When observing the aftermath of an outdoor excursion, understanding specific visual cues is paramount for identifying potential health concerns. This comprehensive guide provides detailed descriptions of various tick bite symptoms pictures, helping to distinguish common reactions from those indicative of serious tick-borne illnesses, ensuring timely recognition and appropriate action.
Tick bite Symptoms Pictures
Recognizing the diverse array of tick bite symptoms pictures is crucial for early detection and treatment of tick-borne diseases. A typical, benign tick bite will often present as a small, red, itchy bump, similar to a mosquito bite, appearing a few hours to a few days after the tick has detached or been removed. This localized reaction, characterized by redness, mild swelling, and itching, is primarily an inflammatory response to the tick’s saliva and the minor trauma of the bite itself. The appearance can vary significantly based on individual sensitivity, the specific tick species involved, and the duration of attachment. Some individuals may develop a slightly raised wheal, while others might only notice a faint pink spot. It is imperative to monitor these initial reactions closely for any changes that might suggest the development of a more serious condition. The site of the tick bite might feel warm to the touch, and persistent itching can lead to scratching, which further irritates the skin and can introduce secondary bacterial infections. These initial localized reactions are often transient, resolving within a few days without specific medical intervention, provided no infection has occurred. However, the absence of a severe local reaction does not rule out the possibility of a tick-borne illness, as many infections may not manifest with prominent local skin changes beyond the initial bite mark.
Beyond the immediate localized irritation, other symptoms might emerge depending on the type of tick and whether it transmitted a pathogen. Non-specific systemic symptoms are often the first indicators of a tick-borne illness, appearing days to weeks post-bite. These can include:
- Fever: Often low-grade initially, but can escalate, sometimes with chills.
- Fatigue: Persistent and unexplained tiredness, disproportionate to activity levels.
- Headache: Ranging from mild to severe, sometimes accompanied by neck stiffness.
- Muscle aches (myalgia): Generalized body pain and soreness.
- Joint pain (arthralgia): Aches in various joints, sometimes migratory.
- Nausea or vomiting: Gastrointestinal disturbances that can accompany systemic illness.
- Loss of appetite: A common symptom of many infections.
- Swollen lymph nodes: Lymphadenopathy, particularly near the bite site or generalized.
These constitutional symptoms, when present, should prompt immediate medical evaluation, especially if they follow a known or suspected tick exposure. The timing and combination of these symptoms provide valuable clues for diagnosis. For instance, a sudden onset of high fever, severe headache, and muscle pain within 14 days of a tick bite might suggest conditions like Rocky Mountain Spotted Fever (RMSF) or anaplasmosis. Conversely, a more gradual onset of fatigue, joint pain, and neurological symptoms could point towards later stages of Lyme disease. Documenting the progression of these symptoms, along with any skin manifestations, is vital for accurate diagnosis and effective tick bite treatment. Recognizing the spectrum of these symptoms, from subtle local irritation to severe systemic illness, is key to managing tick exposures proactively and preventing long-term complications. The visual characteristics of the bite site, especially changes over time, are critical pieces of diagnostic information that tick bite symptoms pictures aim to highlight for public awareness and healthcare provider education.
Signs of Tick bite Pictures
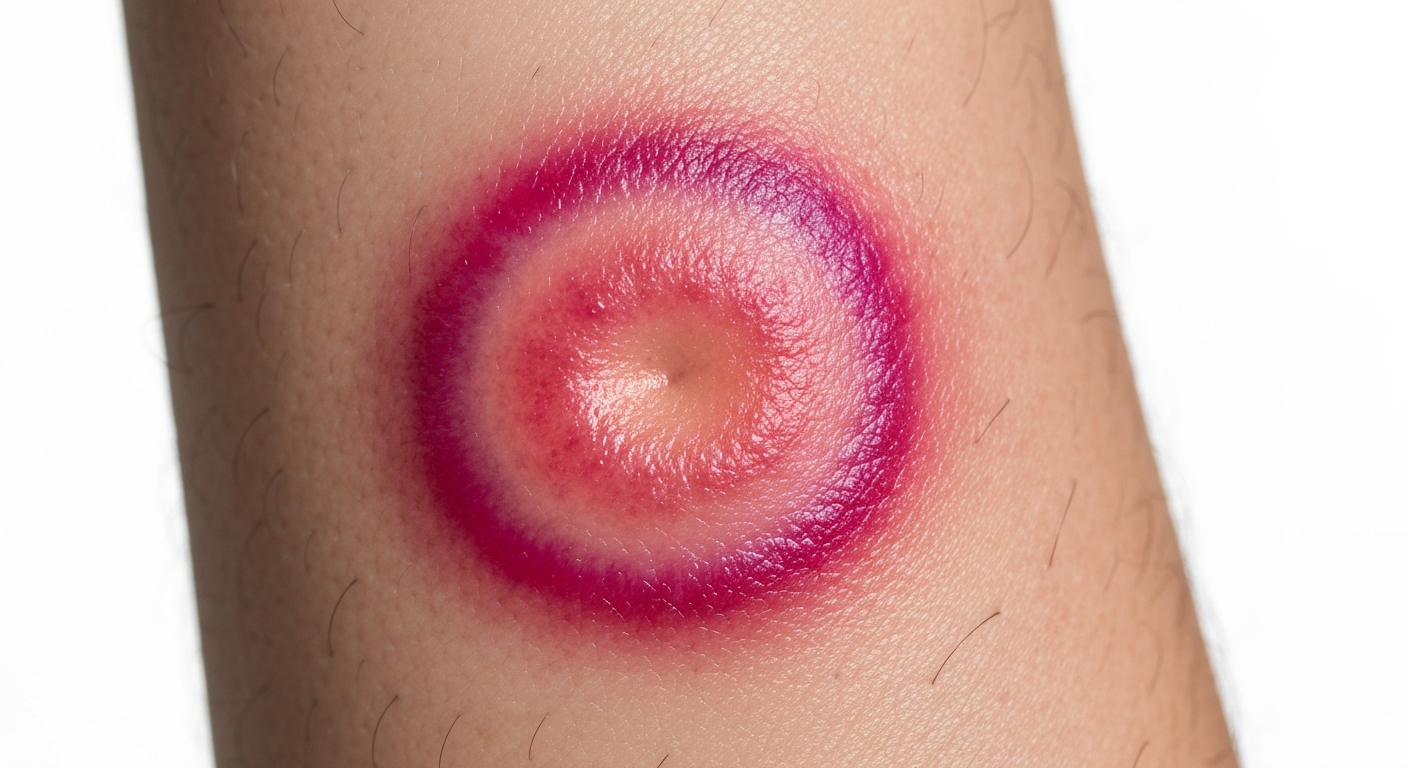
Examining signs of tick bite pictures allows for a visual comparison of various reactions and potential infections. The most direct sign, of course, is the tick itself, still embedded in the skin. Ticks can vary greatly in size, from tiny poppy seeds (nymphs) to engorged adult females resembling a small grape. They are typically dark brown, black, or reddish-brown and have eight legs in their adult stage. Once detached, the bite site often presents as a singular red papule or macule, sometimes with a tiny puncture mark at its center. This small, often itchy, red bump can persist for several days. However, the presence of specific rashes or patterns of redness is a much more significant sign, often indicating a tick-borne infection. For example, the classic “bull’s-eye” rash of Lyme disease, known as erythema migrans (EM), is a crucial diagnostic sign that often appears days to weeks after the bite. This expanding circular or oval rash, which can grow quite large (over 5 cm), may have central clearing, giving it its characteristic target-like appearance. Other rashes, such as the diffuse, maculopapular rash of Rocky Mountain Spotted Fever (RMSF), starting on the wrists and ankles and spreading centripetally, present entirely different visual clues that are critical for diagnosis.
Beyond distinct rashes, other observable signs related to tick bites and subsequent infections include:
- Persistent Local Redness and Swelling: If the initial bite site remains significantly red, swollen, or painful for an extended period (more than a few days) or begins to enlarge, it could be a sign of a localized infection or severe inflammatory reaction.
- Lymphadenopathy: Swollen, tender lymph nodes, particularly those in the drainage area of the bite (e.g., axillary nodes for an arm bite, inguinal nodes for a leg bite), can indicate a systemic immune response to an infection.
- Conjunctivitis: Red, irritated eyes can be a sign of certain tick-borne illnesses, such as tularemia, and might be observed in signs of tick bite pictures depicting affected individuals.
- Jaundice: Yellowing of the skin or eyes, though rare, can be a severe sign of certain tick-borne diseases like babesiosis in advanced stages, indicating liver involvement.
- Petechiae or Purpura: Small, pinpoint red or purple spots (petechiae) or larger bruised areas (purpura) on the skin, not blanching under pressure, can be a grave sign of severe RMSF or other hemorrhagic conditions, indicating capillary damage and coagulation disorders. These are critical signs to identify in any skin rash tick bite images.
- Neurological Changes: Observable signs might include facial palsy (Bell’s palsy), muscle weakness, or changes in gait, which can be late manifestations of Lyme neuroborreliosis.
- Arthritis: Visually observable joint swelling or effusion, particularly in large joints like the knee, can be a sign of Lyme arthritis.
The timeline of these signs is also an important diagnostic element. For example, erythema migrans typically appears within 3 to 30 days, while the RMSF rash usually develops within 2 to 5 days of fever onset. Awareness of these specific visual signs of tick bite pictures, alongside systemic symptoms, significantly aids in the prompt recognition and appropriate management of tick-borne diseases. Healthcare providers rely heavily on these visual cues, combined with patient history and laboratory tests, to confirm diagnoses and initiate effective tick bite treatment protocols. Therefore, a careful and observant approach to monitoring any post-tick exposure changes is paramount for safeguarding health.
Early Tick bite Photos
Early tick bite photos vividly illustrate the immediate and nascent reactions to a tick encounter, often before the onset of systemic symptoms or distinctive rashes. In the hours immediately following a tick bite, the site may appear as a small, slightly reddened area, often no larger than a dime, sometimes with a faint central punctum where the tick’s mouthparts penetrated the skin. This initial inflammation is a localized response to the saliva injected by the tick, which contains various bioactive compounds designed to prevent coagulation and reduce pain, thus facilitating the tick’s feeding. The skin around the bite might feel slightly warm to the touch and could exhibit mild swelling. Itching is a very common early symptom, prompting some individuals to scratch the area, which can further exacerbate redness and introduce minor abrasions. These early, non-specific reactions are largely indistinguishable from other insect bites and do not, in themselves, definitively indicate an infection. However, careful observation of these early changes is vital. The size and intensity of the redness and swelling can vary depending on individual allergic sensitivities; some people might develop a more pronounced localized allergic reaction, forming a larger, itchy welt.
Within the first few days to a week, early tick bite photos might reveal a slight evolution of the bite site. If the tick has been removed, the small punctum may scab over, and the surrounding redness might begin to subside. However, it is during this early window that the first specific signs of certain tick-borne illnesses can start to emerge. For example, the initial stage of an erythema migrans (EM) rash, associated with Lyme disease, can begin as a solid red patch that gradually expands. In its earliest manifestation, it may not yet have developed the classic central clearing of a bull’s-eye. Instead, it might appear as a uniformly red, expanding lesion that is often flat or only slightly raised. Monitoring the diameter of this expanding redness over 24-48 hours is crucial. If the redness at the bite site continues to enlarge beyond 5 centimeters in diameter, it strongly suggests an EM rash, even without the typical target appearance. Other early, subtle changes captured in early tick bite photos might include:
- Persistent Lump: A small, firm lump at the bite site that lasts for several weeks, even after the tick is removed, indicating a granulomatous reaction to retained tick mouthparts.
- Localized Discoloration: Beyond simple redness, some early bites might show a purplish or bruised appearance if there has been minor subcutaneous bleeding.
- Early Peripheral Spread: A subtle expansion of erythema, where the red area slowly increases in size day by day, hinting at the beginning of an EM rash.
- Cluster of Red Spots: In rare cases, multiple small, non-descript red spots might appear around the primary bite site, potentially indicating a localized hypersensitivity.
It is essential to differentiate these early signs from secondary bacterial infections, which might present with increasing pain, pus, warmth, and more intense redness or streaking (lymphangitis) originating from the bite site. The absence of an early, pronounced skin reaction does not negate the risk of a tick-borne disease; some infections, such as anaplasmosis or ehrlichiosis, typically do not cause a characteristic rash at all. Therefore, meticulous examination of early tick bite photos and vigilant self-monitoring, combined with awareness of general systemic symptoms like fever and fatigue, are indispensable for early diagnosis and timely tick bite treatment. Any deviation from a simple, resolving red bump warrants medical consultation and evaluation.
Skin rash Tick bite Images
Skin rash tick bite images are perhaps the most vital visual diagnostic tools for identifying tick-borne illnesses, as many diseases manifest with characteristic dermatological signs. The diversity in these rashes requires careful attention to detail regarding their morphology, distribution, and evolution.
1. Erythema Migrans (EM) – Lyme Disease Rash:
The most iconic rash associated with a tick bite is the erythema migrans, the hallmark of early localized Lyme disease.
- Appearance: It typically begins as a small red spot or papule at the site of the tick bite and gradually expands over several days to weeks, forming an annular (ring-shaped) or oval lesion.
- Classic “Bull’s-Eye” Pattern: Many EM rashes develop central clearing, where the center of the lesion returns to normal skin color or becomes slightly bluish, while the outer edge remains red and often slightly raised. This creates the characteristic “bull’s-eye” or “target” appearance.
- Atypical Presentations: It is crucial to note that not all EM rashes present with central clearing. Some can be uniformly red, without a target appearance, or may be vesicular, bruised, or even necrotic in rare instances. Others may have an atypical shape.
- Size and Location: EM rashes are typically at least 5 cm in diameter and can grow much larger, sometimes exceeding 30 cm. They commonly appear on the thighs, groin, trunk, or armpits, but can occur anywhere the tick attached.
- Symptoms: The rash is usually not painful or itchy, although some individuals may report mild itching, burning, or warmth.
- Multiple EM Lesions: In cases of disseminated Lyme disease, multiple, smaller EM lesions may appear on different parts of the body, often without central clearing, indicating the spread of the infection. These are significant findings in skin rash tick bite images.
- Evolution: If left untreated, the EM rash typically fades within 3 to 4 weeks, but the underlying infection can progress to later stages of Lyme disease.
2. Rocky Mountain Spotted Fever (RMSF) Rash:
RMSF is a severe, potentially fatal tick-borne disease, and its rash is a critical diagnostic sign.
- Timing: The rash typically appears 2 to 5 days after the onset of fever, though some patients may never develop a rash.
- Initial Appearance: It usually starts as small, flat, pinkish-red spots (macules) that blanch when pressed.
- Progression: These macules quickly evolve into raised, firm, red bumps (maculopapules).
- Distribution: The RMSF rash classically begins on the ankles and wrists, then spreads to the palms and soles of the feet, and eventually to the trunk and face (centripetal spread, including extremities). This is a key differentiator in skin rash tick bite images.
- Late Stage: In severe cases, particularly if untreated, the rash can become petechial (small, non-blanching red spots due to capillary damage) or purpuric (larger bruise-like areas), indicating severe vascular damage and a poor prognosis. This stage requires immediate medical attention.
- Symptoms: Accompanied by high fever, severe headache, muscle pain, and often nausea/vomiting.
3. Southern Tick-Associated Rash Illness (STARI) Rash:
STARI is clinically very similar to Lyme disease in its early stages, primarily characterized by a bull’s-eye rash.
- Appearance: Presents as an expanding circular or oval red rash, often with central clearing, closely resembling an EM rash.
- Causative Agent: Associated with the lone star tick (Amblyomma americanum) but is not caused by the Lyme disease bacterium (Borrelia burgdorferi).
- Symptoms: Patients may experience fatigue, headache, fever, and muscle pains similar to early Lyme disease.
- Diagnosis: Differentiating STARI from Lyme disease solely based on skin rash tick bite images can be challenging, and laboratory tests are often required. However, the geographic distribution and exposure to the lone star tick can be indicative.
4. Alpha-gal Syndrome Rash (Red Meat Allergy):
This is a unique allergic reaction triggered by a tick bite, leading to a delayed allergic response to red meat.
- Appearance: The rash typically presents as hives (urticaria) or angioedema (swelling beneath the skin) that appear hours after consuming red meat (mammal products). It is not at the bite site itself but a systemic reaction.
- Timing: The delay in onset (3-6 hours post-ingestion) is characteristic, making it distinct from immediate food allergies.
- Symptoms: In addition to hives, patients can experience itching, gastrointestinal symptoms (nausea, vomiting, diarrhea), nasal congestion, shortness of breath, and potentially life-threatening anaphylaxis.
- Causative Agent: Primarily linked to bites from the lone star tick (Amblyomma americanum) in the US.
5. Anaplasmosis and Ehrlichiosis Rashes:
While not typical, rashes can occasionally occur with these tick-borne bacterial infections.
- Appearance: When present, the rash is usually a non-specific maculopapular rash, resembling measles or rubella. It is rarely petechial.
- Prevalence: Rashes are less common (occurring in less than 10-20% of cases) compared to RMSF or Lyme disease.
- Symptoms: Primarily characterized by high fever, severe headache, malaise, and muscle aches.
6. Tularemia Ulceroglandular Lesion:
Tularemia, though less common, can present with a distinctive skin lesion.
- Appearance: At the site of the tick bite (or other entry point), a painful ulcer may develop, often with a raised border and a black base (eschar).
- Lymphadenopathy: This ulcer is typically accompanied by swollen and often painful regional lymph nodes (lymphadenopathy).
- Symptoms: Patients usually experience fever, chills, and malaise.
7. General Allergic or Irritant Rashes:
Many tick bites, even without disease transmission, can cause localized skin reactions.
- Appearance: A small, red, itchy bump or welt at the bite site. It may be slightly raised and feel warm.
- Duration: These typically resolve within a few days to a week.
- Symptoms: Primarily localized itching, mild discomfort, or sensitivity.
Careful evaluation of skin rash tick bite images, understanding their specific features, timing, and accompanying symptoms, is crucial for accurate diagnosis. Any unusual or spreading rash following a tick bite, particularly if accompanied by systemic symptoms, warrants immediate medical attention to initiate appropriate tick bite treatment.
Tick bite Treatment
Effective tick bite treatment encompasses several stages, beginning with proper tick removal and extending to specific medical interventions for diagnosed tick-borne diseases. The immediate response to finding an attached tick is crucial in preventing infection.
1. Tick Removal:
Prompt and correct tick removal is the first line of defense.
- Tools: Use fine-tipped tweezers. Avoid using bare hands, as this can squeeze the tick and inject more pathogens.
- Technique: Grasp the tick as close to the skin surface as possible. Pull upward with steady, even pressure. Do not twist or jerk the tick, as this can cause the mouthparts to break off and remain in the skin.
- Post-Removal Care: After removing the tick, thoroughly clean the bite area and your hands with rubbing alcohol, an iodine scrub, or soap and water. Dispose of a live tick by placing it in alcohol, sealing it in a plastic bag/container, wrapping it tightly in tape, or flushing it down the toilet. Never crush a tick with your fingers.
- Monitoring: After removal, monitor the bite site and your health for several weeks for any signs of rash or systemic symptoms. Taking a picture of the bite site immediately after removal can be useful for tracking changes, similar to tick bite symptoms pictures for comparison.
2. Post-Exposure Prophylaxis (PEP) for Lyme Disease:
In certain high-risk situations, a single dose of antibiotics may be recommended to prevent Lyme disease.
- Criteria: PEP is typically considered if all of the following conditions are met:
- The attached tick is identified as an adult or nymphal Ixodes scapularis (deer tick).
- The tick is estimated to have been attached for 36 hours or more (based on degree of engorgement or likely exposure time).
- Prophylaxis can be started within 72 hours of tick removal.
- Lyme disease is prevalent in the area.
- The patient has no contraindications to doxycycline (e.g., pregnancy, lactation, children under 8 years of age where doxycycline use is typically avoided unless other options are not suitable for severe illness).
- Medication: Doxycycline, usually a single 200 mg dose for adults.
3. Antibiotic Treatment for Specific Tick-Borne Diseases:
Once a tick-borne illness is diagnosed, specific antibiotic regimens are prescribed. Early treatment is vital to prevent severe complications.
- Lyme Disease Treatment:
- Early Localized (Erythema Migrans): Doxycycline (100 mg twice daily for 10-21 days) is the preferred treatment for adults and children over 8 years. Amoxicillin (500 mg three times daily for 14-21 days) or Cefuroxime axetil (500 mg twice daily for 14-21 days) are alternatives, especially for pregnant women or young children.
- Early Disseminated (e.g., facial palsy, carditis): Longer courses of oral antibiotics (21-28 days) or intravenous antibiotics (e.g., Ceftriaxone) for more severe manifestations.
- Late Stage (e.g., Lyme arthritis, neuroborreliosis): Oral or intravenous antibiotics for 28 days or longer, depending on the severity and specific manifestation.
- Rocky Mountain Spotted Fever (RMSF) Treatment:
- Primary Treatment: Doxycycline (100 mg twice daily for 5-7 days or at least 3 days after fever subsides) is the drug of choice for all ages, including children and pregnant women, due to the severity of the disease and potential for fatal outcomes if untreated. Delay in treatment significantly increases mortality.
- Alternative: Chloramphenicol can be used in rare cases where doxycycline is absolutely contraindicated, but it has significant side effects and is less effective.
- Anaplasmosis and Ehrlichiosis Treatment:
- Primary Treatment: Doxycycline (100 mg twice daily for 10-14 days or for at least 3 days after fever subsides) is highly effective.
- Timing: Treatment should be initiated promptly, often empirically, if these infections are suspected.
- Babesiosis Treatment:
- Treatment Regimen: Typically a combination of Atovaquone (750 mg twice daily) plus Azithromycin (500-1000 mg once daily) for 7-10 days.
- Alternative: Clindamycin (300-600 mg every 6 hours) plus Quinine (650 mg every 8 hours) for 7-10 days, often for more severe cases but with more side effects.
- Tularemia Treatment:
- Primary Treatment: Streptomycin or Gentamicin (parenterally) for 7-14 days.
- Oral Alternatives: Doxycycline or Ciprofloxacin can be used for less severe cases or as step-down therapy.
4. Symptomatic Treatment and Monitoring:
Beyond specific antibiotics, supportive care is crucial.
- Pain and Fever Management: Over-the-counter pain relievers such as acetaminophen or ibuprofen can help manage fever, headache, and body aches.
- Itching Relief: Antihistamines (oral or topical) or topical corticosteroids can alleviate itching at the bite site.
- Alpha-gal Syndrome Management: Strict avoidance of mammalian meat and meat products is the primary management. Antihistamines and corticosteroids can manage allergic reactions, and epinephrine auto-injectors may be prescribed for severe reactions.
- Monitoring for Complications: Patients should be advised to monitor their symptoms closely and report any worsening or new symptoms to their healthcare provider. Follow-up appointments may be necessary.
Understanding the nuances of tick bite treatment, from initial removal to targeted pharmacotherapy, is essential for preventing long-term sequelae from tick-borne diseases. Early recognition of symptoms, guided by resources like tick bite symptoms pictures, significantly improves treatment outcomes. Always consult a healthcare professional for diagnosis and treatment plans for any suspected tick-borne illness.