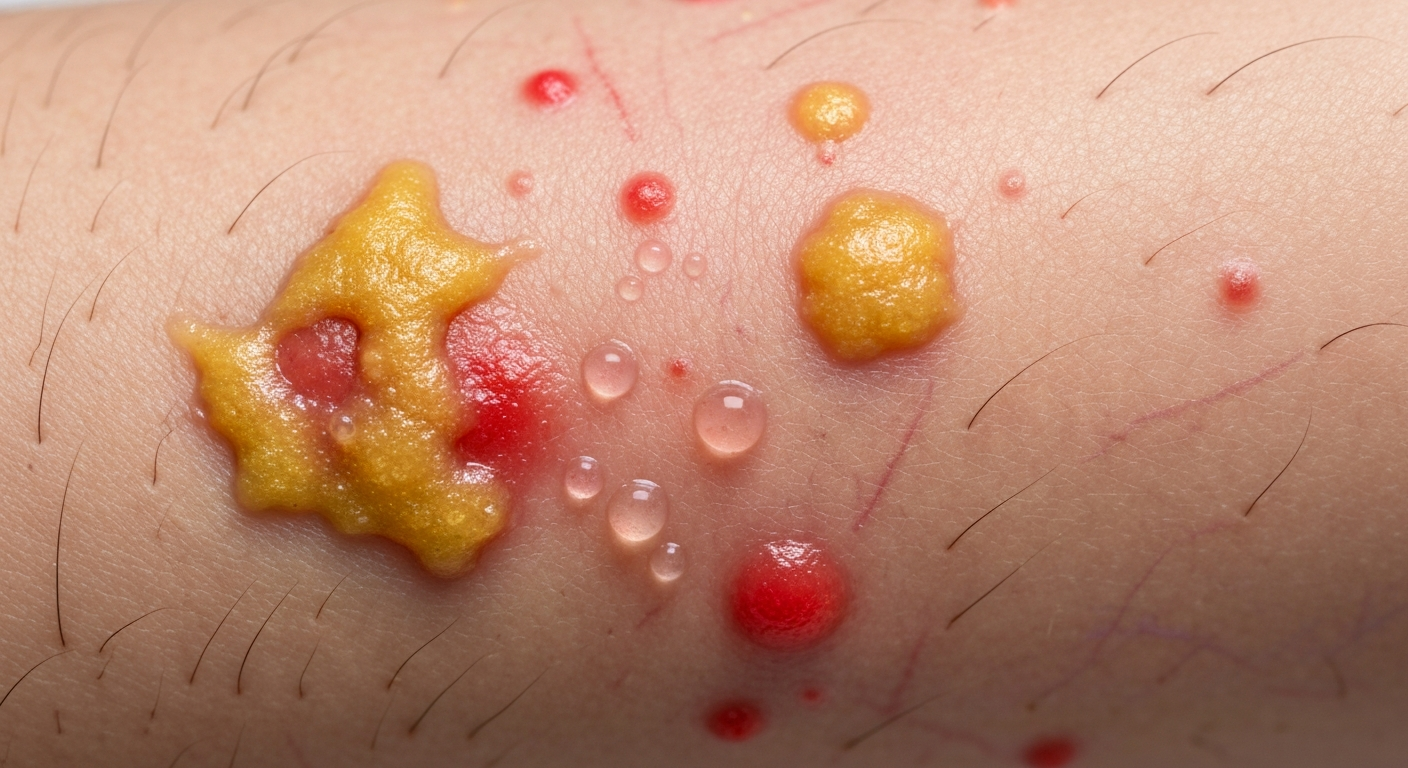
When observing children for signs of skin conditions, it’s crucial to identify characteristic lesions. This article provides an in-depth look at Streptoderma in children symptoms pictures, detailing the visual manifestations of this common bacterial skin infection to aid in early recognition and appropriate intervention. Understanding these visual cues is paramount for parents and caregivers to seek timely medical advice.
Streptoderma in children Symptoms Pictures
Streptoderma in children presents with a variety of distinct visual symptoms, making accurate identification through characteristic skin lesions and patterns essential. These infections, primarily caused by Group A Streptococcus (GAS), manifest differently depending on the specific type of streptoderma and its progression. The initial presentation often involves small, erythematous macules or papules, which quickly evolve into more pronounced vesicular or bullous formations, highly typical for childhood streptococcal infections. The hallmark visual feature is the rapid development of thin-walled vesicles that rupture, leading to the formation of golden-yellow, honey-colored crusts. These crusts are highly diagnostic and are a key indicator when examining streptoderma symptoms in children. The affected areas often appear inflamed and can be tender to the touch, reflecting the underlying bacterial activity. Furthermore, the lesions tend to coalesce, forming larger, irregular patches of crusted skin. The surrounding skin may show signs of erythema and edema, indicating the inflammatory response to the bacterial presence. Observing these distinct visual changes is critical for parents and healthcare providers in recognizing the early stages of the condition. The overall presentation can vary significantly in terms of extent and severity, ranging from localized spots to widespread areas of infection, particularly in younger children with developing immune systems. Awareness of these detailed visual symptoms aids in distinguishing streptoderma from other common childhood dermatological issues.
Key visual characteristics to look for in Streptoderma in children symptoms pictures include:
- Erythematous Macules and Papules: Small, red, flat spots or slightly raised bumps that represent the very initial phase of the infection. These can be easily overlooked but are the precursors to more advanced lesions. Their presence indicates an early inflammatory response to the bacterial invasion.
- Vesicles and Pustules: Within hours, these initial lesions progress into small, fluid-filled blisters (vesicles) or pus-filled blisters (pustules). These are typically fragile and superficial, often described as having a “dewdrop” appearance before rupturing. The fluid inside may start clear and become cloudy.
- Bullae: In some forms, particularly bullous impetigo, larger blisters (bullae) exceeding 0.5 cm in diameter develop. These bullae are typically flaccid and may contain clear or yellowish fluid, eventually collapsing and forming crusts.
- Honey-Colored Crusting: This is perhaps the most characteristic visual sign of streptoderma. After the vesicles or bullae rupture, the serum dries to form distinctive golden-yellow or honey-colored crusts. These crusts often appear “stuck on” the skin and can be quite thick. Their presence is a strong indicator of an active streptococcal infection.
- Excoriations: Due to intense itching, children often scratch the affected areas, leading to linear abrasions and further spread of the infection. These excoriations can complicate the visual diagnosis and introduce secondary bacterial infections.
- Erythema and Edema: The skin surrounding the lesions often appears red (erythematous) and swollen (edematous), reflecting the acute inflammatory process. This redness can extend beyond the immediate lesion borders.
- Regional Lymphadenopathy: Although not a skin symptom, swollen and tender lymph nodes in the areas draining the infected skin (e.g., neck, armpits, groin) are a common associated sign, indicating the body’s immune response to the infection.
- Pruritus: While not visually observable, severe itching is a prominent symptom that often leads to scratching, which in turn contributes to the spread of lesions and the formation of crusts and excoriations.
- Distribution Pattern: Lesions frequently appear on exposed areas such as the face (especially around the mouth and nose), hands, and extremities. In infants, the diaper area can also be a common site for streptococcal infection, presenting with distinct visual patterns of redness and crusting.
Careful observation of these distinct visual cues, particularly the progression from small red spots to characteristic honey-colored crusts, is crucial for accurate identification of streptoderma skin lesions and initiating timely management. The typical visual appearance of streptoderma is highly contagious, and recognition aids in preventing further spread within families and school environments.
Variations in Streptoderma Visual Presentation
The visual presentation of streptoderma can vary depending on the specific subtype, which is important for comprehensive identification when examining Streptoderma in children symptoms pictures. While the underlying cause is often similar, the morphological differences influence the appearance and progression of the skin condition. These variations include:
- Non-bullous Impetigo (Impetigo Contagiosa): This is the most common form of streptoderma and accounts for the majority of cases. Visually, it typically begins as small, red papules that rapidly transform into thin-roofed vesicles or pustules. These superficial lesions quickly rupture, often within hours, to form the classic golden-yellow or honey-colored crusts. The crusts are usually thin and easily detached, revealing an erythematous, moist base beneath. Lesions frequently coalesce, forming larger, irregular patches of crusted skin. Common sites include the face (especially around the mouth and nose), hands, and other exposed areas. The appearance is quite superficial, involving only the epidermis.
- Bullous Impetigo: While more commonly associated with Staphylococcus aureus, streptococci can also cause this form, especially in coinfections. Visually, this type is characterized by the presence of larger, flaccid blisters (bullae) that are greater than 0.5 cm in diameter. These bullae contain clear or turbid fluid and have a distinct, often transparent roof. Unlike non-bullous impetigo, the bullae persist longer before rupturing. When they do rupture, they leave behind a thin, varnish-like crust or a moist, erythematous base. The lesions tend to be fewer in number but larger in size compared to non-bullous impetigo. This form is often seen in infants and young children and can be visually more alarming due to the size of the blisters.
- Ecthyma: This is a more severe, ulcerative form of streptoderma that extends deeper into the dermis. Visually, ecthyma lesions appear as crusted sores that are typically punched-out in appearance. The crusts are thick, adherent, and often dark brown or black, quite different from the superficial honey-colored crusts of impetigo. Upon removal of the crust, a deep, ulcerated base with raised, indurated borders is revealed. These lesions heal slowly and often leave a scar, which is a key visual differentiator from impetigo. Ecthyma most commonly affects the lower extremities and can be associated with poor hygiene, insect bites, or existing skin trauma.
- Perioral/Perinasal Streptoderma: This refers to streptococcal infections specifically localized around the mouth (perioral) or nose (perinasal). Visually, these lesions present as small, often fissured, erythematous patches with fine scaling and occasional crusting. They can be confused with perioral dermatitis or angular cheilitis but have distinct streptococcal features upon closer inspection, often involving more prominent crusts or small vesicles. The irritation from saliva or nasal secretions can exacerbate the visual appearance, making the skin appear perpetually moist or inflamed.
- Streptococcal Cellulitis/Erysipelas: While distinct from typical impetigo, these are deeper streptococcal infections. Erysipelas presents visually as a sharply demarcated, bright red, shiny, and swollen area of skin, often on the face or lower limbs. It has a characteristic “peau d’orange” (orange peel) texture due to lymphatic involvement. Cellulitis is a deeper infection with less distinct borders, appearing as a generalized area of redness, warmth, swelling, and tenderness. While not primary forms of streptoderma in the “impetigo” sense, they are important to consider in the context of invasive streptococcal skin infections in children.
Understanding these visual nuances is essential for accurate diagnosis and tailored treatment, especially when reviewing streptoderma rash in children images and differentiating it from other dermatological conditions.
Signs of Streptoderma in children Pictures
When reviewing signs of Streptoderma in children pictures, one must pay close attention to the dynamic changes in the skin over time, as the infection progresses through various stages, each with its characteristic visual markers. The initial signs are often subtle, easily mistaken for minor irritations, but they rapidly evolve into the more recognizable features. The primary visual sign of a developing streptococcal infection is the appearance of small, red lesions, which quickly become vesicular. These tiny blisters, filled with clear fluid, are fragile and prone to rupture, which is a critical visual event in the progression of the disease. Once ruptured, the key diagnostic visual sign emerges: the formation of unique honey-colored crusts. These crusts are typically yellowish-brown, somewhat thick, and have a distinct “stuck-on” appearance that is highly indicative of streptoderma. This characteristic visual manifestation is a cornerstone for identification in any collection of streptoderma images for children. Beyond the lesions themselves, other visual cues include the surrounding erythema and edema, indicating localized inflammation, and evidence of scratching or excoriations, which can lead to further spread. The distribution of these lesions, often on the face, hands, and extremities, also serves as an important visual sign. It is the combination of these visual signs – the type of lesion, the color and texture of the crusts, the surrounding skin reaction, and the location – that creates a comprehensive picture of streptoderma.
Detailed visual signs to identify in Streptoderma in children pictures:
- Initial Erythematous Macule/Papule: The very first visual sign is often a small, non-descript red spot or slightly raised bump, typically 1-3 mm in diameter. This lesion is usually non-specific, resembling a mosquito bite or a minor irritation, but its rapid evolution distinguishes it. It is often warm to the touch and slightly tender.
- Vesicle or Pustule Formation: Within hours to a day, the macule or papule transforms into a small, superficial, fluid-filled blister (vesicle) or a pus-filled blister (pustule). These vesicles are often described as “dewdrops on a rose petal” due to their delicate, thin roof and erythematous base. The fluid initially clear, may become cloudy or purulent.
- Rupture of Lesion and Weeping: The thin-walled vesicles or pustules are extremely fragile and readily rupture, often due to minor trauma, scratching, or even spontaneously. Visually, this results in an oozing or weeping surface, releasing serous or seropurulent fluid. This moist environment is conducive to bacterial growth and crust formation.
- Formation of Honey-Colored Crusts: This is the most iconic visual sign in Streptoderma in children pictures. The fluid from the ruptured lesions dries to form characteristic golden-yellow or honey-colored crusts. These crusts vary in thickness, can be soft or somewhat firm, and appear to be “glued” onto the skin surface. The specific hue and texture are key for differentiating it from other crusting dermatoses.
- Circinate or Arcuate Lesion Borders: As lesions spread peripherally and heal centrally, they can form distinct ring-shaped (circinate) or arc-shaped (arcuate) patterns, particularly on the trunk or extremities. This spread creates visually interesting and often expanding borders of infection.
- Satellite Lesions: New, smaller lesions often appear around the primary site of infection, visually indicating the contagious nature and spread of the bacteria, often through autoinoculation from scratching. These “satellite” lesions can form a cluster around the main patch of streptoderma.
- Absence of Fever (often): While not a visual sign, it’s an important accompanying characteristic. Most cases of uncomplicated impetigo are not associated with systemic symptoms like fever, helping to visually differentiate it from more severe infections that might present with fever and malaise.
- Post-inflammatory Hyperpigmentation/Hypopigmentation: After the lesions heal, especially in children with darker skin tones, temporary visual changes in skin pigmentation may occur. This can manifest as darker spots (hyperpigmentation) or lighter spots (hypopigmentation) at the site of the healed lesion, which eventually resolves.
- Itching and Discomfort: While not directly visible, the signs of itching (scratch marks, restless behavior in the child) are indirect visual cues that suggest the presence of an irritating skin condition like streptoderma.
The combination of these visual signs provides a comprehensive understanding of streptoderma symptoms pictures, enabling a more precise assessment and guiding appropriate management strategies for pediatric patients. Early recognition based on these visual hallmarks is crucial to prevent complications and limit transmission.
Advanced Visual Signs and Complications
Beyond the typical impetiginous lesions, advanced or complicated streptoderma can present with more severe visual signs that warrant immediate medical attention. When examining Streptoderma in children pictures, it is crucial to recognize these escalated manifestations:
- Extensive Crusting and Coalescence: In severe cases, the lesions may become incredibly numerous and coalesce into vast, contiguous areas of crusted skin. This can cover large parts of the face, limbs, or trunk, presenting a visually alarming picture of widespread infection and skin involvement. The crusts can become very thick and multilayered.
- Deep Ulceration (Ecthyma): As previously mentioned, ecthyma is a serious complication where the infection extends into the dermis. Visually, this is characterized by deeply eroded, “punched-out” ulcers beneath thick, adherent, often dark-brown or black crusts. The removal of these crusts reveals an indurated, inflamed base with purulent discharge. These lesions are typically quite painful and distinct in their visual severity compared to superficial impetigo.
- Cellulitis or Erysipelas: If the streptococcal infection spreads beyond the superficial epidermis and invades deeper dermal and subcutaneous tissues, it can lead to cellulitis or erysipelas. Visually, cellulitis presents as a rapidly spreading area of erythema, warmth, swelling, and tenderness, with poorly defined borders. Erysipelas, a more superficial but still deep infection, displays a raised, sharply demarcated border, often described as an “orange peel” appearance due to lymphatic involvement, with intense redness and a shiny surface. These are visually distinct from the localized impetigo.
- Glomerulonephritis (Post-streptococcal): While not a direct skin sign, a history of widespread streptoderma, particularly ecthyma, can lead to acute post-streptococcal glomerulonephritis (APSGN). Clinical signs include swelling (edema), particularly around the eyes and in the ankles, and changes in urine color (dark or smoky urine due due to hematuria). These are systemic visual indicators of a serious renal complication.
- Scarring: While uncomplicated impetigo typically heals without scarring, deeper forms like ecthyma almost invariably leave permanent scars. Visually, these scars appear as depressed, discolored areas of skin where the ulceration had been. The presence of such scarring retrospectively indicates a more severe initial infection.
- Toxic Shock Syndrome or Necrotizing Fasciitis: In extremely rare and severe instances, invasive streptococcal infections can lead to life-threatening conditions. Visually, toxic shock syndrome might include a diffuse, blanching erythema (sunburn-like rash) followed by desquamation, while necrotizing fasciitis presents as rapidly progressing, intense pain with skin discoloration (redness, purplish hues, bullae, eventual necrosis), swelling, and crepitus. These are critical emergency visual signs.
Recognizing these advanced visual signs and potential complications is vital for effective clinical management and preventing long-term sequelae in children affected by streptoderma. The progression from simple crusting to deep ulcers or widespread erysipelas demands heightened vigilance when interpreting streptoderma in children photos.
Early Streptoderma in children Photos
Identifying early Streptoderma in children photos is crucial for prompt intervention and preventing the spread of this highly contagious bacterial infection. The initial stages of streptoderma are often subtle, making early visual recognition challenging but vitally important. Typically, the infection begins with the appearance of small, erythematous (red) macules or papules on the skin surface. These initial lesions, often no larger than a few millimeters, can easily be mistaken for minor insect bites, allergic reactions, or simple skin irritations, which highlights the need for careful observation. However, their rapid evolution provides the key visual clues for early diagnosis. Within a short period, sometimes just a few hours, these red spots quickly transform into thin-walled vesicles, which are small, fluid-filled blisters. These vesicles are quite fragile and superficial, often appearing like tiny “dewdrops” on an erythematous base. The fluid inside these blisters may initially be clear but soon becomes turbid or yellowish as pus forms, turning them into pustules. The speed of this progression from a simple red spot to a vesicular or pustular lesion is a significant visual marker for early streptococcal skin infections in children. Furthermore, these early lesions are often accompanied by localized redness and slight swelling, indicating the body’s inflammatory response to the bacterial presence. The initial areas affected are typically exposed skin surfaces such as the face (especially around the mouth and nose), hands, and extremities, making them readily visible. Recognizing these initial visual changes is paramount for parents and healthcare providers to distinguish streptoderma from other benign skin conditions and initiate appropriate treatment before the infection becomes more widespread and crusted.
Detailed visual characteristics of early Streptoderma in children photos include:
- Initial Erythematous Macule/Papule:
- Appearance: A small, flat, red spot (macule) or a slightly raised, red bump (papule).
- Size: Typically 1-3 mm in diameter.
- Color: Bright red or pinkish-red, often distinct against normal skin tone.
- Location: Most frequently seen on exposed areas like the face (perioral, perinasal regions), hands, arms, and legs.
- Progression: This is the very first visible sign, preceding blister formation. It may be slightly warm or tender to touch.
- Vesicle Formation (“Dewdrop” Appearance):
- Appearance: Within hours of the initial macule/papule, a small, superficial, fluid-filled blister develops on the erythematous base.
- Size: Still small, often 2-5 mm, but visibly distinct from a flat macule.
- Fluid Content: Initially clear, serum-filled.
- Roof: Extremely thin and fragile, appearing almost transparent, hence the “dewdrop” analogy.
- Surrounding Skin: The area immediately around the vesicle remains erythematous (red).
- Significance: This stage is highly indicative of an evolving impetigo, serving as a critical visual cue for early streptoderma identification.
- Pustule Development:
- Appearance: The fluid within the vesicle becomes cloudy or distinctly yellowish, indicating the presence of pus.
- Texture: Still superficial, but the lesion may appear slightly more opaque than a clear vesicle.
- Significance: The transition from clear fluid to pus signifies the active bacterial proliferation within the lesion, a clear visual indicator of infection.
- Early Rupture and Weeping:
- Appearance: The fragile vesicles or pustules rupture very easily, often spontaneously or with minimal scratching.
- Visual Result: A moist, glistening, denuded area of skin is exposed, often weeping serous fluid. This is a critical stage before crust formation.
- Size of Ruptured Area: Corresponds to the size of the initial vesicle/pustule, often small and round.
- Incipient Honey-Colored Crusting:
- Appearance: As the serous exudate from the ruptured lesion dries, it begins to form a thin, nascent golden-yellow or honey-colored crust.
- Texture: At this early stage, the crust may be very thin and delicate, not yet fully developed into the thick, “stuck-on” appearance of later stages.
- Color: The characteristic golden hue starts to become visible, a definitive visual marker for streptoderma symptoms pictures.
- Significance: The beginning of crust formation is a strong indicator that the infection is rapidly progressing and requires attention.
- Localized Erythema and Edema:
- Appearance: The skin immediately surrounding the early lesions often appears redder (erythematous) and slightly swollen (edematous).
- Extent: This redness is typically localized to the immediate vicinity of the lesion, not widespread.
- Tactile: The area may feel slightly warmer to the touch than unaffected skin.
Observing these precise visual sequences in early Streptoderma in children photos helps in making an accurate and timely diagnosis, which is fundamental for effective treatment and preventing further spread. The rapid evolution from a simple red spot to a crusted lesion is the most important visual timeline to monitor.
Skin rash Streptoderma in children Images
The appearance of a skin rash Streptoderma in children images reveals a distinctive pattern of lesions that are highly suggestive of this bacterial infection. Unlike many viral rashes, streptoderma exhibits specific morphological features and a characteristic progression that sets it apart. The rash typically begins as small, red spots (macules or papules) that quickly evolve into fluid-filled blisters (vesicles or pustules). These lesions are superficial and thin-walled, rupturing easily to exude serum. This serous fluid then dries to form the hallmark golden-yellow or honey-colored crusts that are virtually pathognomonic for streptococcal impetigo. The color, texture, and “stuck-on” appearance of these crusts are critical visual identifiers when examining any childhood streptoderma rash photos. The rash often presents as discrete lesions that can coalesce, forming larger, irregular patches of crusted skin. The surrounding skin is typically inflamed, appearing red and sometimes swollen, especially around the active lesions. Scratching is a common accompaniment, leading to excoriations that can further spread the infection and alter the visual presentation of the rash. The distribution of the rash is also a key visual clue, commonly affecting exposed areas such as the face (especially around the nose and mouth), hands, arms, and legs. In younger children, the diaper area or any skin folds can also be affected, presenting with a similar crusting rash. It’s crucial to differentiate this distinct rash from other common childhood skin conditions like eczema, fungal infections, or viral exanthems, which often lack the characteristic honey-colored crusts and rapid vesicular progression. The visual consistency across various streptoderma cases, particularly the crusting, makes this a recognizable rash pattern.
Key visual characteristics of the skin rash Streptoderma in children images include:
- Characteristic Lesion Morphology:
- Evolutionary Stages: The rash doesn’t appear all at once but evolves through distinct visual stages: red macule/papule -> vesicle/pustule -> ruptured lesion -> honey-colored crust. Different stages may be visible simultaneously across the affected area.
- Crust Appearance: The defining feature is the golden-yellow to honey-colored crust, which often appears thick and seems to be “pasted on” the skin. This visual is paramount in differentiating streptoderma.
- Vesicle/Pustule Nature: Small, superficial, and fragile. They are often short-lived before rupturing.
- Distribution of the Rash:
- Common Locations:
- Face: Frequently seen around the mouth (perioral) and nose (perinasal), as well as on the cheeks and chin. These areas are prone to moisture and minor trauma.
- Extremities: Hands, fingers, arms, and legs, especially areas easily scratched or exposed to environments.
- Diaper Area: In infants, the perineum and gluteal folds can be affected, often confused with severe diaper dermatitis.
- Other Areas: Any site of minor skin trauma (e.g., insect bites, scratches, cuts) can be a portal of entry for the bacteria, leading to localized rash development.
- Pattern of Spread: The rash tends to spread peripherally from an initial site, and new “satellite” lesions can appear in adjacent areas due to autoinoculation.
- Common Locations:
- Associated Skin Changes:
- Erythema: Redness is always present around the active lesions, sometimes extending slightly beyond the immediate crusts.
- Edema: Localized swelling can be noted, especially with more inflammatory lesions or on delicate skin surfaces.
- Excoriations: Visible scratch marks are very common, indicating intense pruritus (itching), and can make the rash appear more irritated or damaged.
- Coalescence: Individual lesions often merge together, forming larger, irregularly shaped patches of crusted skin, creating a visually extensive rash.
- Absence of Widespread Systemic Rash:
- Unlike viral exanthems (e.g., measles, chickenpox), streptoderma primarily causes a localized rash, or several localized patches, rather than a generalized, uniform body rash. This focal nature is a diagnostic visual cue.
- Differentiation from Similar Rashes:
- Herpes Simplex: While herpes can cause vesicles and crusts around the mouth, the clusters of vesicles are typically uniform in size, preceded by tingling, and the crusts are usually drier and less “honey-colored.”
- Contact Dermatitis: Often intensely itchy, with redness, swelling, and sometimes vesicles, but the crusts are not typically honey-colored and the history of allergen exposure is key.
- Fungal Infections (Tinea): Present with annular (ring-shaped) lesions with scaling and central clearing, but generally lack the rapid vesiculation and honey-colored crusting.
- Eczema (Atopic Dermatitis): Characterized by chronically itchy, dry, reddened, and thickened skin. When secondarily infected with bacteria, it can develop crusts, but the underlying eczema features are usually still visible.
A comprehensive assessment of streptoderma rash images requires attention to these intricate visual details, ensuring accurate diagnosis and appropriate treatment strategies. The distinctive crusting pattern is a visual fingerprint of this common childhood skin infection.
Visual Progression and Patterns of Streptoderma Rash
Understanding the visual progression and common patterns displayed in skin rash Streptoderma in children images is paramount for effective clinical assessment. The rash typically doesn’t appear as a static entity but rather as a dynamic process of lesion development, spread, and healing.
- Centrifugal Spread: The rash often starts at a primary site, usually an area of minor skin trauma or pre-existing dermatitis, and then spreads outwards. New lesions (satellite lesions) often develop at the periphery of the main rash, creating an expanding border of infection. This centrifugal pattern is a key visual indicator of active bacterial spread.
- Autoinoculation: A significant visual pattern is the development of new lesions in areas distant from the primary site, often caused by the child scratching an infected area and then touching other parts of their body. This leads to a scattering of similar lesions, particularly on the hands, face, and other easily accessible body parts, visually demonstrating the contagious nature of the infection within the individual.
- Linear Patterns: Sometimes, especially after scratching with an infected fingernail, the rash can appear in a linear fashion, following the path of the scratch. This provides a visual history of how the infection was spread on the child’s skin.
- Perifollicular Involvement: While less common than typical impetigo, streptoderma can sometimes involve hair follicles, leading to folliculitis. Visually, this would appear as small pustules centered around hair shafts, which can then rupture and crust, adding another dimension to the rash presentation.
- Healing Patterns: As the rash heals, the crusts detach, revealing new, often erythematous skin underneath. This new skin may appear slightly pinker or have transient post-inflammatory hyperpigmentation or hypopigmentation, particularly in darker skin types. The absence of scarring (unless it was ecthyma) is a good visual indicator of healing in uncomplicated cases. The healing areas may look somewhat drier and less inflamed than active areas.
- Location-Specific Appearances:
- Perinasal/Perioral: The rash around the nose and mouth often shows a distinct circular or semi-circular pattern, sometimes with fissures at the corners of the mouth (angular cheilitis), which can be due to streptococcal infection. The constant moisture in these areas can make the crusts appear softer or more exudative.
- Scalp: While less common, streptoderma on the scalp can be obscured by hair but may present with crusted lesions, sometimes leading to localized hair loss if severe or complicated by folliculitis.
- Skin Folds: In areas like the armpits, groin, or neck folds, the rash can appear more macerated due to moisture and friction, often leading to more extensive erosion beneath the crusts.
These visual patterns in streptoderma in children pictures offer crucial insights into the infection’s behavior, severity, and potential complications, guiding both diagnosis and management strategies.
Streptoderma in children Treatment
Effective Streptoderma in children treatment focuses on eradicating the bacterial infection, preventing spread, and alleviating symptoms. Treatment typically involves a combination of topical and/or oral antibiotics, along with rigorous hygiene practices. The choice of treatment modality depends on the extent and severity of the infection, as well as the child’s age and overall health. Early initiation of appropriate therapy is crucial not only to resolve the existing lesions but also to prevent potential complications such as acute post-streptococcal glomerulonephritis. For localized and mild cases of streptoderma, topical antibiotic therapy is usually sufficient and highly effective. This approach minimizes systemic exposure to antibiotics. However, for more widespread infections, cases unresponsive to topical treatment, or instances where a deeper infection (like ecthyma) is suspected, oral antibiotics become the cornerstone of therapy. Regardless of the antibiotic regimen, supportive care including gentle wound cleaning and measures to prevent scratching are integral components of comprehensive streptoderma management in children. Proper adherence to the full course of antibiotics is essential to ensure complete eradication of the bacteria and to reduce the risk of recurrence and transmission. Close monitoring for signs of improvement or worsening of the condition is also important during the treatment period.
Topical Antibiotic Treatment for Streptoderma
For localized and mild cases of streptoderma, topical antibiotics are often the first-line treatment. These are applied directly to the affected skin, targeting the bacteria at the site of infection. Key aspects of topical streptoderma treatment include:
- Mupirocin Ointment (Bactroban, Centany):
- Mechanism: A potent bactericidal agent effective against gram-positive bacteria, including Staphylococcus aureus and Streptococcus pyogenes, which are common causes of streptoderma. It inhibits bacterial protein synthesis.
- Application: Applied thinly to the lesions typically 2-3 times daily for 5-7 days. The affected area should be cleaned gently before application.
- Efficacy: Highly effective for superficial impetigo, often showing improvement within a few days.
- Considerations: Generally well-tolerated with minimal side effects. Resistance can occur with overuse, so adherence to the prescribed duration is important.
- Retapamulin Ointment (Altabax):
- Mechanism: A pleuromutilin antibiotic that inhibits bacterial protein synthesis, specifically targeting staphylococci and streptococci.
- Application: Applied thinly to the affected areas twice daily for 5 days.
- Efficacy: Effective for localized impetigo, offering an alternative to mupirocin, especially in cases of suspected mupirocin resistance.
- Considerations: Approved for use in children aged 9 months and older.
- Fusidic Acid Cream/Ointment (not widely available in the US, common in other regions):
- Mechanism: A bacteriostatic or bactericidal agent (depending on concentration) that inhibits bacterial protein synthesis. Effective against staphylococci and streptococci.
- Application: Applied 2-3 times daily for 7 days.
- Efficacy: Very effective for superficial skin infections.
- Considerations: Good penetration into the skin.
- Proper Application Techniques:
- Cleaning: Before applying the topical antibiotic, gently clean the affected skin with mild soap and water, or an antiseptic solution (e.g., chlorhexidine or povidone-iodine diluted solution) to remove crusts and debris. This allows better penetration of the medication. Pat dry.
- Gloves: Parents or caregivers should wash hands thoroughly before and after application, and ideally wear gloves to prevent autoinoculation and spread of the infection.
- Coverage: Ensure the entire lesion, including the surrounding erythematous area, is covered with a thin layer of the ointment.
- Bandaging: While not always necessary, covering the treated lesions with a loose bandage or gauze can prevent scratching, reduce spread, and protect the clothing.
Topical treatment is typically recommended for small, localized lesions, accounting for the majority of mild streptoderma cases in children.
Oral Antibiotic Treatment for Streptoderma
For more widespread streptoderma, infections unresponsive to topical treatment, or deeper infections like ecthyma, oral antibiotics are necessary. These provide systemic eradication of the bacteria. Key aspects of oral streptoderma treatment include:
- Penicillin V (Phenoxymethylpenicillin):
- Mechanism: A beta-lactam antibiotic that inhibits bacterial cell wall synthesis. Highly effective against Group A Streptococcus.
- Dosage: Typically dosed based on weight, 3-4 times daily for 7-10 days.
- Efficacy: Remains a first-line agent for streptococcal infections if penicillin allergy is absent.
- Considerations: Should be taken on an empty stomach for optimal absorption.
- Amoxicillin/Clavulanate (Augmentin):
- Mechanism: Amoxicillin is a penicillin-like antibiotic, and clavulanate is a beta-lactamase inhibitor, protecting amoxicillin from degradation by bacterial enzymes. Effective against a broader spectrum, including Staphylococcus aureus, making it useful for mixed infections.
- Dosage: Typically dosed based on weight, 2-3 times daily for 7-10 days.
- Efficacy: Effective for both streptococcal and staphylococcal components of impetigo.
- Considerations: Can cause gastrointestinal side effects (diarrhea).
- Cephalexin (Keflex):
- Mechanism: A first-generation cephalosporin antibiotic that inhibits bacterial cell wall synthesis. Effective against both streptococci and staphylococci.
- Dosage: Typically dosed based on weight, 2-4 times daily for 7-10 days.
- Efficacy: A common and effective choice for skin and soft tissue infections.
- Considerations: Generally well-tolerated; can be used in patients with mild penicillin allergy (cross-reactivity is low but possible).
- Clindamycin (Cleocin):
- Mechanism: A lincosamide antibiotic that inhibits bacterial protein synthesis. Useful for penicillin-allergic patients and for infections resistant to other antibiotics. Effective against MRSA (methicillin-resistant Staphylococcus aureus) which can co-infect.
- Dosage: Typically dosed based on weight, 3-4 times daily for 7-10 days.
- Efficacy: Good tissue penetration, effective against many common skin pathogens.
- Considerations: Higher risk of causing Clostridioides difficile-associated diarrhea (CDAD).
- Azithromycin (Zithromax):
- Mechanism: A macrolide antibiotic that inhibits bacterial protein synthesis. Useful for penicillin-allergic patients, though streptococcal resistance to macrolides can be an issue.
- Dosage: Often given once daily for 5 days.
- Efficacy: Convenient dosing regimen, but susceptibility testing may be needed due to resistance concerns in some communities.
- Considerations: Can cause gastrointestinal upset.
- Important Considerations for Oral Antibiotics:
- Complete the Full Course: Emphasize the importance of completing the entire prescribed course of antibiotics, even if symptoms improve, to ensure complete eradication of the bacteria and prevent recurrence or development of resistance. This is crucial for preventing complications like glomerulonephritis.
- Allergies: Always ascertain any known antibiotic allergies before prescribing.
- Side Effects: Counsel parents on potential side effects (e.g., diarrhea, nausea, rash) and when to seek further medical advice.
- Drug Interactions: Be aware of potential interactions with other medications the child may be taking.
Oral antibiotics are a vital component in treating more severe or widespread streptoderma infections in children, especially to prevent systemic complications.
Supportive Care and Hygiene Measures
Beyond antibiotics, supportive care and diligent hygiene are critical for managing streptoderma, preventing spread, and promoting healing. These measures are often overlooked but significantly impact the overall outcome of streptoderma in children treatment.
- Gentle Cleaning of Lesions:
- Warm Soapy Water: Gently wash the affected areas with warm water and a mild, unscented soap 2-3 times a day. This helps remove crusts, exudate, and bacteria.
- Antiseptic Solutions: In some cases, healthcare providers might recommend diluted antiseptic solutions (e.g., chlorhexidine or povidone-iodine) to cleanse the lesions, especially for stubborn crusts or widespread involvement. These help reduce bacterial load.
- Soft Cloth/Gauze: Use a soft cloth or gauze to gently dab and loosen crusts. Avoid harsh scrubbing which can irritate the skin and delay healing.
- Preventing Scratching (Pruritus Control):
- Keep Fingernails Trimmed: Short, clean fingernails reduce the risk of further skin damage from scratching and minimize the spread of bacteria.
- Antihistamines: Oral antihistamines (e.g., diphenhydramine, cetirizine) can be prescribed to reduce itching, especially if it interferes with sleep. Reducing pruritus helps prevent excoriations and autoinoculation.
- Mittens/Gloves: For infants and very young children, soft mittens or gloves, especially at night, can prevent scratching and further trauma to the lesions.
- Isolation and Preventing Spread:
- Hand Hygiene: Frequent and thorough handwashing with soap and water is crucial for the child, parents, and caregivers to prevent transmission. Alcohol-based hand sanitizers can be used when soap and water are not available.
- Separate Towels/Linens: Use separate towels, washcloths, and bed linens for the infected child to prevent cross-contamination within the household. Wash these items in hot water.
- Avoid Sharing Personal Items: Do not share clothing, toys, razors, or other personal items that come into contact with the infected skin.
- School/Daycare Exclusion: Children with active, weeping, or uncovered streptoderma lesions should typically be excluded from school or daycare until the lesions are dry, crusted, or effectively treated (usually 24-48 hours after starting antibiotics) to prevent outbreaks.
- Cover Lesions: Keep active lesions covered with loose clothing or sterile gauze and tape whenever possible to minimize direct contact and spread.
- Hydration and Skin Care:
- Moisturizers: Once the acute infection is under control and crusts have fallen off, gentle, hypoallergenic moisturizers can help restore skin barrier function and prevent dryness.
- Avoid Irritants: Steer clear of harsh soaps, perfumed products, or strong detergents that can irritate the healing skin.
- Monitoring for Complications:
- Signs of Worsening: Watch for signs of worsening infection such as increasing redness, swelling, pain, fever, or the development of larger blisters or deep ulcers.
- Post-Streptococcal Glomerulonephritis (APSGN): Educate parents on symptoms of APSGN (e.g., cola-colored urine, swelling around the eyes or ankles, decreased urine output), especially after widespread or recurrent streptoderma, and advise prompt medical evaluation if these occur.
These supportive and hygiene measures are fundamental to a holistic approach to streptoderma in children treatment, promoting faster healing and significantly reducing the risk of spread and complications.