation.
- Thickening or Discoloration of Toenails: While often fungal,
- Tingling or Numbness: While not a visual symptom, patients may report these sensory changes as an
early sign of neuropathy . This lack of sensation is what predisposes them to unnoticed injuries, which then become visible problems. Visually, this leads to the next point. - Unexplained Blisters or Minor Wounds: Because of reduced sensation, a diabetic individual might not feel the friction or pressure that causes blisters or small cuts.
Early diabetic foot photos might show a seemingly innocent blister or a small abrasion that the patient can’t recall injuring, which is a red flag for neuropathy. - Muscle Weakness and Subtle Deformities: Early neuropathy can lead to minor muscle imbalances that, over time, can cause subtle deformities like the beginnings of hammertoes or a flattening of the arch. These are
early physical signs of biomechanical changes. - Edema (Swelling): Mild, localized swelling that is unexplained by injury could be an early indicator of inflammation or even the initial phase of
Charcot foot development . Persistent, mild swelling should always be investigated.
Skin rash Diabetic foot Images
Common
- Fungal Infections (Mycosis):
- Tinea Pedis (Athlete’s Foot): Very common in diabetic patients due to hyperglycemia compromising immune function and providing a favorable environment for fungal growth.
- Appearance: Characterized by redness, scaling, itching, burning, and sometimes blistering, particularly between the toes (interdigital) or on the soles and sides of the feet (‘moccasin’ type). Skin may appear macerated (white, soggy) in between toes.
- Implication: Fissures caused by tinea pedis can be entry points for bacterial infections, including cellulitis.
- Onychomycosis (Fungal Nail Infection):
- Appearance: Toenails become thickened, brittle, discolored (yellow, brown, white), and often crumble at the edges. The nail plate may separate from the nail bed.
- Implication: Can create pressure points under the nail, leading to pain and potentially nail bed ulceration, and acts as a reservoir for fungal spores.
- Tinea Pedis (Athlete’s Foot): Very common in diabetic patients due to hyperglycemia compromising immune function and providing a favorable environment for fungal growth.
- Bacterial Infections:
- Cellulitis: A common bacterial infection of the skin and subcutaneous tissue.
- Appearance: Spreading redness (erythema), warmth, swelling, and tenderness of the affected area. The borders are often ill-defined. Can occur anywhere on the foot, often starting from a break in the skin (e.g., fissure, ulcer, insect bite).
- Implication: Can rapidly spread and lead to deeper tissue infections, including osteomyelitis and sepsis, if not treated promptly with antibiotics.
- Erysipelas: A more superficial form of cellulitis, caused by streptococcal bacteria.
- Appearance: Similar to cellulitis but typically has a sharply demarcated, raised, and erythematous (red) border. Often affects the dorsum of the foot.
- Implication: Like cellulitis, it requires immediate antibiotic treatment.
- Folliculitis/Furuncles: Infections of hair follicles.
- Appearance: Small, red, tender bumps (folliculitis) or larger, painful, pus-filled boils (furuncles/carbuncles) if multiple follicles are involved. Common on the dorsum of the foot or lower leg.
- Implication: Can lead to localized abscesses and potential spread of infection.
- Cellulitis: A common bacterial infection of the skin and subcutaneous tissue.
- Diabetic Dermopathy (Shin Spots):
- Appearance: Small, round or oval, brownish, atrophic (thinned) skin lesions that often appear on the shins but can also be seen on the dorsum of the feet. They are typically asymptomatic and non-itchy.
- Implication: Considered a benign skin manifestation of diabetes, often indicative of microvascular disease, but not directly limb-threatening.
- Necrobiosis Lipoidica Diabeticorum (NLD):
- Appearance: Typically starts as small, red-brown papules that expand into irregular, yellowish-brown patches with a waxy, atrophic center and prominent telangiectasias (visible blood vessels). The borders are often purplish-red. Primarily on the shins but can occur on the feet.
- Implication: The skin in the affected areas can be thin and prone to ulceration with minor trauma, which can be difficult to heal.
- Diabetic Blisters (Bullosis Diabeticorum):
- Appearance: Spontaneous, often painless, non-inflammatory blisters (bullae) that can be large and tense, filled with clear fluid (serous) or sometimes blood (hemorrhagic). They typically appear on the dorsum of the feet and toes.
- Implication: While usually benign and self-healing, they can rupture, creating open wounds that are prone to secondary bacterial infection in diabetic patients.
- Acanthosis Nigricans:
- Appearance: Darkening and thickening of the skin, giving it a velvety texture. While most common in body folds (neck, armpits), it can also affect the dorsum of the feet and toes.
- Implication: A sign of insulin resistance, often seen in individuals with uncontrolled diabetes.
- Dry Skin and Fissures:
- Appearance: Excessively dry, scaly, and sometimes itchy skin, particularly on the heels and soles. Deep cracks (fissures) can develop, which may be painful and bleed.
- Implication: These cracks provide easy entry points for bacteria, increasing the risk of cellulitis and other
diabetic foot infections .
- Contact Dermatitis:
- Appearance: Red, itchy, sometimes blistering rash caused by an allergic reaction to topical agents (creams, ointments), shoe materials, or socks.
- Implication: Can lead to skin breakdown and secondary infection due to scratching or irritation.
Diabetic foot Treatment
Effective
Key components of
- Wound Care and Debridement:
- Regular Dressing Changes: Utilizing advanced wound dressings that maintain a moist wound environment, absorb exudate, and protect the wound from infection. Types include hydrocolloids, foams, alginates, hydrogels, and silver-impregnated dressings.
- Debridement: The removal of necrotic (dead) tissue, foreign material, and callus from the wound bed. This is crucial for promoting healing and reducing the risk of infection. Methods include:
- Surgical Debridement: Using scalpels, scissors, or curettes.
- Autolytic Debridement: Using the body’s own enzymes with occlusive dressings.
- Enzymatic Debridement: Application of topical enzymatic agents.
- Mechanical Debridement: Wet-to-dry dressings (less common now), wound irrigation.
- Biologic Debridement (Maggot Therapy): Using medical-grade maggots to selectively remove necrotic tissue.
- Offloading: Reducing pressure on the ulcerated area is fundamental for healing.
- Total Contact Cast (TCC): Considered the gold standard for neuropathic plantar ulcers, it immobilizes the foot and evenly distributes weight.
- Removable Cast Walkers (RCWs) or Offloading Boots: Provide pressure relief and allow for wound inspection.
- Surgical Shoes and Custom Orthotics: For long-term pressure redistribution and prevention of recurrence.
- Crutches or Wheelchairs: For temporary complete non-weight-bearing in severe cases.
- Infection Management:
- Antibiotic Therapy: Crucial for treating
diabetic foot infections . Selection of antibiotics is guided by wound cultures and sensitivities to target specific bacteria (e.g., broad-spectrum initially, then tailored). Oral antibiotics for mild infections, intravenous for moderate to severe cases, or if osteomyelitis is suspected. - Surgical Drainage: Incision and drainage of abscesses to remove pus and relieve pressure.
- Debridement of Infected Tissue: Removal of infected bone (osteomyelitis) or soft tissue to control the spread of infection.
- Antibiotic Therapy: Crucial for treating
- Vascular Assessment and Revascularization:
- Peripheral Artery Disease (PAD) Management: If
peripheral artery disease is present, improving blood flow is vital for wound healing. - Vascular Consult: Referral to a vascular surgeon for assessment of blood flow.
- Revascularization Procedures:
- Angioplasty and Stenting: Minimally invasive procedures to open blocked arteries.
- Bypass Surgery: Creating a new path for blood flow around a blocked artery using a graft.
- Peripheral Artery Disease (PAD) Management: If
- Glycemic Control:
- Blood Glucose Management: Strict control of blood sugar levels is essential for overall health, improved immune function, and better wound healing outcomes. This involves diet, exercise, oral medications, or insulin.
- Foot Deformity Correction (Charcot Foot Management):
- Immobilization: In the acute phase of
Charcot foot , strict non-weight-bearing and immobilization (e.g., TCC) are crucial to prevent further bone destruction and deformity. - Surgical Reconstruction: In chronic Charcot foot with severe deformity and instability, surgical correction may be necessary to stabilize the foot, remove bony prominences, and prevent ulcer recurrence.
- Immobilization: In the acute phase of
- Amputation:
- Last Resort: Amputation may be necessary in cases of uncontrollable infection, extensive tissue necrosis (gangrene), or severe deformity that cannot be salvaged and poses a threat to life or quality of life.
- Goal: To remove the non-viable part of the limb and preserve as much healthy tissue as possible, aiming for a functional stump for prosthetic fitting.
- Preventative Measures and Education:
- Daily Foot Inspections: Educating patients on how to check their feet daily for cuts, blisters, redness, swelling, or any
diabetic foot symptoms pictures . - Proper Footwear: Wearing well-fitting, protective shoes (therapeutic shoes for high-risk patients) to prevent friction and pressure injuries.
- Foot Hygiene: Regular washing, careful drying (especially between toes), and moisturizing (avoiding between toes).
- Nail Care: Proper trimming of toenails (straight across) by a podiatrist, especially for those with neuropathy or vascular disease.
- Regular Podiatric Care: Routine visits to a podiatrist for callus debridement, nail care, and early detection of problems.
- Smoking Cessation: Crucial for improving circulation and overall health, as smoking severely exacerbates PAD.
- Daily Foot Inspections: Educating patients on how to check their feet daily for cuts, blisters, redness, swelling, or any
- Emerging Therapies:
- Hyperbaric Oxygen Therapy (HBOT): Delivering 100% oxygen at increased atmospheric pressure to improve oxygenation to ischemic wounds.
- Growth Factors and Biologic Skin Substitutes: Topical application of agents or engineered skin grafts to promote wound healing.