Understanding the visual presentation of oral health issues is crucial for timely intervention. This article provides an in-depth look at **Gumboil symptoms pictures**, helping to identify the characteristic features of this common and often painful dental condition. Familiarizing oneself with these visual cues can empower individuals to seek professional dental care promptly.
Gumboil Symptoms Pictures
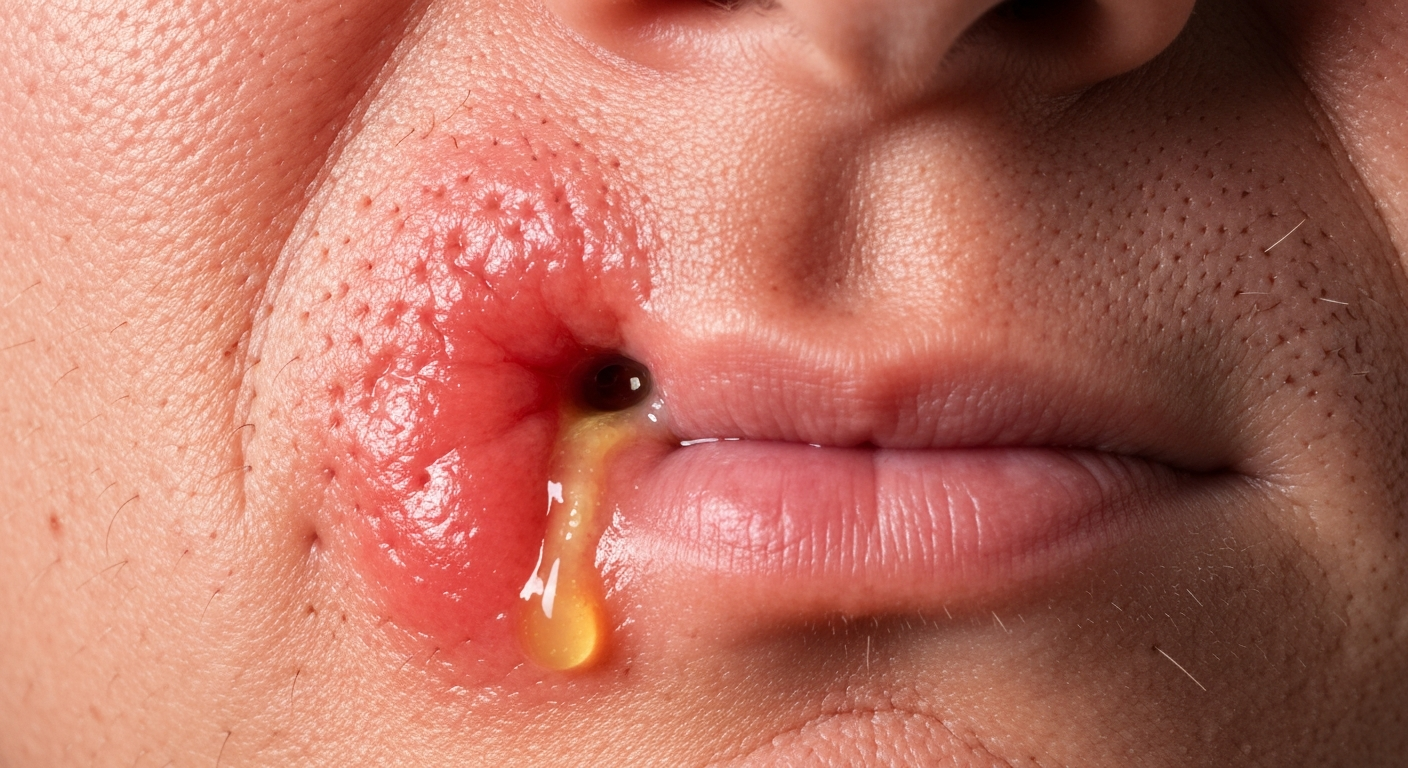
When examining **gumboil symptoms pictures**, several distinct visual characteristics become immediately apparent, reflecting the underlying infection and inflammation. A gumboil, or dental abscess, manifests as a localized collection of pus within the gum tissue or bone, typically near the apex of a tooth root or within the periodontal structures. The visual representation often shows a prominent, localized swelling that demands attention. The primary visual hallmark is a raised, often dome-shaped or pointed lesion on the gum tissue. This elevation is caused by the accumulation of inflammatory exudate and cellular debris. The color of the affected gum area is usually significantly altered. Instead of the healthy pink hue, the gum will appear a vivid red, purplish-red, or even dusky red, indicating intense inflammation and increased blood flow to the region. In some advanced cases or when the pus is close to the surface, a yellowish or whitish center may be visible, which is a clear indicator of a superficial collection of pus ready to drain or already draining.
The texture of the gumboil, as seen in **gumboil symptoms pictures**, can also provide diagnostic clues. It might appear:
- Shiny and Taut: Due to the underlying pressure from pus accumulation, the gum tissue stretched over the swelling may appear unnaturally shiny and feel very tight.
- Soft and Fluctuant: If the pus pocket is well-developed and superficial, touching it lightly might reveal a soft, fluid-filled sensation, indicating the presence of liquid pus. This is known as fluctuation.
- Firm and Indurated: In earlier stages or if the abscess is deeper within the bone, the swelling might feel firm and hard to the touch due to surrounding tissue inflammation and edema rather than just a fluid collection near the surface.
The size of a gumboil can vary significantly, ranging from a small, pimple-like lesion, barely a few millimeters in diameter, to a substantial swelling several centimeters across, potentially distorting facial features if left untreated. Its location is almost always adjacent to an infected tooth, either on the buccal (cheek side) or lingual/palatal (tongue/palate side) gum tissue. Observing **gumboil symptoms pictures** closely reveals not just the swelling itself, but also the surrounding tissue. There might be a general redness and swelling extending beyond the immediate lesion, a sign of diffuse inflammation. Sometimes, a small opening, known as a fistula or sinus tract, can be seen, from which pus might be intermittently draining. This drainage provides temporary relief from pain but signifies an ongoing infection that requires professional dental care. The presence of such a draining tract indicates the body’s attempt to release the pressure from the accumulated pus.
Further visual elements to note in **gumboil symptoms pictures** include:
- Associated Tooth Discoloration: The tooth involved with the gumboil might appear discolored, ranging from grey to dark brown, suggesting pulp necrosis (nerve death) which is often the precursor to a periapical abscess.
- Receding Gum Line: In cases of periodontal abscess, where the infection starts in the supporting tissues around the tooth, there might be signs of gum recession or pockets around the affected tooth.
- Mobility of the Tooth: Although not directly visible in a static picture, a severe gumboil can cause the affected tooth to become slightly mobile or feel “high” in the bite, due to inflammation around its root.
- Local Tenderness and Pain: While pain is a sensation, it’s intrinsically linked to the visual swelling. The gumboil site is typically extremely tender to touch, and the pain can range from a dull ache to a severe, throbbing pain that can radiate to the ear, jaw, or temple. This pain is often exacerbated by biting or chewing on the affected tooth.
- Bad Taste: If the gumboil is draining, patients often report a foul, metallic, or generally unpleasant taste in their mouth, which is due to the pus drainage. This is a key symptomatic indicator when evaluating **gumboil symptoms pictures** in a broader clinical context.
Understanding these detailed visual cues from **gumboil symptoms pictures** is the first step in recognizing the condition and ensuring prompt and effective treatment to prevent further complications. The intensity of color, the degree of swelling, and any evidence of drainage are all critical observations.
Signs of Gumboil Pictures
Beyond the direct visual manifestation of the swelling, **signs of gumboil pictures** encompass a broader spectrum of indicators, some of which are observable in a clinical setting and others inferred from patient reports alongside visual evidence. These signs help to confirm the diagnosis and assess the severity and potential spread of the infection. A key visual sign often present is localized redness and inflammation extending beyond the immediate site of the abscess. This can manifest as a halo of erythema around the core swelling, indicating a spreading inflammatory process. The surrounding gum tissue may also appear puffy or edematous, even if it doesn’t form a distinct pus-filled lesion.
Another significant sign, particularly in more severe or chronic **gumboil pictures**, is the presence of a **sinus tract or fistula**. This appears as a small, often raised, pimple-like lesion on the gum, sometimes with a pinpoint opening from which pus may intermittently drain. This drainage helps to relieve pressure and can lead to a temporary reduction in pain, making the patient believe the problem has resolved, when in fact, the underlying infection persists. The color of the exudate, if visible, can range from yellowish to greenish, signifying bacterial presence and cellular debris. Sometimes, a tiny “gum boil” may appear, burst, drain, and then seemingly disappear, only to recur in the same spot, which is a classic sign of an active, draining sinus tract from a chronic abscess.
Systemic signs, while not directly “pictures” in the visual sense of the gumboil itself, are crucial accompanying indicators that a clinician looks for and which often prompt a patient to seek care. These can sometimes be inferred from a patient’s overall appearance or facial presentation:
- Facial Swelling: A particularly concerning sign is the extension of the swelling from the gum to the face. This can manifest as swelling of the cheek, jawline, or even around the eye, depending on the location and severity of the underlying dental infection. This indicates a significant spread of infection into deeper facial spaces.
- Fever: An elevated body temperature is a common systemic response to infection. Patients with acute gumboils, especially those with spreading infections, may present with a fever and chills.
- Lymphadenopathy: Swelling and tenderness of the lymph nodes in the neck or under the jaw (submandibular or cervical lymph nodes) are common signs that the body’s immune system is actively fighting an infection. These swollen glands can often be palpated and sometimes even visually observed if significantly enlarged.
- Fatigue and Malaise: A general feeling of being unwell, tired, and lethargic often accompanies systemic infections, including severe dental abscesses.
- Difficulty Opening Mouth (Trismus): If the infection spreads to the muscles of mastication, patients may experience difficulty or pain when trying to open their mouth wide.
- Difficulty Swallowing (Dysphagia): In very severe cases, especially if the infection is in the lower jaw and spreads to the floor of the mouth, swallowing can become painful and difficult.
- Intense, Throbbing Pain: While a symptom, the characteristic nature of the pain—often severe, constant, and throbbing, frequently worse when lying down or with heat—is a strong indicator of an acute abscess. This pain can be so intense that it interferes with sleep, work, and daily activities.
- Foul Odor or Taste: The presence of a persistent bad taste in the mouth or halitosis (bad breath) is a strong sign of an ongoing infection, particularly if there is drainage from the abscess.
- Tooth Sensitivity: The affected tooth may become extremely sensitive to hot or cold temperatures, or to pressure when biting. In some cases, the tooth may become non-responsive to thermal changes, indicating nerve death.
When examining **signs of gumboil pictures** in a broader clinical context, it’s essential to consider these accompanying systemic and localized indicators. The presence of any facial swelling, fever, or significant lymph node enlargement elevates the urgency of treatment, as these signs point towards a potentially spreading and more serious infection that could lead to life-threatening complications if left untreated. Recognizing these comprehensive signs alongside the visual appearance of the gumboil is critical for accurate assessment and appropriate management.
Early Gumboil Photos
Identifying an infection in its nascent stages is paramount for effective intervention and to prevent widespread complications. **Early gumboil photos** often reveal subtle cues that might be easily overlooked if one is not specifically looking for them. Unlike the prominent, often painful swelling of a fully developed abscess, an early gumboil typically presents with more nuanced visual and symptomatic indicators. The earliest stage might only show a localized area of slight redness on the gum tissue, often directly adjacent to the neck of a tooth or near the apex of its root. This erythema might be only marginally darker than the surrounding healthy gum and could be mistaken for minor irritation.
In **early gumboil photos**, one might observe a very slight elevation or puffiness of the gum tissue. This isn’t the large, dome-shaped swelling of a mature abscess, but rather a subtle, barely perceptible bulge. It might resemble a small, tender bump, similar to a small pimple, but without an obvious head of pus. The gum texture might appear somewhat smoother or more taut in this localized area, indicating initial fluid accumulation and inflammation beneath the surface. The initial inflammatory response leads to localized edema, which is the root cause of this subtle swelling.
Key visual characteristics often present in **early gumboil photos** include:
- Localized Redness (Erythema): A small, circumscribed area of gum tissue appearing slightly redder than the surrounding healthy gum. This discoloration indicates increased blood flow as part of the initial inflammatory response.
- Minor Swelling or Bulge: A very slight, often tender, elevation of the gum tissue. This could be barely noticeable, appearing as a flattened mound rather than a distinct lump. The size might be only a few millimeters in diameter.
- Increased Sensitivity: While not visually observable, patients often report localized tenderness or sensitivity to touch in the affected area, even before significant swelling is visible. This discomfort can be a precursor to more intense pain.
- Dull Ache or Pressure: Instead of sharp, throbbing pain, an early gumboil might present as a persistent, dull ache or a sensation of pressure in the area, particularly around the involved tooth. This can be intermittent.
- Glossy or Stretched Appearance: The gum tissue in the early affected area might appear slightly more glossy or stretched due to underlying inflammatory fluid, making it less textured than healthy gum tissue.
- Absence of Visible Pus: Crucially, in **early gumboil photos**, there is typically no visible pus pocket or drainage. The infection is still developing, and pus has not yet accumulated to a significant extent or found a path to the surface.
It’s important to differentiate early gumboil signs from other minor gum irritations. For instance, temporary redness from aggressive brushing or food impaction usually resolves quickly and lacks the persistent tenderness or underlying tooth involvement. An early gumboil, however, will likely persist and worsen without intervention. Sometimes, an early gumboil might resemble a canker sore or a small trauma, but careful observation will reveal its association with a specific tooth and its progressive nature.
Recognizing these subtle signs from **early gumboil photos** is essential for preventative dental care. Prompt diagnosis and treatment at this stage can often involve simpler, less invasive procedures, such as a localized cleaning for a periodontal issue or an early root canal intervention for a pulpal infection, thus preventing the development of a large, painful, and potentially complex abscess with facial swelling or systemic complications. Encouraging patients to report even minor or persistent gum discomfort can lead to the early detection of these conditions before they escalate. The visual progression from slight redness and minimal swelling to a more pronounced lesion is a key aspect of monitoring the condition’s development.
Skin rash Gumboil Images
The term “skin rash gumboil images” refers to a specific and significant manifestation of a dental abscess that has spread beyond the oral cavity. While a gumboil typically presents as a swelling on the gum inside the mouth, in some cases, particularly if the infection is chronic or severe, it can find an alternative drainage pathway to the external skin of the face or neck. This is known as a **cutaneous sinus tract** or an **extraoral fistula**. When an abscess tracks through the bone and soft tissues to the skin, it creates a lesion that can be mistaken for a common skin condition, leading to misdiagnosis and inappropriate treatment if the dental origin is not recognized.
In **skin rash gumboil images** showing an extraoral fistula, the appearance is often that of a persistent, localized lesion on the skin, typically in the submandibular region (under the jaw), chin, cheek, or angle of the jaw. The characteristics of this lesion include:
- Pimple-like or Nodule: The initial presentation might be a small, firm, red or pink nodule on the skin, resembling a stubborn pimple or a small boil. It may not immediately be obvious as a dental issue.
- Central Opening (Stoma): As the tract matures, a small opening or “stoma” often develops in the center of the lesion. From this opening, pus, blood, or serous fluid may intermittently drain. The presence of persistent drainage is a strong indicator of an underlying infection.
- Crusting and Scarring: Due to repeated drainage and healing, the skin around the opening can become crusted, excoriated, or discolored. Chronic lesions may lead to fibrous induration and eventual scarring, presenting as a dimpled or puckered area on the skin.
- Recurrent Nature: A key feature identifiable in **skin rash gumboil images** over time is the recurrent nature of the lesion. It may heal temporarily, only to reappear in the exact same spot, often with renewed drainage, as the underlying dental infection continues.
- Associated Inflammation: The skin around the fistula may appear red and inflamed, mimicking a cellulitis or a localized skin infection. However, unlike typical skin infections, an extraoral fistula often fails to respond to conventional antibiotic treatments aimed at skin bacteria alone, because the source of infection is dental.
- Absence of Pain at the Skin Site: Paradoxically, the external skin lesion itself is often painless, especially if it is draining effectively. This can mislead both the patient and healthcare providers into focusing solely on the skin rather than seeking the true dental origin. The pain usually resides in the affected tooth inside the mouth, or the patient might have a history of dental pain that subsided once the fistula formed.
- Location Correlated to Dental Origin: The location of the fistula on the face often corresponds to the tooth involved. For example:
- Fistulas from lower incisors or canines often appear on the chin.
- Those from lower premolars or molars may appear on the cheek or along the jawline.
- Upper teeth infections are less likely to drain externally, but if they do, it might be infraorbital (below the eye) or malar (cheekbone area).
Differentiation from other facial lesions is crucial when viewing **skin rash gumboil images**. It must be distinguished from:
- Acne Vulgaris or Cysts: While appearing pimple-like, extraoral fistulas are typically solitary, persistent, and often have a history of drainage. They do not respond to acne treatments.
- Furuncles (Boils) or Carbuncles: These are skin infections of hair follicles and usually present with acute pain and diffuse inflammation, resolving with appropriate antibiotics or drainage. Dental fistulas are chronic and originate deeper.
- Basal Cell Carcinoma or Squamous Cell Carcinoma: Skin cancers can present as non-healing lesions, but generally lack the draining purulent exudate characteristic of a fistula and have different histological features.
- Salivary Gland Fistulas: These are rare and typically related to trauma or surgery involving salivary glands, and the discharge is saliva, not pus.
The misdiagnosis of an extraoral dental fistula as a primary skin lesion can lead to years of ineffective dermatological treatment, including repeated courses of antibiotics, steroid injections, or even unnecessary surgical excisions, all while the underlying dental infection continues to cause chronic inflammation and potential damage. Therefore, any persistent, non-healing, or recurrent lesion on the face or neck with a history of drainage, especially if associated with dental pain (even if remote), should prompt a thorough dental examination including radiographs to identify the causative tooth. Recognizing these distinct features in **skin rash gumboil images** is vital for correct diagnosis and management.
Gumboil Treatment
Effective **gumboil treatment** is essential not only to alleviate pain and manage the acute infection but also to address the underlying cause and prevent recurrence and further complications. The approach to treatment is dictated by the type of gumboil (periapical, periodontal, pericoronal), the severity of the infection, and the condition of the involved tooth. Regardless of the specific treatment modality, the primary goals are always to eliminate the infection, relieve pain, and preserve the tooth if possible.
The main strategies for **gumboil treatment** include:
1. Incision and Drainage (I&D):
- Purpose: To release the accumulated pus, reduce pressure, and provide immediate pain relief. It’s a critical first step in managing acute, fluctuant abscesses.
- Procedure: A small incision is made into the most fluctuant (softest) part of the abscess using a sterile blade. The pus is allowed to drain out.
- Drainage Maintenance: Sometimes, a small rubber drain (like a Penrose drain) is placed in the incision to keep it open and allow continuous drainage for a few days.
- Benefits: Rapid reduction of swelling and pain, and facilitates the effectiveness of antibiotics.
2. Antibiotic Therapy:
- Purpose: To kill the bacteria causing the infection, especially if there is spreading cellulitis, fever, lymphadenopathy, or if the patient is immunocompromised. Antibiotics alone are rarely sufficient as a definitive treatment because they do not remove the source of infection (necrotic pulp or infected periodontal pocket).
- Commonly Prescribed: Amoxicillin, Clindamycin (for penicillin allergy), Metronidazole (often used in combination with penicillin-based antibiotics for anaerobic coverage).
- Duration: Typically 7-10 days, depending on the severity of the infection.
- Important Note: Antibiotics are an adjunct to, not a substitute for, definitive dental treatment.
3. Root Canal Therapy (RCT):
- Indication: The definitive **gumboil treatment** for periapical abscesses (abscesses originating from an infected tooth pulp).
- Procedure:
- Access is gained to the pulp chamber of the infected tooth.
- The necrotic (dead) or infected pulp tissue, bacteria, and debris are removed from within the root canals.
- The canals are thoroughly cleaned, disinfected, and shaped.
- The cleaned canals are then filled with an inert, biocompatible material (gutta-percha) to seal them and prevent reinfection.
- The tooth is then restored, usually with a crown, to protect it from fracture.
- Benefits: Preserves the natural tooth, eliminates the source of infection, and prevents future abscesses.
4. Tooth Extraction:
- Indication: Considered when the tooth causing the gumboil is extensively damaged, untreatable by root canal therapy, severely compromised by periodontal disease, or if the patient cannot afford or opt for root canal treatment.
- Procedure: The infected tooth is carefully removed from its socket.
- Follow-up: The extraction site is cleaned and may require antibiotics post-operatively. Future options for tooth replacement (implant, bridge, denture) can be discussed.
- Outcome: Eliminates the source of infection, but results in the loss of the natural tooth.
5. Periodontal Treatment:
- Indication: For periodontal abscesses, which originate from bacterial infection in the gum tissues and bone supporting the teeth.
- Procedures:
- Scaling and Root Planing: Deep cleaning procedure to remove plaque, calculus, and bacterial toxins from below the gumline and smooth the root surfaces.
- Periodontal Surgery: May be required to access deeper infected pockets, remove damaged tissue, and reshape bone defects.
- Local Drug Delivery: Placement of antimicrobial agents directly into periodontal pockets.
- Goal: Reduce inflammation, eliminate infection, and stabilize the periodontal health.
6. Pain Management:
- Over-the-Counter (OTC) Analgesics: Non-steroidal anti-inflammatory drugs (NSAIDs) like ibuprofen or naproxen, and acetaminophen, can help manage pain and inflammation.
- Prescription Painkillers: In cases of severe pain, stronger analgesics may be prescribed for a short duration.
7. Home Care and Supportive Measures:
- Warm Salt Water Rinses: Can help soothe the inflamed area, promote drainage, and keep the mouth clean. A teaspoon of salt in a glass of warm water, rinsed several times a day.
- Soft Diet: Avoid hard or sticky foods that might irritate the affected area.
- Good Oral Hygiene: Gentle brushing and flossing around the affected area to maintain cleanliness, while avoiding direct trauma to the gumboil.
The choice of **gumboil treatment** depends heavily on a thorough diagnostic evaluation, including dental X-rays, clinical examination, and patient history. It is crucial to seek professional dental care immediately upon suspecting a gumboil, as untreated infections can lead to serious health complications, including cellulitis, Ludwig’s angina (a severe form of cellulitis that spreads to the floor of the mouth and neck), cavernous sinus thrombosis, and even systemic sepsis. Timely and appropriate intervention is key to a successful outcome and overall oral and systemic health.