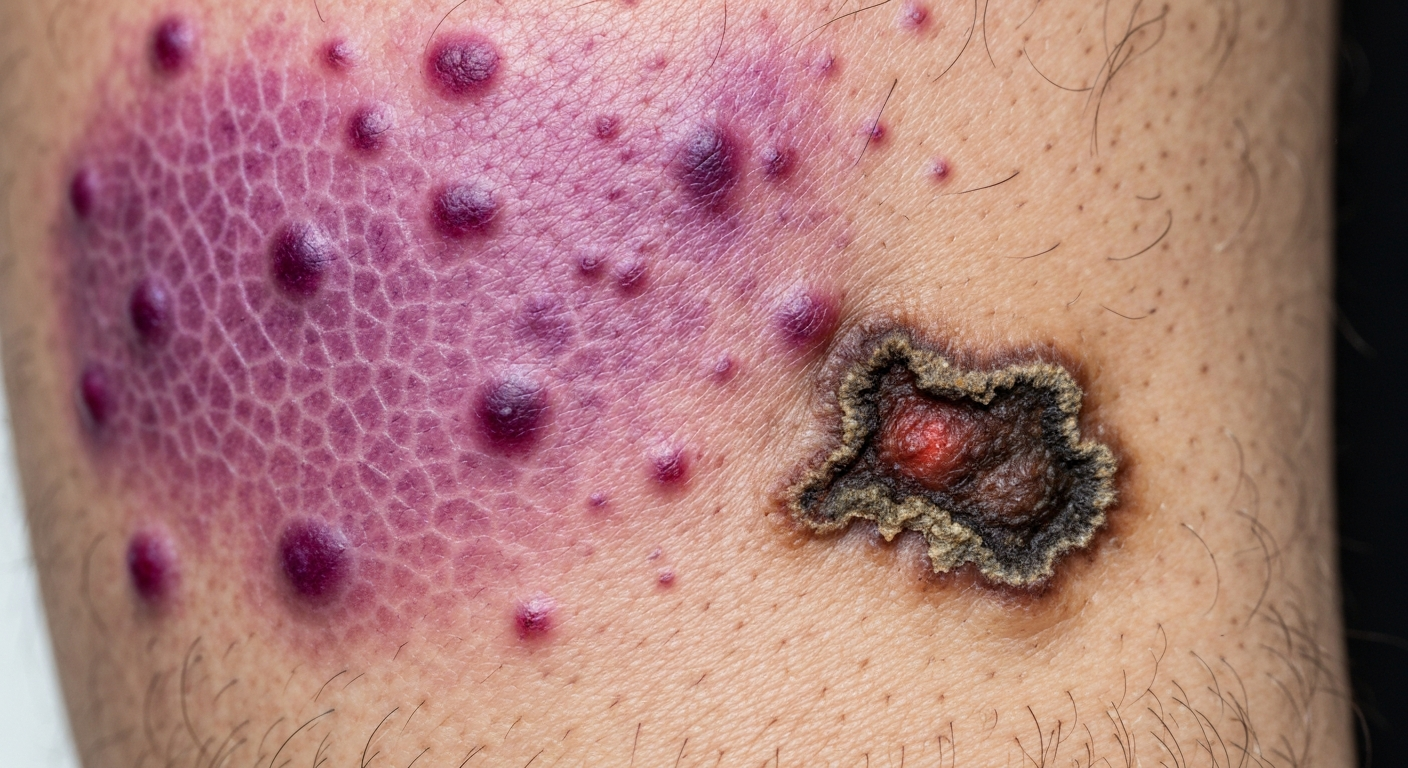
Here are compelling Vasculitis symptoms pictures that showcase the diverse manifestations of this inflammatory condition affecting blood vessels. Understanding these visual cues is crucial for early recognition and management of vasculitis, aiding in prompt diagnosis based on characteristic skin changes.
Vasculitis Symptoms Pictures
Viewing Vasculitis symptoms pictures provides invaluable insight into the varied cutaneous presentations of vessel inflammation. The skin is often the most accessible organ to observe vasculitis, presenting a spectrum of lesions that range from subtle discoloration to severe ulceration. Recognizable patterns in these vasculitis skin manifestations photos help differentiate various types of vasculitis. Common skin findings include palpable purpura, which is a hallmark sign, along with petechiae, ecchymoses, nodules, ulcers, and livedo reticularis. These lesions are direct consequences of blood vessel damage, leakage, and subsequent tissue ischemia. The distribution, morphology, and evolution of these skin changes are critical diagnostic clues in identifying vasculitis. For instance, lesions that are symmetrical or asymmetrical, localized or generalized, or those that favor specific anatomical areas such as the lower extremities, are all important considerations. The presence of pain, itching, or burning associated with these skin changes further supports a diagnosis of vasculitis.
Detailed examination of vasculitis skin lesions photos reveals several key characteristics:
- Palpable Purpura: This is arguably the most common and diagnostically significant cutaneous sign. It appears as raised, red-to-purple lesions that do not blanch under pressure. The palpability arises from perivascular inflammation and extravasation of red blood cells into the dermis. These palpable purpura vasculitis images typically appear on dependent areas like the lower legs and ankles, often in crops.
- Petechiae: Small, pinpoint, non-blanching red or purple spots, usually less than 2 mm in diameter. They indicate minor hemorrhage from capillaries. When numerous and widespread, vasculitis petechiae pictures can suggest a systemic vasculitis.
- Ecchymoses: Larger, non-blanching extravasations of blood, commonly known as bruises. In the context of vasculitis, they can be irregular in shape and may precede ulceration, especially in severe cases. These ecchymoses vasculitis photos demonstrate more extensive vessel damage.
- Nodules: Deep, firm, palpable lesions that can be tender. They represent inflammation in deeper dermal or subcutaneous vessels. Vasculitis nodule images often show erythematous or violaceous nodules that may evolve into ulcerations or necrotic areas.
- Ulcers: Open sores resulting from tissue necrosis due to severe ischemia. These can be very painful, slow to heal, and leave significant scarring. Vasculitis ulcer pictures often depict irregular, deep, punched-out lesions with necrotic bases, indicating severe vascular compromise.
- Livedo Reticularis: A mottled, purplish, net-like discoloration of the skin, caused by impaired blood flow in superficial capillaries. While often benign, when persistent and fixed (not disappearing with warming), livedo reticularis vasculitis images can signal underlying systemic vasculitis, particularly those affecting medium-sized vessels.
- Bullae and Vesicles: Fluid-filled blisters (vesicles are small, bullae are large) can occasionally develop in severe forms of vasculitis where there is significant inflammation and leakage from vessels. Bullous vasculitis photos show these lesions, which often rupture to form ulcers.
- Urticarial Lesions: Hives or wheals that are persistent (lasting more than 24-48 hours in one spot) and often painful or burning rather than itchy, can be a sign of urticarial vasculitis. Urticarial vasculitis pictures may resemble common hives but typically leave a bruise-like discoloration upon fading.
The progression of these symptoms is also key. Initially, a patient might present with erythematous macules (flat red spots) or papules (raised red bumps) that then progress to palpable purpura, and in severe cases, to necrosis and ulceration. The severity of the lesions seen in cutaneous vasculitis symptom pictures often correlates with the extent of systemic involvement, highlighting the importance of thorough evaluation.
Signs of Vasculitis Pictures
Observing signs of vasculitis pictures provides a visual guide to the observable manifestations that point towards blood vessel inflammation. Beyond primary skin lesions, there are other tell-tale signs that can be critical for diagnosis. These signs often reflect not only direct vascular damage but also secondary effects on tissue perfusion and organ function, even if the primary focus remains on cutaneous involvement. Recognizing these subtle or overt signs in vasculitis visual diagnostic aids is paramount for healthcare professionals. The patterns of these signs, their distribution, and their persistence are all crucial pieces of the diagnostic puzzle. The appearance of these signs can vary significantly based on the size of the vessels affected (small, medium, or large) and the specific type of vasculitis.
Key observable vasculitis disease signs photos include:
- Reticular Purpura: A distinct and often alarming sign, characterized by a net-like or branched pattern of purpuric lesions, often with central pallor or necrosis. This “tree-like” pattern suggests occlusion of small-to-medium sized vessels and is a sign of severe ischemia, potentially leading to widespread tissue necrosis. Reticular purpura vasculitis images are indicative of a severe form of vasculitis, often requiring urgent medical attention.
- Digital Ischemia and Gangrene: Reduced blood flow to the fingers and toes can lead to cold, painful digits, color changes (pallor, cyanosis), and ultimately tissue death (gangrene). This is particularly evident in vasculitis affecting medium or large vessels that supply the extremities. Digital ischemia vasculitis pictures show darkened fingertips or toes, often with ulceration or mummification.
- Splinter Hemorrhages: Small, dark red or black streaks under the nails, resembling splinters. These are microinfarcts in the nail bed capillaries and can be a sign of systemic vasculitis, though they can also occur with trauma or endocarditis. Splinter hemorrhage vasculitis photos are subtle but important clues.
- Raynaud’s Phenomenon: While not exclusively a sign of vasculitis, severe and persistent Raynaud’s (triphasic color change in digits upon cold exposure or stress: pallor, cyanosis, then rubor) can be associated with certain types of vasculitis affecting small vessels. Raynaud’s vasculitis images show stark color changes in the digits.
- Cutaneous Infarction: Areas of skin tissue death due to severe arterial occlusion, presenting as well-demarcated, often painful, dark necrotic patches. These can be seen in various sizes and locations. Cutaneous infarction vasculitis photos vividly illustrate the devastating effects of unmanaged vasculitis.
- Mucosal Lesions: Vasculitis can affect mucous membranes, leading to ulcers, petechiae, or bullae in the mouth, nose, or genitals. These mucosal vasculitis pictures are often very painful and can indicate systemic involvement.
- Capillaritis (pigmented purpura): While not strictly vasculitis in all cases, this condition involves inflammation of capillaries, leading to extravasation of red blood cells and hemosiderin deposition, creating rusty, brownish patches, often on the lower legs. Capillaritis images may show the characteristic “cayenne pepper spots.”
- Peripheral Neuropathy: While not a skin sign, the effects of vasculitis on nerves can manifest as sensory changes (numbness, tingling) or motor weakness, which can sometimes be inferred from visible muscle wasting or gait abnormalities, particularly in chronic cases.
Each of these signs, when considered alongside the overall clinical picture and laboratory findings, contributes significantly to pinpointing the specific type of vasculitis. The visual evidence from vasculitis diagnostic signs photos underscores the importance of thorough physical examination and integration of findings.
Early Vasculitis Photos
Recognizing early vasculitis photos is pivotal for timely intervention and preventing disease progression. At its onset, vasculitis may present with subtle and non-specific symptoms, making early diagnosis challenging. However, certain initial skin changes can be highly indicative if carefully observed. These initial vasculitis rash pictures often appear as erythematous (red) macules or papules that might be mistaken for insect bites, allergic reactions, or viral exanthems. What distinguishes early vasculitis is often the persistence of these lesions, their tendency to become purpuric or palpable over hours to days, and sometimes associated symptoms like burning or pain rather than just itching. The progression from simple redness to more definitive signs like palpable purpura is a key characteristic to look for. The location of these early lesions, frequently on dependent areas like the lower extremities, is also an important clue.
Common presentations in first signs of vasculitis images include:
- Erythematous Macules and Papules: Initially, lesions may appear as flat or slightly raised red spots. These are often transient or evolve quickly. Early erythematous vasculitis pictures show these vague reddened areas that precede more definite changes.
- Urticarial-like Lesions: Some forms of vasculitis, particularly urticarial vasculitis, can begin with lesions resembling hives. However, unlike typical urticaria, these lesions tend to be more painful than itchy, persist in one location for over 24-48 hours, and often leave a purpuric or bruised appearance upon fading. Early urticarial vasculitis photos demonstrate this atypical presentation.
- Pinpoint Petechiae: Very small, non-blanching red dots can be among the earliest visible signs, indicating initial capillary damage. These early petechiae vasculitis images can be subtle and easily overlooked.
- Subtle Purpuric Macules: Before becoming fully palpable, purpura can start as flat, non-blanching red or purple spots. Careful observation, perhaps with a dermatoscope, can reveal these changes. Subtle purpuric vasculitis pictures emphasize the importance of close examination.
- Non-specific Rash with Systemic Symptoms: Sometimes, a vague skin rash may accompany systemic symptoms like fever, joint pain, or fatigue. While not diagnostic on its own, a persistent, unusual rash in conjunction with these symptoms warrants further investigation for vasculitis.
- Mild Livedo Reticularis: A faint, often transient, net-like pattern that may become more pronounced with cold exposure. In its early stages, it might not be fixed or prominent, but its presence can be a precursor to more severe vascular compromise. Early livedo reticularis photos show a subtle, reddish-blue mottling.
- Morning Stiffness and Joint Pain with Rash: Though not a direct skin sign, the combination of joint symptoms and a new or evolving skin rash, particularly on the extremities, should raise suspicion for systemic vasculitis.
The challenge with early vasculitis images is that many other conditions can mimic these initial presentations. Therefore, a high index of suspicion, coupled with monitoring for progression and the development of more characteristic signs, is essential for accurate and timely diagnosis. Healthcare providers often rely on a combination of visual cues, patient history, and laboratory tests to confirm vasculitis in its nascent stages.
Skin rash Vasculitis Images
A diverse array of skin rash vasculitis images illustrates the spectrum of cutaneous involvement in vasculitis, from localized lesions to widespread eruptions. The appearance of the rash is highly dependent on the size of the blood vessels affected (small, medium, or large) and the specific immune mechanisms at play. Understanding the morphology and distribution of these vasculitic rashes is crucial for classification and guiding treatment strategies. These vasculitic rash types photos help distinguish between different clinical entities within the broad category of vasculitis, each with its own prognosis and treatment implications. The skin rash in vasculitis is not merely a superficial problem; it often serves as a window into the systemic nature of the disease, reflecting inflammation in deeper organs. The location of the rash, whether it is symmetrical or asymmetrical, and its tendency to recur or progress are all important aspects when reviewing cutaneous vasculitis rash images.
A comprehensive look at various vasculitis skin rash patterns pictures includes:
- Leukocytoclastic Vasculitis (LCV) Rash: The most common form of cutaneous vasculitis, typically presenting as palpable purpura, primarily on the lower extremities. Lesions can also include papules, nodules, vesicles, bullae, and ulcers. LCV rash pictures often show lesions in various stages of evolution, reflecting ongoing inflammation.
- Hypersensitivity Vasculitis Rash: Often synonymous with LCV when the cause is related to drugs or infections. The rash is characteristically palpable purpura, localized or widespread, and may be accompanied by joint pain, fever, and kidney involvement. Hypersensitivity vasculitis rash images will display similar features to LCV.
- Henoch-Schönlein Purpura (IgA Vasculitis) Rash: Characterized by palpable purpura, often with an abdominal component (pain), joint involvement (arthritis), and kidney disease (glomerulonephritis). The rash is typically found on the lower extremities and buttocks, and sometimes on the arms and trunk. Henoch-Schönlein Purpura rash pictures distinctly show these purpuric lesions, particularly in children.
- Polyarteritis Nodosa (PAN) Rash: Affects medium-sized arteries, leading to diverse cutaneous manifestations. The rash can include tender subcutaneous nodules along the course of vessels, livedo reticularis, ulcers, and gangrene. PAN vasculitis rash images might show a combination of these severe symptoms.
- Granulomatosis with Polyangiitis (GPA) (Wegener’s) Rash: While predominantly affecting the respiratory tract and kidneys, GPA can cause various skin lesions, including palpable purpura, subcutaneous nodules, ulcers, and papulonecrotic lesions. Specific to GPA, patients may develop “strawberry gingivitis” (hypertrophic, friable gingivae) and nasal septal perforations. GPA skin rash pictures reflect these diverse and sometimes necrotic lesions.
- Eosinophilic Granulomatosis with Polyangiitis (EGPA) (Churg-Strauss) Rash: Often associated with asthma and eosinophilia. Cutaneous manifestations include palpable purpura, subcutaneous nodules, and sometimes urticarial lesions or livedo reticularis. EGPA vasculitis rash images might show purpuric eruptions along with tender nodules.
- Cryoglobulinemic Vasculitis Rash: Associated with cryoglobulins (antibodies that precipitate in the cold), this vasculitis often presents with palpable purpura, livedo reticularis, ulcers, and Raynaud’s phenomenon, particularly in cold-exposed areas. Cryoglobulinemic vasculitis pictures distinctly show purpura and severe livedo reticularis, often with accompanying leg ulcers.
- Urticarial Vasculitis Rash: A variant where persistent urticarial lesions (hives that last >24-48 hours in one spot) are caused by vasculitis in the superficial dermis. These are often burning or painful and leave post-inflammatory hyperpigmentation or bruising. Urticarial vasculitis rash photos demonstrate this persistent, bruise-like urticaria.
- Erythema Elevatum Diutinum (EED): A rare, chronic, benign form of cutaneous vasculitis presenting with persistent, red-to-yellowish-brown papules, plaques, and nodules, often symmetrically distributed over extensor surfaces. EED vasculitis pictures show these distinctive, chronic lesions.
The detailed examination of skin rash vasculitis images, coupled with a thorough medical history, physical examination, and appropriate laboratory and biopsy findings, is crucial for accurate diagnosis and management. The varied presentations underscore the complexity and systemic nature of vasculitis.
Vasculitis Treatment
Effective Vasculitis treatment aims to suppress the immune system, reduce inflammation, and prevent further damage to blood vessels and organs, thereby managing symptoms and improving patient outcomes. While this article focuses on symptoms, understanding the general approach to treatment is essential for patients and caregivers who observe vasculitis symptoms pictures. Treatment regimens are highly individualized, depending on the type of vasculitis, its severity, the organs involved, and the patient’s overall health. Early diagnosis, often guided by recognition of cutaneous symptoms and signs, is critical for initiating prompt and appropriate therapy to minimize long-term complications. The goal is not only to achieve remission but also to maintain it and manage any residual symptoms or organ damage.
Key components of managing vasculitis symptoms through treatment include:
- Corticosteroids: These are often the first-line therapy for most forms of vasculitis due to their potent anti-inflammatory and immunosuppressive effects. High doses may be used initially to induce remission, followed by a gradual tapering over several months or longer. Common examples include prednisone and methylprednisolone. Corticosteroids significantly reduce inflammation seen in vasculitis inflammation pictures.
- Immunosuppressants (Conventional): For more severe or persistent cases, or to allow for corticosteroid dose reduction, other immunosuppressive drugs are added. These include:
- Cyclophosphamide: A powerful immunosuppressant used in severe, life-threatening vasculitis, particularly those affecting the kidneys, lungs, or brain.
- Methotrexate: Often used for maintenance therapy or less severe forms, particularly in combination with corticosteroids.
- Azathioprine: Another agent frequently used for maintenance of remission, especially after cyclophosphamide.
- Mycophenolate Mofetil: An alternative for maintenance therapy or when other immunosuppressants are not tolerated.
These agents help prevent the immune system from attacking blood vessels, thereby reducing the progression seen in severe vasculitis lesion progression photos.
- Biologic Agents: These newer therapies target specific components of the immune system.
- Rituximab: A monoclonal antibody that targets B cells, commonly used in ANCA-associated vasculitis (GPA, MPA, EGPA) for induction and maintenance of remission.
- Tocilizumab: An IL-6 receptor blocker, approved for Giant Cell Arteritis.
- Mepolizumab: An anti-IL-5 monoclonal antibody, specifically for EGPA.
- Avacopan: A C5a receptor inhibitor, used for ANCA-associated vasculitis.
These agents provide targeted immunosuppression, often with fewer side effects than broad-spectrum immunosuppressants. They are vital in controlling the systemic aspects reflected in severe vasculitis organ involvement images.
- Symptomatic and Supportive Care:
- Pain Management: Analgesics for pain associated with lesions, ulcers, or joint involvement.
- Wound Care: For ulcers or necrotic lesions, meticulous wound care is essential to prevent infection and promote healing. This directly addresses the visible damage in vasculitis ulcer healing pictures.
- Blood Pressure Control: Important, especially if kidney involvement is present.
- Physical Therapy: To maintain joint mobility and muscle strength, particularly if there is neurological involvement or prolonged immobility.
- Lifestyle Modifications: Avoiding triggers (e.g., cold exposure for cryoglobulinemic vasculitis), smoking cessation, and a healthy diet.
- Immunoglobulin Therapy (IVIG): In certain severe, refractory cases, or during pregnancy.
- Plasma Exchange (Plasmapheresis): Used in rapidly progressive and severe forms of vasculitis (e.g., ANCA-associated vasculitis with severe kidney or lung involvement) to quickly remove harmful antibodies from the blood.
The duration of vasculitis therapy can range from several months to years, and some patients may require lifelong maintenance therapy. Regular monitoring for disease activity and treatment-related side effects is crucial. This includes blood tests, urine tests, and imaging studies to assess organ involvement. A multidisciplinary approach, involving rheumatologists, dermatologists, nephrologists, neurologists, and other specialists, is often necessary to provide comprehensive care for patients with vasculitis. The ultimate goal is to achieve long-term remission, improve quality of life, and minimize the visible and internal damage illustrated in vasculitis pathology pictures.