Understanding the visual characteristics of severe foot conditions is crucial for accurate assessment and management. This article offers an in-depth look into Grade 3 flat feet symptoms pictures, providing detailed descriptions of the visual cues and physical manifestations associated with this advanced foot deformity.
Grade 3 flat feet Symptoms Pictures
When examining Grade 3 flat feet symptoms pictures, a trained eye immediately recognizes the profound structural changes and compensatory patterns indicative of severe arch collapse. Patients experiencing Grade 3 flat feet often report a constellation of debilitating symptoms, many of which have visible correlates. These symptoms are not merely discomforts but represent significant biomechanical failure, severely impacting mobility and quality of life. The visual presentation of these symptoms can be stark and informative, guiding both diagnosis and patient education regarding severe flatfoot deformity.
The primary symptom, almost universally reported, is chronic foot pain. This pain can manifest in several areas, and its location often provides clues about the underlying structural damage. In pictures, areas of swelling, redness, or calluses can sometimes highlight the most painful zones and regions of highest stress. Common locations for pain associated with Grade 3 flat feet include:
- Medial Arch Pain: A deep, aching sensation along the inner aspect of the foot, precisely where the medial longitudinal arch should be. In Grade 3 flat feet images, this area appears significantly flattened, often making extensive contact with the ground or showing visible signs of chronic pressure and skin thickening. The pain here is frequently linked to the stretching and eventual failure of critical supporting structures, most notably the posterior tibial tendon and the spring ligament. This severe pronation pain can be disabling.
- Heel Pain (Plantar Fasciitis or Achilles Tendinopathy): Pain under the heel (plantar heel pain) or at the back of the heel (posterior heel pain). The altered gait mechanics, including excessive pronation and hindfoot valgus, significantly increase stress on the plantar fascia attachment and the Achilles tendon insertion. Visual inspection might reveal swelling around the Achilles insertion or tenderness upon palpation, sometimes accompanied by visible heel spurs on imaging.
- Ankle Pain: Often felt intensely on the inner aspect (medial ankle) due to impingement, chronic strain on the deltoid ligament complex, or excessive stretch and inflammation of the posterior tibial tendon. Lateral ankle pain can also occur from compensatory impingement of the fibula against the calcaneus. Pictures of Grade 3 flat feet frequently show a prominent medial malleolus and a visible bulge of soft tissues inferior to it, indicating the degree of talar head displacement and the considerable stress placed on the ankle joint and its supporting ligaments.
- Lateral Foot Pain: Pain along the outside of the foot, which can result from several factors, including the cuboid bone being compressed against the calcaneus (nutcracker effect) due to persistent forefoot abduction, or from the stretch and inflammation of the peroneal tendons as they attempt to stabilize the collapsing arch. This can manifest as visible tenderness on the outside of the foot.
- Lower Leg Fatigue and Pain: Patients frequently describe an overwhelming fatigue, cramping, or aching sensation in their calves and shins after even short periods of standing or walking. This is due to the constant, compensatory overactivity of muscles (like the peroneal muscles) attempting to stabilize the profoundly unstable foot. While not directly visible, the consequence can be observed in a visibly altered, less efficient gait pattern and muscle guarding.
- Knee, Hip, and Lower Back Pain: The severe collapse of the foot arch creates a profound kinetic chain effect, propagating abnormal biomechanics upwards. This leads to altered alignment and increased stress in more proximal joints. Patients may develop or experience worsening of knock-knees (genu valgum), internal rotation of the tibias, and even compensatory pelvic tilt or changes in spinal alignment, all of which can be observed in full-body postural images and contribute to chronic pain in these areas.
Beyond pain, other prominent symptoms with visual correlates offer further diagnostic clues in Grade 3 flat feet pictures:
- Pronounced Arch Collapse: This is the single most defining visual symptom. The medial longitudinal arch is almost entirely absent, with the entire sole of the foot appearing to make extensive, if not complete, contact with the ground. In Grade 3 flat feet photos, this complete collapse is unmistakable, often accompanied by a visible sag or medial prominence of the navicular bone and talar head, making the midfoot appear outwardly convex.
- Visible Swelling: Often consistently present around the medial ankle and along the course of the posterior tibial tendon. This swelling indicates ongoing inflammation and degenerative changes in the severely stretched and often ruptured or dysfunctional supporting structures. Images illustrating Grade 3 flat feet can clearly show soft tissue fullness, edema, and sometimes mild erythema in these chronically stressed regions.
- Difficulty with Footwear: Patients with severe pes planus struggle significantly with finding comfortable and supportive shoes. Shoes often wear out unevenly and rapidly, with excessive wear on the inner sole and heel. The medial upper of the shoe is frequently stretched, bulged, or collapsed. Pictures of worn shoes from Grade 3 flat feet patients graphically demonstrate this abnormal wear pattern, providing powerful visual evidence of the foot’s compromised mechanics and the challenges faced daily.
- Instability and Balance Issues: While not a direct visual symptom itself, the feeling of profound foot and ankle instability can lead to observable compensatory movements, an unsteady or shuffling gait, and frequent stumbles. Patients often describe feeling like their ankle is “giving way” or that they walk on the sides of their feet. This leads to a visibly cautious and altered walking pattern.
- Limited Range of Motion and Rigidity: Especially in the subtalar joint. This rigidity implies that the deformity is fixed and cannot be corrected manually or with active muscle contraction (e.g., standing on tiptoes). This can be observed during physical examination where specific joint movements are severely restricted or absent. In some Grade 3 flat feet images, the foot may appear stiff and less adaptable, maintaining its deformed shape even when non-weight-bearing.
- Increased Forefoot Width and Abduction: Due to significant forefoot abduction (the front of the foot splaying outwards), the foot often appears visibly wider and longer, leading to distinct pressure points and potential development of associated toe deformities. This visual widening compounds shoe fitting difficulties.
- Audible Clicking or Popping: While not visible, some patients report these sounds, indicating joint instability or tendon subluxation, which can sometimes be inferred from visible joint changes and palpation.
Each of these symptoms paints a comprehensive picture of the patient’s experience with Grade 3 flat feet, highlighting the severe impact of this condition. Visual documentation through Grade 3 flat feet symptoms pictures provides invaluable diagnostic and educational information, assisting healthcare providers in accurately assessing the severity of the collapsed arch foot and planning appropriate interventions for severe PTTD.
Signs of Grade 3 flat feet Pictures
The objective signs observed in Grade 3 flat feet pictures are critically diagnostic and unequivocally reveal the extent of the deformity and the severity of structural compromise. These are physical manifestations that can be directly observed by a clinician or clearly seen in photographic documentation, offering crucial insights into the rigidity, severity, and structural failures of the foot. Understanding these visual signs is fundamental for accurate diagnosis, precise classification, and effective treatment planning for severe flatfoot deformity or advanced posterior tibial tendon dysfunction (PTTD).
Key Visual Signs in Static Standing (Weight-Bearing) Positions:
- Pronounced Medial Longitudinal Arch Collapse: In Grade 3 flat feet images, the most striking and undeniable feature is the near-complete, often complete, obliteration of the medial longitudinal arch. The entire sole of the foot, from the heel to the ball, frequently makes full, broad contact with the ground. This extensive and usually rigid collapse is the hallmark of advanced pes planus deformity, distinguishing it from less severe forms of flatfoot.
- Hindfoot Valgus (Severe Heel Eversion): The heel bone (calcaneus) is visibly and severely everted or angled outwards. When viewed from behind, the Achilles tendon often appears to bow outwards (the “bowstring sign” or “Haglund’s deformity”), and the heel is clearly angled laterally relative to the lower leg. This severe eversion indicates significant failure of the medial supporting structures and profound instability of the hindfoot, a critical sign of severe flatfoot instability.
- Forefoot Abduction: The forefoot (the front part of the foot including the toes and metatarsals) appears dramatically splayed outwards relative to the hindfoot. This external rotation of the forefoot is a key component of the overall deformity and directly contributes to the characteristic “too many toes” sign.
- “Too Many Toes” Sign: This is a highly specific and easily recognizable visual indicator. When viewing the patient from directly behind, more than the usual one or two toes (typically three or more, often all five) are clearly visible on the outside (lateral aspect) of the affected foot. This sign is a direct and unmistakable consequence of the combined effects of severe forefoot abduction and hindfoot valgus, where the forefoot rotates externally, bringing a greater number of the lateral toes into view from the posterior perspective. This sign is unequivocally present in Grade 3 flat feet photos.
- Medial Ankle Bulging/Prominence: There is a distinct and often significant bulging or prominence of the talar head and navicular bone on the medial side of the ankle and midfoot. This occurs because the talus collapses medially and downwards out of the ankle mortise, and the navicular bone loses its proper articulation with the talus, becoming visibly displaced and prominent. This visual cue is crucial for identifying the extent of posterior tibial tendon dysfunction (PTTD), spring ligament laxity, and overall midfoot collapse.
- Achilles Tendon Deviation: As previously mentioned, the Achilles tendon often presents with a noticeable lateral curve or deviation, following the outward angle of the heel bone (hindfoot valgus). This visual deviation can indicate chronic stress and altered biomechanical pull on the tendon.
- Midfoot Sag/Breaking: The midfoot region, specifically around the talonavicular and naviculocuneiform joints, often appears to “break” or sag medially, forming a distinctly convex bulge on the inner aspect of the foot instead of the normal concave arch. This visual “breaking” point signifies significant collapse and instability in the central region of the foot.
- Foot Length and Width Changes: Due to the extensive splaying and collapse, the foot may appear visibly longer and significantly wider compared to the unaffected foot (if unilateral) or compared to a normative foot. These visual changes can be quantitatively measured but are also apparent in high-resolution Grade 3 flat feet images.
- Associated Postural Changes: In severe, long-standing cases of Grade 3 flat feet, the compensatory chain reaction can extend proximally, leading to visible knock-knees (genu valgum), internal rotation of the tibias, and even compensatory pelvic tilt or changes in spinal alignment (e.g., scoliosis). Full-body posture pictures can reveal these cascading systemic effects, highlighting the global impact of the foot deformity.
Key Visual Signs in Dynamic (Movement) or Non-Weight-Bearing Positions:
- Inability to Perform a Single Heel Raise (Jack Test Failure or Too Many Toes Test in Dynamic View): When asked to stand on one foot and perform a single heel raise, a patient with Grade 3 flat feet will typically be unable to invert their heel to form an arch. The heel remains in a fixed valgus position, and the arch does not reappear or only minimally reduces, demonstrating a rigid or very severely flexible deformity. This is a critical functional sign often captured in a series of images or video, differentiating rigid flatfoot from flexible flatfoot.
- Altered Gait Pattern: Observational gait analysis will reveal profound and persistent excessive pronation throughout the stance phase, often with a distinctly “flat-footed” or “shuffling” appearance. There is often a noticeable lack of a strong propulsive push-off from the forefoot, with the patient struggling to get onto their toes. The foot appears to remain pronated throughout the entire gait cycle, and the foot may “slap” on the ground. Visual gait analysis provides critical insights into the functional limitations.
- Limited Subtalar Joint Inversion: When the foot is manually manipulated in a non-weight-bearing position, there will be significantly restricted or completely absent subtalar joint inversion, indicating a rigid deformity. This lack of passive correctability is a hallmark of severe, fixed flatfoot and can be demonstrated in examination photos.
- Calluses, Corns, and Other Skin Lesions: Visual evidence of abnormal pressure points, such as thick, often painful calluses, is very common. These are typically found on the medial aspect of the sole, under the collapsed arch, or on the plantar aspect of the metatarsal heads due to altered weight distribution. Corns can appear on the dorsal surfaces of the toes due to compensatory toe deformities like hammertoes or claw toes, rubbing against footwear. These skin changes are direct visual signs of chronically compromised foot mechanics and excessive localized pressure.
Each of these objective signs, when documented through meticulously captured Grade 3 flat feet pictures, contributes to a comprehensive clinical picture, allowing for precise diagnosis, staging of the deformity, and guiding subsequent management strategies for this complex and debilitating condition. The visual evidence provides irrefutable proof of the advanced nature of the foot collapse and its far-reaching consequences.
Early Grade 3 flat feet Photos
The concept of “early Grade 3 flat feet” is nuanced, as Grade 3 by definition represents a severe, often rigid, end-stage deformity where significant structural collapse has occurred. However, “early Grade 3” can be interpreted as the critical transitional phase where a less severe flatfoot (typically Grade 2, characterized by a flexible deformity with moderate arch collapse) progresses to the profound structural and functional compromises characteristic of a rigid Grade 3 deformity. It can also refer to the initial presentation of symptoms and signs that clearly indicate the progression towards or establishment of a severe, potentially rigid, deformity. Documenting these transitional visual changes through early Grade 3 flat feet photos is vital for understanding disease progression and intervening effectively before complete and irreversible rigidity sets in, making treatment significantly more challenging for progressive flatfoot deformity.
During this critical progression towards Grade 3, several visual changes become increasingly apparent and pronounced:
- Worsening and Persistent Arch Collapse: While some arch collapse may have been present in earlier, flexible stages, in early Grade 3 flat feet images, the medial longitudinal arch shows a significant, almost complete, obliteration. The midfoot region that might have previously shown a partial or reducible arch now visibly sags and makes substantial, consistent ground contact, even when the patient attempts to actively engage foot muscles. This is a clear visual progression from a flexible to an increasingly rigid collapse, indicating ligamentous and capsular tightening in the deformed position.
- Increasing and Less Reducible Hindfoot Valgus: The outward angling of the heel (hindfoot valgus) becomes more pronounced and less easily corrected, either actively by the patient or passively by an examiner. If previously it was a subtle or partially reducible deviation, it now presents as a clear, consistent eversion of the calcaneus, even with attempts to correct it manually. The Achilles tendon’s “bowstring” effect becomes more evident and less amenable to simple stretching.
- More Prominent “Too Many Toes” Sign: As forefoot abduction increases due to the progressive collapse, the visibility of lateral toes from a posterior view becomes more striking and consistent. What might have been only one or two toes visible in earlier stages now clearly shows three or more, often all five, indicating a worsening external rotation of the forefoot. This visual sign becomes a constant feature in weight-bearing.
- Persistent and Irreducible Medial Ankle Bulging: The prominence of the talar head and navicular on the inner aspect of the ankle and midfoot becomes more constant, larger, and significantly less reducible. This visual sign reflects increasing laxity or complete failure of the medial supporting structures, particularly the spring ligament and a degenerating posterior tibial tendon, leading to significant talar displacement.
- Early Signs of Rigidity (Failure of Jack Test/Single Heel Rise): This is a key differentiator. Initially, a flatfoot might be flexible, meaning the arch reappears when the patient stands on tiptoes or when the foot is non-weight bearing. In early Grade 3 flat feet photos, attempts to perform a single heel raise will show the arch failing to reform, or only partially forming, and the heel remaining largely in valgus. This inability to actively invert the heel and restore the arch indicates the transition to a more rigid or semi-rigid deformity, where soft tissue contractures and bony adaptations prevent correction.
- Developing Soft Tissue Inflammation and Tendinopathy: Early signs of chronic inflammation, such as subtle but persistent swelling, localized redness, or increased skin temperature around the posterior tibial tendon path or medial ankle, may become more consistent. This indicates ongoing irritation, chronic tenosynovitis, and potential degeneration of the tendon, characteristic of advancing PTTD stages.
- Alterations in Gait Becoming More Apparent and Debilitating: While minor gait abnormalities might be present in earlier stages, in the transition to Grade 3, the gait becomes distinctly “flat-footed,” with a significantly reduced push-off phase, a visibly clumsy foot placement, and a noticeable tendency for the foot to roll inwards excessively throughout the entire stance phase. The patient’s walk may appear labored or shuffling. This can be captured in sequential video or multiple static images during different phases of walking, revealing the functional decline.
- Formation of Early Compensatory Deformities: As the primary foot structure collapses, the forefoot and toes begin to compensate in increasingly visible ways. Early Grade 3 flat feet pictures might show the initial formation of bunions (hallux valgus) or more pronounced hammertoe/claw toe deformities due to altered biomechanics, muscle imbalances, and increased pressure in the toe box. These are visible indicators of the cascading effect of the primary flatfoot deformity.
- Exacerbated Changes in Shoe Wear Patterns: While previously subtle, wear on the medial sole and heel of shoes becomes more rapid and dramatically pronounced. The medial upper of the shoe shows visible stretching, bulging, or complete collapse as the foot sways inward. Documenting these heavily worn shoe patterns provides powerful visual evidence of progression and the immense strain placed on footwear.
Monitoring these evolving visual cues through serial early Grade 3 flat feet photos is crucial for early detection of progression to a severe and rigid deformity, allowing for timely and potentially less invasive interventions to prevent complete and irreversible structural changes and to manage severe foot pain effectively.
Skin rash Grade 3 flat feet Images
While Grade 3 flat feet is fundamentally a complex musculoskeletal condition involving bone alignment, joint integrity, and tendon function, its severe biomechanical distortions and significantly altered pressure distribution can lead to a variety of secondary skin manifestations. These are not true “rashes” in the dermatological sense of an intrinsic skin disease, but rather skin irritations, hypertrophies, or lesions that arise directly from the chronic mechanical stress, excessive friction, abnormal shear forces, and altered moisture environment inherent in a severely pronated and collapsed foot. Documenting these specific changes with skin rash Grade 3 flat feet images provides important visual clues about the specific areas of highest stress, friction, and potential complications, guiding comprehensive patient management for severe foot deformity.
Here are the common secondary skin manifestations, often visible, observed in patients with Grade 3 flat feet:
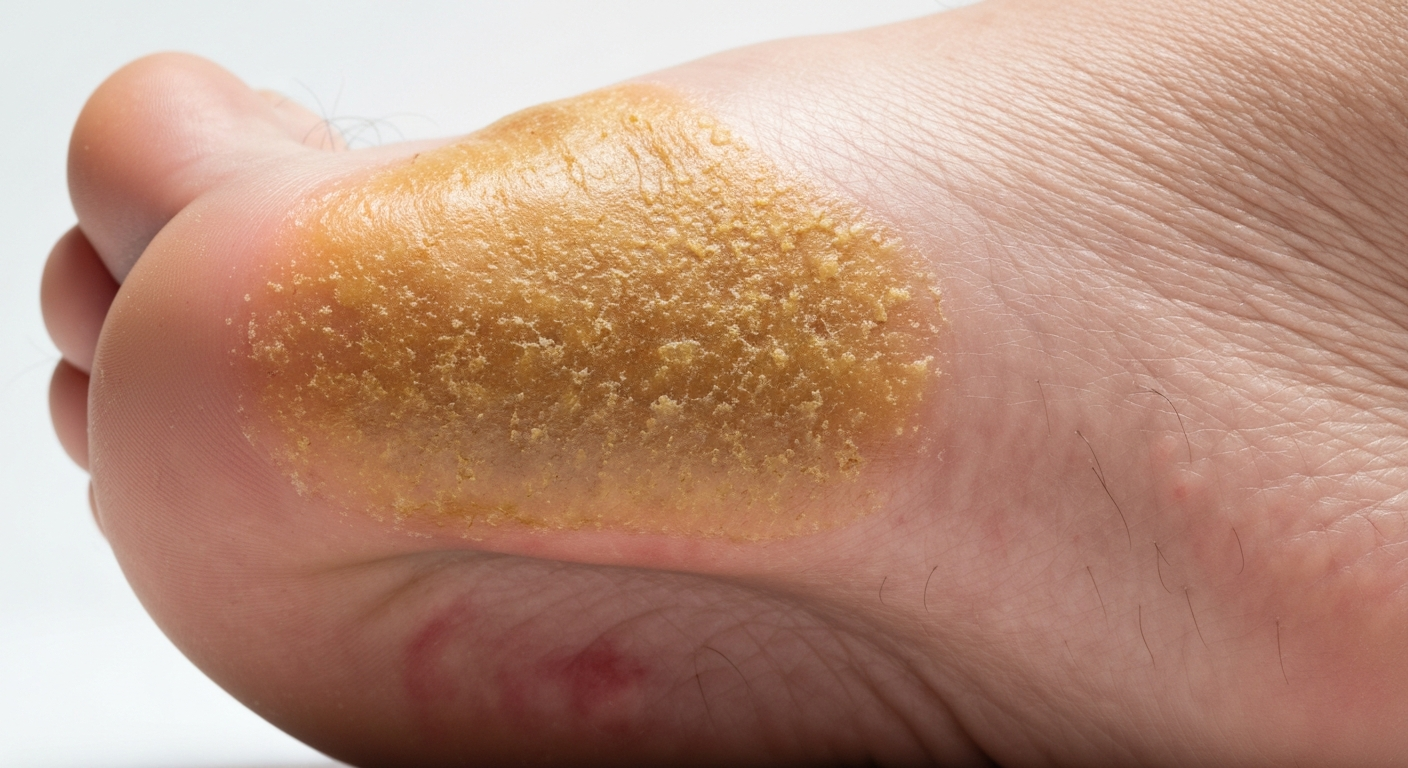
- Hyperkeratosis (Calluses):
- Appearance: Thickened, hardened patches of skin, often appearing yellowish, brownish, or even grayish. They are usually rough to the touch and can be painful, especially when compressed.
- Location: Frequently found on the plantar aspect of the foot, particularly under the collapsed medial longitudinal arch where it makes abnormal contact with the ground (e.g., under the prominent talar head or navicular prominence). They also commonly appear under the metatarsal heads (especially the second, third, and fourth) due to altered weight distribution and forefoot splaying, and sometimes on the medial side of the great toe.
- Cause: Chronic, excessive, and abnormal pressure and friction from the foot’s altered contact with the ground or ill-fitting footwear. In Grade 3 flat feet pictures, these calluses are prominent and unmistakable visual indicators of high-pressure zones, highlighting areas of severe biomechanical stress on the skin.
- Corns (Helomas Dura and Molle):
- Appearance: Small, localized, conical areas of extremely thickened skin, often with a central core, and typically painful when pressed. Hard corns (heloma durum) appear as hard, dense bumps. Soft corns (heloma molle) are whitish, macerated, and rubbery due to moisture, typically found between toes.
- Location: Hard corns are commonly seen on the dorsal surface of the toes (especially the lesser toes) where hammertoe or claw toe deformities cause them to rub against the shoe. Soft corns are most often located between the fourth and fifth toes.
- Cause: Intense, localized pressure and friction from footwear exacerbated by toe deformities (which are frequently secondary to the splaying and collapse of the Grade 3 flat foot) and abnormal toe alignment. Images of severe flat feet often reveal these associated toe deformities and the overlying corns.
- Blisters (Bullae and Vesicles):
- Appearance: Fluid-filled sacs on the skin surface (vesicles are small, bullae are large). They can be clear, bloody, or purulent if infected.
- Location: Any area subjected to intense, acute friction and shear forces, such as the medial arch, heel, or areas rubbing against ill-fitting shoes (e.g., shoe seams, tight toe box).
- Cause: Excessive shearing forces between the skin and footwear, which is highly common in a foot with abnormal biomechanics and altered movement patterns characteristic of Grade 3 flat feet. These are often present in Grade 3 flat feet images, particularly after increased activity, indicating poor shoe fit, inadequate support, or excessive movement within shoes.
- Maceration and Fungal Infections (Tinea Pedis/Athlete’s Foot):
- Appearance: Maceration appears as softened, whitish, wrinkled, and fragile skin, often with a distinct, sometimes foul odor. Fungal infections (tinea pedis) might present with varying degrees of redness (erythema), scaling, flaking, itching, peeling, and sometimes small blisters.
- Location: Frequently between the toes (interdigital spaces), in the collapsed medial arch area where skin-on-skin contact occurs, and in the general plantar region due to increased sweating and poor air circulation.
- Cause: The severe pronation of Grade 3 flat feet can lead to increased sweating, reduced air circulation, and chronic moisture accumulation in the collapsed arch and between the digits. This warm, moist environment is highly conducive to bacterial and fungal growth, leading to maceration and infections. Skin changes in Grade 3 flat feet photos might clearly show this damp, irritated, or infected appearance.
- Bunions (Hallux Valgus) and Bunionettes (Tailor’s Bunion):
- Appearance: A visibly prominent bony bump on the medial side of the base of the big toe (bunion) or on the lateral side of the base of the little toe (bunionette). The skin overlying these prominences can be red, inflamed, swollen (bursitis), shiny, and even ulcerated in severe, chronic cases due to constant shoe pressure.
- Location: Medial aspect of the first metatarsophalangeal joint (bunion) or lateral aspect of the fifth metatarsophalangeal joint (bunionette).
- Cause: While bunions have a complex etiology, the forefoot abduction, splaying, and altered weight-bearing associated with Grade 3 flat feet significantly contribute to their development, progression, and aggravation, leading to visible skin irritation, inflammation, and potential breakdown over the bony prominences.
- Skin Discoloration/Hyperpigmentation:
- Appearance: Darkening of the skin, often a brownish or reddish-brown hue.
- Location: Areas of chronic inflammation, edema (swelling), or persistent pressure. Commonly seen around the medial ankle or lower leg in the presence of chronic venous insufficiency, which can be exacerbated by long-standing foot deformity and altered gait.
- Cause: Long-standing edema and inflammation can lead to hemosiderin staining (from red blood cell breakdown) or post-inflammatory hyperpigmentation. This is a subtle but noticeable change in skin Grade 3 flat feet images over time.
- Ulceration (Pressure Sores/Diabetic Foot Ulcers):
- Appearance: Open sores, wounds, or breaks in the skin, ranging from superficial to deep, often with exposed underlying tissue.
- Location: Typically over bony prominences that experience extreme, chronic pressure (e.g., talar head prominence, metatarsal heads, lateral aspect of the fifth metatarsal) or areas of significant friction, especially if sensation is compromised (e.g., in diabetic patients with neuropathy).
- Cause: While less common in flat feet alone, severe, neglected Grade 3 flat feet with associated rigid deformities, prominent bony structures, and neuropathic or vascular compromise can lead to pressure ulcers. This represents a serious and sight-threatening complication, and wound Grade 3 flat feet images would depict significant tissue damage, often requiring urgent medical attention.
It is crucial to understand that these are secondary skin manifestations resulting from the mechanical stresses imposed by the severe foot deformity, rather than a primary “rash” in the dermatological sense. Identification and thorough documentation of these visible skin changes in Grade 3 flat feet images is essential for comprehensive patient care, as they often require specific local treatment in addition to addressing the underlying biomechanical issue and flatfoot surgical correction.
Grade 3 flat feet Treatment
The treatment of Grade 3 flat feet, particularly when the deformity is rigid or associated with advanced posterior tibial tendon dysfunction (PTTD), is complex and frequently necessitates surgical intervention due to the severity of the structural collapse and the profound impact on function and quality of life. However, a comprehensive management approach often begins with or incorporates non-surgical strategies, especially to manage symptoms, prepare for surgery, or support the foot post-operatively. The ultimate goal of any treatment for severe flatfoot deformity is to alleviate pain, improve foot mechanics, enhance stability, and restore a functional alignment, with visible outcome and functional improvement being primary objectives.
Non-Surgical Management (Visual Impact & Treatment Goals for Severe Flatfoot):
Non-surgical treatments aim to support the foot, redistribute pressure, and reduce symptoms. While they rarely correct a rigid Grade 3 flatfoot, they are crucial for symptomatic relief and preparing the patient for potential surgery.
- Custom Foot Orthotics and Bracing:
- Visual: Custom-molded orthotics are meticulously designed to provide robust support to the medial longitudinal arch, effectively control hindfoot valgus, and minimize forefoot abduction. In Grade 3 flat feet treatment pictures, one can clearly observe the orthotic device actively lifting the arch and correcting the heel position within the shoe, aiming to recreate a more functional foot posture. For more severe cases, or those with significant instability, an Ankle-Foot Orthosis (AFO) might be prescribed. These larger braces visibly stabilize the entire ankle-foot complex, preventing excessive pronation during gait and providing a higher degree of control.
- Goal: Reduce pain by offloading stressed structures, improve dynamic stability, evenly redistribute plantar pressure (thereby reducing callus formation), and prevent further progression of the deformity, especially in severe flexible deformities transitioning to rigidity. They generally improve comfort and function, though they do not typically restore the arch to a truly normal position in a rigid Grade 3 foot.
- Appropriate Footwear:
- Visual: Patients are strongly advised to wear sturdy, supportive shoes with specific features: a deep toe box to accommodate forefoot splaying and potential toe deformities, a firm heel counter to stabilize the hindfoot, and integrated or removable arch support to complement orthotics. Pictures of recommended footwear for Grade 3 flat feet contrast significantly with minimalist or fashion shoes, emphasizing stability, spaciousness, and structural integrity.
- Goal: Provide critical external support, effectively accommodate custom orthotics, minimize friction on bony prominences (thereby reducing calluses, corns, and bunion irritation), and physically help stabilize the severely pronated foot.
- Physical Therapy and Rehabilitation:
- Visual: Physical therapy exercises focus on strengthening key muscles such as the posterior tibial muscle (which visibly courses along the medial ankle) and other intrinsic foot muscles, improving ankle and foot flexibility, and enhancing overall balance and proprioception. Videos or pictures demonstrating Grade 3 flat feet exercises would show specific movements aimed at improving muscle control, reducing compensatory patterns, and enhancing overall lower limb mechanics. Manual therapy may also be employed to mobilize stiff joints.
- Goal: Improve muscle strength and endurance to better support the arch, enhance joint mobility (where possible), reduce pain and inflammation, and optimize gait mechanics.
- Weight Management:
- Visual: While not a direct foot treatment, achieving significant weight loss can visibly reduce the immense mechanical load on the already compromised foot and ankle joints, substantially alleviating symptoms and slowing progression. Before-and-after body composition images can demonstrate the overall health improvement.
- Goal: Decrease the mechanical stress on the severely compromised foot structures, which are ill-equipped to handle excessive load.
- Medications and Injections:
- Visual: Non-steroidal anti-inflammatory drugs (NSAIDs) can reduce visible swelling, erythema, and inflammation associated with PTTD and other soft tissue irritation. Corticosteroid injections may be cautiously used to target specific areas of inflammation (e.g., within the posterior tibial tendon sheath), with the injection site sometimes visible in a clinical photograph.
- Goal: Provide symptomatic relief of pain and inflammation, particularly in cases of severe PTTD or acute flair-ups.
Surgical Management (Visual Outcomes & Detailed Procedures for Grade 3 Flat Feet):
Surgical intervention for Grade 3 flat feet is typically considered when conservative measures have demonstrably failed to control pain or deformity, when pain is debilitating and significantly impacting quality of life, or when the deformity is progressive, rigid, and causing irreversible joint damage. The overarching primary goal is to fundamentally restore a functional, stable, and pain-free foot alignment, preventing further deterioration. Surgical repair of Grade 3 flat feet involves a complex combination of procedures tailored to the individual patient’s specific deformities and underlying pathology, aiming to correct the structural issues and stabilize the foot.
The specific procedures performed depend critically on the exact nature of the deformity, the patient’s age, the flexibility versus rigidity of the foot, and the extent of tendon and ligament damage. Common procedures, often performed in a complex combination, include:
- Soft Tissue Procedures:
- Posterior Tibial Tendon Reconstruction/Transfer: If the posterior tibial tendon is severely torn, elongated, or dysfunctional (a common cause of Grade 3 flat feet), it may be extensively debrided, repaired, or augmented. Often, another healthy tendon (most commonly the flexor digitorum longus tendon) is transferred and rerouted to the navicular bone to substitute for the damaged posterior tibial tendon and help recreate medial arch support. Surgical images would show the tendon being harvested, rerouted through a drill hole, and attached to the navicular bone.
- Spring Ligament Repair/Reconstruction: The spring ligament complex is absolutely crucial for maintaining the integrity of the medial longitudinal arch. If it is found to be ruptured, severely attenuated, or incompetent, it can be directly repaired, shortened, or reconstructed using autograft or allograft tissue.
- Gastrocnemius Recession/Achilles Lengthening: To address an equinus contracture (tightness of the calf muscles and/or Achilles tendon), which very frequently accompanies and significantly exacerbates severe flat feet by preventing proper dorsiflexion and increasing pronation forces. Visibly, this procedure helps the heel sit flatter on the ground, improving ankle mechanics.
- Bony Procedures (Osteotomies – Bone Cuts and Realignment):
- Medializing Calcaneal Osteotomy (MCO): This is a cornerstone procedure for correcting hindfoot valgus. A precise osteotomy (cut) is made in the heel bone (calcaneus), and a segment is shifted medially (inward) by several millimeters. This realigns the mechanical axis of the hindfoot, bringing the Achilles tendon’s pull back into a more central position. Post-operative X-ray images clearly show the corrected alignment of the calcaneus and the hardware (screws) used to fix the bone segment in its new position.
- Lateral Column Lengthening (e.g., Calcaneal Opening Wedge Osteotomy or Evans Osteotomy): A cut is made on the outside (lateral aspect) of the calcaneus, and a bone graft (either from the patient or donor) is inserted to lengthen the lateral column of the foot. This procedure effectively corrects forefoot abduction and helps to recreate the medial longitudinal arch by bringing the forefoot out of its abducted position relative to the hindfoot. Post-operative images demonstrate the restored arch contour and corrected forefoot position.
- Medial Cuneiform Opening Wedge Osteotomy (Cotton Osteotomy): This procedure is performed to specifically elevate the medial column of the midfoot and restore the arch in cases where there is a significant sag or plantarflexion of the medial cuneiform. A bone wedge is inserted into a cut on the medial cuneiform.
- Talar Head Coverage Procedures: In some cases, where the talar head is significantly uncovered (medially prominent), procedures may specifically address this by redirecting soft tissue or performing bony realignments to improve talonavicular joint congruity, often in conjunction with other osteotomies to achieve overall realignment.
- Arthrodesis (Joint Fusion Procedures):
- Subtalar Arthrodesis: This involves surgically fusing the talus and calcaneus (the subtalar joint). This procedure effectively stabilizes the hindfoot and definitively corrects valgus deformity but eliminates all motion at the subtalar joint. It is considered for rigid or severely arthritic subtalar joints.
- Triple Arthrodesis: This is a more extensive fusion procedure, involving the surgical fusion of three critical joints in the hindfoot and midfoot: the talonavicular, calcaneocuboid, and subtalar joints. This procedure is reserved for severe, rigid Grade 3 flat feet with significant, irreversible deformity and arthritic changes, offering maximal correction and stability at the expense of significant joint motion. Post-operative X-rays of triple arthrodesis clearly show the fused joints and dramatically improved anatomical alignment, making the foot appear more “normal” structurally and functionally stable.
Post-Operative Visual Aspects and Rehabilitation:
- Casting/Bracing: Post-operatively, patients will typically be in a non-weight-bearing cast or a controlled ankle motion (CAM) boot for several weeks to months, visibly immobilizing the foot and ankle to allow for proper bone and soft tissue healing and to protect the surgical reconstruction. Pictures of patients post-Grade 3 flat feet surgery will show these protective devices, highlighting the initial phase of recovery.
- Surgical Scarring: Surgical incisions will result in scars, the appearance of which varies depending on the specific surgical approach(es) used, the individual patient’s skin type, and their healing response.
- Improved Foot Alignment: The most significant and gratifying visual outcome of successful surgery is the restoration of a more natural arch contour, a substantial reduction of hindfoot valgus, and correction of forefoot abduction. Before-and-after photos of Grade 3 flat feet surgery powerfully illustrate these dramatic improvements in foot morphology and alignment, providing clear evidence of the surgical success.
- Rehabilitation: Extensive physical therapy post-surgery is absolutely crucial to regain strength, flexibility, proprioception, and proper gait patterns. This includes a structured program of exercises aimed at rebuilding muscle, reducing residual swelling (which can be visibly monitored), and gradually increasing weight-bearing and functional activity.
The overarching goal of Grade 3 flat feet treatment, whether through meticulous non-surgical management or complex surgical reconstruction, is to alleviate debilitating pain, significantly improve foot function and stability, and restore a more anatomically correct and stable foot structure. This comprehensive approach ultimately aims to enhance the patient’s overall quality of life, prevent further complications, and allow for a return to meaningful activities with less pain and greater confidence, profoundly changing the visual and functional presentation of the collapsed arch foot.