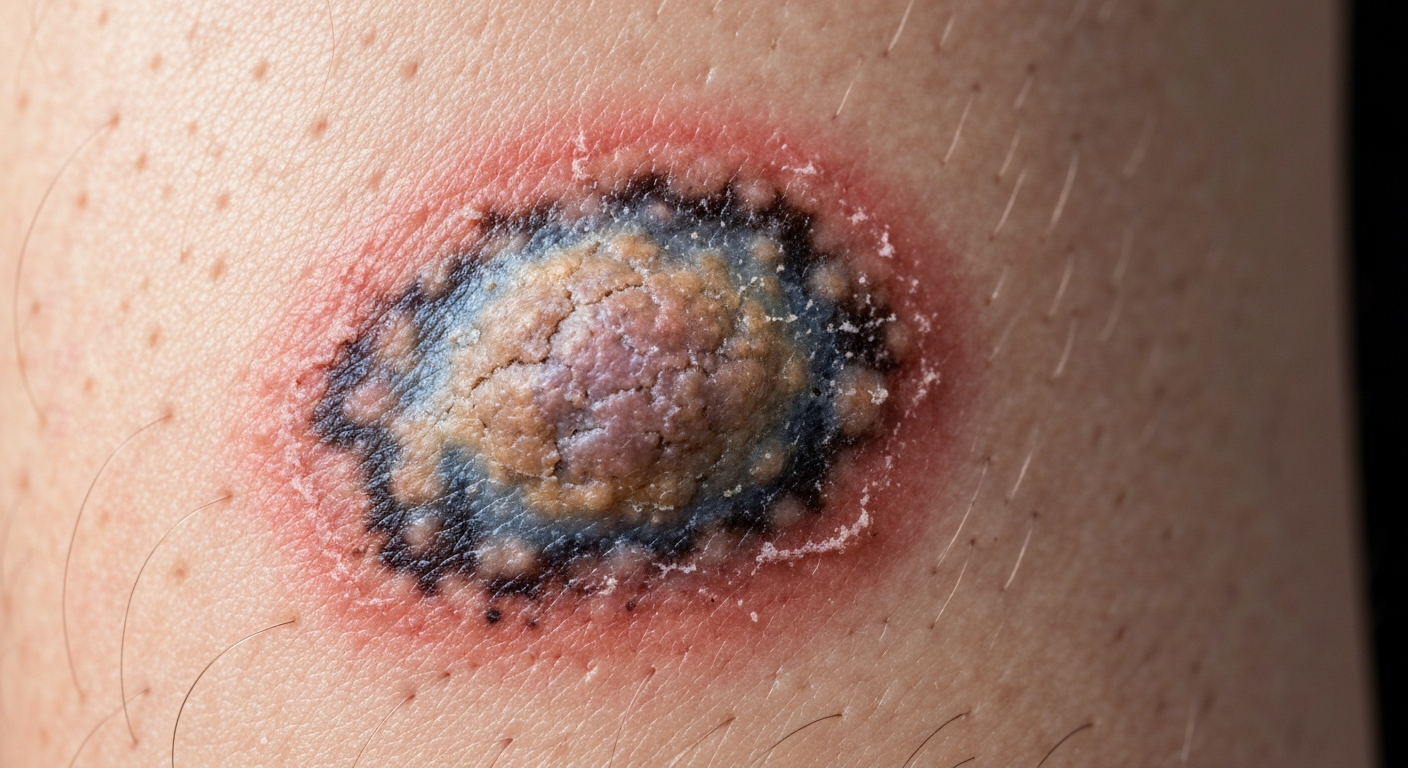
Here we present detailed descriptions to accompany Skin melanoma symptoms pictures, focusing on observable characteristics that are critical for early detection. These visual cues are essential for individuals to recognize potential concerns and seek timely dermatological evaluation, enhancing the chances of successful intervention against this serious skin cancer.
Skin melanoma Symptoms Pictures
Identifying Skin melanoma symptoms early is paramount for effective treatment outcomes. When observing Skin melanoma symptoms pictures, it’s crucial to focus on specific visual characteristics that differentiate malignant lesions from benign moles or other skin imperfections. These symptoms often involve changes in existing moles or the appearance of new, suspicious growths. Understanding these visual signs can significantly aid in self-examination and prompt consultation with a dermatologist for a definitive diagnosis of this aggressive form of skin cancer.
The primary diagnostic tool for assessing suspicious pigmented lesions is the ABCDE rule. This comprehensive guideline helps individuals and medical professionals evaluate moles for potential melanoma based on their visual appearance. Each letter represents a key characteristic to look for when examining Skin melanoma symptoms pictures:
- A for Asymmetry: Benign moles are typically symmetrical, meaning if you were to draw a line through the middle, both halves would largely match. In contrast, one of the most common Skin melanoma symptoms is asymmetry, where one half of the lesion does not match the other half in shape, size, or color distribution. This irregular growth pattern is a strong indicator of potential malignancy and is frequently observed in early melanoma photos.
- B for Border: The borders of a common mole are usually smooth and well-defined. However, a significant melanoma symptom is an irregular border. This can manifest as edges that are notched, scalloped, blurred, ragged, or poorly defined. The pigment might also appear to fade into the surrounding skin rather than having a distinct margin. These uneven or fuzzy edges are critical visual cues in Skin melanoma symptoms pictures.
- C for Color: Uniform color is characteristic of most benign moles. One of the most telling Skin melanoma symptoms is color variation within a single lesion. This can include different shades of brown, tan, or black, as well as areas of red, white, or blue. The presence of multiple colors, or an uneven distribution of color, is a serious warning sign. Sometimes, melanoma may present as a very dark, almost black, spot (often referred to as very dark Skin melanoma photos), or even as an amelanotic (flesh-colored or reddish) lesion, which can be harder to identify without pigmentation.
- D for Diameter: Most benign moles are relatively small, typically less than 6 millimeters (about the size of a pencil eraser). While melanoma can be smaller, a diameter greater than 6mm is a common sign. However, the more critical aspect is a lesion that is growing in diameter. Any mole that is noticeably increasing in size over weeks or months should be considered suspicious. Rapid growth is a particularly alarming symptom often highlighted in images of evolving skin lesions.
- E for Evolving: This is arguably the most crucial sign of Skin melanoma. Any mole that is changing or evolving in any way—in size, shape, color, elevation, or new symptoms such as itching, tenderness, bleeding, or crusting—warrants immediate medical attention. This “evolution” encompasses all the other ABCDE criteria over time. A mole that feels different (itchy, painful, sensitive) or looks different (flaky, scaly, oozing) is a strong indicator of potential melanoma. These dynamic changes are frequently depicted in sequential Skin melanoma symptoms pictures, demonstrating progression.
Beyond the ABCDEs, other Skin melanoma symptoms can include:
- New Lesion Appearance: The emergence of a new, suspicious mole or dark spot on the skin, especially after the age of 30, should be carefully monitored.
- Elevated or Lumpy Texture: While some benign moles can be raised, a new elevation or a palpable lump developing within an existing mole can be a sign of nodular melanoma, a more aggressive subtype.
- Itching or Tenderness: A mole that persistently itches, burns, or feels tender to the touch without any obvious cause can be an early symptom of melanoma.
- Bleeding or Oozing: Any mole that spontaneously bleeds, oozes fluid, or develops a crust without being provoked by injury is a significant red flag for melanoma.
- Non-Healing Sore: A sore that appears on the skin and does not heal within a few weeks, especially if it’s pigmented, should be evaluated by a doctor.
- Satellite Lesions: Small, new pigmentations that appear around a larger, suspicious lesion (known as “satellite metastases”) indicate advanced melanoma.
These detailed descriptions of Skin melanoma symptoms provide a comprehensive guide for anyone examining their skin or reviewing Skin melanoma symptoms pictures. Early detection through careful observation of these signs remains the most effective strategy for successful melanoma treatment.
Signs of Skin melanoma Pictures
Observing the specific signs of Skin melanoma in pictures can be highly informative for recognizing potential malignancy. These signs often go beyond simple color or shape and delve into the texture, growth patterns, and symptomatic presentation of the lesion. When analyzing signs of Skin melanoma pictures, it’s vital to consider the overall context of the lesion’s appearance and how it compares to surrounding skin or other benign moles. Recognizing these visual indicators is a critical step toward early diagnosis and improved outcomes for individuals with this dangerous skin cancer.
The visual characteristics that constitute signs of Skin melanoma are diverse and can vary depending on the type of melanoma. Here are key signs to look for:
- Variegated Pigmentation: This is a cornerstone sign frequently seen in signs of Skin melanoma pictures. Instead of a uniform brown, black, or tan, melanoma often exhibits a chaotic mix of colors. This can include shades of black, various browns, and tan, but also striking areas of red, white, or blue. The red might indicate inflammation or regression, while white areas could suggest areas where the body’s immune system has attempted to fight the cancer. Blue or bluish-gray hues suggest deeper penetration of the pigment.
- Irregularity in Shape and Outline: While asymmetry covers the overall shape, the detailed outline of the lesion is also a critical sign. The border might be jagged, fuzzy, or “geographic,” meaning it resembles an irregular landmass on a map. These uneven contours are rarely seen in benign moles and are strong indicators in visual melanoma detection.
- Surface Changes: The texture of a melanoma can evolve. What might start as a flat lesion can become raised, bumpy, or develop a rough, scaly, or crusty surface. These changes in elevation and texture are significant signs of progression often visible in signs of Skin melanoma pictures. Ulceration, where the skin surface breaks down, leading to an open sore, is also a serious sign.
- Growth and Expansion: Any pigmented lesion that is noticeably increasing in size over a period of weeks or months is highly suspicious. This growth can be in diameter, but also in height (elevation). Documenting size changes with sequential photos can be invaluable for tracking this critical sign of skin cancer.
- “Ugly Duckling” Sign: This concept is increasingly emphasized in dermatology. The “ugly duckling” is a mole that looks distinctly different from all the other moles on an individual’s skin. Most people tend to have moles that resemble each other to some extent. If one mole stands out as an outlier in terms of size, shape, color, or texture, it should be considered a suspicious lesion and investigated. This comparative sign is extremely useful when reviewing signs of Skin melanoma pictures in the context of an individual’s overall mole pattern.
- Inflammation or Redness Around the Lesion: While melanoma itself is pigmented, an inflammatory halo or persistent redness surrounding a mole can be a sign. This might indicate the body’s immune response to the tumor or local irritation. This redness can sometimes be mistaken for an infection or irritation, delaying accurate diagnosis.
- New Onset of Symptoms: The development of new symptoms like persistent itching, tenderness, pain, burning, or a stinging sensation within or around a mole is a significant sign. Moles should generally not cause discomfort. The sudden appearance or worsening of these symptoms warrants immediate attention and is a crucial part of identifying suspicious lesions in signs of Skin melanoma pictures.
- Nodularity: The appearance of a firm, elevated, dome-shaped, or polypoid growth within or alongside a pre-existing flat lesion. This indicates a nodular growth pattern, which can be characteristic of nodular melanoma, a more aggressive subtype. These lesions often have a uniform dark color but can also be amelanotic (lacking pigment).
- Regression Areas: Patches of white, gray, or bluish-white within a pigmented lesion can signify areas where the body’s immune system has caused the melanoma cells to regress. While this might sound positive, it indicates an active biological process within the lesion and is a strong sign of malignancy. These areas of regression can make the lesion appear even more heterogeneous in color.
- Finger and Toenail Involvement (Subungual Melanoma): For acral lentiginous melanoma affecting the nails, signs include a dark streak (melanonychia striata) that gradually widens or changes color, especially if it extends to the nail fold (Hutchinson’s sign). Bleeding under the nail or nail dystrophy (thickening, lifting, cracking) in the absence of trauma are also serious signs. These presentations are distinct and important to recognize in signs of Skin melanoma pictures.
- Location on Palms, Soles, or Mucous Membranes: While melanoma is often associated with sun-exposed skin, it can appear on areas not typically exposed to the sun, such as the palms of the hands, soles of the feet, and mucous membranes (mouth, nasal passages, genital/anal regions). Lesions in these areas, particularly if they are pigmented and exhibit any of the ABCDE signs, warrant high suspicion.
By diligently looking for these diverse signs of Skin melanoma, especially in conjunction with the ABCDE rule, individuals can improve their chances of detecting this formidable skin cancer at an early, more treatable stage. Dermatological expertise is essential for confirmation and management.
Early Skin melanoma Photos
Examining early Skin melanoma photos is crucial for recognizing the subtle indicators that distinguish nascent malignancies from benign moles. In its earliest stages, melanoma can be highly curable, emphasizing the importance of vigilant self-examination and professional skin screenings. Early detection relies on identifying small, often inconspicuous changes that might not yet present with all the classic ABCDE characteristics. Understanding what constitutes an early melanoma helps to catch this skin cancer before it progresses into more advanced, difficult-to-treat stages. When viewing early Skin melanoma photos, look for nuances that might be easily overlooked.
The characteristics of early Skin melanoma in photos often present as:
- Subtle Asymmetry: While established melanoma clearly shows asymmetry, early lesions might exhibit only a slight, almost imperceptible unevenness in shape. One half may be marginally larger or differently contoured than the other. This can be a very faint deviation from perfect symmetry, easily missed without careful scrutiny.
- Slight Border Irregularities: The borders might not be overtly notched or scalloped, but rather subtly fuzzy, slightly blurred at points, or have very minor, localized indentations. The edge might not be uniformly crisp all around, suggesting nascent irregular growth. These minor deviations from a perfectly smooth, round, or oval border are key in early melanoma identification.
- Limited Color Variation: Instead of dramatic multi-color displays, early melanomas might show only two shades of brown or black, or perhaps a small area of lighter or darker pigmentation within a largely uniform lesion. A new speck of dark brown or black within an existing tan mole can be a significant early sign. Sometimes, early lesions might present as a very uniform dark brown or black, but with an irregular shape, challenging the common perception of multi-colored melanomas.
- Small but Suspicious Diameter: While the “D” in ABCDE suggests a diameter larger than 6mm, early melanomas can be smaller. A lesion of 3-5mm with any of the other suspicious features (asymmetry, irregular border, subtle color changes) should still raise concern. The critical factor is not just the absolute size, but the presence of other worrying signs within a small lesion, or a small lesion that is growing.
- Incidental Changes (Evolving): Even minor changes over a period of weeks or months are critical. This could be a very slight increase in size, a barely noticeable shift in color intensity, or the development of a mild itch or tenderness in a previously asymptomatic mole. The evolution might not be dramatic, but any consistent change from a mole’s baseline appearance is important.
- Flat or Slightly Elevated Lesions: Many early melanomas, particularly superficial spreading melanoma, start as flat or only very slightly raised lesions. They might feel only marginally different from the surrounding skin. The subtle elevation might only be detectable by touch or by observing the lesion from an angle where light casts a slight shadow.
- New Onset, Single Lesion: While melanoma can arise from existing moles, many early melanomas appear as entirely new lesions on previously clear skin. The appearance of a single new, pigmented spot, especially in adults over 30, that looks different from other moles warrants attention.
- The “Ugly Duckling” in Miniature: Even among smaller moles, one might subtly stand out. It may not be dramatically different in size or color, but its overall morphology (shape, subtle border, pigment pattern) makes it look “different” from the individual’s other moles. This comparative difference, even if slight, is crucial for early detection.
- Dysplastic Nevi Comparison: Early melanoma photos often share similarities with dysplastic nevi (atypical moles), which are benign but can resemble melanoma and have a higher risk of developing into melanoma. Dysplastic nevi also exhibit some asymmetry, irregular borders, and color variation. The key difference is often the degree of these irregularities and the presence of ongoing evolution in melanoma. Regular monitoring of such atypical moles is essential.
Early detection is the most effective defense against melanoma. Therefore, recognizing these subtle signs in early Skin melanoma photos, performing regular self-skin exams, and seeking professional dermatological evaluation for any suspicious skin changes are vital preventive measures. Dermatologists often utilize dermoscopy to magnify and illuminate skin lesions, allowing for the visualization of deeper, microscopic features that can confirm an early melanoma diagnosis.
Skin rash Skin melanoma Images
While Skin melanoma is primarily a pigmented lesion, there are instances where Skin melanoma images might be confused with a common skin rash or present with inflammatory features that mimic one. It is crucial to understand these distinctions, as misdiagnosis can lead to dangerous delays in treatment for this aggressive skin cancer. Unlike a typical rash, which usually presents as widespread inflammation, itching, or eruption across a larger skin area, melanoma is generally a single, evolving lesion. However, certain presentations or reactions around a melanoma can lead to confusion, making accurate identification from Skin rash Skin melanoma images challenging without expert medical evaluation.
Here’s how Skin melanoma can sometimes be confused with or present features resembling a skin rash:
- Inflammatory Halo: A melanoma might sometimes be surrounded by a red, inflamed area, which can be mistaken for a localized rash or skin irritation. This inflammation can be due to the body’s immune response to the cancerous cells or secondary irritation if the mole is frequently scratched due to itching. In such Skin rash Skin melanoma images, the central lesion remains the key focus, but the surrounding redness can distract.
- Itching and Irritation: Persistent itching (pruritus) is a common symptom of melanoma. Individuals may scratch the mole, leading to excoriations, bleeding, or secondary infection, which can then develop into a localized inflammatory reaction. This can look like an irritated rash, especially if the person isn’t carefully observing the underlying mole.
- Amelanotic Melanoma: This is a particularly challenging type of melanoma to diagnose as it lacks the typical dark pigmentation. Amelanotic melanoma can appear as a pink, red, or flesh-colored lesion, sometimes resembling a benign mole, a small lump, a scar, a persistent wart, a bug bite, or even a patch of eczema or dermatitis. These lesions can be flat or raised and may be crusted or ulcerated, making them highly prone to misdiagnosis in Skin rash Skin melanoma images.
- Ulceration or Crusting: An advanced melanoma can ulcerate and bleed, forming a crust. The persistent open wound and surrounding inflammation might be misinterpreted as a persistent sore, a non-healing rash, or an infection, especially if the underlying pigmented lesion isn’t clearly recognized.
- Regression: In some cases, parts of a melanoma might undergo regression, where the immune system attacks and clears some cancer cells. This can leave behind areas of white or grey discoloration, which might be interpreted as scarring or an unusual form of skin irritation rather than a sign of active melanoma.
Conditions that can be confused with Skin melanoma, often due to presenting as a “rash-like” or atypical lesion, include:
- Seborrheic Keratosis: These are common, benign skin growths that often appear as brown, black, or tan lesions with a “pasted-on” or “warty” appearance. They can be itchy, inflamed, and sometimes flake or crust, leading to confusion with melanoma, particularly nodular or ulcerated melanoma. However, unlike melanoma, seborrheic keratoses typically have a very uniform, often greasy, surface and a clearer border.
- Basal Cell Carcinoma (BCC): The most common form of skin cancer, BCC can sometimes present as a red, pearly, or flesh-colored papule that may ulcerate and bleed. While generally distinct from melanoma, pigmented basal cell carcinoma can have dark areas, adding to diagnostic confusion.
- Squamous Cell Carcinoma (SCC): This skin cancer can appear as a red, scaly patch, an open sore, or a raised growth that may crust or bleed. These features can sometimes overlap with an inflamed or ulcerated melanoma.
- Dermatofibroma: These are benign, firm, dome-shaped skin lesions that are often pink, red, or brownish. They can sometimes be itchy or tender and can mimic a small nodular melanoma. A key diagnostic feature is the “dimple sign,” where the lesion indents when squeezed.
- Cherry Angiomas: These are common, benign skin growths made of blood vessels. They appear as small, bright red to purple papules and can sometimes be mistaken for very dark or nodular melanoma, especially if they are thrombosed and appear almost black.
- Eczema or Contact Dermatitis: While typically presenting as widespread itchy, red, and scaly patches, a very localized patch of eczema or dermatitis that becomes chronic or atypical might raise suspicion for an amelanotic melanoma.
- Psoriasis: Localized plaques of psoriasis, especially if irritated or appearing on atypical sites, could be confused with some forms of inflammatory skin cancer.
- Pyogenic Granuloma: This is a benign vascular lesion that grows rapidly and bleeds easily, often resembling an ulcerated or nodular amelanotic melanoma.
Given the potential for misdiagnosis, any persistent, non-healing “rash,” unusual bump, or changing pigmented lesion, especially one that bleeds, itches, or refuses to resolve, must be evaluated by a dermatologist. Professional assessment, often involving dermoscopy and biopsy, is critical for distinguishing true Skin melanoma from benign conditions and ensuring appropriate treatment.
Skin melanoma Treatment
Understanding Skin melanoma treatment options is essential for patients and caregivers, as early and appropriate intervention significantly impacts prognosis. While the previous sections focused on identifying Skin melanoma symptoms pictures, this section outlines the primary therapeutic approaches for this aggressive skin cancer. The choice of treatment depends heavily on the stage of the melanoma, its location, the patient’s overall health, and genetic mutations identified within the tumor. A multidisciplinary team, including dermatologists, surgical oncologists, medical oncologists, and radiation oncologists, typically collaborates to develop a personalized treatment plan for each patient dealing with skin cancer.
Here are the principal Skin melanoma treatment modalities:
Surgical Excision
Surgical removal of the melanoma is the primary treatment for most early-stage melanomas and is often the first step in managing more advanced cases.
- Wide Local Excision: This is the standard surgical procedure where the melanoma, along with a surrounding margin of healthy-appearing skin, is removed. The width of the margin depends on the thickness (Breslow depth) of the melanoma. Thinner melanomas require smaller margins (e.g., 0.5-1 cm), while thicker melanomas require wider margins (e.g., 1-2 cm) to ensure all cancer cells are removed and to minimize the risk of recurrence.
- Sentinel Lymph Node Biopsy (SLNB): For melanomas of intermediate thickness or those with other high-risk features, an SLNB may be performed. This procedure identifies and removes the first lymph node(s) to which the cancer cells would likely spread. If the sentinel node contains cancer, it indicates that the melanoma may have spread beyond the primary site, influencing further treatment decisions.
- Therapeutic Lymph Node Dissection (TLND): If cancer is found in the sentinel lymph nodes, or if enlarged, cancerous lymph nodes are detected clinically, a TLND (also known as a completion lymphadenectomy) may be performed to remove all lymph nodes in the affected area.
Immunotherapy
Immunotherapy harnesses the body’s own immune system to fight cancer cells. It has revolutionized the treatment of advanced melanoma and is now often used in adjuvant settings (after surgery) for earlier stages.
- Checkpoint Inhibitors: These drugs block proteins (like PD-1, PD-L1, or CTLA-4) that normally prevent the immune system from attacking cancer cells. By “releasing the brakes” on the immune system, these inhibitors allow T-cells to recognize and destroy melanoma cells.
- PD-1 Inhibitors: Drugs like pembrolizumab (Keytruda) and nivolumab (Opdivo) are commonly used. They target the PD-1 protein on immune cells.
- CTLA-4 Inhibitors: Ipilimumab (Yervoy) targets the CTLA-4 protein, promoting a more robust anti-tumor immune response.
- Combination Therapy: Combining PD-1 and CTLA-4 inhibitors (e.g., nivolumab plus ipilimumab) can be more effective but may also have increased side effects.
- Oncolytic Virus Therapy: Talimogene laherparepvec (T-VEC, Imlygic) is a modified herpes virus that is injected directly into melanoma tumors. It replicates within the cancer cells, causing them to burst and die, and also stimulates an immune response against the remaining cancer cells.
Targeted Therapy
Targeted therapy focuses on specific genes or proteins in cancer cells that drive their growth and survival. This treatment is effective for melanomas with specific genetic mutations.
- BRAF/MEK Inhibitors: Approximately half of all melanomas have a mutation in the BRAF gene. For these patients, drugs that inhibit BRAF (e.g., vemurafenib, dabrafenib, encorafenib) and/or MEK (e.g., cobimetinib, trametinib, binimetinib) can be highly effective. MEK inhibitors are often used in combination with BRAF inhibitors to enhance efficacy and reduce side effects. These oral medications are particularly powerful for metastatic melanoma with the specific mutation.
Radiation Therapy
Radiation therapy uses high-energy X-rays or other particles to kill cancer cells or inhibit their growth. It is not typically the primary treatment for melanoma but has important roles.
- Adjuvant Radiation: May be used after surgery for patients with high-risk melanomas, particularly those with positive lymph nodes, to reduce the risk of local recurrence.
- Palliative Radiation: Can be used to relieve symptoms caused by advanced melanoma, such as pain from bone metastases or neurological symptoms from brain metastases.
- Radiation for Inoperable Tumors: In some cases, for tumors that cannot be surgically removed due to location or patient health, radiation therapy may be considered.
Chemotherapy
Chemotherapy uses drugs to kill cancer cells. While less effective than immunotherapy and targeted therapy for most melanomas, it still has a role in certain situations.
- Dacarbazine (DTIC) and Temozolomide: These are traditional chemotherapy agents sometimes used for advanced melanoma, especially when immunotherapy or targeted therapy is not an option or has stopped working.
- Combination Chemotherapy: Occasionally, combinations of chemotherapy drugs may be used.
Adjuvant Therapy
Adjuvant therapy refers to additional treatment given after the primary treatment (usually surgery) to kill any remaining cancer cells and reduce the risk of the cancer coming back.
- Immunotherapy (e.g., pembrolizumab, nivolumab) and targeted therapy (e.g., BRAF/MEK inhibitors for BRAF-mutated melanoma) are increasingly being used as adjuvant therapies for patients with Stage IIB/C, Stage III, and even some Stage IV melanomas after complete surgical removal, significantly improving recurrence-free survival.
The field of Skin melanoma treatment is rapidly evolving, with ongoing research continually introducing new and more effective therapies. Patients diagnosed with melanoma should discuss all available treatment options with their oncology team to determine the most appropriate and personalized plan for their specific stage and characteristics of their skin cancer.