Viewing Periodontosis symptoms pictures is crucial for early detection and understanding the progression of severe gum disease. These visual aids help individuals and healthcare professionals identify the characteristic signs of periodontal destruction, ranging from inflamed gingiva to advanced bone loss, allowing for timely intervention and management.
Periodontosis Symptoms Pictures
Examining Periodontosis symptoms pictures reveals a range of visible indicators signifying advanced gum disease. These symptoms often progress silently, making visual recognition vital for preventing further damage and potential tooth loss. Understanding these visual cues can empower individuals to seek professional dental care promptly.
- Severe Gingival Inflammation and Redness: One of the most prominent signs in Periodontosis symptoms pictures is intensely red, often purplish, gums. This redness is indicative of significant inflammation and increased blood flow to the infected tissues. Unlike healthy pink gums, diseased gingiva appears engorged and hyperemic, sometimes extending to the interdental papillae, which may appear blunted or swollen.
- Swollen and Puffy Gums: Affected gum tissues often appear swollen and puffy, losing their firm, stippled texture. This edematous appearance is due to the accumulation of inflammatory exudates and fluids within the gum tissues. In Periodontosis symptoms pictures, this swelling can make the gums look bloated, sometimes obscuring parts of the tooth surface.
- Chronic Gum Bleeding: Spontaneous gum bleeding or bleeding upon gentle probing, brushing, or flossing is a hallmark symptom. While not always directly visible in static images, severe instances can show dried blood residue on tooth surfaces or within the gingival margins. This bleeding is a direct result of the fragile, inflamed blood vessels within the diseased periodontal tissues.
- Gum Recession and Exposed Tooth Roots: As periodontosis progresses, the gum tissue pulls away from the teeth, exposing the roots. Periodontosis symptoms pictures frequently highlight significant gum recession, making teeth appear longer than usual. Exposed roots are often discolored, sensitive, and more susceptible to decay, visually altering the smile line and tooth aesthetics.
- Pus Formation and Discharge (Suppuration): In advanced cases, pus may be visible emanating from the gumline or periodontal pockets, especially when pressure is applied to the gums. This yellowish or whitish discharge is a clear sign of active bacterial infection and host immune response. Periodontosis symptoms pictures might capture this exudate, indicating a severe stage of the disease.
- Tooth Mobility and Shifting: As the bone supporting the teeth is destroyed, teeth can become loose and may even shift position. This can lead to new gaps or widening spaces between teeth, or a change in how the upper and lower teeth fit together. Visual evidence in Periodontosis symptoms pictures might show teeth splaying outwards or new diastemas developing.
- Persistent Bad Breath (Halitosis): While halitosis itself is not a visual symptom, the severe bacterial load and tissue destruction responsible for Periodontosis symptoms pictures are often accompanied by a strong, unpleasant odor. The presence of plaque, calculus, and necrotic tissue provides a fertile ground for anaerobic bacteria producing volatile sulfur compounds.
- Pain or Tenderness: Although subjective, severe periodontosis can cause discomfort, pain, or tenderness in the gums, especially during chewing or brushing. Visual correlation might be seen with extremely inflamed or raw-looking gum areas.
- Calculus and Plaque Buildup: Extensive hard (calculus) and soft (plaque) deposits on the teeth, particularly along the gumline and between teeth, are often evident in Periodontosis symptoms pictures. These deposits harbor bacteria and contribute significantly to the inflammatory process, making them a key visual diagnostic factor.
- Darkening or Brown Staining of Teeth: Exposed root surfaces due to recession are more porous and prone to staining from food, beverages, and tobacco, appearing darker than the enamel. This discoloration is often clearly visible in images showcasing advanced gum recession.
- Tooth Loss or Missing Teeth: In its most severe stages, periodontosis can lead to the loss of teeth due to irreversible destruction of supporting structures. Periodontosis symptoms pictures of individuals with advanced disease may reveal missing teeth or significant gaps where teeth once were, underscoring the devastating impact of the condition.
- Changes in Bite Alignment: As teeth become mobile and shift, the bite can change, leading to malocclusion. This can be subtly observed in Periodontosis symptoms pictures where the alignment of teeth no longer appears harmonious or where specific teeth seem to be protruding.
Signs of Periodontosis Pictures
Beyond subjective symptoms, Signs of Periodontosis Pictures highlight objective clinical findings that healthcare professionals use for diagnosis. These visual signs provide concrete evidence of the disease’s presence and severity, often reflecting underlying tissue destruction. Understanding these diagnostic signs is crucial for effective treatment planning and managing advanced gum disease.
- Deep Periodontal Pockets: While periodontal pockets themselves are measured with a probe and not directly visible, their presence leads to visible signs. Gums may appear detached from the tooth surface, creating spaces where plaque and bacteria accumulate. Signs of Periodontosis Pictures may subtly show the enlarged gingival sulcus or a rolled gingival margin due to chronic inflammation and tissue destruction extending apically.
- Clinical Attachment Loss (CAL): This refers to the apical migration of the epithelial attachment, indicating loss of tooth-supporting structures. Visually, CAL manifests as gum recession and exposed root surfaces. Signs of Periodontosis Pictures often starkly depict varying degrees of root exposure, which directly corresponds to the extent of attachment loss.
- Altered Gingival Contours: Healthy gums have a scalloped margin that closely hugs the teeth. In periodontosis, this contour is often lost, appearing blunted, swollen, or irregular. The interdental papillae may be flattened or receded, leaving triangular spaces between teeth. These altered contours are key in Signs of Periodontosis Pictures.
- Furcation Involvement: In multi-rooted teeth, severe bone loss can expose the furcation area (the anatomical area where the roots diverge). This is a critical sign of advanced disease. While often diagnosed radiographically and by probing, severe cases might show visible defects or deepened recession around the furcation in Signs of Periodontosis Pictures.
- Tooth Migration and Spacing: As mentioned in symptoms, tooth movement is a definitive sign of weakened support. Signs of Periodontosis Pictures can graphically illustrate teeth that have drifted, rotated, or tilted, creating new diastemas or worsening existing ones. This is particularly noticeable in the anterior (front) teeth.
- Bone Loss (Radiographic Evidence): Although X-rays are not “pictures” in the conventional sense for this context, the visual effects of bone loss are critical. The consequences of bone loss—such as tooth mobility, root exposure, and changes in tooth position—are direct visual signs. Radiographs (which are visual) would show reduced alveolar bone height and density, confirming the extent of periodontal destruction. While not directly a “photo,” the clinical signs are a direct manifestation of this underlying loss.
- Increased Tooth Sensitivity: Exposed root surfaces are often hypersensitive to hot, cold, sweet, or touch due to the exposure of dentinal tubules. While not a direct visual sign, patients often report this symptom, and its presence correlates strongly with visually evident root exposure in Signs of Periodontosis Pictures.
- Abfraction or Abrasion Lesions: While not caused by periodontosis directly, these wedge-shaped or V-shaped defects at the gumline are more commonly observed on exposed root surfaces due to gum recession. These lesions are visually distinct and can be prominent in Signs of Periodontosis Pictures showing exposed roots, contributing to tooth sensitivity and further aesthetic concerns.
- Darkened or Black Triangles: When the interdental papilla recedes, the space between the teeth, near the gumline, appears as a dark triangle. These “black triangles” are common in periodontosis and are clearly visible in Signs of Periodontosis Pictures, often causing aesthetic distress and food impaction.
- Abscess Formation: Acute exacerbations of periodontosis can lead to periodontal abscesses, appearing as localized, tender, red, and swollen areas on the gum, sometimes with a draining fistula. These are distinct and alarming visual Signs of Periodontosis Pictures requiring immediate attention.
- Altered Occlusion: The way teeth come together can be severely affected by tooth migration and loss of supporting bone. Observing uneven wear patterns or specific teeth making premature contact can be subtle visual clues in Signs of Periodontosis Pictures, even if the primary diagnostic is dynamic.
Early Periodontosis Photos
Identifying Early Periodontosis Photos is crucial for timely intervention, as the initial stages of periodontal disease can often be subtle and easily overlooked. These early visual cues differentiate from simple gingivitis, indicating the beginning of irreversible attachment loss. Recognizing these subtle signs allows for prompt treatment and can prevent the progression to more severe forms of periodontosis.
- Mild Gingival Redness: In Early Periodontosis Photos, the gums may exhibit a slight, diffuse redness, particularly along the gumline. This is often more pronounced than healthy pink, stippled gums but not yet the intense, purplish hue of advanced inflammation. The redness may be localized to specific areas rather than generalized.
- Slight Swelling of the Gums: The gums might appear slightly swollen or puffy, losing some of their normal firmness and knife-edge appearance. This early edema can make the gingival margins look somewhat rounded or blunted compared to healthy tissue. This subtle swelling is a key feature in Early Periodontosis Photos.
- Occasional Bleeding on Brushing or Flossing: While not directly visible in a static photo, the history of occasional bleeding during oral hygiene practices is a critical early symptom. In Early Periodontosis Photos, this might be inferred by subtle signs of inflammation that predispose to bleeding. The gums may appear a little raw or irritated after a hygiene demonstration.
- Loss of Gingival Stippling: Healthy gums often have a textured, orange-peel-like appearance known as stippling. In Early Periodontosis Photos, one might notice a loss of this stippling, making the gum surface appear smoother and shinier. This indicates early edema and inflammation in the connective tissue.
- Shiny Appearance of Gums: Due to increased fluid accumulation and loss of stippling, the gingiva in Early Periodontosis Photos might have a slightly shiny or glossy appearance, reflecting light differently than firm, healthy tissue.
- Mild Gum Recession (Initial Stages): Very subtle recession might be present, where the gumline has just barely started to pull away from the tooth, potentially exposing only a millimeter or less of the root surface. This is a critical indicator in Early Periodontosis Photos differentiating early periodontitis from gingivitis, as it signifies early attachment loss.
- Slight Tenderness to Touch: Patients might report a mild tenderness or sensitivity when the gums are touched or brushed. While not a visual, this symptom often accompanies the visible early signs in Early Periodontosis Photos.
- Subtle Changes in Gum Contour: The finely scalloped contour of the gum margin might begin to show subtle rounding or blunting, particularly around the interdental papillae, in Early Periodontosis Photos. The papillae might appear slightly swollen and less pointed.
- Increased Pocket Depths (Probing Depths): Although probing depths are measured clinically and not directly seen in Early Periodontosis Photos, the subtle signs of inflammation and early recession are indicative of deepening sulci that are beginning to form periodontal pockets (typically 4-5mm).
- Minor Plaque and Calculus Accumulation: Even in early stages, some visible plaque and calculus deposits along the gumline and interdental spaces can be seen in Early Periodontosis Photos. These deposits serve as irritants and a nidus for bacterial growth, driving the initial inflammatory response.
- Lack of Specific Pain: Often, the insidious nature of early periodontosis means there is little to no specific pain reported by the patient, despite the visible inflammation. This absence of pain is why visual identification from Early Periodontosis Photos is so critical.
Skin rash Periodontosis Images
It is critical to clarify that periodontosis, as a localized oral inflammatory disease, does not directly cause skin rash Periodontosis images. However, certain systemic diseases can manifest with both severe periodontal disease (often resembling periodontosis) and distinct skin rashes or lesions. Therefore, when discussing skin rash Periodontosis images, we are referring to mucocutaneous manifestations of underlying systemic conditions that are also associated with severe periodontal destruction.
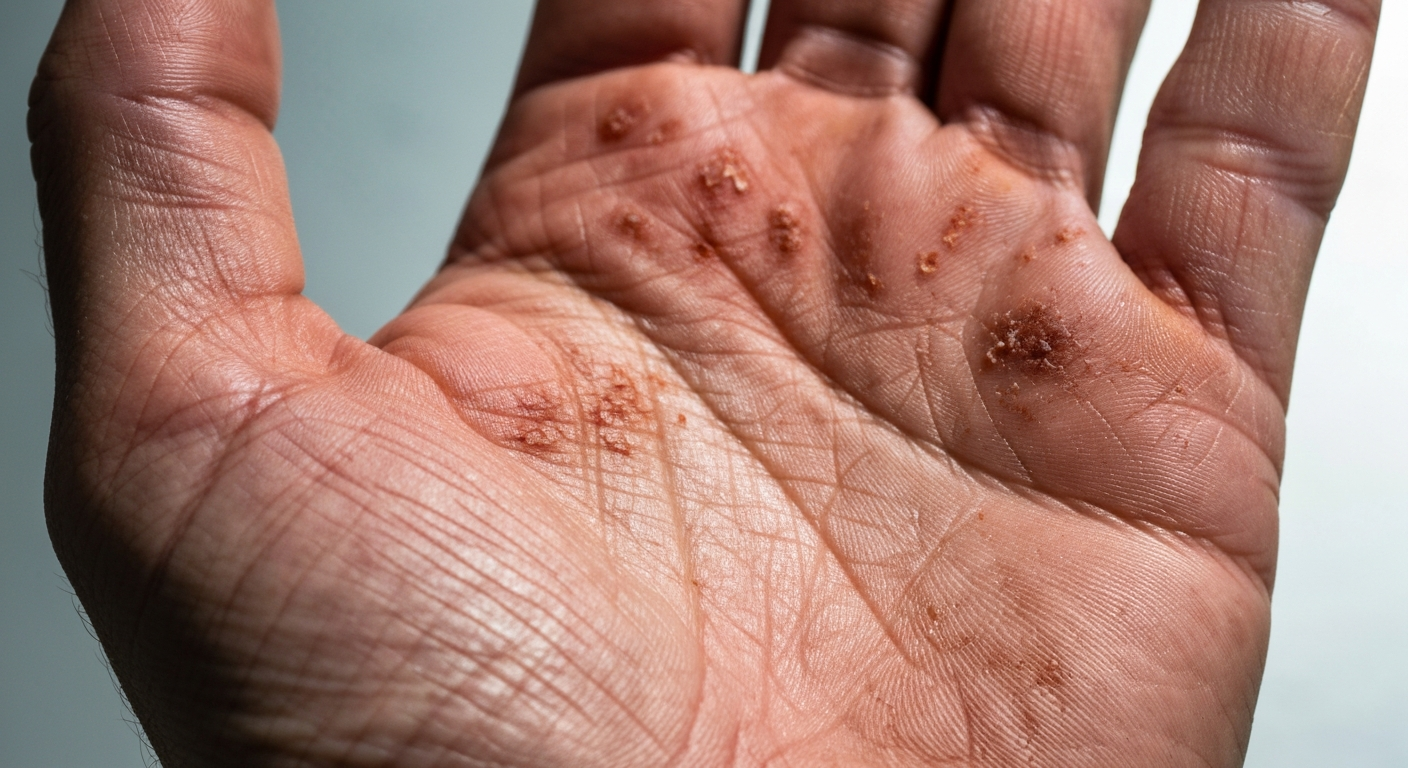
- Papillon-Lefèvre Syndrome (PLS):
- Oral Manifestations: This rare autosomal recessive disorder is characterized by severe early-onset periodontitis affecting both primary and permanent dentition, leading to premature tooth loss. The periodontitis often resembles aggressive periodontosis.
- Skin Rash Characteristics: Skin rash Periodontosis images related to PLS would show hyperkeratosis of the palms and soles (palmar-plantar hyperkeratosis). The skin appears red, scaly, and thickened, sometimes with fissures. These lesions can be diffuse or localized. Erythema and scaling may also affect other areas like knees and elbows.
- Langerhans Cell Histiocytosis (LCH):
- Oral Manifestations: LCH can present with severe periodontal involvement, including gingival inflammation, rapid bone loss, mobile teeth, and soft tissue masses. Oral lesions can mimic periodontal abscesses or rapidly destructive periodontitis.
- Skin Rash Characteristics: Skin rash Periodontosis images in LCH patients might show seborrheic dermatitis-like rashes, petechiae, purpura, or papules, particularly on the scalp, trunk, and intertriginous areas. These lesions can be yellowish-brown or reddish-brown and may crust or ulcerate.
- Leukemia (e.g., Acute Myeloid Leukemia – AML):
- Oral Manifestations: Leukemic infiltrates can cause severe gingival enlargement (leukemic gingival hypertrophy), making gums appear swollen, boggy, and prone to bleeding. This can exacerbate periodontal destruction.
- Skin Rash Characteristics: Skin rash Periodontosis images associated with leukemia include leukemia cutis (cutaneous infiltrates presenting as nodules, papules, or plaques, often reddish-brown), purpura, petechiae (small red spots from bleeding under the skin), and ecchymoses (larger bruises). These can appear anywhere on the body.
- Cyclic Neutropenia:
- Oral Manifestations: Recurrent episodes of severe gingivitis, periodontitis, and oral ulcerations due to fluctuating neutrophil counts. This predisposes individuals to severe periodontal breakdown.
- Skin Rash Characteristics: While not a direct rash, patients may experience recurrent skin infections (e.g., furunculosis, cellulitis) and oral ulcers, which might be captured in Skin rash Periodontosis images if the skin lesions are prominent during neutropenic episodes.
- Crohn’s Disease (Orofacial Granulomatosis):
- Oral Manifestations: Oral Crohn’s can present with diffuse or nodular swelling of the lips and cheeks, “cobblestoning” of the oral mucosa, deep linear ulcers, and persistent gingivitis/periodontitis.
- Skin Rash Characteristics: Skin rash Periodontosis images in Crohn’s patients might reveal erythema nodosum (tender, red nodules, usually on the shins), pyoderma gangrenosum (painful, rapidly enlarging ulcers with violaceous borders), or perianal lesions like skin tags and fissures.
- Lichen Planus:
- Oral Manifestations: Reticular (white lacy network), erosive, or ulcerative lesions on the buccal mucosa, tongue, and gingiva. Erosive lichen planus of the gingiva can mimic severe desquamative gingivitis.
- Skin Rash Characteristics: Skin rash Periodontosis images related to Lichen Planus would show characteristic purplish, polygonal, pruritic (itchy) papules, often on the flexor surfaces of the wrists, forearms, and lower legs. They may have fine white lines (Wickham’s striae).
- Pemphigus Vulgaris and Pemphigoid:
- Oral Manifestations: These autoimmune blistering diseases can cause severe oral ulcerations and desquamative gingivitis, where the outer layer of gum tissue peels away, leading to raw, bleeding surfaces. This can lead to severe periodontal complications.
- Skin Rash Characteristics: Skin rash Periodontosis images for Pemphigus show flaccid blisters that easily rupture, leaving painful erosions, while Pemphigoid typically presents with tense bullae (blisters) that are more resistant to rupture, often on the skin.
- Ehlers-Danlos Syndrome (Type VIII):
- Oral Manifestations: Characterized by severe, generalized early-onset periodontitis with rapid attachment loss and tooth mobility, often resembling periodontosis, along with fragile oral mucosa.
- Skin Rash Characteristics: Skin rash Periodontosis images of patients with Ehlers-Danlos Syndrome would demonstrate extremely fragile, hyperextensible skin, abnormal scarring (atrophic scars), easy bruising, and poor wound healing.
- HIV/AIDS:
- Oral Manifestations: HIV-associated periodontal diseases include linear gingival erythema, necrotizing ulcerative gingivitis (NUG), and necrotizing ulcerative periodontitis (NUP), which are rapidly progressive and destructive, resembling severe periodontosis. Other oral lesions like candidiasis, hairy leukoplakia, and Kaposi’s sarcoma are common.
- Skin Rash Characteristics: Skin rash Periodontosis images in HIV patients can be varied, including Kaposi’s sarcoma (purplish-red skin lesions), folliculitis, seborrheic dermatitis, xerosis (dry skin), fungal infections, and various drug eruptions.
- Diabetes Mellitus:
- Oral Manifestations: Diabetics have a significantly increased risk and severity of periodontitis, often resembling rapidly progressive forms. Poor glycemic control exacerbates inflammation and bone loss.
- Skin Rash Characteristics: Skin rash Periodontosis images related to diabetes are numerous: diabetic dermopathy (shin spots), necrobiosis lipoidica diabeticorum (yellowish-red plaques with central atrophy), acanthosis nigricans (darkening and thickening of skin folds), candidiasis, and various bacterial skin infections.
Periodontosis Treatment
While Periodontosis treatment does not appear in “pictures” in the same way symptoms do, understanding the therapeutic approaches is critical to reversing or halting the progression seen in Periodontosis symptoms pictures. The goal of Periodontosis treatment is to eliminate infection, reduce inflammation, regenerate lost tissues, and prevent further damage, thereby improving the visible clinical signs and overall oral health. Comprehensive management involves both non-surgical and surgical interventions.
- Non-Surgical Periodontosis Treatment:
- Scaling and Root Planing (SRP): This deep cleaning procedure is the cornerstone of non-surgical Periodontosis treatment. It involves the meticulous removal of plaque, calculus, and bacterial toxins from above and below the gumline (scaling) and smoothing the root surfaces (root planing) to eliminate rough spots where bacteria can accumulate. This reduces inflammation and allows the gums to reattach to the cleaned root surfaces.
- Oral Hygiene Instruction: Essential for long-term success, patients are taught proper brushing techniques (e.g., modified Bass technique), flossing, and the use of interdental brushes to control plaque buildup. Effective home care is vital for preventing recurrence and maintaining the results of Periodontosis treatment.
- Antimicrobial Rinses: Prescription mouthwashes containing chlorhexidine gluconate are often prescribed to reduce bacterial load, especially after SRP, or for maintenance. These rinses help control the bacterial populations responsible for the destruction seen in Periodontosis symptoms pictures.
- Local Antibiotics: For persistent or isolated deep pockets, antibiotics can be delivered directly into the periodontal pockets using gels, chips, or microspheres. These locally delivered antimicrobials help eliminate specific bacteria.
- Systemic Antibiotics: In cases of aggressive or rapidly progressing periodontosis, systemic antibiotics (e.g., amoxicillin, metronidazole, doxycycline) may be prescribed to combat generalized bacterial infection throughout the body, particularly when specific pathogenic bacteria are identified.
- Host Modulatory Agents: Low-dose doxycycline (subantimicrobial dose doxycycline) can be used as an adjunct to SRP. It inhibits destructive enzymes (matrix metalloproteinases) produced by the body in response to infection, thereby slowing tissue breakdown without exerting an antimicrobial effect.
- Regular Professional Cleanings (Maintenance Therapy): Following initial active Periodontosis treatment, a regular schedule of periodontal maintenance (usually every 3-4 months) is crucial. These appointments involve cleaning, re-evaluation of periodontal health, and reinforcement of oral hygiene practices.
- Surgical Periodontosis Treatment:
- Flap Surgery (Pocket Reduction Surgery): When non-surgical methods are insufficient, surgical intervention is necessary to access and clean deeper periodontal pockets and reshape bone. The gum tissue is lifted back (a flap is created) to allow direct visualization and thorough cleaning of root surfaces and removal of diseased tissue and bone. The flap is then repositioned and sutured. This procedure effectively reduces pocket depths, which are often prominent in advanced Periodontosis symptoms pictures.
- Bone Grafting: If significant bone loss has occurred (visible as extensive defects in Periodontosis symptoms pictures), bone grafts can be used to regenerate lost bone. Graft materials (autogenous, allogenic, xenogenic, or alloplastic) are placed into the bone defects to stimulate new bone growth and support the teeth.
- Guided Tissue Regeneration (GTR): This technique uses barrier membranes (resorbable or non-resorbable) to selectively block the fast-growing epithelial cells from migrating into the healing area, thereby allowing slower-growing bone, cementum, and periodontal ligament cells to regenerate. GTR aims to rebuild the lost supporting structures of the tooth.
- Soft Tissue Grafts (Gum Grafts): Used to treat gum recession and cover exposed root surfaces, which are common in Periodontosis symptoms pictures. Tissue can be taken from the palate or another donor source and grafted onto the affected area to cover roots, reduce sensitivity, and improve aesthetics.
- Crown Lengthening: Sometimes performed to expose more tooth structure for restorative procedures or to improve the gumline’s aesthetic appearance by removing gum tissue and/or bone. This can be relevant when uneven gum contours are part of the Periodontosis symptoms pictures.
- Hemisection or Root Resection: In multi-rooted teeth with severe furcation involvement or extensive bone loss around one root, the affected root may be surgically removed to save the remaining healthy portion of the tooth.
- Tooth Extraction: In cases of extreme bone loss, severe mobility, untreatable infection, or extensive destruction where saving the tooth is not feasible, extraction may be the only option. This prevents the spread of infection and allows for prosthetic replacement.
- Adjunctive and Supportive Therapies:
- Laser Therapy: Used as an adjunct to SRP, lasers can help remove diseased tissue and decontaminate pockets, potentially promoting healing and reducing bacterial load.
- Smoking Cessation: Smoking is a major risk factor and significantly impairs healing. Counseling and support for smoking cessation are critical components of Periodontosis treatment.
- Management of Systemic Conditions: For individuals with associated systemic diseases (as discussed in Skin rash Periodontosis Images), optimal management of conditions like diabetes or immune disorders is paramount for successful periodontal therapy outcomes.
- Nutritional Counseling: A balanced diet supports overall health and immune function, which is beneficial for periodontal health and healing.