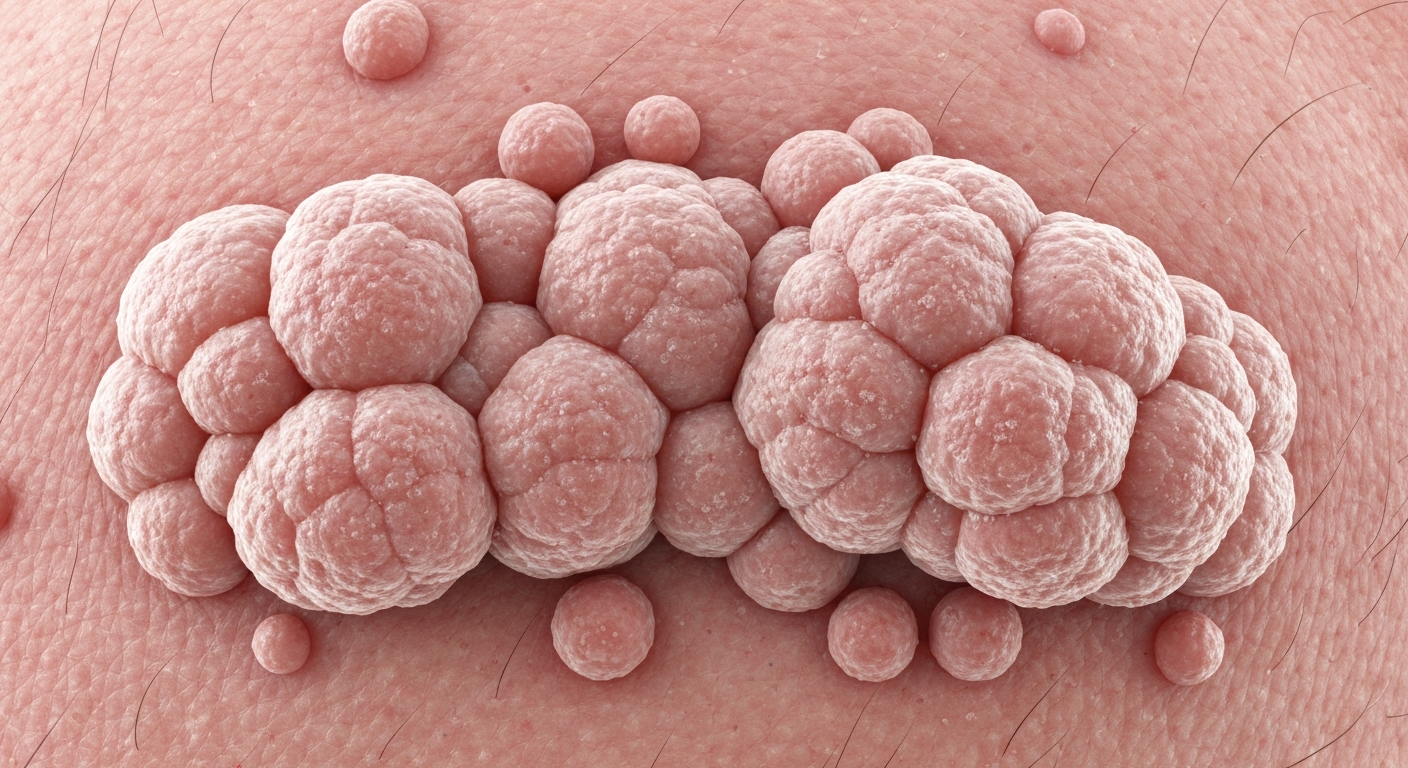
Condylomas symptoms pictures are crucial for understanding and identifying these common skin growths. This comprehensive guide details the diverse presentations of condylomas, offering insights into their varied appearances to aid in recognition.
Condylomas Symptoms Pictures
Understanding Condylomas symptoms pictures is paramount for early detection and management. Condylomas, also known as genital warts, present with a wide array of visual characteristics that can vary significantly based on their location, duration, and the individual’s immune response. These lesions are typically flesh-colored, pink, or brownish, but can also appear white or hyperpigmented, making their visual identification a nuanced process. Their texture can range from smooth and velvety to rough and verrucous, often described as cauliflower-like in more advanced stages. The sizes of condylomas are equally variable, starting as pinpoint papules and potentially growing into large, confluent masses that can obscure anatomical features. It is important to observe not only the primary morphology but also the distribution and any associated symptoms.
Common symptoms and visible characteristics associated with condylomas include:
- Papules: Small, raised bumps on the skin or mucous membranes. These are often the initial presentation, ranging from 1 mm to several millimeters in diameter.
- Nodules: Larger, firmer raised lesions that can be solitary or grouped.
- Plaques: Flat-topped, elevated areas formed by the coalescence of multiple papules, giving a broader, often irregular appearance.
- Verrucous appearance: A rough, warty, or cauliflower-like texture, particularly common in established lesions. This distinct morphology is a strong indicator of condylomas.
- Sessile or Pedunculated: Lesions can be broad-based (sessile) or attached by a stalk (pedunculated), especially noticeable in areas prone to friction.
- Color variations:
- Flesh-colored: Blending with surrounding skin, making them subtle.
- Pink or Reddish: Indicating increased vascularity or inflammation.
- White: Especially after exposure to moisture or in oral/mucosal areas.
- Brownish or Hyperpigmented: More common in individuals with darker skin tones or in older lesions.
- Itching (Pruritus): A common subjective symptom, particularly with larger or perianal lesions, leading to scratching and potential secondary infection.
- Burning or Discomfort: Sensations of irritation, especially in sensitive areas like the genitals or anus.
- Bleeding: Trauma to fragile warts, particularly during intercourse, defecation, or scratching, can cause minor bleeding.
- Pain: While often painless, larger or ulcerated lesions, or those in high-friction areas, can cause localized pain.
- Discharge: Rarely, extensive anogenital condylomas can be associated with an abnormal discharge, especially if secondary infection is present.
The distribution of condylomas is a critical diagnostic factor. They primarily affect anogenital regions but can also manifest in other areas. Specific locations where Condylomas symptoms pictures are frequently observed include:
- Genital Area (Males):
- Shaft of the penis
- Glans penis (head)
- Frenulum
- Coronal sulcus (groove behind the glans)
- Scrotum
- Pubic area
- Genital Area (Females):
- Labia majora
- Labia minora
- Clitoris
- Vaginal introitus (opening)
- Vaginal walls
- Cervix (often only visible during gynecological exam)
- Perineum (area between vagina and anus)
- Anorectal Area:
- Perianal skin (skin around the anus)
- Anal canal (internal lesions, often requiring anoscopy for visualization)
- Buttocks
- Oral Cavity:
- Lips
- Tongue
- Buccal mucosa (inner lining of cheeks)
- Palate (roof of the mouth)
- Oropharynx (back of the throat)
- Laryngeal Area:
- Vocal cords (can cause hoarseness or respiratory issues, especially in recurrent respiratory papillomatosis)
- Epiglottis
- Trachea
- Less Common Sites:
- Eyelids
- Conjunctiva
- Nasal cavity
- Axilla (armpit)
- Groin folds
- Digits (fingers and toes, particularly periungual)
The morphology and presentation can be highly variable, emphasizing the need for professional medical evaluation when any suspicious lesions appear. Observing the characteristic features in Condylomas symptoms pictures is an initial step, but confirmation requires clinical assessment.
Signs of Condylomas Pictures
When examining Signs of Condylomas Pictures, one must focus on the objective, observable characteristics that distinguish these lesions from other dermatological conditions. The clinical signs are what a healthcare provider specifically looks for during an examination, often using magnification or specific diagnostic aids. These signs are critical for accurate diagnosis and for differentiating condylomas from benign skin tags, molluscum contagiosum, or even more serious conditions.
Key observable signs in Condylomas Pictures include:
- Exophytic Growth: The lesions typically grow outwards from the skin surface, creating a raised profile. This is a hallmark sign, whether it’s a small papule or a large confluent mass.
- Verrucous (Warty) Surface: The irregular, rough, often fissured surface texture is highly characteristic. This can be more pronounced in older or larger lesions.
- Cauliflower-like Appearance: A descriptive term for aggregated, highly irregular, lobulated growths that mimic the texture of a cauliflower floret. This sign is almost pathognomonic for condylomas.
- Pink or Flesh-toned Hue: The predominant color, reflecting the vascularity and keratinization of the lesion. Variations to white or brownish are also common.
- Acetowhitening: This is a crucial diagnostic sign. Upon application of a 3-5% acetic acid solution (vinegar) for 5-10 minutes, HPV-infected epithelial cells, including those in condylomas, will turn white. This change is due to the acid dehydrating and coagulating cellular proteins, particularly those associated with increased nuclear density and keratinization, which are features of HPV infection.
- Intensity of Whitening: Denser, more active lesions tend to whiten more intensely and rapidly.
- Borders: The whitening often highlights the distinct borders of subclinical or flat lesions that might otherwise be invisible to the naked eye.
- Transient Nature: The acetowhite change is temporary, usually fading within minutes after the acid is removed.
- Multiple Lesions and Clustered Distribution: Condylomas often appear in groups or clusters, reflecting the localized spread of the human papillomavirus (HPV). They can be scattered across an area or coalesce into larger plaques.
- Location-Specific Signs:
- Penile Condylomas: Often found on the frenulum, coronal sulcus, or inner surface of the foreskin in uncircumcised males. They can be filiform (finger-like) or flat.
- Vulvar Condylomas: Commonly found on the labia majora and minora, vaginal introitus, and clitoris. They tend to be moist and can be irritated by clothing.
- Vaginal/Cervical Condylomas: Often flat or slightly raised, sometimes only detectable by colposcopy (magnified examination of the cervix/vagina) after acetowhitening.
- Perianal Condylomas: Frequently large, multiple, and can extend into the anal canal. They are often pruritic and can bleed, presenting as a significant concern for discomfort.
- Oral Condylomas: Typically solitary or few, appearing as small, raised, often whitish or pinkish papules on the lips, tongue, or buccal mucosa.
- Absence of Central Umbilication: This distinguishes condylomas from molluscum contagiosum, which characteristically has a central dimple.
- Non-Pustular Nature: Unlike bacterial infections or some forms of acne, condylomas do not typically contain pus unless secondarily infected.
Observing these specific signs in Condylomas Pictures, especially the characteristic verrucous morphology and the response to acetic acid, provides strong evidence for diagnosis. These visual cues are essential tools for clinicians in distinguishing condylomas from a broad range of dermatological differentials, thereby guiding appropriate treatment strategies and patient counseling. Regular self-examination and prompt medical consultation are advised for any suspicious skin changes, emphasizing the importance of recognizing these distinct visual signs.
Early Condylomas Photos
Recognizing Early Condylomas Photos is vital for timely intervention and preventing the spread and growth of lesions. In their initial stages, condylomas can be subtle and easily mistaken for other minor skin irregularities or even overlooked entirely. They often begin as very small, discrete papules that may not cause any symptoms like itching or pain, making visual identification challenging for the untrained eye. Early detection is key to managing HPV infection manifestations effectively.
Typical characteristics of Early Condylomas Photos include:
- Minute Papules:
- Size: Usually 1-2 mm in diameter, appearing as tiny, barely raised bumps.
- Color: Often flesh-colored, blending seamlessly with the surrounding skin, or very light pink. This makes them difficult to spot without close inspection.
- Texture: Initially smooth or slightly granular to the touch. The characteristic verrucous or cauliflower-like texture develops as the lesions mature and grow.
- Shape: Round or dome-shaped.
- Solitary or Few in Number: In the very early stages, lesions may appear as single, isolated bumps before spreading or coalescing.
- Subtle Appearance: They may lack the pronounced warty texture of more established lesions, making them appear more like small skin tags, moles, or even benign follicular papules.
- Location-Specific Early Presentations:
- Genital Skin: Small, flesh-colored bumps on the inner thighs near the genitals, pubic area, or surface of the labia/penis.
- Mucosal Surfaces: On moist areas like the vaginal introitus, inside the foreskin, or anal margin, they might appear as slightly whitish or translucent papules due to hydration.
- Asymptomatic Nature: Most early condylomas do not cause itching, pain, or discomfort, which often delays seeking medical attention. The absence of symptoms contributes to their silent progression.
- Growth Progression: Over weeks to months, if left untreated, these early papules will:
- Increase in Size: Grow larger in diameter and height.
- Increase in Number: New lesions may appear in the vicinity, indicating localized spread.
- Coalesce: Individual papules merge to form larger plaques or more extensive lesions.
- Develop Verrucous Texture: The surface becomes rougher, more irregular, and takes on the characteristic warty or cauliflower-like appearance.
- Acetowhitening as an Early Diagnostic Aid: Even subclinical or very early lesions that are not visible to the naked eye can turn acetowhite (white upon application of acetic acid). This technique is invaluable for identifying early HPV manifestations that would otherwise be missed.
It is crucial for individuals to be aware of any new or unusual bumps in anogenital or oral areas. Regular self-examination, particularly after bathing when skin is clean and relaxed, can aid in identifying these subtle early changes. When observing any suspicious bumps, especially those that persist or grow, consulting a healthcare professional is imperative. A clinician can perform a thorough examination, often using magnification (e.g., colposcopy or dermoscopy), and apply acetic acid to detect even the most nascent lesions. Early diagnosis and treatment of condylomas not only addresses the physical lesions but also contributes to preventing further transmission and potential complications, highlighting the significance of recognizing these initial presentations in Early Condylomas Photos.
Skin rash Condylomas Images
When examining Skin rash Condylomas Images, it’s important to understand that while condylomas are specific types of growths, extensive or numerous lesions can sometimes present in a manner that resembles a generalized skin rash. This can lead to confusion with other dermatological conditions, emphasizing the need for careful differential diagnosis. The “rash” appearance of condylomas typically occurs when multiple individual warts cluster closely together or coalesce into large plaques, covering a significant surface area of the skin or mucous membrane.
Characteristics of condylomas that can mimic a skin rash include:
- Widespread Distribution: Multiple lesions scattered across an anatomical region, rather than a single isolated growth. For instance, extensive perianal condylomas can cover the entire anal region and extend onto the buttocks, appearing as a broad, irregular rash.
- Confluent Plaques: Individual papules growing together to form larger, continuous patches. These plaques can have an uneven, bumpy, or verrucous surface, giving the impression of an abnormal skin texture rather than discrete warts.
- Erythema (Redness): While primary condylomas are often flesh-colored, associated irritation, inflammation, or secondary infection can lead to surrounding or intrinsic redness, making the area appear inflamed like a typical rash.
- Pruritus (Itching): Intense itching is a common symptom with condylomas, particularly in the anogenital region. Persistent scratching can lead to excoriations, lichenification (thickening of the skin), and further inflammation, which can mimic chronic eczematous rashes.
- Moisture and Maceration: In intertriginous areas (skin folds), condylomas can become macerated (softened and whitened by moisture) and irritated, leading to a raw, rash-like appearance that might be confused with fungal infections or intertrigo.
Differentiating Skin rash Condylomas Images from other conditions requires careful clinical evaluation. Here are key distinctions:
- Molluscum Contagiosum:
- Condylomas: Verrucous, irregular surface, often cauliflower-like.
- Molluscum: Smooth, dome-shaped papules with a characteristic central umbilication (dimple).
- Herpes Simplex Virus (HSV) Lesions:
- Condylomas: Solid papules/warts, persistent.
- HSV: Clustered vesicles (blisters) on an erythematous base, which then ulcerate and crust over, recurrent episodes.
- Syphilis (Condyloma Lata):
- Condylomas: Verrucous, often pedunculated, firm.
- Condyloma Lata: Broad, flat-topped, moist, gray-white lesions, highly contagious, associated with secondary syphilis. Serological tests confirm syphilis.
- Skin Tags (Acrochordons):
- Condylomas: Warty, often multiple, may respond to acetic acid.
- Skin Tags: Soft, fleshy, pedunculated papules, typically smooth, not associated with HPV infection in the same manner.
- Seborrheic Keratoses:
- Condylomas: Found predominantly in anogenital/oral areas, often verrucous.
- Seborrheic Keratoses: “Stuck-on” appearance, greasy, waxy, often pigmented, common on trunk and face, not limited to anogenital area.
- Lichen Planus:
- Condylomas: Warty, often exophytic.
- Lichen Planus: Pruritic, polygonal, purple, planar papules and plaques. Oral lichen planus has characteristic Wickham’s striae (white lacy network).
- Psoriasis (Inverse Psoriasis):
- Condylomas: Warty, generally not scaly in typical presentation.
- Inverse Psoriasis: Smooth, red, well-demarcated plaques without typical scaling, found in skin folds.
- Squamous Cell Carcinoma (SCC) or Bowenoid Papulosis:
- Condylomas: Benign warty lesions.
- SCC/Bowenoid Papulosis: May clinically mimic condylomas but are precancerous or cancerous. Biopsy is essential for definitive diagnosis.
When confronted with a rash-like presentation in the anogenital or oral region, especially one that is persistent, growing, or unusual, clinical suspicion for condylomas should be high. The characteristic verrucous texture, response to acetic acid, and the presence of satellite lesions are strong indicators. A healthcare provider will perform a thorough visual inspection, potentially use dermoscopy, and may perform a biopsy if there is any diagnostic uncertainty or concern for malignancy. Relying solely on generalized “Skin rash Condylomas Images” can be misleading without professional medical assessment.
Condylomas Treatment
While this article primarily focuses on Condylomas symptoms pictures and identification, understanding the available treatment options is a crucial component of comprehensive management. The goal of condylomas treatment is to remove visible lesions, alleviate symptoms, and prevent further spread, though it does not eradicate the underlying human papillomavirus (HPV) infection itself. Therefore, recurrence is common. Treatment selection depends on several factors, including the size, number, location, and morphology of the warts, patient preference, cost, and the clinician’s experience. A combination of approaches is sometimes employed.
Treatment modalities for condylomas can be broadly categorized into patient-applied topical therapies and clinician-applied therapies.
Patient-Applied Topical Therapies:
- Imiquimod Cream (Aldara, Zyclara):
- Mechanism: An immune response modifier that stimulates the body’s immune system to produce interferon and other cytokines, which then attack the HPV-infected cells.
- Application: Applied by the patient to the warts typically 3 times a week (Aldara) or daily for a limited duration (Zyclara) before bedtime, washed off in the morning.
- Side Effects: Local skin reactions such as erythema, erosion, flaking, itching, and burning are common. Systemic flu-like symptoms are rare.
- Efficacy: Effective for external genital and perianal warts, with clearance rates ranging from 50-70%.
- Podofilox Solution or Gel (Condylox):
- Mechanism: An antimitotic agent that inhibits cell division, leading to necrosis of the wart tissue.
- Application: Applied by the patient twice daily for 3 consecutive days, followed by 4 days of no treatment. This cycle is repeated for up to 4-6 weeks.
- Side Effects: Local irritation, erosion, pain, inflammation, and burning are frequent.
- Efficacy: Generally effective for small to medium-sized external warts. Not for internal or extensive use due to systemic absorption risk.
- Sinecatechins Ointment (Veregen):
- Mechanism: A green tea extract with antioxidant and antiviral properties, thought to inhibit HPV growth and proliferation.
- Application: Applied three times daily to the warts until complete clearance or for up to 16 weeks.
- Side Effects: Local reactions like erythema, itching, burning, pain, and ulceration.
- Efficacy: Indicated for external genital and perianal warts.
Clinician-Applied Therapies:
- Cryotherapy (Liquid Nitrogen):
- Mechanism: Freezing the warts with liquid nitrogen, causing cellular destruction and blistering, followed by sloughing of the wart tissue.
- Application: Applied by a clinician using a spray or cotton swab. Repeated every 1-2 weeks for several sessions.
- Side Effects: Pain, blistering, ulceration, temporary hypopigmentation or hyperpigmentation.
- Efficacy: Highly effective for external and some internal warts, suitable for most locations.
- Trichloroacetic Acid (TCA) or Bichloroacetic Acid (BCA):
- Mechanism: A strong chemical acid that causes chemical coagulation and necrosis of the wart proteins.
- Application: Applied directly to the warts by a clinician, usually weekly.
- Side Effects: Pain, burning, ulceration. Care must be taken to protect surrounding healthy skin.
- Efficacy: Effective for small, moist warts. Can be used for vaginal or cervical warts by experienced clinicians.
- Surgical Excision:
- Mechanism: Physical removal of the warts using a scalpel, scissors, or curette.
- Application: Performed under local anesthesia. Can be used for solitary or large lesions, or those resistant to other treatments.
- Side Effects: Pain, scarring, infection, bleeding.
- Efficacy: Provides immediate clearance, lower recurrence rates for excised lesions. Useful for diagnostic biopsy.
- Electrocautery:
- Mechanism: Burning the warts using an electrically heated probe, coagulating and destroying the tissue.
- Application: Performed under local anesthesia.
- Side Effects: Pain, scarring, smoke plume with potential HPV transmission risks.
- Efficacy: Effective for various sizes and numbers of warts.
- Laser Therapy (CO2 Laser):
- Mechanism: Uses a concentrated beam of light to vaporize wart tissue.
- Application: Performed under local or general anesthesia, especially for extensive or recurrent warts, or in sensitive areas.
- Side Effects: Pain, scarring, post-operative discomfort, smoke plume.
- Efficacy: Very effective for extensive or difficult-to-treat warts, including urethral or anal canal lesions.
- Intralesional Interferon Injections:
- Mechanism: Direct injection of interferon into the warts to stimulate a localized antiviral immune response.
- Application: Less commonly used now due to systemic side effects and availability of other effective treatments.
- Side Effects: Flu-like symptoms, pain at injection site.
- Efficacy: Can be effective for some resistant warts.
Other Considerations for Condylomas Treatment:
- No Cure for HPV: It is crucial for patients to understand that treating the warts removes the visible lesions but does not eradicate the HPV virus from the body, meaning new warts can emerge.
- Recurrence: Warts can recur within months of treatment, even with successful clearance. Follow-up examinations are necessary.
- Prevention: HPV vaccination (Gardasil 9) is highly effective in preventing infection with the types of HPV that cause most genital warts and several HPV-related cancers. Consistent condom use can reduce, but not eliminate, the risk of transmission.
- Treatment in Pregnancy: Certain treatments are contraindicated during pregnancy (e.g., podofilox, imiquimod). Surgical removal or cryotherapy are often preferred options.
- Immunocompromised Individuals: Patients with weakened immune systems (e.g., HIV-positive) may have more extensive, aggressive, and recalcitrant warts, requiring more intensive and prolonged treatment.
The choice of Condylomas treatment should always be made in consultation with a healthcare professional, considering the individual circumstances and the appearance seen in Condylomas symptoms pictures. Effective management involves not only treating existing lesions but also counseling patients on prevention and the potential for recurrence.