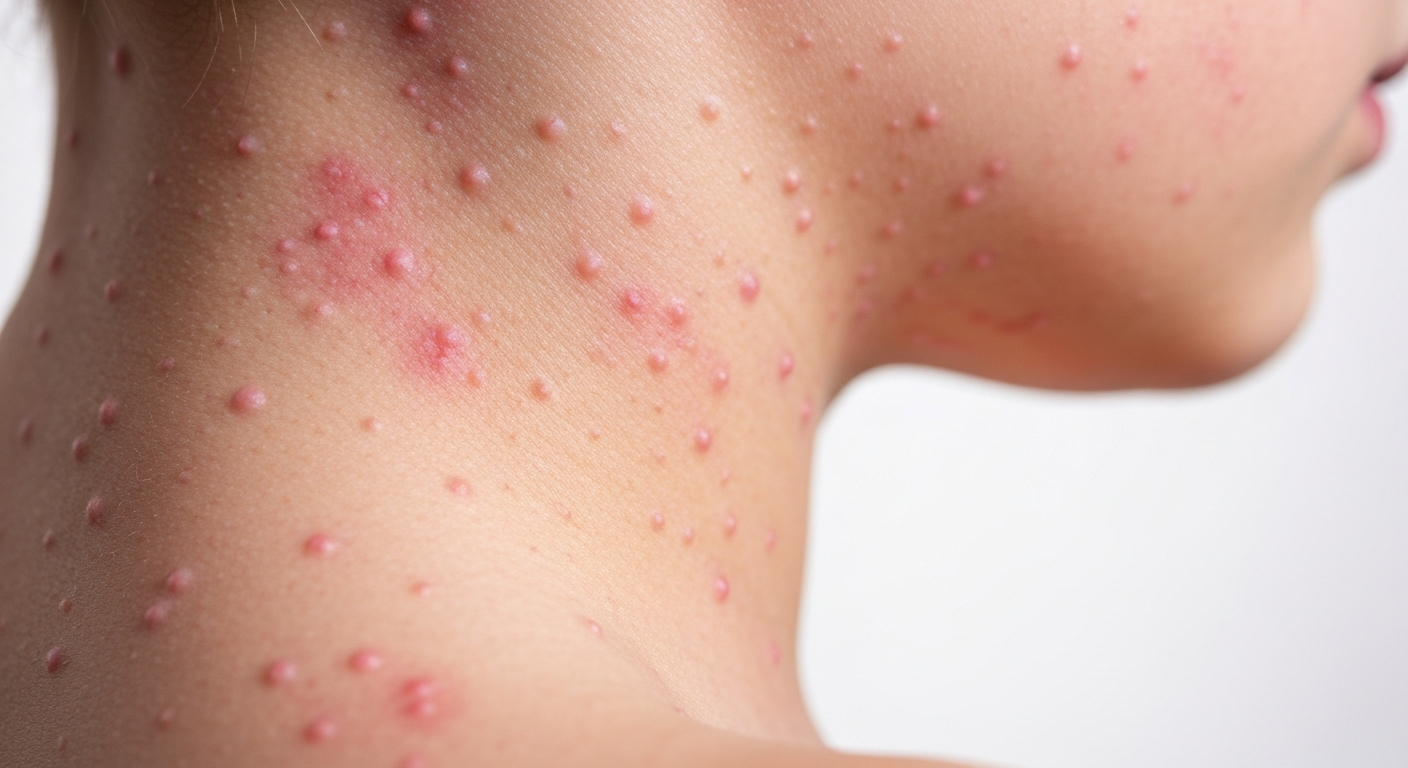
Recognizing the visual manifestations of Rubella in children is crucial for early identification and appropriate care. This guide offers a detailed look at
Rubella in children Symptoms Pictures
Rubella, often referred to as German measles, presents with a constellation of symptoms in children, many of which are visually distinct. Understanding these
Observing a child with
Comprehensive List of Rubella Symptoms in Children:
- Low-Grade Fever (Pyrexia):
A mild elevation in body temperature is one of the earliest signs. This fever typically ranges from 99.5°F (37.5°C) to 100.4°F (38°C) and rarely exceeds 101°F (38.3°C). Visually, a child may appear slightly flushed, particularly across the cheeks and forehead. Their skin might feel warm to the touch. The fever usually precedes the rash by one to five days and often subsides quickly once the rash fully develops. It is generally not severe enough to cause significant distress or lethargy in the child, making it a subtle initial indicator of
Rubella in children . - Lymphadenopathy (Swollen Lymph Nodes):
Swollen and tender lymph nodes are a hallmark symptom of Rubella. These are most commonly found in the postauricular (behind the ears), posterior cervical (back of the neck), and suboccipital (at the base of the skull) regions. On visual inspection and gentle palpation, these nodes may appear as small, pea-sized to bean-sized lumps under the skin. They are typically firm but mobile and can be tender to the touch, though not excessively painful. The skin overlying the swollen nodes usually remains normal in color and texture, without redness or warmth, unless there is a secondary infection. This lymphadenopathy can develop several days before the rash and may persist for one to two weeks after the rash has faded. In
Rubella in children pictures , one might discern a slight fullness or bulge in these neck and head regions. - Maculopapular Rash:
The characteristic
Rubella rash is a diffuse, erythematous (reddish), maculopapular eruption. It consists of small, flat, red spots (macules) and slightly raised bumps (papules) that are typically 1-4 mm in diameter. The rash begins on the face and neck, often appearing first around the hairline and behind the ears, then rapidly spreads downwards to the trunk and extremities within 24 hours. The spots may coalesce, particularly on the face, giving the skin a patchy reddish appearance. This rash is usually fine, discrete, and lighter pink in color compared to other common childhood rashes like measles. It is generally not itchy, or only mildly pruritic, and fades quickly, typically disappearing within three days, leaving no discoloration or scaling. The transient nature and distinctive pattern of spread are key visual identifiers inRubella in children symptoms pictures . - Malaise (General Feeling of Unwellness):
Children infected with Rubella often experience a general feeling of being unwell, or malaise. This can manifest as a lack of energy, tiredness, and a disinterest in usual activities. While not a directly visual symptom, it can contribute to a child’s overall appearance of being subdued or somewhat lethargic. They might seem less playful or more irritable than usual. This symptom usually begins concurrently with the fever and often resolves as the rash progresses, indicating the peak of the illness. Parents might observe a child spending more time resting or requiring more comfort than usual.
- Mild Conjunctivitis:
Inflammation of the conjunctiva (the membrane lining the eyelids and covering the white part of the eye) can occur, though it is usually mild. Visually, the whites of the eyes might appear slightly reddened or bloodshot. There may be minimal tearing or mild sensitivity to light (photophobia). Unlike bacterial conjunctivitis, there is typically no significant purulent discharge. The eyes might look a bit watery or glossy. This symptom is generally transient and resolves without specific intervention. In
Rubella in children photos , one might observe a subtle redness in the sclera. - Upper Respiratory Symptoms:
Some children may develop mild upper respiratory symptoms resembling a common cold. These can include a runny nose (rhinorrhea) with clear discharge, a mild sore throat (pharyngitis), and a cough. Visually, a child might have a visibly dripping nose or frequently wipe their nose. Their throat might appear slightly red upon examination, though severe redness or pus is uncommon. These symptoms are typically mild and non-specific, often preceding the rash and resolving quickly. They contribute to the overall picture of a viral illness in its early stages.
- Arthralgia (Joint Pain):
While more common in adolescent girls and adult women, older children with Rubella may experience joint pain (arthralgia), particularly in the fingers, wrists, and knees. This is not directly visible but can be inferred by a child’s reluctance to move specific joints, limping, or complaints of discomfort. There is typically no visible swelling or redness of the joints in children. The pain is usually transient and resolves without long-term complications, but it can contribute to a child’s general irritability and discomfort during the acute phase of illness.
- Forscheimer Spots:
These are small, pinpoint red macules or petechiae that can sometimes be observed on the soft palate (the fleshy back part of the roof of the mouth) before or concurrently with the skin rash. Visually, upon examining the child’s mouth, these spots appear as discrete, tiny red dots against the paler pink background of the soft palate. They are non-blanching, meaning they do not disappear when pressed. Forscheimer spots are not always present, but when observed, they can be a helpful diagnostic sign for
Rubella in children .
Signs of Rubella in children Pictures
Differentiating between symptoms (what a patient feels) and signs (what a clinician observes) is important, particularly when dealing with
From the subtle swelling of lymph nodes to the characteristic rash, each sign offers a piece of the diagnostic puzzle. Recognizing these
Observable Signs of Rubella in Children:
- Generalized Lymphadenopathy (Swollen Glands):
This is arguably the most consistent and visually impactful sign. While mentioned under symptoms, its objective presence makes it a primary sign. The swelling of lymph nodes, especially in the postauricular, posterior cervical, and suboccipital areas, can often be visibly detected as small, firm bulges under the skin. On palpation, they are enlarged, discrete, and slightly tender. The skin over these nodes typically appears normal in color and temperature. In
Rubella in children pictures , one might perceive a subtle prominence behind the ears or along the neck. The extent of swelling can vary, but these nodes are reliably palpable in most cases, often lasting longer than the rash itself, sometimes for several weeks. - Erythematous Maculopapular Rash Distribution:
The distinctive pattern of the
Rubella rash is a key visual sign. It commences on the face, particularly the forehead, hairline, and behind the ears, before descending rapidly to cover the trunk and extremities within 24 hours. The rash is characterized by discrete, pinkish-red macules and papules that may become confluent on the face, creating a flushed appearance. On the trunk, the lesions tend to remain more discrete. The rapid spread and relatively short duration (1-3 days) are characteristic. Unlike measles, theRubella rash in children images would show a finer, lighter pink rash that often appears less intensely red and does not become intensely confluent across the body. The fading of the rash also follows a top-down pattern. - Mild Ocular Redness (Conjunctival Injection):
A mild, non-purulent inflammation of the conjunctiva is an observable sign. The whites of the child’s eyes may appear faintly bloodshot or injected, characterized by visible fine red blood vessels. There is usually no significant discharge, but eyes might appear slightly watery or teary. Photophobia (sensitivity to light) can sometimes be elicited, where the child squints or turns away from bright light. This ocular sign is typically subtle and resolves concurrently with other acute symptoms. It contributes to the overall picture of mild viral illness often seen in
Rubella in children . - Oral Lesions (Forscheimer Spots):
As an observable sign, Forscheimer spots on the soft palate are specific, though not consistently present. These are small, dark-red macules or petechiae that appear on the soft palate or uvula. When inspecting the child’s mouth, these tiny, non-blanching red spots can be seen against the paler pink mucosa. They are distinct from Koplik’s spots of measles and are typically fewer in number. Their presence, if noted, can be a valuable diagnostic clue in
Rubella in children photos of the oral cavity. They usually resolve spontaneously within a day or two. - Behavioral Changes due to Malaise:
While subjective in part, a child’s general demeanor and activity level can be an observable sign. Children with Rubella may appear unusually quiet, lethargic, or irritable. They might show reduced interest in play, seek more comfort, or simply want to rest more. Their facial expression might convey tiredness or discomfort. These subtle behavioral changes, when combined with other physical signs, paint a clearer picture of illness. Parents often report a noticeable decrease in their child’s usual energy levels and enthusiasm.
- Absence of Severe Respiratory Distress or Cough:
Crucially, what is often *absent* can be as informative as what is present. In
Rubella in children , while mild upper respiratory symptoms like a runny nose or a slight cough can occur, there is typically an absence of severe, barking cough, significant respiratory distress, or wheezing often seen in other respiratory illnesses. This absence helps differentiate Rubella from conditions like measles or bronchiolitis. The breathing pattern remains normal, and there are no visible signs of labored breathing or cyanosis. - Pinkish Hue of Rash:
The color of the rash is a significant observable sign.
Rubella rash images typically show a lighter, rose-pink, or pale red eruption compared to the deeper, brick-red color of measles. This lighter hue is consistent across the body, though it might appear slightly more intense on the face where lesions are often confluent. This subtle color difference is an important visual diagnostic marker for differentiating Rubella from other exanthematous diseases.
Early Rubella in children Photos
Identifying
The first few days of Rubella infection in children are characterized by a gradual onset of non-specific symptoms. These
Key Features of Early Rubella in Children:
- Subtle Onset of Low-Grade Fever:
The very first sign of
early Rubella in children is often a barely noticeable low-grade fever. The child may simply feel slightly warmer than usual, with an oral temperature typically not exceeding 100.4°F (38°C). Visually, the child might have a very faint flush to their cheeks or seem a little less vibrant. They may not complain of feeling unwell, or their complaints might be vague. This initial fever usually lasts for a short period, often 12-24 hours, before the rash appears. It is a crucial early indicator, but its mildness often leads to it being overlooked inearly Rubella pictures . - Initial Lymph Node Swelling (Occipital, Postauricular):
One of the most reliable
early Rubella signs is the palpable, and sometimes subtly visible, enlargement of lymph nodes, particularly those at the base of the skull (suboccipital) and behind the ears (postauricular). These nodes may feel like small, firm, slightly tender peas or beans under the skin. There is typically no associated redness or warmth of the overlying skin. This swelling can occur up to a week before the rash emerges, making it an excellent early diagnostic clue. Inearly Rubella in children photos , one might perceive a very slight puffiness or fullness in these areas, particularly when viewed from certain angles or through gentle palpation outlines. - Mild Malaise and Fatigue:
Before the rash, children often exhibit a general sense of being unwell. They might be less energetic, more quiet, or require more sleep. Their play may be less enthusiastic. Visually, a child might appear more subdued, with a slightly tired expression. This fatigue is usually not profound but marks a noticeable shift from their usual energetic state. Parents might note that their child is “not quite themselves.”
- Slight Ocular Redness or Watery Eyes:
A very mild conjunctivitis can be among the
initial Rubella symptoms . The eyes might appear slightly red or watery, without significant purulent discharge. There may be mild light sensitivity. This is often subtle and might be mistaken for irritation or early allergic reaction.Early Rubella photos might capture a hint of redness in the whites of the eyes or an unusual glistening due to increased tearing. - Non-Specific Upper Respiratory Symptoms:
Some children may experience mild cold-like symptoms such as a runny nose with clear discharge, a very mild sore throat, or a dry cough. These symptoms are typically not severe enough to cause significant distress or interfere with daily activities. Visually, a child might have a slightly runny nose or clear nasal discharge. The throat might appear mildly pinkish upon inspection. These early respiratory symptoms often resolve quickly once the rash appears.
- Subtle Skin Changes Pre-Rash:
Occasionally, before the classic maculopapular rash, there may be an extremely faint, transient erythema (redness) on the face or upper trunk. This is often so faint that it is difficult to distinguish and rapidly evolves into the more defined rash. It might present as a general blush or a very fine, almost invisible, mottling of the skin. This phase is extremely transient and often missed in the progression of
Rubella in children . - Forscheimer Spots (Early Oral Manifestation):
The appearance of Forscheimer spots on the soft palate can be an early sign, occurring before or concurrently with the skin rash. These are tiny, pinpoint, red macules or petechiae that are visible upon careful inspection of the child’s mouth and throat. They are non-blanching and distinctive, offering a visual cue within the oral cavity before widespread skin manifestations become apparent. Their presence confirms an active viral infection. In
early Rubella in children photos of the palate, these small red spots could be visible. - Increased Irritability or Fussiness:
Due to the general malaise, mild fever, and discomfort from swollen glands or arthralgia, some children may become more irritable or fussy in the early stages. While not a direct visual sign, it affects their demeanor and interaction, which parents can observe. They may cry more easily or resist normal routines. This behavioral change can be an indirect indicator of the onset of illness, preceding more definitive physical signs of
Rubella .
Skin rash Rubella in children Images
The
When examining
Detailed Description of the Rubella Skin Rash in Children:
- Onset and Initial Appearance:
The
Rubella skin rash typically begins on the face, specifically around the hairline, behind the ears, and on the forehead and cheeks. It appears as small, discrete, faint pinkish-red macules (flat spots) and papules (slightly raised bumps). These initial lesions are generally 1-4 mm in diameter. The texture of the skin may feel slightly bumpy, especially when observed closely or touched. Unlike the blotchy onset of measles, Rubella’s rash is often finer and less intense at its initiation. Inskin rash Rubella in children images , one would notice these delicate, individual spots emerging on the face. - Distribution and Progression:
From the face, the
Rubella rash rapidly spreads downwards to the neck, trunk, and then to the extremities (arms and legs) within a single day (approximately 24 hours). This cephalocaudal (head-to-foot) spread is characteristic. On the face, the lesions may coalesce, giving the appearance of a generalized flush or patchy redness. However, on the trunk and extremities, the lesions tend to remain more discrete, with areas of normal-appearing skin between the spots. The palms and soles are typically spared from the rash. The rapid progression across the body is a hallmark feature distinguishing it inRubella rash pictures . - Color and Intensity:
The color of the
Rubella rash is a distinctive light pink or rose-red hue. It is generally paler and less intensely erythematous than the rash of measles or scarlet fever. The intensity of the color may vary slightly, appearing somewhat brighter on the face due to confluence, but maintaining its light pink character overall. The rash blanches (turns white) when pressed, indicating capillary dilation rather than hemorrhage. This lighter pigmentation is a key visual differentiator when comparingGerman measles rash images with other childhood exanthems. - Texture and Size of Lesions:
The lesions are primarily maculopapular, meaning a mix of flat spots and slightly raised bumps. The papules are subtle, often described as having a “fine” or “sandpaper-like” texture when felt gently, but this is less pronounced than in scarlet fever. Each lesion is typically small, often not exceeding 4 mm in diameter. The uniform size and diffuse distribution contribute to the overall fine appearance of the rash across the body. The discrete nature of the lesions on the trunk is a key feature.
- Absence of Itching or Mild Pruritus:
In most children, the
Rubella rash is either non-itchy or causes only very mild itching. This contrasts significantly with the often intensely pruritic rashes of chickenpox or eczema. A child with Rubella typically does not scratch the rash, and there are usually no visible excoriations (scratch marks) associated with the eruption. This lack of significant pruritus is a helpful clinical observation. - Duration and Resolution:
The
Rubella skin rash is notable for its brief duration. It usually fades and disappears within one to three days, often resolving in the same order it appeared, starting from the face and moving downwards. As it resolves, the rash typically leaves no permanent marks, discoloration, or fine scaling. The skin returns to its normal appearance without desquamation (peeling), which can be seen in some other rashes. The rapid resolution is a crucial distinguishing feature when observingRubella images over time. - Comparison Points (Implicit):
While not directly comparing, the description implicitly highlights differences. For instance, the fine, discrete, light pink nature of the
Rubella rash is distinctly different from the coarser, darker, confluent, and longer-lasting rash of measles. Similarly, the absence of vesicles (blisters) differentiates it from chickenpox, and the less intense, non-scarlatiniform appearance separates it from scarlet fever. These subtle visual distinctions are critical for healthcare professionals. - Mucosal Involvement (Forscheimer Spots):
While primarily a skin rash, the oral cavity can sometimes show Forscheimer spots (small, pinpoint red macules or petechiae on the soft palate). These are not part of the generalized skin rash but are mucosal manifestations that can accompany the skin eruption. Their presence visually confirms a systemic infection and provides an additional diagnostic clue when observing a child with
Rubella .
Rubella in children Treatment
The treatment for
Parents seeking information on
Comprehensive Strategies for Rubella Treatment in Children:
- Rest and Recuperation:
Encourage ample rest, as this helps the child’s body conserve energy to fight the infection. A quiet environment free from excessive stimulation is beneficial. While children may experience mild malaise, forcing bed rest is usually unnecessary. Allowing them to engage in quiet activities like reading, drawing, or watching age-appropriate media can maintain spirits while promoting rest. Adequate rest supports the immune system’s response to the
Rubella virus and aids in a quicker recovery fromRubella symptoms . - Hydration:
Maintaining adequate fluid intake is critical, especially if the child has a fever or mild sore throat. Offer small, frequent sips of water, clear broths, diluted juices, or oral rehydration solutions. Popsicles can be soothing for a sore throat and contribute to fluid intake. Dehydration can exacerbate general malaise and extend the feeling of unwellness. Ensuring good hydration helps the body manage the mild fever and supports overall bodily functions during
Rubella in children . - Fever and Pain Management:
For fever or any mild body aches (arthralgia), over-the-counter medications such as acetaminophen (Tylenol) or ibuprofen (Advil, Motrin) can be administered according to age and weight guidelines. Always consult a pediatrician or pharmacist for correct dosing. These medications help reduce discomfort and lower fever, making the child feel more comfortable. Aspirin should be avoided in children due to the risk of Reye’s syndrome. Managing fever and pain directly addresses two of the most uncomfortable
Rubella symptoms . - Isolation and Prevention of Spread:
Children with Rubella are contagious for about one week before the rash appears and for about one week after the rash has faded. During this period, it is crucial to keep the child home from school, daycare, or other public settings to prevent transmission. Special care should be taken to avoid contact with pregnant women, as Rubella can cause severe birth defects (Congenital Rubella Syndrome) if contracted during pregnancy. Hand hygiene is also important. This preventive measure is a critical part of
Rubella management . - Relief for Mild Conjunctivitis:
If mild conjunctivitis is present, a clean, warm compress applied gently to the eyes can help soothe irritation. Avoid rubbing the eyes. Keeping the eyes clean of any minimal discharge is also important. Typically, no specific eye drops are needed unless a secondary bacterial infection occurs, which is rare. Addressing ocular discomfort contributes to the child’s overall comfort during
Rubella in children . - Comfort Measures for Rash (if applicable):
While the
Rubella rash is usually not itchy, if there is any mild pruritus, cool baths or loose, comfortable clothing can help. Avoid harsh soaps or vigorous scrubbing that could irritate the skin. Calamine lotion is generally not necessary but could be used if itching is bothersome. The focus is to keep the child comfortable as the rash naturally fades within a few days. - Nutritional Support:
Offer bland, easily digestible foods if the child has a poor appetite. Small, frequent meals may be better tolerated than large ones. Do not force eating if the child is reluctant, as hydration is more critical. Once their appetite returns, resume a normal, balanced diet to support recovery. Good nutrition plays a role in the body’s healing process from
Rubella in children . - Monitoring for Complications:
Although Rubella in children is typically mild, parents should monitor for any signs of unusual complications, such as:
- Encephalitis: Severe headache, stiff neck, seizures, significant changes in consciousness. (Very rare)
- Thrombocytopenia: Unusual bruising, petechiae (small red spots from bleeding under the skin) that are not part of the rash, nosebleeds. (Rare)
- Arthritis: Persistent or severe joint pain and swelling, especially in older children, though usually resolves spontaneously.
Any concerning symptoms should prompt immediate medical attention. While these complications are exceedingly rare in children with uncomplicated Rubella, vigilance is important. Regular check-ins with the pediatrician are advised if there are concerns about the child’s recovery from
Rubella in children symptoms . - Follow-up with Healthcare Provider:
A follow-up visit may not be necessary if the child recovers completely and all symptoms resolve within the expected timeframe. However, if symptoms persist, worsen, or if parents have any concerns about their child’s health, consulting a healthcare provider is recommended. This ensures that any unexpected developments are addressed promptly and appropriate guidance is provided for
Rubella in children treatment .