Exploring the visual indicators of bacterial skin infections is crucial for early recognition and intervention. This article provides detailed descriptions corresponding to
Pyoderma Symptoms Pictures
When examining
Common visual presentations of pyoderma include:
Erythema: Redness of the skin, often around the site of infection, indicating inflammation and increased blood flow. This can range from a faint pink blush to a vibrant, angry red hue, typically warm to the touch.Edema: Swelling of the affected area due to fluid accumulation, making the skin appear puffy or raised. This swelling can be localized or spread, depending on the extent of the infection, and is a prominent feature in manyPyoderma symptoms pictures .Pustules: Small, raised bumps on the skin filled with pus, which is a collection of dead white blood cells, bacteria, and tissue debris. These lesions are usually yellow, white, or greenish and are characteristic of many pyodermas, providing direct evidence of bacterial activity.Vesicles and Bullae: Small (vesicles) or large (bullae) fluid-filled blisters that can contain clear fluid initially, but often become cloudy or purulent as the infection progresses. Bullous impetigo, for instance, is characterized by large, fragile bullae that rupture to form crusts.Crusts: Dried exudates (serum, pus, blood) that form a scab-like covering over eroded or ulcerated skin. Honey-colored crusts are pathognomonic for impetigo, one of the most common forms of pyoderma, and are frequently highlighted inPyoderma symptoms pictures .Erosions and Ulcerations: Areas where the epidermis has been lost (erosions) or where the skin layers are deeply excavated (ulcerations). Ecthyma, a deeper form of impetigo, is characterized by punched-out ulcers covered with thick, adherent crusts.Folliculitis: Inflammation of hair follicles, appearing as small, red bumps or pustules centered around a hair follicle. This can occur anywhere hair grows, including the scalp, face, trunk, and extremities, often seen as multiple discrete lesions inPyoderma symptoms pictures .Furuncles (Boils): Deeper infections of hair follicles that extend into the surrounding dermis and subcutaneous tissue, forming painful, red, swollen nodules with a central pus-filled core that may eventually rupture and drain. These are typically larger and more indurated than simple folliculitis.Carbuncles: Clusters of interconnected furuncles that form a larger, deeper, and more extensive infection, often with multiple draining sinuses. Carbuncles are very painful and can cause systemic symptoms, presenting as large, inflamed masses inPyoderma symptoms pictures .Cellulitis: A spreading bacterial infection of the dermis and subcutaneous tissue, characterized by diffuse redness, warmth, swelling, and tenderness. The borders are often ill-defined, and streaking (lymphangitis) may be present, indicating lymphatic spread. This is a more severe form of bacterial skin infection that can stem from untreated pyoderma.Abscesses: Localized collections of pus within the skin or deeper tissues, often encapsulated, forming a painful, fluctuating lump. These typically require incision and drainage in addition to antibiotic therapy.
Understanding these specific features within
Signs of Pyoderma Pictures
The
Key observable signs in
Inflammation: Evidenced by prominent redness (erythema), swelling (edema), warmth, and tenderness upon touch. The inflammatory halo around a lesion is a strong indicator of an active infection.Purulent Discharge: The presence of pus, which can be yellow, white, green, or brown, often observed oozing from lesions, especially after they rupture. This purulence is a definitive sign of bacterial activity and is a common finding in detailedsigns of Pyoderma pictures .Crusting and Scabbing: Formation of dried serum and pus over ruptured lesions. As mentioned, honey-colored crusts are classic for impetigo, but other forms of pyoderma can have darker, more adherent scabs, particularly in ecthyma.Pain and Tenderness: While not directly visible in pictures, the context often implies this sign, especially with deeper infections like furuncles and carbuncles, which appear significantly inflamed and indurated.Warmth: The affected skin area feels warmer than the surrounding healthy skin due to increased blood flow from inflammation. This is often described as a tactile sign, but visually, the intense erythema insigns of Pyoderma pictures can suggest it.Lymphadenopathy: Swollen and tender regional lymph nodes, indicating that the lymphatic system is responding to the infection. While not a direct skin sign, significant skin infections, especially on the extremities, can show correlating signs of lymph node involvement elsewhere in diagnosticsigns of Pyoderma pictures .Fever and Malaise: Systemic signs, though not visible on the skin, often accompany more severe or widespread pyoderma, such as cellulitis or carbuncles. The overall appearance of a patient in a medical setting might implicitly convey these systemic effects.Induration: Hardening or thickening of the skin due to inflammation and edema, particularly noticeable in deeper infections like cellulitis, furuncles, and carbuncles. The skin feels firm and dense to the touch.Tracking or Streaking: Red lines extending from the primary infection site towards regional lymph nodes (lymphangitis), indicating the spread of bacteria through lymphatic channels. This is a critical sign of advancing infection and is often visible in more serioussigns of Pyoderma pictures .Itching (Pruritus): While scratching itself can cause secondary excoriations, the underlying itch is a common symptom reported by patients and can be inferred from signs of scratching in somesigns of Pyoderma pictures .Fissures and Rhagades: Cracks or linear breaks in the skin, especially in areas of chronic inflammation or dryness, which can serve as entry points for bacteria or occur secondary to inflammation.Hemosiderin Staining: Brownish discoloration of the skin, particularly after resolution of deep or recurrent infections, due to the deposition of iron from red blood cell breakdown. This indicates previous significant inflammation and bleeding in the skin layers.Scarring and Post-inflammatory Hyperpigmentation/Hypopigmentation: Changes in skin texture and color that remain after the pyoderma has healed, especially following deeper lesions like ecthyma or carbuncles. These are lastingsigns of Pyoderma pictures that show the aftermath of the infection.
Careful observation of these signs in
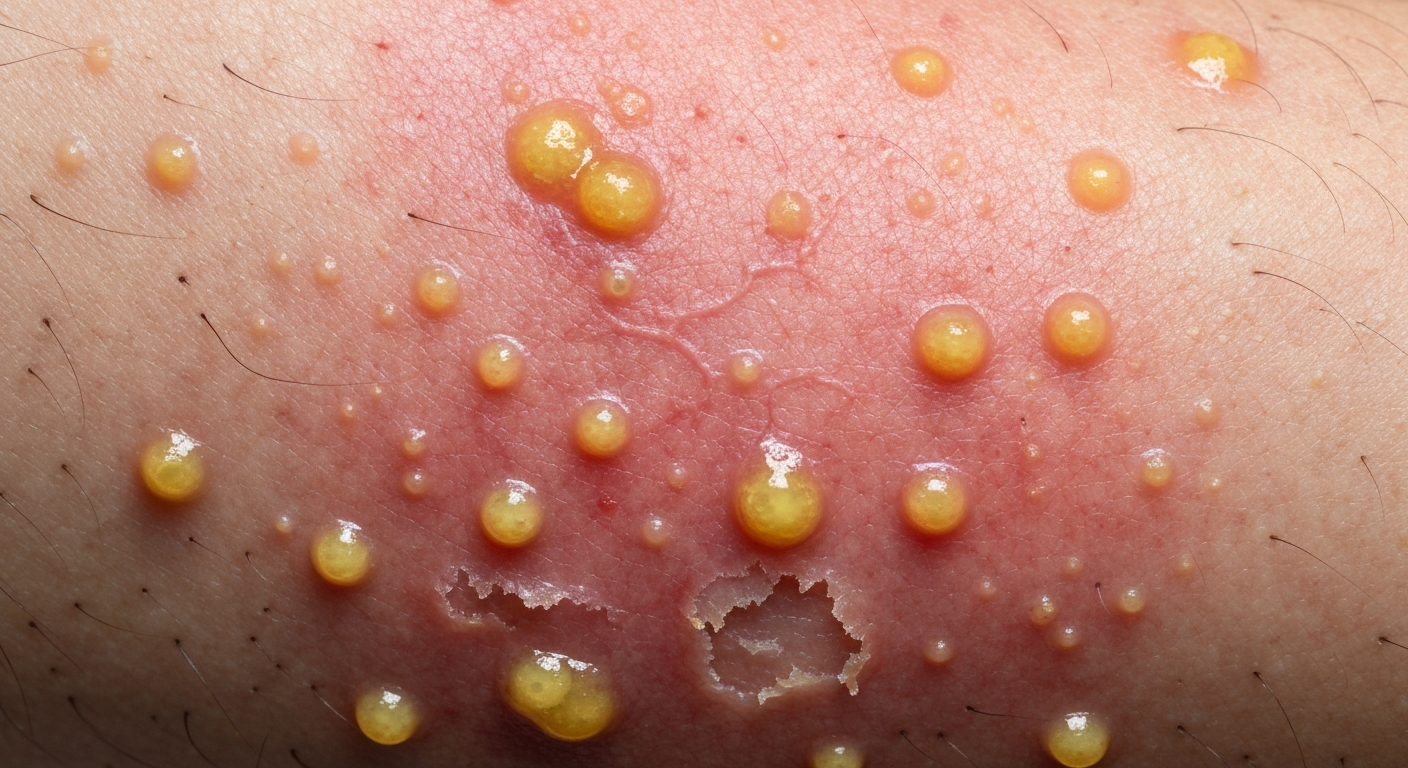
Early Pyoderma Photos
Common presentations in
Small Red Papules: The initial sign of many pyodermas, particularly impetigo or folliculitis, where a small, red, raised bump appears on the skin. These papules may be slightly tender or itchy and are often the first visible hint of an underlying bacterial process.Pinpoint Pustules: Very small, discrete collections of pus that may develop rapidly from papules. These can appear as tiny white or yellow “pimples” and are a clear indicator of bacterial activity, often observed centered around hair follicles in early folliculitis.Tiny Vesicles: Small, clear fluid-filled blisters that can quickly turn cloudy or rupture. In early impetigo, these vesicles are often fragile and ephemeral, rapidly progressing to erosions and crusts.Early Pyoderma photos often capture these delicate initial formations.Localized Erythema: A focused patch of redness, often warm to the touch, indicating the beginning of an inflammatory response. This can be the precursor to more diffuse cellulitis if not addressed, starting as a small area of discoloration.Perifollicular Redness: A subtle reddening around the base of individual hair follicles, signaling the start of folliculitis. This can progress to a pustule within the follicle, making it a key feature inEarly Pyoderma photos depicting hair-bearing areas.Slight Swelling or Induration: A barely perceptible elevation or hardening of the skin texture, which may be felt before it is clearly seen. This early edema is a response to bacterial toxins and inflammatory mediators.Pruritus (Itching): While not a visual sign, intense itching can lead to scratching, which creates excoriations that appear as linear abrasions or small scabs. These can then become entry points for bacteria, making their appearance inEarly Pyoderma photos an indirect sign of potential infection onset.Tenderness upon Palpation: Although not directly imageable, the context of a patient presenting with discomfort on touch of a specific skin area is often documented alongsideEarly Pyoderma photos , guiding the visual examination.Discomfort or Mild Pain: A localized sensation of irritation or pain at the site of the nascent lesion, indicating tissue damage or nerve involvement from the bacterial presence.Minimal Drainage: Occasionally, a very small amount of clear or slightly cloudy fluid may be observed, which soon dries to form a thin crust. This is often seen in very early impetigo before the characteristic honey-colored crusts fully develop.No Systemic Symptoms: Typically, at the very early stages, patients will not exhibit fever, chills, or widespread malaise. The infection is usually localized to the skin surface.Discrete Lesions: Early pyoderma often starts as one or a few distinct lesions, rather than a widespread rash. This discrete nature helps pinpoint the initial site of infection before secondary spread occurs.
By carefully examining
Skin rash Pyoderma Images
Characteristic features found in
Widespread Impetigo: Impetigo contagiosa, especially in children, can present as multiple, rapidly spreading lesions that cover a significant area of skin. These lesions are characterized by vesicles and bullae that rupture and form classic honey-colored crusts, often merging into a large, crusted plaque.Folliculitis Rash: An eruption of numerous small, red papules or pustules, each centered around a hair follicle, spread across a hairy area such as the back, chest, scalp, or legs. This can be caused by bacterial (e.g., Staphylococcus aureus) or sometimes fungal infections, but bacterial folliculitis is a common pyoderma.Ecthyma (Multiple Lesions): While typically deeper and more localized, severe cases or immunocompromised individuals might develop multiple ecthymatous lesions that, when clustered, can give the appearance of a severe, ulcerative rash. These are characterized by punched-out ulcers with thick, adherent crusts.Cellulitis with Satellite Lesions: Although cellulitis is typically a spreading erythema, the presence of smaller, distinct pustules or vesicles (satellite lesions) within or at the periphery of the main cellulitic patch can suggest a bacterial etiology and contribute to a rash-like presentation, especially in immunocompromised individuals.Erysipelas (Diffuse, Sharply Demarcated Rash): A superficial form of cellulitis caused by Streptococcus pyogenes, characterized by a bright red, edematous, warm, and sharply demarcated rash. While usually a single lesion, its size and rapid spread can sometimes be considered a rash-like presentation, often on the face or legs.Intertriginous Pyoderma: Bacterial infections that occur in skin folds (e.g., armpits, groin, under breasts), exacerbated by moisture and friction. These can present as erythematous, macerated (softened and whitish from moisture) patches with pustules, erosions, and fissures, forming a rash-like pattern in the affected folds.Pyoderma Gangrenosum (Atypical Rash): While not a primary bacterial infection, pyoderma gangrenosum lesions often become secondarily infected. These begin as small papules, pustules, or nodules that rapidly ulcerate into painful, necrotic ulcers with violaceous, undermined borders. When multiple lesions occur, they can form a very atypical and severe “rash.”Superficial Perianal Pyoderma: A bacterial infection around the anus, typically seen in children, presenting as an intensely red, well-demarcated rash with little scaling. It can be quite itchy and tender.Necrotizing Fasciitis (Rapidly Spreading, Severe Rash): A severe, rapidly progressive bacterial infection that affects the fascia. While initially presenting as a small painful area of redness, it quickly spreads, causing skin discoloration (purplish), blistering, necrosis, and crepitus, forming a rapidly evolving and extremely serious rash.Hidradenitis Suppurativa with Secondary Infection: Chronic inflammatory condition affecting apocrine sweat glands, often leading to abscesses, sinus tracts, and scarring. These lesions are highly prone to secondary bacterial infection, creating a challenging, widespread rash-like appearance of inflamed nodules and draining areas.Skin Grafts with Infection: Post-surgical skin grafts, when infected, can show signs of a spreading bacterial rash, including erythema, exudate, and possible graft failure. These images highlight the compromised healing process.
The appearance of
Pyoderma Treatment
Effective
Primary modalities for
Topical Antibiotics: Mupirocin: Often the first-linePyoderma treatment for localized impetigo or minor folliculitis. It is applied directly to the lesions to inhibit bacterial growth. Highly effective against Staphylococcus aureus (including MRSA) and Streptococcus pyogenes.Fusidic Acid: Another potent topical antibiotic, particularly useful for staphylococcal skin infections. It helps to reduce bacterial load and promote healing of superficial pyodermas.Retapamulin: A newer topical pleuromutilin antibiotic approved for impetigo caused by susceptible Staphylococcus aureus or Streptococcus pyogenes.Erythromycin or Clindamycin (topical forms): Less commonly used as primary pyoderma treatments due to resistance, but can be considered in specific cases or for acne-related folliculitis.Bacitracin/Polymyxin B (Neosporin-type products): While over-the-counter, these are generally less effective for established pyoderma and more suited for minor cuts and scrapes to prevent infection.
Oral Antibiotics: Penicillinase-resistant Penicillins (e.g., Dicloxacillin, Flucloxacillin): Frequently used for staphylococcal infections that are extensive, deeper, or not responding to topical agents. These are effectivePyoderma treatment options for cellulitis, furuncles, and carbuncles.Cephalosporins (e.g., Cephalexin): Broad-spectrum antibiotics often prescribed for a range of pyodermas, including impetigo, folliculitis, and cellulitis, offering good coverage against common Gram-positive bacteria.Macrolides (e.g., Azithromycin, Erythromycin, Clarithromycin): AlternativePyoderma treatment for patients with penicillin allergy. However, increasing resistance, especially among staphylococci, can limit their utility.Clindamycin: Effective against both staphylococcal and streptococcal infections, particularly useful in cases involving anaerobic bacteria or in suspected MRSA infections.Doxycycline/Minocycline/Trimethoprim-Sulfamethoxazole (TMP-SMX): Common choices for community-acquired Methicillin-resistant Staphylococcus aureus (CA-MRSA) infections, which are becoming increasingly prevalent causes of pyoderma.Linezolid/Vancomycin: Reserved for severe, systemic, or resistant infections, often requiring intravenous administration in a hospital setting for serious pyoderma.
Incision and Drainage (I&D): Abscesses, Furuncles, Carbuncles: Surgical drainage is often the definitivePyoderma treatment for these localized collections of pus. It helps relieve pain, removes the source of infection, and facilitates healing. Antibiotics may or may not be needed post-drainage depending on severity and systemic signs.Wound Debridement: Removal of necrotic (dead) tissue is essential for deeper infections like ecthyma or in cases where extensive tissue damage has occurred, allowing healthy tissue to heal.
Supportive Care and Hygiene: Warm Compresses: Applying warm, moist compresses to furuncles and carbuncles can help promote drainage and reduce discomfort, aiding in thePyoderma treatment process.Antiseptic Washes (e.g., Chlorhexidine, Benzoyl Peroxide): Used to reduce bacterial colonization on the skin, especially in individuals prone to recurrent pyoderma, acting as a preventative measure.Regular Washing with Mild Soap: Maintaining good personal hygiene is fundamental to preventing the spread and recurrence of bacterial skin infections.Covering Lesions: Covering active lesions, especially impetigo, can help prevent spread to others and reduce self-inoculation.Pain Management: Over-the-counter pain relievers (e.g., ibuprofen, acetaminophen) can help manage discomfort associated with inflammatory pyoderma.Addressing Predisposing Factors: Identifying and managing underlying conditions such as diabetes, eczema, poor hygiene, or immunosuppression is crucial for long-term control and preventing recurrent pyoderma.Cleanliness of Clothing and Linens: Washing clothes, towels, and bed linens in hot water can help eliminate bacteria and prevent reinfection or spread within a household, forming a key part of comprehensivePyoderma treatment and prevention.
Management of Recurrent Pyoderma: Nasal Decolonization: For recurrent staphylococcal infections, screening for nasal carriage of S. aureus (including MRSA) and subsequent decolonization with intranasal mupirocin may be necessary.Bleach Baths: Diluted bleach baths can be recommended for individuals with recurrent staphylococcal infections, particularly those with atopic dermatitis, to reduce skin bacterial load.Antimicrobial Soaps: Persistent use of antiseptic soaps or body washes can help reduce superficial bacterial colonization over time.Environmental Cleaning: Thorough cleaning of shared surfaces, gym equipment, and communal spaces can help reduce transmission of resistant strains in high-risk environments.
The choice of