This article provides a visual guide and detailed descriptions of herpes symptoms on various parts of the body. Understanding the diverse manifestations of herpes on the body symptoms pictures is crucial for early identification and management, helping individuals distinguish viral eruptions from other skin conditions. We delve into the characteristic appearance of lesions, their progression, and associated signs to aid in recognition.
Herpes on the body Symptoms Pictures
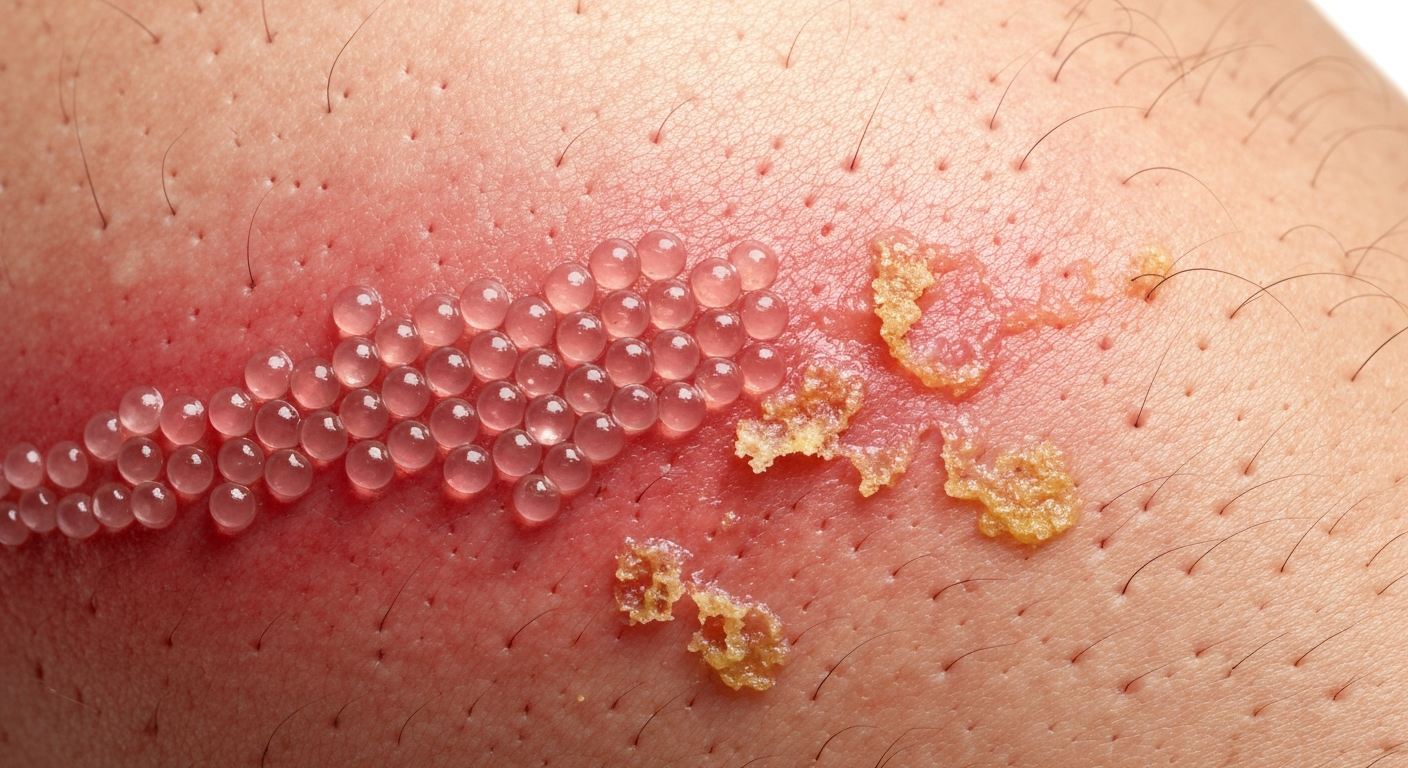
Recognizing the visual cues of herpes on the body is paramount for proper diagnosis. The characteristic lesions typically begin as small, red bumps that quickly evolve into fluid-filled blisters. These herpes symptoms are often grouped in clusters on an erythematous (reddened) base, presenting a distinct appearance that differentiates them from solitary pimples or insect bites. As the infection progresses, these vesicles may rupture, weep fluid, and then form crusts before healing. The locations can vary widely, affecting the trunk, limbs, buttocks, back, or even less common areas, making a comprehensive understanding of body herpes lesions essential for identification.
The progression of herpes on the body symptoms follows a predictable pattern, although the duration and intensity can differ based on the individual’s immune status and whether it’s a primary infection or a recurrence. Visual identification focuses on the morphology of the lesions and their distribution. Understanding these stages through typical herpes outbreaks pictures can significantly aid in self-assessment before medical consultation. It’s crucial to look for the classic presentation of grouped vesicles, which is a hallmark of the herpes simplex virus or varicella-zoster virus reactivation.
Detailed visual characteristics of herpes on the body skin lesions include:
- Erythematous Base: The area beneath and immediately surrounding the blisters appears reddened and inflamed, indicative of an active infection. This redness can be tender to the touch and often precedes the actual blister formation.
- Clustered Vesicles: Perhaps the most definitive visual sign, herpes lesions typically appear as multiple small blisters, often ranging from 1-3 mm in diameter, tightly packed together. These clusters can merge to form larger, irregular plaques of blistering.
- Fluid-Filled Blisters: Initially, these vesicles contain clear, serous fluid. Over time, particularly if they become infected or as the body’s immune response progresses, the fluid may appear cloudy or yellowish (pustular).
- Blister Rupture and Ulceration: The fragile blisters often rupture spontaneously or through friction, leaving behind shallow, painful open sores or ulcers. These ulcers are typically round or oval with a reddish base.
- Crusting and Scabbing: Following rupture, the ulcers begin to dry and form yellowish or brownish crusts (scabs). This stage signifies the beginning of the healing process, and the scabs eventually fall off, often without leaving scars unless the lesions were picked or severely infected.
- Post-inflammatory Pigmentation: After healing, the affected skin may temporarily appear darker (hyperpigmentation) or lighter (hypopigmentation) than the surrounding skin, which usually fades over time.
- Unilateral Distribution (for Zoster): In cases of herpes zoster (shingles), a common form of herpes on the body, the rash typically follows a dermatomal pattern, meaning it appears on one side of the body along the path of a single nerve. This unilateral band-like distribution is highly characteristic.
Signs of Herpes on the body Pictures
Beyond the visible rash, several other signs of herpes on the body can manifest, often preceding or accompanying the skin lesions. These prodromal symptoms are critical indicators that an outbreak is imminent or active, and recognizing them can prompt earlier intervention. Individuals frequently report localized sensations such as tingling, itching, burning, or even sharp pain in the area where the rash subsequently appears. These neurological symptoms are due to the virus traveling along nerve pathways to the skin surface. Understanding these sensory herpes outbreak signs is crucial for individuals who experience recurrent episodes of body herpes, as it allows for proactive management strategies.
The constellation of symptoms associated with herpes on the body can also include systemic manifestations, particularly during a primary infection or in immunocompromised individuals. These general signs underscore the body’s broader response to the viral activity. Early recognition of these varied herpes symptoms pictures, encompassing both skin changes and general discomfort, empowers individuals to seek timely medical advice. Paying attention to these subtle yet significant precursors can aid in better managing the condition and potentially reducing the severity and duration of the outbreak.
Key signs of herpes on the body to look for include:
- Prodromal Symptoms:
- Tingling Sensation: A ‘pins and needles’ feeling, or a slight buzzing, often described as paresthesia, in the area where lesions will emerge. This can occur hours to days before the visible rash.
- Itching: Intense, localized itching that cannot be attributed to dryness or other common skin irritations. This is one of the earliest and most common sensory indicators.
- Burning Sensation: A sensation of heat or burning in the affected skin region, sometimes accompanied by tenderness to touch.
- Pain or Hypersensitivity: Localized pain, ranging from mild discomfort to sharp, shooting pains, can be experienced. The skin may also become unusually sensitive to light touch or temperature changes.
- Localized Skin Changes Prior to Vesicles:
- Redness (Erythema): A patch of skin may become noticeably redder than the surrounding area, often signaling the inflammatory process has begun.
- Swelling: Slight localized swelling or puffiness may be observed, making the skin feel taut or raised.
- Warmth: The affected skin area might feel warmer to the touch compared to adjacent skin.
- Systemic Symptoms (More common in primary infections or extensive outbreaks):
- Fever: An elevated body temperature, particularly in conjunction with other symptoms, can indicate a systemic viral response.
- Body Aches and Pains: Generalized muscle aches or joint pain, similar to flu-like symptoms.
- Headache: A common systemic symptom, often accompanying fever.
- Fatigue: A feeling of extreme tiredness or lack of energy.
- Swollen Lymph Nodes: Lymph nodes near the affected area (e.g., in the armpit if the rash is on the arm or chest, or groin if on the leg/buttock) may become enlarged, tender, and palpable as the immune system responds to the infection.
- Gastrointestinal Upset: Nausea or general malaise, though less common, can also be present.
- Neurological Symptoms (Especially with Herpes Zoster):
- Neuralgia: Persistent or severe nerve pain (postherpetic neuralgia) can occur during or after the rash, especially with shingles, and can last for weeks, months, or even years after the visible lesions have healed.
- Increased Skin Sensitivity: The affected dermatome can remain hypersensitive to touch, temperature, and even air currents.
Early Herpes on the body Photos
Identifying early herpes on the body photos is crucial for timely diagnosis and management, as treatment is most effective when initiated during the nascent stages of an outbreak. The very first visible manifestation of herpes on the body typically begins with an area of localized redness. Within hours to a couple of days, small, raised red bumps, known as papules, start to form within this reddened area. These papules quickly progress into characteristic small, clear, fluid-filled vesicles (blisters) that are often tightly grouped together. This rapid evolution from redness to papules to clustered vesicles is a hallmark of early herpes outbreaks, providing a distinct visual signature for those seeking to understand first signs of herpes.
The initial appearance of these lesions can sometimes be mistaken for insect bites, folliculitis, or allergic reactions, highlighting the importance of recognizing the specific pattern and progression characteristic of herpes on the body. Unlike many other skin conditions, herpes blisters tend to be uniform in size within a cluster and are situated on a visibly inflamed base. Paying close attention to the development sequence and the localized symptoms like tingling or burning that often precede the rash can further confirm the suspicion of an early herpes infection. Prompt recognition allows for the initiation of antiviral therapy, which can significantly reduce the severity, duration, and pain associated with the outbreak.
Detailed characteristics for identifying early herpes on the body photos:
- Initial Redness (Erythema):
- Appears as a localized patch of inflamed, red skin.
- Often precedes any visible bumps or blisters by several hours to a day.
- May be accompanied by itching, tingling, or burning sensations.
- Formation of Papules:
- Small, solid, raised red bumps develop within the erythematous area.
- These are typically 1-2 mm in diameter and can feel slightly firm to the touch.
- Often appear in a cluster or linearly, indicating the underlying nerve path involvement.
- Development of Vesicles (Small Blisters):
- Papules rapidly transform into small, clear, fluid-filled blisters.
- These vesicles are often uniform in size (typically 1-3 mm) and appear in tightly packed clusters on the red base.
- The fluid inside is initially clear and serous, giving the blisters a shiny or translucent appearance.
- This clustered, vesicular appearance is highly diagnostic of early herpes lesions.
- Location and Distribution:
- Can appear on any part of the body (trunk, limbs, buttocks, face, scalp).
- Often localized to a specific area, especially in recurrent outbreaks.
- For herpes zoster (shingles), the early lesions will appear along a single dermatome (nerve path) on one side of the body, creating a band-like pattern.
- Accompanying Symptoms:
- Localized pain, tenderness, or increased sensitivity to touch in the affected area.
- Persistent itching or burning, even before the blisters are fully formed.
- Mild swelling around the developing cluster of lesions.
- Distinguishing from Other Conditions:
- Unlike insect bites, herpes lesions are typically multiple, clustered, and develop systematically from papules to vesicles on a red base.
- Unlike folliculitis, which involves hair follicles, herpes lesions are usually superficial and not necessarily centered around a hair.
- Unlike allergic reactions, herpes lesions are rarely migratory or widespread initially and follow a specific viral progression.
Skin rash Herpes on the body Images
The skin rash of herpes on the body presents with highly characteristic features that are often visually diagnostic. This rash is predominantly recognized by its signature appearance of clustered vesicles on an erythematous base. As observed in typical herpes rash images, these fluid-filled blisters are tightly grouped and localized to a specific area of the skin, reflecting the viral activity along nerve pathways. The fluid within the vesicles is initially clear, but it can become cloudy or purulent over time before the blisters eventually rupture. Understanding the morphology and evolution of these herpes skin lesions is paramount for distinguishing them from other dermatological conditions and confirming a diagnosis of body herpes rash.
The progression of the herpes rash involves several stages, all of which contribute to its distinctive visual profile. After the initial vesicular stage, the blisters break open, leaving behind shallow, often painful, erosions or ulcers. These open sores then begin to dry and form yellow-brown crusts or scabs, a clear indicator that the healing process has commenced. The complete cycle from initial redness to scab formation and eventual healing typically takes 7 to 14 days, though it can be longer in severe cases or in immunocompromised individuals. Observing these different stages of herpes rash pictures provides a comprehensive view of how the infection manifests on the skin.
Detailed visual characteristics of the skin rash herpes on the body:
- Erythematous Macules and Papules:
- The rash often begins as red, flat spots (macules) that quickly become raised, red bumps (papules). These appear on a reddened background, indicating inflammation.
- They are typically the initial visible signs after the prodromal symptoms.
- Vesicular Eruption:
- The hallmark of the herpes rash is the rapid development of small (1-5 mm), clear, fluid-filled blisters (vesicles) from the papules.
- These vesicles are almost always grouped in tight clusters, giving a “dewdrop on a rose petal” appearance when they are clear on a red base.
- The fluid may become cloudy (seropurulent) or yellowish over several days, indicating white blood cell presence or secondary infection.
- Ulceration and Erosion:
- The fragile vesicles rupture easily, either spontaneously or due to friction, leading to shallow, painful open sores called ulcers or erosions.
- These ulcers typically have a reddish base and may weep clear or yellowish fluid.
- They are a significant source of pain and are highly contagious.
- Crusting and Scabbing:
- As the ulcers heal, they begin to dry out and form thick, yellowish or brownish crusts (scabs).
- These scabs protect the underlying healing skin and are a sign that the lesion is no longer highly infectious, though caution is still advised.
- The scabs eventually fall off, usually without scarring, unless the lesions were particularly deep, infected, or picked.
- Distribution Patterns:
- Localized Clusters: Most common, affecting a small, defined area of the body.
- Dermatomal (Herpes Zoster/Shingles): The rash follows the path of a single nerve, appearing as a band-like stripe on one side of the body. This pattern is highly specific to varicella-zoster virus reactivation.
- Widespread or Disseminated: Less common, typically seen in immunocompromised individuals, where the rash can spread over larger areas or even be generalized. This requires urgent medical attention.
- Color Changes:
- Initial redness, followed by clear vesicles, then potentially cloudy fluid, leading to yellowish/brownish scabs.
- Post-inflammatory hyperpigmentation (darkening) or hypopigmentation (lightening) can occur after healing, which usually fades over time.
- Associated Symptoms with the Rash:
- Persistent itching, burning, and pain in the rash area.
- Tenderness to touch, sometimes severe, especially in nerve-rich areas.
- Swelling around the clustered lesions.
- Systemic symptoms like fever, fatigue, or swollen lymph nodes can accompany the rash, especially during primary outbreaks.
Herpes on the body Treatment
Effective herpes on the body treatment primarily focuses on antiviral medications, which work by inhibiting viral replication, thereby reducing the severity and duration of outbreaks, and in some cases, preventing recurrence. Early initiation of treatment is critical, ideally within 24-72 hours of the first symptoms or rash appearance, for optimal effectiveness. These antiviral agents can significantly alleviate pain, shorten the healing time of lesions, and decrease the risk of transmission. Beyond prescription medications, various supportive care measures and lifestyle adjustments play a crucial role in managing herpes outbreaks on the body, providing comprehensive relief and improving quality of life for individuals dealing with recurrent herpes symptoms.
Management strategies for body herpes also involve symptomatic relief and preventive measures to minimize future outbreaks and protect others. Understanding the available treatment options, including both acute therapy for active outbreaks and suppressive therapy for frequent recurrences, empowers individuals to actively participate in their care. Consulting a healthcare professional for an accurate diagnosis and a personalized treatment plan is essential, as the approach may vary depending on the type of herpes virus, the location of the lesions, the frequency of outbreaks, and the individual’s overall health status. Adherence to prescribed treatments and incorporating self-care practices can profoundly impact the course and impact of herpes on the body.
Comprehensive herpes on the body treatment approaches include:
- Antiviral Medications (Prescription):
- Acyclovir (Zovirax): One of the oldest and most commonly prescribed antivirals. It is highly effective in reducing the duration and severity of herpes outbreaks. Dosing varies for initial outbreaks, recurrent episodes, and suppressive therapy.
- Valacyclovir (Valtrex): A prodrug of acyclovir, meaning it’s converted to acyclovir in the body. It has improved bioavailability, allowing for less frequent dosing and greater convenience for patients. Often preferred for its ease of use.
- Famciclovir (Famvir): Another antiviral with good efficacy, particularly known for its effectiveness in treating herpes zoster (shingles), reducing pain and the risk of postherpetic neuralgia.
- Mechanism: These drugs work by interfering with the virus’s ability to replicate its DNA, effectively slowing down the viral infection and allowing the immune system to gain control.
- Usage: Can be used for episodic treatment (at the first sign of an outbreak) or for suppressive therapy (daily dose to prevent outbreaks).
- Pain Management:
- Over-the-Counter Pain Relievers: Non-steroidal anti-inflammatory drugs (NSAIDs) like ibuprofen or naproxen, and acetaminophen (Tylenol), can help manage pain and fever associated with outbreaks.
- Topical Anesthetics: Creams or ointments containing lidocaine or benzocaine can provide localized pain relief by numbing the affected area.
- Prescription Pain Medications: For severe pain, especially in cases of extensive herpes zoster or postherpetic neuralgia, stronger prescription pain relievers may be necessary.
- Neuropathic Pain Medications: Gabapentin or pregabalin may be prescribed for persistent nerve pain, particularly after shingles.
- Topical Treatments (Symptomatic Relief):
- Cool Compresses: Applying a clean, cool, damp cloth to the lesions can help soothe discomfort, reduce itching, and dry out blisters.
- Petroleum Jelly: Can be applied to lesions after they’ve crusted to keep them moist and prevent cracking, potentially aiding healing and reducing scarring.
- Zinc Oxide Cream: May help to dry out lesions and promote healing.
- Calamine Lotion: Can provide relief from itching and irritation.
- Preventive Measures and Lifestyle Adjustments:
- Stress Reduction: Stress is a known trigger for herpes outbreaks. Techniques such as meditation, yoga, mindfulness, and adequate sleep can help.
- Immune System Support: A healthy diet rich in vitamins and minerals, regular exercise, and avoiding smoking and excessive alcohol can bolster the immune system.
- Avoid Triggers: Identifying and avoiding personal triggers (e.g., sun exposure, specific foods, illness) can help reduce the frequency of recurrences. Sunscreens can be beneficial for those whose outbreaks are triggered by UV light.
- Good Hygiene: Keeping the affected area clean and dry can prevent secondary bacterial infections. Washing hands thoroughly after touching lesions is crucial to prevent spread to other body parts or individuals.
- Avoid Touching/Picking Lesions: This can delay healing, increase the risk of scarring, and spread the virus.
- Vaccination (for Shingles): The herpes zoster vaccine (Shingrix) is highly recommended for adults aged 50 and older to prevent shingles and its complications, such as postherpetic neuralgia.
- Management of Complications:
- Secondary Bacterial Infections: If lesions become infected with bacteria, antibiotics (oral or topical) may be prescribed.
- Eye Involvement: If herpes lesions occur near the eyes, prompt ophthalmological evaluation is crucial to prevent serious complications like herpes keratitis, which can lead to vision loss.
- Disseminated Herpes: For widespread or systemic infections, especially in immunocompromised patients, intravenous antiviral therapy and hospitalization may be necessary.