Exploring the visual indicators of Marfan syndrome is crucial for early detection and intervention. This article aims to provide a comprehensive look at the various manifestations, guiding users through distinct Marfan syndrome symptoms pictures without showing actual images. Understanding these visual signs can empower individuals and healthcare providers alike.
Marfan syndrome Symptoms Pictures
Individuals with Marfan syndrome often present with a distinctive combination of physical characteristics, many of which are visually striking and crucial for identification. These Marfan syndrome symptoms pictures, though described textually, aim to paint a clear mental image of what to look for, covering skeletal, ocular, and cardiovascular manifestations.
Skeletal System Manifestations (Visual Descriptions):
- Tall Stature and Slender Build: A hallmark visual sign is unusually tall height combined with a disproportionately thin, lanky body frame. This contributes to the overall appearance of someone with Marfanoid habitus.
- Long Limbs (Dolichostenomelia): The arms and legs are notably longer in proportion to the trunk. When standing, arms may appear to reach further down the thighs than typical. This disproportion is a key visual clue.
- Long Fingers and Toes (Arachnodactyly): Fingers and toes are slender, elongated, and sometimes noticeably curved. This gives a “spider-like” appearance to the digits, a classic sign easily observed in Marfan syndrome symptoms pictures. Specific tests include:
- Thumb Sign (Steinberg Sign): When the thumb is fully adducted across the palm, its entire distal phalanx projects beyond the ulnar border of the hand. This is a very strong visual indicator.
- Wrist Sign (Walker Sign): The tip of the thumb and the tip of the fifth finger overlap when grasped around the contralateral wrist. This shows increased wrist circumference relative to the bones and is another common visual sign.
- Pectus Excavatum (Sunken Chest): The sternum and rib cage are sunken inwards, creating a visible depression in the center of the chest. The severity can vary, from subtle to quite pronounced, impacting the contour of the torso.
- Pectus Carinatum (Pigeon Chest): Less common than pectus excavatum, but also a visible chest wall deformity where the sternum protrudes outwards. This creates a noticeable outward bulge of the chest.
- Scoliosis and Kyphosis: Curvature of the spine, either sideways (scoliosis) or an excessive outward curve of the upper back (kyphosis), is frequently observed. These spinal deformities are often visible upon inspection of the back, creating uneven shoulders or a prominence of one side of the rib cage.
- Joint Hypermobility: Joints may appear unusually flexible, with individuals able to extend limbs beyond the normal range of motion. This might be seen in hyperextended elbows, knees, or fingers, creating an appearance of unusual suppleness.
- Pes Planus (Flat Feet): The arches of the feet are flattened, often severely, leading to the entire sole of the foot making contact with the ground. This visual sign is evident when examining the feet.
- High Arched Palate and Crowded Teeth: Inside the mouth, the roof of the mouth (palate) is often unusually high and narrow. This can lead to dental crowding and an altered facial structure, though less immediately obvious than other skeletal signs.
Ocular System Manifestations (Visual Descriptions):
- Lens Dislocation (Ectopia Lentis): This is one of the most specific ocular signs. The lens of the eye shifts out of its normal central position, usually upwards and outwards. In some cases, the displaced lens may be visible upon careful inspection, especially when pupils are dilated, appearing as an abnormal reflection or position within the pupil.
- Myopia (Nearsightedness): While not directly visible, severe myopia is common. Patients often wear thick corrective lenses, which can be an indirect visual cue.
- Corneal Flatness: The cornea may appear flatter than usual, which is detectable during an eye exam.
- Strabismus (Crossed Eyes) or Amblyopia (Lazy Eye): These conditions, resulting from vision problems, are visually evident as misalignment of the eyes.
Cardiovascular System Manifestations (Visual Descriptions):
While most cardiovascular issues are internal, certain signs can indirectly suggest underlying problems or are detected during examinations. These are critical aspects that inform the comprehensive understanding of Marfan syndrome symptoms pictures, even if not immediately obvious from a casual glance.
- Aortic Dilation and Dissection: These severe conditions are internal and not visible externally, but they are the most life-threatening aspects of Marfan syndrome. Monitoring for symptoms like sudden chest or back pain is crucial, which could lead to an urgent clinical presentation.
- Mitral Valve Prolapse: Similar to aortic issues, this is an internal finding, detected by auscultation (listening to heart sounds).
- Thin, Stretchy Skin: While more general, some individuals exhibit skin that appears more lax or stretchy, particularly around joints, which can be an indirect sign.
Signs of Marfan syndrome Pictures
Beyond the most prominent features, numerous other signs of Marfan syndrome pictures offer crucial diagnostic clues. These signs often require a keen eye or specific examination techniques to identify, providing a more detailed picture of the syndrome’s pervasive effects across the body systems.
Refined Skeletal Signs and Proportions:
- Reduced Upper-to-Lower Segment Ratio: The measurement from the top of the head to the pubis, compared to the measurement from the pubis to the floor, reveals that the lower segment is disproportionately long. This specific ratio deviation is a strong diagnostic indicator.
- Arm Span Exceeding Height: When arms are outstretched, the distance from fingertip to fingertip is significantly greater than the individual’s height. This “wingspan” is a classic visual and measurable sign.
- Joint Laxity and Instability: Beyond hypermobility, some joints, particularly shoulders, hips, and patellae, may visibly sublux (partially dislocate) or dislocate more easily. This can manifest as an unusual ‘looseness’ or clicking sensation in the joints.
- Protruding Acetabulum: The hip socket (acetabulum) can be unusually deep, known as protrusio acetabuli. While not directly visible, it affects gait and posture, leading to an altered stance that might be observed.
- Vertebral Erosions (Dural Ectasia): Expansion of the dura mater (the membrane surrounding the spinal cord) can erode the vertebrae, especially in the lumbosacral region. While not an external sign, severe dural ectasia can contribute to back pain and neurological symptoms, impacting posture or movement.
- Patellar Dislocation: The kneecap may visibly shift out of place, causing pain and instability. This can be seen as an obvious deformity of the knee joint during an episode.
Facial Features (Visual Characteristics):
- Long, Narrow Face (Dolichocephaly): The head shape is often elongated and narrow.
- Deep-Set Eyes: Eyes may appear sunken within the eye sockets.
- Downward-Slanting Palpebral Fissures: The opening between the eyelids (palpebral fissure) may slant downwards laterally, giving a characteristic facial expression.
- Enophthalmos: The eyeballs are noticeably recessed into the orbits.
- Malar Hypoplasia: Underdevelopment of the cheekbones, contributing to a flatter midface appearance.
- Micrognathia or Retrognathia: The lower jaw may be unusually small (micrognathia) or set back (retrognathia), contributing to an abnormal profile.
- High Arched Palate and Dental Malocclusion: Revisited, these oral features can lead to a narrow dental arch and misaligned teeth, visually altering the mouth’s appearance.
Skin and Integumentary Signs:
- Atrophic Striae (Stretch Marks): These are distinct, often purplish or reddish, then fading to silvery-white, linear marks on the skin. They frequently appear in unusual locations not typically associated with weight gain or pregnancy, such as the shoulders, lower back, and hips, even in individuals who haven’t undergone significant growth spurts or weight changes. These spontaneous stretch marks are a key visible sign in many with Marfan syndrome.
- Hernias: Increased propensity for inguinal or incisional hernias, which can appear as visible bulges under the skin, especially with straining.
- Recurrent Pneumothorax: While not a direct skin sign, a history of spontaneous lung collapse can indirectly suggest the underlying connective tissue weakness of Marfan syndrome, though it’s an internal event.
Neurological Signs (Indirect Visual Cues):
- Headaches and Back Pain: While not visually direct signs, chronic headaches or persistent back pain, particularly in the lower back, can be secondary to dural ectasia and may influence posture or facial expressions of discomfort, providing indirect visual cues.
- Foot Deformities: Aside from flat feet, bunions or hammertoes may develop, altering the visible structure of the foot.
Early Marfan syndrome Photos
Identifying Marfan syndrome in infants and young children can be challenging, as many classic features develop over time. However, certain early signs, even subtle ones, can alert clinicians. Understanding what to look for in early Marfan syndrome photos – or descriptions of such – is vital for timely diagnosis and management. These initial indicators often lay the groundwork for the more pronounced features seen in adulthood.
Infancy and Early Childhood Indicators:
- Failure to Thrive (Less Common but Possible): Some infants may have difficulty gaining weight, though this is not a specific Marfan sign.
- Hypotonia (Low Muscle Tone): Infants may appear “floppy,” with less resistance to movement in their limbs. This can be observed in their posture and how they hold their body.
- Skeletal Proportions: Even in infancy, slightly longer limbs relative to the trunk might be discernible, though not as pronounced as later. The infant may appear lanky.
- Foot Deformities: Severe flat feet (pes planus) may be present early on.
- Chest Wall Deformities: Subtle pectus excavatum or carinatum may begin to develop and become noticeable as the child grows.
- Scoliosis: Early onset scoliosis can appear in childhood, presenting as an asymmetry in the back or shoulders. Regular postural checks are important.
- Ocular Signs:
- Ectopia Lentis: Lens dislocation can be present at birth or develop in early childhood, leading to vision problems that might be noticed by parents (e.g., child not tracking objects, unusual eye movements).
- Severe Myopia: High degrees of nearsightedness requiring early corrective lenses.
- Facial Features: The long, narrow face and deep-set eyes may begin to be apparent in childhood, subtly distinguishing the child’s features.
Adolescent Onset and Progression:
As children enter adolescence, growth spurts can exacerbate existing features and bring new ones to prominence, making early Marfan syndrome photos from this period particularly illustrative of symptom progression.
- Rapid Increase in Height: A sudden and disproportionate growth spurt, often leading to a height significantly above peers.
- Exaggeration of Skeletal Features:
- Arachnodactyly: Fingers and toes become noticeably longer and more slender.
- Joint Hypermobility: Becomes more apparent, with increased range of motion in joints.
- Scoliosis and Kyphosis: Existing curves may worsen rapidly during growth spurts, requiring closer monitoring. The visible spinal deformity becomes more pronounced.
- Pectus Deformities: Chest wall abnormalities typically become more evident and may deepen or protrude further.
- Appearance of Striae: Spontaneous stretch marks on the back, shoulders, and hips often emerge during adolescence, even without significant weight changes. These linear skin lesions are a key visual marker in adolescent Marfan syndrome.
- Cardiovascular Monitoring: While not visually explicit, early and routine cardiovascular screening becomes paramount in adolescence, as aortic dilation can progress silently.
- Dental Issues: Continued development of a high-arched palate and crowded teeth, potentially affecting speech or eating.
The progression of these signs emphasizes the importance of ongoing clinical surveillance, especially when one or more suggestive features are observed in a child or adolescent. Early recognition of these developing characteristics is critical for early diagnosis and intervention in Marfan syndrome.
Skin rash Marfan syndrome Images
When considering “skin rash Marfan syndrome images,” it’s important to clarify that Marfan syndrome is not typically characterized by a conventional inflammatory “rash” or allergic skin eruption. Instead, the skin manifestations of Marfan syndrome relate to the underlying connective tissue fragility. The most prominent and diagnostically relevant skin sign is the presence of atrophic striae. Other related skin findings reflect the systemic nature of the disorder.
Key Skin Manifestations (Not a Typical Rash):
- Atrophic Striae (Stretch Marks): This is the most common and visually significant skin finding.
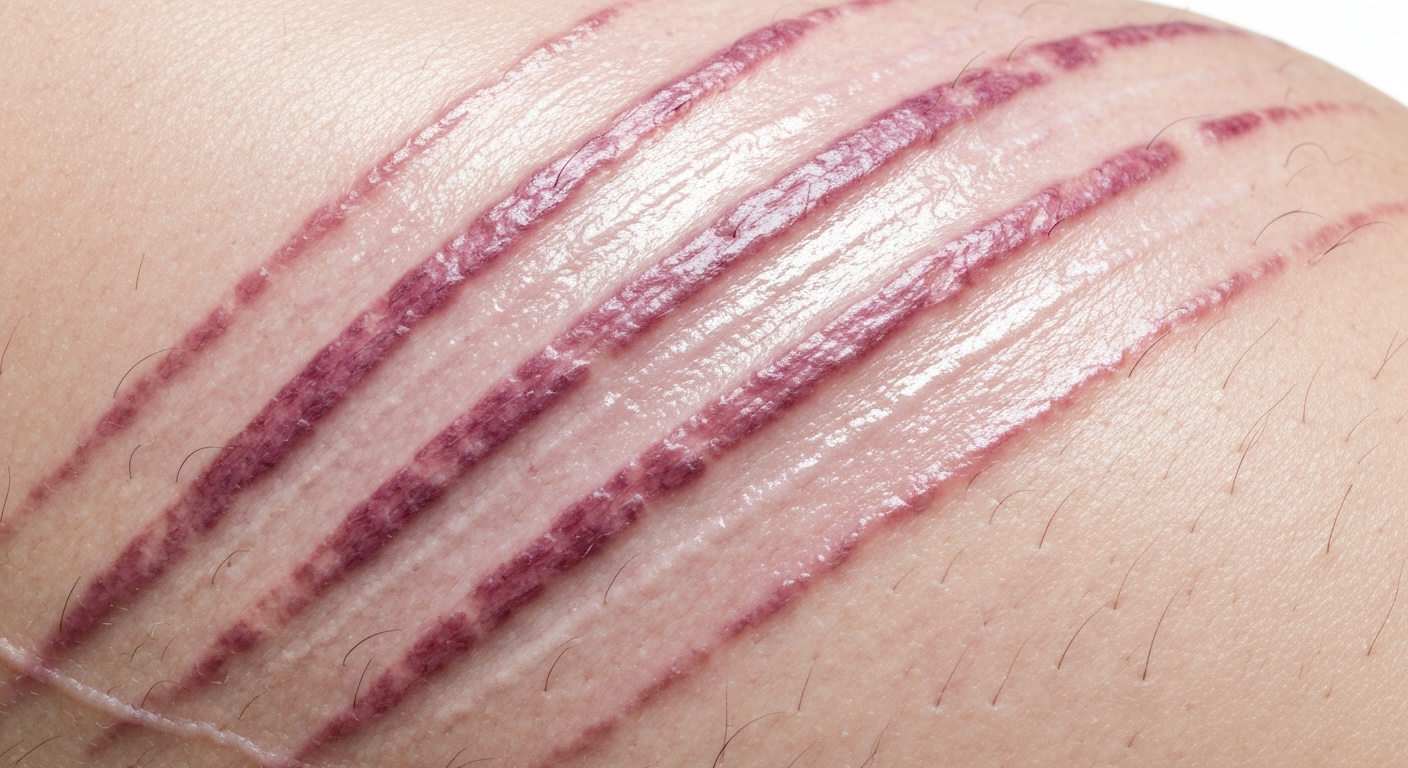
- Appearance: These are linear, band-like lesions in the skin, initially often reddish or purplish, which then fade over time to become shiny, white, or silvery. They have a thin, atrophic (thinned) appearance.
- Location: Unlike typical stretch marks from rapid weight changes or pregnancy, Marfan striae frequently occur in unusual locations such as the shoulders (deltoid region), upper arms, lower back (lumbar area), buttocks, and hips. They can also appear on the breasts, abdomen, and thighs.
- Cause: They are believed to result from the intrinsic weakness of the connective tissue (specifically collagen and elastic fibers) in the dermis, which makes the skin less resilient to normal mechanical stresses, leading to tears in the dermis even without significant stretching.
- Visual Impact: The presence of numerous, widespread, and spontaneously occurring striae, especially in these atypical areas, is a strong visual clue for Marfan syndrome.
- Skin Laxity and Elasticity:
- Appearance: Some individuals with Marfan syndrome may have skin that appears softer, smoother, or more velvety to the touch. It might also show increased laxity, meaning it can be stretched further than typical before returning to its original position.
- Location: This general characteristic can be observed across the body, particularly in areas with greater movement or stress.
- Visual Impact: While not as distinct as striae, this quality contributes to the overall impression of altered connective tissue.
- Increased Risk of Hernias:
- Appearance: Hernias (e.g., inguinal, umbilical, incisional) manifest as visible bulges under the skin where an organ or tissue protrudes through a weakened area in the muscle wall.
- Location: Common sites include the groin (inguinal hernia) or around the navel (umbilical hernia).
- Cause: The connective tissue weakness predisposes individuals to these ruptures.
- Visual Impact: A visible, often reducible, lump or swelling is characteristic of a hernia.
- Poor Wound Healing/Abnormal Scarring (Less Common but Noted):
- Appearance: While not a primary diagnostic criterion, some individuals may experience slower wound healing or develop wider, atrophic scars after injury or surgery.
- Visual Impact: Scars may appear thinner or more stretched than expected.
Distinguishing Marfan Skin Findings from Other Conditions:
It is crucial to differentiate these skin findings from true inflammatory rashes, allergic reactions, or dermatological conditions not related to connective tissue disorders. The skin signs in Marfan syndrome are primarily structural and related to the integrity of the dermal components rather than an inflammatory process. Therefore, when discussing “skin rash Marfan syndrome images,” the focus should strongly remain on descriptions of striae and general skin texture rather than inflammatory lesions.
Marfan syndrome Treatment
The treatment for Marfan syndrome is multi-faceted, focusing on managing symptoms, preventing complications, and improving quality of life. Given the systemic nature of the disorder, a multidisciplinary approach involving cardiologists, ophthalmologists, orthopedic surgeons, and geneticists is essential. The goal is to monitor closely and intervene proactively, especially concerning the life-threatening cardiovascular manifestations. While this section doesn’t relate to “pictures,” it outlines the comprehensive care required for individuals with Marfan syndrome.
Cardiovascular Management (Critical Focus):
This is the most critical aspect of Marfan syndrome treatment due to the risk of aortic dissection and rupture.
- Medication:
- Beta-blockers: Medications like atenolol or metoprolol are often prescribed to reduce heart rate and the force of blood ejection from the heart, thereby decreasing stress on the aortic wall.
- Angiotensin Receptor Blockers (ARBs): Drugs such as losartan or irbesartan have shown promise in reducing aortic growth, potentially even more effectively than beta-blockers in some cases, by modulating TGF-β signaling.
- Blood Pressure Control: Strict control of blood pressure is essential to minimize stress on the aorta.
- Regular Monitoring:
- Echocardiograms: Annual or more frequent echocardiograms are crucial to measure aortic root diameter and assess valve function.
- MRI/CT Scans: Periodic imaging of the entire aorta (from chest to pelvis) is often recommended to monitor for dilation or aneurysms in other segments of the aorta.
- Surgical Intervention:
- Aortic Root Replacement: Prophylactic surgery to replace the dilated aortic root with a composite graft (Dacron tube with an artificial valve) is typically performed when the aortic diameter reaches a certain threshold (e.g., 4.5-5.0 cm), or if there’s rapid growth. This surgery significantly reduces the risk of dissection.
- Valve-Sparing Aortic Root Replacement: In some cases, the aortic valve can be preserved while replacing the dilated aortic root, maintaining the patient’s own valve.
- Other Aortic Surgeries: Repair or replacement of other parts of the aorta (e.g., descending aorta) if aneurysms develop.
Ocular Management:
- Corrective Lenses: Glasses or contact lenses to correct myopia and astigmatism.
- Cataract Surgery: If cataracts develop.
- Glaucoma Treatment: Medications or surgery if intraocular pressure is elevated.
- Lens Surgery (Lensectomy): If ectopia lentis causes significant vision impairment that cannot be corrected with glasses, surgical removal of the dislocated lens may be necessary.
- Retinal Detachment Repair: Prompt surgical intervention if retinal detachment occurs.
Skeletal Management:
- Orthopedic Bracing/Surgery for Scoliosis:
- Bracing: For moderate scoliosis, a brace may be used to prevent further curve progression, especially during growth spurts.
- Spinal Fusion Surgery: For severe or progressive scoliosis (curves typically >40-50 degrees), surgical correction and fusion may be necessary to stabilize the spine and prevent further deformity.
- Chest Wall Deformity Repair:
- Pectus Excavatum/Carinatum Repair: Surgical correction (Nuss procedure or Ravitch procedure) may be considered for severe deformities that cause respiratory compromise, cosmetic concern, or pain.
- Foot Arch Supports/Orthotics: To provide support for flat feet and alleviate pain.
- Pain Management: For joint pain or back pain, physical therapy, anti-inflammatory medications, and lifestyle modifications.
- Physical Therapy: To strengthen muscles, improve posture, and manage joint hypermobility or pain.
Other Management Strategies:
- Genetic Counseling: Essential for affected individuals and their families to understand the inheritance pattern, risks, and reproductive options.
- Lifestyle Modifications: Avoiding strenuous activities, contact sports, and activities that involve sudden increases in blood pressure (e.g., heavy lifting, isometric exercises) to protect the aorta.
- Pregnancy Management: Women with Marfan syndrome require specialized cardiovascular care during pregnancy due to the increased risk of aortic dissection.
- Psychological Support: Counseling and support groups can help individuals cope with the chronic nature of the condition and its potential impact on daily life.
Ongoing research continues to refine treatments and strategies for Marfan syndrome, with a focus on understanding the underlying genetic mechanisms to develop targeted therapies. Regular, lifelong follow-up with a dedicated medical team is paramount for optimal outcomes in managing this complex disorder.