This article delves into the visual characteristics and various presentations of hemangiomas, providing detailed descriptions to accompany Hemangioma symptoms pictures. Understanding these distinct appearances is crucial for identification and subsequent management of these common vascular birthmarks.
Hemangioma Symptoms Pictures
When reviewing Hemangioma symptoms pictures, a range of visual cues immediately stands out, defining these distinct vascular lesions. The appearance of a hemangioma is highly variable, influenced by its depth, stage of development, and location. Superficial hemangiomas, often referred to as strawberry hemangiomas, are among the most commonly encountered types. These typically present as bright red, raised lesions with a distinct lobulated or bumpy surface, resembling a ripe strawberry. The intensity of the red color can vary from a light crimson to a deep scarlet, often becoming more vivid during periods of crying or straining due to increased blood flow. The texture is usually soft and compressible, feeling spongy to the touch.
Deep hemangiomas, also known as cavernous hemangiomas or subcutaneous hemangiomas, present a different set of visual characteristics in Hemangioma symptoms pictures. These lesions develop beneath the skin’s surface and may appear as a bluish or purplish mass, sometimes with a faint overlying telangiectatic (spider-vein like) network. The skin above a deep hemangioma might be normal in color, or slightly discolored. These deeper lesions tend to be more diffuse and less defined than their superficial counterparts, often feeling rubbery or doughy upon palpation. They can cause swelling or a noticeable bulge in the affected area, and their color can intensify when the child is crying or straining, similar to superficial hemangiomas, due to engorgement of the vascular channels.
Mixed hemangiomas combine features of both superficial and deep components. In such Hemangioma symptoms pictures, one might observe a bright red, raised superficial component overlying a deeper, bluish mass. This combination can result in a complex and often larger lesion, with significant elevation and a distinct coloration gradient. The edges of hemangiomas, particularly infantile hemangiomas, are typically well-defined during their proliferative phase, creating a clear demarcation from the surrounding normal skin. However, in larger or more diffuse lesions, the borders can be less distinct, blending gradually into the healthy tissue. The size of hemangiomas shown in Hemangioma symptoms pictures can range from a pinprick size at onset to several centimeters or even larger, covering extensive anatomical areas.
Key visual indicators to observe in Hemangioma symptoms pictures include:
- Coloration: Bright red (superficial), bluish-purple (deep), or a combination. The color may deepen with crying or straining.
- Texture: Soft, spongy, rubbery, or doughy. Often lobulated or bumpy for superficial types.
- Elevation: Raised above the skin surface (superficial) or a palpable subcutaneous mass (deep).
- Shape: Typically irregular or somewhat oval/round, with well-defined or diffuse borders.
- Location: Commonly found on the head and neck, but can appear anywhere on the body, including internal organs, though external presentation is usually what is seen in symptom pictures.
- Growth Pattern: Pictures may show rapid growth during the first few months of life, a key characteristic of infantile hemangioma.
Understanding these visual characteristics helps in the initial identification of these common vascular birthmarks and distinguishes them from other skin lesions. The detailed observation of these symptoms as presented in various Hemangioma symptoms pictures is invaluable for medical professionals and parents alike.
Signs of Hemangioma Pictures
The signs of hemangioma pictures often extend beyond mere appearance, capturing the dynamic nature and potential implications of these skin lesions. One of the most critical signs is the rapid growth phase, or proliferating hemangioma, which is evident in many image series. Initially, a hemangioma might appear as a faint red mark, a pale spot, or a network of tiny blood vessels. Within the first few weeks or months after birth, these precursor signs quickly develop into a more prominent, raised, and intensely colored lesion. Pictures documenting this growth can show a marked increase in size, height, and vascularity over a relatively short period, typically peaking around 5-7 months of age for infantile hemangiomas. This proliferative phase is characterized by a high rate of endothelial cell division, leading to the rapid expansion of the lesion.
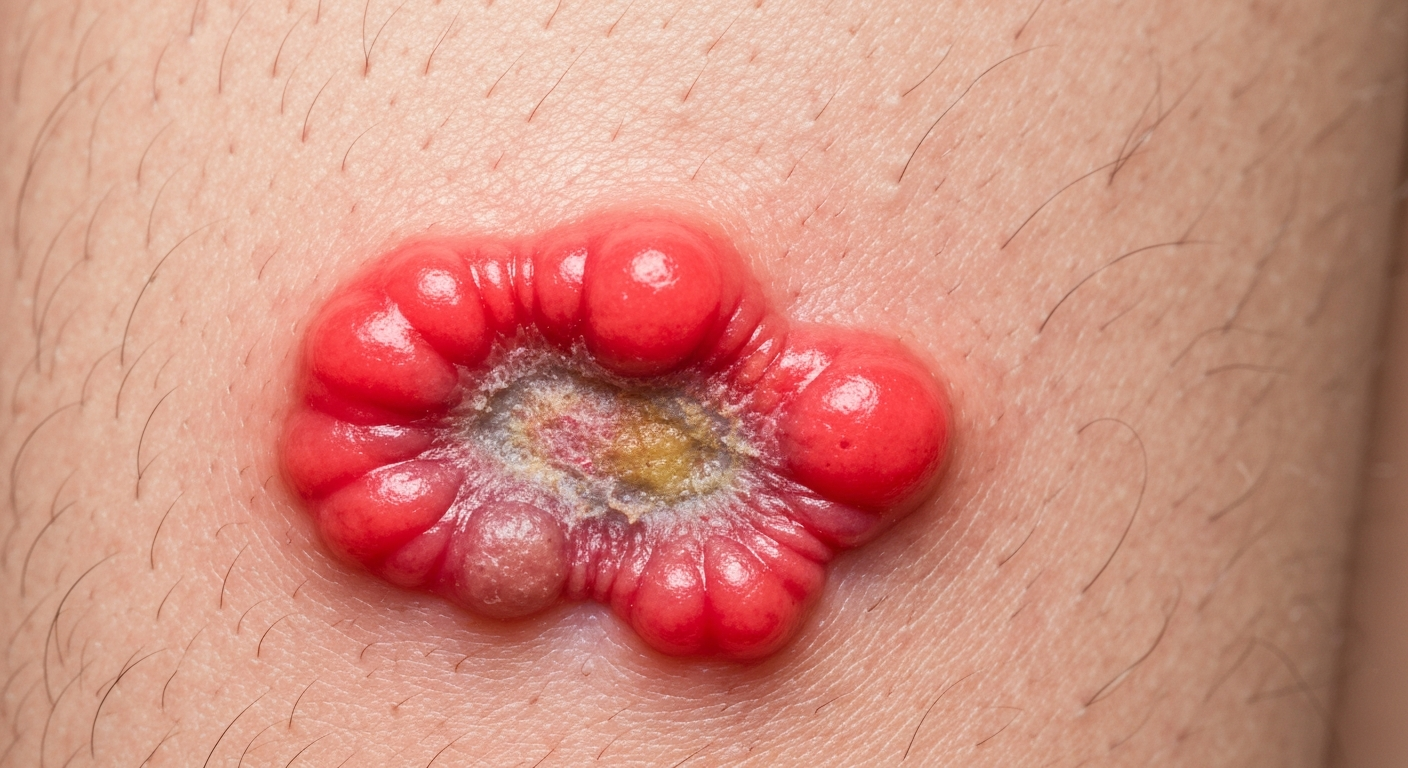
Another crucial sign visible in Hemangioma symptoms pictures relates to their location and potential for complications. Hemangiomas near sensitive areas like the eye, nose, mouth, or groin can present with specific signs of functional impairment. For instance, an hemangioma on the eyelid might obscure vision, leading to signs of amblyopia (lazy eye), while those around the mouth can interfere with feeding. Hemangiomas in the diaper area or skin folds are particularly prone to ulceration, a common and painful complication. Pictures of ulcerated hemangiomas reveal an open wound, often with a grayish or yellowish base, surrounded by a red, inflamed border. These images highlight not just the lesion itself, but the secondary signs of pain, infection, and potential scarring.
In addition to growth and complications, signs of hemangioma pictures also illustrate the involution phase, where the hemangioma naturally regresses. This process, known as involuting hemangioma, typically begins after the first year of life and can continue for several years. Pictures taken during involution show the lesion gradually losing its bright red color, becoming duller, often turning a grayish or purplish hue. The texture also changes, becoming softer, flatter, and sometimes demonstrating a telangiectatic (spider-vein like) network as the lesion resolves. Residual skin changes after complete involution might include some telangiectasias, skin atrophy, textural changes, or slight discoloration, which are also important signs to recognize in long-term observational photos.
Specific signs to look for in signs of hemangioma pictures:
- Early Precursors: Faint red macular patch, pallor, or telangiectatic macule visible shortly after birth.
- Rapid Proliferation: Marked increase in size, elevation, and color intensity within the first few months, indicating a proliferating hemangioma.
- Functional Impairment: Lesions causing visual obstruction (eyelid), airway compromise (neck/airway), feeding difficulties (lip/mouth), or hearing impairment (ear canal).
- Ulceration: Open sores, crusting, bleeding, or signs of secondary infection, especially in high-friction areas. These ulcerated hemangiomas are particularly painful.
- Regression (Involution): Fading color (from bright red to dull red, purple, or gray), flattening of the lesion, softening of texture, and visible telangiectasias within the regressing tissue.
- Segmental Hemangiomas: Large, plaque-like lesions that follow a dermatomal distribution, potentially associated with PHACE syndrome (Posterior fossa malformations, Hemangioma, Arterial anomalies, Cardiac defects, Eye abnormalities). These represent a distinct category of vascular birthmark.
- “Blueberry Muffin Baby” Syndrome: Though rare, this appearance, characterized by diffuse bluish-purple skin nodules, can indicate extensive multifocal hemangiomatosis or congenital hemangiomas with potential systemic involvement, a serious sign requiring immediate medical attention.
Observing these various signs across different stages and presentations in Hemangioma symptoms pictures provides a comprehensive understanding of the condition’s progression and potential complications, guiding appropriate intervention strategies.
Early Hemangioma Photos
Examining early Hemangioma photos is critical for understanding the initial presentation and subsequent rapid development of these common vascular birthmarks. Unlike other birthmarks that are often present at birth, infantile hemangiomas typically appear a few days to a few weeks after birth. The earliest signs can be very subtle, often leading parents to initially overlook them or mistake them for a scratch or a bruise. In many early Hemangioma photos, the lesion might first manifest as a faint red macule (a flat spot) with indistinct borders, a pale area that later turns red, or a very subtle telangiectatic patch where tiny blood vessels are visible. Sometimes, the initial presentation is simply a small, barely perceptible reddish dot or a cluster of tiny red capillaries, which then begins its characteristic rapid growth.
Within the first month of life, these subtle precursors start to change. Early Hemangioma photos from this period often show the lesion becoming slightly raised, with an intensifying red color. This is the beginning of the proliferative phase, where the endothelial cells rapidly multiply. For superficial hemangiomas (also known as strawberry hemangiomas), the lesion quickly evolves into a bright red, raised papule or nodule, with the characteristic bumpy or lobulated surface becoming more pronounced. The color saturation increases significantly, making the lesion much more noticeable. Parents observing these early changes in their child’s skin are often the first to notice the characteristic rapid growth. It’s important to recognize that this early, rapid growth is a hallmark of infantile hemangiomas and sets them apart from other congenital vascular lesions.
For deep or mixed hemangiomas, the earliest signs in early Hemangioma photos can be even more challenging to identify. A deep hemangioma might initially present as a subtle swelling or a slight bluish discoloration beneath the skin, without the prominent red surface component. These subcutaneous lesions might not become obviously apparent until they have grown to a larger size, manifesting as a soft, palpable mass. The skin overlying a deep hemangioma might appear normal or slightly discolored, making initial diagnosis more difficult without careful palpation or further imaging. However, even these deep lesions show signs of rapid growth in early stages, with the swelling becoming more pronounced over weeks.
Key initial presentations captured in early Hemangioma photos:
- Red Macule: A flat, red spot that may be mistaken for a scratch or mosquito bite.
- Pale Patch: An area of pallor on the skin that subsequently develops into a red lesion.
- Telangiectatic Patch: A subtle network of visible fine blood vessels.
- Small Papule: A slightly raised, often faintly red bump, appearing within days or weeks of birth.
- Bluish Discoloration: For deep hemangiomas, a subtle bluish tint beneath the skin, potentially with some swelling.
- Rapid Proliferation: The most defining feature visible in serial early Hemangioma photos, showing significant growth in size and prominence over weeks to months, typically peaking around 5-7 months of age. This differentiates them from congenital hemangiomas, which are fully formed at birth.
- “Halo” of Pallor: Sometimes, a faint pale rim around a developing hemangioma can be seen, though less common.
The progression seen in early Hemangioma photos emphasizes the dynamic nature of these lesions. Early identification is crucial for monitoring and, if necessary, timely intervention, particularly for those in high-risk locations or those showing signs of rapid, problematic growth. Parents should be encouraged to monitor any suspicious spots on their newborn and consult a healthcare professional, especially if rapid changes are observed.
Skin rash Hemangioma Images
The distinction between a skin rash and a hemangioma is a critical aspect when evaluating skin rash Hemangioma images. While some superficial hemangiomas, particularly early or unusually flat ones, might be initially confused with certain types of rashes, key characteristics readily differentiate them. A typical strawberry hemangioma, for instance, is a specific type of red birthmark that is a benign tumor of endothelial cells, not an inflammatory reaction like most rashes. In skin rash Hemangioma images, a hemangioma usually appears as a well-demarcated, raised, often lobulated bright red lesion. Unlike many rashes that tend to be diffuse, itchy, or blanchable (lose color when pressed), hemangiomas have a consistent appearance and feel.
When examining skin rash Hemangioma images, consider the following differentiating factors:
- Texture and Elevation: Hemangiomas are almost always raised above the skin surface (unless deep), with a distinct, often bumpy or spongy texture. Rashes, in contrast, can be maculopapular (flat and bumpy), vesicular (blister-like), or urticarial (hives-like), and rarely have the specific firm-yet-compressible feel of a hemangioma.
- Coloration Stability: The bright red color of a superficial hemangioma is due to densely packed blood vessels and typically does not blanch completely when pressed, unlike many inflammatory rashes which temporarily turn white. The color of a hemangioma is also stable over time, unless it’s growing or involuting, whereas rash colors can vary daily or with treatment.
- Growth Pattern: Infantile hemangiomas exhibit a characteristic growth phase in the first few months of life, increasing in size and prominence. Rashes, on the other hand, typically spread, resolve, or change in pattern rather than growing as a cohesive, localized mass.
- Symptoms: Most hemangiomas are asymptomatic, meaning they do not itch or cause discomfort unless they are ulcerated or located in a high-friction area. Rashes are frequently accompanied by itching, burning, stinging, or pain.
- Onset: Infantile hemangiomas typically appear days to weeks after birth, whereas many neonatal rashes (e.g., erythema toxicum neonatorum) appear within the first few days and resolve quickly. Allergic rashes or viral exanthems usually have a sudden onset due to an external trigger or systemic illness.
- Border Definition: Hemangiomas often have clear, well-defined borders separating them from normal skin, especially during their proliferative phase. Many rashes have irregular, spreading, or ill-defined borders.
There are instances where a hemangioma can be complicated by inflammation or infection, which might cause it to resemble an angry rash. For example, an ulcerated hemangioma can present with redness, swelling, and purulent discharge around the open wound, mimicking an infected skin lesion. However, careful examination will still reveal the underlying hemangioma structure. Pictures of these complicated cases are particularly challenging but underscore the importance of accurate diagnosis to ensure proper treatment. Similarly, extensive segmental hemangiomas can cover a large area, appearing somewhat plaque-like, which might, at a glance, be misidentified as a widespread skin condition. However, their characteristic vascular proliferation distinguishes them.
It is important to remember that while a skin rash Hemangioma image might show some superficial similarities, the underlying pathology and clinical course are vastly different. Consulting a dermatologist or pediatrician for accurate diagnosis is always recommended when a new skin lesion appears on an infant. Understanding these visual distinctions helps in avoiding misdiagnosis and ensuring appropriate management for these common red birthmarks, which are benign vascular tumors and not inflammatory dermatoses.
Hemangioma Treatment
The approach to Hemangioma treatment is highly individualized, depending on the hemangioma’s type, size, location, rate of growth, presence of complications, and the child’s overall health. Not all hemangiomas require active intervention; many infantile hemangiomas are small, asymptomatic, and located in areas where they pose no functional or cosmetic risk, allowing for a strategy of watchful waiting. However, for those requiring intervention, a range of effective treatment options is available, as often highlighted in before-and-after Hemangioma symptoms pictures of successful cases.
Pharmacological Treatments:
The most significant advancement in Hemangioma treatment has been the use of beta-blockers:
- Oral Propranolol: This is currently the first-line systemic treatment for problematic infantile hemangiomas. Propranolol works by constricting blood vessels, decreasing blood flow to the hemangioma, inhibiting angiogenesis (the formation of new blood vessels), and inducing apoptosis (programmed cell death) of hemangioma cells. Its effectiveness is particularly evident in reducing the size, color, and elevation of rapidly proliferating lesions. Treatment typically starts at a low dose and is gradually increased, continuing for several months to a year or more. The visual improvement seen in Hemangioma symptoms pictures after several weeks of propranolol is often dramatic, with lesions becoming paler, softer, and flatter.
- Topical Timolol: For smaller, superficial hemangiomas, especially those not at risk for ulceration or functional impairment, topical timolol gel or solution can be an effective alternative. Applied directly to the lesion, timolol also constricts blood vessels and inhibits growth, often leading to a reduction in color and volume. This treatment is less invasive than oral medication and typically has fewer systemic side effects, making it suitable for mild to moderate strawberry hemangiomas.
- Corticosteroids: Historically used before beta-blockers, systemic corticosteroids (e.g., prednisone) can be used for rapidly growing or life-threatening hemangiomas. They work by inhibiting hemangioma growth. However, due to significant potential side effects (e.g., growth retardation, immunosuppression), they are now typically reserved for cases unresponsive to or intolerant of propranolol. Intralesional corticosteroids can be used for smaller, localized lesions, often providing temporary reduction.
Laser Therapy:
- Pulsed Dye Laser (PDL): This laser targets the superficial blood vessels, making it effective for treating residual telangiectasias or areas of redness after a hemangioma has largely involuted. It can also be used in some cases to treat ulcerated hemangiomas by promoting healing and reducing pain. PDL is generally less effective for treating the bulk of a rapidly growing hemangioma but is excellent for improving skin texture and reducing residual red color that might be seen in post-involution Hemangioma symptoms pictures.
Surgical Excision:
- Surgical removal is an option for certain hemangiomas, particularly those that are small, well-demarcated, or have completed their involution and left behind significant residual skin changes (e.g., fibrofatty residuum, redundant skin). It is also considered for ulcerated lesions that are unresponsive to medical therapy, or for hemangiomas causing functional impairment that cannot be managed otherwise. Early surgical excision might be considered for small, rapidly growing lesions in cosmetically sensitive areas, to prevent extensive proliferation and improve long-term cosmetic outcomes. Surgical removal offers a definitive solution and can significantly improve the appearance as demonstrated in post-operative Hemangioma symptoms pictures.
Treatment for Complications:
- Ulceration: This painful complication requires prompt attention. Treatment includes pain management, wound care (e.g., topical antibiotics, occlusive dressings), and often systemic or topical beta-blockers to accelerate healing. Laser therapy can also be beneficial in promoting re-epithelialization.
- Functional Impairment: Hemangiomas affecting vision, breathing, or feeding often necessitate aggressive systemic treatment with propranolol to shrink the lesion rapidly and prevent permanent damage.
Watchful Waiting:
- For many small, uncomplicated infantile hemangiomas, the most appropriate “treatment” is observation. Given that most hemangiomas eventually involute naturally, careful monitoring by a healthcare professional is sufficient. This approach minimizes unnecessary medical intervention and its associated risks. Parents are usually provided with detailed information and Hemangioma symptoms pictures to understand the natural course of involution and identify any signs of complications that would necessitate active intervention.
The decision to treat a hemangioma and the choice of treatment modality are complex, requiring careful consideration of various factors by an experienced multidisciplinary team, including pediatricians, dermatologists, plastic surgeons, and sometimes ophthalmologists or ENT specialists. The goal of Hemangioma treatment is always to ensure the best possible functional and cosmetic outcome for the child, minimizing morbidity and distress.