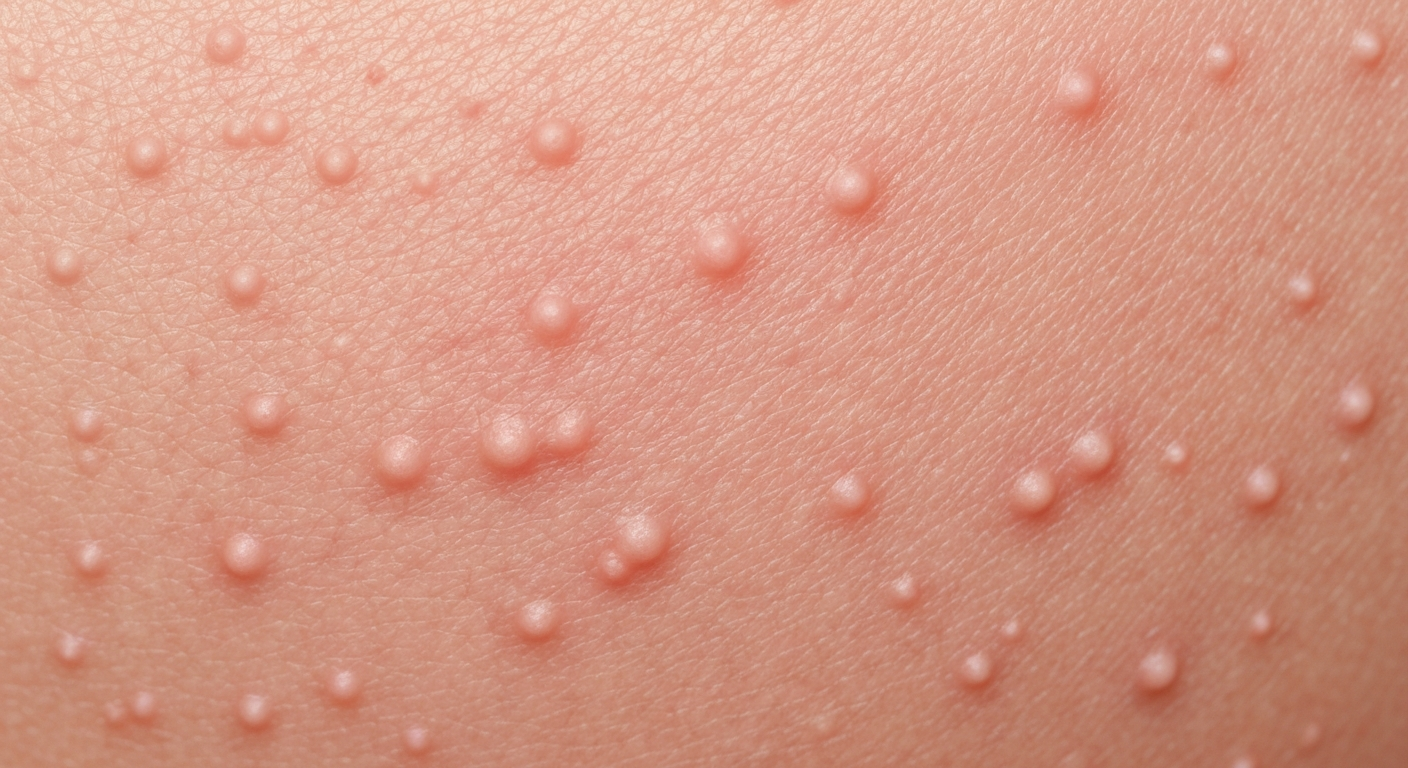
Understanding what does Folliculitis look like symptoms pictures is crucial for timely identification and effective management of this common inflammatory skin condition. This detailed guide provides comprehensive visual descriptions and symptom breakdowns to help individuals recognize the diverse presentations of follicular inflammation across various body parts and types.
Folliculitis Symptoms Pictures
When examining Folliculitis symptoms pictures, one immediately notices the characteristic appearance of inflamed hair follicles. The primary visual markers are small, red bumps or pus-filled pimples that are distinctly centered around a hair shaft. These lesions can manifest in various forms, ranging from superficial pustules to deep, painful nodules, often affecting areas rich in hair follicles such as the scalp, face, neck, back, chest, buttocks, and legs. The inflammatory process around the hair follicle is key to its visual identification. The coloration of the lesions is typically erythematous, meaning red, and this redness can vary in intensity depending on the degree of inflammation and the patient’s skin tone, appearing brighter red on lighter skin and more purplish or dark red on darker complexions. Many individuals report significant discomfort associated with these visual symptoms.
Detailed examination of folliculitis visual symptoms often reveals an array of characteristics:
- Erythematous Papules: These are small, solid, red bumps, typically less than 5 millimeters in diameter. Each papule is visibly associated with a hair follicle, sometimes with a tiny hair shaft penetrating its center. The redness signifies inflammation, and these papules can be tender to the touch or itch intensely. They are often the earliest visible sign of folliculitis before pus formation.
- Pustules: These are definitive hallmarks of many forms of folliculitis. Pustules are small, raised lesions filled with white or yellowish pus. Similar to papules, they are consistently centered on a hair follicle. The pus indicates an accumulation of white blood cells fighting an infection, which can be bacterial, fungal, or sometimes sterile inflammation. These pustules may spontaneously rupture, leading to crust formation.
- Pruritus (Itching): While not a direct visual symptom in folliculitis images symptoms, itching is a pervasive complaint that often leads to secondary visual signs like excoriations (scratch marks), skin thickening (lichenification) from chronic rubbing, or post-inflammatory hyperpigmentation. The intensity of itching can vary significantly based on the type of folliculitis, with fungal folliculitis (e.g., Pityrosporum folliculitis) often being notoriously itchy.
- Pain and Tenderness: Deeper forms of folliculitis, such as boils (furuncles) or carbuncles, are usually accompanied by significant pain and tenderness to touch. Even superficial folliculitis can cause mild discomfort, especially when the affected area is pressed or rubbed. The pain often correlates with the size and depth of the inflammatory lesion.
- Crusting: After pustules rupture or lesions dry, a yellowish or brownish crust can form over the affected follicle. This crust is composed of dried serum, pus, and cellular debris. The presence of crusting often indicates a bacterial component or a lesion that has been traumatized, such as by scratching.
- Swelling and Edema: The skin surrounding the inflamed follicles may appear slightly swollen or edematous. This localized swelling contributes to the overall redness and tenderness of the affected area, making the lesions stand out more prominently against the unaffected skin.
- Hair Involvement: A critical diagnostic feature is the involvement of the hair follicle itself. In many cases, a hair can be seen emerging from the center of the papule or pustule, or the hair may appear entrapped or ingrown beneath the skin surface, especially in conditions like pseudofolliculitis barbae. When the hair follicle is severely damaged, temporary or permanent hair loss (alopecia) can occur in the affected patch.
- Post-inflammatory Changes: After the active lesions resolve, they can leave behind darker spots (post-inflammatory hyperpigmentation) or lighter spots (post-inflammatory hypopigmentation), particularly on individuals with darker skin tones. Scarring can also occur, especially with deep or recurrent infections.
The distribution of folliculitis lesions is also an important visual clue. Folliculitis on the scalp often presents as small, itchy, sometimes painful bumps that can be mistaken for acne. Beard folliculitis (sycosis barbae) typically affects men’s beard area, manifesting as persistent, inflamed pustules and papules. Folliculitis on the back and chest can be widespread, resembling an acne breakout, but closer inspection reveals the follicular centering. Buttock folliculitis often appears as red, tender bumps, sometimes mistaken for pimples, usually caused by friction or pressure. Leg folliculitis is common, especially after shaving or waxing, presenting as red, sometimes pus-filled bumps along the hair growth pattern.
Specific types of folliculitis have unique visual characteristics:
- Bacterial Folliculitis: Most commonly caused by Staphylococcus aureus. Visually, these are classic red papules and pustules, often with a yellow purulent center. They can be tender and sometimes itchy. Severe cases can lead to boils (furuncles), which are deeper, painful, pus-filled lumps, and carbuncles (clusters of boils).
- Pityrosporum Folliculitis (Malassezia Folliculitis): Caused by yeast (Malassezia species). Characterized by monomorphic (uniform in size and shape) itchy red papules and pustules, predominantly on the upper back, chest, and sometimes the shoulders or face. The itch is often disproportionately intense compared to the size of the lesions. These fungal folliculitis photos rarely show large pus-filled lesions but rather numerous small, uniform bumps.
- Pseudomonas Folliculitis (Hot Tub Folliculitis): Caused by Pseudomonas aeruginosa, usually acquired from contaminated hot tubs or swimming pools. The rash appears 1-2 days after exposure, presenting as itchy red bumps and pustules, often concentrated in areas covered by swimwear. These hot tub folliculitis pictures typically show widespread, intensely pruritic lesions.
- Pseudofolliculitis Barbae: A non-infectious condition often seen in individuals with curly hair who shave. It results from hair curling back into the skin after shaving, causing an inflammatory reaction. Visually, it presents as inflamed papules and pustules, with ingrown hairs often visible as dark dots or loops beneath the skin surface. This condition is a common cause of razor bumps images.
- Eosinophilic Folliculitis: A rare form often associated with HIV/AIDS or certain medications. Characterized by intensely itchy, red bumps and pustules, especially on the face, neck, and upper trunk. These lesions can be recurrent and persistent, differing from typical bacterial forms in their severe pruritus and often atypical presentation.
Understanding these varied presentations captured in folliculitis symptoms photos is crucial for accurate self-assessment and medical diagnosis. The core visual component remains the inflammatory lesion centered on a hair follicle, but specific features like pus quality, lesion uniformity, itch intensity, and distribution can provide important clues about the underlying cause.
Signs of Folliculitis Pictures
When analyzing signs of Folliculitis pictures, the focus shifts to observable, objective indications that a healthcare professional would identify. These signs provide a more clinical perspective on the condition’s manifestation. The fundamental sign is the presence of follicular inflammation, which visually translates into specific skin changes. The signs are often consistent regardless of the underlying cause, though subtle differences can help narrow down the diagnosis. The evolution of these signs over time can also be indicative of the disease’s progression or response to treatment. For instance, a reduction in redness and swelling would be a positive sign of healing.
Key folliculitis clinical signs observed include:
- Perifollicular Erythema: This refers to the redness specifically surrounding the opening of the hair follicle. It’s often one of the earliest signs, indicating inflammation localized to the follicular unit. On darker skin tones, this erythema might appear as a darker brown or purplish discoloration rather than bright red. This concentric redness around each hair is a tell-tale sign in folliculitis dermatology pictures.
- Follicular Papules: These are palpable, raised solid bumps centered on a hair follicle. They indicate an inflammatory infiltrate within and around the follicle. The texture can range from smooth to slightly rough. The size is typically small, often 1-3 mm, but can be larger in deeper forms.
- Follicular Pustules: These are small, circumscribed elevations of the skin containing pus, again, distinctly centered on a hair follicle. The pus can be sterile (e.g., in some drug-induced folliculitis) or contain bacteria or yeast. The color of the pus can vary from white to yellow, sometimes with a greenish tinge if certain bacteria like Pseudomonas are involved. Pustules are definitive signs of active infection or significant inflammation.
- Hair Shaft Involvement: This is a critical diagnostic sign. In many cases, a hair shaft can be visibly seen emerging from the center of the papule or pustule. In other instances, particularly in pseudofolliculitis barbae, the hair might be seen coiling back into the skin or growing horizontally within the superficial epidermis, causing irritation. The presence of hair, or evidence of a hair follicle, differentiates folliculitis from other skin conditions like non-follicular acne or eczema.
- Crusts and Scales: Once pustules rupture or lesions begin to resolve, serous fluid and pus dry to form crusts. These can be honey-colored (impetiginized) if secondary bacterial infection is prominent, or simply yellowish-brown. Scaling might also be present, especially in fungal folliculitis, indicating increased epidermal turnover or inflammation.
- Excoriations: Visible scratch marks are a common sign, especially when folliculitis is intensely itchy. These can range from superficial linear abrasions to deeper scratches, and they signify the patient’s reaction to pruritus. Excoriations can also introduce secondary bacterial infections, complicating the clinical picture.
- Localized Edema and Induration: The skin surrounding the follicular lesions may feel firm (indurated) or appear swollen (edematous) due to inflammatory fluid accumulation. This is more pronounced in deeper infections like furuncles and carbuncles, where a significant area of skin can become hard and swollen.
- Regional Lymphadenopathy: In cases of extensive or deep folliculitis, particularly boils and carbuncles, regional lymph nodes (e.g., in the neck for scalp folliculitis, in the groin for leg folliculitis) may become swollen and tender. This systemic sign indicates a more significant infection and an active immune response.
- Post-inflammatory Pigmentary Changes: After the active lesions heal, the affected areas often show changes in skin coloration. Post-inflammatory hyperpigmentation (PIH) appears as darker brown or purplish spots, common in individuals with darker skin tones. Post-inflammatory hypopigmentation (PIH) results in lighter areas, indicating a temporary or sometimes permanent loss of melanin. Scarring, particularly with deeper lesions, is another long-term sign. These pigmentary changes are frequently observed in folliculitis aftermath pictures.
The distribution pattern is another critical visual sign. Scalp folliculitis signs often involve the crown or occipital regions, sometimes leading to areas of patchy hair loss if chronic or severe. Facial folliculitis signs are common in the beard area in men (sycosis barbae) or around the mouth and nose (perioral folliculitis). Folliculitis on the trunk (back, chest) or buttocks often presents with numerous lesions in a widespread pattern, which can be misidentified as acne. Extremity folliculitis signs, particularly on the legs, are frequently associated with shaving or tight clothing, appearing in rows or clusters. The pattern helps distinguish folliculitis from other dermatological conditions.
Specific signs can also point to certain types of folliculitis:
- Gram-Negative Folliculitis: Often occurs in individuals on long-term oral antibiotics for acne. Visually, it presents as large pustules, sometimes cystic lesions, typically on the face, especially around the nose and chin, after a period of improvement from acne.
- Oil Folliculitis: Caused by exposure to insoluble oils (e.g., petroleum products, cutting oils). Characterized by papules and pustules, often on the forearms or thighs, depending on exposure areas. These are occupational folliculitis signs for workers.
- Tinea Barbae: A fungal infection of the beard area, sometimes confused with bacterial folliculitis. The signs include inflamed, scaly papules and pustules, often with broken hairs or hair loss (alopecia), and can sometimes present with deep, boggy nodules (kerion). Close inspection or specific diagnostic tests are crucial.
In summary, the objective signs of folliculitis, as depicted in folliculitis diagnostic images, are rooted in the inflammatory response of the hair follicle. From the initial perifollicular erythema and papule formation to pustulation, crusting, and potential long-term pigmentary changes or scarring, these visual cues provide essential information for accurate diagnosis and management. Recognizing these detailed signs is paramount for both patients and clinicians.
Early Folliculitis Photos
Recognizing early Folliculitis photos is crucial for prompt intervention and preventing the progression of the condition. At its nascent stage, folliculitis can be subtle and easily mistaken for minor skin irritations or nascent pimples. However, careful observation reveals specific characteristics that distinguish it as an inflammatory process centered around a hair follicle. The initial presentation is often mild, but awareness of these subtle cues can make a significant difference in management. The key is to look for the earliest signs of inflammation specifically involving a hair-bearing pore.
The primary initial folliculitis signs typically include:
- Pinpoint Redness Around a Hair Follicle: One of the very first signs is a tiny area of erythema (redness) directly surrounding the opening of a hair follicle. This might be no larger than the head of a pin. This localized redness indicates the earliest inflammatory response to an irritant or pathogen attacking the follicle. It’s important to distinguish this from general skin redness; the follicular centering is key.
- Minute Red Bumps (Micropapules): These are very small, barely raised, red bumps that appear directly at the site of a hair follicle. They are often non-tender at this stage or only mildly so. These micropapules represent the initial cellular infiltrate into the follicular structure. They might feel slightly rough or textured if run over with a fingertip.
- Subtle Itching or Tingling Sensation: Before visible lesions fully develop, some individuals report a localized itching, burning, or tingling sensation in the affected area. This subjective symptom often precedes the emergence of a clear papule or pustule and serves as an early warning sign that something is amiss with the skin. The itch is usually mild but can progress.
- Slightly Raised Hair Follicle Opening: In some earliest folliculitis pictures, the opening of the hair follicle itself may appear slightly raised or more prominent than surrounding follicles, even before overt redness or pus is visible. This subtle elevation is due to initial swelling within the follicular unit.
- Formation of a Small, Clear or White-Headed Pimple: Within hours to a day of the initial redness, a tiny, clear fluid-filled vesicle or a small white-headed pustule may form directly at the center of the red bump. This is the classic, early folliculitis lesion, indicating the accumulation of inflammatory cells. The pus is usually minimal at this stage and might be barely discernible.
- Localized Warmth: Though often subtle and requiring close attention, a slight increase in local skin temperature may be detected by touch in the very early stages, indicating active inflammation.
The context in which nascent folliculitis images appear is also significant. For example, early folliculitis after shaving (post-shave folliculitis) might manifest as tiny red dots along the shaved area, appearing within hours of shaving. Hot tub folliculitis early stages typically show numerous small, itchy red bumps appearing on the torso or limbs 12-48 hours after exposure to contaminated water. Early stages of buttock folliculitis might start as a few isolated, slightly red, firm bumps that are mildly uncomfortable when sitting.
Differentiating early folliculitis from other common skin phenomena is critical. Unlike typical acne vulgaris, early folliculitis lesions are almost exclusively centered on hair follicles and often lack the associated comedones (blackheads/whiteheads). Unlike insect bites, which can also be red and itchy, early folliculitis lesions are smaller, more numerous, and directly linked to hair follicles. Unlike general irritation or chafing, the inflammation in folliculitis is focal to the follicular unit.
Specific examples of early presentations:
- Early Bacterial Folliculitis: Begins as a small, slightly red papule that quickly progresses to a pinpoint pustule. The hair shaft is often visible. May be mildly tender.
- Early Fungal Folliculitis (Pityrosporum): Typically presents as very small, uniform, red-to-flesh-colored papules or pustules, often on the chest or back. The key here is the uniformity and often intense itch, even at an early stage, often appearing suddenly in warm, humid conditions.
- Early Pseudofolliculitis Barbae: Manifests as small, irritated red bumps in the beard area, often appearing a day or two after shaving. The earliest sign might be a tiny dark spot visible where a hair is beginning to curl back into the skin, causing initial inflammation.
The ability to identify these initial skin changes folliculitis helps individuals seek appropriate care sooner, potentially preventing more widespread outbreaks, deeper infections, or chronic issues. Early recognition allows for the application of targeted topical treatments or adjustments in hygiene practices before the condition escalates. Therefore, careful attention to these subtle, hair-follicle-centered signs in first signs folliculitis pictures is paramount.
Skin rash Folliculitis Images
Skin rash Folliculitis images showcase a widespread eruption of inflamed hair follicles, often covering a significant area of the body. Unlike isolated bumps, a folliculitis rash implies multiple lesions clustered together or distributed over a region, creating a distinct pattern that can sometimes be mistaken for other dermatological conditions like acne, eczema, or even allergic reactions. The key to identifying folliculitis as the cause of a rash lies in observing the consistent follicular centering of each individual lesion within the larger eruption. The appearance of the rash can vary widely based on the underlying cause, the affected body part, and the patient’s skin type.
When observing folliculitis rash patterns, look for:
- Clustered Eruptions: Often, the lesions appear in groups or clusters, particularly in areas prone to friction, sweating, or irritation. For example, folliculitis on the buttocks often appears as multiple red bumps in clusters due to pressure and occlusion.
- Diffuse Distribution: In conditions like hot tub folliculitis or severe bacterial folliculitis, the rash can be widespread over the torso, limbs, or back, sometimes affecting hundreds of follicles. This diffuse nature gives it a “rash-like” appearance rather than isolated lesions.
- Linear Patterns: Especially evident in shaving rash folliculitis (pseudofolliculitis barbae or general irritation after shaving), the lesions may follow the path of a razor, appearing in lines or rows. This pattern provides a strong clue regarding the etiology.
- Monomorphic vs. Polymorphic:
- Monomorphic Rashes: Seen in conditions like Pityrosporum folliculitis, where the individual papules and pustules are remarkably uniform in size, shape, and appearance. This uniformity is a strong diagnostic indicator. These monomorphic folliculitis rash pictures are distinct.
- Polymorphic Rashes: More common in bacterial folliculitis, where one might see a mix of papules, pustules, excoriations, and crusted lesions at various stages of development.
- Coloration and Texture: The rash typically appears red (erythematous) on lighter skin, potentially with a purplish or brownish hue on darker skin tones. The texture can be bumpy (papular) or contain visible pus (pustular). The skin between the lesions may or may not be inflamed, depending on the severity and type of folliculitis.
- Associated Symptoms within the Rash:
- Intense Pruritus: A common feature, especially in fungal and hot tub folliculitis. The patient’s scratching can lead to excoriations and secondary infection within the rash area.
- Burning Sensation: Some types of folliculitis, particularly those on the scalp or face, can cause a burning sensation accompanying the rash.
- Tenderness or Pain: The rash may be tender to touch, especially if the lesions are deep or numerous.
Specific body areas exhibit characteristic folliculitis rash locations and appearances:
- Scalp Folliculitis Rash: Often manifests as multiple itchy, red bumps, sometimes pustular, on the scalp. Chronic cases can lead to patchy hair loss or scarring alopecia. This can be mistaken for dandruff or other scalp conditions.
- Back and Chest Folliculitis Rash: A very common presentation, frequently mistaken for acne. The rash consists of numerous red papules and pustules, typically centered around hair follicles on the upper back, shoulders, and chest. It’s often worse in individuals who sweat heavily or wear tight clothing.
- Buttock Folliculitis Rash: Appears as a collection of red, sometimes pus-filled, tender bumps on the buttocks. It’s often exacerbated by prolonged sitting, tight clothing, or friction. The lesions can be numerous, forming a significant rash.
- Leg Folliculitis Rash: Commonly seen after shaving or waxing, presenting as a rash of red bumps and pustules along the hair-bearing areas of the legs. This is particularly prevalent on the thighs and lower legs, often displaying a linear pattern corresponding to shaving strokes.
- Armpit (Axillary) Folliculitis Rash: Can occur due to shaving, sweating, and friction in the armpits. Presents as irritated red bumps, sometimes pustular, which can be itchy and tender.
- Groin Folliculitis Rash: Similar to armpit folliculitis, often due to shaving, friction, and moisture. Presents as red papules and pustules in the groin area, which can be particularly uncomfortable.
Differential diagnosis is crucial when viewing rash pictures folliculitis to distinguish it from other conditions:
- Acne Vulgaris: While visually similar, acne typically includes comedones (blackheads and whiteheads) and affects areas rich in sebaceous glands, not just hair follicles. Folliculitis lesions are exclusively follicular.
- Eczema/Dermatitis: Eczema rashes are often very itchy, red, scaly, and ill-defined patches, but they do not typically show discrete follicular pustules and are not strictly centered on hair follicles.
- Heat Rash (Miliaria): Appears as tiny red bumps or blisters, usually in skin folds or areas of sweat accumulation. While also associated with sweat, heat rash is due to blocked sweat ducts, not hair follicles, and typically lacks pus.
- Drug Eruptions: Certain medications can cause follicular-like rashes. These are usually more widespread and generalized, and a detailed drug history is essential.
The overall impression from widespread folliculitis rash images is one of irritated skin with numerous, discrete inflammatory lesions, each tied to a hair follicle. Recognizing these specific characteristics within a larger rash presentation is vital for accurate diagnosis and determining the appropriate course of treatment. The pattern, distribution, and individual lesion morphology all contribute to the definitive identification of folliculitis as the underlying cause of the skin rash.
Folliculitis Treatment
While the previous sections focused on folliculitis symptoms and appearance, understanding Folliculitis Treatment is the natural next step for anyone identifying these signs. Treatment strategies aim to eradicate the causative agent (bacteria, fungus, etc.), reduce inflammation, relieve symptoms, and prevent recurrence. The approach depends heavily on the type, severity, and extent of the folliculitis, as well as the underlying cause. Self-care measures are often effective for mild cases, but persistent or severe folliculitis frequently requires medical intervention. It’s important to stress that treatment should be guided by a healthcare professional, especially for recurrent or deep infections.
General Principles for managing folliculitis:
- Hygiene: Regular, gentle cleansing of the affected area with mild, antiseptic soaps or washes.
- Avoid Irritants: Minimize friction from tight clothing, harsh scrubbing, or abrasive materials.
- Hair Removal Practices: If shaving is a trigger, switch to electric razors, shave in the direction of hair growth, or explore other hair removal methods like laser hair removal.
- Moisture Management: Keep skin dry, especially in areas prone to sweating. Use breathable fabrics.
Specific folliculitis medical treatments:
I. Topical Treatments: These are often the first line of defense for superficial and localized folliculitis.
- Topical Antibiotics:
- Mupirocin Cream/Ointment: Highly effective against Staphylococcus aureus. Applied directly to the lesions.
- Clindamycin Lotion/Gel: Used for bacterial folliculitis, particularly helpful in reducing inflammation.
- Erythromycin Topical Solution: Another option for bacterial infections.
- Benzoyl Peroxide Washes/Creams: Possesses both antibacterial and anti-inflammatory properties. Can be used as a wash or leave-on treatment. Useful for folliculitis on back treatment.
- Topical Antifungals: For fungal (Malassezia/Pityrosporum) folliculitis.
- Ketoconazole Cream/Shampoo: Applied to affected skin or used as a shampoo for scalp/body.
- Selenium Sulfide Shampoo: Similar to ketoconazole, can be used as a body wash.
- Ciclopirox Cream/Gel: Another effective antifungal agent.
- Econazole Cream: Broad-spectrum antifungal.
- Topical Steroids: Used short-term to reduce itching and inflammation, especially in non-infectious or very itchy forms, or as an adjunct to anti-infective therapy.
- Hydrocortisone Cream: Mild steroid for superficial relief.
- Mometasone Furoate or Triamcinolone Acetonide Cream: Mid-potency steroids for more significant inflammation, used with caution to avoid side effects.
- Other Topical Agents:
- Salicylic Acid: Helps to exfoliate and unblock follicles, useful in pseudofolliculitis barbae.
- Glycolic Acid: Similar exfoliating properties, improving skin texture and preventing ingrown hairs.
- Retinoids (e.g., Tretinoin Cream): Can help normalize follicular keratinization, preventing blockage and inflammation, particularly in chronic or pseudofolliculitis barbae.
II. Oral Medications: Prescribed for widespread, deep, or recalcitrant folliculitis, or when topical treatments are insufficient.
- Oral Antibiotics: For bacterial folliculitis. The choice depends on the specific bacteria and local resistance patterns.
- Cephalexin: Commonly used for Staphylococcal infections.
- Doxycycline/Minocycline: Tetracyclines with anti-inflammatory properties, often used for moderate to severe cases.
- Flucloxacillin: Another effective antibiotic against Staph.
- Ciprofloxacin (for Pseudomonas): Specific for hot tub folliculitis, if severe and persistent.
- Oral Antifungals: For extensive or resistant fungal folliculitis.
- Fluconazole: Effective for Malassezia (Pityrosporum) folliculitis.
- Itraconazole: Another option for fungal infections, often used for more resistant cases.
- Oral Antihistamines: To alleviate severe itching associated with certain types of folliculitis, improving comfort and preventing excoriations.
III. Procedures and advanced folliculitis therapies:
- Incision and Drainage: For boils (furuncles) and carbuncles, a healthcare provider may need to incise and drain the pus to relieve pain and promote healing. This is a critical step for deep, painful lesions.
- Laser Hair Removal: For chronic, recurrent folliculitis, especially pseudofolliculitis barbae or folliculitis on the legs/bikini area, laser hair removal can be a highly effective long-term solution by destroying the hair follicle itself, thus preventing inflammation. This is a common folliculitis prevention method.
- Photodynamic Therapy (PDT): May be considered for severe, refractory cases, especially for Gram-negative folliculitis or recalcitrant forms.
Folliculitis prevention strategies:
- Maintain Good Hygiene: Shower regularly, especially after sweating or exercise. Use mild, antibacterial soaps or washes if prone to folliculitis.
- Shaving Techniques:
- Use a clean, sharp razor or electric shaver.
- Shave in the direction of hair growth.
- Use lubricating shaving cream or gel.
- Rinse the blade frequently.
- Apply a soothing, non-comedogenic aftershave balm.
- Consider alternative hair removal methods if shaving exacerbates the condition.
- Avoid Tight Clothing: Wear loose, breathable clothing, especially in warm and humid environments, to reduce friction and sweat accumulation.
- Hot Tubs and Pools: Ensure hot tubs and pools are properly chlorinated and maintained. Shower immediately after using them.
- Moisturize: Keep skin hydrated with non-comedogenic lotions to maintain skin barrier function.
- Avoid Picking or Squeezing: Do not pick, squeeze, or scratch folliculitis lesions, as this can worsen inflammation, spread infection, and lead to scarring.
- Diet and Lifestyle: While not a primary cause, some individuals find that certain dietary changes or stress reduction can help manage chronic inflammatory skin conditions.
Regular follow-up with a dermatologist is crucial for managing chronic or recurrent folliculitis, as they can accurately diagnose the specific type and tailor the most effective folliculitis management plan. With appropriate treatment and preventative measures, most cases of folliculitis can be effectively controlled or resolved, minimizing discomfort and preventing complications like scarring or hyperpigmentation.