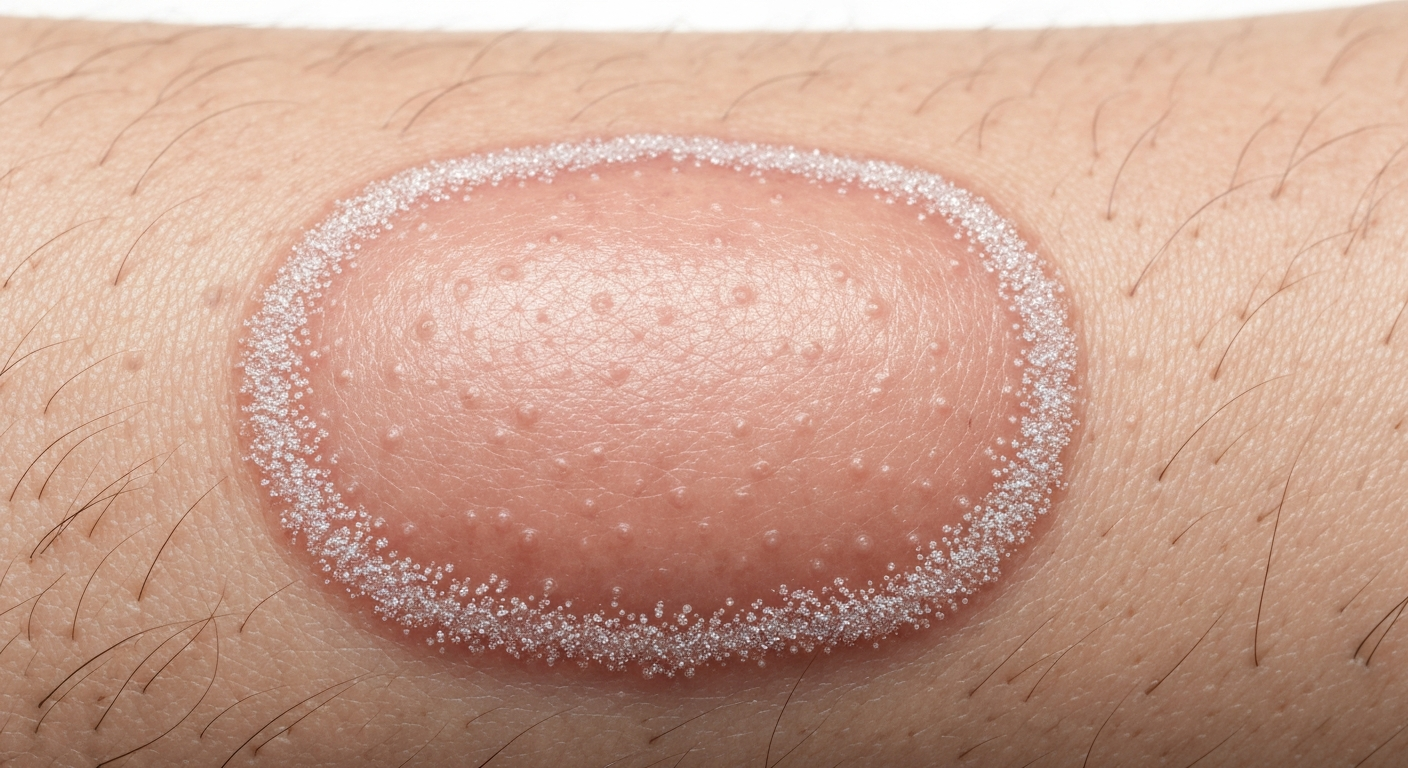
Understanding Ringworm in children symptoms pictures is crucial for prompt identification and effective treatment of this common fungal infection. This detailed guide explores the various manifestations of ringworm across different body parts, providing comprehensive insights into its appearance and progression for parents and caregivers.
Ringworm in children Symptoms Pictures
Ringworm, medically known as dermatophytosis or tinea, presents with a diverse range of symptoms in children, often making visual identification through pictures an invaluable tool. The classic presentation of ringworm is a red, itchy, scaly rash that forms a ring-like pattern, which gives the condition its misleading name – it is caused by a fungus, not a worm. However, the appearance can vary significantly depending on the affected body part, the child’s immune response, and the specific fungal species involved. When examining Ringworm in children symptoms pictures, observers should look for a combination of visual cues to accurately identify the infection.
The primary visual characteristics often captured in images illustrating ringworm in children include:
- Annular Lesions: These are the hallmark ring-shaped patches. The center of the lesion may appear clearer or less inflamed than the raised, red, scaly border. This central clearing is a strong indicator visible in many ringworm pictures.
- Erythema: Redness is a very common symptom, particularly around the active edges of the rash. This can range from a light pink to a deep, fiery red, especially in inflamed areas.
- Scaling: The affected skin often presents with fine, silvery, or yellowish scales. These scales are essentially dead skin cells accumulating due to the fungal activity.
- Pruritus: While not directly visible in ringworm symptom pictures, severe itching is a nearly universal symptom that often leads to excoriations (scratch marks) which can be seen in images.
- Raised Borders: The edge of the ringworm lesion is typically raised, slightly bumpy, or vesiculated (containing small fluid-filled blisters). This raised border is where the fungus is most active.
- Alopecia: In cases of tinea capitis (ringworm of the scalp), hair loss is a prominent symptom. This can manifest as patchy bald spots where hair shafts have broken off at or near the skin surface, often accompanied by scaling and inflammation.
- Pustules and Vesicles: In more severe or inflamed cases, particularly in specific locations or with secondary bacterial infections, small pustules (pus-filled bumps) or vesicles (small blisters) may be observed within the lesions or along the borders.
- Crusting: Over time, especially if scratched or if secondary infections occur, the lesions can develop yellowish or brownish crusts.
- Hyperpigmentation or Hypopigmentation: After the active infection subsides, the affected skin might show temporary changes in pigmentation, appearing either darker (hyperpigmented) or lighter (hypopigmented) than the surrounding skin.
Understanding these general presentations is the first step when reviewing Ringworm in children symptoms pictures, but specific locations often present with unique challenges and variations. For instance, ringworm on the face may be less distinctly annular due to muscle movement, while ringworm on the feet (athlete’s foot) can present with peeling and cracking between the toes. Accurately identifying ringworm symptoms in children requires careful attention to these nuances.
Variations of Ringworm Symptoms in Children by Location:
The appearance of pediatric ringworm can differ significantly depending on the body area affected, a crucial aspect to consider when evaluating Ringworm in children symptoms pictures.
- Tinea Corporis (Body Ringworm): This is the most classic form, characterized by the iconic circular or oval red patches with raised, scaly borders and central clearing. These lesions can occur anywhere on the trunk, limbs, or face. Multiple lesions may be present and can merge, creating larger, more irregular patterns. Itching is prominent.
- Tinea Capitis (Scalp Ringworm): This form is particularly common in school-aged children and often requires oral antifungal treatment.
- “Gray Patch” Ringworm: Characterized by patches of dull gray scales and brittle hair that breaks off easily, leading to areas of partial alopecia. The scalp itself may not show overt inflammation initially.
- “Black Dot” Ringworm: Hair breaks off at the scalp surface, leaving behind tiny black dots (stubs of broken hair shafts) in the hair follicles. Scaling and inflammation are also common.
- Inflammatory Tinea Capitis (Kerion): This is a severe, highly inflamed form presenting as a boggy, pus-filled, painful mass with significant hair loss, often accompanied by swollen lymph nodes in the neck and fever. It requires urgent medical attention to prevent permanent scarring and hair loss. Pictures of kerion will show a very distinct, often alarming, presentation.
- Pustular Ringworm: Small pustules may develop on the scalp in affected areas, signaling inflammation and potential secondary bacterial infection.
- Tinea Cruris (Jock Itch): Affects the groin area, inner thighs, and buttocks. It typically presents as red, itchy, scaly patches with well-defined, often raised borders. The rash usually spares the scrotum in boys. This form is often intensely itchy and can be exacerbated by sweat and friction.
- Tinea Pedis (Athlete’s Foot): Common in older children and adolescents.
- Interdigital Type: The most common, showing scaling, redness, and cracking between the toes, particularly between the fourth and fifth toes. It can be very itchy and sometimes accompanied by a burning sensation.
- Moccasin Type: Affects the sole and sides of the foot, presenting as chronic dryness, scaling, and thickening of the skin, resembling a moccasin pattern. It can involve one or both feet.
- Vesiculobullous Type: Characterized by the sudden appearance of fluid-filled blisters (vesicles) or larger bullae, often on the soles or sides of the feet, accompanied by intense itching and redness.
- Tinea Manuum (Hand Ringworm): Less common in children than feet or body ringworm, it often presents with chronic dryness, scaling, and mild redness on the palms or fingers, sometimes resembling chronic eczema. It can be unilateral, affecting only one hand.
- Tinea Unguium (Onychomycosis – Nail Ringworm): Affects the fingernails or toenails. In children, it’s less common but possible, especially if other forms of ringworm are present. Symptoms include:
- Thickening of the nail plate.
- Discoloration (yellow, brown, white).
- Brittleness or crumbling of the nail.
- Separation of the nail from the nail bed (onycholysis).
- Distortion of the nail shape.
- Tinea Faciei (Facial Ringworm): Can be difficult to diagnose as the typical ring-like pattern may be less distinct due to the thinness of facial skin and muscle movements. It often presents as red, scaly patches that may be slightly raised and itchy. It can be confused with other facial rashes.
When reviewing Ringworm in children symptoms pictures, it is critical to observe the distribution, morphology, and associated features of the rash. The presence of multiple lesions, varying sizes, and the characteristic central clearing with active borders are strong indicators of a fungal infection. Understanding these visual cues helps in differentiating ringworm from other common pediatric skin conditions.
Signs of Ringworm in children Pictures
Identifying the signs of ringworm in children through pictures requires a keen eye for dermatological details. These signs are the observable manifestations that point towards a fungal infection, providing crucial diagnostic clues. Unlike subjective symptoms (like itching), signs are objective and can be visually confirmed, making them ideal for photographic documentation and identification. Healthcare professionals and parents often rely on clear signs of ringworm in children pictures to guide preliminary assessment.
Here are the key visual signs of ringworm in children commonly depicted in dermatological photography:
- Erythematous Annular Patches: As previously mentioned, these are red, circular, or oval patches. The redness is often more pronounced at the periphery of the lesion. Photos frequently highlight the stark contrast between the inflamed border and the clearing center.
- Raised, Serpiginous Borders: The active edge of the ringworm lesion is typically elevated, creating a palpable ridge. This border can be described as serpiginous (wavy or snake-like) or arcuate (arc-shaped). In ringworm images, these raised borders often appear distinct and well-demarcated from the surrounding healthy skin. Small vesicles or pustules may sometimes be observed along this leading edge, indicating active fungal growth.
- Fine to Coarse Scaling: The presence of dry, flaky skin is a consistent sign. The scales can range from very fine, almost powdery, to thicker, more adherent flakes. In children’s skin rash pictures of ringworm, the scaling is often clearly visible within the lesion and especially along the advancing margins.
- Central Clearing: A defining characteristic where the center of the ring appears less inflamed, sometimes almost normal skin color, or slightly hypopigmented. This effect is a strong diagnostic sign in many ringworm cases, as the fungus tends to spread centrifugally from a central point, consuming nutrients at the edges and leaving a relatively healed center.
- Broken Hair Shafts (Tinea Capitis): For scalp ringworm, specific signs include areas where hair has broken off close to the scalp, leaving stubble or “black dots.” This is a critical sign for diagnosing tinea capitis and preventing permanent hair loss. Pictures demonstrating patches of alopecia with accompanying scales are highly indicative.
- Follicular Pustules and Papules: In some forms, particularly inflammatory tinea capitis (kerion) or deeply seated body ringworm, visible pus-filled bumps (pustules) or small solid bumps (papules) may be present, often at the hair follicles. These signs indicate a more intense inflammatory response.
- Inflammation and Edema: Swelling (edema) and generalized inflammation (redness, warmth) are common signs, particularly in acute or more severe infections. The skin within and surrounding the lesion may appear puffy or engorged.
- Onycholysis and Nail Dystrophy (Tinea Unguium): In cases of nail ringworm, visual signs include the nail plate lifting off the nail bed (onycholysis), significant thickening (hyperkeratosis), discoloration (yellow, brown, white, or opaque), and brittleness or crumbling of the nail. These signs are distinctly visible in specialized nail ringworm pictures.
- Excoriations: While not a primary sign of the fungus itself, scratch marks from intense itching are frequently observed in ringworm images. These can indicate the severity of pruritus and potential for secondary bacterial infections.
- Satellite Lesions: Smaller, distinct lesions appearing near the primary ringworm patch are often seen. These satellite lesions indicate the spread of the fungus to adjacent skin.
When examining signs of ringworm in children pictures, it’s vital to consider the child’s age, overall health, and any recent exposures to infected individuals or pets. The morphology of the lesions, their distribution, and any associated hair or nail changes collectively paint a comprehensive picture for accurate diagnosis of pediatric ringworm symptoms. A thorough visual inspection is often the first and most critical step in identifying this prevalent skin condition.
Early Ringworm in children Photos
Catching early ringworm in children is paramount for swift treatment and preventing spread. The initial stages of a fungal infection can be subtle, making diagnosis challenging, but distinctive enough for identification through well-documented early ringworm in children photos. These initial signs may not always present as the classic “ring” immediately but evolve over time. Understanding these incipient manifestations is key for parents and caregivers to seek timely medical advice for pediatric skin concerns.
What to look for in early ringworm in children photos:
- Small, Red Papule or Macule: Ringworm often begins as a small, slightly reddish bump (papule) or a flat, discolored spot (macule) on the skin. This initial lesion may be no larger than a pea and might be easily mistaken for an insect bite or a common skin irritation. These are the very first observable ringworm early symptoms.
- Subtle Scaling: Even in its nascent stages, a very fine, almost imperceptible scale might be present on the surface of the initial red spot. This scaling can become more prominent as the lesion slightly enlarges. Photos taken at this stage might require high resolution to capture this detail.
- Mild Itching: Although not visible in photos, mild itching is often one of the earliest subjective symptoms reported by children. This can prompt parents to inspect the skin more closely. The absence of intense itching does not rule out early ringworm.
- Slightly Expanding Redness: Over a few days to a week, the initial spot will begin to expand centrifugally, forming a slightly larger, circular area of redness. The edges might still be ill-defined at this point, but the overall area of involvement grows. This expansion is a key feature to observe in a series of early ringworm progression pictures.
- Emerging Border Definition: As the lesion expands, the characteristic raised border starts to become more noticeable. This border might still be very thin and only slightly elevated, not yet forming the prominent ridge seen in more advanced cases. The central clearing might not be evident yet, or only very subtly present.
- Hair Involvement (Early Tinea Capitis): In the case of scalp ringworm, early signs can include:
- Localized Dullness or Brittleness of Hair: A specific patch of hair might appear slightly duller, coarser, or break more easily than the surrounding hair. This can be subtle and might only be noticed when styling the child’s hair.
- Minimal Scaling on Scalp: Small patches of fine, powdery scales on the scalp, which may initially be mistaken for dandruff, can be an early indicator.
- Small Area of Hair Loss: Very early, barely noticeable thinning of hair in a localized spot before complete breakage or baldness occurs.
- Mild Inflammation of Hair Follicles: Close inspection might reveal slightly reddened hair follicles within the affected patch, sometimes with tiny pustules.
- Absence of Significant Pain or Warmth: Unlike bacterial infections that often present with pain, significant warmth, and pus, early ringworm typically does not cause these symptoms unless it progresses to an inflammatory stage or develops a secondary bacterial infection.
When examining early ringworm in children photos, it’s crucial to look for patterns of growth and subtle changes in skin texture and color. The lesion might not yet have the full “ring” appearance, but the progression from a small, red spot to an expanding area with a developing border is highly indicative. Early detection of these ringworm beginnings allows for topical antifungal treatments to be highly effective, often preventing the need for oral medications and reducing the risk of transmission to others. Parents should be vigilant for any persistent or spreading skin lesions in their children, especially those accompanied by itching, and consult a pediatrician for accurate diagnosis and management of children’s skin conditions.
Skin rash Ringworm in children Images
The term “skin rash Ringworm in children images” encapsulates the visual diagnostic aspect of dermatophytosis, highlighting the various ways this fungal infection manifests on a child’s skin. Since ringworm is primarily a visible rash, images serve as crucial references for identification, understanding progression, and differentiating it from other common pediatric skin conditions. These images often showcase the distinct morphology that guides both parents and healthcare providers in recognizing the infection and determining appropriate care for children’s skin health.
When reviewing “skin rash Ringworm in children images,” one expects to see a range of presentations, each providing valuable diagnostic clues:
- Classic Annular (Ring-Shaped) Rash: The most iconic type, these images clearly show the circular or oval patches of redness with a raised, scaly, and often intensely itchy border. The center typically appears clearer, less inflamed, or even normal skin tone. This central clearing is a powerful visual sign. The active edge may also exhibit small papules or vesicles.
- Tinea Corporis Variations: Images of body ringworm can show single lesions or multiple coalescing lesions, forming larger, more irregular shapes. The borders might be distinctly arcuate or serpiginous. On darker skin tones, the erythema might be less pronounced, with hyperpigmentation or hypopigmentation being more visible, making the texture and scaling crucial visual indicators.
- Scalp Ringworm (Tinea Capitis) Presentations:
- Patches of Hair Loss and Scaling: These images display distinct areas of partial or complete hair loss on the scalp, often accompanied by significant scaling. The hair shafts in these patches may appear dull, broken, or “black dots.”
- Kerion Images: Pictures of kerion will show a dramatically inflamed, boggy, pus-filled, and painful lesion on the scalp, often with crusting and matted hair. This severe inflammatory reaction requires immediate medical attention and is a distinct visual sign.
- Groin Rash (Tinea Cruris) Visuals: Images of jock itch in children will often show a well-demarcated, red, scaly rash in the groin area, typically sparing the scrotum. The borders are usually raised and can be quite prominent, distinguishing it from diaper rash or intertrigo which tend to affect skin folds symmetrically.
- Foot Rash (Tinea Pedis) Images:
- Interdigital Peeling and Redness: Images might show macerated, peeling, and red skin between the toes, particularly the lateral toes. Fissures or cracks in the skin are common.
- Moccasin-Type Scaling: Pictures depicting chronic athlete’s foot often show extensive dryness, scaling, and thickening of the skin on the soles and sides of the feet, forming a “moccasin” distribution.
- Vesicular Outbreaks: Acute presentations might show clusters of small blisters or fluid-filled vesicles on the soles or sides of the feet, which can be intensely itchy.
- Nail Ringworm (Tinea Unguium) Photos: Images of affected nails demonstrate thickening, discoloration (yellow, brown, white), brittleness, and crumbling of the nail plate. There might also be evidence of onycholysis (separation of the nail from the nail bed). These are distinct from healthy nail appearances and require specialized treatment.
- Facial Ringworm (Tinea Faciei) Depictions: These images might show less typical ring-shaped lesions due to facial muscle movement and cosmetic application. Often, they present as red, scaly, and slightly raised patches that can be confused with other facial dermatoses like eczema or psoriasis. Careful attention to the subtle raised border and central clearing, even if incomplete, is vital.
- Atypical or Confluent Lesions: In some children, especially those with compromised immune systems or prolonged infection, the lesions might not form perfect rings but instead appear as diffuse, irregular patches of scaling, redness, and inflammation. These images underscore the variability of ringworm manifestations.
When analyzing “skin rash Ringworm in children images,” it’s important to differentiate ringworm from conditions like eczema (atopic dermatitis), psoriasis, pityriasis rosea, contact dermatitis, and impetigo. Key differentiating factors in images include the well-defined, raised, and often clearer-centered border of ringworm, the presence of specific hair or nail changes, and the absence of the characteristic features of other conditions (e.g., vesicles of chickenpox, silvery scales of psoriasis on extensor surfaces, or honey-colored crusts of impetigo). Consulting comprehensive visual guides and medical professionals is crucial for accurate diagnosis based on pictures of skin rashes in children to ensure the right course of action for managing pediatric skin infections.
Ringworm in children Treatment
Effective Ringworm in children treatment is essential to alleviate symptoms, prevent the spread of the infection, and avoid complications. The choice of treatment depends heavily on the location and severity of the ringworm, as well as the child’s age and overall health. While topical antifungal medications are often sufficient for skin ringworm, scalp ringworm (tinea capitis) and nail ringworm (tinea unguium) almost always require oral antifungal therapy due to the fungal infection being deep within the hair follicles or nail plate. Prompt and consistent treatment is key for successful eradication of the fungal infection.
Topical Antifungal Treatments for Ringworm in Children:
For most cases of tinea corporis, tinea cruris, tinea pedis, and tinea manuum, topical antifungal creams, lotions, gels, or sprays are the first line of ringworm treatment for children. These medications work by killing the fungus or inhibiting its growth. They typically need to be applied twice daily for 2-4 weeks, even if the rash appears to clear sooner, to ensure complete eradication. It’s crucial to apply the medication to the entire affected area and slightly beyond the visible border of the rash.
Common active ingredients in over-the-counter (OTC) and prescription topical antifungals include:
- Azoles: This class includes drugs like miconazole (Desenex, Lotrimin AF), clotrimazole (Lotrimin AF), ketoconazole (Nizoral), and econazole. They work by disrupting the fungal cell membrane.
- Allylamines: Terbinafine (Lamisil AT) and naftifine (Naftin) are highly effective, especially against dermatophytes. They are fungicidal, meaning they kill the fungus directly.
- Benzylamines: Butenafine (Lotrimin Ultra) is another fungicidal option with good efficacy.
- Other Antifungals: Tolnaftate (Tinactin) is a fungistatic agent (inhibits growth) often available OTC.
Application Guidelines for Topical Treatment:
- Wash and dry the affected area thoroughly before application.
- Apply a thin layer of cream or ointment to cover the entire lesion and extend at least 1-2 cm beyond its visible borders.
- Apply consistently as directed by a healthcare provider, typically once or twice daily.
- Continue treatment for at least 1-2 weeks after the rash has visibly cleared to prevent recurrence, often for a total duration of 2-4 weeks.
- Wash hands thoroughly before and after applying medication.
Oral Antifungal Treatments for Ringworm in Children:
Oral antifungal medications are necessary for deeper or more widespread infections, particularly tinea capitis and tinea unguium, which topical treatments cannot penetrate effectively. They are also used for severe cases of body ringworm or when topical treatments have failed. These medications work systemically throughout the body.
Common oral antifungals prescribed for ringworm in children include:
- Griseofulvin: This is often the first-line oral treatment for tinea capitis in children, approved for pediatric use and generally well-tolerated. It needs to be taken with fatty foods to improve absorption and is typically prescribed for 6-12 weeks for scalp ringworm.
- Terbinafine: Highly effective against dermatophytes and can be used for tinea capitis, tinea pedis, and tinea unguium. Treatment duration varies but can be shorter than griseofulvin for some indications (e.g., 2-4 weeks for tinea capitis, longer for nail infections).
- Itraconazole: Another broad-spectrum antifungal that can be used for various forms of ringworm, including tinea capitis and tinea unguium. It’s often prescribed in pulse dosing regimens (taken for one week, then three weeks off, repeated).
- Fluconazole: While less commonly used for tinea capitis compared to griseofulvin or terbinafine, it can be an option, especially for specific fungal species or in cases where other treatments are not tolerated.
Important Considerations for Oral Treatment:
- Duration: Oral treatments typically require several weeks to months to be effective, especially for scalp and nail infections. Adherence to the full course is critical to prevent recurrence.
- Side Effects: Oral antifungals can have side effects such as gastrointestinal upset, headaches, and liver enzyme elevations. Liver function tests may be required before and during treatment, particularly with long-term use.
- Drug Interactions: Oral antifungals can interact with other medications. It is crucial to inform the prescribing doctor of all medications the child is taking.
- Administration: Some medications are available in liquid suspension, making them easier for children to take.
Supportive Measures and Prevention of Ringworm in Children:
In addition to specific antifungal medications, several supportive measures can aid in the healing process and prevent the spread or recurrence of ringworm in children:
- Good Hygiene:
- Wash affected skin daily with soap and water and dry thoroughly.
- For tinea capitis, use an antifungal shampoo (e.g., ketoconazole or selenium sulfide) a few times a week, as prescribed, to reduce fungal shedding, although this is not a standalone treatment for the infection itself.
- Change clothes, especially underwear and socks, daily.
- Avoid sharing personal items like hats, combs, brushes, towels, and clothing.
- Clothing and Footwear:
- Wear loose-fitting, breathable clothing made of cotton to reduce moisture and friction in affected areas (e.g., groin, body).
- For tinea pedis, wear clean cotton socks and well-ventilated shoes. Avoid synthetic socks and tight shoes.
- Change socks frequently if feet sweat excessively.
- Go barefoot at home when possible to allow feet to air out.
- Environmental Control:
- Disinfect contaminated surfaces and items, such as shower floors, gym equipment, and combs.
- Wash bedding and towels frequently in hot water.
- Check family members and pets for signs of ringworm, as they can be sources of re-infection. Treat infected pets through a veterinarian.
- Avoid Scratching: Trim fingernails short to minimize skin damage from scratching, which can lead to secondary bacterial infections or spread the fungus to other body parts.
- Educate the Child: Explain to the child why they shouldn’t scratch and the importance of hygiene to prevent spreading the infection.
- Return to School/Daycare: Generally, children can return to school or daycare once treatment has started, but it’s always best to check with the school’s policy and inform them if necessary, particularly for tinea capitis.
By combining appropriate antifungal medications with meticulous hygiene and preventive strategies, Ringworm in children treatment can effectively resolve the infection, alleviate discomfort, and protect other family members and peers from contracting this common yet highly contagious fungal condition. Always consult a healthcare professional for an accurate diagnosis and personalized treatment plan for pediatric fungal infections.