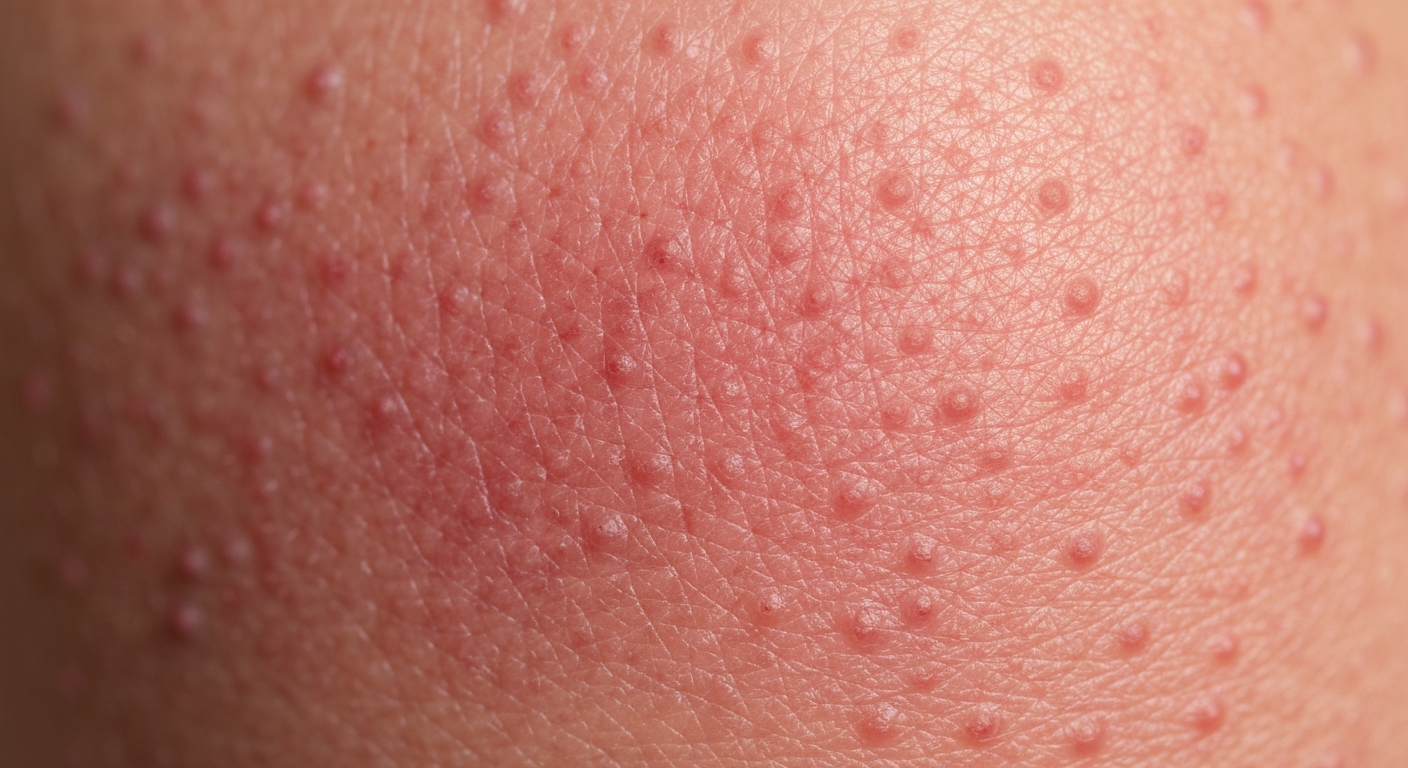
What Does A Yeast Infection Look Like Symptoms Pictures can reveal a wide spectrum of appearances depending on the affected body part, but typically involve distinct patterns of redness, inflammation, and characteristic discharges or lesions. Understanding these visual cues is crucial for identifying potential candidiasis and seeking appropriate care. These visual characteristics are often accompanied by intense itching and discomfort.
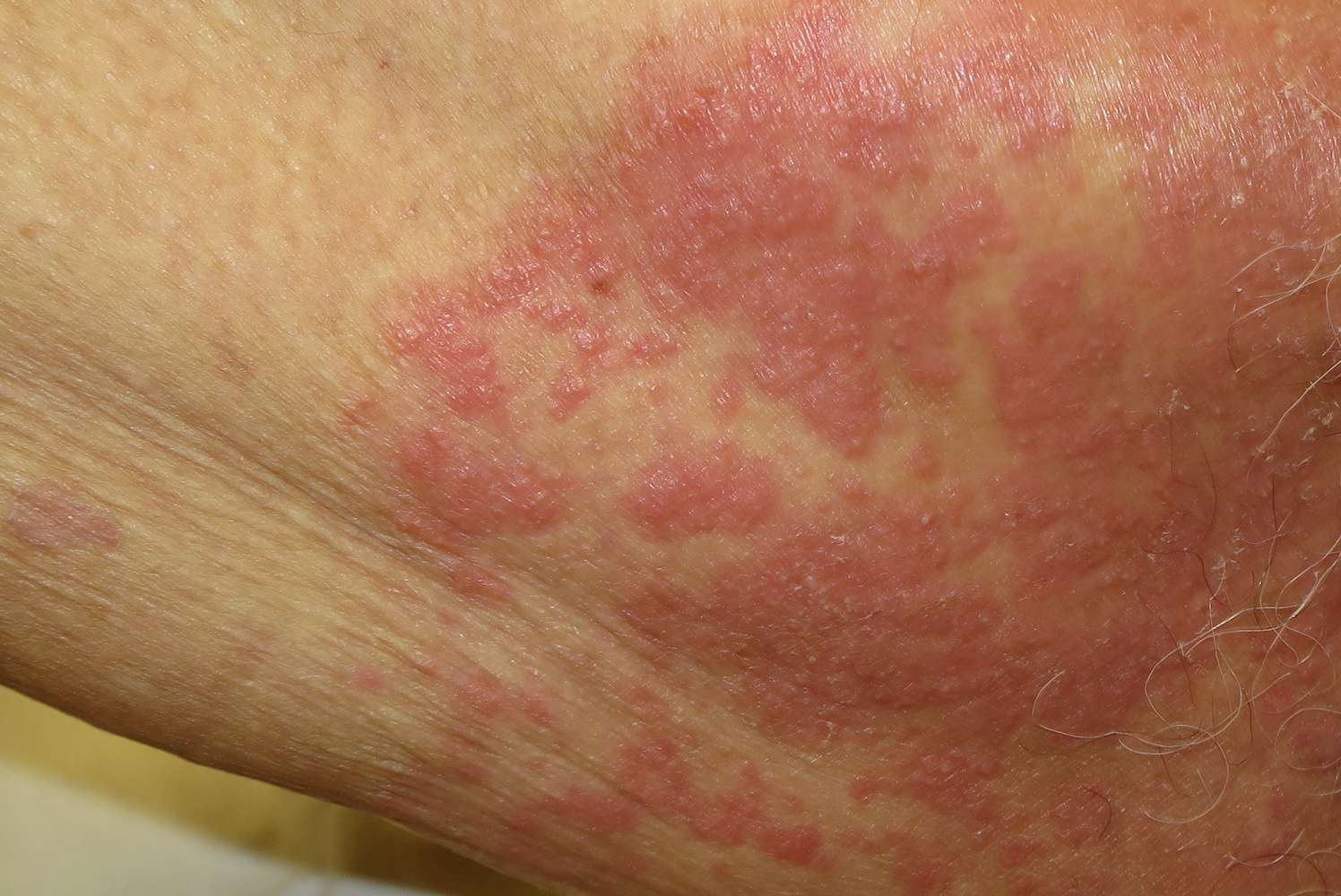
Yeast infection Symptoms Pictures
Visual identification of a yeast infection, also known as candidiasis, often begins with observing distinct changes on the skin or mucous membranes. The appearance can vary significantly based on the location of the infection, but common themes include redness, swelling, and specific types of lesions or discharges. For instance, a vaginal yeast infection presents with classic symptoms that are clearly visible upon examination, including changes in the vulva and vagina itself. A penile yeast infection will show different but equally distinctive visual cues on the glans and foreskin. Oral thrush, common in infants and immunocompromised individuals, manifests with a unique white coating inside the mouth, which can sometimes extend to the throat.
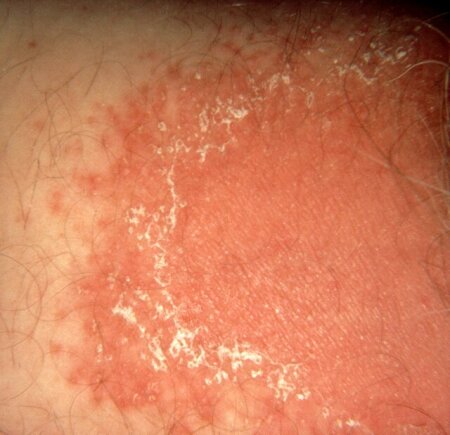
Vaginal Yeast infection Pictures
A vaginal yeast infection, or vulvovaginal candidiasis, presents with several unmistakable visual symptoms. The vulva, the external genital area, often appears distinctly inflamed. This inflammation typically manifests as intense redness, known as erythema, which can range from a bright pink to a deep, fiery red. Swelling of the labia minora and majora is also common, making the tissues look puffy and sometimes shiny. Upon closer inspection, the skin of the vulva may appear irritated and possibly excoriated due to persistent scratching. Tiny cracks or fissures, particularly in the skin folds, might also be present, which can be painful and indicate the severity of the inflammation.
Internally, the vaginal walls can also exhibit significant signs of inflammation. A prominent visual symptom is the characteristic vaginal discharge. This discharge is typically thick, white, and often described as having a cottage cheese-like or clumpy consistency. It may adhere to the vaginal walls or collect in the vaginal opening. Unlike some bacterial infections, yeast infection discharge usually has little to no odor, or a very faint, yeasty smell. The vaginal mucosa itself may appear red and swollen, and in more severe cases, white patches or plaques resembling the discharge can be seen adhering to the walls, which might be difficult to wipe away without causing some irritation or bleeding.
- Vulvar Redness: Intense erythema, ranging from bright pink to fiery red, often extending to the perineum.
- Vulvar Swelling: Noticeable puffiness or edema of the labia, making the tissues appear distended.
- Vaginal Discharge: Thick, white, clumpy, cottage cheese-like discharge, often without strong odor.
- Mucosal Plaques: White, adherent patches or films on the vaginal walls, often difficult to remove.
- Fissures/Cracks: Small, painful cracks in the skin folds of the vulva, indicative of severe irritation.
- Excoriation: Scratches or skin damage on the vulva due to intense itching.
Oral Thrush (Oropharyngeal Candidiasis) Pictures
Oral thrush, or oropharyngeal candidiasis, presents with very distinct visual characteristics inside the mouth. The most prominent symptom is the appearance of creamy white lesions or patches on various surfaces within the oral cavity. These patches are commonly found on the tongue, inner cheeks, roof of the mouth (palate), and sometimes on the tonsils and back of the throat. The texture of these lesions is often described as curd-like or cottage cheese-like, and they may be slightly raised.
A key diagnostic feature of these white patches is that they can usually be scraped off. However, attempting to scrape them off often reveals underlying red, inflamed, and sometimes bleeding tissue. This underlying redness, known as erythema, is another significant visual sign of oral candidiasis. In more severe cases, especially in immunocompromised individuals, these patches can become extensive, covering large areas of the mouth and making eating and swallowing painful. The corners of the mouth might also show signs of angular cheilitis, characterized by redness, cracking, and scaling at the commissures, which is also a form of yeast infection.
- White Patches: Creamy, curd-like white lesions on the tongue, inner cheeks, palate, or tonsils.
- Underlying Redness: Erythema and inflammation revealed when white patches are scraped away, sometimes with minor bleeding.
- Raised Lesions: Patches may appear slightly elevated from the mucosal surface.
- Angular Cheilitis: Redness, cracking, and scaling at the corners of the mouth.
- Glossitis (rare): Swelling and redness of the tongue, possibly with papillae atrophy.
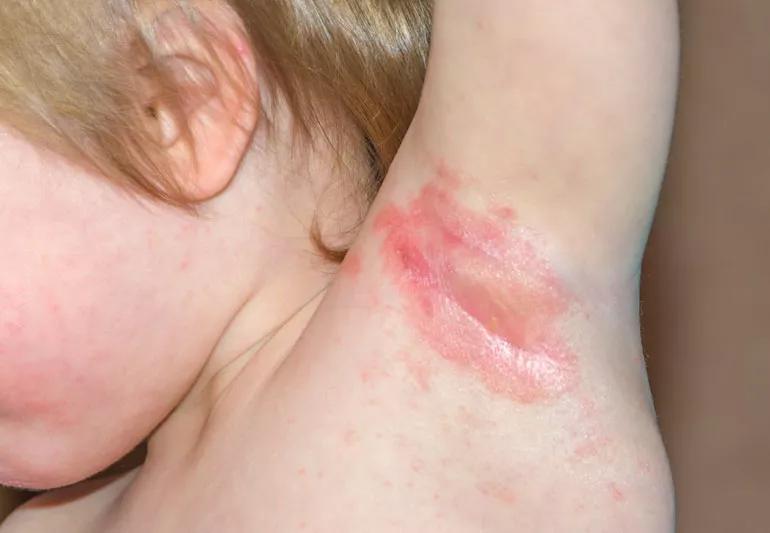
Skin Fold Yeast infection (Intertrigo) Pictures
Candidal intertrigo is a yeast infection that occurs in skin folds, where moisture and friction create an ideal environment for yeast proliferation. Common locations include under the breasts, in the armpits, in the groin folds (inguinal region), between the buttocks, and in abdominal skin folds (pannus). The classic visual presentation of intertrigo is a brightly erythematous (red) rash, often with a moist or macerated appearance in the center of the fold. The redness is typically well-demarcated, meaning it has a clear, defined border.
A hallmark visual sign of candidal intertrigo, which helps differentiate it from other skin irritations, is the presence of “satellite lesions.” These are smaller, often pustular or papular lesions that appear just outside the main erythematous patch, scattered like satellites around a planet. The skin within the main rash can look shiny, glazed, and sometimes scaly or peeling at the edges. Small erosions, crusting, or even superficial pustules may be observed, particularly in the deepest parts of the fold. The affected area often has a distinct, unpleasant yeasty odor due to microbial overgrowth and skin maceration.
- Bright Red Rash: Intense erythema within the skin fold, often with a glistening appearance.
- Well-Demarcated Borders: Clear and distinct edges of the rash.
- Satellite Lesions: Small papules or pustules scattered beyond the main border of the rash.
- Maceration: Whitish, soggy appearance of the skin in the center of the fold due to moisture.
- Scaling/Peeling: Fine scaling or peeling skin, especially at the periphery of the rash.
- Small Pustules/Vesicles: Tiny fluid-filled bumps or pus-filled lesions within the rash.
- Fissures: Cracks in the deepest parts of the skin folds, particularly if severe.
Signs of Yeast infection Pictures
The signs of a yeast infection provide crucial visual clues for diagnosis. These signs move beyond general symptoms to specific, observable characteristics that can be captured in pictures. These include the texture of lesions, specific patterns of spread, and the nature of any associated discharge or skin changes. Recognizing these distinct visual signs across different body locations is key to identifying candidal infections effectively. For instance, the unique pattern of satellite lesions in skin folds is a very specific sign. Similarly, the ability to scrape away white patches in oral thrush, revealing an erythematous base, is a tell-tale sign.
Penile Yeast infection (Candidal Balanitis) Pictures
Candidal balanitis, a yeast infection affecting the head of the penis (glans) and sometimes the foreskin, presents with several distinct visual signs. The most common sign is redness (erythema) and inflammation of the glans. This redness can be diffuse or appear in patchy areas. Small, shiny red bumps or papules are frequently observed on the glans, and these may sometimes be associated with tiny pustules. The skin of the glans and foreskin can also appear irritated, swollen, and sometimes glistening or macerated, especially in uncircumcised men where moisture can accumulate under the foreskin.
Another common sign is an itchy, burning sensation, which may lead to excoriation (skin damage from scratching). In some cases, a white, thick, or cheesy discharge may accumulate under the foreskin or in the coronal sulcus (the groove between the glans and the shaft). This discharge is visually similar to the cottage cheese-like discharge seen in vaginal yeast infections. The skin might also show areas of peeling or desquamation, particularly if the infection has been present for some time. Fissures or cracks, especially around the meatus (urethral opening) or foreskin, can also be present, indicating a more severe inflammatory response.
- Redness (Erythema): Inflammation of the glans and/or foreskin, often appearing patchy or diffuse.
- Small Red Bumps/Papules: Tiny, shiny red lesions on the glans, sometimes with satellite lesions.
- Pustules: Small, pus-filled bumps, particularly around the inflamed areas.
- Swelling: Mild to moderate edema of the glans and foreskin.
- White Discharge: Thick, cheesy, or cottage cheese-like substance under the foreskin or in the coronal sulcus.
- Peeling Skin: Areas of desquamation or flaking on the glans or foreskin.
- Fissures: Cracks in the skin, especially around the foreskin or meatus, often painful.
Diaper Rash Yeast infection Pictures
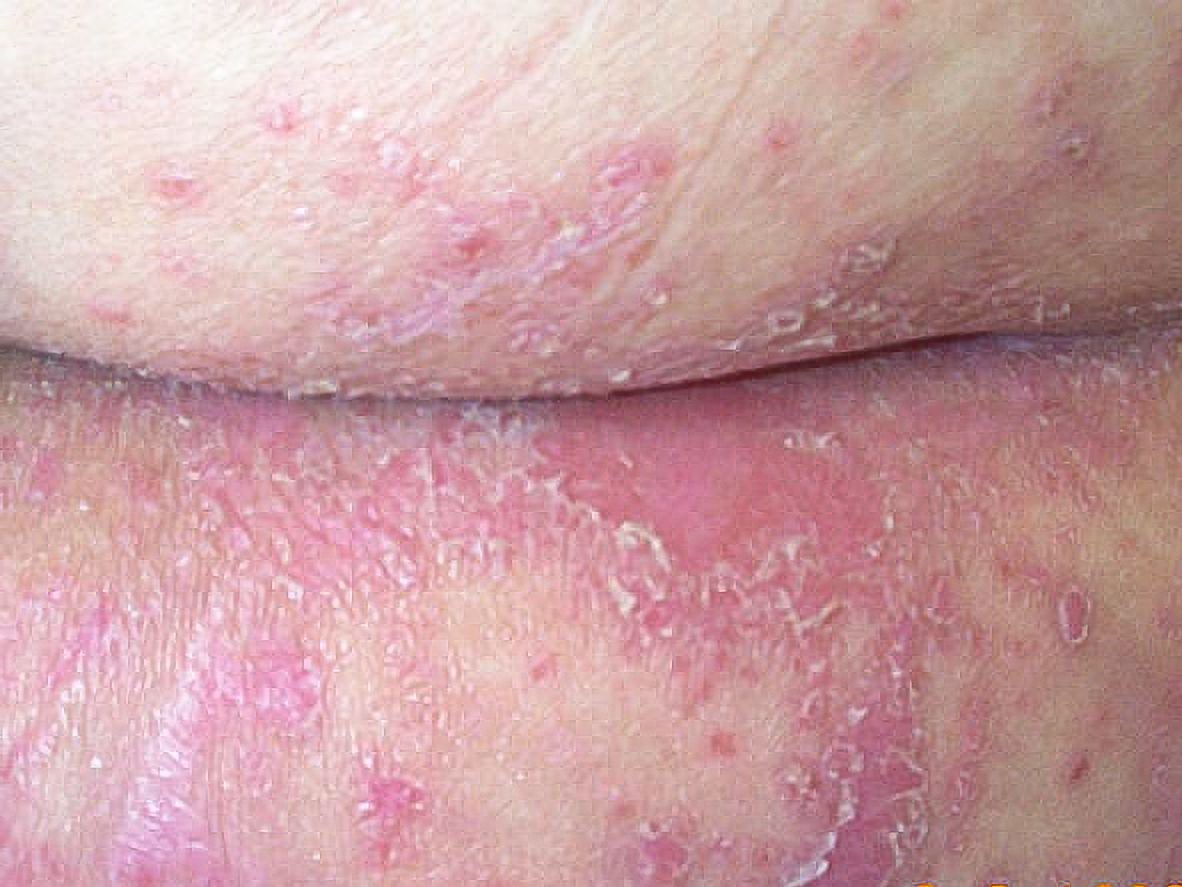
A diaper rash complicated by a yeast infection (candidal diaper dermatitis) has specific visual signs that differentiate it from regular irritant diaper rash. While an irritant diaper rash typically affects convex surfaces (where the diaper rubs), a candidal diaper rash often involves skin folds (groin creases, around the genitals) and exhibits a characteristic bright red, beefy appearance. The borders of the rash are usually well-defined and can have a raised, scaly edge. The skin within the rash might look shiny and moist.
The most distinctive sign, similar to candidal intertrigo, is the presence of satellite lesions. These are small, erythematous papules or pustules scattered beyond the main border of the confluent redness, extending into surrounding healthy-looking skin. These satellite lesions are a strong indicator of a yeast component. In severe cases, the skin can appear raw, weeping, or even ulcerated, especially if left untreated. The anus and buttocks may also show involvement. The rash often appears more intense and persistent than a typical irritant diaper rash, failing to respond to conventional barrier creams alone.
- Bright Red, Beefy Rash: Intense erythema, often appearing glossy, primarily in skin folds and around genitals.
- Well-Demarcated Borders: Sharp, clear edges of the rash, often with a slightly raised, scaly rim.
- Satellite Lesions: Small red papules or pustules scattered beyond the main rash border.
- Moist/Weeping Skin: Skin may appear wet or oozing in the affected areas.
- Pustules/Vesicles: Tiny fluid-filled or pus-filled bumps, particularly in the folds.
- Raw/Eroded Areas: Skin may appear denuded or ulcerated in severe cases.
Nail Yeast infection (Candidal Onychomycosis/Paronychia) Pictures
Yeast infections affecting the nails (onychomycosis) or the skin around the nails (paronychia) present with specific visual signs. Candidal onychomycosis typically causes the nail plate to become discolored, often turning white, yellow, brown, or even greenish. The nail may also become thickened, brittle, and develop ridges or grooves. In some cases, the nail can separate from the nail bed (onycholysis). The infection often starts at the nail folds and spreads to the nail plate, particularly in individuals with chronic moisture exposure.
Candidal paronychia, an infection of the nail fold, is characterized by redness, swelling, and tenderness of the skin surrounding the nail, often at the base or sides. The cuticle may be absent, and pus can sometimes be expressed from under the nail fold, especially if a secondary bacterial infection is present. The nail itself may develop transverse ridges or discoloration as a result of the inflamed matrix. Chronic paronychia, common in individuals whose hands are frequently wet (e.g., dishwashers, healthcare workers), can lead to significant deformity of the nail plate over time. These visual signs can be quite painful and persistent if not addressed.
- Nail Discoloration: White, yellow, brown, or greenish discoloration of the nail plate.
- Nail Thickening: Hypertrophy of the nail plate, making it appear thicker and sometimes crumbly.
- Nail Ridges/Grooves: Development of lines or depressions across the nail.
- Onycholysis: Separation of the nail plate from the nail bed.
- Red/Swollen Nail Folds: Erythema and edema of the skin surrounding the nail, often tender.
- Pus Exudate: Possible pus drainage from under the inflamed nail fold (paronychia).
- Cuticle Loss: Absence or retraction of the cuticle.
Early Yeast infection Photos
Identifying an early yeast infection through photos can be challenging as the initial signs are often subtle before significant inflammation or discharge develops. However, recognizing these nascent visual changes can lead to quicker treatment and prevent the infection from worsening. Early stages are characterized by mild irritation, slight discoloration, and sometimes a barely noticeable change in texture. These early signs of candidiasis should not be overlooked, particularly in individuals prone to recurrent infections. Early detection through visual cues can significantly improve outcomes.
Early Vaginal Yeast infection Pictures
In the very early stages of a vaginal yeast infection, the visual symptoms may be quite subtle. There might be a slight, barely perceptible redness or pinkness of the vulvar skin, rather than the intense fiery red seen in more advanced infections. Minor swelling may be present, making the labia look slightly plumper than usual. The initial discharge may not yet be the thick, clumpy, cottage cheese-like consistency; instead, it might appear as a slightly increased amount of clear or milky white discharge, perhaps a little thicker than normal, but not yet overtly clumpy. Women might notice an unusual moistness or a mild, uncharacteristic film on the vulva. The itching sensation might be mild at this point, leading to only occasional scratching, and excoriations would typically be absent. A slight burning sensation might be present, particularly during urination or intercourse, even without prominent visible signs.
- Mild Vulvar Pinkness/Redness: A faint erythema, less intense than a full-blown infection.
- Slight Labial Swelling: Barely noticeable puffiness of the labia.
- Subtle Discharge Change: Slightly increased, perhaps milky white or slightly thicker than usual, not yet clumpy.
- Minimal Irritation: Skin might look slightly sensitive but without significant excoriation.
- No Prominent Fissures: Cracks or deep irritation are typically absent in the early stages.
Early Oral Thrush Photos
The initial manifestation of oral thrush can be very localized and subtle. Small, pinhead-sized white spots or patches may appear on the tongue or inner cheeks. These early lesions might resemble milk residue or small food particles. Unlike milk, however, they will likely be difficult to wipe away with a gentle rub. The underlying tissue might show only a very faint pinkness or mild redness when the white spots are disturbed, not the deep erythema seen in more established thrush. The patches might not be extensive or confluent, appearing as isolated spots. Infants might show these tiny white spots without significant distress, and adults might notice a slightly altered taste or a mild sensation of “fuzziness” in the mouth before the patches become more prominent. The lips might also show very slight drying or a hint of angular cheilitis at the corners, but without severe cracking.
- Tiny White Spots: Small, isolated white patches, often resembling milk curds, on the tongue or inner cheeks.
- Faint Underlying Redness: Minimal erythema when attempting to remove the spots.
- Localized Patches: Not yet widespread or confluent over large areas of the mouth.
- Subtle Oral Sensation: A mild “furry” feeling or altered taste before visible lesions become prominent.
- Minimal Angular Cheilitis: Very slight redness or dryness at the mouth corners, not yet cracked.
Early Skin Fold Yeast infection Photos
An early candidal intertrigo might begin with a diffuse, mild pinkish-red discoloration in the deepest part of a skin fold, such as under the breast or in the groin. The skin might feel slightly moist or warm, but overt maceration (whitish, soggy appearance) might not yet be present. Satellite lesions, a key indicator, are usually absent in the earliest stages or are very few and tiny, easily overlooked. The edges of the rash might not be sharply demarcated initially; instead, the redness might fade subtly into surrounding normal skin. There might be a mild itching sensation, but significant scaling, pustules, or erosions are generally not visible at this point. The skin might just look generally irritated or slightly inflamed, rather than exhibiting the full spectrum of a well-established candidal intertrigo. The area might only show a slight sheen due to increased moisture.
- Diffuse Mild Pinkness: Faint erythema in the deepest part of a skin fold.
- Subtle Moisture/Warmth: Increased dampness without overt maceration or weeping.
- Absent/Sparse Satellite Lesions: Very few or no smaller lesions outside the main rash area.
- Indistinct Borders: Redness that gradually blends into normal skin, not sharply defined.
- No Significant Scaling/Pustules: Clear signs of irritation and deeper lesions are typically absent.
Skin rash Yeast infection Images
Yeast infections manifest on the skin in various forms, often mimicking other dermatological conditions. However, candidal rashes have unique visual characteristics that distinguish them. These rashes can appear in virtually any skin fold, under occlusive dressings, or areas subjected to chronic moisture. The appearance is often fiery red, glistening, and can be accompanied by peculiar satellite lesions. Understanding these patterns is essential for accurate identification through pictures, especially when differentiating from bacterial infections, fungal infections (dermatophytes), or irritant dermatitis. The specific morphology of the lesions, including pustules, vesicles, and erosions, provides critical diagnostic information.
Groin Yeast infection (Tinea Cruris vs. Candidal Intertrigo) Pictures
A yeast infection in the groin (candidal intertrigo) shares some similarities with tinea cruris (jock itch), which is caused by dermatophyte fungi, but has distinct visual differences. Candidal intertrigo in the groin presents as a bright red, often moist or weeping rash that typically involves the skin folds, including the labia in women or the scrotum in men, and extends onto the inner thighs. The color is usually a more intense, beefy red compared to the often duller, brownish-red of tinea cruris. A key differentiating visual feature for candidal intertrigo is the presence of satellite lesions: small papules or pustules scattered around the main, confluent erythematous patch. The border of candidal intertrigo is usually sharp and clearly defined, but unlike tinea cruris, it typically does not have a raised, active, scaly edge with central clearing. The skin often appears macerated in the depths of the folds. Tinea cruris, conversely, often presents with a more annular (ring-shaped) appearance, a distinct raised, scaly, active border, and central clearing, and typically spares the scrotum. The visual characteristics of the scaling also differ, with candidiasis often having more fine, superficial scaling or a glistening appearance, whereas tinea cruris can have more prominent, coarser scales.
- Bright Red/Beefy Rash: Intense erythema in groin folds and surrounding skin.
- Moist/Weeping Appearance: Skin often appears damp and macerated in the folds.
- Satellite Lesions: Small papules or pustules scattered beyond the main rash border, a critical visual differentiator.
- Sharp, Defined Borders: Clear demarcation of the rash, but often lacks the raised active border of tinea cruris.
- Involvement of Scrotum/Labia: Candidal intertrigo frequently involves these areas, unlike tinea cruris.
- Fine Scaling/Glistening: Skin may show fine scales or a shiny, glazed look.
- Fissures/Cracks: Common in deep folds due to inflammation and moisture.
Foot Yeast infection (Interdigital Candidiasis) Pictures
While most common foot fungal infections are caused by dermatophytes (tinea pedis), yeast can also infect the feet, particularly between the toes (interdigital candidiasis). This infection is typically found in the web spaces, most often between the fourth and fifth toes, where conditions are warm and moist. The visual presentation includes significant redness, maceration (whitish, soggy, soggy appearance of the skin), and often painful erosions or fissures. The skin in the affected web space will appear intensely red, often peeling or flaking at the edges. Unlike tinea pedis, which can present with scaling and dryness, interdigital candidiasis is typically very moist and sometimes exudes a watery discharge. The borders are often ill-defined, blending into the macerated skin. Pustules or small vesicles may also be seen. The area is usually very itchy and can have a distinct, somewhat sweet or “yeasty” odor. The infection can sometimes spread to the sole of the foot or other toes, but is most characteristic in the interdigital spaces. If severe, a white, thick film of macerated skin can be pulled away, revealing raw, red skin underneath.
- Intense Redness: Fiery red erythema in the web spaces between toes.
- Maceration: Whitish, soggy, waterlogged appearance of the skin.
- Erosions/Fissures: Painful cracks or raw areas in the skin.
- Peeling/Flaking Skin: Desquamation, particularly at the edges of the affected area.
- Moist Exudate: Often appears very damp, sometimes with clear fluid.
- Pustules/Vesicles: Small fluid-filled or pus-filled bumps may be present.
- Ill-Defined Borders: The redness often merges gradually with surrounding skin.
Generalized Skin Candidiasis Pictures
While localized yeast infections are common, generalized cutaneous candidiasis can occur, especially in individuals with compromised immune systems, diabetes, or in very moist environments. The visual presentation can be extensive, covering large areas of the trunk, limbs, or back. It manifests as confluent patches of bright red erythema, often with the characteristic satellite lesions extending outwards. The skin may appear shiny, inflamed, and sometimes edematous. Small pustules or vesicles might be scattered throughout the affected areas. In severe cases, the skin can become severely exfoliated or denuded, leading to large areas of raw, weeping skin. The rash can be intensely itchy and uncomfortable, leading to significant excoriation. The patterns can be quite varied, from widespread intertrigo-like eruptions in multiple skin folds to a more generalized folliculitis-like appearance with multiple small pustules around hair follicles. Recognition in images depends on identifying the consistent theme of intense erythema, moisture, and satellite lesions across disparate skin areas.
- Widespread Erythema: Extensive areas of bright red, inflamed skin over the trunk, limbs, or multiple skin folds.
- Confluent Patches: Red areas that merge into larger, continuous rashes.
- Satellite Lesions: Distinct small papules or pustules scattered peripherally to the main rash, a key indicator.
- Shiny/Glistening Appearance: Due to inflammation and moisture accumulation.
- Scattered Pustules/Vesicles: Small bumps containing pus or fluid throughout the rash.
- Exfoliation/Erosion: Peeling or raw areas, particularly in severe or chronic cases.
- Folliculitis-like Pattern: Sometimes presents as pustules centered around hair follicles.
Yeast infection Treatment
While this article focuses on the visual aspects of yeast infections, understanding how treatment impacts these visual signs is crucial. Treatment aims to eliminate the Candida fungus, thereby resolving the inflammation, reducing discharge, and restoring the skin or mucous membranes to their normal appearance. The visible resolution of symptoms is the primary indicator of successful treatment for candidiasis, often documented through subsequent pictures. The speed of visible improvement can vary depending on the severity and location of the infection, as well as the chosen treatment modality. Both topical and systemic antifungal medications are used, and each has a characteristic effect on the visual presentation of the infection as it heals.
Visual Resolution with Topical Antifungals
Topical antifungal creams, ointments, powders, or solutions are commonly used for superficial yeast infections like candidal intertrigo, diaper rash, and mild vaginal or penile infections. Visually, within a few days of starting treatment, one typically observes a reduction in the intense redness and inflammation. The skin becomes less fiery and starts to fade to a lighter pink. Any maceration or weeping will begin to dry out, and the skin will look less shiny and less irritated. Satellite lesions, if present, are usually the first to resolve, disappearing as the yeast population is brought under control. The characteristic discharge of vaginal or penile candidiasis will also visibly decrease in volume and lose its thick, clumpy consistency, returning to a more normal appearance. The skin will start to heal, with any fissures or erosions gradually closing and the skin texture becoming smoother and less inflamed. It’s important to continue treatment for the full prescribed duration, even after visual symptoms improve, to prevent recurrence.
- Decreased Redness: Fading of the intense erythema to a lighter pink or normal skin tone.
- Reduced Swelling: Diminishment of edema in affected tissues (e.g., vulva, glans, skin folds).
- Drying of Maceration: Resolution of the soggy, whitish appearance, with skin becoming drier.
- Disappearance of Satellite Lesions: Rapid fading and resolution of smaller papules or pustules.
- Normalization of Discharge: Reduction in thick, clumpy discharge, returning to normal appearance.
- Healing of Fissures/Erosions: Visible closure and smoothing of skin cracks and raw areas.
- Reduced Scaling/Flaking: Skin texture becomes smoother and less desquamated.
Visual Resolution with Oral Antifungals
Systemic antifungal medications, taken orally, are typically reserved for more severe, widespread, or recurrent yeast infections, such as extensive oral thrush, invasive candidiasis, or stubborn vaginal or penile infections that don’t respond to topicals. The visual changes seen with oral antifungal treatment are often more rapid and comprehensive. For oral thrush, the creamy white patches will visibly start to recede and become easier to wipe away, eventually disappearing completely, revealing healthy-looking pink mucosa underneath. The underlying redness and inflammation will also subside. For systemic skin candidiasis, the widespread redness, satellite lesions, and pustules will visibly diminish across all affected body areas. The skin will look less inflamed, less shiny, and begin to return to its normal color and texture. Discharge from vaginal or penile infections will also clear up quickly. Oral medications target the yeast internally, leading to a more generalized and often quicker resolution of visible symptoms, including those not easily reached by topical treatments. This rapid visual improvement can be reassuring to patients.
- Rapid Clearing of Patches: Oral thrush lesions visibly reduce and disappear quickly, revealing healthy mucosa.
- Generalized Reduction in Redness: Widespread fading of erythema across all affected skin areas.
- Comprehensive Lesion Resolution: Disappearance of satellite lesions, pustules, and other specific candidal features over larger areas.
- Normalization of Mucosa: Oral tissues revert to a healthy pink appearance without signs of inflammation.
- Full Resolution of Discharge: Complete clearing of any abnormal discharge associated with vaginal or penile candidiasis.
- Improved Skin Texture: Skin becomes smoother, less inflamed, and less prone to maceration or peeling.
Preventive Measures and Their Visual Impact
Preventative measures also have a direct impact on the visual presentation of skin and mucosal health, by preventing the recurrence of yeast infections. By maintaining good hygiene, ensuring skin folds are kept dry, and wearing breathable clothing, individuals can avoid the conditions that visually manifest as candidal intertrigo or diaper rash. For instance, promptly changing diapers prevents the prolonged moisture and irritation that visually precedes candidal diaper dermatitis. For individuals prone to vaginal yeast infections, avoiding tight clothing and certain irritants helps maintain a visually healthy vulvar and vaginal environment, free from redness and discharge. Controlling underlying conditions like diabetes visually prevents the widespread inflammatory skin and mucosal changes associated with chronic candidiasis. The visual absence of the described symptoms is a strong indicator that preventive strategies are effective. Adherence to these measures helps maintain visually healthy, intact skin and mucous membranes, preventing the tell-tale signs of a yeast overgrowth from ever appearing or returning, thus maintaining optimal skin integrity and comfort. The visual goal of prevention is a clear, unblemished, and non-inflamed appearance of all areas susceptible to yeast growth.
- Maintained Dryness: Prevents the visible maceration and redness in skin folds.
- Healthy Skin Barrier: Intact, uncompromised skin visually resists yeast invasion.
- Clear Mucous Membranes: Absence of white patches or abnormal discharge in oral or genital areas.
- No Recurrent Redness/Inflammation: Prevention of repeat erythema and swelling in prone areas.
- Intact Skin Folds: Visually healthy, non-irritated, and uncracked skin in intertriginous zones.
- Normal Skin Color/Texture: Absence of the fiery red, shiny, or peeling appearance characteristic of yeast rashes.