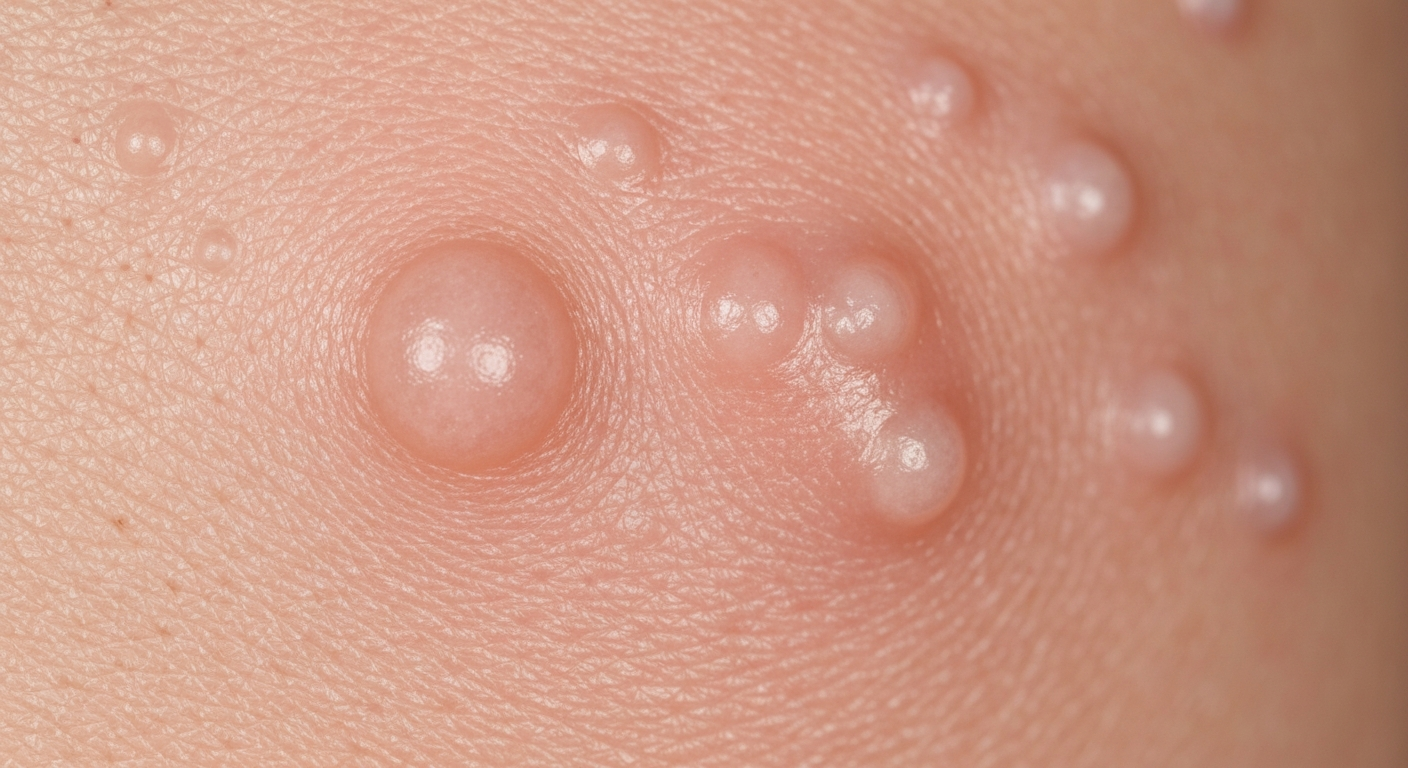
Understanding what does Milia look like symptoms pictures is crucial for accurate self-assessment and effective management. These small, pearl-like cysts present with distinct visual characteristics, allowing individuals to identify them based on their appearance and associated lack of traditional skin rash symptoms.
Milia Symptoms Pictures
When examining milia symptoms pictures, the most prominent visual characteristic is the appearance of small, raised, dome-shaped bumps on the skin. These lesions are typically white or yellowish, firm to the touch, and non-tender. Unlike acne or other inflammatory lesions, milia do not have a central pore or opening, nor do they exhibit signs of inflammation such as redness, swelling, or pus. They are essentially tiny cysts filled with trapped keratin, a protein found in skin, hair, and nails.
The size of individual milia usually ranges from 1 to 2 millimeters in diameter, though they can sometimes be smaller or slightly larger. They often appear in clusters, especially around the eyes, nose, and cheeks, but can also be found on other parts of the face and body. The distinct coloration—often described as pearly white or creamy yellow—is a key identifier in milia appearance. These keratin cysts are superficial, lying just beneath the outermost layer of the skin (epidermis), which contributes to their characteristic opaque look.
Primary milia occur spontaneously and are common in newborns (neonatal milia), where they are often observed on the nose, chin, and cheeks. In adults, primary milia can develop on the eyelids, forehead, and around the eyes. They are benign and typically resolve on their own in infants but may persist in adults or require intervention. Secondary milia, on the other hand, develop as a result of trauma to the skin, such as burns, blistering skin conditions (e.g., bullous pemphigoid, epidermolysis bullosa), long-term steroid cream use, certain medical procedures (like dermabrasion or laser resurfacing), or even after severe sun exposure. The visual distinction in secondary milia pictures might include their presence within scars or areas of previously damaged skin, sometimes exhibiting a slightly more irregular distribution.
Important visual characteristics to note in milia symptom photos include:
- Coloration: Predominantly white or yellowish-white, giving them a pearl-like or seed-like quality.
- Size: Small, typically 1-2 mm in diameter, but can vary slightly.
- Shape: Distinctly dome-shaped, raised above the skin surface with a smooth, firm texture.
- Distribution: Often clustered, particularly on the face (cheeks, nose, eyelids, forehead) but can appear anywhere.
- Lack of inflammation: A crucial differentiating factor from other skin lesions; milia are not red, painful, itchy, or swollen. They lack the inflamed halo often seen around pimples or insect bites.
- Non-pustular: They do not contain pus, unlike pustules associated with acne. They are solid, keratin-filled cysts.
- Surface texture: The skin overlying milia is usually smooth and unbroken, contributing to their encapsulated appearance.
Observing milia pictures helps in understanding that these are distinct, self-contained entities, unlike diffuse rashes or blotches. They do not spread or change rapidly in size once formed, and their presence is purely cosmetic unless they become irritated by friction or improper attempts at extraction. The surrounding skin usually appears normal, highlighting the isolated nature of each milium.
Signs of Milia Pictures
When reviewing signs of milia pictures, one immediately observes the unmistakable tiny, white or yellow bumps that are a hallmark of this common skin condition. These are not merely visual symptoms but actual physical signs that help in identification. The most critical sign is the distinct appearance of encapsulated keratin within the dermis, manifesting as a small, firm, raised lesion. Unlike other skin eruptions, milia lack any associated inflammatory signs, meaning there’s no redness, tenderness, or warmth around the individual bumps. This non-inflammatory nature is a key diagnostic sign that distinguishes milia from acne, folliculitis, or allergic reactions.
The typical milia signs observed in photographs include:
- Pearly or Opaque Bumps: Each milium appears as a small, pearly-white or yellowish lesion, reflecting the trapped keratin beneath the skin’s surface. The opacity is due to the compacted nature of the keratin.
- Smooth, Dome-Shaped Protrusions: The lesions are perfectly round or dome-shaped, feeling smooth to the touch and having clear, well-defined borders. They do not have irregular shapes or ragged edges.
- Lack of Central Pore: Unlike blackheads or whiteheads (comedones), milia do not have an open pore or a visible plug that can be squeezed out easily. Attempting to squeeze them typically results in no discharge and can cause skin damage.
- Asymptomatic Nature: Milia are generally asymptomatic. They do not itch, burn, or cause pain. This lack of sensation is a significant diagnostic sign and contrasts sharply with many other skin conditions that present with similar-sized bumps.
- Persistent Presence: Once formed, milia tend to persist for weeks, months, or even longer unless they are naturally exfoliated or medically extracted. They do not typically come and go quickly like inflammatory pimples.
- Common Locations: While milia can appear anywhere, their common presentation on the face, particularly around the eyes, on the cheeks, nose, and forehead, is a recognizable sign in milia photos. They can also occur on the chest, back, and even genitals, especially in secondary forms.
Different types of milia exhibit subtle variations in their presentation that can be seen in milia pictures by type:
- Neonatal Milia: These are seen in up to 50% of newborns and babies, typically appearing on the nose, cheeks, chin, and forehead. They are usually abundant and often appear within the first few weeks of life, resolving spontaneously within a few months. The photos of neonatal milia signs show numerous, very tiny, widespread white bumps on baby skin.
- Primary Milia (Children and Adults): Similar in appearance to neonatal milia but occurring outside the neonatal period. They are more persistent and may appear singly or in small clusters. Locations include eyelids, forehead, temples, and genital areas.
- Juvenile Milia: A rare genetic form, often associated with inherited conditions such as Basal Cell Nevus Syndrome or Rombo Syndrome. Juvenile milia photos might show milia alongside other characteristic skin lesions or abnormalities.
- Milia en Plaque: This is a rarer form where milia appear on an erythematous (red), edematous (swollen) plaque. It most commonly affects the eyelids, behind the ears, or on the jawline. While individual milia are non-inflammatory, the surrounding skin in milia en plaque pictures shows inflammation, making it an important variant to recognize.
- Multiple Eruptive Milia: Characterized by the sudden onset of numerous milia, appearing in crops over weeks or months. These often appear on the face, upper arms, and trunk. Eruptive milia images typically show a more widespread distribution, almost resembling a rash due to their sheer number.
- Secondary Milia: These develop following skin trauma or damage, such as burns, blistering diseases, prolonged use of topical steroids, or after cosmetic procedures. The signs of secondary milia often include their presence within scar tissue or areas of previous injury, suggesting a different etiology than primary milia.
In summary, the key signs of milia observable in photographs are their specific morphology (small, firm, white/yellow, dome-shaped, non-inflammatory bumps lacking a central pore) and their distribution. These visual cues are critical for differentiating milia from other skin conditions and understanding their underlying nature as keratin retention cysts.
Early Milia Photos
Observing early milia photos reveals the nascent stages of these small, keratin-filled cysts, which can be quite subtle. At their onset, milia often appear as incredibly tiny, almost pinprick-sized white or yellowish dots that are just barely perceptible. They begin as microscopic plugs of keratin forming within the hair follicles or eccrine sweat ducts, eventually growing into the more recognizable dome-shaped bumps. The progression from an initial, nearly invisible blockage to a distinct milium can take weeks or even months, depending on various factors including skin type, age, and individual exfoliation rates.
The initial appearance of developing milia might be mistaken for simply slightly textured skin or very minute pores that are somewhat occluded. They typically lack any redness or inflammation even at their earliest stages, maintaining their non-inflammatory characteristic from the very beginning. In early milia pictures, one might see:
- Microscopic Size: The very first signs of milia are often less than 1 mm, appearing as fine grains or specks on the skin surface.
- Subtle Elevation: They may only be slightly raised, making them more noticeable by touch than by sight initially.
- Faint Coloration: The white or yellowish hue might be very pale, especially on lighter skin tones, making them blend in more readily with the surrounding skin.
- Isolated or Sparse Distribution: Early on, milia might appear as single, isolated lesions rather than clusters. Over time, more may develop in proximity, or existing ones may become more numerous.
- Areas of Fine Lines: Due to their common locations (e.g., around the eyes), initial milia can sometimes appear within fine lines or wrinkles, making them even harder to distinguish without close inspection.
For individuals prone to milia, particularly those with drier skin or after certain skin procedures, paying close attention to these early indications can be beneficial. Milia onset is often gradual. For instance, after a severe sunburn or certain dermatological treatments like laser resurfacing, new milia may begin to form as the skin heals and regenerates. In these cases, post-procedure milia photos will show numerous small, new lesions emerging over the treated area. The skin’s healing process can trap keratin and dead skin cells, leading to their formation.
In infants, early neonatal milia can appear within days of birth, manifesting as a sprinkle of tiny white spots, primarily on the nose and cheeks. These are classic examples of early, primary milia that often resolve spontaneously as the infant’s skin matures. For adults, detecting early milia formation often involves examining areas like the eyelids, temples, and upper cheeks with good lighting. The texture might feel slightly gritty or bumpy before the individual milia become distinctly visible. Products that clog pores or certain heavy creams can sometimes contribute to the formation of early milia by trapping dead skin cells and keratin, leading to their eventual emergence.
Recognizing early milia is primarily about acknowledging the very subtle changes in skin texture and color before the lesions become fully developed. This can be challenging without the benefit of magnified images, but understanding the progression from a tiny keratin plug to a visible milium helps in anticipating and potentially preventing their full development.
Skin rash Milia Images
While milia are not technically a skin rash, the term “skin rash milia images” is often used by individuals searching for visual comparisons because milia can sometimes appear in clusters, leading to a rash-like appearance, especially in conditions like multiple eruptive milia or when numerous secondary milia develop after skin trauma. It’s crucial to understand the fundamental difference: a true rash is typically characterized by inflammation, redness, itching, burning, or a diffuse change in skin texture and color across an area. Milia, by contrast, are discrete, non-inflammatory cysts.
When someone observes what they perceive as a “milia rash,” they are likely seeing a concentration of individual milia. In milia clusters photos, the skin is peppered with multiple small, white, or yellowish bumps. These clusters often occur on the face, particularly around the eyes and on the cheeks, but can also appear on the neck, chest, or back. The key differentiating factor from an actual rash is the lack of surrounding redness or inflammation for each individual lesion. The skin between the milia often appears completely normal in color and texture.
Specific scenarios where milia might mimic a rash include:
- Multiple Eruptive Milia: This condition involves the sudden appearance of numerous milia over weeks or months, often on the face, upper arms, or trunk. The sheer number and density of the milia can give the impression of a widespread eruption, leading people to search for “eruptive milia rash pictures.” However, even in this form, the individual milia retain their non-inflammatory character.
- Neonatal Milia: In infants, the abundance of tiny, white bumps on the nose, cheeks, and forehead can be quite extensive, leading parents to describe it as a baby skin rash. While harmless and self-resolving, these baby milia images show a widespread distribution that could be confused with an inflammatory rash.
- Secondary Milia after Damage: After severe burns, extensive blistering, or abrasive skin treatments, numerous milia can form in the healing areas. These post-trauma milia images might show a widespread distribution of milia across the damaged skin, which, from a distance, could be mistaken for a healing rash.
- Milia en Plaque: This rare variant does involve an erythematous (red) and edematous (swollen) plaque, on which milia are embedded. In this specific case, the underlying inflammatory plaque *is* a type of rash, with the milia forming within it. Milia en plaque images clearly show the inflamed base with the characteristic white milia embedded within it, making it an exception to the general non-inflammatory rule for milia.
Differentiating milia from skin rashes in pictures requires careful observation of several features:
- Inflammation: True rashes (like allergic dermatitis, acne vulgaris, rosacea, or folliculitis) almost always involve redness, swelling, and often itching or pain. Milia do not.
- Pus or Fluid: Many rashes (e.g., acne pustules, eczema vesicles) involve pus-filled or fluid-filled lesions. Milia are solid, keratin-filled cysts.
- Surface Opening: Conditions like blackheads and whiteheads (comedones) have a central pore. Milia do not.
- Texture Uniformity: While milia are uniform, true rashes often show variations in lesion type (papules, pustules, vesicles, scales, crusts) within the same area.
Looking at milia skin pictures side-by-side with images of common rashes like acne, eczema, or contact dermatitis highlights these crucial differences. For example, in acne, you would see various lesions like blackheads, whiteheads, red papules, and pustules, often with surrounding inflammation. Eczema images would show patches of red, itchy, scaly skin. Milia images, even when clustered, will consistently show discrete, non-reddened, white/yellow bumps. Understanding these visual cues is essential for accurate self-diagnosis and for seeking appropriate advice, distinguishing between harmless milia and potentially more serious skin rashes.
Milia Treatment
Addressing milia treatment options involves understanding that while many milia, especially in newborns, resolve spontaneously, persistent or cosmetically bothersome milia in adults often require intervention. The goal of milia removal is to safely extract the trapped keratin without damaging the surrounding skin or causing scarring. Self-extraction at home is generally discouraged due to the risk of infection, inflammation, and scarring, as milia are encapsulated and cannot be simply “popped” like a pimple.
A comprehensive approach to how to treat milia includes professional procedures, targeted topical treatments, and preventative skincare strategies.
Professional Milia Removal Procedures:
These are the most effective and safest methods for getting rid of established milia. A trained dermatologist or aesthetician will perform these procedures.
- Manual Extraction:
- Procedure: The most common method. A sterile lancet or a fine needle is used to create a tiny incision or prick on the top of the milium. The keratin plug is then gently extracted using a comedone extractor or by applying gentle pressure.
- Benefits: Highly effective, immediate results, minimal downtime, and usually no scarring when performed correctly.
- Ideal for: Individual or scattered milia, especially around delicate areas like the eyes.
- Keywords: milia extraction, professional milia removal, dermatologist milia treatment.
- Cryotherapy:
- Procedure: Liquid nitrogen is applied to individual milia, freezing and destroying the cyst. The frozen milium will then blister and eventually fall off.
- Benefits: Effective for stubborn milia; can treat multiple lesions.
- Considerations: Risk of temporary pigmentation changes (hypopigmentation or hyperpigmentation), especially on darker skin tones.
- Keywords: cryotherapy for milia, freezing milia, dermatologist milia removal.
- Laser Ablation:
- Procedure: A pulsed dye laser or a CO2 laser can be used to open and destroy the milia. The laser precisely targets the cyst, vaporizing the keratin.
- Benefits: Very precise, suitable for numerous milia or those in sensitive areas. Quick recovery.
- Considerations: Can be more expensive; requires specialized equipment and expertise.
- Keywords: laser treatment for milia, CO2 laser milia, pulsed dye laser milia.
- Electrocautery/Diathermy:
- Procedure: A fine, heated needle is used to burn and destroy the milium.
- Benefits: Effective for individual, persistent milia.
- Considerations: Requires precision to avoid scarring; can cause minor discomfort.
- Keywords: electrocautery milia, diathermy milia removal.
- Chemical Peels:
- Procedure: Applying chemical solutions (e.g., glycolic acid, salicylic acid, lactic acid) to the skin can promote exfoliation and encourage the milia to resolve.
- Benefits: Can help with widespread, superficial milia, and improve overall skin texture.
- Considerations: Usually requires multiple sessions; may cause temporary redness and peeling.
- Keywords: chemical peels for milia, glycolic acid peel, salicylic acid peel.
- Dermabrasion/Microdermabrasion:
- Procedure: These procedures involve exfoliating the outermost layers of the skin using a rapidly rotating brush (dermabrasion) or fine crystals/diamond tips (microdermabrasion). This can help dislodge superficial milia.
- Benefits: Improves overall skin texture and can remove superficial milia.
- Considerations: More effective for very superficial milia; dermabrasion has a longer recovery time than microdermabrasion.
- Keywords: microdermabrasion for milia, dermabrasion milia treatment.
Topical Milia Treatments (Often Used in Conjunction with Professional Care):
Certain topical agents can help prevent new milia formation or encourage existing ones to surface and resolve. These are typically used as part of a regular skincare routine.
- Retinoids (Vitamin A derivatives):
- Mechanism: Topical retinoids (e.g., tretinoin, adapalene, tazarotene) increase cell turnover and promote exfoliation, helping to prevent keratin from becoming trapped. They can also help existing superficial milia to resolve.
- Examples: Retin-A, Differin, Tazorac.
- Application: Applied nightly to clean, dry skin.
- Considerations: Can cause initial dryness, redness, and peeling (retinization); always use sunscreen.
- Keywords: topical retinoids for milia, tretinoin milia, adapalene milia treatment.
- Alpha Hydroxy Acids (AHAs):
- Mechanism: AHAs like glycolic acid or lactic acid are chemical exfoliants that loosen dead skin cells, preventing keratin buildup and promoting shedding.
- Examples: Glycolic acid cleansers, toners, or serums; lactic acid lotions.
- Application: Incorporated into a daily or weekly skincare routine.
- Considerations: Can increase sun sensitivity; start with lower concentrations to assess tolerance.
- Keywords: AHA for milia, glycolic acid milia treatment, lactic acid for milia.
- Salicylic Acid (BHA):
- Mechanism: A beta hydroxy acid that is oil-soluble, allowing it to penetrate into pores and exfoliate from within. While primarily for acne, it can help prevent milia in some cases by keeping pores clear.
- Application: Often found in cleansers, toners, and spot treatments.
- Considerations: Can be drying; use sparingly if skin is sensitive.
- Keywords: salicylic acid milia, BHA for milia.
Milia Prevention and Skincare:
Preventative measures are key for individuals prone to milia. A consistent and appropriate skincare routine can significantly reduce their occurrence.
- Gentle Cleansing:
- Use a mild, non-comedogenic cleanser twice daily to remove dirt, oil, and dead skin cells without stripping the skin.
- Keywords: milia prevention skincare, gentle cleanser for milia.
- Regular Exfoliation:
- Incorporate regular, gentle exfoliation to prevent dead skin cell buildup. This can be achieved through mild physical exfoliants (very fine scrubs, sparingly) or chemical exfoliants (AHAs, BHAs, retinoids).
- Keywords: exfoliation for milia, preventing milia.
- Non-Comedogenic Products:
- Always choose makeup, moisturizers, and sunscreens labeled “non-comedogenic” or “oil-free,” meaning they are formulated not to clog pores.
- Keywords: non-comedogenic products for milia, oil-free skincare.
- Sun Protection:
- Excessive sun exposure can damage the skin and thicken the outer layer, potentially trapping keratin. Use a broad-spectrum SPF 30+ sunscreen daily.
- Keywords: sunscreen for milia, sun protection milia.
- Avoid Heavy/Occlusive Products:
- Rich, heavy creams or ointments, especially around the eyes, can sometimes contribute to milia formation by creating an occlusive barrier that traps dead skin cells. Opt for lighter, gel-based formulations if prone to milia.
- Keywords: avoid heavy creams milia, light moisturizer for milia.
- Diet and Hydration:
- While not a direct cause, maintaining a healthy diet rich in vitamins and antioxidants, and staying well-hydrated, supports overall skin health, which can indirectly aid in preventing skin issues.
- Keywords: diet for healthy skin, hydration and milia.
For individuals with neonatal milia, no treatment is typically necessary as they usually disappear within a few weeks or months. Parents should avoid picking or squeezing them. For adults, consulting a dermatologist is the best course of action to determine the most suitable milia treatment plan based on the type, location, and number of milia, as well as individual skin characteristics.