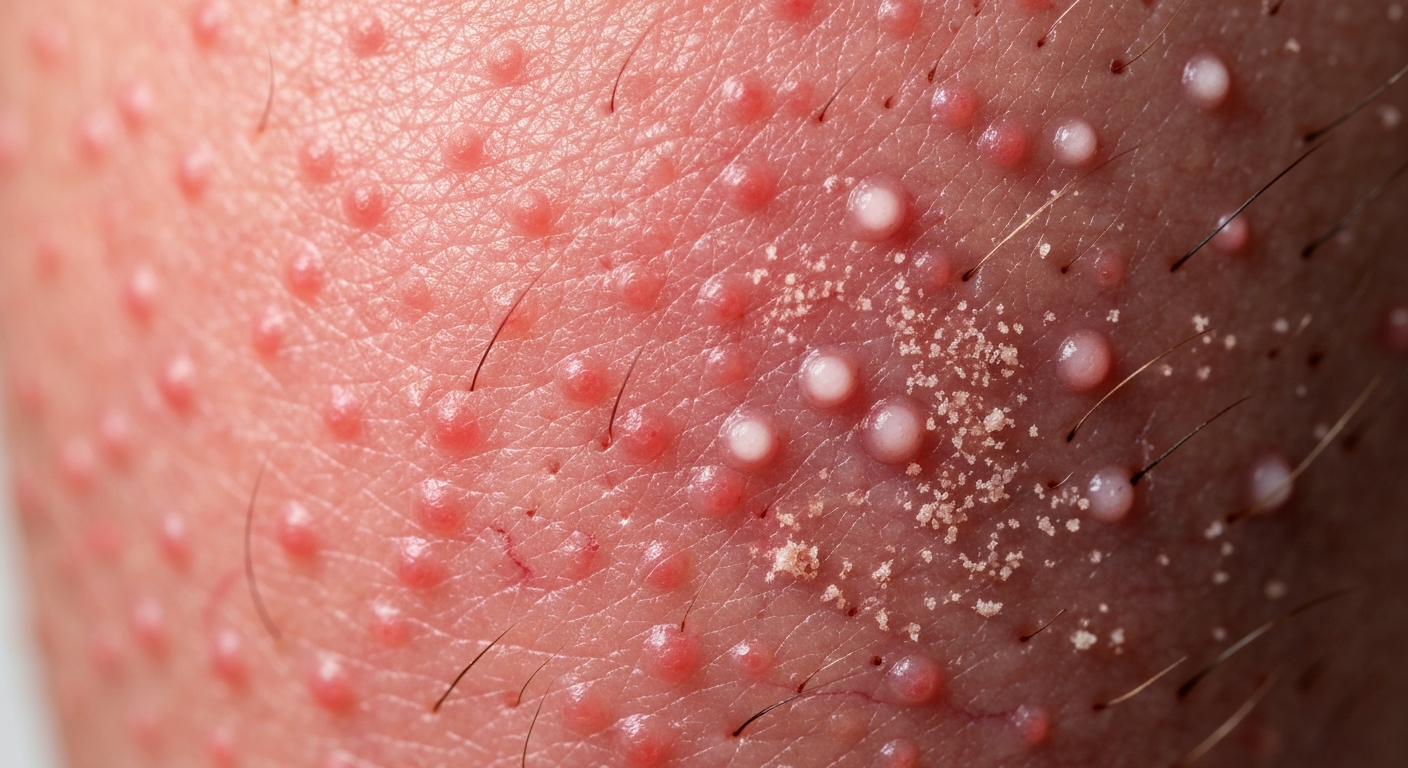
This article provides an in-depth look at **Demodicosis on the face symptoms pictures**, offering crucial insights for recognizing and understanding this common skin condition. We detail the varied manifestations, from subtle early signs to more pronounced skin rashes, to aid in visual recognition and guide appropriate management strategies for **Demodex mite infestations**.
Demodicosis on the face Symptoms Pictures
Understanding the varied **Demodicosis on the face symptoms pictures** is essential for accurate identification and timely intervention. Facial demodicosis, caused by an overpopulation of **Demodex mites**, primarily **Demodex folliculorum** and **Demodex brevis**, can present with a wide array of visual symptoms that often mimic other dermatological conditions. The clinical presentation is highly variable and depends on factors such as the individual’s immune response, skin type, and the density of the mite infestation. Patients frequently report a combination of subjective symptoms and objective signs visible on the skin.
Common **Demodex facial symptoms** include:
- Erythema (Redness): One of the most pervasive **demodicosis skin symptoms** is persistent or intermittent facial redness. This erythema can be diffuse, covering large areas like the cheeks, forehead, and chin, or localized in patches. It often presents as a flushed appearance, sometimes mistaken for rosacea. The redness can fluctuate in intensity, worsening with environmental triggers or stress.
- Papules: Small, solid, raised bumps without pus are a characteristic **demodicosis rash on face** feature. These papules are often reddish or skin-colored and can be firm to the touch. They may appear singly or in clusters, frequently found around the nose, mouth, and on the cheeks. Their presence indicates inflammation within the hair follicles or sebaceous glands where the mites reside.
- Pustules: Similar to papules but containing pus, pustules are another common manifestation. These small, elevated lesions with a white or yellow center are indicative of an inflammatory response, often to the mite’s byproducts or associated bacterial flora. Pustules can be a significant cosmetic concern and may lead to discomfort.
- Scaling and Flaking: Fine, bran-like scaling, especially around the eyebrows, nose, and hairline, is a frequent symptom. This occurs due to accelerated skin cell turnover and inflammation. The skin may feel rough or dry to the touch, and flaking can be more noticeable after washing or in dry environments.
- Itching (Pruritus): While not always present, moderate to severe itching, particularly worse at night, is a strong indicator of **demodex mites symptoms**. This nocturnal exacerbation is thought to be due to increased mite activity as they emerge from follicles. The itching can lead to scratching, which further irritates the skin and can cause excoriations.
- Burning Sensation: Many individuals with facial demodicosis report a burning or stinging sensation on the affected skin areas. This discomfort can be persistent or triggered by topical products, sunlight, or temperature changes.
- Skin Sensitivity: Increased skin sensitivity to various stimuli, including cosmetics, sun exposure, wind, and hot or cold temperatures, is common. The skin barrier may be compromised, leading to heightened reactions.
- Rough or Uneven Skin Texture: The accumulation of mites and their waste products within follicles can lead to a coarse, irregular, or sandpaper-like texture of the skin. This altered texture is a subtle but significant **demodex face symptom**.
- Follicular Pustules/Perifollicular Redness: Close inspection may reveal small pustules directly emerging from hair follicles, surrounded by a halo of redness. This indicates active inflammation centered around the mite-infested follicle.
- Telangiectasias (Visible Blood Vessels): In chronic or severe cases, especially those resembling rosacea, fine, dilated blood vessels may become visible on the surface of the skin, particularly on the cheeks and nose. This is a sign of long-term inflammation and vascular changes.
- Blepharitis-like Symptoms: When Demodex mites infest the eyelashes, symptoms can include crusting around the eyelids, itching, irritation, eyelash loss (madarosis), and a gritty sensation in the eyes. This is known as Demodex blepharitis and often coexists with facial demodicosis.
- Increased Oiliness (Seborrhea): While some might experience dryness, others may notice an increase in facial oiliness due to irritation of the sebaceous glands where **Demodex brevis** often resides. This can contribute to a shiny appearance.
- Thickened Skin (Phymatous Changes): In very rare, chronic, and severe cases, typically untreated for extended periods, demodicosis can contribute to skin thickening, particularly around the nose (rhinophyma), resembling advanced rosacea. However, demodicosis is more often a trigger or exacerbating factor for rosacea rather than its sole cause.
Recognizing these diverse **Demodex skin manifestations** in context is crucial for healthcare professionals and individuals seeking diagnosis. The variability necessitates a careful clinical assessment, often supported by microscopic examination for definitive confirmation of **Demodex mites on face**. Early recognition of these **facial demodicosis symptoms** can prevent progression and improve treatment outcomes.
Signs of Demodicosis on the face Pictures
The objective **signs of Demodicosis on the face pictures** provide critical visual cues for clinicians and are often distinct from subjective symptoms reported by patients. These signs are what a healthcare provider directly observes during a physical examination and are paramount for making an accurate diagnosis of **facial demodex infestation**. The presentation can range from subtle alterations in skin texture and color to prominent inflammatory lesions, frequently overlapping with other dermatological conditions, particularly rosacea. Understanding these **visible demodex signs** helps differentiate demodicosis and guide targeted therapies.
Key **Demodex mite infestation signs** observed on the face include:
- Erythema, Persistent or Transient:
- Diffuse Redness: A widespread, often symmetrical redness affecting the central face—cheeks, nose, forehead, and chin. This erythema can be persistent or episodic, often worsening with heat, spicy foods, alcohol, or emotional stress. It is a hallmark **sign of demodex**.
- Perifollicular Erythema: Localized halos of redness around individual hair follicles, indicating inflammation specifically at the site of mite habitation. This can give the skin a subtly mottled or speckled reddish appearance.
- Papules:
- Moniform Papules: Small (1-3mm), firm, dome-shaped papules, typically red or pink. These are often discrete but can coalesce, giving a bumpy texture to the skin. Their uniform appearance can be a clue for **facial demodicosis**.
- Follicular Papules: Papules centered around hair follicles, often presenting as small, slightly raised bumps that may be skin-colored or erythematous. These are direct evidence of inflammation within the mite-infested follicle.
- Pustules:
- Sterile Pustules: Small, pus-filled lesions, often without an obvious bacterial component, indicating an inflammatory response to mites or their byproducts. They are frequently observed on the cheeks and forehead.
- Follicular Pustules: Pustules that clearly originate from a hair follicle opening, sometimes with a hair shaft visibly protruding from the center. This is a very specific **sign of demodex overgrowth**.
- Scaling and Roughness:
- Fine, Branny Scales: Delicate, powdery flakes of skin, particularly visible in the eyebrows, nasolabial folds, and along the hairline. This scaling is a result of disturbed epidermal turnover.
- Follicular Scales/Plugs: Small, horny plugs or scales within the follicular openings, sometimes referred to as ‘demodex dust’. These can be seen with magnification and are characteristic of severe infestations, especially of Demodex folliculorum.
- Rough, Sandpaper-like Texture: A generalized coarsening of the skin texture, particularly noticeable on palpation. This is due to chronic inflammation and follicular changes.
- Telangiectasias:
- Visible Blood Vessels: Fine, thread-like dilated capillaries that are apparent on the skin surface, typically on the cheeks and nose. While often associated with rosacea, they can also be exacerbated or induced by chronic inflammation from demodicosis.
- Edema (Swelling):
- Mild Facial Swelling: Subtle puffiness or swelling, particularly in acute flare-ups or in areas of intense inflammation. This is often accompanied by erythema and warmth.
- Demodex Frosting/Follicular Spicules: A unique sign, sometimes referred to as “demodex frost,” where tiny, pointed follicular projections or spicules are visible, especially when the skin is stretched. These are believed to be the hardened remnants of follicular contents or mite bodies and are pathognomonic for **demodicosis diagnosis**.
- Perioral Dermatitis-like Eruptions: A rash characterized by small papules and pustules, often with some scaling, specifically around the mouth. While a distinct condition, demodicosis can mimic or contribute to perioral lesions.
- Blepharitis and Ocular Signs:
- Collarettes: Cylindrical dandruff-like scales at the base of the eyelashes, a highly specific sign of Demodex blepharitis.
- Red, Itchy Eyelids: Inflammation and irritation of the eyelid margins.
- Eyelash Loss (Madarosis): Thinning or loss of eyelashes due to chronic follicular damage.
- Excoriations: Linear erosions or crusts caused by scratching due to intense pruritus. These are secondary signs but can be prominent if itching is severe.
The combination of these **signs of demodicosis** on the face, coupled with patient history, helps differentiate it from conditions like acne, perioral dermatitis, eczema, and seborrheic dermatitis. Definitive diagnosis often involves microscopy of skin scrapings or biopsy to confirm the presence and density of **Demodex mites**. Early recognition of these **visible demodicosis symptoms** is key to effective management.
Early Demodicosis on the face Photos
Recognizing **early Demodicosis on the face photos** is crucial because the initial signs of a **Demodex mite infestation** can be subtle and easily mistaken for other common skin issues such as mild acne, sensitive skin reactions, or even just general facial redness. These initial manifestations are often dismissed, leading to delayed diagnosis and potentially more advanced disease. Awareness of these nuanced **early demodex symptoms** empowers individuals and clinicians to seek and provide appropriate care sooner, preventing the progression to more severe inflammatory conditions.
The subtle nature of **initial demodicosis signs** makes them challenging to identify without a high index of suspicion. Here are detailed descriptions of what to look for in **early Demodicosis on the face photos**:
- Subtle, Intermittent Redness:
- Transient Flushing: One of the very first signs might be an increased tendency for the face to flush, especially after consuming hot beverages, spicy foods, alcohol, or in response to emotional stress or changes in temperature. This flushing might be more persistent than usual or occur more frequently.
- Mild, Patchy Erythema: Rather than widespread, diffuse redness, early demodicosis might present with small, ill-defined patches of pinkish or light red discoloration, often on the cheeks, nose, or forehead. This redness may not be constant and could fade and reappear.
- Fine, Barely Noticeable Scaling:
- Micro-scaling: Very fine, dust-like or powdery scales that are only visible upon close inspection, perhaps under magnification or when the skin is dry. These scales can be found in the eyebrows, nasolabial folds, or on the central forehead. They may be so subtle that they are perceived as mild dryness rather than a skin condition.
- Slightly Rough Texture: The skin might feel subtly rough or gritty to the touch, almost like very fine sandpaper. This is often felt before it is seen and indicates early follicular involvement.
- Mild Itching or Tingling:
- Occasional Pruritus: A mild, intermittent itch, often described as an annoying tickle or crawl. This itching may be worse at night, though not necessarily severe enough to disrupt sleep. It might be localized to specific areas rather than generalized across the face.
- Tingling or Prickling Sensation: Some individuals report a slight tingling, prickling, or stinging sensation, particularly after applying products or when exposed to environmental triggers. This indicates heightened skin sensitivity.
- Subtle Changes in Skin Texture/Pore Appearance:
- Slightly Enlarged Pores: Pores may appear subtly more prominent or somewhat clogged, especially on the nose and cheeks. This is due to the mites residing within the follicles and potentially causing minor obstruction or inflammation.
- Dullness or Lack of Radiance: The skin might lose some of its natural luminosity, appearing a bit dull or lacklustre. This can be attributed to microscopic inflammation and surface irregularities.
- Isolated or Very Sparse Papules:
- Occasional Small Bumps: Infrequent, tiny, flesh-colored or slightly reddish bumps that are often mistaken for singular acne breakouts or clogged pores. These papules are usually non-inflamed and do not typically contain pus in the very early stages. They tend to be isolated rather than clustered.
- Increased Skin Reactivity:
- Sensitivity to Products: Previously well-tolerated skincare products, makeup, or sunscreens might start causing mild irritation, redness, or a stinging sensation. This points to a compromised skin barrier and increased underlying inflammation.
- Environmental Sensitivity: The skin may become more reactive to elements like wind, cold, sun exposure, or humidity, leading to increased discomfort or redness.
- Minor Eyelid Symptoms:
- Mild Eyelash Itching: A very subtle itchiness along the eyelash line, especially in the mornings. This can be an early sign of Demodex blepharitis co-occurring with facial demodicosis.
- Few Flakes on Eyelashes: Tiny, almost invisible flakes at the base of the eyelashes, sometimes only noticeable when applying mascara or during close inspection.
- Feeling of “Unclean” Skin:
- Some individuals describe a persistent feeling that their skin isn’t quite clean, even after washing, or that it feels “off.” This subjective sensation can sometimes precede more overt visual signs.
- Rosacea-like Demodicosis Rash:
- Erythematotelangiectatic Rosacea-like: This is perhaps the most common presentation. The rash is characterized by persistent central facial erythema, affecting the cheeks, nose, forehead, and chin. It may be accompanied by visible blood vessels (telangiectasias). Unlike typical rosacea, the redness in demodicosis can sometimes be more diffuse and less prone to episodic flushing, though flushing can still occur. The skin may also feel persistently warm.
- Papulopustular Rosacea-like: This form involves numerous small, red papules and pustules scattered across the erythematous areas of the face. These lesions typically lack comedones (blackheads/whiteheads), which helps differentiate them from acne vulgaris. The papules are often monomorphic, meaning they are similar in size and appearance, and can be relatively uniform.
- Granulomatous Demodicosis: A rarer and more severe form that can resemble granulomatous rosacea. It presents with firm, reddish-brown to yellowish-brown papules or nodules, often with a granulomatous inflammation pattern on histology. These lesions are typically more persistent and can be challenging to treat.
- Papular and Pustular Demodicosis Rash:
- Erythematous Papules: Numerous small (1-4mm), red, firm bumps that are often centered around hair follicles. These papules can be widespread across the face or localized to specific areas like the perioral or perinasal regions. They typically do not have a follicular opening with a visible sebaceous plug.
- Follicular Pustules: Small, pus-filled lesions that arise directly from the hair follicles. These are often sterile (non-bacterial) and represent an inflammatory reaction to the mites or their associated bacterial flora. They can be tender and contribute significantly to facial discomfort.
- Acneiform Eruptions: The rash can closely mimic acne, with scattered papules and pustules. However, the key differentiating factor is the general absence of true comedones (blackheads and whiteheads) in demodicosis. If comedones are present, demodicosis might be an exacerbating factor for pre-existing acne.
- Perioral and Perinasal Demodicosis Rash:
- Perioral Dermatitis-like: Small, erythematous papules and pustules concentrated around the mouth (perioral), sometimes sparing a narrow rim around the lips. This presentation often includes some fine scaling and can extend to the nasolabial folds and around the nose (perinasal). This is a common location for **facial demodex rash**.
- Periorbital Involvement: In some cases, the rash can extend to the areas around the eyes, though typically not on the eyelids themselves unless Demodex blepharitis is also present.
- Eczema-like/Dermatitis-like Demodicosis Rash:
- Scaling and Dryness: A rash characterized by prominent scaling, flaking, and dry patches, often accompanied by underlying erythema. This can be mistaken for seborrheic dermatitis, especially when affecting the eyebrows, nasolabial folds, and forehead. The skin may feel rough and irritated.
- Diffuse Erythema with Exfoliation: Widespread redness with generalized fine peeling or exfoliation, giving the skin a dull or damaged appearance. This form often correlates with a high density of mites.
- Hyperpigmented Demodicosis:
- In individuals with darker skin tones, inflammation from demodicosis can sometimes lead to post-inflammatory hyperpigmentation (PIH), manifesting as darker spots or patches after papules or pustules resolve. This can be a significant cosmetic concern.
- Demodex Frosting / Spicule Formation:
- A unique visual sign where tiny, often invisible to the naked eye, follicular projections or “spicules” can be seen upon stretching the skin. These are often described as ‘demodex frost’ and are indicative of high mite density within the follicles. This specific **demodicosis rash appearance** is highly suggestive of the condition.
- Ivermectin Cream (1%):
- Mechanism: A potent antiparasitic agent that is highly effective against Demodex mites. It also possesses anti-inflammatory properties, which help reduce redness and papules.
- Application: Typically applied once daily to affected facial areas.
- Benefits: Often very effective, well-tolerated, and can lead to significant reduction in mite counts and improvement in clinical symptoms. It’s often considered a cornerstone of **demodicosis therapy**.
- Keywords: **ivermectin for demodex**, **topical ivermectin demodicosis**, **demodex cream treatment**.
- Metronidazole Cream/Gel (0.75% or 1%):
- Mechanism: Primarily an anti-inflammatory agent, it helps reduce erythema and inflammatory papules/pustules. It may have some mild activity against Demodex, but its main role is symptom control.
- Application: Usually applied once or twice daily.
- Benefits: Effective for reducing inflammation and rosacea-like symptoms. Often used in combination with other anti-mite agents.
- Keywords: **metronidazole demodicosis**, **topical metronidazole for demodex**, **facial demodicosis anti-inflammatory**.
- Permethrin Cream (5%):
- Mechanism: A synthetic pyrethroid with strong acaricidal (mite-killing) properties.
- Application: Often used as an off-label treatment, applied to the face overnight, usually once or twice a week, or as directed by a physician. Care must be taken around sensitive areas like the eyes.
- Benefits: Highly effective at killing mites.
- Keywords: **permethrin demodicosis treatment**, **kill demodex mites**, **acaricidal cream**.
- Crotamiton Cream (10%):
- Mechanism: Has both scabicidal and antipruritic (anti-itch) properties.
- Application: Applied to affected areas, usually twice daily.
- Benefits: Can be useful for relieving itching associated with demodicosis.
- Keywords: **crotamiton for demodex itch**, **demodex itch relief**.
- Sulfur Preparations (e.g., 5-10% Sulfur Ointment/Wash):
- Mechanism: Possesses both acaricidal and keratolytic properties, helping to kill mites and exfoliate the skin. Also has anti-inflammatory effects.
- Application: Available in washes, soaps, and ointments. Applied daily or as directed.
- Benefits: An older but still effective **demodex treatment** option, especially for milder cases or as an adjunct. Can be drying or irritating for some.
- Keywords: **sulfur demodicosis**, **sulfur wash for demodex**, **natural demodex treatment**.
- Azelaic Acid Gel/Cream (15% or 20%):
- Mechanism: Has anti-inflammatory, antimicrobial, and mild keratolytic effects. While not directly acaricidal, it significantly reduces the inflammatory component of demodicosis.
- Application: Applied twice daily.
- Benefits: Very effective for reducing redness, papules, and pustules, and generally well-tolerated.
- Keywords: **azelaic acid demodicosis**, **rosacea demodicosis treatment**.
- Benzyl Benzoate Lotion/Emulsion (10-25%):
- Mechanism: A potent acaricide.
- Application: Used off-label, often applied for a few days, then discontinued. Can be irritating.
- Benefits: Strong mite-killing action.
- Keywords: **benzyl benzoate demodex**, **strong demodex treatment**.
- Oral Ivermectin:
- Mechanism: Systemic antiparasitic agent that reaches the mites via the bloodstream. Highly effective at rapidly reducing mite populations.
- Dosage: Typically given as a single dose (e.g., 200 µg/kg), repeated after 7-14 days.
- Benefits: Rapid onset of action, can clear lesions quickly, especially in more resistant or severe cases. Essential for **managing Demodex mites** when topicals fail.
- Keywords: **oral ivermectin demodicosis**, **systemic demodex treatment**, **severe facial demodex**.
- Oral Metronidazole:
- Mechanism: Systemic anti-inflammatory and antibiotic properties.
- Dosage: Various regimens, often for several weeks.
- Benefits: Useful for significant inflammatory papules and pustules.
- Keywords: **oral metronidazole demodex**, **inflammatory demodicosis**.
- Oral Tetracyclines (e.g., Doxycycline, Minocycline):
- Mechanism: At sub-antimicrobial doses (e.g., low-dose doxycycline), these medications exert potent anti-inflammatory effects, primarily by inhibiting metalloproteinases, which are involved in inflammation and tissue breakdown in rosacea and demodicosis.
- Dosage: Low doses (e.g., 20mg doxycycline twice daily) for several weeks to months.
- Benefits: Excellent for reducing redness, papules, and pustules, especially when the condition mimics rosacea.
- Keywords: **doxycycline demodicosis**, **tetracycline for demodex**, **anti-inflammatory oral treatment**.
- Gentle Skincare Routine:
- Use mild, non-foaming cleansers to avoid irritating compromised skin.
- Avoid harsh scrubbing, abrasive exfoliants, and alcohol-based toners.
- Keywords: **demodicosis skincare**, **gentle facial cleanser demodex**.
- Moisturizers:
- Use non-comedogenic, fragrance-free moisturizers to support the skin barrier, especially with drying treatments.
- Keywords: **demodex moisturizer**, **skin barrier repair demodex**.
- Sun Protection:
- Daily use of broad-spectrum sunscreen (SPF 30+) is crucial, as UV exposure can exacerbate inflammation and rosacea-like symptoms.
- Keywords: **sunscreen demodex**, **demodex sun protection**.
- Avoidance of Triggers:
- Identify and avoid personal triggers that worsen redness or flushing, such as spicy foods, alcohol, hot beverages, and extreme temperatures.
- Keywords: **demodex triggers**, **avoid rosacea triggers**.
- Eyelid Hygiene (for Demodex Blepharitis):
- If ocular demodicosis is present, daily eyelid hygiene using specific lid scrubs (e.g., tea tree oil-based) or warm compresses is essential.
- Keywords: **demodex blepharitis treatment**, **eyelid hygiene demodex**.
- Tea Tree Oil (TTO) Products:
- Mechanism: TTO has demonstrated acaricidal properties against Demodex mites. It is often used in diluted forms in cleansers, wipes, or as an ingredient in professional treatments.
- Caution: Concentrated TTO can be highly irritating. Use only diluted products formulated for facial use, or under professional guidance.
- Keywords: **tea tree oil for demodex**, **natural demodex remedy**.
- Regular follow-up with a dermatologist is important to monitor treatment efficacy, adjust medications, and manage potential side effects.
- Maintenance therapy, often with topical ivermectin or metronidazole, may be necessary to prevent recurrence, as Demodex mites are a natural inhabitant of human skin and complete eradication is not the goal, but rather population control.
- Keywords: **demodicosis recurrence prevention**, **demodex long-term management**.
These **subtle facial demodicosis** indicators are often overlooked, as they don’t always cause significant distress or prompt a visit to a dermatologist. However, being attuned to these early changes can lead to earlier diagnosis of **Demodex overgrowth** and prevent the development of a more pronounced **demodicosis skin rash**. When multiple of these mild symptoms persist or worsen over time, it warrants consideration of demodicosis as a potential underlying cause.
Skin rash Demodicosis on the face Images
The **skin rash Demodicosis on the face images** often reveal a highly polymorphic presentation, making it one of the “great imitators” in dermatology. The rash can vary significantly in appearance, from widespread erythema with fine scaling to prominent papules and pustules resembling acne or rosacea. Understanding the different forms of **demodicosis rash pictures** is essential for accurate clinical diagnosis and effective treatment planning. The specific morphology of the rash is influenced by the density of the Demodex mite infestation, the individual’s immune response, and the predominant mite species (Demodex folliculorum typically causes follicular irritation, while Demodex brevis is linked to sebaceous gland issues).
Here are detailed descriptions of common **Demodex facial rash** types:
The morphology and distribution of these **demodicosis rash on face** presentations can vary greatly among individuals. A thorough clinical examination, often combined with a microscopic examination of skin scrapings to identify Demodex mites, is critical for definitive diagnosis. Ignoring these **Demodex rash symptoms** can lead to chronic skin inflammation and progression of the condition.
Demodicosis on the face Treatment
Effective **Demodicosis on the face treatment** strategies aim to reduce the population of Demodex mites, control inflammation, alleviate symptoms, and prevent recurrence. Given the chronic nature of Demodex infestations and their frequent association with rosacea-like symptoms, a multifaceted approach combining topical and sometimes oral medications is often necessary. The choice of treatment depends on the severity of the **facial demodicosis**, the specific symptoms, and individual patient factors. It is crucial to emphasize that self-diagnosis and self-treatment can be ineffective or even harmful; a definitive diagnosis by a healthcare professional is paramount before initiating any **demodex treatment options**.
Here are comprehensive **treatment options for facial demodex**:
1. Topical Medications (First-Line Treatment):
2. Oral Medications (For more severe or widespread cases, or when topical treatments are insufficient):
3. Adjunctive Therapies and Skincare Practices:
4. Follow-up and Maintenance:
Successful **treatment of Demodicosis on the face** requires a consistent approach and patience, as improvements may take several weeks to months. A definitive diagnosis through microscopic examination is key to selecting the most appropriate and effective **Demodex mite treatment**. Understanding the underlying causes and available therapies is crucial for effective **demodicosis management** and improving patient quality of life.